Abstract
Objective
To investigate the epidemiological features in children after the coronavirus disease 2019 (COVID-19) pandemic.
Methods
This study collected throat swabs and serum samples from hospitalized pediatric patients of Renmin Hospital of Wuhan University, Wuhan, Hubei province, China before and after the COVID-19 pandemic. Respiratory infected pathogens [adenovirus (ADV), influenza virus A/B (Flu A/B), parainfluenza virus 1/2/3 (PIV1/2/3), respiratory syncytial virus (RSV), Mycoplasma pneumoniae (MP), and Chlamydia pneumoniae (CP)] were detected. The pathogens, age, and gender were used to analyze the epidemiological features in children after the COVID-19 pandemic.
Results
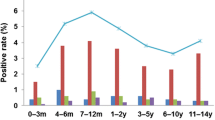
The pathogen detection rate was significantly higher in females than in males (P<0.05), and the infection of PIV1 and MP was mainly manifested. After the COVID-19 pandemic, PIV1, PIV3, RSV, and MP had statistically different detection rates among the age groups (P<0.05), and was mainly detected in patients aged 0–6 years, 0–3 years, 0–3 years, and 1–6 years, respectively. When comparing before the COVID-19 pandemic, the total detection rate of common respiratory pathogens was lower (P<0.05). Except for the increase in the detection rate of PIV1 and CP, the infection rate of other pathogens had almost decreased.
Conclusion
The prevention and control measures for the COVID-19 pandemic effectively changed the epidemiological features of common respiratory tract infectious diseases in pediatric children.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Bicer S, Giray T, Çöl D, et al. Virological and clinical characterizations of respiratory infections in hospitalized children. Ital J Pediatr, 2013,39:22
Jain S, Williams DJ, Arnold SR, et al. CDC EPIC Study Team. Community acquired pneumonia requiring hospitalization among U.S. children. N Engl J Med, 2015,372: 835 845
Wang H, Gu J, Li X, et al. Broad range detection of viral and bacterial pathogens in bronchoalveolar lavage fluid of children to identify the cause of lower respiratory tract infections. BMC Infect Dis, 2021,21(1):152
Miller EK, Linder J, Kraft D, et al. Hospitalizations and outpatient visits for rhinovirus-associated acute respiratory illness in adults. J Allergy Clin Immunol, 2016, 137 (3):734–743
Kumar V. Influenza in Children. Indian J Pediatr, 2017,84(2):139–143
GBD 2015 LRI Collaborators. Estimates of the global, regional, and national morbidity, mortality, and aetiologies of lower respiratory tract infections in 195 countries: a systematic analysis for the Global Burden of Disease Study 2015. Lancet Infect Dis, 2017,17(11):1133–1161
Garcia-Garcia ML, Calvo Rey C, Del Rosal Rabes T. Pediatric Asthma and Viral Infection. Arch Bronconeumol, 2016,52(5):269–273
Shachor-Meyouhas Y, Hadash A, Kra-Oz Z, et al. Adenovirus Respiratory Infection among Immunocompetent Patients in a Pediatric Intensive Care Unit During 10-year period: Co-morbidity is common. Isr Med Assoc J, 2019,21(9):595–598
Goikhman Y, Drori Y, Friedman N, et al. Adenovirus load correlates with respiratory disease severity among hospitalized pediatric patients. Int J Infect Dis, 2020, 97:145–150
Yoon YK, Park CS, Kim JW, et al. Guidelines for the antibiotic use in children with lower respiratory tract infections. Infect Chemother, 2017,49(4):326–352
Waites KB, Xiao L, Liu Y, et al. Mycoplasma pneumoniae from the respiratory tract and beyond. Clin Microbiol Rev, 2017,30(30):747e809
Kutty PK, Jain S, Taylor TH, et al. Mycoplasma pneumoniae among children hospitalized with community-acquired pneumonia. Clin Infect Dis, 2019,68(1):5–12
Yoon IA, Hong KB, Lee HJ, et al. Radiologic findings as a determinant and no effect of macrolide resistance on clinical course of Mycoplasma pneumoniae pneumonia. BMC Infect Dis, 2017,17(1):402
Zhu N, Zhang D, Wang W, et al. China Novel Coronavirus Investigating and Research Team. A novel coronavirus from patients with pneumonia in China. N Engl J Med, 2019,382(8):727–733
Ward C, Baker K, Marks S, et al. Determining the Agreement Between an Automated Respiratory Rate Counter and a Reference Standard for Detecting Symptoms of Pneumonia in Children: Protocol for a Cross-Sectional Study in Ethiopia. JMIR Res Protoc, 2020,9(4):e16531
Unger SA, Bogaert D. The respiratory microbiome and respiratory infections. J Infect, 2017,74(Suppl 1):S84–S88
Dagne H, Andualem Z, Dagnew B, et al. Acute respiratory infection and its associated factors among children under-five years attending pediatrics ward at University of Gondar Comprehensive Specialized Hospital, Northwest Ethiopia: institution-based cross-sectional study. BMC Pediatrics, 2020,20:93
Critchley IA, Brown SD, Traczewski MM, et al. National and regional assessment of antimicrobial resistance among community-acquired respiratory tract pathogens identified in a 2005–2006 U.S. Faropenem surveillance study. Antimicrob Agents Chemother, 2007,51(12):4382–4389
Wang J, Wang Z. Strengths, Weaknesses, Opportunities and Threats (SWOT) Analysis of China’s Prevention and Control Strategy for the COVID-19 Epidemic. Int J Environ Res Public Health, 2020,17(7):2235
Liu R, Shen BZ, Zhang QY, et al. Etiological analysis of respiratory tract infection in 12 881 hospitalized children in Wuhan city. Med J Wuhan Univ, 2020,41:791–795
Na R, Zhang JY, Si P, et al. Epidemiological characteristics of common non-bacterial pathogens in 18252 children with acute respiratory infections. CHN MCH, 2019,34:3490–3492
Fiala J, Brázdová Z. A comparison between the lifestyles of men and women—parents of school age children. Cent Eur J Public Health, 2000,8(2):94–100
Zhang GQ, Pan HQ, Hu XX, et al. The role of isolation rooms, facemasks and intensified hand hygiene in the prevention of nosocomial COVID-19 transmission in a pulmonary clinical setting. Infect Dis Poverty, 2020,9(1):104
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
The authors declared no conflict of interest.
Additional information
This work was supported by grants from the Fundamental Research Funds for the Central Universities (No. 2042022kf1215), the Special Funds for Innovation in Scientific Research Program of Zhongshan (No. 2020AG024), Chinese Foundation for Hepatitis Prevention and Control: TianQing Liver Disease Research Fund Subject (No. TGQB20210109), the Open Funds of Key Laboratory of Diagnosis and Treatment of Digestive System Tumors of Zhejiang Province (No. KFJJ-202005 and No. KFJJ-201907), the Open Research Program of the State Key Laboratory of Virology of China (No. 2021KF002 and No. 2021KF006), the Natural Science Foundation of Hubei Province (No. 2020CFB619), and Wuhan Municipal Health Research Foundation (No. WX21Z36).
Rights and permissions
About this article
Cite this article
Ma, Je., Ma, Qf., Wang, W. et al. Analysis of Common Respiratory Infected Pathogens in 3100 Children after the Coronavirus Disease 2019 Pandemic. CURR MED SCI 42, 1094–1098 (2022). https://doi.org/10.1007/s11596-022-2635-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11596-022-2635-z