Abstract
Background
Many surgeons are still hesitant to do arthroscopic anterior cruciate ligament reconstruction (ACL) in patients above 40 years old.
Purpose
The effect of ACL reconstruction on functional outcomes in patients above 40 years of age.
Materials and methods
Patients of age > 40 years who underwent ACL reconstruction were enrolled in the study. Functional outcomes (Lysholm, WOMAC score, and Tegner activity scale), pain (VAS score), and knee stability (KT-1000) were assessed at final follow-up and compared with pre-operative scores. All patients were followed up for a minimum of 2 years.
Results
A total of 112 patients were included in the study. Eighty-eight were males and 24 were females. The mean age at the time of surgery was 44.8 ± 5.6 years (40–63 years). The mean Lysholm score was improved from 64.1 ± 11.7 to 87.2 ± 5.9 (p = 0.0001). Similarly, the WOMAC score was also improved from 8.8 ± 6.9 to 2.3 ± 1.9 (p = 0.0001). The mean side-to-side difference (KT-1000) also improved from 6.65 ± 2.25 mm to 2.32 ± 1.45 mm (p = 0.0001). More than 70% of the patients had excellent or good outcomes. Median pre-injury Tegner activity scale was 5 (3–8) and the median post-ACLR Tegner activity scale was 5 (3–7; p = 1).
Conclusion
ACL reconstruction in patients > 40 years of age results in good functional outcomes and knee stability.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Anterior cruciate ligament (ACL) tear is a common injury among young athletes [1], however, in recent times, these injuries are commonly seen among middle-aged persons also as more and more people are getting motivated to participate in a physically active healthy lifestyle. Arthroscopic ACL reconstruction (ACLR) is the treatment of choice for these injuries in young active adults [2]. However, there is still a dilemma over the treatment of ACL injuries in middle-aged patients [3]. Previously set, an arbitrary upper age limit of 40 years is now challenged by many authors and they reported good functional outcomes after ACL reconstruction in above 40 years old of patients [4,5,6,7,8,9]. Despite satisfactory results of ACLR in middle-aged patients, many surgeons are still reluctant to perform ACL reconstruction in patients above 40 years of age especially in recreational sportspersons. Even the American Academy of Orthopaedic Surgeons (AAOS) guidelines recommend ACL reconstruction in 18–35 years young active athletes, there is no clear recommendation for patients above 40 years [10]. In Asia, where more than 2/3rd of the population is between 15 and 65 years, it is important to have clear guidelines about the management of ACL reconstruction in different age groups. The present study was aimed to analyze the outcomes of ACL reconstruction with hamstring tendon graft in patients > 40 years and give clarification regarding the management of ACL tear in middle-aged patients. It was hypothesized that functional outcomes and mechanical knee stability would be significantly improved after arthroscopic ACL reconstruction in these patients.
Materials and methods
This was a retrospective study. A total of 112 patients of age > 40 years who underwent ACL reconstruction were included in the study. ACL reconstruction was performed using semitendinosus-gracilis graft with preserved tibial insertion by transportal technique [11]. Graft fixation was done at the femoral end using endobutton and at the tibial end, free ends were suture back at the insertion. Partial meniscectomy was done for unstable meniscal tears. The Outerbridge classification was used to grade the chondral damage. Inclusion criteria were patients of either sex having clinically and radiologically diagnosed ACL tear and X-ray showing osteoarthritis ≤ grade 3 (Kellgren and Lawrence grade). Exclusion criteria were: (1) previously operated on the same knee, (2) multi-ligamentous injury, (3) inflammatory arthritis like rheumatoid arthritis, (4) patients who underwent alignment corrective procedure along with ACL reconstruction and (5) insufficient data.
All patients underwent a similar rehabilitation protocol for a minimum of 6 months. From day 1, full-weight bearing walking with a brace, knee range of movement, and straight leg raise exercises were started. These exercises were continued for 6 weeks. After 6 weeks, gym cycling and half squats were started along with previous exercises and at 3 months, jogging and full squats were added. These exercises were continued for a minimum of 6 months.
Functional outcomes were assessed using the Lysholm score and the Western Ontario and McMaster Universities Osteoarthritis Index (WOMAC) [12] score both pre-operatively and postoperatively at the final follow-up. As Lysholm score includes factors like limp, pain, stairs climbing, instability, swelling, etc., it mainly assesses the daily functional movements. However, for the sportsperson, return to pre-injury activity level is also important, therefore, Tegner activity scale was also used at final follow-up and it was compared with the pre-injury status of the patients.
Knee laxity was measured using KT-1000 arthrometer pre-operatively and postoperatively at the final follow-up by the research fellow. The uninjured knee was tested first followed by the injured knee. At the time of testing, a bolster was kept under the thigh to keep the knee at 30 degrees of knee flexion. KT-1000 was recalibrated to zero every time before measuring the anterior translation of the tibia. The mean of three readings was taken to minimize the error. KT-1000 difference was calculated by subtracting anterior translation of tibia between affected and normal knee. The pain was scaled using VAS score pre-operatively and postoperatively at the final follow-up. All the patients were followed up for a minimum of 2 years.
In the present study, a comparison between matched young cohorts (< 40 years) was not done due to chances of selection bias on the basis of the Tegner activity scale, mean interval between injury and surgery, concomitant secondary pathology, and compliance to post-operative rehabilitation.
Statistics
Quantitative data were given as mean ± SD. Multiple t tests were applied to compare the quantitative data (Lysholm, WOMAC, Tegner activity scale, VAS score, and KT-1000). Shapiro–Wilk test was performed to check the normal distribution of data. Multiple t tests were performed for parametric values and Mann–Whitney test was used for non-parametric values. Categorical variables were reported as counts and percentages. All statistical analyses were performed at a significance level of α = 0.05. The analysis was conducted using IBM SPSS STATISTICS (version 22.0).
Results
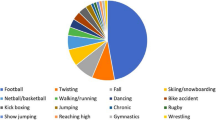
Eighty-eight were male and 24 were females. The mean age was 44.8 ± 5.6 years (40–63 years). The mean follow-up was 50.39 ± 32.36 months (24–112 months). In the present study, most of the patients enrolled were recreational sportspersons, only 3 patients were professional sportspersons. Details of patients involved in different sports are given in Table 1. In this study, 51% of the patients had grade 2 or more chondral damage and 58% of the patients had concomitant meniscal tear (Table 2). It was observed that functional outcomes after ACLR improved significantly. Lysholm score after ACLR improved from 64.14 ± 11.7 to 87.21 ± 5.91 (p = 0.0001). Similarly, WOMAC score also reduced significantly after ACL reconstruction (8.82 ± 6.9 to 2.31 ± 1.9; p = 0.0001). There was also significant relief in pre-operative pain (Table 3). The mean side-to-side difference was also reduced from 6.65 ± 2.25 mm to 2.32 ± 1.45 mm (p ≤ 0.000001). More than 70% of the patients had excellent or good outcomes (Table 4). The median pre-injury Tegner activity scale was 5 (3–8) and the median post-ACLR Tegner activity scale was 5 (3–7; p = 1).
Discussion
The major finding of the present study was that there was a significant improvement in the functional outcomes and mechanical knee stability after ACLR in patients age > 40 years. Management of ACL tear conservatively in above 40 years of age is outdated now, with most of the studies in the literature are in favor of surgical management [7, 9, 13,14,15,16,17,18]. Previously, theoretical points, such as pre-existing chondral damage, arthrofibrosis, and poor wound healing, that were considered against the surgical management in elderly patients do not hold true, as instability episodes lead to further chondral and meniscal damage which ultimately leads to more severe osteoarthritis. Even the presence of grade ≥ 3 chondral damage at the time of ACLR is not a contraindication, as good results were observed in patients even with full-thickness chondral damage [19,20,21].
Many previous studies reported satisfactory results after ACL reconstruction even in patients > 50 years [22,23,24,25,26,27,28]. Raju et al. reported good functional outcomes after ACL reconstruction in 75-year-old patients [29]. Toanen et al. reported excellent results of ACL reconstruction even in patients above 60 years of age [30]. This suggests that physiological age and activity levels are more paramount than chronological age.
Ciccotti et al. reported that non-operative treatment of ACL tear led to satisfactory outcomes in more than 80% of patients aged > 40 years with an ACL tear [31]. However, other than this study, no other study reported good functional outcomes with conservative treatment. Further, conservative treatment is associated with lifestyle modifications. In today’s world, where non-communicable disease constitutes 70% of deaths, people are opting for a more active and healthy lifestyle, therefore, lifestyle modifications are not advisable.
In the present study, the mean Lysholm score was 87.21 at the final follow-up. A recent meta-analysis study reported Lysholm score improved to 90.5 at the final follow-up in patients above 40 years [32]. Guido et al. reported a mean Lysholm score of nearly 88 at the end of 1 year and 90 at the end of a 2-year follow-up [33]. In the present study, not only the functional outcome improved but also the pain and mechanical knee stability improved significantly. Improvement in pain could be because of arthroscopic lavage and partial meniscectomy [34].
Conservative treatment for an ACL tear in patients > 40 years of age has been associated with residual knee laxity [35] which causes increase chances of meniscal and chondral damage, which ultimately leads to osteoarthritis (OA) knee [36]. However, the role of ACL reconstruction in the prevention of knee OA is controversial but it improves the knee kinematically to prevent secondary injuries to the knee [37, 38].
The results of the present study further emphasize the importance of ACL reconstruction in active middle-age patients. Management of ACL tear is important in middle-age patients also, and the results of present study suggested that ACLR not only improved knee stability but it also helps in returning to pre-injury activity and alleviating pain.
This study has some limitations— there is a discrepancy in male-to-female ratio, as majority of the patients were males; second, this was not a comparative study, matched cohorts were not available for comparison; third, it was a retrospective study; hence, there are chances of recall bias.
Conclusion
ACL reconstruction in patients above 40 years of age results in good functional outcomes and increased knee stability.
References
Turati M, Rigamonti L, Zanchi N et al (2021) An arthroscopic repair technique for proximal anterior cruciate tears in children to restore active function and avoid growth disturbances. Knee Surg Sports Traumatol Arthrosc. https://doi.org/10.1007/s00167-020-06367-w
Gupta R, Kapoor A, DavidMasih G (2020) Prevalence of concomitant knee injuries associated with anterior cruciate ligament tear in kabaddi and football players. J Clinic Orthop Trauma 23:160–165
Buss DD, Min R, Skyhar M, Galinat B, Warren RF, Wickiewicz TL (1995) Nonoperative treatment of acute anterior cruciate ligament injuries in a selected group of patients. Am J Sports Med 23(2):160–165
Heier KA, Mack DR, Moseley JB, Paine R, Bocell JR (1997) An analysis of anterior cruciate ligament reconstruction in middle-aged patients. Am J Sports Med 25(4):527–532
Brandsson S, Kartus J, Larsson J, Eriksson BI, Karlsson J (2000) A comparison of results in middle-aged and young patients after anterior cruciate ligament reconstruction. Arthroscopy 16(2):178–182
Gee AO, Kinsella S, Huffman GR, Sennett BJ, Tjoumakaris FP (2013) Anterior cruciate ligament reconstruction in patients aged> 40 years: a case-control study. Physician sportsmed 41(1):30–34
Brown CA, McAdams TR, Harris AHS, Maffulli N, Safran MR (2013) ACL reconstruction in patients aged 40 years and older: a systematic review and introduction of a new methodology score for ACL studies. Am J Sports Med 41(9):2181–2190
Tay KS, Tan AHC (2018) Clinical outcomes, return to sports, and patient satisfaction after anterior cruciate ligament reconstruction in young and middle-aged patients in an asian population: a 2-year follow-up study. Arthroscopy 34(4):1054–1059
Corona K, Ronga M, Morris B et al (2020) Comparable clinical and functional outcomes after anterior cruciate ligament reconstruction over and under 40 years of age. Knee Surg Sports Traumatol Arthrosc 28(6):1932–1945
Shea KG, Carey JL (2015) Management of anterior cruciate ligament injuries: evidence-based guideline. J Am Acad Orthop Surg 23(5):e1–e5
Gupta RK, Aggarwal S, Aggarwal V, Garg SK, Kumar S (2010) Preserved insertions of the semitendinosus and gracilis tendons (STG) in ACL reconstruction: a new surgical technique with preliminary results. Curr Orthop Pract 21(4):409–414
Antosh IJ, Svoboda SJ, Peck KY, Garcia ESJ, Cameron KL (2018) Change in KOOS and WOMAC scores in a young athletic population with and without anterior cruciate ligament injury. Am J Sports Med 46(7):1606–1616
Bohnsack M, Rühmann O, Lück K, Wirth C (2002) The influence of age on the outcome of anterior cruciate ligament reconstruction. Z Orthop Ihre Grenzgeb 140(2):194–198
Fabio C, Ludovico C, Andrea F, Raffaele I, Carolina C, Antonio P (2013) Knee stability after anterior cruciate ligament reconstruction in patients older than forty years: comparison between different age groups. Int orthop 37(11):2265–2269
Desai N, Björnsson H, Samuelsson K, Karlsson J, Forssblad M (2014) Outcomes after ACL reconstruction with focus on older patients: results from The Swedish National Anterior Cruciate Ligament Register. Knee Surg Sports Traumatol Arthrosc 22(2):379–386
Kim DK, Park G, Kuo L-T, Park WH (2019) Patients older than 50 years had similar results of knee strength and anteroposterior stability after ACL reconstruction compared to younger patients. Knee Surg Sports Traumatol Arthrosc 27(1):230–238
Damborg F, Nissen N, Kuur E (2002) Reconstruction of the anterior cruciate ligament in patients over 40 years of age. Ugeskr Laeger 164(9):1217–1220
Legnani C, Terzaghi C, Borgo E, Ventura A (2011) Management of anterior cruciate ligament rupture in patients aged 40 years and older. J Orthop Traumatol 12(4):177–184
Noyes FR, Barber-Westin SD (1997) Anterior cruciate ligament reconstruction with autogenous patellar tendon graft in patients with articular cartilage damage. Am J Sports Med 25(5):626–634
Shelbourne KD, Wilckens JH (1993) Intraarticular anterior cruciate ligament reconstruction in the symptomatic arthritic knee. Am J Sports Med 21(5):685–689
Hjermundrud V, Bjune TK, Risberg MA, Engebretsen L, Årøen A (2010) Full-thickness cartilage lesion do not affect knee function in patients with ACL injury. Knee Surg Sports Traumatol Arthrosc 18(3):298–303
Blyth MJ, Gosal HS, Peake WM, Bartlett RJ (2003) Anterior cruciate ligament reconstruction in patients over the age of 50 years: 2-to 8-year follow-up. Knee Surg Sports Traumatol Arthrosc 11(4):204–211
Dahm D, Wulf C, Dajani K, Dobbs R, Levy B, Stuart M (2008) Reconstruction of the anterior cruciate ligament in patients over 50 years. JBJS 90(11):1446–1450
Trojani C, Sané J-C, Coste J-S, Boileau P (2009) Four-strand hamstring tendon autograft for ACL reconstruction in patients aged 50 years or older. Orthop Traumatol Surg Res 95(1):22–27
Iorio R, Iannotti F, Ponzo A et al (2018) Anterior cruciate ligament reconstruction in patients older than fifty years: a comparison with a younger age group. Int Orthop 42(5):1043–1049
Weng C-J, Yeh W-L, Hsu K-Y et al (2020) Clinical and functional outcomes of anterior cruciate ligament reconstruction with autologous hamstring tendon in patients aged 50 years or older. Arthroscopy 36(2):558–562
Costa GG, Grassi A, Perelli S et al (2019) Age over 50 years is not a contraindication for anterior cruciate ligament reconstruction. Knee Surg Sports Traumatol Arthrosc 27(11):3679–3691
Panisset J-C, Gonzalez J-F, de Lavigne C et al (2019) ACL reconstruction in over-50 year-olds: comparative study between prospective series of over-50 year-old and under-40 year-old patients. Orthop Traumatol Surg Res 105(8):S259–S265
Vaishya R, Dhiman RS, Vaish A (2014) Anterior cruciate ligament reconstruction in a 75 years old man: a case report with review of literature. Chin J Traumatol 17(2):121–124
Toanen C, Demey G, Ntagiopoulos PG, Ferrua P, Dejour D (2017) Is there any benefit in anterior cruciate ligament reconstruction in patients older than 60 years? Am J Sports Med 45(4):832–837
Ciccotti MG, Lombardo SJ, Nonweiler B, Pink M (1994) Non-operative treatment of ruptures of the anterior cruciate ligament in middle-aged patients. Results after long-term follow-up. JBJS 76(9):1315–1321
Mall NA, Frank RM, Saltzman BM, Cole BJ, Bach BR Jr (2016) Results after anterior cruciate ligament reconstruction in patients older than 40 years: how do they compare with younger patients? A systematic review and comparison with younger populations. Sports Health 8(2):177–181
Wierer G, Runer A, Hoser C, Herbst E, Gföller P, Fink C (2017) Acute ACL reconstruction in patients over 40 years of age. Knee Surg Sports Traumatol Arthrosc 25(5):1528–1534
Karpinski K, Mueller-Rath R, Niemeyer P, Angele P, Petersen W (2019) Subgroups of patients with osteoarthritis and medial meniscus tear or crystal arthropathy benefit from arthroscopic treatment. Knee Surg Sports Traumatol Arthrosc 27(3):782–796
Fitzgerald GK, Axe MJ, Snyder-Mackler L (2000) A decision-making scheme for returning patients to high-level activity with nonoperative treatment after anterior cruciate ligament rupture. Knee Surg Sports Traumatol Arthrosc 8(2):76–82
Louboutin H, Debarge R, Richou J et al (2009) Osteoarthritis in patients with anterior cruciate ligament rupture: a review of risk factors. Knee 16(4):239–244
Tsoukas D, Fotopoulos V, Basdekis G, Makridis KG (2016) No difference in osteoarthritis after surgical and non-surgical treatment of ACL-injured knees after 10 years. Knee Surg Sports Traumatol Arthrosc 24(9):2953–2959
Paschos NK (2017) Anterior cruciate ligament reconstruction and knee osteoarthritis. World J Orthop 8(3):212
Funding
No funding was received for the present study.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
Authors have no conflict of interest.
Ethical approval
This was a retrospective study, therefore, ethical approval was not taken for this study.
Consent for participation
Consent was received from all the patients.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Gupta, R., Kapoor, A., Singhal, A. et al. Good functional outcomes in patient’s age > 40 years after anterior cruciate ligament reconstruction with hamstring tendon graft: a retrospective study. Sport Sci Health 17, 931–935 (2021). https://doi.org/10.1007/s11332-021-00754-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11332-021-00754-7