Abstract
The ε4 allele of the APOE gene is thought to increase risk from amnestic mild cognitive impairment (aMCI) to Alzheimer’s disease. Cognitive decline in the condition is increasingly considered to worsen functional disconnections in brain network composed of gray matter and white matter. Nevertheless, Whether APOEε4 targets specific white matter functional connectivity in patients with aMCI remains mostly unexplored, mainly due to the challenges of detecting BOLD signals in white matter. Here, we applied a novel approach to investigate APOEε4-related specific bundles and cortical area alterations in aMCI subjects, in order to characterize white matter-gray matter functional connectivity differences throughout the brain. We analyzed 75 patients with aMCI and 76 demographically matched normal controls. The aMCI APOEε4 carriers showed decreased functional connectivity located at left corticospinal tract, bilateral posterior limb of internal capsule, and right temporopolaris, which was different from the regions of aMCI-related changes. We further found that recognition scores were positively associated with the right temporopolaris in aMCI APOEε4 carriers. Collectively, the data provide new evidence that APOEε4 genotype exerts a negative impact on neural activity in both gray and white matter in aMCI, which potentially contributes to functional disconnection and memory decline. A novel method provides full-scale measuring effect of disease conditions on functional architecture throughout the brain. Trial registration: https://www.ClinicalTrials.gov (Identifier: NCT02225964). Registered January 2014.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Alzheimer’s disease (AD) is a common neurodegenerative disorder manifested as cognitive disability and serious loss of daily living abilities for the elderly. Given the prevalence of this disorder, which imposes enormous socioeconomic burden on both the family and the society (Jia et al. 2019), and that there have been no effective treatment to date, early diagnosis and management have become highly imperative. Amnestic mild cognitive impairment (aMCI) is an early stage of AD, a condition in which people experience more severe memory loss than their age but their daily life has not yet been affected. It is an intermediate state between normal cognitive aging and dementia, about 10–15% of which will eventually convert to AD dementia.
It has long been established that the human Apolipoprotein E (APOE) gene has three gene types (APOEε2, APOEε3, APOEε4) and APOEε4 has been confirmed to be related to an increased risk for developing AD (Yamazaki et al. 2019). It is now clear that brain disconnection is a dominant feature of cognitive dysfunction (Veitch et al. 2019), in which white matter (WM) plays an important role since it is essential for efficient neurotransmission across cortical and subcortical regions. WM also experiences a series of alterations during the process of aging (Liu et al. 2017), which necessarily contributes to cognitive decline.
Notwithstanding a plethora of studies on brain structure and function that have been conducted during the past decades, none of them have focused on how the APOEε4 allele modulates WM from the functional perspective. WM has been widely recognized as being nourished by much less oxygenated blood and thus tends to generate much weaker BOLD signals in response to neural events (Gawryluk et al. 2014). However, it should be noted that the oxygen extraction fractions of WM are comparable to that of gray matter (GM) (Raichle et al. 2001). Moreover, in the low frequency range 0.01–0.1 Hz in a resting state, researchers can also measure significant fluctuations of BOLD signal in WM (Gore et al. 2019). In fact, there has been growing evidences suggesting that resting state BOLD signals in WM are reliably detectable by applying appropriate methods (Farago et al. 2019, Li et al. 2019a, b). To date, resting state fMRI has been utilized to explore functional connectivity in WM (Li et al. 2019b) or between WM and GM (Peer et al. 2017) and how the functional connectivity in WM was altered by pathology, such as pontine stroke (Wang et al. 2019), Parkinson’s disease (Ji et al. 2019), Alzheimer’s disease (Zhao et al. 2020), schizophrenia (Yang et al. 2019, Fan et al. 2020), epilepsy (Jiang et al. 2019), and migraine (Farago et al. 2019).
Recently Ding et al. proposed a graph based framework to define functional connectivity of WM bundles with segmented cortical volumes and measure alterations in WM functional connectivity (Ding et al. 2018, Gore et al. 2019), which offers a novel standardized tool for studying changes of functional connectivity in WM in disease conditions. In the present study, we employ this new framework to characterize WM-GM functional connectivity differences throughout the brain in APOEε4 non-carriers (aMCI vs. normal controls) and in aMCI (APOEε4 carriers vs. non-carriers). The purpose of this investigation is, to characterize functional connectivity profile in GM and WM underlying aMCI and APOE genotype, which may potentially provide novel biomarkers for early screening of population at great risk for AD.
Methods
Participants
All participants in the present study, including 151 right-handed Han Chinese subjects (75 aMCI and 76 normal controls (NC) ), were recruited from Xuanwu Hospital of Capital University. The diagnosis of aMCI met the following criteria (Albert et al. 2011): (1) the Han nationality, right-handed (the Edinburgh handedness scale score > 40 points); (2) subjective memory declined complaint; (3) objective memory impairments (below or equal to 1.5 SD of age- and education- adjusted norms on the memory tests); (4) total Clinical Dementia Rating (CDR) score ≤ 0.5; (5) independent activities of daily living. Individuals with no memory or other cognitive complaints, normal performance on standardized cognitive tests as well as a CDR score of 0 were included as NC. The exclusion criteria were as follows: (1) suffered from stroke; (2) Hamilton Depression Rating Scale score greater than or equal to 24 points; (3) other nervous system or systemic diseases, causing cognitive impairment; (4) contraindications for MRI; (5) a history of psychosis or congenital mental growth retardation.
Participants underwent a clinical screening questionnaire and a battery of neuropsychological tests (MMSE, MoCA, AVLT and CDR), had blood work taken, and received a functional MRI. APOE genotyping was performed according to the standard methods (Sanger, Shanghai, China). Participants who had one or more ε4 allele were assigned to APOEε4 carriers (APOEε4+), while those with an ε3 homozygote were assigned to APOEε4 non-carriers (APOEε4-). Individuals with the ε2 allele were excluded. After matching NC with aMCI on age and gender, we obtained a sample of 151 subjects: 38 aMCI APOEε4+, 37aMCI APOEε4-, and 76 NC APOEε4- subjects. Participants’ demographic information, their cognitive performance and APOE status are summarized in Table 2. The study was approved by the Medical Research Ethics Committee of Xuanwu Hospital of Capital University. The written informed consent was obtained from each patient and NC subject before study.
Functional imaging
Image acquisition
All participants were scanned on either a 3.0 T MRI scanner (Magnetom Tim Trio; Siemens, Erlangen, Germany) or 3.0 T TOF PET/MR scanner (Signa PET/MR, GE Healthcare, WI, USA). Resting-state fMRI images were acquired using a gradient-echo echo-planar imaging sequence: TR = 3000 ms, TE = 30 ms, flip angle = 90, matrix = 64 × 64, voxel size = 3.0 × 3.0 × 3.48 mm3, gap = 0 mm, number of slices = 43, 124 time points. During resting-state fMRI, subjects were asked to lie quietly with their eyes open without performing any functional tasks. As anatomical references, T1-weighted images were acquired in axial planes, using 3D magnetization-prepared rapid gradient-echo sequence (MP-RAGE) sequences with repetition time (TR) = 1600 msec, echo time (TE) = 2.15 msec, flip angle = 9,voxel size 1.0 × 1.0 × 1.0 mm3, field of view 256 × 256, slice thickness = 1 mm,no gap on the Siemens scanner (Sun et al. 2016), and repetition time/echo time = 6.9 ms/2.98 ms, flip angle = 12°, inversion time = 450 ms, field of view = 256 × 256 mm2, matrix = 256 × 256,slice thickness = 1 mm, no interslice gap, and voxel size = 1 × 1 × 1 mm3 on the GE scanner (Li et al. 2019c). To exclude possible scanner-specified effects on the data, scanners types were treated as covariates in the statistical analysis.
Image preprocessing
The functional data were preprocessed using the spm12 toolbox (http://www.fil.ion.ucl.ac.uk/spm/software/spm12). The detail of the pipeline can be found in Ding et al. (Ding et al. 2018). Briefly, the fMRI images were corrected for slice timing differences and head movements. Next, the T1-weighted images were co-registered to the fMRI data and were subsequently segmented into GM, WM, and CSF. Further, the co-registered T1 image was spatially normalized to the Montreal Neurological Institute (MNI) space, along with the anatomical segments and the fMRI images. Linear regression was performed to remove the signal drifting of the voxel-wise time courses of the normalized fMRI data. Finally, the time courses were filtered by a band-pass filter (0.01–0.1 Hz). All registration results were assessed by visually inspecting the output pictures from DPABI(Data Processing & Analysis for (Resting-State) Brain Imaging, DPABI) (Yan et al. 2016) toolbox for quality control of normalizations. Any mis-registered subject was resent to the pipeline and manually set the landmark point (anterior commissure) for the initialization of the registration.
Region of interest definitions and image analysis
GM and WM regions of interest definitions in this study were based on the conceptual framework proposed by Ding et al. (Ding et al. 2018). The GM was parcellated into 82 regions (41 in each hemisphere) on the basis of Brodmann’s definitions (https://www.nitrc.org/projects/wfu_pickatlas/). Meanwhile, 48 bundle regions (21 bundles in each hemisphere and 6 commissure bundles, Table 1) were constructed from the JHU ICBM-DTI-81 WM atlas (Mori et al. 2008). In addition, all bundle regions were further constrained within each subject’s WM mask threshold tightly at 0.95, so as to avoid partial volume effects from nearby GM regions. Finally, BOLD signals were averaged across voxels within each of the GM regions and WM bundles defined above to produce a mean time series, which was subsequently used to derive pairwise temporal correlations between these GM regions and WM bundles.
Statistical analysis
All statistical analyses were performed with SPSS (v. 20, IBM, Armonk, NY). Two-tailed t-test was used for comparing the group differences in demographic variables and cognitive performance. Categorical variables were analyzed by the chi-square test. To compare the group differences in correlation coefficients of BOLD signals in the GM region and WM bundle, One-way ANOVAs were performed with age, gender, years of education, and scanner type as covariates. Multiple comparisons were corrected by using the two-sample t tests with a false-positive correction P<(1/48) for WM bundles and P<(1/82) for GM regions (Lynall et al. 2010).To determine the relationships between the imaging data and neuropsychological variables, a partial correlation analysis was conducted in aMCI APOEε4 carriers and non-carriers group. Age, gender and education level were considered as covariates. P < 0.05 is considered significant.
Results
Demographics and behavioral measures
Based on evidence that effects of APOE genotype on cognition differences are inconsistent, we examined the performance of neuropsychological tests in aMCI APOEε4 carriers and non-carriers, specifically memory dimensions (immediate recall, delayed recall and recognition). There were significantly poorer scores in AVLT-immediate recall and AVLT-recognition (all P < 0.05) in aMCI APOEε4 carriers (Table 2). These findings suggest that APOE genotype modulates brain function.
WM-GM functional connectivity in aMCI
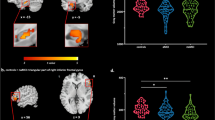
We firstly investigated the aMCI-related abnormality of WM-GM functional connectivity in APOEε4 non-carriers (aMCI vs. NC) (Fig. 1). Compared with NC, the aMCI APOEε4- group showed decreased functional connectivity in left praeparietalis, as well as increased correlation coefficient in right retrolimbica granularis (Fig. 2a) (P < 0.05). There was no significant difference in WM functional connectivity between the two groups (Fig. 2b). These findings demonstrate that the aMCI-related functional connectivity abnormality mainly in GM.
The effect of aMCI on the temporal correlations in BOLD signals between WM bundles and GM regions in APOEε4 non-carriers. Average maps(A,B); Difference maps(C,D). A and B panels are for the aMCI and NC group, respectively. C panel: aMCI group are smaller than NC in functional connectivity. D panel: NC group are greater than aMCI in functional connectivity. Hot colors (red and yellow) denote positive differences
WM-GM functional connectivity differences by APOEε4 genotype
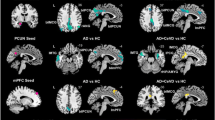
We next evaluated the impact of the APOEε4 genotype on WM-GM functional connectivity in aMCI (APOε4 + vs. APOε4-) (Fig. 3). Figure 3a and b show average maps of WM-GM functional connectivity for the aMCI APOε4 + group (3A) and aMCI APOEε4- group (3B). The differences between the two groups are given in Fig. 3c and d, with 3C showing WM-GM functional connectivity of the aMCI APOε4 + group smaller than that of aMCI APOEε4- and 3D showing WM-GM functional connectivity of the aMCI APOε4- group greater than that of aMCI APOEε4+. Figure 4 shows the significant differences in specific GM and WM tracts functional areas between the two groups (P < 0.05). Relative to the non-carriers, the aMCI APOEε4 carriers demonstrated significantly reduced functional connectivity of GM in the bilateral temporal lobe, frontal lobe, retrolimbica agranularis, as well as in right visual cortex and praeparietalis (Fig. 4a). Besides, the functional connectivity of WM was decreased in bilateral posterior limb of internal capsule, external capsule, and superior fronto- occipital fasciculus, right uncinate fasciculus and superior cerebellar peduncle, left corticospinal tract, and pontine crossing tract (Fig. 4b). Furthermore, there were significant differences of functional connectivity in right temporopolaris, left corticospinal tract, and bilateral posterior limb of internal capsule (corrected). It is apparent from the observations that the aMCI-related decrease in WM-GM functional connectivity seems to aggravate in APOEε4 carriers.
The effect of APOEε4 on the temporal correlations in BOLD signals between WM bundles and GM regions in aMCI. Average maps(A,B); Difference maps(C,D). A and B panels are for the aMCI APOEε4 carriers and non-carriers, respectively. C panel: aMCI APOEε4 carriers are smaller than non-carriers in functional connectivity. D panel: aMCI APOEε4 non-carriers are greater than carriers in functional connectivity. Hot colors (red and yellow) denote positive differences
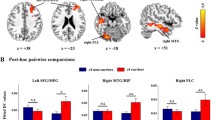
Differences between aMCI APOEε4 carriers (red) and non-carriers(green) in the averaged correlations in the GM region (A) and WM bundle (B). One stars (*) denote P < 0.05 from paired and two tailed t tests of Z score of the mean correlation coefficient. Two stars (**) denote*significant differences with correction
Relation of difference regions by APOEε4 genotype with neuropsychological measures
To better assess whether APOEε4 allelic load modulates the association between WM-GM functional connectivity and cognitive performance, correlations were sought between the functional connectivity in the above four regions (corrected) and scores of neuropsychological tests in aMCI APOEε4 carriers and non-carriers respectively. In aMCI APOEε4 carriers group, a positive correlation was found between AVLT-recognition scores and the averaged correlation coefficient in the right temporopolaris (Fig. 5, P < 0.05), but no significant correlation in aMCI APOEε4 non-carriers group (Fig. 5, P = 0.615). These findings indicate that APOEε4 allelic exerts negative effects on brain function serving word recognition in aMCI.
Discussion
The present study was designed to determine the effect of APOEε4 genotype on WM-GM functional connectivity in aMCI patients. To our knowledge this is the first study that investigates alterations of WM functional connectivity in aMCI APOEε4 carriers and non-carriers. Experiments from this study show that decreased functional connectivity by APOEε4 genotype is located at the right temporopolaris, left corticospinal tract, and bilateral posterior limb of internal capsule, which differs from the regions of aMCI-related changes. Moreover, there is a significant positive correlation between AVLT-recognition scores and decreased functional connectivity in the right temporopolarisis in aMCI APOEε4 carriers.
Lower immediate and recognition memory scores were found in the aMCI APOEε4 carriers than in the non-carriers, indicating worse memory impairment in the carriers. This observation is similar to previous studies (Whitehair et al. 2010). Kerchner et al. revealed that there was a negative effect of APOEε4 carrier status on delayed recall and recognition scores in aMCI (Kerchner et al. 2014). Not only MCI or AD but also cognitively healthy APOEε4 carriers exhibit worse cognitive scores and accelerated memory decline (O’Donoghue et al. 2018, Fan et al. 2019).
We found a significant difference in functional connectivity between aMCI APOE ε4 carriers and non-carriers in the right temporopolaris. The APOE ε4 allele contributes to reduced functional connectivity in this region in aMCI. To date, the cortical regions affected by APOEɛ4 allele are not identical. Several MRI studies suggest that the APOEε4 is associated with hippocampus, surrounding medial temporal lobe structures (Suridjan et al. 2015, Cacciaglia et al. 2018). In fact, temporopolaris is interconnected with hippocampus, entorhinal, and parahippocampal cortices, which is crucial for memory processe.The effective connectivity between the right temporopolaris and left anterior hippocampus supports the integration of episodic memory (Pehrs et al. 2018). We also demonstrate that decreased functional connectivity in the right temporopolaris correlated positively with AVLT-recognition scores in aMCI APOEε4 carriers. Recognition performance has been found sensitive to early memory decline (Smirni et al. 2019) and progression from aMCI to AD (De Simone et al. 2019). It may be unified with findings from other studies in which the medial temporal lobes and other brain structures make up a large-scale episodic memory network for successful memory processing.
It is interesting to observe that decreased WM functional connectivity is located at left corticospinal tract and bilateral posterior limb of internal capsule in aMCI APOEε4 carriers. The physiological basis of the functional changes in WM is presently not understood. BOLD effects in WM may reflect vascular responses to the need of neurotransmission in WM or physical coupling with cortical vascular changes (Gore et al. 2019). Many studies of aging brains observed WM tract disruption, increased inflammation, dilation of the perivascular space, and demyelination (Liu et al. 2017, Weiner et al. 2017). These changes in WM may influence intrinsic signal transduction and contributes to cognitive impairment. The precise mechanism by which APOEε4 is associated with the WM damage remains unclear. Evidence suggests that APOEε4 has been linked to Aβ deposition and triggers Tau phosphorylation (Slot et al. 2019), which likely disrupts WM in AD that impacts neurovascular coupling therein (Liu et al. 2019). Impaired WM integrity in the cingulum bundle and fornix were also observed in AD (Kantarci et al. 2017) and MCI (Metzler-Baddeley et al. 2012), while corticospinal tracts were relatively preserved (Lee et al. 2015). A diffusion tensor imaging study has shown moderate effects of APOEε4 on WM integrity in the vicinity of the lentiform nucleus in NC, but not in AD (Kljajevic et al. 2014). In a multicenter European DTI study, lower FA values in the inferior fronto-occipital, corpus callosum, and internal and external capsule were observed in the APOE4 carriers of elderly individuals compared to noncarriers. Compared to the findings from the DTI study, our analysis indicated decreased functional connectivity in the left corticospinal tract and bilateral posterior limb of internal capsule in aMCI APOEε4 carriers as compared to non-carriers. While there is convergence between the two studies, there is also discrepancy between them, which may arise from different sensitivities of the two imaging modalities. Nonetheless, the discrepancy attests to the complementary nature of DTI and fMRI, and our new findings provide novel insights into the manner by which WM functionality is affected by APOEε4 in aMCI.
It should be mentioned that this research comes with a few limitations. First, the small sample sizes used in this study limit to draw any firm conclusions and should be viewed cautiously. In addition, we are unable to separate APOEε4 dose subgroups in this work, which would require much large sample sizes. Indeed, the infrequent occurrence of APOEε4 in the population has resulted in small APOEε4 samples in most neuroimaging studies (O’Donoghue et al. 2018). In future studies, large imaging datasets should be acquired for examining the reproducibility of the results. Second, the APOEε4 + group in normal control was not available in this study because of the low APOEε4 carrier prevalence in healthy individuals. Thus, we were unable to compare the potential interaction effects of aMCI and APOEε4 on WM-GM functional connectivity. Third, data acquisitions using different MRI scanners may in principle increase inter-subject variance and adversely affect the confidence of the results. To control for discrepancies between data, we compared the difference in raw data between two MRI scanners prior to the study and no significant difference was found. To further ameliorate the potential confound, the data were statistically analyzed with scanner types as covariates. Finally, there are some common concerns on WM BOLD studies, which include the potential effect of partial volume averaging, temporal resolution of BOLD time series, or other confounding factors such as head motion, signal drifting, and cardiopulmonary fluctuations. In spite of large efforts that have been made to minimize these effects (Ding et al. 2018), they could not be removed entirely from our data.
Conclusions
In conclusion, the current study identifies decreased activity in specific WM tracts and GM regions in aMCI APOEε4 carriers. Recognition memory deficit is positively correlated with APOE-related GM vulnerabilities in patients with aMCI. Our findings support the notion that it would be important to examine the functional aspects of WM to extend and deepen our understanding of pathophysiological mechanisms by which AD evolves, which may hold the potential to offer new approaches for therapeutic interventions of the disease.
References
Albert, M. S., DeKosky, S. T., Dickson, D., Dubois, B., Feldman, H. H., Fox, N. C., Gamst, A., Holtzman, D. M., Jagust, W. J., Petersen, R. C., Snyder, P. J., Carrillo, M. C., Thies, B., & Phelps, C. H. (2011). The diagnosis of mild cognitive impairment due to Alzheimer’s disease: recommendations from the National Institute on Aging-Alzheimer’s Association workgroups on diagnostic guidelines for Alzheimer’s disease. Alzheimer’s & Dementia, 7(3), 270–279.
Cacciaglia, R., Molinuevo, J. L., Falcon, C., Brugulat-Serrat, A., Sanchez-Benavides, G., Gramunt, N., Esteller, M., Moran, S., Minguillon, C., Fauria, K., Gispert, J. D. and A. study (2018). Effects of APOE-epsilon4 allele load on brain morphology in a cohort of middle-aged healthy individuals with enriched genetic risk for Alzheimer’s disease. Alzheimer’s & Dementia 14(7): 902–912.
De Simone, M. S., Perri, R., Fadda, L., Caltagirone, C., & Carlesimo, G. A. (2019). Predicting progression to Alzheimer’s disease in subjects with amnestic mild cognitive impairment using performance on recall and recognition tests. Journal of Neurology, 266(1), 102–111.
Ding, Z., Huang, Y., Bailey, S. K., Gao, Y., Cutting, L. E., Rogers, B. P., Newton, A. T., & Gore, J. C. (2018). Detection of synchronous brain activity in white matter tracts at rest and under functional loading. Proceedings of the National Academy of Sciences 115(3), 595–600.
Fan, J., Tao, W., Li, X., Li, H., Zhang, J., Wei, D., Chen, Y., & Zhang, Z. (2019). The Contribution of Genetic Factors to Cognitive Impairment and Dementia: Apolipoprotein E Gene, Gene Interactions, and Polygenic Risk. International Journal of Molecular Sciences, 20(5).
Fan, Y. S., Li, Z., Duan, X., Xiao, J., Guo, X., Han, S., et al. (2020). Impaired interactions among white-matter functional networks in antipsychotic-naive first-episode schizophrenia. Human Brain Mapping, 41(1), 230–240.
Farago, P., Toth, E., Kocsis, K., Kincses, B., Vereb, D., Kiraly, A., et al. (2019). Altered resting state functional activity and microstructure of the white matter in migraine with aura. Frontiers in Neurology, 10, 1039.
Gawryluk, J. R., Mazerolle, E. L., & D’Arcy, R. C. (2014). Does functional MRI detect activation in white matter? A review of emerging evidence, issues, and future directions. Frontiers in Neurology, 8, 239.
Gore, J. C., Li, M., Gao, Y., Wu, T. L., Schilling, K. G., Huang, Y., et al. (2019). Functional MRI and resting state connectivity in white matter - a mini-review. Magnetic Resonance Imaging, 63, 1–11.
Ji, G. J., Ren, C., Li, Y., Sun, J., Liu, T., Gao, Y., et al. (2019). Regional and network properties of white matter function in Parkinson’s disease. Human Brain Mapping, 40(4), 1253–1263.
Jia, L., Quan, M., Fu, Y., Zhao, T., Li, Y., Wei, C., Tang, Y., Qin, Q., Wang, F., Qiao, Y., Shi, S., Wang, Y. J., Du, Y., Zhang, J., Zhang, J., Luo, B., Qu, Q., Zhou, C., Gauthier, S., Jia, J. & C. Group for the Project of Dementia Situation in (2019). Dementia in China: epidemiology, clinical management, and research advances. Lancet Neurology.
Jiang, Y., Song, L., Li, X., Zhang, Y., Chen, Y., Jiang, S., et al. (2019). Dysfunctional white-matter networks in medicated and unmedicated benign epilepsy with centrotemporal spikes. Human Brain Mapping, 40(10), 3113–3124.
Kantarci, K., Murray, M. E., Schwarz, C. G., Reid, R. I., Przybelski, S. A., Lesnick, T., et al. (2017). White-matter integrity on DTI and the pathologic staging of Alzheimer’s disease. Neurobiology of Aging, 56, 172–179.
Kerchner, G. A., Berdnik, D., Shen, J. C., Bernstein, J. D., Fenesy, M. C., Deutsch, G. K., Wyss-Coray, T., & Rutt, B. K. (2014). APOE epsilon4 worsens hippocampal CA1 apical neuropil atrophy and episodic memory. Neurology, 82(8), 691–697.
Kljajevic, V., Meyer, P., Holzmann, C., Dyrba, M., Kasper, E., Bokde, A. L., Fellgiebel, A., Meindl, T., Hampel, H., Teipel, S. and E. s. group (2014). The epsilon4 genotype of apolipoprotein E and white matter integrity in Alzheimer’s disease. Alzheimers Dement, 10(3), 401–404.
Lee, S. H., Coutu, J. P., Wilkens, P., Yendiki, A., Rosas, H. D., Salat, H. D., & I. Alzheimer’s disease Neuroimaging. (2015). Tract-based analysis of white matter degeneration in Alzheimer’s disease. Neuroscience, 301, 79–89.
Li, J., Biswal, B. B., Wang, P., Duan, X., Cui, Q., Chen, H., & Liao, W. (2019a). Exploring the functional connectome in white matter. Human Brain Mapping, 40(15), 4331–4344.
Li, M., Newton, A. T., Anderson, A. W., Ding, Z., & Gore, J. C. (2019b). Characterization of the hemodynamic response function in white matter tracts for event-related fMRI. Nature Communications, 10(1), 1140.
Li, X., Wang, X., Su, L., Hu, X., & Han, Y. (2019c). Sino Longitudinal Study on Cognitive Decline (SILCODE): protocol for a Chinese longitudinal observational study to develop risk prediction models of conversion to mild cognitive impairment in individuals with subjective cognitive decline. British Medical Journal Open, 9(7), e028188.
Liu, H., Yang, Y., Xia, Y., Zhu, W., Leak, R. K., Wei, Z., et al. (2017). Aging of cerebral white matter. Ageing Research Reviews, 34, 64–76.
Liu, X., Hou, D., Lin, F., Luo, J., Xie, J., Wang, Y., & Tian, Y. (2019). The role of neurovascular unit damage in the occurrence and development of Alzheimer’s disease. Reviews in the Neurosciences, 30(5), 477–484.
Lynall, M. E., Bassett, D. S., Kerwin, R., McKenna, P. J., Kitzbichler, M., Muller, U., & Bullmore, E. (2010). Functional connectivity and brain networks in schizophrenia. The Journal of Neuroscience, 30(28), 9477–9487.
Metzler-Baddeley, C., Hunt, S., Jones, D. K., Leemans, A., & Aggleton, J. P. and M. J. O’Sullivan (2012). Temporal association tracts and the breakdown of episodic memory in mild cognitive impairment. Neurology 79(23), 2233–2240.
Mori, S., Oishi, K., Jiang, H., Jiang, L., Li, X., Akhter, K., Hua, K., Faria, A. V., Mahmood, A., Woods, R., Toga, A. W., Pike, G. B., Neto, P. R., Evans, A., Zhang, J., Huang, H., Miller, M. I., van Zijl, P., & Mazziotta, J. (2008). Stereotaxic white matter atlas based on diffusion tensor imaging in an ICBM template. Neuroimage, 40(2), 570–582.
O’Donoghue, M. C., Murphy, S. E., Zamboni, G., Nobre, A. C., & Mackay, C. E. (2018). APOE genotype and cognition in healthy individuals at risk of Alzheimer’s disease: A review. Cortex; A journal devoted to the study of the nervous system and behavior, 104, 103–123.
Peer, M., Nitzan, M., Bick, A. S., Levin, N., & Arzy, S. (2017). Evidence for functional networks within the human brain’s white matter. The Journal of Neuroscience, 37(27), 6394–6407.
Pehrs, C., Zaki, J., Taruffi, L., Kuchinke, L., & Koelsch, S. (2018). Hippocampal-temporopolar connectivity contributes to episodic simulation during social cognition. Scientific Reports, 8(1), 9409.
Raichle, M. E., MacLeod, A. M., Snyder, A. Z., Powers, W. J., Gusnard, D. A., & Shulman, G. L. (2001). A default mode of brain function. Proceedings of the National Academy of Sciences of the United States of America, 98(2), 676–682.
Slot, R. E. R., Kester, M. I., Van Harten, A. C., Jongbloed, W., Bouwman, F. H., Teunissen, C. E., et al. (2019). ApoE and clusterin CSF levels influence associations between APOE genotype and changes in CSF tau, but not CSF Abeta42, levels in non-demented elderly. Neurobiology of Aging, 79, 101–109.
Smirni, D., Smirni, P., Di Martino, G., Fontana, M. L., Cipolotti, L., Oliveri, M., & Turriziani, P. (2019). Early detection of memory impairments in older adults: standardization of a short version of the verbal and nonverbal Recognition Memory Test. Neurological Sciences , 40(1), 97–103.
Sun, Y., Dai, Z., Li, Y., Sheng, C., Li, H., Wang, X., et al. (2016). Subjective cognitive decline: Mapping functional and structural brain changes-a combined resting-state functional and structural MR imaging study. Radiology, 281(1), 185–192.
Suridjan, I., Pollock, B. G., Verhoeff, N. P., Voineskos, A. N., Chow, T., Rusjan, P. M., et al. (2015). In-vivo imaging of grey and white matter neuroinflammation in Alzheimer’s disease: a positron emission tomography study with a novel radioligand, [18F]-FEPPA. Molecular Psychiatry, 20(12), 1579–1587.
Veitch, D. P., Weiner, M. W., Aisen, P. S., Beckett, L. A., Cairns, N. J., Green, R. C., Harvey, D.,Jack, C. R. Jr., Jagust, W., Morris, J. C., Petersen, R. C., Saykin, A. J., Shaw, L. M., Toga, A. W.,Trojanowski, J. Q. & I.Alzheimer'sDiseaseNeuroimaging. (2019). Understanding disease progression and improving Alzheimer’s disease clinical trials: Recent highlights from the Alzheimer’s Disease Neuroimaging Initiative. Alzheimer’s & Dementia, 15(1), 106–152.
Wang, J., Yang, Z., Zhang, M., Shan, Y., Rong, D., Ma, Q., et al. (2019). Disrupted functional connectivity and activity in the white matter of the sensorimotor system in patients with pontine strokes. Journal of Magnetic Resonance Imaging, 49(2), 478–486.
Weiner, M. W., Veitch, D. P., Aisen, P. S., Beckett, L. A., Cairns, N. J., Green, R. C., et al. (2017). Recent publications from the Alzheimer’s Disease Neuroimaging Initiative: Reviewing progress toward improved AD clinical trials. Alzheimer’s & Dementia, 13(4), e1–e85.
Whitehair, D. C., Sherzai, A., Emond, J., Raman, R., Aisen, P. S., Petersen, R. C., et al. (2010). Influence of apolipoprotein E varepsilon4 on rates of cognitive and functional decline in mild cognitive impairment. Alzheimer’s & Dementia, 6(5), 412–419.
Yamazaki, Y., Zhao, N., Caulfield, T. R., Liu, C. C., & Bu, G. (2019). Apolipoprotein E and Alzheimer disease: pathobiology and targeting strategies. Nature Reviews Neurology, 15(9), 501–518.
Yan, C. G., Wang, X. D., Zuo, X. N., & Zang, Y. F. (2016). DPABI: data processing & analysis for (Resting-State) brain imaging. Neuroinformatics, 14(3), 339–351.
Yang, C., Zhang, W., Yao, L., Liu, N., Shah, C., Zeng, J., Yang, Z., Gong, Q., & Lui, S. (2019). Functional Alterations of White Matter in Chronic Never-Treated and Treated Schizophrenia Patients. Journal of Magnetic Resonance Imaging.
Zhao, J., Du, Y. H., Ding, X. T., Wang, X. H., & Men, G. Z. (2020). Alteration of functional connectivity in patients with Alzheimer’s disease revealed by resting-state functional magnetic resonance imaging. Neural Regeneration Research, 15(2), 285–292.
Acknowledgements
We thank the dedicated participants and staff of Xuanwu Hospital for data collection, including Yu Sun, Xiaoni Wang, Guanqun Chen, Weina Zhao, Bin Mu, Ziqi Wang, Yuxia Li, Ying Chen, Xuanyu Li, Wenying Du, Jiachen Li, Xing Zhao, Qin Yang, Xiaoqi Wang, Jun Wang, and Liu Yang.
Funding
This work was supported by The National Key Research and Development Program of China (2016YFC1306300, 2018YFC1312001), National Natural Science Foundation of China (Grant 61633018, 81871438).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest and disclosure
No conflict of interest.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Lin, H., Li, M., Zhan, Y. et al. Disrupted white matter functional connectivity in aMCI APOEε4 carriers: a resting-state study. Brain Imaging and Behavior 15, 1739–1747 (2021). https://doi.org/10.1007/s11682-020-00367-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11682-020-00367-7