Abstract
The association between exposure to ambient particulate matter (PM) and reduced lung function parameters has been reported in many works. However, few studies have been conducted in developing countries with high levels of air pollution like China, and little attention has been paid to the acute effects of short-term exposure to air pollution on lung function. The study design consisted of a panel comprising 86 children from the same school in Nanjing, China. Four measurements of lung function were performed. A mixed-effects regression model with study participant as a random effect was used to investigate the relationship between PM2.5 and lung function. An increase in the current day, 1-day and 2-day moving average PM2.5 concentration was associated with decreases in lung function indicators. The greatest effect of PM2.5 on lung function was detected at 1-day moving average PM2.5 exposure. An increase of 10 μg/m3 in the 1-day moving average PM2.5 concentration was associated with a 23.22 mL decrease (95% CI: 13.19, 33.25) in Forced Vital Capacity (FVC), a 18.93 mL decrease (95% CI: 9.34, 28.52) in 1-s Forced Expiratory Volume (FEV1), a 29.38 mL/s decrease (95% CI: -0.40, 59.15) in Peak Expiratory Flow (PEF), and a 27.21 mL/s decrease (95% CI: 8.38, 46.04) in forced expiratory flow 25–75% (FEF25–75%). The effects of PM2.5 on lung function had significant lag effects. After an air pollution event, the health effects last for several days and we still need to pay attention to health protection.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Air pollution is a major global public health problem, and numerous studies have shown that exposure to air pollution seriously affects the health of the population (Epa 2009). Atmospheric PM is the main component of air pollution, and elevated concentrations of PM are associated with an increased incidence of respiratory symptoms and decreased lung function (Epa 2009; Ward and Ayres 2004). Decreased lung function parameters suggest restrictive ventilatory dysfunction. The association between exposure to ambient PM and reduced lung function parameters has been reported in many studies (D'Amato et al. 2010; Delfino et al. 2004; Gauderman et al. 2015; He et al. 1993; Jacobson et al. 2012; Oftedal et al. 2008; Urman et al. 2014; Yamazaki et al. 2011; Zwozdziak et al. 2016). Children are in the growth and development phase and they are sensitive to air pollution; therefore, the impact of air pollution on children’s health is of great concern (Ginsberg et al. 2005; He et al. 1993; Tzivian 2011). Analysis of the relationship between air pollution and lung function indicators in children can help to improve understanding of the impact of air pollution on the health of children’s respiratory system. These results can be used to improve implementation of protective measures to prevent greater damage to the health of children’s respiratory systems.
The effect of air pollutants on lung function depends on the type of pollutant, duration of exposure, and ambient concentration (D'Amato et al. 2010). However, most studies have been conducted in developed countries with low levels of air pollution. Fewer studies have been conducted in developing countries where there are high levels of air pollution such as China. Most studies have focused on the chronic effects of air pollution on lung function (Gehring et al. 2013; Roy et al. 2012; Spyratos et al. 2014; Wong et al. 2016) and less focused on the acute effects of short-term exposure to air pollution on lung function (Dales et al. 2009; Epton et al. 2008; Zwozdziak et al. 2016). Few studies have analyzed the lag effect of air pollution. Therefore, the impact of air pollution on lung function has yet to be fully and accurately understood.
The aim of this study was to assess the short-term effects of PM2.5 on repeated measurements of lung function among school-age children. Stationary-source 24-h average PM2.5 was also evaluated. In addition, we examined relationships of lung function parameters to 24-h mean PM2.5 exposures for the period preceding lung function measurement, including the current and previous days.
Methods
Study population and design
This prospective cohort study was conducted in Nanjing, located in eastern China, which has a total area of 6597 km2 and resident population of 8,187,800. It is a modern industrial city, and urbanization has resulted in a significant increase in the number of motor vehicles, leading to serious air pollution. Two primary schools were selected for this study. Both schools have a large number of students and are located in densely populated area, with most students living nearby. We recruited students from grades three to five. During the period 2014–2015, we administered a questionnaire survey to study participants and their parents. Students who completed the questionnaire were tested lung function four times, with testing conducted during winter season in 2014 and 2015. A total of 86 students were enrolled, and each child underwent a total of four pulmonary function tests. A consent form to participate in the study was signed by the parents of all participating children.
Data collection
Air pollution and meteorological data
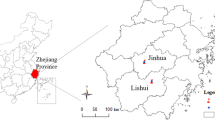
Daily air pollution data for PM2.5 from January 1, 2014 to December 31, 2015 were derived from Ruijin road and Maiqiao fixed-site monitoring stations of the National Air Pollution Monitoring System, which are the nearest monitoring stations to the schools, according to the latitude and longitude information of each school (Fig. 1). To control for the influence of meteorological factors on lung function, we also obtained data of daily mean temperature and relative humidity from January 1, 2014 to December 31, 2015 at Nanjing station (No. 58238) from the meteorological data network of the China Meteorological Administration.
Lung function measurement
Four measurements of lung function were performed during 2014 to 2015 (in December 2014, January 2015, November 2015, and December 2015). Lung function measures were performed by specialists, and the same electronic spirometer (Chest HI-801, Chest Inc., Tokyo, Japan) was used for all testing. All pulmonary function tests were done according to published standards (Miller et al. 2005). With the participant standing and wearing a nose clip, pulmonary function tests were repeated so as to obtain at least three reproducible forced expiratory flow curves. Lung function indicators included FVC, FEV1, PEF, and FEF25–75%.
Questionnaire
In the baseline survey, basic participant information, such as residential characteristics, lifestyles, and other data were obtained via questionnaires that were completed by the students and their parents. The information collected included age, sex, height, weight, passive smoking status, whether there were air purifiers or pets in the home, whether the home had been renovated within the past 1 year, and other information.
Statistical analysis
A mixed-effects regression model with study participant as a random effect was used to investigate the relationship between PM2.5 and lung function (Liu and Hedeker 2006). The effect estimates were expressed as the increase in lung function per 10-μg/m3 increase in PM2.5 concentration. The model was adjusted for age, sex, BMI, passive smoking, daily mean temperature, and relative humidity. The mixed-effects model was based on the following equation:
where Yij represents the lung function indicators (FVC, FEV1, PEF, FEF25–75%); β0 is the overall intercept; β1 is the regression coefficient for PM2.5; β2 …βn are the regression coefficients for the covariates in the model; ξj is the random effect for the study participant; j represents the study participant; i identifies the workday, and eij is the residual error term.
Exposure to PM2.5 concentration at the current day (lag0) and period lags (lag01, lag02, lag03, e.g. lag01 would be the 1-day moving average PM2.5 exposure, the average PM2.5 concentration of the current day and 1 day before lung function measurement) were examined using the model.
We also performed stratified analyses by sex (boys, girls) and BMI (overweight, not overweight) for the association between 1-day moving average PM2.5 exposure and lung function indicators. Overweight classification is based on the Chinese school-age children and adolescents overweight, obesity screening body mass index value classification criteria.
Sensitivity analyses were performed to test robustness of the results. We performed sensitivity analyses by including three confounding factors (whether the participant’s home had air purifiers, pets, or had been renovated within the past 1 year) in the analysis model individually; and these confounding factors were entered into the model at the same time.
Data analysis was performed using R version 3.3.1 software and the lme4 package.
Results
Characteristics of study participants
We followed 86 primary school students in Nanjing during 2014–2015. The study population characteristics are shown in Table 1. Male and female students accounted for 57.0% and 43.0% of the study population, respectively, with mean age at baseline of 9 years old. At baseline, 27 students (31.4%) were exposed to passive smoking; only 5 families (5.81%) had pets, 9 families (10.5%) had air purifiers, and 17 families (19.8%) had renovated their home in the past year.
Results of descriptive data analysis
Table 2 shows the results of descriptive analysis for lung function, air pollution, and meteorological data. The mean, standard deviation, minimum, quartile, median, and maximum measurements of lung function indicators, air pollution data, and meteorological data are presented. The mean concentration of PM2.5 was 84.3 μg/m3; this was higher than the Chinese ambient air quality guidelines for PM2.5 of 75 mg/m3 for a 24-h average, and much higher than the World Health Organization ambient air quality guidelines of 25 mg/m3.
Effects of PM2.5 on lung function
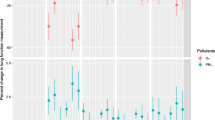
Figure 2 shows the associations between per 10 μg/m3 increase in PM2.5 concentrations for the current day and moving average exposure, and lung function alteration. An increase of 10 μg/m3 in the current day PM2.5 concentration was associated with a 9.83 mL decrease (95% CI: 2.46, 17.19) in FVC, a 8.06 mL decrease (95% CI: 1.06, 15.06) in FEV1, a 7.90 mL/s decrease (95% CI: -13.63, 29.44) in PEF, and a 11.61 mL/s decrease (95% CI: -2.05, 25.28) in FEF25–75%. No statistically significant associations were found between current day PM2.5 exposure and PEF, FEF25–75%. We found statistically significant associations between 1-day and 2-day moving average PM2.5 exposure and lung function indicators. The largest effect sizes were, a 23.22 mL (95% CI: 13.20, 33.25) decrease in FVC, a 18.93 mL (95% CI: 9.34, 28.52) decrease in FEV1, a 29.38 mL/s (95% CI: -0.40, 59.15) decrease in PEF, and a 27.21 mL/s (95% CI: 8.38, 46.04) decrease in FEF25–75% while the 1-day moving average PM2.5 concentration increased 10 μg/m3.
Results of stratified analyses
The results of stratified analyses were presented in Table 3. The acute effects of PM2.5 on lung function indicators in girls subgroup were greater in boys subgroup. And in BMI subgroups, greater associations between PM2.5 and lung function indicators were found in overweight subgroup, though these differences were not significant.
Results of sensitivity analyses
Table 4 shows results of the sensitivity analyses. When including the three confounding factors (air purifiers, pets, or home renovation in the past year) in the analysis model, individually or at the same time, changes in the effects of PM2.5 on lung function were very small compared with the main model analysis results, which suggests that our results were relatively robust.
Discussion
In this study, we analyzed the relationship between PM2.5 exposure and lung function by repeated measurements of lung function among 86 primary school students at two primary schools in Nanjing. We found that an increase in the current day, 1-day and 2-day moving average PM2.5 concentration was associated with decreases in lung function indicators. The association between current day PM2.5 exposure and FVC, FEV1 had statistical significance whereas no significant effects were detected for PEF and FEF25–75%. For 1-day and 2-day moving average PM2.5 exposure, except PEF, the acute effects of PM2.5 exposure were significant on FVC, FEV1 and FEF25–75%. These results suggest that short-term exposure to PM2.5 may affect healthy lung function, and the effects of PM2.5 on lung function has significant lag effects. This indicates that health protection measures should be maintained even a day or two after the end of an air pollution event. Compared with previous studies, in this study we focused on lung function indicators and also considered the lag effect of air pollution, to more fully reflect the impact of PM2.5 exposure on lung function. In addition, we used a linear mixed-effects model to analyze the data. Use of this model improved the test efficacy, as compared with most other analyses performed using GEE. The results of this work are important for understanding ways to improve protection of human respiratory health.
We found that an increase in the current day PM2.5 concentration was associated with a decrease in lung function indicators, although the changes in PEF and FEF25–75% were not statistically significant. And many previous studies have reported that the effects of current day PM2.5 exposure are statistically significant (Dales et al. 2009; Jacobson et al. 2012; Zwozdziak et al. 2016). For example, Zwozdziak et al. conducted a panel study of healthy schoolchildren in Poland aged 13–14 years and found that the reduction of FVC and PEF per interquartile range (IQR) for PM2.5 was 2.1% and 5.2%, respectively (Zwozdziak et al. 2016). In Brazil, Jacobson et al. conducted a panel study comprising 309 children aged 6–15 years; they found that the 24-h PM2.5 means ranged from 6.39 to 99.91 mg/m3. In addition, per 10-mg/m3 increase in PM2.5, the reduction in the PEF average varied between 0.26 L/min (95% CI: –0.49, −0.04) and 0.38 L/min (95% CI: –0.71, −0.04) (Jacobson et al. 2012).
In our study, we found that the greatest effect of PM2.5 on lung function was detected at 1-day moving average PM2.5 exposure; the effect of 2-day moving average PM2.5 exposure on lung function remained statistically significant. These results are in agreement with a review (Li et al. 2012) concluding that many outcomes of the associations between air pollution and lung function depend on the number of lag days. Results for lags of hours to days have been presented in only a few studies. A study of 182 elementary schoolchildren with physician-diagnosed asthma in Canada (Dales et al. 2009) showed that an IQR increase (6.0 mg/m3) in the previous 24-h mean concentration of PM2.5 was associated with a 0.54% (95% CI: 0.06, 1.02) decrease in FEV1 at bedtime (p = 0.027). Similar to our results, an Brazilian study by Jacobson et al. evaluated effects by considering air pollution levels on the current day or at 1- or 2- day lags and the averages of 0–1-day, 1–2-day, and 0-, 1-, and 2-day lags (Jacobson et al. 2012). The author found an average reduction of 0.41 L/min (95% CI: –0.76, −0.06) in the PEF for lag1 and 0.49 L/min (95% CI: –0.91, −0.07) for lag 0–1 cumulative exposure per an increase of 10 mg/m3 in PM2.5. The effects of same-day exposure, lag2, lag1–2, and lag 0–2 were not significant. A study in the United States (Delfino et al. 2004) showed that the most robust associations were for lag0 and 2-, 4-, or 5-day averages, with associations ranging between −4% and −22% of predicted FEV1 per IQR increase in personal PM. Although the statistically significant lag time for PM2.5 exposure was different, these results suggest that there is a hysteresis effect on the effect of PM2.5 exposure on lung function. The previous day’s exposure has the greatest impact on lung function, and the effect lasts for 2–5 days. These results highlight that when there is an air pollution event, the second day after the event is likely to be the time for the symptoms of lung function decline appear and the number of respiratory emergencies increase. Even after the end of an air pollution event, the health effects last for several days and we still need to pay attention to health protection.
Economic growth in China has been accompanied by a tremendous increase in energy consumption, emission of air pollutants, and number of poor air quality days. Air pollution has become one of the top environmental concerns in the country (Vennemo et al. 2009). However, there are few studies about the effects of short-term air pollution on lung function of children in China. We found no published works on the relationship between short-term exposure of PM2.5 and lung function in children. A study from Shenyang, China (Kasamatsu et al. 2006) examined the effects of winter PM air pollution on lung function among school-age children. The results of that study indicated that a 10 μg/m3-increase in PM7 caused changes in lung function parameters: FVC (−15.08 mL; 95% CI: –26.98, −3.02), FEV1 (−13.97 mL; 95% CI: –25.08, −3.02), PEF (−26.98 mL; 95% CI: –57.94, 5.08) in boys, and FVC (−13.02 mL; 95% CI: –23.02,–3.02), FEV1 (−10.95 mL; 95% CI: –20.0, −0.95), and PEF (15.08 mL; 95% CI: –15.08, 46.03) in girls. Unlike our results, the acute effects of PM2.5 exposure for boys were a little greater than girls.
Lung function tests are one of the primary measures to screen for respiratory diseases. These tests are important for early detection of lung and airway lesions, assessing the severity and prognosis of disease, evaluating the efficacy of drugs or other treatment methods, and identifying the causes of dyspnea. FVC is the best current measurement items, which can reflect the greater airway expiratory resistance. And it can be used as an auxiliary diagnostic tool for chronic bronchitis, bronchial asthma and emphysema. Among them, the amount of gas exhaled in the first second is called 1 s forced expiratory volume (FEV1), FEV1 and FVC are reduced in patients with pulmonary disease such as pulmonary fibrosis, and in patients with obstructive pulmonary disease such as asthma, FEV1 reduction is more pronounced than FVC. PEF mainly reflects the strength of the respiratory muscles and airway obstruction. Through the comparison of different time points within a day to help the diagnosis of the disease (Pellegrino et al. 2005). Exploring the effects of air pollution on lung function indicators can help improve understanding of the effects of air pollution on respiratory health. In this study, we found that short-term exposure to PM2.5 may affect lung function, and the effects of PM2.5 on lung function has significant lag effects. These prompted us that in an air pollution event, we should do some protective measures to protect our health, such as wearing masks, reducing outdoor activity time, closing doors and windows. A few days after the air pollution event, we also need pay attention to the health of the respiratory system, and avoid excessive physical activity.
The mechanisms of human lung injury caused by particles have been researched by several authors. The ability of PM to induce oxidative stress in the airways has been proposed as an important biological mechanism (Kelly 2003). Oxidative stress mediated by particles may arise from direct generation of reactive oxygen species from the surface of particles or from soluble compounds, such as transition metals or organic compounds (polyaromatic hydrocarbons) (Risom et al. 2005).
Our study has several strengths. We measured various lung function indicators, including FVC, FEV1, PEF, and FEF25–75%; most studies of children have only measured FEV1 and PEF (Li et al. 2012). Additionally, a linear mixed-effects model was used to analyze the data; GEEs have been used in most other analyses. The results of a systematic review (Ward and Ayres 2004) showed that random effects models produced larger estimates. Our study examined the lag effects of air pollution on lung function, a topic analyzed in few published studies. However, this study also has some unavoidable limitations. The sample size was small; however, we performed four repeated measurements of lung function and analyzed the data using a mixed-effects model. Air pollution data were obtained from the monitoring station nearest each school; accurate exposure data from the study participant were not obtained. Monitoring instruments that can be carried by individuals should be used in future studies, to obtain precise air pollution exposure data. In addition, we did not control for the effects of other air pollutants on lung function. The basic information of participants was obtained from questionnaire which was conducted only in the baseline survey, did not repeat in the second year. But, the time between four surveys was short and the information changed little. Lastly, this study was conducted in a single city; multicenter studies based on the same framework system are needed in the future.
Conclusion
Our study indicated that an increase in PM2.5 concentration was associated with a decrease in lung function indicators among children, suggesting that short-term exposure to PM2.5 may affect children’s health of lung function. In addition, the effects of PM2.5 on lung function showed significant lag effects. This information highlights the importance of maintaining health protection measures up to several days after the end of an air pollution event. Analysis of the relationship between air pollution and children’s lung function indicators can help to determine the impact of air pollution on the health of children’s respiratory systems so as to implement timely protective measures to prevent further health damage to children’s health. Further research is needed to examine the lag effects of PM pollution on children’s lung function. In future studies, portable monitoring instruments should be used to obtain precise air pollution exposure data. In addition, more multicenter studies based on the same framework system should be undertaken.
References
D'Amato G, Cecchi L, D'Amato M, Liccardi G (2010) Urban air pollution and climate change as environmental risk factors of respiratory allergy: an update. Journal of investigational allergology & clinical immunology: official organ of the International Association of Asthmology (INTERASMA) and Sociedad Latinoamericana de Alergia e Inmunología 20:95
Dales R, Chen L, Frescura AM, Liu L, Villeneuve PJ (2009) Acute effects of outdoor air pollution on forced expiratory volume in 1 s: a panel study of schoolchildren with asthma. Eur Respir J 34:316–323
Delfino RJ, Quintana PJE, Floro J, Samimi BS, Kleinman MT, Liu LS et al (2004) Association of [fev.Sub.1] in asthmatic children with personal and microenvironmental exposure to airborne particulate matter. Environ Health Perspect 112:932–941
Epa US. 2009. Integrated science assessment for particulate matter (final report). US EPA - Environmental Protection Agency
Epton MJ, Dawson RD, Brooks WM, Kingham S, Aberkane T, Cavanagh JA et al (2008) The effect of ambient air pollution on respiratory health of school children: a panel study. Environ Health 7:1–11
Gauderman WJ, Urman R, Avol E, Berhane K, Mcconnell R, Rappaport E et al (2015) Association of improved air quality with lung development in children. N Engl J Med 372:905–913
Gehring U, Gruzieva O, Agius RM, Beelen R, Custovic A, Cyrys J, Eeftens M, Flexeder C, Fuertes E, Heinrich J, Hoffmann B, de Jongste JC, Kerkhof M, Klümper C, Korek M, Mölter A, Schultz ES, Simpson A, Sugiri D, Svartengren M, von Berg A, Wijga AH, Pershagen G, Brunekreef B (2013) Air pollution exposure and lung function in children: the escape project. Environ Health Perspect 121:1357–1364
Ginsberg GL, Foos BP, Firestone MP (2005) Review and analysis of inhalation dosimetry methods for application to children's risk assessment. Journal of Toxicology & Environmental Health Part A 68:573–615
He QC, Lioy PJ, Wilson WE, Chapman RS (1993) Effects of air pollution on children's pulmonary function in urban and suburban areas of Wuhan, people's Republic of China. Arch Environ Health 48:382–391
Jacobson LS, Hacon SS, Castro HA, Ignotti E, Artaxo P, Ac PDL (2012) Association between fine particulate matter and the peak expiratory flow of schoolchildren in the brazilian subequatorial amazon: a panel study. Environ Res 117:27–35
Kasamatsu J, Shima M, Yamazaki S, Tamura K, Sun G (2006) Effects of winter air pollution on pulmonary function of school children in Shenyang, China. Int J Hyg Environ Health 209:435–444
Kelly FJ (2003) Oxidative stress: its role in air pollution and adverse health effects. Occupational & Environmental Medicine 60:612–616
Li S, Williams G, Jalaludin B, Baker P (2012) Panel studies of air pollution on children’s lung function and respiratory symptoms: a literature review. J Asthma 49:895–910
Liu LC, Hedeker D (2006) A mixed-effects regression model for longitudinal multivariate ordinal data. Biometrics 62:261–268
Miller MR, Hankinson J, Brusasco V, Burgos F, Casaburi R, Coates A, Crapo R, Enright P, van der Grinten C, Gustafsson P, Jensen R, Johnson DC, MacIntyre N, McKay R, Navajas D, Pedersen OF, Pellegrino R, Viegi G, Wanger J, ATS/ERS Task Force. (2005) Standardisation of spirometry. Eur Respir J 26:319–338
Oftedal B, Brunekreef B, Nystad W, Madsen C, Walker SE, Nafstad P (2008) Residential outdoor air pollution and lung function in schoolchildren. Epidemiology 19:129–137
Pellegrino R, Viegi G, Brusasco V, Crapo RO, Burgos F, Casaburi R, Coates A, van der Grinten C, Gustafsson P, Hankinson J, Jensen R, Johnson DC, MacIntyre N, McKay R, Miller MR, Navajas D, Pedersen OF, Wanger J (2005) Interpretative strategies for lung function tests. Eur Respir J 26:948–968
Risom L, Møller P, Loft S (2005) Oxidative stress-induced DNA damage by particulate air pollution. Mutat Res 592:119–137
Roy A, Hu W, Wei F, Korn L, Chapman RS, Zhang J (2012) Ambient particulate matter and lung function growth in chinese children. Epidemiology 23:464–472
Spyratos D, Sioutas C, Tsiotsios A, Haidich AB, Chloros D, Triantafyllou G et al (2014) Effects of particulate air pollution on nasal and lung function development among greek children: a 19-year cohort study. Int J Environ Health Res 25:1–10
Tzivian L (2011) Outdoor air pollution and asthma in children. Journal of Asthma Official Journal of the Association for the Care of Asthma 48:470–481
Urman R, Mcconnell R, Islam T, Avol EL, Lurmann FW, Vora H et al (2014) Associations of children's lung function with ambient air pollution: joint effects of regional and near-roadway pollutants. Thorax 69:540–547
Vennemo H, Aunan K, Lindhjem H, Seip HM (2009) Environmental pollution in China: status and trends. Review of Environmental Economics & Policy 3:209–230
Ward DJ, Ayres JG (2004) Particulate air pollution and panel studies in children: a systematic review. Occupational & Environmental Medicine 61:e13–e113
Wong SL, Coates AL, To T (2016) Exposure to industrial air pollutant emissions and lung function in children: Canadian health measures survey, 2007 to 2011. Health Rep 27:3
Yamazaki S, Shima M, Ando M, Nitta H, Watanabe H, Nishimuta T (2011) Effect of hourly concentration of particulate matter on peak expiratory flow in hospitalized children: a panel study. Environ Health 10:15
Zwozdziak A, Sówka I, Willak-Janc E, Zwozdziak J, Kwiecińska K, Balińska-Miśkiewicz W (2016) Influence of pm 1 and pm 2.5 on lung function parameters in healthy schoolchildren—a panel study. Environmental Science & Pollution Research International 23:23892–23901
Acknowledgments
We thank the Jiangsu Provincial Center for Disease Control and Prevention for their help in examing and recruiting the study subjects. We are grateful to the schoolchildren who participated in the study.
Funding
This study was funded by National Natural Science Foundation of China (Grant:91543111, 21277135, 4170123), Beijing Natural Science Foundation(7172145), National High-level Talents Special Support Plan of China for Young Talents.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Responsible editor: Philippe Garrigues
Rights and permissions
About this article
Cite this article
Xu, D., Zhang, Y., Zhou, L. et al. Acute effects of PM2.5 on lung function parameters in schoolchildren in Nanjing, China: a panel study. Environ Sci Pollut Res 25, 14989–14995 (2018). https://doi.org/10.1007/s11356-018-1693-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11356-018-1693-z