Abstract
Objective
To explore the demographic and disease-related factors associated with acupuncture response in patients with chronic tension-type headache (CTTH).
Methods
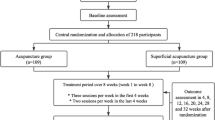
Using data from a randomized clinical trial (218 cases) consisting of 4 weeks of baseline assessment, 8 weeks of treatment, and 24 weeks of follow-up, participants were regrouped into responders (at least a 50% reduction in monthly headache days at week 16 compared with baseline) and non-responders. Twenty-three demographic and disease-related factors associated with acupuncture response in 183 participants were analyzed by multivariable logistic regression.
Results
One hundred and nineteen (65.0%) participants were classified as responders. Four factors were significantly independently associated with acupuncture response, including treatment assignment, headache intensity at baseline, and 2 domains [general health (GH) and social functioning (SF)] from the 36-Item Short Form Health Survey quality of life questionnaire. Treatment assignment was associated with non-response: participants receiving true acupuncture were 3-time more likely to achieve a CTTH response than those receiving superficial acupuncture [odds ratio (OR) 0.322, 95% confidence interval (CI) 0.162 to 0.625, P=0.001]. Compared with patients with mild-intensity headache, patients with moderate-intensity headache were twice as likely to respond to acupuncture (OR 2.001, 95% CI 1.020 to 4.011, P=0.046). The likelihood of non-response increased by 4.5% with each unit increase in the GH grade (OR 0.955, 95% CI 0.917 to 0.993, P=0.024) while decreased by 3.8% with each unit increase in the SF grade (OR 1.038, 95% CI 1.009 to 1.069, P=0.011).
Conclusions
Greater headache intensity, lower GH score, and higher SF score were associated with better acupuncture responses in CTTH patients. These 3 factors require independent validation as predictors of acupuncture effectiveness in CTTH.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Data Availability Statement
The raw data supporting the conclusions of this article will be made available by the authors, without undue reservation.
References
Robbins MS. Diagnosis and management of headache: a review. JAMA 2021;325:1874–1885.
Rizzoli P, Mullally WJ. Headache. Am J Med 2018;131:17–24.
Headache Classification Committee of the International Headache Society. The international classification of headache disorders, 3rd edition (beta version). Cephalalgia 2013;33:629–808.
Kahriman A, Zhu S. Migraine and tension-type headache. Semin Neurol 2018;38:608–618.
Burch R. Migraine and tension-type headache: diagnosis and treatment. Med Clin North Am 2019;103:215–233.
Schneider S, Junghaenel DU, Broderick JE, Ono M, May M, Stone AA. II. Indices of pain intensity derived from ecological momentary assessments and their relationships with patient functioning: an individual patient data meta-analysis. J Pain 2021;22:371–385.
Mata J, Sanchís P, Valentí P, Hernández B, Aguilar JL. Treatment of headache disorders with acupuncture: a 6-year retrospective study. Acupunct Med 2021;39:452–460.
Schiller J, Karst M, Kellner T, Zheng W, Niederer D, Vogt L, et al. Combination of acupuncture and medical training therapy on tension type headache: results of a randomised controlled pilot study. Cephalalgia 2021;41:879–893.
Schiller J, Niederer D, Kellner T, Eckhardt I, Egen C, Zheng W, et al. Effects of acupuncture and medical training therapy on depression, anxiety, and quality of life in patients with frequent tension-type headache: a randomized controlled study. Cephalalgia 2023;43:3331024221132800.
Tao QF, Wang XY, Feng SJ, Xiao XY, Shi YZ, Xie CR, et al. Efficacy of acupuncture for tension-type headache prophylaxis: systematic review and meta-analysis with trial sequential analysis. J Neurol 2023;270:3402–3412.
Linde K, Allais G, Brinkhaus B, Fei Y, Mehring M, Shin BC, et al. Acupuncture for the prevention of tension-type headache. Cochrane Database Syst Rev 2016;4:Cd007587.
Zheng H, Gao T, Zheng QH, Lu LY, Hou TH, Zhang SS, et al. Acupuncture for patients with chronic tension-type headache: a randomized controlled trial. Neurology 2022:https://doi.org/10.1212/WNL.0000000000200670.
Xiong ZY, Liu XY, Ma PH, Sun CY, Sun CY, Liu TL, et al. Placebo response among different types of sham acupuncture for low back pain: a systematic review and meta-analysis of randomized controlled trials. Chin J Integr Med 2023;29:941–950.
Shi LJ, Tian ZY, Hu XY, Xiu WC, Jiao RM, Hu XY, et al. Approach to assess adequacy of acupuncture in randomized controlled trials: a systematic review. Chin J Integr Med 2023;29:730–737.
Witt CM, Schutzler L, Ludtke R, Wegscheider K, Willich SN. Patient characteristics and variation in treatment outcomes: which patients benefit most from acupuncture for chronic pain?. Clin J Pain 2011;27:550–555.
Hao XA, Xue CC, Dong L, Zheng Z. Factors associated with conflicting findings on acupuncture for tension-type headache: qualitative and quantitative analyses. J Altern Complement Med 2013;19:285–297.
AlShareef SM. The prevalence of and risk factors for restless legs syndrome: a nationwide study. Front Psychiatry 2022;13:987689.
Hu NJ, Liu YQ, Zhao MY, Wang P, Wu GW, Hu SQ, et al. Influence of the intensity, components, and spreading of the Deqi sensation on the analgesic effect of SP6 needling in primary dysmenorrhea patients: a secondary analysis of a randomised controlled trial. Evid Based Complement Alternat Med 2019;2019:6462576.
Diener HC, Kronfeld K, Boewing G, Lungenhausen M, Maier C, Molsberger A, et al. Efficacy of acupuncture for the prophylaxis of migraine: a multicentre randomised controlled clinical trial. Lancet Neurol 2006;5:310–316.
Linde K, Streng A, Jürgens S, Hoppe A, Brinkhaus B, Witt C, et al. Acupuncture for patients with migraine: a randomized controlled trial. JAMA 2005;293:2118–2125.
Kim TH, Lee MS, Birch S, Alraek T. Plausible mechanism of sham acupuncture based on biomarkers: a systematic review of randomized controlled trials. Front Neurosci 2022;16:834112.
Zhang J, Li Z, Li Z, Li J, Hu Q, Xu J, et al. Progress of acupuncture therapy in diseases based on magnetic resonance image studies: a literature review. Front Hum Neurosci 2021;15:694919.
Zhao L, Chen J, Li Y, Sun X, Chang X, Zheng H, et al. The long-term effect of acupuncture for migraine prophylaxis: a randomized clinical trial. JAMA Intern Med 2017;177:508–515.
Chae Y, Chang DS, Lee SH, Jung WM, Lee IS, Jackson S, et al. Inserting needles into the body: a meta-analysis of brain activity associated with acupuncture needle stimulation. J Pain 2013;14:215–222.
Jung WM, Shim W, Lee T, Park HJ, Ryu Y, Beissner F, et al. More than Deqi: spatial patterns of acupuncture-induced bodily sensations. Front Neurosci 2016;10:462.
Holroyd KA, Labus JS, Carlson B. Moderation and mediation in the psychological and drug treatment of chronic tension-type headache: the role of disorder severity and psychiatric comorbidity. Pain 2009;143:213–222.
Yuan D, Zhang Y, Li Q, Lv Y, Li X, Yu Y, et al. Factors affecting preventive treatment outcomes for patients with newly diagnosed chronic migraine and their compliance with treatment recommendations in Chongqing Province, China: an open-label prospective study with retrospective baseline. Front Neurol 2020;11:227.
Fernandez-de-Las-Penas C, Palacios-Cena M, Valera-Calero JA, Cuadrado ML, Guerrero-Peral A, Pareja JA, et al. Understanding the interaction between clinical, emotional and psychophysical outcomes underlying tension-type headache: a network analysis approach. J Neurol 2022;269:4525–4534.
Yang CP, Chang MH, Li TC, Hsieh CL, Hwang KL, Chang HH. Predicting prognostic factors in a randomized controlled trial of acupuncture versus topiramate treatment in patients with chronic migraine. Clin J Pain 2013;29:982–987.
Zheng H, Huang W, Li J, Zheng Q, Li Y, Chang X, et al. Association of pre- and post-treatment expectations with improvements after acupuncture in patients with migraine. Acupunct Med 2015;33:121–128.
Carreon LY, Djurasovic M, Dimar JR 2nd, Owens RK 2nd, Crawford CH 3rd, Puno RM, et al. Can the anxiety domain of EQ-5D and mental health items from SF-36 help predict outcomes after surgery for lumbar degenerative disorders? J Neurosurg Spine 2016;25:352–356.
Sherman KJ, Cherkin DC, Ichikawa L, Avins AL, Barlow WE, Khalsa PS, et al. Characteristics of patients with chronic back pain who benefit from acupuncture. BMC Musculoskelet Disord 2009;10:114.
Caponnetto V, Deodato M, Robotti M, Koutsokera M, Pozzilli V, Galati C, et al. Comorbidities of primary headache disorders: a literature review with meta-analysis. J Headache 2021;22:71.
Yeung WF, Chung KF, Yu YB, Lao L. What predicts a positive response to acupuncture? A secondary analysis of three randomised controlled trials of insomnia. Acupuncture Med 2017;35:24–29.
Probyn K, Bowers H, Caldwell F, Mistry D, Underwood M, Matharu M, et al. Prognostic factors for chronic headache: a systematic review. Neurology 2017;89:291–301.
Li X, Dai Q, Shi Z, Chen H, Hu Y, Wang X, et al. Clinical efficacy and safety of electroacupuncture in migraine treatment: a systematic review and network meta-analysis. Am J Chin Med 2019;47:1755–1780.
Buse D, Manack A, Serrano D, Reed M, Varon S, Turkel C, et al. Headache impact of chronic and episodic migraine: results from the American Migraine Prevalence and Prevention study. Headache 2012;52:3–17.
Martínez-Pías E, Guerrero ÁL, Sierra Á, Trigo J, García-Azorín D. Daily headache in chronic migraine is a predictive factor of response in patients who had completed three sessions of OnabotulinumtoxinA. Toxins (Basel) 2021;13:432.
Acknowledgement
We sincerely thank all participants for their participation in the study.
Author information
Authors and Affiliations
Contributions
Cao W, Wang L, and Hou TH: conceptualization; Zou ZH, Yang Q, and Chen SJ: investigation; Hou TH, Zheng H, and Wang HY: data curation; Shi YZ, Zheng QH, and Qin D: methodology; Xiao XJ and Li Y: project administration; Li Y: supervision, validation; Cao W and Wang L: writing–original draft; Cao W and Xiao XJ: writing–review & editing. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
The authors declare no competing interests.
Additional information
Supported by the International Cooperation Program of Science and Technology Department of Sichuan Province, China (No. 2016HH0007)
Rights and permissions
About this article
Cite this article
Cao, W., Wang, L., Hou, Th. et al. Disease-Related Factors Associated with Acupuncture Response in Patients with Chronic Tension-Type Headache: A Secondary Analysis of A Randomized Controlled Trial. Chin. J. Integr. Med. 30, 684–691 (2024). https://doi.org/10.1007/s11655-023-3615-2
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11655-023-3615-2