Abstract
Background
Laparoscopic transcystic common bile duct exploration (LTCBDE) is used to treat cholecystolithiasis and choledocholithiasis. This study aimed to investigate the safety, effectiveness and generalisability of LTCBDE in patients with cholecystolithiasis and choledocholithiasis based on our LTCBDE experience within 8 years.
Methods
Four hundred patients with cholecystolithiasis and choledocholithiasis (including 62 of cholecystolithiasis and choledocholithiasis with common bile duct no-dilatation) treated with LTCBDE at a single centre from January 2014 to February 2022 were retrospectively evaluated. They were divided into the first 200 and last 200 LTCBDE cases. The disease characteristics, cystic duct incision methods, surgical outcomes and follow-up data were analysed retrospectively. Each patient was followed up for > 3 months.
Results
Four hundred patients underwent LTCBDE, including 188 males and 212 females aged from 15 to 91 years (average age: 56 years). LTCBDE was successful in 377 (94.3%) patients, while treatment was converted to laparoscopic choledocholithotomy with T-tube drainage in 23 (5.8%), owing to intraoperative choledochoscope insertion failure. The CBD diameter (10.89 ± 1.76 vs 9.97 ± 2.39, P < 0.05), cystic duct diameter (4.62 ± 1.03 vs 5.03 ± 1.29, P < 0.05), and operation time (164.60 ± 24.30 vs 135.34 ± 30.00, P < 0.05). Residual stones were found in six (1.5%) patients and removed during the second operation; post-operative bile leakage was found in one (0.3%) patient, who was discharged safely after the second operation.
Conclusions
Phase I LTCBDE is safe and effective in treating cholecystolithiasis and choledocholithiasis. With continuous technological advances, LTCBDE has been effectively promoted and applied.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Choledocholithiasis secondary to cholecystolithiasis is a common clinical disease, and its incidence in patients with cholecystolithiasis is about 10–15%.1,2 Common bile duct (CBD) stones can cause acute pancreatitis, acute obstructive septic cholangitis, cholestatic shock and other serious complications.3,4 There are many treatments for cholecystolithiasis and choledocholithiasis, including open choledocholithotomy + cholecystectomy, endoscopic retrograde cholangiopancreatography (ERCP) + stage II LC, laparoscopic choledocholithotomy (laparoscopic common bile duct exploration [LCBDE]) + T-tube drainage + LC, LCBDE + stage I suturing + LC and laparoscopic transcystic common bile duct exploration (LTCBDE) + LC.5,6,7,8,9,10,11 However, the optimal treatment for these diseases remains controversial.
Although open choledocholithotomy is the traditional treatment procedure, it can fully expose the CBD and cystic bile duct under direct vision, allowing for the most thorough removal of stones. However, open operation is highly invasive, has a long post-operative recovery time, and is prone to complications, such as post-operative infection, haematobilia, bile duct leakage and bile duct stenosis.12 Although ERCP is a generally accepted surgical procedure, 5–11% of patients develop post-operative complications, such as pancreatitis, duodenal perforation, bile reflux and Oddis sphincter injury.13,14
With the development of laparoscopic technology, LCBDE has gradually become favoured by doctors. This technology avoids Oddis sphincter injury and yields a small surgical trauma, rapid post-operative recovery and ideal treatment results. LCBDE is divided into two types, according to the stone extraction route: laparoscopic choledocholithotomy and LTCBDE. It is currently divided into T-tube drainage and primary bile duct suturing, according to the diverse treatment procedures for the CBD. T-tube placement during LCBDE is a safe treatment option that lowers the risk of bile leakages and bile duct strictures and facilitates the treatment of residual stones. However, approximately 15% of patients who undergo T-tube drainage develop complications, such as water and electrolyte disorders, biliary peritonitis after T-tube removal and T-tube displacement.15,16 The T-tube must be placed for an extended period following operation, which has a negative impact on patients’ quality of life. At present, the literature is increasingly inclined to primary suturing.17,18 Although primary suturing of the bile duct avoids the complication of long-term T-tube placement, stones must be completely exhausted. There is still controversy on how to further treat residual stones if they occur after primary suturing of the bile duct. Simultaneously, without T-tube support after primary bile duct suturing, bile duct stenosis may occur post-operatively.
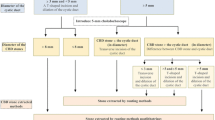
Shapiro et al. 19 first proposed LTCBDE in 1991. LTCBDE is the most physiological operation method, which involves inserting a choledochoscope through the cystic duct without incising the CBD, thereby avoiding the risk of bile leakage and bile duct stricture caused by placing a T-tube for drainage or primary suturing of the CBD while preserving the function of the sphincter of Oddis. However, the difficulty of using this technology restricts its application. The greatest difficulty with this technology is the insertion of a choledochoscope into the CBD through the cystic duct. With the gradual maturity of this technology, our team proposed three different cystic duct incision methods to facilitate the insertion of a choledochoscope into the CBD through the cystic duct. For patients with cystic duct dilatation, a transverse incision can be selected; for patients with a thinner cystic duct, a T-shaped incision or microincision of the cystic duct can be selected.20 Using these methods flexibly, especially the microincision of cystic duct, LTCBDE can be completed in most patients. Based on these experiences, our team also attempted to conduct LTCBDE in some patients with cholecystolithiasis and choledocholithiasis with CBD no-dilatation (Fig. 1). LTCBDE has been previously reported as safe and effective for patients without CBD dilatation.21
Multiple medical centres have gradually implemented LTCBDE with the support of our team by continuously familiarising themselves with the three abovementioned methods, resulting in efficient promotion and application and greater patient benefits. At present, LTCBDE has not been effectively applied in many countries, and we hope that our efforts will improve the application of this technology.
Therefore, we retrospectively evaluated 400 patients who underwent LTCBDE in our institution over the past 8 years, aiming to explore the safety and effectiveness of this technology. Through the continuous maturity and promotion of our technology, LTCBDE has been effectively promoted and implemented.
Materials and Methods
Patients
A retrospective data analysis was conducted on 400 consecutive patients who underwent LTCBDE + LC at a single centre (The Second Affiliated Hospital of Nanchang University) from January 2014 to February 2022. The pre-operative diagnosis was based on clinical features (e.g. right upper abdominal pain, jaundice and cholangitis history), imaging (e.g. abdominal ultrasound, upper abdominal computed tomography [CT], and magnetic resonance cholangiopancreatography [MRCP]) findings suggestive of CBD stones, and laboratory test results (e.g. elevated bilirubin, alkaline phosphatase [ALP], and/or gamma-glutamyl transferase levels). In general, abdominal ultrasound, upper abdominal CT and liver function blood tests are first-line examinations for the diagnosis of cholecystolithiasis and choledocholithiasis. Herein, MRCP was performed when the presence of stones was unclear based on the findings of the abovementioned examinations. The exclusion criteria were as follows: (1) biliary tract neoplasms, (2) Mirizzi syndrome, (3) intrahepatic bile duct stones and (4) severe acute pancreatitis requiring ERCP.
Clinical Data
The clinical information for this study included patient demographic characteristics (e.g. age, sex, American Society of Anesthesiologists Classification, laboratory test results, history of abdominal operation and reasons for ERCP failure), patient disease characteristics (e.g. diameter of the cystic duct and CBD, number of CBD stones and maximum diameter of CBD stones), and surgical outcomes (e.g. cystic duct incision, stone removal method, handling of the cystic duct stump, reasons for surgical failure, duration of operation and post-operative adverse events). Pre-operative imaging examinations (e.g. abdominal ultrasound, upper abdominal CT and MRCP) were performed to evaluate the disease characteristics of the bile duct anatomy, cystic duct diameter, CBD diameter and number of gallstones. This study was approved by the Ethics Committee of The Second Affiliated Hospital of Nanchang University, and informed consent was obtained from all patients.
Operative Techniques
The patients were placed in the supine position with their head and trunk tilted 15° to the left. CO2 pneumoperitoneum was established after general anaesthesia and maintained at 12–14 mmHg (1 mmHg = 0.133 kPa). For LTCBDE, the four-hole method was used. The first 10-mm trocar was placed 10 mm below the umbilicus as an observation hole, and a 30-degree laparoscope was placed. The other three trocars were placed under direct laparoscopic view: A 12-mm trocar was placed under the xyphoid process as the main operating hole, and two 5-mm trocars were placed 5 cm below the intersection of the right midclavicular line and rib margin and 8 cm below the intersection of the right anterior axillary line and rib margin as the auxiliary operating holes.
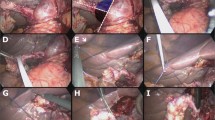
The fat tissue was carefully dissected and removed at the Calot triangle and the confluence of the cystic duct and CBD, exposing the gallbladder tube, gallbladder artery and confluence of the cystic duct and CBD. The cystic artery was clamped and cut off using an absorbable clip. The proximal end of the cystic duct was clamped using a titanium clip to prevent flow of bile and stones from the gallbladder. The cystic duct incision was based on the diameter of the cystic duct and size of the stone (Fig. 2). In general, if the diameter of the cystic duct is > 5 mm, a direct transverse incision of the cystic duct is the first option (Fig. 2A and B); herein, an attempt was made to place a 5-mm flexible choledochoscope into the CBD after routine dilatation of the cystic duct using a balloon catheter. If the diameter of the cystic duct is < 5 mm, the anterior wall of the cystic duct must be incised T-shaped (Fig. 2C and D) with the support of a balloon catheter, and the choledochoscope must then be placed. If the choledochoscope cannot be placed, a microincision (Fig. 2E and F) should be made at the confluence of the cystic duct and CBD, and the choledochoscope can then be inserted.
During the operation, a 5-mm flexible choledochoscope from under the xyphoid process 12-mm trocar through the cystic duct into the CBD and direct exposure of CBD stones. In general, CBD stones are removed using a metal basket. Some stone incarceration in the CBD cannot be removed using a metal basket; therefore, it can be removed via laser lithotripsy (U-100 system, World of Medicine, Berlin, Germany). After successful removal of stones, the distal bile duct and intrahepatic bile duct were carefully examined two to three times, and the number of stones was compared with the results of the pre-operative imaging examinations (abdominal ultrasound, upper abdominal CT and MRCP) to ensure that the stones were removed. The residual ends of the cystic duct were ligated using absorbable clips or sutures. Finally, the gallbladder and stones were removed, and a drainage tube was placed in the Winslow hole. For patients in whom LTCBDE failed, LCBDE + T-tube drainage was performed to ensure stone removal.
Post-operative Care and Follow-up
Post-operatively, the patients recovered in a quiet and stable state in the general ward for hepatobiliary operation. Routine blood test results, liver function, bile leakage, drainage tube extubation time, post-operative hospital stay duration and other patient data were evaluated and analysed. Follow-up at the clinic 2 weeks after discharge and telephone follow-up every 3 months were conducted. When abnormal bilirubin levels or persistent right upper abdominal pain was found during follow-up, abdominal CT or MRCP was performed to screen for bile duct stenosis or residual stones. Other follow-up indicators included the general situation of the patients, diet and operation-related discomfort.
Statistical Analysis
We used IBM SPSS version 25.0 (SPSS Inc., Chicago, IL, USA) for the statistical analysis. All continuous variables were presented as means ± standard deviations and classification data as numbers and percentages. The Cochran–Mantel–Haenszel χ2 test was used to compare the demographic characteristics and clinical manifestations between the first 200 and last 200 LTCBDE cases. P < 0.05 was considered to be statistically significant.
Results
In the past 8 years, a total of 400 patients with suspected or diagnosed cholecystolithiasis and choledocholithiasis underwent LTCBDE. Of them, 188 (47%) were males, and 212 (53%) were females; 26 (6.5%) were older than 80 years. The demographic characteristics and clinical manifestations of the first and second groups were similar (Table 1); however, the patients with cholecystolithiasis and choledocholithiasis with CBD no-dilatation (2.5% vs 28.5%, P < 0.001), CBD diameter (10.89 ± 1.76 vs 9.97 ± 2.39 mm, P < 0.05), cystic duct diameter (4.62 ± 1.03 vs 5.03 ± 1.29 mm, P < 0.05), number of CBD stones (2.01 ± 0.95 vs 1.79 ± 0.86, P < 0.05), pre-operative total bilirubin level (44.97 ± 33.83 vs 37.92 ± 33.89 μmol/L, P = 0.039) and pre-operative ALP level (361.14 ± 308.75 vs 203.89 ± 159.39 U/L, P = 0.010).
The intraoperative data are summarised in Table 2. The LTCBDE success rate was 91.5% and 97.0% in the first and second groups, respectively (P = 0.018). The reason for LTCBDE failure was the intraoperative inability to insert the choledochoscope into the cystic duct. Laparoscopic choledocholithotomy and T-tube drainage were performed in 23 (5.8%) patients in whom LTCBDE failed; the rate among the last 200 LTCBDE cases was significantly lower than that among the first 200 LTCBDE cases (3.0% vs 8.5%, P = 0.018). Thirty-one (7.8%) patients with incarcerated stones underwent laser lithotripsy, and the utilisation rate of laser lithotripsy in the first and second groups was 3.0% and 12.5%, respectively (P < 0.001). No stones were found during operation in 10 (2.5%) patients. The operation time in the first and second groups was 164.60 ± 24.30 and 135.34 ± 30.00 min, respectively (P < 0.05), and the estimated intraoperative blood loss amount was 42.23 ± 36.77 and 32.63 ± 30.59 mL, respectively (P < 0.05).
The post-operative results are summarised in Table 3. The overall incidence of post-operative complications in the 400 patients was relatively low (2%), with residual stones being the main complication observed (1.5%). The stones of 377 (94.3%) patients who underwent LTCBDE were all removed. One (0.3%) patient developed acute peritonitis on the second day after operation. Emergency laparotomy and suturing revealed perforation of the duodenal ulcer. The patients recovered smoothly after operation; 23 (5.7%) patients in whom treatment was converted to LTCBDE + T-tube drainage during operation returned to the hospital for T-tube cholangiography 1–2 months after operation. Among them, six (26%) patients had residual stones. The patients underwent a second operation, and the stones were removed through the T-tube. One (4.3%) patient in whom treatment was converted to LTCBDE + T-tube drainage during operation had an ink-green liquid drained from the Winslow hole after operation. Laparoscopic exploration was performed when the conservative treatment was ineffective. Bile leakage was observed in the T-tube suture, and suture reinforcement was performed. The general condition of the patient was stable post-operatively. There was no significant difference in the post-operative hospital stay duration and drainage tube extraction time between the two groups.
The follow-up period ranged from 3 to 12 months, with an average duration of 6 months. During follow-up, no bile leakage, bile duct stenosis, bile duct injury, residual stones or other complications occurred in the patients in whom LTCBDE was successful.
Discussion
LTCBDE is an effective and minimally invasive method for treating cholecystolithiasis combined with choledocholithiasis. The stone clearance rate is 85–95%.3,4,5,6,7,8,9,10,11,12,22 This technique does not destroy the function of duodenal papilla or damage the CBD. Compared with LCBDE + LC, complications after operation, such as water and electrolyte disorders, bile duct stenosis and bile leakage caused by indwelling T-tube placement, are avoided with LTCBDE.23 Compared with ERCP + LC, complications, such as Oddis sphincter injury, duodenal perforation, pancreatitis and bile reflux caused by ERCP are avoided with LTCBDE.24,25,26 Furthermore, LTCBDE yields a shorter hospital stay duration and lower hospitalisation costs than do other procedures.20,21,22,23,24,25,26,27
The function of the cystic duct is similar to that of the sphincter and can coordinate gallbladder filling. The diameter of the confluence of the cystic duct and CBD is wider than that of the CBD. When the CBD is blocked, the diameter of the cystic duct can be expanded to > 1 cm, which makes the expansion of the confluence of the cystic duct and CBD more obvious.28 The anatomical characteristics of the cystic duct and CBD create favourable conditions for LTCBDE. However, the difficulty of LTCBDE is the insertion of a choledochoscope into the cystic duct. Our centre overcame this difficulty by selecting a transverse incision, T-shaped incision and microincision at the confluence of the cystic duct and CBD for different diameters of the cystic duct.20,21 A balloon catheter was used to expand the cystic duct during microincision or T-shaped incision at the confluence of the cystic duct and CBD to avoid simultaneous incision of the anterior and posterior walls of the cystic duct. If these three methods are used during operation, a choledochoscope could not be inserted into the CBD through the cystic duct. It is then recommended to convert treatment to LCBDE + T-tube drainage during operation.
Because LTCBDE requires the insertion of a choledochoscope into the CBD through the cystic duct, there is a certain degree of limitation in patient selection. In the first 200 LTCBDE cases herein, a large proportion of treatments were converted to LCBDE during operation owing to the lack of experience in screening patients in the early stage. As a result, the patients in whom treatment was converted to LCBDE needed to carry T-tubes. When the stones were not removed completely, they needed a second operation, which inconvenienced their daily lives. Therefore, pre-operative MRCP should comprehensively evaluate the diameter of the cystic duct, diameter of the CBD and course of the CBD to assess whether patients are suitable for LTCBDE. Our centre suggests that the diameter of the cystic duct in patients who undergo LTCDBE should be ≥ 30 mm and that the number of stones should be ≤ 5.20 In terms of the timing of operation, it is best to operate within 72 h of diagnosis; in this time period, the degree of abdominal adhesion and inflammation is less, which is conducive to the operation. Furthermore, liver function should not be seriously impaired before operation. If the pre-operative bilirubin level is high, the tube should be placed during operation.
ERCP + phase II LC is the first treatment option for patients with cholecystolithiasis, choledocholithiasis and non-dilatation of the CBD.29 However, in the treatment of such patients, we encountered various reasons (Billroth II or Roux-en-Y gastric operation, presence of duodenal papillary diverticulum, patient intolerance or operator or technical difficulties) that led to ERCP failure. Such patients are prone to developing biliary strictures after operation because the CBD itself does not expand. Initially, we selected LCBDE + LC, while placing T-tubes for support, so as to prevent post-operative biliary stricture. However, indwelling T-tube placement reduces the quality of life of patients and can easily cause complications, such as water and electrolyte disorders and bile leakage.30 Therefore, based on our experience of a large number of LTCBDE cases,20,21,22,23,24,25,26,27,28,29,30,31 we began to perform LTCBDE in patients with cholecystolithiasis, choledocholithiasis and non-dilatation of the CBD in whom ERCP failed, and the research results have been reported in the literature. Based on our previous study findings, LTCBDE is also safe and effective for patients with non-dilatation of the CBD.21
After the choledochoscope was inserted into the CBD, it was not recommended to use water directly for pressure flushing at the beginning, which would cause some stones to enter the intrahepatic bile duct. Usually, most stones can be directly removed using a metal basket. Incarcerated stones need to be broken using laser and then removed using a metal basket. With the popularisation of laser lithotripsy and metal baskets, the stone extraction time has been effectively shortened; consequently, the operation time has been significantly shortened. After the stones were removed, the distal and intrahepatic bile ducts were repeatedly explored to avoid residual stones in our study. The number of stones removed should be consistent with the number of pre-operative imaging examinations performed. If the number is inconsistent, it is necessary to continue exploring the bile duct to ensure that all stones are removed.
Because more non-dilated CBD patients were included in the second group, linear lithotripsy was used more frequently there. In this part of the patients, the CBD itself is not dilated, and if secondary CBD stones are present and the number of stones is greater or the diameter of the stones is larger, the stones tend to be incarcerated in the CBD. The second group had larger stone diameters than the first group and included more patients with non-dilated CBD, resulting in smaller CBD diameters than the first group, so the probability of stones becoming incarcerated in the CBD was greater than in the first group. The number of stones in the first group was higher than in the second group because the early selection of patients focused on the number of stones rather than on their diameter; as far as possible in the technology that is not yet in the mature stage, as much as possible patients with smaller stone diameter are to be selected. Although the number of stones in the first group was higher than in the second group, the stones were smaller in diameter and the diameter of the CBD was larger, so there was less chance of stones becoming incarcerated in the CBD.
Cystic duct stumps should be carefully treated. Different treatment methods must be selected according to different incision methods. For patients with transverse incisions, an absorbable clip is used to clamp the stump; for those with T-shaped incisions with a certain distance from the confluence of the cystic duct and CBD, an absorbable clip can also be used for direct clamping. However, for patients with T-shaped incisions near the confluence and microincision at the confluence of the cystic duct and CBD, absorbable sutures should be used to treat the stump. This procedure does not injure the CBD and only involves the dilated portion of the confluence of the cystic duct and CBD; therefore, the development of biliary strictures may be reduced after operation.
Complications, such as bile leakage and bile duct stenosis, are likely to occur after biliary operation. Attention should be paid to the following two points to prevent post-operative bile leakage: Firstly, CBD stones should be removed; otherwise, post-operative residual stones will lead to bile duct obstruction, and an increase in bile duct pressure will lead to bile leakage at the stump of the cystic duct. Secondly, when an absorbable clip is used to clamp the stump of the cystic duct, the clip should completely fix the stump of the cystic duct. Suturing the confluence of the cystic duct and CBD ensures a full-thickness suture. For a T-shaped incision that has reached confluence and microincision, the anterolateral wall of the CBD and the lateral-posterior wall of the cystic duct must be sutured. CBD injury should be avoided during suturing to avoid post-operative bile duct stenosis as much as possible.
Liver function was assessed within 3 days after operation. If the post-operative bilirubin level is high, residual calculus may be considered. During follow-up, the patients were asked whether there were post-operative abdominal pain, jaundice, fever and other symptoms to rule out biliary obstruction caused by residual stones, and MRCP was performed to check for residual stones in the CBD and cystic duct stump. In this study, no patients were lost to follow-up. During follow-up, no complications, such as biliary stricture, bile leakage or residual stones, were found in the patients in whom LTCBDE was successful. If residual CBD stones are present after operation, the optimal scheme for further treatment is still uncertain. To date, no patient has reported any residual stones after LTCBDE at our centre.
Our study found that the operation time of the last 200 LTCBDE cases was significantly shorter than that of the first 200 LTCBDE cases, reflecting the learning curve required to perform this procedure. The surgeon’s proficiency in this technique is reflected in the operation time. This study included all patients who underwent LTCBDE in our centre; differences in the surgeon performing the procedure will also lead to differences in the operation time. With the development of technology, laser lithotripsy has gradually been applied in clinical practice. Laser lithotripsy for incarcerated stones significantly shortens the operation time. With cystic duct incision, flexible use of the three abovementioned cystic duct incision methods can significantly shorten the operation time and reduce the probability of conversion to LCBDE. Through regression analysis, it was found that the regression coefficient value of cystic duct diameter (mm) was − 0.051 (t = − 5.394, P = 0.000 < 0.01), which meant that the size of cystic duct diameter (mm) would have a significant negative impact on whether to convert to LCBDE. Some patients with a history of upper abdominal operation and abdominal adhesions can also have a prolonged operation time.
There are still some difficulties in learning the LTCBDE method. Before learning LTCBDE, we suggest accumulating sufficient experience with LCBDE and choledochoscopy. Because there is a physiological angle between the cystic duct and CBD, it is necessary for the operator to have a relatively skilled choledochoscopic technique to facilitate the operation and avoid residual stones when using a choledochoscope to examine the intrahepatic bile duct. When LTCBDE is performed in patients with non-dilatation of the CBD, it is necessary to continue on the basis of extensive experience with LTCBDE of CBD expansion to avoid damage to the CBD as much as possible.
With the continuous maturity of our technology, we have organised LTCBDE learning classes every 3 months since last year, hoping that more surgeons can learn and master this technology. With our help, many medical centres can perform LTCBDE independently on the basis of constant familiarity with the three abovementioned cystic duct incision methods. LTCBDE has been effectively promoted and applied, so that more patients can benefit from it.
Our study has some limitations. Firstly, because the sample size was relatively small, especially that of the patients with non-dilatation of the CBD, we need to increase the sample size to further verify the study findings. Secondly, this study had a retrospective design, which may cause a certain deviation in the results; thus, multicentre clinical trials are needed to confirm the findings.
In summary, this study confirmed that LTCBDE is safe and effective in the treatment of cholecystolithiasis and choledocholithiasis. With the continuous maturity of our technology and continuous efforts, LTCBDE has been effectively promoted and applied.
Data Availability
The data that support the findings of this study are available from the corresponding author, [Lu Fang], upon reasonable request.
References
1 Tazuma S. Gallstone disease: Epidemiology, pathogenesis, and classification of biliary stones (common bile duct and intrahepatic). Best practice & research Clinical gastroenterology 2006;20(6):1075-1083.
2 Zhang W, Wang BY, Du XY, Fang WW, Wu H, Wang L, Zhuge YZ, Zou XP. Big-data analysis: A clinical pathway on endoscopic retrograde cholangiopancreatography for common bile duct stones. World journal of gastroenterology 2019;25(8):1002-1011.
3 Portincasa P, Di Ciaula A, de Bari O, Garruti G, Palmieri VO, Wang DQ. Management of gallstones and its related complications. Expert review of gastroenterology & hepatology 2016;10(1):93-112.
4 Elmunzer BJ, Noureldin M, Morgan KA, Adams DB, Coté GA, Waljee AK. The Impact of Cholecystectomy After Endoscopic Sphincterotomy for Complicated Gallstone Disease. The American journal of gastroenterology 2017;112(10):1596-1602.
5 Boerma D, Schwartz MP. Gallstone disease. Management of common bile-duct stones and associated gallbladder stones: Surgical aspects. Best practice & research Clinical gastroenterology 2006;20(6):1103-1116.
6 Williams EJ, Green J, Beckingham I, Parks R, Martin D, Lombard M. Guidelines on the management of common bile duct stones (CBDS). Gut 2008;57(7):1004-1021.
7 Khaled YS, Malde DJ, de Souza C, Kalia A, Ammori BJ. Laparoscopic bile duct exploration via choledochotomy followed by primary duct closure is feasible and safe for the treatment of choledocholithiasis. Surgical endoscopy 2013;27(11):4164-4170.
8 Aawsaj Y, Light D, Horgan L. Laparoscopic common bile duct exploration: 15-year experience in a district general hospital. Surgical endoscopy 2016;30(6):2563-2566.
9 Lyass S, Phillips EH. Laparoscopic transcystic duct common bile duct exploration. Surgical endoscopy 2006;20 Suppl 2:S441-445.
10 van Dijk AH, Lamberts M, van Laarhoven CJ, Drenth JP, Boermeester MA, de Reuver PR. Laparoscopy in cholecysto-choledocholithiasis. Best practice & research Clinical gastroenterology 2014;28(1):195-209.
11 Lacitignola S, Minardi M. Management of common bile duct stones: a ten-year experience at a tertiary care center. JSLS : Journal of the Society of Laparoendoscopic Surgeons 2008;12(1):62-65.
12 Petelin JB. Laparoscopic common bile duct exploration. Surgical endoscopy 2003;17(11):1705-1715.
13 Loperfido S, Angelini G, Benedetti G, Chilovi F, Costan F, De Berardinis F, De Bernardin M, Ederle A, Fina P, Fratton A. Major early complications from diagnostic and therapeutic ERCP: a prospective multicenter study. Gastrointestinal endoscopy 1998;48(1):1-10.
14 Wang P, Li ZS, Liu F, Ren X, Lu NH, Fan ZN, Huang Q, Zhang X, He LP, Sun WS, Zhao Q, Shi RH, Tian ZB, Li YQ, Li W, Zhi FC. Risk factors for ERCP-related complications: a prospective multicenter study. The American journal of gastroenterology 2009;104(1):31-40.
15 Ahmed I, Pradhan C, Beckingham IJ, Brooks AJ, Rowlands BJ, Lobo DN. Is a T-tube necessary after common bile duct exploration? World journal of surgery 2008;32(7):1485-1488.
16 Wu X, Yang Y, Dong P, Gu J, Lu J, Li M, Mu J, Wu W, Yang J, Zhang L, Ding Q, Liu Y. Primary closure versus T-tube drainage in laparoscopic common bile duct exploration: a meta-analysis of randomized clinical trials. Langenbeck's archives of surgery 2012;397(6):909-916.
17 Yin Z, Xu K, Sun J, Zhang J, Xiao Z, Wang J, Niu H, Zhao Q, Lin S, Li Y. Is the end of the T-tube drainage era in laparoscopic choledochotomy for common bile duct stones is coming? A systematic review and meta-analysis. Annals of surgery 2013;257(1):54-66.
18 Estellés Vidagany N, Domingo Del Pozo C, Peris Tomás N, Díez Ares J, Vázquez Tarragón A, Blanes Masson F. Eleven years of primary closure of common bile duct after choledochotomy for choledocholithiasis. Surgical endoscopy 2016;30(5):1975-1982.
19 Shapiro SJ, Gordon LA, Daykhovsky L, Grundfest W. Laparoscopic exploration of the common bile duct: experience in 16 selected patients. Journal of laparoendoscopic surgery 1991;1(6):333-341.
20 Fang L, Wang J, Dai WC, Liang B, Chen HM, Fu XW, Zheng BB, Lei J, Huang CW, Zou SB. Laparoscopic transcystic common bile duct exploration: surgical indications and procedure strategies. Surgical endoscopy 2018;32(12):4742-4748.
21 Fang L, Huang J, Zheng H, Duan ZQ, Liu TD, Xiong H, Li W, Fu XW, Gao JF, Le H, Hu W, Liang B, Zhu XG. Laparoscopic transcystic common bile duct exploration in patients with a nondilated common bile duct. Annals of palliative medicine 2021;10(12):12845-12856.
Phillips EH, Rosenthal RJ, Carroll BJ, Fallas MJ. Laparoscopic trans-cystic-duct common-bile-duct exploration. Surgical endoscopy 1994;8(12):1389–1393; discussion 1393–1384.
23 Zhu HY, Xu M, Shen HJ, Yang C, Li F, Li KW, Shi WJ, Ji F. A meta-analysis of single-stage versus two-stage management for concomitant gallstones and common bile duct stones. Clinics and research in hepatology and gastroenterology 2015;39(5):584-593.
24 Zhao ZH, Hu LH, Ren HB, Zhao AJ, Qian YY, Sun XT, Su S, Zhu SG, Yu J, Zou WB, Guo XR, Wang L, Li ZS, Liao Z. Incidence and risk factors for post-ERCP pancreatitis in chronic pancreatitis. Gastrointestinal endoscopy 2017;86(3):519-524.e511.
25 Lyu Y, Cheng Y, Wang B, Xu Y, Du W. What is impact of nonsteroidal anti-inflammatory drugs in the prevention of post-endoscopic retrograde cholangiopancreatography pancreatitis: a meta-analysis of randomized controlled trials. BMC gastroenterology 2018;18(1):106.
26 Vezakis A, Fragulidis G, Polydorou A. Endoscopic retrograde cholangiopancreatography-related perforations: Diagnosis and management. World journal of gastrointestinal endoscopy 2015;7(14):1135-1141.
27 Czerwonko ME, Pekolj J, Uad P, Mazza O, Sanchez-Claria R, Arbues G, de Santibañes E, de Santibañes M, Palavecino M. Laparoscopic Transcystic Common Bile Duct Exploration in the Emergency Is as Effective and Safe as in Elective Setting. Journal of gastrointestinal surgery : official journal of the Society for Surgery of the Alimentary Tract 2019;23(9):1848-1855.
28 Feng Q, Huang Y, Wang K, Yuan R, Xiong X, Wu L. Laparoscopic Transcystic Common Bile Duct Exploration: Advantages over Laparoscopic Choledochotomy. PloS one 2016;11(9):e0162885.
29 Manes G, Paspatis G, Aabakken L, Anderloni A, Arvanitakis M, Ah-Soune P, Barthet M, Domagk D, Dumonceau JM, Gigot JF, Hritz I, Karamanolis G, Laghi A, Mariani A, Paraskeva K, Pohl J, Ponchon T, Swahn F, Ter Steege RWF, Tringali A, Vezakis A, Williams EJ, van Hooft JE. Endoscopic management of common bile duct stones: European Society of Gastrointestinal Endoscopy (ESGE) guideline. Endoscopy 2019;51(5):472-491.
30 Poulose BK, Arbogast PG, Holzman MD. National analysis of in-hospital resource utilization in choledocholithiasis management using propensity scores. Surgical endoscopy 2006;20(2):186-190.
31 Lei J, Wang J, Li Q, Wu P, Yuan R, Zhu H, Zou S, Shao J, Fang L. Laparoscopic Transcystic Common Bile Duct Exploration: T-Shaped Incision of Cystic Duct with FREDDY Laser Lithotripsy. Journal of laparoendoscopic & advanced surgical techniques Part A 2016;26(8):646-651.
Acknowledgements
We would like to thank the contributions of all of the patients in our retrospective study.
Funding
This work was supported by the National Natural Science Foundation of China (Grant No. 82160578); the Natural Science Foundation of Jiangxi Province (Grant Nos. 20212BCJ23024, 20202BAB216029, and 20202BABL206095); the Health Department of Jiangxi Province (Grant Nos. 20198020, 202210033); and the Education Department of Jiangxi Province (Grant No. GJJ190019).
Author information
Authors and Affiliations
Contributions
Conception and design of the manuscript: Bo Liang, Lu Fang, and Jian Huang. Acquisition of data: Yuting Fan, Liangzhi Xu, Jinghang Liu, Xinguo Tang, and Wei Hu. Analysis and interpretation of data: Lu Fang, Jian Huang, Tiande Liu, Hu Xiong, Wen Li, and Xiaowei Fu. Drafting of the manuscript: all the authors. Critical revision of the final version to be published: all the authors. Approval of the final version to be published: all the authors.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Huang, J., Hu, W., Liu, J. et al. Laparoscopic Transcystic Common Bile Duct Exploration: 8-Year Experience at a Single Institution. J Gastrointest Surg 27, 555–564 (2023). https://doi.org/10.1007/s11605-023-05594-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11605-023-05594-z