Abstract
Objective
This study aimed to investigate the safety and efficacy of endovascular aortic repair (EVAR) for the treatment of an abdominal aortic aneurysm (AAA) with a hostile neck anatomy (HNA).
Methods
From January 1, 2015 to December 31, 2019, a total of 259 patients diagnosed with an AAA who underwent EVAR were recruited into this study. Based on the morphological characteristics of the proximal neck anatomy, the patients were divided into the HNA group and the friendly neck anatomy (FNA) group. The patients were followed up for up to 4 years.
Results
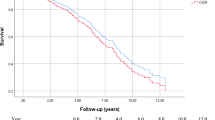
The average follow-up time was 1056.1±535.5 days. Type I endoleak occurred in 4 patients in the HNA group, and 2 patients in the FNA group. Neither death nor intraoperative switch to open repair occurred in either group. The time of the operation was significantly longer in the HNA group (FNA vs. HNA, 99.2±51.1 min vs. 117.5±63.8 min, P=0.011). There were no significant differences in short-term clinical success rate (P=0.228) or midterm clinical success rate (P=0.889) between the two groups. The overall mortality rate was 10.4%, and Kaplan-Meier survival analysis indicated that the two groups had similar cumulative survival rates at the end of the follow-up period (P=0.889).
Conclusion
EVAR was feasible and safe in patients with an AAA with a proximal HNA. The early and midterm results were promising; however, further studies are needed to verify the long-term effectiveness of EVAR.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Brown LC, Powell JT. Risk factors for aneurysm rupture in patients kept under ultrasound surveillance. UK Small Aneurysm Trial Participants. Ann Surg, 1999,230(3):189–196
Glimåker H, Holmberg L, Elvin A, et al. Natural history of patients with abdominal aortic aneurysm. Eur J Vasc Surg, 1991,5(2):125–130
Moll FL, Powell JT, Fraedrich G, et al. Management of abdominal aortic aneurysms clinical practice guidelines of the European society for vascular surgery. Eur J Vasc Endovasc Surg, 2011,41(Suppl 1):S1–S58
Bengtsson H, Bergqvist D. Ruptured abdominal aortic aneurysm: a population-based study. J Vasc Surg, 1993,18(1):74–80
Szilagyi DE, Hageman JH, Smith RF, et al. Spinal cord damage in surgery of the abdominal aorta. Surgery, 1978,83(1):38–56
Parodi JC, Palmaz JC, Barone HD, et al. Transfemoral intraluminal graft implantation for abdominal aortic aneurysms. Ann Vasc Surg, 1991,5(6):491–499
Chadi SA, Rowe BW, Vogt KN, et al. Trends in management of abdominal aortic aneurysms. J Vasc Surg, 2012,55(4):924–928
Li FF, Shang XK, Du XL, et al. Rapamycin Treatment Attenuates Angiotensin II-induced Abdominal Aortic Aneurysm Formation via VSMC Phenotypic Modulation and Down-regulation of ERK1/2 Activity. Curr Med Sci, 2018,38(1):93–100
Ding YC, Zhang XJ, Zhang JX, et al. Progression and Regression of Abdominal Aortic Aneurysms in Mice. Curr Med Sci, 2021,41(5):901–908
Stather PW, Sayers RD, Cheah A, et al. Outcomes of endovascular aneurysm repair in patients with hostile neck anatomy. Eur J Vasc Endovasc Surg, 2012,44(6):556–561
Buth J, van Marrewijk CJ, Harris PL, et al. Outcome of endovascular abdominal aortic aneurysm repair in patients with conditions considered unfit for an open procedure: a report on the EUROSTAR experience. J Vasc Surg, 2002,35(2):211–221
Antoniou GA, Georgiadis GS, Antoniou SA, et al. A meta-analysis of outcomes of endovascular abdominal aortic aneurysm repair in patients with hostile and friendly neck anatomy. J Vasc Surg, 2013,57(2):527–538
Sakalihasan N, Limet R, Defawe OD, et al. Abdominal aortic aneurysm. Lancet (London, England),2005,365(9470):1577–1589
Chaikof EL, Blankensteijn JD, Harris PL, et al. Reporting standards for endovascular aortic aneurysm repair. J Vasc Surg, 2002,35(5):1048–1060
Setacci F, Sirignano P, de Donato G, et al. AAA with a challenging neck: early outcomes using the endurant stent-graft system. Eur J Vasc Endovasc Surg, 2012,44(3):274–279
Dillavou ED, Muluk SC, Rhee RY, et al. Does hostile neck anatomy preclude successful endovascular aortic aneurysm repair?. J Vasc Surg, 2003,38(4):657–663
Choke E, Munneke G, Morgan R, et al. Outcomes of endovascular abdominal aortic aneurysm repair in patients with hostile neck anatomy. Cardiovasc Intervent Radiol, 2006,29(6):975–980
Cox DE, Jacobs DL, Motaganahalli RL, et al. Outcomes of endovascular AAA repair in patients with hostile neck anatomy using adjunctive balloon-expandable stents. Vasc Endovascular Surg, 2006,40(1):35–40
EVAR trial participants. Endovascular aneurysm repair versus open repair in patients with abdominal aortic aneurysm (EVAR trial 1): randomised controlled trial. Lancet (London, England),2005,365(9478):2179–2186
Hoshina K, Ishimaru S, Sasabuchi Y, et al. Outcomes of Endovascular Repair for Abdominal Aortic Aneurysms: A Nationwide Survey in Japan. Ann Surg, 2019,269(3):564–573
Hultgren R, Granath F, Swedenborg J, et al. Different disease profiles for women and men with abdominal aortic aneurysms. Eur J Vasc Endovasc Surg, 2007,33(5):556–560
Kent KC, Zwolak RM, Egorova NN, et al. Analysis of risk factors for abdominal aortic aneurysm in a cohort of more than 3 million individuals. J Vasc Surg, 2010,52(3):539–548
Dahl M, Frost L, Sogaard R, et al. A population-based screening study for cardiovascular diseases and diabetes in Danish postmenopausal women: acceptability and prevalence. BMC Cardiovasc Disord, 2018,18(1):20
Oliver-Williams C, Sweeting MJ, Turton G, et al. Lessons learned about prevalence and growth rates of abdominal aortic aneurysms from a 25-year ultrasound population screening programme. Br J Surg, 2018,105(1):68–74
Carpenter JP, Baum RA, Barker CF, et al. Impact of exclusion criteria on patient selection for endovascular abdominal aortic aneurysm repair. J Vasc Surg, 2001,34(6):1050–1054
Thompson MM. Controlling the expansion of abdominal aortic aneurysms. Br J Surg, 2003,90(8):897–898
Anjum A, Powell JT. Is the incidence of abdominal aortic aneurysm declining in the 21st century? Mortality and hospital admissions for England & Wales and Scotland. Eur J Vasc Endovasc Surg, 2012,43(2):161–166
Jacomelli J, Summers L, Stevenson A, et al. Update on the prevention of death from ruptured abdominal aortic aneurysm. J Med Screen, 2017,24(3):166–168
Lawrence VA, Cornell JE, Smetana GW, et al. Strategies to reduce postoperative pulmonary complications after noncardiothoracic surgery: systematic review for the American College of Physicians. Ann Intern Med, 2006,144(8):596–608
AbuRahma AF, Campbell J, Stone PA, et al. The correlation of aortic neck length to early and late outcomes in endovascular aneurysm repair patients. J Vasc Surg, 2009,50(4):738–748
Walker J, Tucker LY, Goodney P, et al. Adherence to endovascular aortic aneurysm repair device instructions for use guidelines has no impact on outcomes. J Vasc Surg, 2015,61(5):1151–1159
Stather PW, Wild JB, Sayers RD, et al. Endovascular aortic aneurysm repair in patients with hostile neck anatomy. J Endovasc Ther, 2013,20(5):623–637
Schanzer A, Greenberg RK, Hevelone N, et al. Predictors of abdominal aortic aneurysm sac enlargement after endovascular repair. Circulation, 2011,123(24):2848–2855
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
The authors declare that they have no conflicts of interest.
Author Yi-qing LI is a member of the Editorial Board for Current Medical Science. The paper was handled by other editors and has undergone rigorous peer review process. Author Yi-qing LI was not involved in the journal’s review of, or decisions related to, this manuscript.
Additional information
This work was supported financially by grants from the National Natural Science Foundation of China (No. 81900432) and the Science Foundation of Union Hospital (No. F016.02004.21003.124).
Rights and permissions
About this article
Cite this article
Ke, Zx., Chen, Gz., Hu, K. et al. Safety and Efficacy of Endovascular Aortic Repair for Abdominal Aortic Aneurysms with a Hostile Neck Anatomy. CURR MED SCI 43, 1221–1228 (2023). https://doi.org/10.1007/s11596-023-2822-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-023-2822-6