Abstract
Partial bladder outlet obstruction (pBOO) is characterized by exaggerated stretch, hydrodynamic pressure, and inflammation which cause significant damage and fibrosis to the bladder wall. Several studies have implicated hypoxia in its pathophysiology. However, the isolated progressive effects of hypoxia on bladder cells are not yet defined. Sub-confluent normal human bladder smooth muscle cells (hbSMC) were cultured in 3% O2 tension for 2, 24, 48, and 72 h. RNA, cellular proteins, and secreted proteins were used for gene expression analysis, immunoblotting, and ELISA, respectively. Transcription of hypoxia-inducible factor (HIF)1α and HIF2α were transiently induced after 2 h of hypoxia (p < 0.05), whereas HIF3 was upregulated after 72 h (p < 0.005). HIF1 and HIF3α proteins were significantly induced after 2 and 72 h, respectively. VEGF mRNA increased significantly after 24 and 72 h (p < 0.005). The inflammatory cytokines, TGFB (protein and mRNA), IL 1β, 1L6, and TNFα (mRNA) demonstrated a time-dependent increased expression. Furthermore, the anti-inflammatory cytokine IL-10 was downregulated after 72 h (p < 0.05). Evidence of smooth muscle cell dedifferentiation included increased αSMA, vimentin, and desmin. Evidence of pro-fibrotic changes included increased CTGF, SMAD 2, and SMAD 3 as well as collagens 1, 2, 3, and 4, fibronectin, aggrecan, and TIMP 1 transcripts (p < 0.05). Total collagen proteins also increased time-dependently (p < 0.05). Together, these results show that exposure of hbSMC to low oxygen tension results in intense hypoxic cascade, including inflammation, de-differentiation, pro-fibrotic changes, and increased extracellular matrix expression. This elucidates mechanisms of hypoxia-driven bladder deterioration in bladder cells, which is important in tailoring in vivo experiments and may ultimately translate into improved clinical outcomes.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Partial bladder outlet obstruction (pBOO) occurs as a sequela of benign prostate hyperplasia, posterior urethral valve disease, urethral stricture disease, cancer, and neural tube defects. The resistance to voiding initially results in a compensatory response, with bladder smooth muscle hypertrophy. However, excessive, prolonged exposure can lead to decompensation (Levin et al. 1990). A myriad of factors including stretch, hypoxia, hydrodynamic pressure, and/or inflammation are involved in the etiology of bladder damage. Also, in the aged population, hypoxia has been known to correlate with increased urological disorders (Pinggera et al. 2008).
In the early development of pBOO, there is a sequential process of inflammation, hypertrophy, and eventually culminating in fibrosis (Metcalfe et al. 2010). Further in its development, the obstructed hypercontractile bladder is exposed to more frequent yet prolonged cycles of ischemia during the filling and voiding stages (Schröder et al. 2001). Even though many studies have identified hypoxia in the muscle layer of the obstructed bladder, the effects of hypoxia as a sole stressor on bladder injury remain unknown.
The ability of many cell types to sense and respond to reduced oxygen tensions is essential for their survival. The major protein central to mediating this protective response is the hypoxia-inducible factor (HIF) (Guillemin and Krasnow 1997). The HIF family is characterized by a heterodimeric structure and consists of three known members: HIF1, HIF2, and HIF3. Structurally, each member consists of a stable and uniformly distributed β-subunit and an oxygen-sensitive, hypoxia-inducible α-subunit. During hypoxia, the α-subunit is stabilized via prolyl hydroxylase inhibition and subsequently dimerizes with the β-subunit. The α-β dimer is a transcription factor for stimulating the transcription of key genes. These genes encode for numerous cytoprotective proteins to combat the deleterious effects of hypoxia (Guillemin and Krasnow 1997). One key protective protein is the vascular endothelial growth factor (VEGF), a major angiogenic factor responsible for stimulating vascular growth.
In many clinical conditions, hypoxia is known to promote pro-inflammatory mediators and cytokines; transforming growth factor beta (TGFβ) is a master regulator of cell growth, proliferation, differentiation, and the epithelial-mesenchymal transition (EMT). Stimulation of the TGFβ-SMAD pathway results in the downstream activation of connective tissue transforming growth factor (CTGF); this inevitably leads to increased collagen deposition. Not only does TGFβ act independently to augment extracellular matrix production, exposure to hypoxia has similar effects at the level of transcription and translation (Falanga et al. 1991; Chen et al. 2005). Two key intermediary processes involved in increased collagen production are an upregulation of tissue inhibitors of metalloproteases (TIMP) and an activation of myofibroblasts (Desmoulier et al. 1993; Macpherson et al. 1993; Higgins et al. 2007).
In order to understand the mechanisms involved in the development of pBOO, we hypothesized that exposing normal bladder smooth muscle cells to hypoxia would stimulate inflammation and induce a fibrotic phenotype.
Materials and Methods
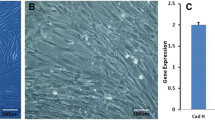
Established normal human bladder smooth cells were purchased from ScienCell Research Laboratories (Carlsbad, CA) in 2015, and their smooth muscle phenotype was confirmed by their culture characteristics and the expression of the smooth muscle markers; h-caldesmon, desmin, α smooth muscle actin (αSMA) as well as the absence of l-caldesmon as previously established (Huber 1997; Zheng 2012). They were cultured in complete smooth muscle medium containing smooth muscle growth factors (1×), fetal bovine serum (10%), and 1 × 1000 U/ml penicillin and 1000 mg/ml streptomycin from ScienCell Research Laboratories. Cells were cultured in humidified air at 37°C with 5% CO2.
Exposure to hypoxia
Cells between passages 3 and 10 were used for this experiment. 2 × 106 cells/100-mm culture dish were maintained at normoxic conditions of 21% O2 in humidified air, 5% CO2, 74% N2 at 37°C; hypoxic conditions were defined as a gas mixture of 3% O2, 5% CO2, 92% N2 at 37°C for 2, 24, 48, or 72 h, maintained in a Thermo Scientific series II water jacket CO2 incubator (Waltham, MA). For controls, equal numbers of cells were maintained under normoxic conditions for an equivalent length of time.
Quantitative real-time PCR
Immediately at the end of the specified period of hypoxic or normoxic culture of cells, spent medium was frozen, cells were washed with cold PBS and lysed, and RNA was extracted using RNeasy Mini kit (Qiagen, Valencia CA). One microgram of total RNA sample was reverse transcribed using Quantitect Reverse Transcription kit (Qiagen). Real-time PCR reaction was set up using the Kapa Sybr Fast qPCR Kit (Kapa Biosystems, Boston, MA) and specific oligo-dt primer sets for genes of interest (Table 1). An initial enzyme activation at 95°C for 3 min and subsequent 40 cycles of denaturing (95°C, 2 s) and annealing/extension (60°C, 30 s) were all carried out in a Bio-Rad CFX96 real-time system (Kallang, Singapore). Gene expression of hypoxic cultured samples relative to its normoxic cultured control were normalized to an average of two endogenous controls, β actin and 18S, using the comparative Ct method and expressed as 2−ΔΔct.
Western blot analysis
Hypoxic or normoxic incubated cells were washed with cold PBS and lysed in a RIPA-protease inhibitor cocktail on ice. Protein concentration of lysates was determined using Pierce™ BCA Protein Assay Kit (Waltham, MA) and denatured at 98°C for 5 min in an sodium dodecyl sulphate (SDS)-loading buffer. Forty-microgram protein volumes were separated by 10% SDS polyacrylamide gel electrophoresis (SDS-PAGE). Transferred proteins on nitrocellulose membranes were blocked with 5% non-fat milk in TBS 0.05% Tween 20. Primary antibody incubation was done overnight at 4°C using anti-human HIF1α (1:2000, #AF1935), HIF2α (1:1000, #AF2997) (R&D Systems), HIF3α (whole serum, PCRP-HIF3A-1B1, IOWA DSHB, Iowa City, IA), vimentin (1:1000, #5741), and tubulin (1:10,000, #2144) (Cell Signalling Boston, MA). Protein bands were developed by incubation in secondary antibodies conjugated to horseradish peroxidase (Cell Signalling #7076, Santa Cruz #sc2768) and visualized using SuperSignal chemiluminescence substrate (Thermo Scientific).
ELISA for TGFβ and total collagen
Secreted TGFβ1 in culture media was determined using Quantikine ELISA from R&D Systems (Minneapolis, MN) as previously described (Chouhan et al. 2015). Briefly, latent TGFβ1 in 100 μl of harvested culture media was activated and total concentration was determined by immunoreaction to pre-coated monoclonal human TGFβ1 using the quantitative sandwich enzyme immunoassay technique according to manufacturers’ instructions. Total synthesized collagen was determined using Chondrex hydroxyproline assay kit (WA). Samples were hydrolyzed with concentrated HCl at 120°C for 24 h, and hydroxyproline levels were estimated from a subsequent chromogenic reaction. Total collagen level in each sample was calculated as the percentage of hydroxyproline divided by 13.5 as already described (Neuman and Logan 1950). All ELISA tests were carried out in duplicates for n = 3.
Statistical analysis
Data was analyzed using GraphPad prism 6.0 software (GraphPad Prism Inc., La Jolla, CA). Differences between groups were assessed using one-way analysis of variance (ANOVA) followed by Dunnett’s multiple comparison test. All values were expressed as mean ± standard error; p < 0.05 was considered statistically significant.
Results
Hypoxia-inducible factor and pro-angiogenic response
The incubation of normal bladder smooth muscle cells in 3% hypoxia induced immediate and significant effects (Fig. 1). Levels of HIF1α and HIF2α rose by 2.3- and 2.7-fold, respectively, by 2 h hypoxia (p < 0.05 for both), but there were no increases in transcript levels at subsequent times. HIF3α transcript levels did not exhibit any increase until 48 h at which point values rose by 2.6-fold (p < 0.05); this positive effect was further amplified by 5.8-fold following 72 h (p < 0.005). HIF1 and HIF3α proteins were significantly upregulated only after 2 and 72 h, respectively, whereas HIF2α protein demonstrated only a slight increase after 24 h. The pattern of VEGF expression paralleled that of HIF1α and HIF2α. VEGF levels increase by 5-fold after 2 h; by 24 h, expression had increased by a factor 10.4 relative to control (p < 0.005). Despite a transient decline in values by 48 h, there was a 16.2-fold increase after 72 h.
Hypoxia-inducible factor and pro-angiogenic response. (A, B) Human bladder smooth muscle cells responded to hypoxia by transient upregulation of transcription of HIF 1 and 2 α. (C) upregulation of HIF3α transcripts after 48 and 72 h of hypoxia. (D) Hypoxia induces transcription of VEGF after 24 and 72 h of hypoxia. Graph represents mean ± SEM and n = 5. One-way ANOVA followed by Dunnet’s multiple comparison was used to compare each hypoxic group with its corresponding normoxic controls (*p < 0.05, **p < 0.005, ***p < 0.0005). Normoxic controls were assigned an expression of 1. (E) Western blot for the HIF proteins demonstrates upregulation of HIF 1α protein (~116 kDa) after 2 h, slight increase in HIF2α (~115 kDa) after 24 h, and a significant increase in HIF3α (~70 kDa) after 72 h of hypoxia. Tubulin protein bands were used to show the equality of loaded total proteins of each sample.
Inflammatory cytokines
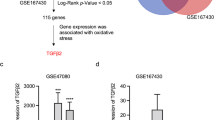
TGF-B1 transcripts increased 2.7-fold over 48 h (p < 0.05) and by a total 4.4-fold after 72 h (p < 0.005) (Fig. 2). TGFβ1 protein levels reflected the increases in gene expression; between 24 and 72 h, there was a time-dependent increase of 27% (p < 0.005), 28% (p < 0.05), and 55% (p < 0.005), respectively. TNFα transcripts increased to 2.7-fold after 48 h (p < 0.005), and by 3.2-fold after 72 h (p < 0.005). IL 1β gene expression also increased by 3.2-fold after 72 h (p < 0.005), whereas IL-6 expression increased 8.9-fold by 24 h (p < 0.005). At 72 h, fold increases had reached 12.6 after 72 h (p < 0.005). Transcript levels of the anti-inflammatory cytokine, IL-10 exhibited a consistent decline; at the completion of the time, course levels had dropped to 44% relative to control (p < 0.005).
Hypoxia-induced inflammatory cytokine production. (A, B) Hypoxia-induced increased TGFβ1 transcription and translation. Total TGFβ1 protein in bladder smooth muscle cell culture medium after hypoxic incubation was activated and measured by ELISA. (C) TNF α, (D) interleukin 1β, and (E) interleukin 6 transcripts were upregulated during hypoxia. (F) Downregulation of interleukin 10 transcription during hypoxic stress (*p < 0.05, **p < 0.005, ***p < 0.0005, ****p < 0.0001, represents comparison between hypoxic groups and their normoxic controls).
Smooth muscle dedifferentiation, EMT, and pro-fibrotic response
Since smooth muscle dedifferentiation is associated with increased cell migration and high extracellular matrix production similar to what occurs in myofibroblast activation and EMT, we assessed it using the expression of αSMA, vimentin, and desmin (Fig. 3). A pro-fibrotic response was also assessed via an upregulation of three key genes, SMAD 2, SMAD 3, and CTGF. The human detrusor smooth muscle cells responded to hypoxia by increasing the transcription of αSMA in a time-dependent manner. A 5.6-fold increase (p < 0.05) in expression was recorded after 48 h followed by a 7.5-fold increase (p < 0.005) over normoxic controls. Both vimentin and desmin transcript levels increased 5-fold after 72 h (p < 0.0005) while vimentin protein showed a progressive increase with increasing duration of hypoxia. Expression of SMAD 2 increased by 3.6-fold after 48 h (p < 0.05), and both SMAD 2 and 3 increased by 5-fold after 72 h (p < 0.005 for both). CTGF increased by 2.7 (p < 0.05) after 72 h of hypoxic culture.
Hypoxia-induced smooth muscle cell dedifferentiation and pro-fibrotic response. (A) Increased gene expression of αSMA, vimentin, and desmin indicative of dedifferentiation of normal smooth muscle cells during hypoxia. (B) Western blot analysis of vimentin show increasing protein with increasing duration of hypoxia. Distinct bands for vimentin were detected at ~57 kDa (C) pro-fibrotic genes; SMAD 2, SMAD 3, and CTGF were upregulated after 72 h hypoxia (n = 5).
Extracellular matrix production and breakdown
Collagens 1, 2, 3, and 4, fibronectin, and aggrecan are key components in fibrosis; protein and transcript levels were measured in hbSMC during hypoxia (Fig. 4). TIMP 1 was also assessed as a measure of inhibition to the breakdown of these fibrotic proteins. Collagen 1 transcripts exhibited a consistent increase over the entire time course, with a 3.4-fold increase after 2 h eventually reaching a maximum fold increase of 12 by 72 h (p < 0.05 and p < 0.005, respectively). Collagen 2 transcript levels showed a 4-fold increase by 72 h (p < 0.005); collagen 3 exhibited a similar increase, although a 5-fold increase was evident at 48 and 72 h (p < 0.05). Collagen 4 transcripts rose by almost 8-fold following 72 h hypoxia (p < 0.005).
Hypoxia-induced extracellular matrix production. Human bladder smooth muscle cells responded to hypoxia by the exponential increase in production of components of the extracellular matrix. Newly synthesized collagen in media was estimated from the total concentration of hydroxyproline. TIMP 1 levels were also upregulated.
Total secreted collagen remained at control values until 24 h at which point levels rose by 100% (p < 0.0001); values remained consistently elevated during prolong hypoxia. Fibronectin transcripts showed a consistent increase from 1.9- to 3.9-fold; p < 0.005 for values between 24 and 72 h. Both aggrecan and TIMP 1 had a similar patterns of expression; 2 h exposure to hypoxia induced a 3-fold increase in mRNA (p < 0.05). Levels dropped to control levels by 24 h and then after 72 h, both aggrecan and TIMP rose again by 4.6- and 2.6-fold, respectively (p < 0.005 for both).
Discussion
Bladder outlet obstruction is a serious urological condition that can lead to irreversible bladder and renal damage (Levin et al. 1990). Animal studies have shown that pBOO results in a significant decrease in blood flow to the bladder muscle layer which correlates with contractile dysfunction (Schröder et al. 2001) and increased collagen production (Metcalfe et al. 2010). The initiation and progression of pBOO is associated with an increased expression of pro-inflammatory, pro-fibrotic, and angiogenic genes, namely HIF, TGFβ, SMADS, VEGF, αSMA, CTGF, TNFα, IL 1β, and collagen. However, these responses are due to a combined multi-component stress involving stretching, increased hydrodynamic pressure, inflammation, and hypoxia. Other studies have delineated the role of stretching, mechanical deformation, inflammation, and elevated hydrodynamic pressure as single stressors (Howard et al. 2005; Chen et al. 2012). However, the exact role of hypoxia in the progression of this pathological process has not yet been investigated. Therefore, this study was designed to test the hypothesis that normal bladder smooth muscle cells exposed to hypoxia, without the confounding effects of stretching or contracting forces, will lead to an inflammatory response and a pro-fibrotic phenotype.
HIF expression pattern in hypoxia and pro-angiogenic response
The importance of the HIF transcriptional factor to cell survival has been well-established (Guillemin and Krasnow 1997). In our study, the transcription and translation of both HIF1 and HIF2α were transiently upregulated in response to short-term hypoxia (2–24 h). This is consistent with findings from other cells (Norman et al. 2000; Shi et al. 2007). Meanwhile, some previous studies on cells from the cerebral cortex, hippocampus, lung, heart, and Chinese hamster ovary cells have reported that the transcription of HIF1 and HIF2α is not affected by hypoxia (Heidbreder et al. 2003) and is exclusively under post-translational regulation. In our study, HIF1α upregulation during the early phase of hypoxia (2 h) may be an emergency response mechanism that ensures stable levels of HIFα proteins in order to ensure that an immediate cytoprotective response is mounted. The increase in VEGF mRNA after 24 h is consistent with the proven relationship involving a HIF-mediated pro-angiogenic effect.
As far as we are aware, our study is the first to document the involvement of HIF3α in human bladder cells with a primary role in cytoprotective responses to prolong hypoxia. Interestingly, the role of HIF3α in mediating responses to hypoxia is not ubiquitous; HIF3α has been found to be tissue and organ-specific. In the previous study examining the involvement of HIF3α in hypoxia in multiple rodent organs, HIF3α expression was elevated in rat brain, lung, and heart tissues with no effect on HIF1α and HIF2α. This finding suggests that there may be a protective role mediated by HIF3α during hypoxia that is independent of HIF1α and HIF2α (Heidbreder et al. 2003). In our study, HIF3α genes and protein were significantly expressed after 72 h of hypoxia when HIF1 and HIF2α proteins had resumed normoxic control levels. These results are congruous with a role of HIF3α that is complementary to that of HIF1α and HIF2α. This purported mechanism provides an explanation of a biphasic upregulation of VEGF where VEGF transcripts had increased again following 72 h when only HIF3α was the sole up-stream factor. Conversely, the inverse relationship between HIF1α and HIF2α with HIF3 has been suggested to be the result of HIF3α-mediated suppression of HIF1α and HIF2α expression (Hara et al. 2001).
Hypoxia-induced inflammatory cytokine production
The major regulatory role of TGFβ in fibrosis makes it a very important marker in fibrotic diseases. In our study using human bladder smooth muscle cells as an in vitro model, hypoxia stimulated TGFβ1 expression at both mRNA and protein levels in a time-dependent manner; this is consistent with a previous study using human hepatic stellate cells (Zheng et al. 2012). Of more physiologic relevance, TGF β1 expression has been found to increase in whole animal models of pBOO (Shi et al. 2009).
Hypoxia also induced the expression TNFα, IL 1β, and IL 6 which are all part of the acute phase proteins secreted in response to inflammation. However, expression of IL 10 was downregulated in a time-dependent pattern. This is consistent with the study of trophoblast cells of pre-eclamptic pregnancies that reported a similar pattern of reduced IL 10 and increased IL 6 when exposed to hypoxia (Bowen et al. 2005). Data from our current study demonstrate that isolated hypoxic stress can produce a robust inflammatory response. Prior studies focusing specifically on pBOO have attributed the inflammatory response to contractility, bladder remodeling, and functional deterioration (Bowen et al. 2005; Shi et al. 2009; Metcalfe et al. 2010; Yildirim et al. 2013). In our results, the initial robust IL6 response we detected was most likely responsible for the direct inhibition of TNFα transcription over the first 24 h. The first incidence of TNF upregulation occurred after 48 h, which corresponded to a marked decline in IL 6. Thus, our findings are consistent with a previously established inhibitory effect of IL 6 on both TNFα and IL 1β expression (Barton 1997). Unexpectedly, TNFα and IL 1β mRNA levels increased significantly after 72 h when IL6 remained elevated. This suggests that there may be other important factors and mediators of interplay here; IL 10 is typically referred to as an anti-inflammatory (and anti-fibrotic) cytokine where suppression of IL 10 levels has pro-inflammatory sequelae (Shi et al. 2013). We found a time-dependent decline in IL 10 transcripts, with values reaching significance after 48–72 h. Despite an initial inhibitory effect of IL 6 on TNF over the first 24 h, it is possible that the secondary protracted effect was governed by the loss of IL 10. Whether the biphasic response of TNFα throughout extended periods of hypoxia is regulated by the ratio of IL 10/IL 6 as opposed to absolute transcript levels remains to be established.
Smooth muscle cell dedifferentiation, EMT, and pro-fibrotic response
In our study, the epithelial to mesenchymal transition and the smooth muscle cell dedifferentiation was profound. A pro-fibrotic response involving TGF β transcription and translation was evident at the early stage (<24 h) followed by a progressive increase in αSMA throughout the entire period of hypoxia; this is congruous with the findings in proximal tubular cells (Manotham et al. 2004). Later stage development of pro-fibrotic response was evidenced by increases in desmin, a proven index of late stage fibrosis. Importantly, our results strongly suggest a relationship between prolong hypoxia, HIF3α, and EMT (using vimentin as a marker) in bladder smooth muscle cells. Exploring this area further may have therapeutic potentials in obstructive bladder conditions.
Increased synthesis and decreased breakdown of extracellular matrix proteins are the hallmark events characteristic of fibrosis. The pro-fibrotic response of human bladder smooth muscle cells in our study was pronounced; total collagen protein increased by 100%. Synthesis of the four central matrix components in our model was the direct result of an early and progressive upregulation of collagens 1 and 3. Collagens 1 and 3 are the key interstitial collagens most commonly found in obstructive bladder fibrosis (Metcalfe et al. 2010; Jiang et al. 2015). The significance of the later stage increases in collagens 2 and 4 transcription may be related to a secondary mechanism of matrix formation following initial pro-fibrotic events. TGFβ also plays a key role in fibronectin synthesis at transcriptional and translational levels; fibronectin is an essential substrate for αSMA synthesis (Dugina et al. 2001). From our results, both the fibronectin gene and secreted TGFβ1 protein were significantly upregulated after 24 h hypoxia and further increased throughout prolonged exposure. αSMA expression was only increased after 48 h, likely secondary to increase in both fibronectin and TGFβ1.
Although our data indicate that there is a concerted cellular effort resulting in an overall increase in multiple metabolic pathway of fibrosis. The marked increase in expression of TIMP 1 reaffirms the ability of hypoxia to induce and sustain fibrotic pathways via multiple regulatory control mechanisms. Our data demonstrating the involvement of two opposing mechanisms, matrix synthesis, and proteolytic inhibition are consistent with those of a previous study focusing on human renal fibroblasts cultured in low oxygen tensions (Norman et al. 2000).
The data presented in this study provides strong evidence for the mechanistic detail as follows; Exposure of the bladder smooth muscle cells to hypoxia lead to an upregulation of HIF. Increases in HIF transcription triggered the observed increase in SMAD 2 and SMAD 3 transcription presumably via the formation of a HIF-SMAD complex as has been previously established (Sánchez-Elsner et al. 2001). Subsequent increases in SMAD proteins provided greater amounts of substrate for TGF β1-mediated phosphorylation. This activation of SMAD 2/3 promoted the formation of the trimeric protein complex responsible for CTGF expression which, in turn, stimulated the increase in secreted matrix components (collagen 1–4, fibronectin, aggrecan). In reference to pBOO, these events are fundamental to the pathological development of fibrosis and inhibition of the TGFβ-SMAD pathway in pBOO results in a significant reduction in fibrosis (Jiang et al. 2015).
Conclusion
This study has provided overwhelming evidence that hypoxia exposure, as a single isolated stress without the confounding effects of stretching and hydrodynamic pressures, can induce fibrotic phenotype in smooth muscle cells mechanistically via inflammation, smooth muscle de-differentiation, and a pro-fibrotic switch in normal human bladder smooth muscle cells characterized by increased ECM production. This work gives foundational understanding of hypoxia-driven bladder deterioration which we hope will eventually translate into improved clinical outcomes.
References
Barton BE (1997) IL-6: insights into novel biological activities. Oct Clin Immunol Immunopathol(1):16–20
Bowen RS, Gu Y, Zhang Y, Lewis DF, Wang Y (2005) Hypoxia promotes interleukin-6 and -8 but reduces interleukin-10 production by placental trophoblast cells from preeclamptic pregnancies. J Soc Gynecol Investig 12(6):428–432
Chen CP, Yang YC, Su TH, Chen CY, Aplin JD (2005) Hypoxia and transforming growth factor-beta 1 act independently to increase extracellular matrix production by placental fibroblasts. J Clin Endocrinol Metab 90(2):1083–1090
Chen L, Wei TQ, Wang Y, Zhang J, Li H, Wang KJ (2012) Simulated bladder pressure stimulates human bladder smooth muscle cell proliferation via the PI3K/SGK1 signaling pathway. J Urol 188(2):661–667
Chouhan VS, Dangi SS, Babitha V, Verma MR, Bag S, Singh G, Sarkar M (2015) Stimulatory effect of luteinizing hormone, insulin-like growth factor-1, and epidermal growth factor on vascular endothelial growth factor production in cultured bubaline luteal cells. Theriogenology S0093-691X(15):00325–00328
Desmouliere A, Geinoz A, Gabbiani F, Gabbiani G (1993) Transforming growth factor-beta-1 induces alpha-smooth muscle actin expression in granulation tissue myofibroblasts and in quiescent and growing cultured fibroblasts. J Cell Biol 122:103–111
Dugina V, Fontao L, Chaponnier C, Vasiliev J, Gabbiani G (2001) Focal adhesion features during myofibroblastic differentiation are controlled by intracellular and extracellular factors. J Cell Sci 114(Pt 18):3285–3296
Falanga V, Qian SW, Danielpour D, Katz MH, Roberts AB, Sporn MB (1991) Hypoxia upregulates the synthesis of TGF-beta 1 by human dermal fibroblasts. J Invest Dermatol 97(4):634–637
Guillemin K, Krasnow MA (1997) The hypoxic response: huffing and HIFing. Cell 89:9–12
Hara S, Hamada J, Kobayashi C, Kondo Y, Imura N (2001) Expression and characterization of hypoxia-inducible factor (HIF)-3alpha in human kidney: suppression of HIF-mediated gene expression by HIF-3alpha. Biochem Biophys Res Commun 287(4):808–813
Heidbreder M, Fröhlich F, Jöhren O, Dendorfer A, Qadri F, Dominiak P (2003) Hypoxia rapidly activates HIF-3alpha mRNA expression. FASEB J 17(11):1541–1543
Higgins DF, Kimura K, Bernhardt WM, Shrimanker N, Akai Y, Hohenstein B, Saito Y, Johnson RS, Kretzler M, Cohen CD, Eckardt KU, Iwano M, Haase VH (2007) Hypoxia promotes fibrogenesis in vivo via HIF-1 stimulation of epithelial-to-mesenchymal transition. J Clin Invest 117:3810–3820
Howard PS, Kucich U, Coplen DE, He Y (2005) Transforming growth factor-beta1-induced hypertrophy and matrix expression in human bladder smooth muscle cells. Urology 66(6):1349–1353
Huber PA (1997) Caldesmon. Int J Biochem Cell Biol 29(8–9):1047–1051
Jiang X, Chen Y, Zhu H, Wang B, Qu P, Chen R, Sun X (2015) Sodium tanshinone IIA sulfonate ameliorates bladder fibrosis in a rat model of partial bladder outlet obstruction by inhibiting the TGF-β/Smad pathway activation. PLoS One 10(6):e0129655
Levin RM, Longhurst PA, Monson FC, Kato K, Wein AJ, Greenland JE, Brading AF (1990) Effect of bladder outlet obstruction on the morphology, physiology, and pharmacology of the bladder. Prostate Suppl 3:9–26
MacPherson BR, Leslie KO, Lizaso KV, Schwarz JE (1993) Contractile cells of the kidney in primary glomerular disorders: an immunohistochemical study using an anti-alpha-smooth muscle actin monoclonal antibody. Hum Pathol 24(7):710–716
Manotham K, Tanaka T, Matsumoto M, Ohse T, Inagi R, Miyata T, Kurokawa K, Fujita T, Ingelfinger JR, Nangaku M (2004) Transdifferentiation of cultured tubular cells induced by hypoxia. Kidney Int 65(3):871–880
Metcalfe PD, Wang J, Jiao H, Huang Y, Hori K, Moore RB, Tredget EE (2010) Bladder outlet obstruction: progression from inflammation to fibrosis. BJU Int 106(11):1686–1694
Neuman RE, Logan MA (1950) The determination of hydroxyproline. J Biol Chem 184(1):299–306
Norman JT, Clark IM, Garcia PL (2000) Hypoxia promotes fibrogenesis in human renal fibroblasts. Kidney Int 58(6):2351–2366
Pinggera GM, Mitterberger M, Steiner E, Pallwein L, Frauscher F, Aigner F, Bartsch G, Strasser H (2008) Association of lower urinary tract symptoms and chronic ischaemia of the lower urinary tract in elderly women and men: assessment using colour Doppler ultrasonography. BJU 102(4):470–474
Sánchez-Elsner T, Botella LM, Velasco B, Corbí A, Attisano L, Bernabéu C (2001) Synergistic cooperation between hypoxia and transforming growth factor-beta pathways on human vascular endothelial growth factor gene expression. J Biol Chem 276(42):38527–38535
Schröder A, Chichester P, Kogan BA, Longhurst PA, Lieb J, Das AK, Levin RM (2001) J Urol. Effect of chronic bladder outlet obstruction on blood flow of the rabbit bladder 165(2):640–646
Shi B, Zhu Y, Laudon V, Ran L, Liu Y, Xu Z (2009) Alterations of urine tgf-beta1 and bfgf following bladder outlet obstruction: a predictor for detrusor contractibility? Urol Int 82(1):43–47
Shi JH, Guan H, Shi S, Cai WX, Bai XZ, Hu XL, Fang XB, Liu JQ, Tao K, Zhu XX, Tang CW, Hu DH (2013) Protection against TGF-β1-induced fibrosis effects of IL-10 on dermal fibroblasts and its potential therapeutics for the reduction of skin scarring. Arch Dermatol Res 305(4):341–352
Shi YF, Fong CC, Zhang Q, Cheung PY, Tzang CH, Wu RS, Yang M (2007) Hypoxia induces the activation of human hepatic stellate cells LX-2 through TGF-beta signaling pathway. FEBS Lett 581(2):203–210
Yildirim A, Başeskioğlu B, Temel HE, Erkasap N, Yenilmez A, Uslu S, Ozer C, Ozkurt M, Dönmez T (2013) Effect of αlipoic acid and silymarin on bladder outlet obstruction. Exp Ther Med 5(2):596–602
Zheng Y, Chang S, Boopathi E, Burkett S, John M, Malkowicz SB, Chacko S (2012) Generation of a human urinary bladder smooth muscle cell line. Vitro Cell Dev Biol Anim 48(2):84–96
Acknowledgments
We acknowledge the Northern Alberta Urology Foundation for funding this project.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflicts of interest
All authors have no conflicts of interest.
Additional information
Editor: Tetsuji Okamoto
Rights and permissions
About this article
Cite this article
Wiafe, B., Adesida, A., Churchill, T. et al. Hypoxia-increased expression of genes involved in inflammation, dedifferentiation, pro-fibrosis, and extracellular matrix remodeling of human bladder smooth muscle cells. In Vitro Cell.Dev.Biol.-Animal 53, 58–66 (2017). https://doi.org/10.1007/s11626-016-0085-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11626-016-0085-2