Abstract
Topping-off technique has been proposed to prevent adjacent-segment degeneration/disease following spine fusion surgery. Nevertheless, few studies have investigated biomechanics of the fusion surgery with topping-off device under whole-body vibration (WBV). This biomechanical study aimed to investigate the vibration characteristics of human lumbar spine after topping-off surgery, and also to evaluate the effect of bony fusion on spine biomechanics. Based on a healthy finite-element model of lumbosacral spine (L1–sacrum), the models of topping-off surgery before and after bony fusion were developed. The simulated surgical procedures consisted of interbody fusion with rigid stabilizer at L4–L5 segment (rigid fusion) and dynamic stabilizer at degenerated L3–L4 segment. An interspinous implant, Device for Intervertebral Assisted Motion (DIAM, Medtronic Inc., Minnesota, USA), was used as the dynamic stabilizer. The stress responses of spine segments and implants under a vertical cyclic load were calculated and analyzed. The results showed that compared with rigid fusion alone, the topping-off technique significantly decreased disc stress at transition segment (L3–L4) as expected, and resulted in a slight increase in disc stress at its supra-adjacent segment (L2–L3). It indicated that the topping-off stabilization using DIAM might provide a good tradeoff between protection of transition segment and deterioration of its supra-adjacent segment during WBV. Also, it was found that bony fusion decreased stress in L4 inferior endplate and rigid stabilizer but had nearly no effect on stress in DIAM and L3–L4 disc, which was helpful to determine the biomechanical differences before and after bony fusion.
Graphical abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
1 Introduction
Adjacent-segment degeneration/disease (ASD) is a major concern after spine fusion surgery [1]. According to a meta-analysis study [2], the occurrence of radiograph ASD and symptoms ASD was 26.6% and 8.5%, respectively, in lumbar position after the surgery. It implied that the fusion surgery was associated with significant risk of ASD. Although the exact mechanism remains uncertain, biomechanical changes after spine fusion surgery likely played a primary role in developing ASD [3]. Numerous studies, both experimental and numerical [4,5,6,7], suggested that the stress (e.g., disc stress and intradiscal pressure), facet loading, and mobility at adjacent segments of the fusion one were increased. Many researchers believed that the rigid fixation system, commonly used to stabilize the spine after fusion surgeries, increased stiffness of the fixed segment much more than desired and contributed to the abnormal forces and hypermobility at its adjacent segments, thus resulting in the development of ASD [8, 9].
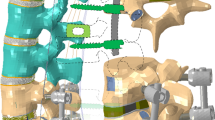
Based on the aforementioned biomechanical evidences for ASD, a new posterior stabilization method named topping-off technique, in terms of hybrid use of the rigid and dynamic stabilizers, was proposed to prevent hypermobility and overstress at the segment adjacent to the fusion level and thus reduce the risk of ASD [10]. In the application of topping-off technique, the fusion segment was immobilized by a rigid stabilizer, and the segment above the fusion level (i.e., transition segment) was further protected by a dynamic stabilizer, as illustrated in Fig. 1. The dynamic stabilizer used in topping-off surgery was either a pedicle-based stabilization device (e.g., Dynesys, NFlex, Cosmic) or an interspinous process device (e.g., Coflex, Wallis, DIAM) [11, 12], which had less rigid and could provide the segment with flexibility [13, 14].
To evaluate the biomechanical effect of topping-off technique on spine segments, several experimental and finite-element studies have been conducted in recent years. For example, an in vitro experimental study of Kong et al. [15] demonstrated that L5–S1 lumbar fusion with topping-off device using Coflex in L4–L5 was able to restrict range of motion (ROM) for flexion/extension at the transition segment (L4–L5) compared with rigid fusion alone and had no significant effect on ROM at its supra-adjacent segment (L3–L4). A finite-element study of Lee et al. [16] reported that compared with L4–L5 rigid fusion alone, the topping-off technique using NFlex or DIAM in L3–L4 decreased intradiscal pressure at the transition segment (L3–L4) under flexion, extension, lateral bending, and axial rotational moments, but increased the stress at its supra-adjacent segment (L2–L3) in all loading directions except under extension. However, most of these existing biomechanical studies were performed under a static loading condition such as bending and torsion moments, and very few dealt with the condition of whole-body vibration (WBV).
WBV is a situation where human body vibrates due to external vibration excitation and is typically present in vehicles [17]. It was demonstrated in previous studies that the cyclic loading encountered due to WBV exposure could generate higher stress responses in spinal tissues than the static loading with equivalent magnitudes [18, 19]. At present, WBV has been considered a significant risk factor for degenerative lumbar spinal disorders and low back pain [20, 21]. Considering the fact that the patients undergoing lumbar spine surgery may also be exposed to WBV in their daily life and work (e.g., driving a car or riding on a bus), recent years have seen increasing interests and demands in analyzing biomechanical responses of the postsurgical spine to WBV [17, 22, 23]. Accordingly, the goal of this study was to investigate the biomechanics of human lumbar spine (L1–sacrum) after the topping-off surgery under WBV by means of finite-element analysis. In clinical practice, topping-off technique is often used following single-level posterior or transforaminal lumbar interbody fusion (PLIF or TLIF) when ASD has already occurred [12, 24, 25], so the PLIF and TLIF at L4–L5 with a moderately degenerated disc at L3–L4 were considered in this study. In addition, the differences in vibration responses of the implanted spine between early and late postoperative stages (before and after bony fusion) still remained unclear. Therefore, we also evaluated the effect of bony fusion on biomechanics of the implanted spine under WBV.
2 Materials and methods
2.1 Finite-element simulation of surgical procedures and implants
The healthy finite-element model of human lumbosacral spine, developed and validated previously [26], was employed in this study (Fig. 2A). Geometry of the model was reconstructed from computed tomography (CT) scans of a healthy volunteer. The model includes vertebral bodies, posterior bony elements, intervertebral discs, and seven ligaments. Each vertebral body consists of a cancellous inner core surrounded by a cortical shell (including endplate). Each intervertebral disc consists of a nucleus pulposus surrounded by an annulus ground substance comprising fiber layers. Material properties assigned to the spinal components are shown in Table 1.
Using the aforementioned healthy model as a baseline, L4–L5 rigid fusion with a moderately degenerated L3–L4 intervertebral disc was initially simulated. Two interbody fusion approaches, PLIF and TLIF, were considered in this study. To simulate the PLIF surgical procedure, partial laminectomy and medial facetectomy were performed at L4–L5 segment with removal of the entire nucleus, posterior portion of the annulus, supraspinous ligament, interspinous ligament, and ligamentum flavum, and two PLIF cages were inserted into L4–L5 intervertebral space (Fig. 2B). To simulate the TLIF surgical procedure, the left facet joint, entire nucleus, and posterior-left portion of the annulus at L4–L5 segment were removed, and a TLIF cage was inserted into L4–L5 intervertebral space (Fig. 2C). The sizes of PLIF and TLIF cages are 25 mm depth × 9 mm width × 12 mm height (surface area: 330 mm2 for 2 PLIF cage) and 10 mm depth × 30 mm width × 12 mm height (surface area: 185 mm2), respectively [27], and all the cages were filled with cancellous bone to simulate the embedded bone graft. For the PLIF and TLIF models, the L4–L5 fusion segment underwent a conventional rigid stabilizer instrumentation using bilateral pedicle screws and titanium rods. Also, a moderate disc degeneration at L3–L4 segment for these two rigid fusion models was simulated by changing the disc height and material property of the nucleus, which has been described in detail in our previous work [28]. Specifically, the height of healthy L3–L4 disc was decreased (about by 33%), and the material values (Young’s modulus) of healthy L3–L4 nucleus were increased (from C10 = 0.12, C01 = 0.03 to C10 = 0.17, C01 = 0.041, as shown in Table 1).
Subsequently, based on these developed rigid fusion models (Fig. 2B and C), an interspinous implant, Device for Intervertebral Assisted Motion (DIAM, Medtronic Inc., Minnesota, USA), consisting of a “H”-shape silicone core with a polyester cover [29], was further inserted between spinous process of L3 and L4, where the interspinous ligament was removed for DIAM insertion, to construct the topping-off model (Fig. 3). To prevent instability and secure the prosthesis, DIAM and spinous processes were connected by the tightening ligatures that were modeled using tension-only spring elements [16, 30]. Assigned material properties to the implants in the finite-element models are also shown in Table 1.
2.2 Contact definitions and boundary conditions
The interfaces between the graft and endplate, as well as the cage and endplate were defined as surface-to-surface contact to simulate early postoperative stage after cage placement (before bony fusion). A friction coefficient of 0.3 was assigned to the graft-endplate interface to mimic a more physiologic situation [31], where the surfaces of bone graft were not fused to the endplates. A higher friction coefficient of 0.8 was assigned to the cage-endplate interface because the cage has serrations on the contact surfaces that are supposed to prevent motion of the cage [32]. The interface between the DIAM and spinous processes was also defined as surface-to-surface contact with a friction coefficient of 0.2 [29]. The interface between the pedicle screw and vertebra was assumed to be completely bonded via node sharing as a result of successful surgery. In addition, to simulate late postoperative stage after cage placement (after bony fusion), the graft-endplate and cage-endplate interfaces were changed to tie constraint.
The developed finite-element models were completely fixed at the caudal part of sacrum and were loaded with a compressive follower pre-load of 400 N. Furthermore, additional sinusoidal vertical force of 40 N at the frequency of 5 Hz was applied to simulate WBV condition. The loading scenario has been used and detailedly described in our previous studies [19, 33]. To consider pre-tension of the ligatures for DIAM, an initial tension force of 120 N was applied for secure tightening [16]. Vibration responses of the models were calculated using transient dynamic analysis. The von Mises stress in spine segments and implants was chosen as the evaluation indices, which were collected and plotted as time-dependent curves. As suggested by the literature [18, 34], the stress was defined as the average of the stresses in the elements used to build the corresponding tissues of the models, and vibration amplitude of the stress was defined as maximum minus minimum values of the obtained dynamic response curve. The commercial finite-element analysis software ABAQUS/Standard (Dassault Systems Simulia Corp., Providence, RI, USA) and pre-processing software ANSA (BETA CAE Systems S.A., Thessaloniki, Greece) were employed in this study.
3 Results
3.1 Biomechanical effect of topping-off technique on transition and its supra-adjacent spine segments
Time-domain dynamic responses of the disc stress at transition segment (L3–L4) and its supra-adjacent segment (L2–L3) are displayed in Fig. 4. The maximum value and vibration amplitude of these response curves were summarized in Fig. 5. Compared with rigid fusion alone, the topping-off technique significantly decreased the stress response at L3–L4 segment as observed from Fig. 4A and B. For example, the maximum stress and vibration amplitude for PLIF with DIAM was 0.198 MPa and 0.071 MPa, respectively, which was 32.9% and 50.7% lower than those (0.295 MPa and 0.144 MPa) for PLIF alone. However, it was observed from Fig. 4C and D that the topping-off technique caused a slight increase in the stress response at L2–L3 segment. For example, the maximum stress and vibration amplitude for PLIF with DIAM were 0.370 MPa and 0.111 MPa, respectively, which was 3.9% and 3.7% higher than those (0.356 MPa and 0.107 MPa) for PLIF alone. From Figs. 4 and 5, it was also found that there was no obvious difference in the disc stress at both L3–L4 and L2–L3 between PLIF and TLIF.
Comparison of A maximum value and B vibration amplitude of the dynamic response curves in terms of disc stress (illustrated in Fig. 4) between the rigid fusion models and the topping-off models using DIAM
3.2 Biomechanical effect of bony fusion on the topping-off models
Time-domain dynamic responses of the stress in L4 inferior endplate, rigid stabilizer, DIAM, and L3–L4 disc before and after bony fusion for the topping-off models are displayed in Fig. 6. The maximum value and vibration amplitude of these response curves are listed in Table 2. As demonstrated, the bony fusion significantly decreased the stress responses of endplate and rigid stabilizer (Fig. 6A and B). For example, the maximum stress in L4 inferior endplate and rigid stabilizer for PLIF with DIAM after bony fusion was 0.73 MPa and 5.2 MPa, respectively, which was 54.9% and 59.4% lower than those (1.62 MPa and 12.8 MPa) before bony fusion, and the corresponding vibration amplitude after bony fusion was 0.19 MPa and 1.5 MPa, respectively, which was 9.5% and 16.7% lower than those (0.21 MPa and 1.8 MPa) before bony fusion. However, the bony fusion had nearly no effect on stress responses of DIAM and L3–L4 disc (Fig. 6C and D). To demonstrate the differences in the stress distribution before and after bony fusion, contour plots of the stress in L4 inferior endplate and rigid stabilizer are presented in Fig. 7, which depicts high stress concentration before bony fusion, whereas low stress concentration was observed after bony fusion. In addition, from Figs. 6 and 7 and Table 2, it was also found that the PLIF led to lower stress in L4 inferior endplate and rigid stabilizer than TLIF.
4 Discussion
In our previous studies, biomechanical responses of lumbar spine after single-level interbody fusion surgery supplemented with a conventional single-level rigid stabilizer to WBV had been investigated [23]. Furthermore, in the present study, a biomechanical comparison between the conventional rigid stabilization and the topping-off stabilization was conducted under WBV. It was found that vibration characteristics of the investigated spine segments were different between the rigid fusion and topping-off models (Figs. 4 and 5). As expected, dynamic response of the disc stress at transition segment (L3–L4) was significantly lower in the topping-off model than that in the rigid fusion model (Figs. 4A and B and 5), implying that the dynamic stabilizer (DIAM) helped to absorb much of the vibration energy. This is because the DIAM device suppressed mechanical compensation from fusion segment (L4–L5) to transition segment. The present predicted results showed a consistent trend with previous studies conducted under static loading (bending and torsion moments) [34, 35], indicating that the dynamic stabilizer used in topping-off stabilization can show loading-sharing ability at transition segment regardless of loading condition. In contrast, dynamic response of the disc stress at supra-adjacent segment (L2–L3) was slightly higher when using the topping-off technique (Figs. 4C and D and 5). This is because the increased stiffness due to DIAM instrumentation at transition segment induced mechanical compensation to its supra-adjacent segment. Previous studies reported that the protection of transition segment and the deterioration of its supra-adjacent segment was a tradeoff problem for the topping-off technique [34, 36, 37]. Overall, the present results, in terms of significantly decreased stress at transition segment and slightly increased stress at its supra-adjacent segment, indicated that the topping-off stabilization using DIAM might provide a good tradeoff between the protection and deterioration under vibration loading. Also, the present study provided a biomechanical evidence for the effectiveness of topping-off technique in preventing ASD after the fusion surgery [10, 12].
By reviewing the published finite-element simulation studies concerning lumbar interbody fusion, the current authors found that according to whether or not the graft was fused to the endplate, either a surface-to-surface contact [31, 32, 38] or a tie constraint [7, 9, 16] was defined between the surfaces of graft and endplate to simulate early or late postoperative stage. However, few studies explored the biomechanical differences between these two definitions. Also, only the tie constraint was considered in our previous finite-element studies associated with WBV [23]. Therefore, in the present study we tried to compare the definition of tie constraint with the definition of surface-to-surface contact. In other words, the difference in biomechanics of the implanted spine before and after bony fusion was investigated. It was found that the bony fusion decreased dynamic responses of the stress in L4 inferior endplate and rigid stabilizer (Fig. 6A and B and Table 2), implying that the bony fusion is helpful in reducing the risk of bone failure and breakage for the rigid stabilizer. Moreover, a more uniform stress distribution in the endplate was observed after the bony fusion (Fig. 7). This might be attributed to the difference in load afforded by the graft before and after bony fusion. When the graft was not fused to the endplate, it could transmit compression force only, but after fusion, the graft could help to control the distraction and rotation forces. Because compressive stiffness of this fused level was not affected, dynamic responses of the stress in DIAM and L3–L4 disc at the transition segment was nearly unchanged (Fig. 6C and D and Table 2). In addition, recent in vitro experimental studies reported that the lumbar interbody fusion procedures using cage designs with larger footprint size had higher subsidence resistance [27, 39]. The results presented in Figs. 6A and 7A and Table 2 also showed that the endplate stress in cage-endplate interface for PLIF (having a larger cage footprint) was lower than that for TLIF. It implies that the PLIF might face lower risk of cage subsidence than TLIF, which was consistent with the abovementioned experimental results. Due to the fact that larger footprint interbody devices allow for higher loading sharing through anterior column and thus decrease the loading sharing through posterior fixation system [38], the PLIF led to lower stress in rigid stabilizer than TLIF (Figs. 6B and 7B and Table 2).
There were some limitations and potential future direction for the present study. Finite-element model geometry was obtained from a unique specimen, so the computed absolute values might be unrepresentative of an average person. Nevertheless, the tendency of the predicted results was not affected because all the investigated models were constructed based on the same intact model. Like many other finite-element studies, the present models also did not include the degenerative changes caused by osteophytes, endplate sclerosis, and annular tears due to limitation of data source. In addition, the topping-off technique using pedicle-based dynamic stabilization device was not investigated here, which might present different biomechanical behavior compared with the present interspinous process device, and we will try to reveal their biomechanical differences in the following study. Also, the effect of WBV and these different posterior stabilization devices on biomechanical responses of lumbar paraspinal muscles of the patients undergoing the fusion surgery will be investigated using an in vivo experimental method in the future work.
5 Conclusion
The present study attempted to quantitatively evaluate the effect of topping-off stabilization and bony fusion on biomechanics of the implanted lumbar spine exposed to vertical WBV by means of finite-element analysis. In conclusion, under the vibration loading, the topping-off technique using DIAM device provided a good tradeoff between protection of transition segment (L3–L4) and deterioration of supra-adjacent segment (L2–L3). The bony fusion altered vibration characteristics of the fusion segment (L4–L5), at which the dynamic responses of stress in endplate and rigid stabilizer were significantly decreased. However, the bony fusion had little effect on the stress response of DIAM and L3–L4 disc at the transition level. These findings may be helpful in understanding biomechanics of the topping-off stabilization and determining biomechanical differences of the implanted lumbar spine before and after bony fusion during WBV, and thus may provide a reference regarding lumbar vibration protection of the patients undergoing the surgical instrumentation for clinical studies.
References
Hashimoto K, Aizawa T, Kanno H, Itoi E (2019) Adjacent segment degeneration after fusion spinal surgery-a systematic review. Int Orthop 39(8):1459–1464
Xia XP, Chen HL, Cheng HB (2013) Prevalence of adjacent segment degeneration after spine surgery: a systematic review and meta-analysis. Spine 38(7):597–608
Park P, Garton HJ, Gala VC, Hoff JT, McGillicuddy JE (2004) Adjacent segment disease after lumbar or lumbosacral fusion: review of the literature. Spine 29(17):1938–1944
Akamaru T, Kawahara N, Tim Yoon S, Minamide A, Su Kim K, Tomita K et al (2003) Adjacent segment motion after a simulated lumbar fusion in different sagittal alignments: a biomechanical analysis. Spine 28(14):1560–1566
Ma JX, Jia HB, Ma XL, Xu WG, Yu JT, Feng R et al (2014) Evaluation of the stress distribution change at the adjacent facet joints after lumbar fusion surgery: a biomechanical study. Proc Inst Mech Eng H 228(7):665–673
Zhu ZQ, Liu CJ, Wang KF, Zhou J, Wang JF, Zhu Y et al (2015) Topping-off technique prevents aggravation of degeneration of adjacent segment fusion revealed by retrospective and finite element biomechanical analysis. J Orthop Surg Res 10:10
Cao LL, Liu YM, Mei W, Xu JG, Zhan S (2020) Biomechanical changes of degenerated adjacent segment and intact lumbar spine after lumbosacral topping-off surgery: a three-dimensional finite element analysis. BMC Musculoskelet Disord 21(1):104
Cabello J, Cavanilles-Walker JM, Iborra M, Ubierna MT, Covaro A, Roca J (2013) The protective role of dynamic stabilization on the adjacent disc to a rigid instrumented level. An in vitro biomechanical analysis. Arch Orthop Trauma Surg 133(4):443–448
Chen CS, Shih SL (2018) Biomechanical analysis of a new lumbar interspinous device with optimized topology. Med Biol Eng Comput 56(8):1333–1341
Chou PH, Lin HH, An HS, Liu KY, Su WR, Lin CL (2017) Could the topping-off technique be the preventive strategy against adjacent segment disease after pedicle screw-based fusion in lumbar degenerative diseases? A systematic review. Biomed Res Int 2017:4385620
Fan YP, Zhou SB, Xie T, Yu ZF, Han X, Zhu LL (2019) Topping-off surgery vs posterior lumbar interbody fusion for degenerative lumbar disease: a finite element analysis. J Orthop Surg Res 14(1):476
Wang W, Sun XY, Zhang TT, Sun SY, Kong C, Lu SB (2020) Topping-off technology versus posterior lumbar interbody fusion in the treatment of lumbar disc herniation: a meta-analysis. Biomed Res Int 2020:2953128
Wilke HJ, Drumm J, Häussler K, Mack C, Steudel WI, Kettler A (2008) Biomechanical effect of different lumbar interspinous implants on flexibility and intradiscal pressure. Eur Spine J 17(8):1049–1056
Lin HM, Liu CL, Pan YN, Huang CH, Shih SL, Wei SH et al (2014) Biomechanical analysis and design of a dynamic spinal fixator using topology optimization: a finite element analysis. Med Biol Eng Comput 52(5):499–508
Kong C, Lu SB, Hai Y (2015) Zang L Biomechanical effect of interspinous dynamic stabilization adjacent to single-level fusion on range of motion of the transition segment and the adjacent segment. Clin Biomech 30(4):355–359
Lee CH, Kim YE, Lee HJ, Kim DG, Kim CH (2017) Biomechanical effects of hybrid stabilization on the risk of proximal adjacent-segment degeneration following lumbar spinal fusion using an interspinous device or a pedicle screw-based dynamic fixator. J Neurosurg Spine 27(6):643–649
Xu M, Yang J, Lieberman I, Haddas R (2019) The effect of surgical alignment in adult scoliotic spines on axial cyclic vibration: a finite element study. J Comput Inf Sci Eng 19(2):UNSP 021006
Goel VK, Park H, Kong WZ (1994) Investigation of vibration characteristics of the ligamentous lumbar spine using the finite element approach. J Biomech Eng 116(4):377–383
Guo LX, Fan W (2018) Dynamic response of the lumbar spine to whole-body vibration under a compressive follower preload. Spine 43(3):E143–E153
Bovenzi M, Schust M, Mauro M (2017) An overview of low back pain and occupational exposures to whole-body vibration and mechanical shocks. Med Lav 108(6):419–433
Wade KR, Schollum ML, Robertson PA, Thambyah A, Broom ND (2016) ISSLS Prize Winner: Vibration really does disrupt the disc: a microanatomical investigation. Spine (Phila Pa 1976) 41(15):1185–1198
Rohlmann A, Hinz B, Bluthner R, Graichen F, Bergmann G (2010) Loads on a spinal implant measured in vivo during whole-body vibration. Eur Spine J 19(7):1129–1135
Fan W, Guo LX, Zhao D (2019) Stress analysis of the implants in transforaminal lumbar interbody fusion under static and vibration loadings: a comparison between pedicle screw fixation system with rigid and flexible rods. J Mater Sci Mater Med 30:118
Oikonomidis S, Ashqar G, Kaulhausen T, Herren C, Siewe J, Sobottke R (2018) Clinical experiences with a PEEK-based dynamic instrumentation device in lumbar spinal surgery: 2 years and no more. J Orthop Surg Res 13:196
Bredow J, Lohrer L, Oppermann J, Scheyerer MJ, Sobottke R, Eysel P et al (2017) Pathoanatomic risk factors for instability and adjacent segment disease in lumbar spine: how to use topping off? Biomed Res Int 2017:2964529
Fan W, Guo LX (2017) Influence of different frequencies of axial cyclic loading on time-domain vibration response of the lumbar spine: a finite element study. Comput Biol Med 86:75–81
Palepu V, Helgeson MD, Molyneaux-Francis M, Nagaraja S (2019) The effects of bone microstructure on subsidence risk for ALIF, LLIF, PLIF, and TLIF spine cages. J Biomech Eng 141(3):031002
Guo LX, Fan W (2017) The effect of single-level disc degeneration on dynamic response of the whole lumbar spine to vertical vibration. World Neurosurg 105:510–518
Más Y, Gracia L, Ibarz E, Gabarre S, Peña D, Herrera A (2017) Finite element simulation and clinical follow-up of lumbar spine biomechanics with dynamic fixations. PLoS One 12(11):e0188328
Anasetti F, Galbusera F, Aziz HN, Bellini CM, Addis A, Villa T et al (2010) Spine stability after implantation of an interspinous device: an in vitro and finite element biomechanical study. J Neurosurg Spine 13(5):568–575
Agarwal A, Palepu V, Agarwal AK, Goel VK, Yildirim ED (2013) Biomechanical evaluation of an endplate-conformed polycaprolactone-hydroxyapatite intervertebral fusion graft and its comparison with a typical nonconformed cortical graft. J Biomech Eng 135(6):061005
Guo LX, Yin JY (2019) Finite element analysis and design of an interspinous device using topology optimization. Med Biol Eng Comput 57(1):89–98
Guo LX, Fan W (2019) Impact of material properties of intervertebral disc on dynamic response of the human lumbar spine to vertical vibration: a finite element sensitivity study. Med Biol Eng Comput 57(1):221–229
Chien CY, Kuo YJ, Lin SC, Chuang WH, Luh YP (2014) Kinematic and mechanical comparisons of lumbar hybrid fixation using dynesys and cosmic systems. Spine 39(15):E878–E884
Chuang WH, Lin SC, Chen SH, Wang CW, Tsai WC, Chen YJ et al (2012) Biomechanical effects of disc degeneration and hybrid fixation on the transition and adjacent lumbar segments: trade-off between junctional problem, motion preservation, and load protection. Spine 37(24):E1488–E1497
Mageswaran P, Techy F, Colbrunn RW, Bonner TF, McLain RF (2012) Hybrid dynamic stabilization: a biomechanical assessment of adjacent and supraadjacent levels of the lumbar spine. J Neurosurg Spine 17(3):232–242
Hudson WR, Gee JE, Billys JB, Castellvi AE (2011) Hybrid dynamic stabilization with posterior spinal fusion in the lumbar spine. SAS J 5(2):36–43
Faizan A, Kiapour A, Kiapour AM, Goel VK (2014) Biomechanical analysis of various footprints of transforaminal lumbar interbody fusion devices. J Spinal Disord Tech 27(4):E118–E127
Peck JH, Kavlock KD, Showalter BL, Ferrell BM, Peck DG, Dmitriev AE (2018) Mechanical performance of lumbar intervertebral body fusion devices: an analysis of data submitted to the Food and Drug Administration. J Biomech 78:87–93
Funding
This project is supported by the National Natural Science Foundation of China (Grant No. 52005089, 51875096) and Fundamental Research Funds for the Central Universities (Grant No. N2103010).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare no competing interests.
Additional information
Publisher's note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Fan, W., Guo, LX. Biomechanical investigation of topping-off technique using an interspinous process device following lumbar interbody fusion under vibration loading. Med Biol Eng Comput 59, 2449–2458 (2021). https://doi.org/10.1007/s11517-021-02458-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11517-021-02458-z