Abstract
The COVID-19 pandemic introduced additional health challenges for people who use substances (PWUS) amid the overdose crisis. Numerous harm reduction services, including supervised consumption sites (SCS) across Canada, faced shutdowns and reduced operating capacity in order to comply with public health measures. Mobile Overdose Response Services (MORS) are novel overdose prevention technologies that allow those who are unable to access alternative means of harm reduction to consume substances under the virtual supervision of a trained operator. Here, we examine the role of MORS in the context of the COVID-19 pandemic. A total of 59 semi-structured interviews were conducted with the following key interest groups: PWUS, healthcare providers, harm reduction workers, MORS operators, and the general public. Inductive thematic analysis informed by grounded theory was used to identify major themes pertaining to the perception of MORS. As the pandemic shifted the public focus away from harm reduction, many participants viewed MORS as an acceptable strategy to reduce the harms associated with solitary substance and alleviate the sense of isolation driven by social distancing measures. While the pandemic may have increased the utility of MORS, concerns surrounding personal privacy and confidentiality remained. Overall, MORS were perceived as a useful adjunct service to address the unmet needs PWUS during the pandemic and beyond.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
North America continues to contend with unprecedented rise in fatal drug overdoses, primarily involving the synthetic opioid analogue fentanyl [1, 2]. In 2016, British Columbia became the first jurisdiction in Canada to declare drug-related overdoses and deaths as a public health emergency [3]. Other regions across the country have also begun to see similar trends in increasing opioid toxicity deaths [1], leading to more demand and provision of overdose prevention and harm reduction services, including supervised consumption services (SCS), overdose prevention sites (OPS), take-home naloxone kits, safer supply, and more [4,5,6,7].
Amid the overdose crisis, the COVID-19 pandemic brought additional challenges to the healthcare system and social services that were available to people who use substances (PWUS) [8,9,10,11]. Many harm reduction and outreach programs faced reductions in operating hours, capacity, staffing, or outright closure [9,10,11] in order to accommodate public health and social distancing measures, driving many to use substances alone [9, 10, 12]. These measures ran contrary to the public health messaging in which PWUS were directed to “never use alone” [12,13,14].
Even with resumed operations of SCS and other harm reduction programs post-pandemic, high rates of mortality and morbidity associated with illicit substance use still remained a prevalent issue [1, 15]. This has been attributed to the increasing toxicity of unregulated synthetic opioids, the presence of adulterants in the drug supply such as xylazine and benzodiazepines, and poly-substance use involving stimulants [1, 16]. In light of this, more comprehensive overdose prevention tools are needed to accommodate a growing demographic of people who may not be able to reach SCS/OPS.
Spotting is a grassroots alternative harm reduction method that allow PWUS to consume substances under the virtual supervision of others (e.g., phone calls) [17]. One of the advantages of spotting is that it offers autonomy in overdose response planning since PWUS often rely on friends or their loved ones to monitor them during use (for instance, such a plan may not need to involve emergency services) [17]. Previous literature has examined the benefits and limitations of informal spotting among PWUS; however, we are unaware of studies that have qualitatively examined formal virtual interventions in the context of isolation, the pandemic, and public health measures.
Mobile Overdose Response Services (MORS) are formalized overdose prevention technologies designed to support those who do not have access to SCS/OPS or alternative spotting methods. Several types of MORS are currently available in Canada [9]. One is the National Overdose Response Service [18], a nationwide hotline service that people can dial from any province or territory. Another example is the Brave app [19], a mobile application with hotline features. Both services allow PWUS to connect with a peer operator (often with lived experience of substance use) who can supervise their consumption and initiate an emergency response in the event of an overdose. In the United States, Never Use Alone provides a similar peer-led service [20]. In addition, British Columbia and Alberta have developed their own timer-based mobile applications: Connect by Lifeguard [21] and the Digital Overdose Response System [22], respectively. While these services do not connect users to a peer operator, they can dispatch an emergency response if the client is unable to shut off or reset the application timer.
With increasing reliance on telemedicine and virtual facilitation of patient-provider communication in healthcare settings, it is important to understand the value of these formal spotting technologies from the perspectives of PWUS and other key interest groups. The aim of this study was to qualitatively examine the role of MORS during the COVID-19 pandemic to better inform the provision of these virtual services going forward in future public health emergencies.
Methods
Participant Recruitment and Sampling
This qualitative study was designed to examine the ways in which MORS could fill the gaps in harm reduction services and other supports for PWUS during public health emergencies, specifically the COVID-19 pandemic. The interviewees consisted of PWUS, healthcare providers, harm reduction workers, MORS operators, and the general public. This Canada-wide study was open to individuals who met the following inclusion criteria: (1) 18 years of age or older; (2) able to communicate in English; (3) able to provide informed consent; and (4) have access to a mobile device. Participants were recruited through snowball, purposive, and convenience sampling using pre-existing networks known to the research team. All participants were notified that the information that they share during the interviews would remain confidential and anonymous. A verbal informed consent was obtained before proceeding with the interview. Supplementary mental health and addiction support were available if participants became distressed, although no one accessed them.
Semi-structured Interviews
The interview guide was created in collaboration with MORS operators, PWUS, and the research team based on questions from government and health officials on how best to support PWUS during the pandemic. The interviews were conducted by two evaluators (SJ and LA) from a third-party research organization specializing in qualitative research between November 2021 and April 2022. The evaluators and the participants had no previously established relationship with each other and were the only individuals present during the call. The telephone interviews ranged from 20 to 60 min and were recorded using TapeACall. Honorariums were provided only to PWUS in the amount of $50.00 CAD.
Coding and Thematic Analysis
Inductive thematic analysis was performed to identify the prevalent themes that reflected the perceptions of participants toward MORS and their relevance during the COVID-19 pandemic. Coding was completed using Dedoose software. The first three transcripts were collectively inspected by the two evaluators to ensure alignment between the identified themes. After this step, each evaluator independently coded half of the transcripts using a jointly created codebook. The finished transcripts were continuously reviewed by their counterpart throughout this process. Any discrepancies in coding were discussed between the evaluators and the principal investigator (MG) to arrive at a consensus. Once the initial coding was complete, a representative sample of relevant quotations for each theme was reviewed with the consulting project manager (KM). Member checking was conducted by sharing a paper format of the key themes with the participants.
The work was supported through funds from a Health Canada grant whose mandate was to look at the effects of the pandemic on harm reduction resources. We used the Consolidated Criteria for Reporting Qualitative Research (COREQ) checklist to report the results. The study complies with the Tri-Council Policy Statement for Ethical Conduct for Research Involving Humans (TCPS 2) and the Helsinki Declaration [23]. It was approved by the University of Calgary Conjoint Health Research Ethics Board (REB21-1655).
Results
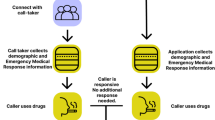
A total of 59 semi-structured interviews consisted of 25 PWUS, 10 healthcare providers, 6 harm reduction workers, 6 MORS operators, and 12 members of the public. The following key themes pertaining to the use of MORS during COVID-19 were identified: (1) reduced availability of SCS and other harm reduction services, (2) opportunity to bridge the gap in mental health services for PWUS, (3) overall acceptability and attitude towards MORS, and (4) concerns pertaining to privacy and confidentiality. A summary of the findings can also be found in Fig. 1.
-
Theme 1: MORS can help mitigate the reduced capacity of traditional harm reduction services during public health emergencies.
Indeed, the COVID-19 pandemic brought unforeseen changes to public health priorities, potentially neglecting the needs of PWUS. Participants noted how the social distancing measures brought a sudden halt to the already scarce harm reduction resources and that the public health focus did not consider the needs of vulnerable populations. This was thought to further marginalize PWUS, harm reduction advocates, and front-line addiction workers.
I think COVID had kind of caused this issue to take a backseat. Where I feel like three years ago we were really starting to get into it. And it was really starting to kind of like go towards the right direction. And then suddenly it’s like oh pandemic, let’s focus on that. Where this problem isn’t going away. Mental health is at its all-time worst. Substance abuse is at its all-time worst. People’s necessity to escape the world around them is probably at an all-time high. (General Public).
While pandemic-related public health measures (e.g., gathering restrictions) were deemed necessary to curb the transmission of COVID-19, this posed additional risks for PWUS who were more likely to consume substances alone during this time. In addition, many PWUS expressed frustrations towards the reduced capacity of SCS, resulting in individuals waiting longer in line than usual. Some also felt apprehensive about contracting the virus, which convinced them to use alone in their home or private residence. Both PWUS and MORS operators felt that the use of MORS was preferable to using substances alone and could be used to minimize the risk of overdose associated with solitary use.
People didn’t want to go out and so it would be, in their mind perhaps, safer to use the app or make the phone call instead of having to go out of their homes and go to an actual site, or use with their buddies. You know that maybe they didn’t want to use it with their buddies because of the fear of COVID. (PWUS).
The Safe Consumption site I was going to, they did cut back the amount of number of people – of people you can go in there to use…So, I ended up going there and waiting for three hours – two, three hours – to get in to use. And most of the time, I’d just end up being like, “F** it,” and going to use on the street or going home…I definitely used to go in person way more to use before COVID, because they had more availability for people to go in there, so. (PWUS).
Yes, for sure. I mean, I think, you know, more so over the last sort of year-ish, when places like Toronto were literally locked down, like, you couldn’t leave. Well, how are you supposed to get out and go to a safe injection site? Or how are you supposed to go out and go to meeting if you’re feeling like you're struggling, and you don’t want to use? You know, all those things were taken away from us. So, COVID has had, I think, a huge impact on people who didn’t have those extra resources available. (MORS Operator).
With COVID-19 […] a lot of people are sitting in their own homes, a lot of people are not accessing supervised consumption service for various reasons […] there was a reduction in capacity […] a lot of booths were shut down, every other booth was open, which led to long lineups. A lot of people were worried about going into these sites, because they were afraid of being exposed to COVID […] So many of them were using alone at home, or not interacting or engaging with other individuals, which they should be doing in order to keep themselves alive. (MORS Operator).
The utility of MORS may have improved during the pandemic by providing a virtual spotting service, removing the struggle to locate a physical site. In addition, some respondents perceived MORS an effective adjunct harm reduction service that can mitigate for the reduced operating capacity and closures of SCS/OPS.
With COVID everybody being in lockdown and that there’s – and you know in your own little cohorts. It’s been tough, and of course and we know that use has gone up. And I would hope that people have accessed it a whole lot more. Just knowing that, that is available to them and it is a safety measure for them. (PWUS).
With all the restrictions that come along with COVID […] like at our site we’re only allowed 10 people in at a time and so if it’s minus 50 you don’t want to have to wait outside in the cold to consume or waiting to consume while other people inside are consuming, you know? […] COVID has made people very paranoid, in some ways, to be around other people and whatnot. So at least this way, yeah, you’re in the comfort of your own home, you know the whole cleanliness aspect of it, the whole sanitized, you know what’s happening in your house and who’s in your house. So, I definitely think that COVID would contribute to people wanting to just be able to do it virtually. (Community Harm Reduction Worker).
I think they’re [MORS] super important. I think they’re lifesaving. I think especially with COVID that they are more important, now more than ever, especially with people, you know, consuming drugs now at home, rather than out, because there are restrictions. (General Public).
-
Theme 2: MORS may be an innovative strategy to alleviate the sense of isolation and improve mental health supports experienced by PWUS during the pandemic.
During the interview, participants noted the complex interplay between isolation, mental health, and substance use. There were suggestions that MORS could help rekindle social relationships and allay the sense of isolation with services such as the National Overdose Response Service hotline and Brave app, which are facilitated by operators with lived experience of substance use as opposed to the automatic countdown services like Digital Overdose Response System app.
Follow-up support, [with] someone who was non-judgemental […] it’s just nice to hear someone’s voice when you’re worried if you’re going to live or die. (PWUS).
-
Theme 3: The pandemic may have shifted the way virtual harm reduction supports are viewed and accepted.
Many participants stated that the pandemic escalated the overall awareness and acceptability of MORS by normalizing the use of technologies and online services, especially regarding healthcare delivery.
Through COVID it’s kind of enlightened everybody that everything doesn’t have to be in person. Virtual is now somewhat normal for people. So, whereas even three years ago the thought might have seemed a little bit silly, or like there wouldn’t be uptake on it, but now I think everybody is more in tune with virtual services of different sorts. (General Public).
I think COVID has definitely thrown in you know that physical divide. Where you’re probably doing a lot more on your own. And I think a lot more people due to the fact that you know we are in COVID. There are a lot more Zoom activities. A lot more of our world is now virtually based. So, I would say that would probably cause a lot of people to be more comfortable than they used to be with virtual services. (General Public).
Conversely, some participants believed that the pandemic did not necessarily ramp up interest among PWUS in using MORS. One healthcare provider stated, “A lot of vulnerable people, although they are aware of COVID-19, they don’t necessarily let it affect their lives.” Thus, interviewees felt that COVID-19 would not necessarily be a strong determinant in whether PWUS would opt for MORS, especially for those in a state of drug-seeking.
I don’t think that that [COVID] would be a factor [to use MORS] when you’re in a state that you’re drug-seeking. I think COVID is the last concern that you have. (Healthcare Provider).
-
Theme 4: MORS continue to contend with issues surrounding privacy and confidentiality.
Despite the ability of some MORS to offer peer connection during periods of isolation, some individuals preferred to use automated app versions to protect their privacy and identity. When asked if they would be open to using MORS during the pandemic, some already had other reliable systems in place to support them, including access to a spotter in order to mitigate the risk of overdose while using alone.
I don’t think so. […] I got my pastor and I talk to him and I’m kind of a pretty private guy and I don’t like everybody knowing what I do. (PWUS).
Discussion
To our knowledge, this is the first study to examine the perceptions of Canadian key interest groups towards MORS in the context of the COVID-19 pandemic. The federal government and local jurisdictions imposed public health measures that included social distancing, travel restrictions, and closure of non-essential businesses and services [24, 25]. Difficulty accessing harm reduction services during this time have been well-documented [9], along with a sharp spike in overdose deaths that spanned the breadth of demographics [1, 26, 27]. Participants in our study voiced similar issues, citing how the pandemic shifted health focus away from the overdose crisis and left many to feel abandoned without adequate support. In addition, pressure to create more easily transportable substances led to a less reliable drug supply filled with a greater number of adulterants, altering drug tolerance and heightening the risk of fatal overdose [24]. Some interviewees expressed concerns about contracting the virus while waiting in line to use SCS or consuming substances in confined spaces where others were present. The fears surrounding COVID-19 contraction among PWUS are well-warranted, as these groups are more susceptible to adverse health outcomes due to substance use-related immunosuppression and concomitant lung diseases [24, 28]. Due to the remote and virtual modality of MORS, they may be useful adjunctive services that can minimize risks to the physiological health and safety of PWUS, especially those with chronic conditions.
Our study highlighted the various ways in which MORS may support PWUS not only as a life-saving intervention but to mitigate worsened mental health in general. The sense of isolation and loss of community support experienced during COVID-19 may have driven many PWUS to use substances alone [9, 29]. The hotline-based services were perceived to be more beneficial in this regard, whereas automatic app-based services were seen as more limited in their capacity to create connections and reduce isolation. Nonetheless, the authors are aware that many automated app-based services do provide lists of resources that might prove useful. The ability of MORS to offer mental health services during a public health emergency is significant, given the toll of the pandemic on mental health and associated increases in substance use [30, 31].
Reliance on telemedicine grew substantially during the pandemic, with an estimated 24–42% of physician services in Canada being offered virtually at some point [32]. Opioid agonist treatments, safer supply, and mental health services were not exempt to this trend [33]. There was a mixed sentiment among participants regarding whether the pandemic has helped spur the scalability of MORS. For instance, ownership of a mobile device (which is needed to use MORS) may not always be feasible given the prevalence of financial hardships among PWUS [34]. However, for those who do have the technological access, MORS have been deemed a much-needed service to complement physical harm reduction services in dealing with public health measures and increased prevalence of solitary substance use.
Lastly, our findings have shown concerns regarding privacy and confidentiality when using MORS among our participants, some opting for automated countdown apps or tapping into their personal network when consuming substances. The same concerns have also been documented in studies that have explored the barriers to utilizing SCS [35]. Given that PWUS are vulnerable groups that often contend with stigma and scrutiny in public spaces [30, 36, 37], ways to address these concerns should be thoroughly considered in the future provision and improvement of these services.
The general consensus among participants that MORS are a viable strategy to address the overdose crisis while limiting the spread of COVID-19 is encouraging. Even though Canada has lifted COVID-19 measures as of 2022 [38], it is worth noting that the unique benefits of MORS might be applied to other circumstances in which physical and social isolation becomes necessary. That said, the authors believe that MORS should not be a replacement for other harm reduction tools that are more widely studied like the SCS, outreach programs, and needle exchange programs[39,40,41,42]. Rather, they should be regarded as adjunctive services that might be scaled as needed particularly during pandemics and other public health crises in order to minimize morbidity and mortality associated with substance use.
Strength, Limitations, and Future Directions
One strength of this study is the large sample size that engaged the perspectives of various key interest groups. However, the use of snowball sampling through existing networks may have introduced a selection bias. The study also required participants to have access to mobile devices or access to a phone and be familiar with MORS; thus, we may have captured the opinions of a specific demographic of PWUS in Canada. This study also did not address other virtual harm reduction technologies currently on the market including wearable devices, bathroom sensors, and overdose buttons. A future nationwide study with a large sample size (particularly PWUS) and the inclusion of more interest groups could enhance the usefulness and generalizability of these findings.
Conclusion
The dual crisis of the COVID-19 pandemic and the opioid epidemic has been detrimental to PWUS and the harm reduction community at large. MORS may be useful in mitigating some of these concerns by reducing solitary use and possibly the spread of COVID-19 and other infectious diseases. Future research should consider how hotline-based services may reduce isolation for service users outside of a pandemic environment, particularly for those who may be hiding their substance use from their support systems.
Data Availability
The data that support the findings of this study are available on request from the corresponding author, M.G. The data are not publicly available due to the sensitivity of substance use and interview transcripts containing information that could compromise the privacy of research participants.
References
Health Canada. Opioid- and stimulant-related harms — Canada.ca. Published 2023. Accessed July 19, 2023. https://health-infobase.canada.ca/substance-related-harms/opioids-stimulants/
Ayoo K, Mikhaeil J, Huang A, Wąsowicz M. The opioid crisis in North America: facts and future lessons for Europe. Anaesthesiol Intensive Ther. 2020;52(2):139–47. https://doi.org/10.5114/ait.2020.94756.
BC Gov News. Provincial health officer declares public health emergency | BC Gov News. Published April 14, 2016. Accessed February 5, 2024. https://news.gov.bc.ca/releases/2016HLTH0026-000568
Pauly B, Wallace B, Pagan F, et al. Impact of overdose prevention sites during a public health emergency in Victoria. Canada PLoS One. 2020;15(5):e0229208. https://doi.org/10.1371/journal.pone.0229208.
Health Canada. Supervised consumption explained: types of sites and services. Published May 15, 2018. Accessed July 31, 2023. https://www.canada.ca/en/health-canada/services/substance-use/supervised-consumption-sites/explained.html
Canadian Centre on Substance Use and Addiction. The availability of take-home naloxone in Canada.; 2016. https://www.ccsa.ca/sites/default/files/2019-05/CCSA-CCENDU-Take-Home-Naloxone-Canada-2016-en.pdf. Accessed 12 Sept 2023.
Foreman-Mackey A, Pauly B, Ivsins A, Urbanoski K, Mansoor M, Bardwell G. Moving towards a continuum of safer supply options for people who use drugs: a qualitative study exploring national perspectives on safer supply among professional stakeholders in Canada. Subst Abuse Treat Prev Policy. 2022;17(1):66. https://doi.org/10.1186/s13011-022-00494-y.
Weicker SA, Speed KA, Hyshka E, Mrochuk M, Kosteniuk B, Dong K. Emergency department care for patients who use opioids during the COVID-19 pandemic. Can J Emerg Med. 2022;24(2):123–5. https://doi.org/10.1007/s43678-021-00229-1.
Russell C, Ali F, Nafeh F, Rehm J, LeBlanc S, Elton-Marshall T. Identifying the impacts of the COVID-19 pandemic on service access for people who use drugs (PWUD): a national qualitative study. J Subst Abuse Treat. 2021;129:108374. https://doi.org/10.1016/j.jsat.2021.108374.
Cassie R, Hayashi K, DeBeck K, et al. Difficulty accessing supervised consumption services during the COVID-19 pandemic among people who use drugs in Vancouver, Canada. Harm Reduct J. 2022;19(1):126. https://doi.org/10.1186/s12954-022-00712-7.
Minoyan N, Høj SB, Zolopa C, Vlad D, Bruneau J, Larney S. Self-reported impacts of the COVID-19 pandemic among people who use drugs: a rapid assessment study in Montreal, Canada. Harm Reduct J. 2022;19(1):38. https://doi.org/10.1186/s12954-022-00620-w.
Canadian Centre on Substance Use and Addiction. Impacts of the COVID-19 Pandemic on Substance Use Treatment Capacity in Canada. Published online 2020. https://www.ccsa.ca/impacts-covid-19-pandemic-substance-use-treatment-capacity-canada. Accessed 12 Sept 2023.
Alberta Health Services. Spike in opioid overdose calls prompts public warning. Alberta Health Services. Published 2019. https://www.albertahealthservices.ca/news/Page14902.aspx. Accessed 3 Feb 2024.
Vancouver Coastal Health. Overdose response, Naloxone & training | Vancouver Coastal Health. Accessed February 3, 2024. https://www.vch.ca/en/overdose-response-naloxone-training
Health Canada. Modelling opioid-related deaths during the overdose crisis. Published November 26, 2020. Accessed February 21, 2024. https://www.canada.ca/en/health-canada/services/opioids/data-surveillance-research/modelling.html
Russell C, Law J, Bonn M, Rehm J, Ali F. The increase in benzodiazepine-laced drugs and related risks in Canada: the urgent need for effective and sustainable solutions. Int J Drug Policy. 2023;111:103933. https://doi.org/10.1016/j.drugpo.2022.103933.
Perri M, Kaminski N, Bonn M, et al. A qualitative study on overdose response in the era of COVID-19 and beyond: how to spot someone so they never have to use alone. Harm Reduct J. 2021;18(1):85. https://doi.org/10.1186/s12954-021-00530-3.
NORS. National Overdose Response Service. NORS. https://www.nors.ca/about. Accessed 10 Jan 2024.
Brave. Brave Coop. https://brave.coop/. Accessed 17 Jan 2024.
Never Use Alone. Never Use Alone – No Judgment, No Shaming, No Preaching, Just LOVE! https://neverusealone.com/. Accessed 13 Dec 2023.
Lifeguard Digital Health Inc. Lifeguard Digital Health. https://lifeguarddh.com/. Accessed 17 Jan 2024.
Digital Overdose Response System. DORS. https://www.dorsapp.ca. Accessed 17 Jan 2024.
World Medical Association. World Medical Association Declaration of Helsinki: ethical principles for medical research involving human subjects. JAMA. 2013;310(20):2191. https://doi.org/10.1001/jama.2013.281053.
Ali F, Russell C, Nafeh F, Rehm J, LeBlanc S, Elton-Marshall T. Changes in substance supply and use characteristics among people who use drugs (PWUD) during the COVID-19 global pandemic: a national qualitative assessment in Canada. Int J Drug Policy. 2021;93:103237. https://doi.org/10.1016/j.drugpo.2021.103237.
Urrutia D, Manetti E, Williamson M, Lequy E. Overview of Canada’s answer to the COVID-19 pandemic’s first wave (January–April 2020). Int J Environ Res Public Health. 2021;18(13):7131. https://doi.org/10.3390/ijerph18137131.
Ghose R, Forati AM, Mantsch JR. Impact of the COVID-19 pandemic on opioid overdose deaths: a spatiotemporal analysis. J Urban Health. 2022;99(2):316–27. https://doi.org/10.1007/s11524-022-00610-0.
Butler A, Croxford R, McLeod KE, et al. The impact of COVID-19 on opioid toxicity deaths for people who experience incarceration compared to the general population in Ontario: a whole population data linkage study. PLoS One. 2023;18(10):e0293251. https://doi.org/10.1371/journal.pone.0293251.
Cowan E, Khan MR, Shastry S, Edelman EJ. Conceptualizing the effects of the COVID-19 pandemic on people with opioid use disorder: an application of the social ecological model. Addict Sci Clin Pract. 2021;16(1):4. https://doi.org/10.1186/s13722-020-00210-w.
Schneider KE, Allen ST, Rouhani S, et al. Increased solitary drug use during COVID-19: an unintended consequence of social distancing. Int J Drug Policy. 2023;111:103923. https://doi.org/10.1016/j.drugpo.2022.103923.
Mental Health Commission of Canada. Mental health and substance use during COVID-19: spotlight on youth, older adults & stigma. Mental Health Commission of Canada. Published August 10, 2023. Accessed August 10, 2023. https://mentalhealthcommission.ca/resource/poll-covid-19-youth-older-adults-stigma/
Shankar R, Bhattacharya V. Trends in substance use and abuse during COVID-19 among the general population. Addict Health. 2022;14(4):296–308. https://doi.org/10.34172/ahj.2022.1274.
Husak L, Sovran V, Ytsma A, Comeau M. Impact of the COVID-19 pandemic on virtual care: a major shift for physicians and patients. Healthc Q. 2022;25(3):11–3. https://doi.org/10.12927/hcq.2022.26948.
Perri M, Guta A, Gagnon M, et al. Developing a digital health strategy for people who use drugs: lessons from COVID-19. Digit Health. 2021;7:205520762110284. https://doi.org/10.1177/20552076211028404.
Tsang VWL, Papamihali K, Crabtree A, Buxton JA. Acceptability of technological solutions for overdose monitoring: perspectives of people who use drugs. Subst Abuse. 2021;42(3):284–93. https://doi.org/10.1080/08897077.2019.1680479.
Bardwell G, Strike C, Mitra S, et al. “That’s a double-edged sword”: exploring the integration of supervised consumption services within community health centres in Toronto. Canada Health Place. 2020;61:102245. https://doi.org/10.1016/j.healthplace.2019.102245.
Muncan B, Walters SM, Ezell J, Ompad DC. “They look at us like junkies”: influences of drug use stigma on the healthcare engagement of people who inject drugs in New York City. Harm Reduct J. 2020;17(1):53. https://doi.org/10.1186/s12954-020-00399-8.
Bowles JM, Kolla G, Smith LR, Scheim A, Dodd Z, Werb D. Disease-related stigma among people who inject drugs in Toronto amidst the COVID-19 pandemic. Drug Alcohol Depend Rep. 2023;7:100167. https://doi.org/10.1016/j.dadr.2023.100167.
Public Health Agency of Canada. Government of Canada to remove COVID-19 border and travel measures effective October 1. Published September 25, 2022. Accessed August 21, 2023. https://www.canada.ca/en/public-health/news/2022/09/government-of-canada-to-remove-covid-19-border-and-travel-measures-effective-october-1.html
Marshall BD, Milloy MJ, Wood E, Montaner JS, Kerr T. Reduction in overdose mortality after the opening of North America’s first medically supervised safer injecting facility: a retrospective population-based study. The Lancet. 2011;377(9775):1429–37. https://doi.org/10.1016/S0140-6736(10)62353-7.
Fernandes RM, Cary M, Duarte G, et al. Effectiveness of needle and syringe programmes in people who inject drugs – An overview of systematic reviews. BMC Public Health. 2017;17(1):309. https://doi.org/10.1186/s12889-017-4210-2.
Rammohan I, Gaines T, Scheim A, Bayoumi A, Werb D. Overdose mortality incidence and supervised consumption services in Toronto, Canada: an ecological study and spatial analysis. Lancet Public Health. 2024;9(2):e79–87. https://doi.org/10.1016/S2468-2667(23)00300-6.
Strike C, Miskovic M. Scoping out the literature on mobile needle and syringe programs—review of service delivery and client characteristics, operation, utilization, referrals, and impact. Harm Reduct J. 2018;15(1):6. https://doi.org/10.1186/s12954-018-0212-3.
Acknowledgements
The authors would like to acknowledge the contributions of Health Canada’s Substance Use and Addictions Program (SUAP) and the Canadian Institutes of Health Research (CIHR) for helping fund this project. We would also like to thank the National Overdose Response Service (NORS) and Grenfell Ministries for helping recruit participants. We also appreciate the work of Three Hive Consulting in conducting interviews and aiding with analysis. Health Canada’s Substance Use and Addictions Program (SUAP) Grant [Agreement Number 2122-HQ-000021] and the Canadian Institutes of Health Research (CIHR) Grant [Funding Reference Number (FRN) 181006] supported this work (M.G). The study design, data collection and analysis, interpretation of results, or the decision to submit for publication was done independently of SUAP and CIHR. Health Canada’s views are not necessarily represented by the views expressed in this article.
Author information
Authors and Affiliations
Contributions
B.S. and M.G. both contributed equally to the interpretation and writing of the main manuscript text. All authors provided data interpretation, revision, and feedback. S.J. was involved in the data collection and interpretation of results. M.G. conceptualized the study and acquired funding. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Ethics Approval and Consent to Participate
The study was conducted as part of a quality improvement project and received ethical approval from the University of Calgary Conjoint Health Research Ethics Board (REB21-1655).
Consent for Publication
Not applicable.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Seo, B., Rioux, W., Rider, N. et al. Bridging the Gap in Harm Reduction Using Mobile Overdose Response Services (MORS) in the Context of the COVID-19 Pandemic: A Qualitative Study. J Urban Health 101, 252–261 (2024). https://doi.org/10.1007/s11524-024-00846-y
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11524-024-00846-y