Abstract
Purpose
A new classification system is proposed to help the interpretation of drug-induced sleep endoscopy (DISE). The purpose is to create a classification system that improves upon existing systems designed to assess suitability of lateral wall surgery such as expansion pharyngoplasty whilst improving the reliability of the classification.
Methods
A qualitative study into the difficulties trainees had with existing systems was used to identify key issues that needed to be addressed. A visual description of the palate, tonsils, lateral pharyngeal wall, tongue base, epiglottis (PTLTbE) classification was developed. Preliminary data on the inter-rater reliability of PTLTbE were collected. Twenty junior doctors were asked to interpret 5 DISE videos using the PTLTbE classification, and the kappa and percentage agreement were calculated.
Results
The Krippendorff alpha ranged between 0.56 and 0.86 for individual DISE videos which compared favourably with the results from those who also completed the VOTE classification (range 0.31 to 0.66). The overall percentage agreement for PTLTbE was 90.1%.
Conclusions
There are a number of advantages of the PTLTbE system over other existing DISE classifications. (1) Tonsillar obstruction is separated from lateral pharyngeal wall collapse. (2) Interobserver reliability is improved, critical to improve communication, patient outcomes and future research. (3) The learning curve to use this system is short. Most doctors did not need to refer to the classification images as an aide-memoire after a few uses of the PTLTbE system. A fuller examination of the reliability of the PTLTbE system is underway along with examination of its use in clinical settings.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Obstructive sleep apnoea (OSA) is a disease process which results in repeated upper airway obstruction during sleep resulting in characteristic symptoms, signs, and complications. The gold-standard therapy for OSA is continuous positive airway pressure (CPAP); unfortunately, the tolerability of this intervention is poor, with reports of only 34.1% of patients using CPAP enough to reduce the morbidity associated with OSA [1]. Positional therapy is confined to patients who have clear improvement in their OSA when typically sleeping in the non-supine position and is an attractive strategy in this sub-population [2]. Mandibular advancement devices are often an excellent option in some patients; however, their efficacy appears dependent on anatomical phenotypes and compliance, which is often suboptimal [3]. A recent review of non-invasive treatment options for OSA compared CPAP with other treatment modalities [4]. The authors make the point that subjective and objective measures often contradict each other, and further research into this discrepancy is warranted. Patients therefore seek alternative therapies [5], which often require identification of the level of upper airways obstruction to allow a targeted treatment option.
Drug-induced sleep endoscopy (DISE) was first described by Croft and Pringle [6] in our institution in 1991, and it has since become one of the most widely used methods of investigating the upper airway during sleep worldwide. By passing a flexible nasendoscope into the upper airway during light anaesthetic sedation, it is possible to recreate the probable obstructive features seen during normal physiological sleep [7]. It is currently the only clinically acceptable way of obtaining a dynamic endoscopic examination of obstruction during a state similar to natural sleep. Difficulties in the interpretation of what is observed during DISE have limited its use and confounded results. Numerous classification systems have been described [8,9,10,11], but no single system has been agreed upon [7]. There also seems to be a significant learning curve to the interpretation of DISE with expert clinicians providing different results to more junior colleagues [12]. DISE therefore becomes accessible only to those clinicians who have significant experience in its use and have become comfortable with interpreting the results.
The authors believed there was a niche for a new classification system in which the observer reliability was high whilst still providing the information needed to communicate the obstructive level clearly to the reader. The novel classification system presented in this article, we believe, succeeds in this respect. In addition, with the impact of lateral pharyngeal wall surgery such as expansion pharyngoplasty [13], a further nuanced classification system has been developed to accommodate these treatment options.
Methods
The authors performed a preliminary investigation into the difficulties that ENT surgeons in training had with current classifications. Qualitative semi-structured interviews were conducted at the study centre immediately following DISE procedures to ascertain the points that trainees found difficult in DISE interpretation. Perceived ambiguity appeared to be most prevalent issue in many of the classification systems for juniors, for example, understanding the difference between partial or complete obstruction, or where exactly certain obstructive levels were in the pharynx. When asked to record a percentage obstruction at a defined specific level, most were unable to reliably differentiate anything more precisely than a 50% obstruction i.e. ‘is there less or more than 50% obstruction at the tongue base’. Attempting to delineate 25% obstructive levels (e.g. is there a 0–25%/25–50%/50–75% or > 75% obstruction) seemed to challenge even the more experienced practitioners and led to extremely poor inter- and intra-rater reliability. The reason for this was assumed to be that the upper airway is a changeable dynamic organ during sleep, which cycles through obstruction and reopening with each breath. It was also noted by the authors that many inexperienced clinicians often attempted to perceive the most glaring abnormality on a DISE but often missed the more subtle signs that the senior practitioner spotted regularly. An example of this would be the identification of large tonsils but failed to appreciate the obstruction caused by a coexisting tongue base collapse.
Focusing on these difficulties whilst attempting to replicate the meticulous precision of the TNM cancer staging system [14] greatly improved the acceptability of our new classification system. A considerable amount of time was dedicated to improve the ease of remembering the new classification system, as clinicians found referring to a table or aide-de-memoire cumbersome. For this reason, a visual classification system was adopted as it seemed to provide the easiest method of remembering the system.
PTLTbE (palate, tonsils, lateral pharyngeal wall, tongue base, epiglottis) was finally decided upon as the name of the classification system. Admittedly, this is a far from elegant name, but it has the advantage of forcing the user to individually assess each location in order of a normal flexible nasendoscope examination. The classification is provided below with a detailed description for each level in turn.
Each part of the PTLTbE classification is considered in turn and follows the routine of a normal nasendoscopic examination. No attempt is made to identify the most important site of obstruction; the opinion of the observer is intentionally repressed to a minimum. Some levels are very similar to other classification systems, which is again intentional. The palatal level denoted by the ‘P’ moniker is similar to the ‘Velum’ in the VOTE classification [9] and the ‘Nose’ in the NOHL classification [11]. It has been simplified somewhat by combining lateral and circumferential collapse as in our testing it seemed these were easily confused. Therefore in the PTLTbE system, the palate level is divided into ‘Normal or P0’, ‘Anterior posterior collapse (AP) or P1’, and ‘Circumferential collapse or P2’ as seen in Fig. 1.
During nasendoscopy, the soft palate is viewed from the postnasal space or nasopharynx. In ‘normal’ individuals who do not snore, the soft palate and uvula remain relatively motionless during respiration. When viewed from the postnasal space, the pharyngolarynx is clearly seen behind the palate. If no flutter causing snoring or obstruction is observed at this level, the P level is provided the class 0 or zero. The authors suggest inserting this as a subscript (similar to the GRABAS scale [15]) which aids readability (e.g. P0). Class 0 in any of the levels denotes no obstruction or normal so therefore P0 T0 L0 Tb0 E0 would be considered a completely normal examination. P1 describes an AP collapse or flutter seen at the uvula without nasopharyngeal lateral wall collapse. P2 finally is circumferential collapse, which is synonymous with both lateral and circumferential collapse in the VOTE and NOHL classification systems. The distinction between lateral and circumferential collapse was difficult to describe clearly, and juniors found identifying the difference difficult. The distinction between AP collapse and circumferential collapse was necessary as it features as exclusion criteria in some operations, for example in hypoglossal nerve stimulator trials [16]. Figure 1 has more detail about the palatal level.
Advancing the nasendoscope further into the pharynx allows a view of the upper airway that is very familiar to those trained with nasendoscopy. Positioning of the nasendoscope should be approximately at the level of the base of the uvula or an area close to it that allows an adequate view of the larynx. In this classification positioning, the nasendoscope directly above the anterior commissure is used to denote a reasonable midpoint landmark. It is important to try and avoid shifting posteriorly toward the posterior pharyngeal wall to gain a better view of the larynx. Although this is standard procedure in a clinical examination with nasendoscopy, this change of position would artifactually alter the classification results at some levels in this, and any other classification. For example in the case of very large tonsils, an adequate view of the larynx is possible by descending down close to the vocal cords and directing the scope posteriorly. Claiming therefore that the tonsils are not obstructing the airway in this situation would be incorrect. The authors have therefore attempted to be as clear as possible with the defining of each level, and so clear guidance for the positioning of the nasendoscope is paramount to the success of a correct interpretation during DISE.
Again, T0 is a normal situation with respect to palatine tonsils. There has either been a previous tonsillectomy or the palatine tonsils are not visualised during DISE. The difference between T1 and T2 is based on the percentage obstruction of the airway by observed palatine tonsils. Less than 50% obstruction is considered to be a T1 and 50% or greater is classified as T2. To aid in the calculation of percentage obstruction, the anterior commissure is again used as the midpoint of the airway. Imaginary cross hairs (depicted in green in Fig. 2) are recommended for use by the observer that centres on the anterior commissure. This effectively divides the airway into 4 roughly equal quadrants. This aids the observer to judge if the tonsillar obstruction is less than or greater than 50% obstruction. Observers ought to understand that tonsils commonly obstruct from the lower two quadrants toward the midline. The reverse is true for lateral wall collapse. Appreciation of this will aid the observer to differentiate between tonsillar and lateral wall obstruction.
The use of quadrants greatly improved the accuracy of the percentage calculation of obstruction in our testing. Some classifications (Croft and Pringle [8]) provide information about inspiratory and expiratory phases in relation to airway collapse. The purpose of this in the Croft and Pringle classification is to express severity and prognosticate the challenges for surgical management of these patients. Breathing phase data represents an avenue of research that has not yet been fully investigated and so although important, this information is not included in the PTLTbE classification due to the increase in complexity involved and the subsequent impact on interobserver reliability. As mentioned above, this classification is purely intended as a clinical communication tool rather than an exhaustive and precise classification of the subtle nuances seen by expert DISE practitioners. More information about the tonsillar level is provided in Fig. 2.
The observation of the lateral pharyngeal wall level is very similar to the tonsillar level. The nasendoscope is positioned in the same location, and again, the anterior commissure is used as an imaginary midpoint with crosshairs aiding in percentage obstruction calculation. L0 therefore describes a normal examination of the lateral pharyngeal wall, with no significant obstruction seen. Often there is a flicker of movement (less than 5%), with respiration that should be disregarded as a variant of normal. Also large palatine tonsils may occasionally pull the lateral wall into the airway and make interpretation challenging. Attention to detail and focusing only on the lateral pharyngeal wall help one formulate a reasonable interpretation. L1 is therefore less than 50% obstruction of the airway with L2 is 50% or greater obstruction seen. The diagrams and explanation provided in Fig. 3 will aid understanding for this level.
With the PTLTbE classification, there are no levels that exclude the use of other classes in different levels. For example, there might have been a clash with classifying a 100% obstruction at the tonsil level and then a similar level of obstruction at the lateral pharyngeal wall. It is clearly impossible to achieve a greater than 100% obstruction of the airway, and so the PTLTbE system allows for this eventuality. It is therefore entirely possible to have a result of P0 T2 L2 Tb0 E0 and not contradict itself. The use of ‘50% or greater’ for class 2 obstructions at these levels means that the example provided above describes a patient who has 50% obstruction at the tonsil level and an equal 50% at the lateral pharyngeal wall level. The authors would recommend the observer to try and decide whether the tonsils or lateral wall have a larger impact on the airway as the chances of an exactly 50:50 split are extremely unlikely. If making this decision proves to be difficult, adopting a T2 L2 class would be a reasonable option indicating that there is a significant airway obstruction from both of these levels. Understanding this will help the clinician prognosticate the likely success or failure of an operation for a patient. For example in the case of a P0 T2 L0 Tb0 E0 (i.e. just tonsillar obstruction), the surgeon can be reasonably confident that a tonsillectomy would be of benefit for their patient (excluding of course other co-morbidities such as obesity or pulmonary disease). If on the other hand there is an element of coexisting lateral pharyngeal wall collapse, the surgeon would moderate assurances that a tonsillectomy would be as successful.
One should pay careful attention to L2 collapse that is truly 100%. Many of these patients have snoring noise generation from the lateral pharyngeal walls vibrating a column of air meeting at the midline. Therefore, to eliminate snoring as well as airway obstruction, treatment to this lateral wall would be necessary. This population also often display characteristic bulging of the lateral pharyngeal walls posterior to the palatopharyngeus fold. The authors have named this the ‘Pharyngeal Cushions’, which are easily seen in the outpatients setting in severe sleep-disordered breathing patients.
The addition of the lateral pharyngeal wall level in this classification was made to clear ambiguity in other classifications. Having a tonsillectomy or an expansion pharyngoplasty is two very different operations for two separate pathologies; therefore, appreciating this in a classification was required. The concentric, lateral, and AP collapse options available in other classifications resulted in confusion during our initial qualitative interview study when designing this classification.
The extent of the airway is discernibly different at the tongue base level. The tongue base is structurally inferior to the palatine tonsils and therefore does not occupy a similar airway level. Here, the actual useable airway is the distance between the anterior commissure and the posterior pharyngeal wall (shown in green in Fig. 4). Therefore, the airway midpoint for calculating a 50% obstruction at this level is actually the midpoint of this imaginary line (when viewed from the same nasendoscopy location as described before). Tb0 is therefore a tongue base that does not push the epiglottis posteriorly over the laryngeal inlet. Typically the vallecula is seen in the Tb0 class. Tb1 is when less than 50% of the airway at this level is being obstructed by a tongue base that is collapsing posteriorly over the laryngeal inlet. Tb2 therefore is 50% or greater obstruction at this level. The bulk of the epiglottis is included in the calculation of percentage obstruction so long as the tongue base is pushing it posteriorly. Therefore, the laryngeal surface of the epiglottis should be used as the point of maximal obstruction rather than the tongue base anterior to it. An epiglottis that moves posteriorly without the aid of the tongue base collapsing on to it should be interpreted as an epiglottic problem and not a tongue base obstruction. In the event of a tongue base that has collapsed posteriorly with coexisting epiglottic collapse, the observer will need to take both levels into consideration when interpreting these situations (e.g. P0 T2 L0 Tb1 E1 or P0 T2 L0 Tb2 E1).
Positioning of the nasendoscope can be difficult when interpreting this level. As mentioned previously, there is a tendency to direct the nasendoscope posteriorly to gain a better view of the larynx that would produce an artifactual improvement in the scoring here. Also, if there are significant coexisting obstructive elements at the tonsillar and lateral pharyngeal wall levels, then the practitioner may have to descend down to an appropriate point in the pharynx to gain an adequate view.
The epiglottis rarely has an obstructive effect on the airway, but this can be achieved in a surprising number of different ways. The most common variant is the so-called epiglottic trapdoor that is depicted in Fig. 5. Other variants include an infolding of the epiglottis similar to what is seen in infant laryngomalacia (also known as ‘omega shaped’ or ‘horse-shoe epiglottis’). The effect of other laryngomalacia type obstructions (for example the indrawing of redundant arytenoid mucosa) is also very rarely seen in adults. None of these variants are manifestly more severe than the other forms, and therefore, the decision was made to reduce the ‘E’ level to two classes. In effect, you either have an epiglottic obstructive pathology or not. More detail about this level is again provided in Fig. 5. It is important to note that an epiglottis that is pushed posteriorly by a collapsing tongue base is not an epiglottic pathology and should not be considered as such.
The final result is expressed similar to the GRABAS scale with each level provided an individual class that are independent of each other. Senior clinicians will be able to interpret a PTLTbE result relatively easily. For example, P1 T0 L1 Tb2 E0 would represent a patient with lateral pharyngeal wall and palatal flutter, but the main problem would be tongue base collapse. Tongue base reduction and limited lateral pharyngeal wall surgery would be required for improved airway along with palatal surgery to reduce snoring. Typically, sleep-disordered breathing manifests as a multilevel obstruction, and the PTLTbE classification is able to describe this effectively. Senior clinicians may well choose to add extra information in addition to the PTLTbE system such as the effect of chin lift, jaw thrust, or vertical mouth opening [17]. This can be incorporated into the system by the following notation for each manoeuvre, e.g. using the example above, P1 T0 L1 Tb2 E0 could change to P1 T0 L0 Tb1 E0 with chin lift, and P0 T0 L0Tb0 E0 with jaw thrust. The implication being that a mandibular advancement device (MAD) would be of benefit to this patient in terms of airway and snoring [18]. Further data may be described by the inclusion of information when the classification is altered with a given protrusion of the mandible. A recent example would be the use of remotely controlled mandibular protrusion during DISE [19], or with the use of a simulation bite [20]. Conceivably similar alterations may be measured using a reliable classification system when a patient is moved from a supine to a non-supine position [21], or with head rotation [22]. The research potential of a classification tool with good inter-rater reliability would more freely allow clinicians to perform multi-centre trials without results being possibly skewed.
To assess the interobserver reliability of the classification, 20 junior doctors (who previously had not performed DISE) were taught the PTLTbE classification and then showed 5 DISE videos. These videos were selected by the first author to show the range of different abnormalities. These novices scored the videos using the PTLTbE classification system and their results were compared with the author’s own interpretation. Five of the 20 junior doctors were taught the VOTE and the PTLTbE classifications, and the inter-rater reliability of each was compared. The study participants were permitted to return and alter their results if they noticed something later that they did not see on first inspection. This was allowed to reduce bias against the classification system that the participant decided to use first.
Krippendorff alpha kappa was calculated for each video using the PTLTbE classification, and an overall percentage agreement was calculated for each of the PTLTbE domains and the system overall. Preliminary results based on the 5 junior doctors who were taught both PTLTbE and VOTE were also calculated.
Results
The PTLTbE Krippendorff alpha for video 1 = 0.86, video 2 = 0.54, video 3 = 0.82, video 4 = 0.66, and video 5 = 0.71. This compared favourably with the results from those who also completed the VOTE classification for each video (video 1 = 0.47, video 2 = 0.47, video 3 = 0.66, video 4 = 0.36, and video 5 = 0.31). The scale on the level of agreement proposed by Landis and Koch [23] is as follows: kappa coefficient ≤ 0 = poor, 0.01–0.20 = slight, 0.21–0.40 = fair, 0.41–0.60 = moderate, 0.61–0.80 = good–substantial, and 0.81–1 = almost perfect.
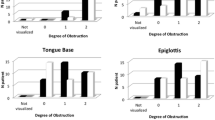
When investigating each domain of the PTLTbE classification, the first author’s findings were used as a ‘gold standard’ and variability from that was calculated using a simple percentage agreement score (percentage of study sample who scored exactly the same as the first author).
Palatal domain—91.43% agreement
Tonsil domain—97.14% agreement
Lateral pharyngeal wall domain—86.67% agreement
Tongue base domain—77.14% agreement
Epiglottis domain—90.1%
Overall percentage agreement—90.1%
The results suggest that there were certain obstructive level combinations which were less adequately interpreted than others. Due to the low sample size (5 videos shown to 20 doctors), it would be difficult to prove significance here, and therefore, this was not calculated.
Discussion
The main differences between the PTLTbE classification and some of the other systems currently available are that it:
Separates tonsillar obstruction from lateral pharyngeal wall collapse. Since each structure is anatomically different and have different treatment options (tonsillectomy vs pharyngoplasty), this addition was considered essential.
Has excellent reliability particularly with interobserver agreement. This is critical in a busy sleep centre and for future research.
Has a short learning curve to use this system. Most doctors did not need to refer to the classification images as an aide-de-memoire after a few uses of the PTLTbE system.
PTLTbE classification has shown to have an excellent interobserver agreement across 20 different assessors when assessing 5 DISE videos. The lowest level of agreement was found at the tongue base level (77.14%) and also partly at the lateral wall level (86.67%). The assumption is that attempting to identify the position of the anterior commissure when it is actively obscured from view would make this judgement difficult to construct. Lateral pharyngeal wall obstruction is also often confused with tonsillar obstruction, hence the likely difficulty in this domain.
Gillespie et al. [24] showed that the interobserver agreement between three assessors when using DISE index classification was moderate-good ((k = 0.65; 95% CI, 0.62–0.69), (k = 0.65; 95% CI, 0.61–0.69), (k = 0.62; 95% CI, 0.10–0.38)). In addition, they showed that interobserver agreement decreased when the three assessors used VOTE classification ((k = 0.28; 95% CI, 0.16 to 0.40), (k = 0.24; 95% CI, 0.10–0.38), (k = 0.29; 95% CI, 0.16 to 0.41)). The rational for the difference in result was not clearly explained and still subject to further scrutiny.
Vroegop et al. [12] showed that the interobserver agreement when assessing upper airway collapse amongst 90 non-experienced assessors at the palatal level, oropharyngeal level, tongue base, hypopharyngeal level, and epiglottis level has the kappa coefficient of − 0.03, 0.09, 0.33, 0.08, and 0.23 respectively. In addition, they showed interobserver agreement when assessing upper airway collapse amongst 7 experienced assessors at the palatal level, oropharyngeal level, tongue base, hypopharyngeal level, and epiglottis level had the kappa coefficient of 0.51, 0.48, 0.71, 0.03, and 0.51. In this study, assessors observed six DISE videos and were asked to score the upper airway collapse at obstruction level (palate, oropharynx, tongue base, hypopharynx, epiglottis), obstruction direction (anteroposterior, concentric, lateral), and degree of collapse (none; partial or complete collapse).
Carrasco-Llatas et al. [25] assessed interobserver agreement for 31 DISE videos comparing interpretation by an experienced and non-experienced assessor using modified VOTE classification. Kappa coefficient was 0.1667, 0.7742, 0.5571, and 0.4768 at the soft palate, oropharynx, tongue base, and epiglottis respectively.
The interobserver agreement of the PTLTbE system compared with the three mentioned studies is significantly higher; however, the results may be misleading. The author explained and coached the junior doctors in the use of the PTLTbE classification and ensured understanding before starting the reliability study. In addition, the sample size was small, and further research is required here. The ability of untrained doctors being able to use the classification without one-on-one tuition is currently being investigated in a larger study. Our results however are encouraging and we believe that the PTLTbE system has some advantages over other existing classifications and may result in a unified DISE classification system which can help advance practices. We are undertaking a larger study into the benefits of this system as well as testing its appropriateness for clinical use (Fig. 6).
References
Rotenberg BW, Murariu D, Pang KP (2016) Trends in CPAP adherence over twenty years of data collection: a flattened curve. J Otolaryngol Head Neck Surg 45(1):43
Yingjuan M, Siang WH, Leong Alvin TK, Poh HP (2019) Positional therapy for positional obstructive sleep apnea. Sleep Med Clin 14(1):119–133
Bartolucci ML, Bortolotti F, Raffaelli E, D’Antò V, Michelotti A, Alessandri Bonetti G (2016) The effectiveness of different mandibular advancement amounts in OSA patients: a systematic review and meta-regression analysis. Sleep Breath 20(3):911–919
Gao YN, Wu YC, Lin SY, Chang JZ, Tu YK (2019) Short-term efficacy of minimally invasive treatments for adult obstructive sleep apnea: a systematic review and network meta-analysis of randomized controlled trials. J Formos Med Assoc 118(4):750–765
Aurora RN, Casey KR, Kristo D, Auerbach S, Bista SR, Chowdhuri S, Karippot A, Lamm C, Ramar K, Zak R, Morgenthaler TI, American Academy of Sleep Medicine (2010) Practice parameters for the surgical modifications of the upper airway for obstructive sleep apnea in adults. Sleep. 33(10):1408–1413
Croft CB, Pringle M (1991) Sleep nasendoscopy: a technique of assessment in snoring and obstructive sleep apnoea. Clin Otolaryngol Allied Sci 16:504–509
De Vito A, Carrasco Llatas M, Ravesloot MJ et al (2018 Dec) European position paper on drug-induced sleep endoscopy: 2017 update. Clin Otolaryngol 43(6):1541–1552
Pringle MB, Croft CB (1993) A grading system for patients with obstructive sleep apnoea-based on sleep nasendoscopy. Clin Otolaryngol Allied Sci 18:480–484
Kezirian EJ, Hohenhorst W, de Vries N (2011) Drug-induced sleep endoscopy: the VOTE classification. Eur Arch Otorhinolaryngol 268:1233–1236
Bachar G, Nageris B, Feinmesser R, Hadar T, Yaniv E, Shpitzer T, Eidelman L (2012) Novel grading system for quantifying upper-airway obstruction on sleep endoscopy. Lung. 190:313–318
Vicini C, De Vito A, Benazzo M et al (2012) The nose oropharynx hypopharynx and larynx (NOHL) classification: a new system of diagnostic standardized examination for OSAHS patients. Eur Arch Otorhinolaryngol 269:1297–1300
Vroegop AVMT, Vanderveken OM, Wouters K, Hamans E, Dieltjens M, Michels NR, Hohenhorst W, Kezirian EJ, Kotecha BT, de Vries N, Braem MJ, van de Heyning P (2013) Observer variation in drug-induced sleep endoscopy: experienced versus non-experienced ear, nose, and throat surgeons. Sleep. 36(6):947–953
Pang KP, Woodson BT (2007) Expansion sphincter pharyngoplasty: a new technique for the treatment of obstructive sleep apnea. Otolaryngol Head Neck Surg 137(1):110–114
Edge SB, Compton CC (2010) The American Joint Committee on Cancer: the 7th edition of the AJCC cancer staging manual and the future of TNM. Ann Surg Oncol 17(6):1471–1474
Hirano M (1981) Clinical examination of voice. Springer
Strollo PJ Jr, Soose RJ, Maurer JT, de Vries N, Cornelius J, Froymovich O, Hanson RD, Padhya TA, Steward DL, Gillespie MB, Woodson BT, Van de Heyning PH, Goetting MG, Vanderveken OM, Feldman N, Knaack L (2014) Strohl KP; STAR trial group. Upper-airway stimulation for obstructive sleep apnea. N Engl J Med 370(2):139–149
Vroegop AV, Vanderveken OM, Van de Heyning PH, Braem MJ (2012) Effects of vertical opening on pharyngeal dimensions in patients with obstructive sleep apnoea. Sleep Med 13(3):314–316
Johal A, Hector MP, Battagel JM, Kotecha BT (2007) Impact of sleep nasendoscopy on the outcome of mandibular advancement splint therapy in subjects with sleep-related breathing disorders. J Laryngol Otol 121(7):668–675
Dieltjens M, Braem MJ, Op de Beeck S, AVMT V, Kazemeini E, Van de Perck E, Beyers J, Kastoer C, Wouters K, Willemen M, Verbraecken JA, Vanderveken OM (2019) Remotely controlled mandibular positioning of oral appliance therapy during polysomnography and drug-induced sleep endoscopy compared with conventional subjective titration in patients with obstructive sleep apnea: protocol for a randomized crossover trial. Trials 20(1):615
Vroegop AV, Vanderveken OM, Dieltjens M, Wouters K, Saldien V, Braem MJ, Van de Heyning PH (2013) Sleep endoscopy with simulation bite for prediction of oral appliance treatment outcome. J Sleep Res 22(3):348–355
Yalamanchili R, Mack WJ, Kezirian EJ (2019) Drug-induced sleep endoscopy findings in supine vs nonsupine body positions in positional and nonpositional obstructive sleep apnea. JAMA Otolaryngol Head Neck Surg 145(2):159–165
Safiruddin F, Koutsourelakis I, de Vries N (2014) Analysis of the influence of head rotation during drug-induced sleep endoscopy in obstructive sleep apnea. Laryngoscope. 124(9):2195–2199
Landis JR, Koch GG (1977) The measurement of observer agreement for categorical data. Biometrics. 33(1):159–174
Gillespie MB, Reddy RP, White DR, Discolo CM, Overdyk FJ, Nguyen SA (2013) A trial of drug-induced sleep endoscopy in the surgical management of sleep-disordered breathing. Laryngoscope. 123(1):277–282
Carrasco-Llatas M, Zerpa-Zerpa V, Dalmau-Galofre J (2017) Reliability of drug-induced sedation endoscopy: interobserver agreement. Sleep Breath 21(1):173–179
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflict of interest.
Ethical approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Presentation at conferences
Sleep Congress Rimini Italy 2016—presented first version of classification
ERS London, UK 2018—presented draft version of classification
AAO-HNS 2018 Annual meeting Atlanta—presented final version of classification
Rights and permissions
About this article
Cite this article
Veer, V., Zhang, H., Mandavia, R. et al. Introducing a new classification for drug-induced sleep endoscopy (DISE): the PTLTbE system. Sleep Breath 24, 1685–1693 (2020). https://doi.org/10.1007/s11325-020-02035-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11325-020-02035-y