Abstract
Background
Chronic kidney disease (CKD) has become a major public health problem across the globe, leading to various complications. This study aimed to construct a nomogram to predict the 4-year risk of CKD among Chinese adults.
Methods
The study was based on the China Health and Retirement Longitudinal Study (CHARLS). A total of 3562 participants with complete information in CHARLS2011 and CHARLS2015 were included, and further divided into the training cohort and the validation cohort by a ratio of 7:3. Univariate and multivariate logistic regression analyses were used to select variables of the nomogram. The nomogram was evaluated by receiver-operating characteristic curve, calibration plots, and decision curve analysis (DCA).
Results
In all, 2494 and 1068 participants were included in the training cohort and the validation cohort, respectively. A total of 413 participants developed CKD in the following 4 years. Five variables selected by multivariate logistic regression were incorporated in the nomogram, consisting of gender, hypertension, the estimated glomerular filtration rate (eGFR), hemoglobin, and Cystatin C. The area under curve was 0.809 and 0.837 in the training cohort and the validation cohort, respectively. The calibration plots showed agreement between the nomogram-predicted probability and the observed probability. DCA indicated that the nomogram had potential clinical use.
Conclusions
A predictive nomogram was established and internally validated in aid of identifying individuals at increased risk of CKD.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic kidney disease (CKD) is irreversible decreased kidney function shown by glomerular filtration rate (GFR) of less than 60 mL/min·1.73 m2, or markers of kidney damage, or both, of at least 3 months duration, regardless of the underlying cause [1]. Global estimated prevalence of CKD was 13.4% (11.7–15.1%) [2]. The prevalence varies within countries, which was reported to be around 11% in high-income countries, including the USA and Australia [1]. A study conducted in China found that the CKD prevalence was 10.8% (10.2–11.3%) among Chinese adults [3]. CKD, raising widespread concerns in recent years, has become a major public health problem across the globe, leading to irreversible nephron loss, end-stage renal disease (ESRD), cardiovascular events, and/or premature death [4]. The global prevalence of CKD is still increasing owing to the rising rates of hypertension, diabetes, obesity, and aging [5].
People usually will not be diagnosed with CKD until severe damages emerge for the lack of obvious clinical symptoms in the early stages of CKD [6]. Patients with CKD are at high risk of poor prognosis and death, since a considerable amount of patients are suffering from hypertension, diabetes, severe electrolyte, or structural abnormalities [7]. To date, the appropriate treatment of older patients with CKD is not clear [4].
Primary risk factors for CKD include aging, blood pressure levels, diabetes status, serum lipid status, obesity, smoking, and alcohol consumption [8,9,10,11]. There are already some prediction models for CKD, mainly applied to the USA or western population [12, 13], which were not suitable for the Chinese population. Reasons for its inappropriateness were threefold: differences between the European ancestry populations and the East Asian ancestry populations due to allelic variation, the varied prevalence of the most common risk factors for CKD, such as older age, hypertension, diabetes, and so on, and the different prevalence of CKD in the US and China [14,15,16,17,18,19]. As for models in China, some models were developed targeting the Chinese population with hypertension or type 2 diabetes mellitus [20, 21]. Chien’s model for the incidence of CKD was limited to its homogeneous participants from one health center with a median 2.2 follow-up years from 2003 to 2007 [22]. Owing to the earth-shaking changes in the economy, drastic alteration in healthy lifestyles, and the emerging environmental problems in the past decades [23, 24], it is indispensable to develop a new prediction model for CKD targeting Chinese adults to identify individuals at high risk for CKD, and then, timely interventions could be carried out. Nomogram has been accepted to be a reliable graphical tool to predict, consisting of a set of scales that each scale represents a characteristic of the study population in recent years [25,26,27], which was convenient to apply for clinicians. Yet, nomogram was rarely utilized to predict the risk of CKD. In the present study, based on the China Health and Retirement Longitudinal Study (CHARLS), we aimed to develop a nomogram to predict the 4-year risk of CKD among Chinese elderly adults.
Materials and methods
The data were obtained from the China Health and Retirement Longitudinal Study (CHARLS), a nationwide study among Chinese adults aged 45 years or older and their spouses. The national baseline survey for the study was conducted between June 2011 and March 2012 (CHARLS2011), and respondents across 150 counties/districts were recruited using a multistage sampling strategy [28]. Detailed information regarding the demographic background and biomedical findings were collected at baseline and each follow-up (every 2 years) using a structured questionnaire. The present study included participants recruited in CHARLS2011 and re-examined in CHARLS2015 where blood sample collections were done.
Variables associated with CKD in previous studies were extracted as follows: age, gender, body mass index (BMI), hypertension, diabetes, stroke, asthma, triglyceride (TG), total cholesterol (TC), low-density lipoprotein cholesterol (LDL), high-density lipoprotein cholesterol (HDL), serum creatinine (SCr), smoking status, drinking status, Cystatin C, hemoglobin, uric acid at baseline, and SCr at follow-up.
Due to the low awareness of CKD [29], the estimated glomerular filtration rate (eGFR) was calculated to accurately estimate the kidney function in the Chinese population using coefficient-modified CKD Epidemiology Collaboration (CKD-EPI) equation from Japanese [30]: eGFR (mL/min/1.73 m2) = 0.813 × 141 × min (SCr/κ, 1)α × max (SCr/κ,1)−1.209 × 0.993Age × 1.021 [if female] × 1.159 [if black], where κ is 0.7 for females and 0.9 for males, α is − 0.329 for females and − 0.411 for males, min indicates the minimum between SCr/κ and 1, and max indicates the maximum between SCr/κ and 1. In the study, individuals with eGFR < 60 mL/min/1.73 m2 can be diagnosed with CKD according to the clinical practice guideline for the evaluation and management of chronic kidney disease [31].
A total of 14,574 participants with two visits in CHARLS 2011 and CHARLS 2015 were originally involved in the study. Participants were excluded for the following reasons: (1) no available information on the variables stated above; (2) extreme BMI values (< 15 kg/m2 or > 55 kg/m2); (3) participants diagnosed with CKD at baseline. Finally, 3562 participants were included in the study.
All participants were randomly divided into the training cohort and the validation cohort by a ratio of 7:3. Descriptive statistics (median, the first quartile, and the third quartile for skewed continuous data, and frequencies and percentages for categorical data) were used to report the baseline demographics and clinical characteristics. Differences between groups were analyzed using Chi-square tests for categorical variables and Wilcoxon rank-sum tests for skewed continuous variables.
Univariate and multivariate logistic regression analyses were used to establish a model for predicting the risk of CKD. The variables with a p value less than 0.1 in the univariate analysis were entered into the stepwise multivariate logistic regression to determine the final risk factors for CKD. The predictive nomogram was constructed based on the final logistic model with the data of the training cohort and externally validated using the data of the validation cohort.
The performance of the nomogram was assessed by the discriminate ability, predictive accuracy, and clinical application value of the model, using a receiver-operating characteristic (ROC) curve, calibration plot, and decision curve analysis. The discriminate ability of the model was determined by the area under the receiver-operating characteristic curve (AUC), which ranged from 0.5 (no discrimination) to 1 (perfect discrimination). The calibration plot describes the degree of fit between the actual risk of CKD and the nomogram-predicted risk of CKD. Decision curve analysis (DCA) was used to assess the utility of the nomogram.
All the statistical analyses were performed with SAS 9.4 statistical software (SAS Institute Inc., Cary, North Carolina) and R version 4.1.0 software (http://www.R-project.org/). The tests were two‐tailed, and p < 0.05 was taken as statistically significant.
Results
A total of 3562 participants (28.97% men and 71.03% women) were included in the study and randomly divided into a training cohort and a validation cohort by a ratio of 7:3. A total of 413 participants developed CKD in the following 4 years. The overall cumulative incidence of CKD was 11.59%. The basic demographics and clinical characteristics of the training cohort and validation cohort are depicted in Table 1. Except for smoking status, there were no statistically significant differences in all the other variables. The training cohort had a higher proportion of smokers.
Table 2 displays the results of the univariate and multivariate logistic regression analysis for risk predictors relevant to incident CKD in the training cohort. In the univariate analysis, age (OR 1.042), hypertension (OR 1.889), total cholesterol (OR 1.004), uric acid (OR 1.365), and Cystatin C (OR 22.828) were positively associated with CKD (p < 0.01), while male (OR 0.315), smoking (OR 0.503), drinking (OR 0.448), eGFR (OR 0.958), and hemoglobin (OR 0.827) were negatively associated with CKD (p < 0.01). These factors were entered in the multivariate stepwise logistic regression analysis. The multivariate analysis showed that male (OR 0.051), hypertension (OR 1.406), eGFR (OR 0.880), hemoglobin (OR 0.840), and Cystatin C (OR 2.478) were associated with CKD (p < 0.001), which were risk predictors in the final model. The VIF values were all < 3, indicating that no collinearity existed among selected variables.
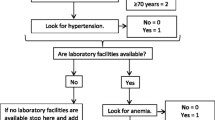
According to the results in Table 2, the final model containing gender, eGFR, hypertension, hemoglobin, and Cystatin C was used to construct a predicting nomogram for the 4-year risk of CKD among Chinese adults. Figure 1 shows the nomogram to predict the incident probability of participants. The total points were related to the risk of CKD.
A constructed nomogram to predict the risk of CKD for participants. Density plots of total points, Cystatin C, Hb, and eGFR showed their distribution. For gender and HTN, the distribution was reflected by the size of the box (the smaller one represented male or Yes and the bigger one represented female or No). Each factor was given a point based on the nomogram. The final total points were obtained by adding the individual score of each of the five risk factors and then obtaining the estimated probability. HTN hypertension, Hb hemoglobin, GFR estimated glomerular filtration rate, CKD chronic kidney disease
Finally, we verified the accuracy of the nomogram. As shown in Fig. 2, AUC in the training cohort and the validation cohort was 0.809 and 0.837 (shown in Fig. 2a and d), respectively. At the best threshold, the specificity and sensitivity rates in the training cohort were 83.1% and 67.9%, respectively. The calibration plots, which examine the consistencies between the nomogram-predicted probability and the observed probability, displayed considerable predictive accuracy of the nomogram to predict CKD in the training cohort (Fig. 2b) and the validation cohort (Fig. 2e). Additionally, DCA, a statistical model to decide whether the prediction model has utility in supporting clinical decisions, showed that the model had potential clinical application value. When the risk threshold ranged from 0.04 to 0.89 in the training cohort (Fig. 2c) and from 0.03 to 0.68 in the validation cohort (Fig. 2f), the nomogram had greater net benefit than either the treat-all-patients strategy or the treat-none strategy.
Evaluation of the nomogram model. (1) Receiver-operating characteristic curve for the nomogram in the training cohort (a) and the validation cohort (d). (2) Nomogram calibration plot in the training cohort (b) and the validation cohort (e). When the solid line (performance nomogram) was closer to the dotted line (ideal model), the prediction accuracy of the nomogram was better. (3) Decision curve analysis for the prediction model in the training cohort (c) and the validation cohort (f). The red solid line is from the prediction model, the gray line is for all participants with CKD, and the solid horizontal line indicates that no participants have CKD. The graph depicts the expected net benefit per patient relative to the nomogram prediction of CKD risk
Discussion
We developed and validated a nomogram for predicting the 4-year risk of CKD among the Chinese adults based on the data from CHARLS 2011 and CHARLS 2015. The model included five variables, containing gender, hypertension, eGFR, hemoglobin, and Cystatin C. The evaluation of the nomogram illustrated that the model performed well and it may be able to help in the prevention of CKD. Any physical examination center could identify participants who are at higher risk for CKD, by the aid of this nomogram, and then make professional suggestions, such as managing blood pressure and anemia, to slow the progression of renal function decline for the participants.
CKD is currently known to be associated with various complications, including cancer, cardiovascular disease, osteoporosis, kidney failure, mortality, and poor quality of life for survivors in general [32,33,34,35,36]. In most recent studies of prediction models for CKD, attention had been given to the progression of CKD [37,38,39,40]. Models for the risk of CKD in the overall general population are relatively few in the last decade. In 2011, Nynke developed a prediction model to identify individuals at increased risk for developing progressive CKD and found that age, urinary albumin excretion, systolic BP, C-reactive protein, and known hypertension were predictors [13]. In 2019, Robert developed a prediction model based on age, sex, race, eGFR, history of cardiovascular disease, ever smoker, hypertension, BMI, and albuminuria concentration [41]. The model was observed to have high discrimination and variable calibration in diverse populations, but they did not conduct a decision curve analysis to evaluate its clinical utility. Lin [20] and Wan [21] developed prediction models for renal disease in Chinese patients with type 2 diabetes mellitus and hypertension, respectively, which were not suitable for the general population. In 2017, Chien developed a point system to estimate chronic kidney disease risk at 4 years [22], with age topping the list. The limitation of the study was the homogeneity of participants, limited to patients in one hospital, and the participants were followed up from 2003 to 2007. In the past 2 decades, with the development of economic and social development, there were dramatic changes in healthy lifestyles of participants, which could potentially impact the prevalence of CKD. Besides, increasing environmental pollution problems deserve attention as well, imposing huge threat on public health, resulting in substantial disease burden in terms of excess number of premature deaths, disability-adjusted life-year loss, and kidney disease [42,43,44]. Under the circumstances, it is imperative to establish the current predictive model of CKD.
Gender was a predictor for CKD. Previous studies indicated that CKD was more common among women than men in most areas [45, 46]. The reasons for this discrepancy across gender may be due in part to gender-related inequities, with more women lacking food, education, or economic power, directly or indirectly impacting the risk for kidney diseases [47]. A review found that women were at higher risk for CKD development in Asia [48], and a cross-sectional study conducted in China revealed that the female gender was significantly associated with low eGFR as well [3]. Our results proved the higher risk of CKD in female again. Since the current medical management of CKD patients was gender-blind [49], it is demanded to bridge the gap aiming at slowing the progression of CKD in women.
Laboratory parameters were often used in the prediction model [50, 51]. Our nomogram included hemoglobin, Cystatin C, and eGFR. It was known that CKD progression contributed to declining hemoglobin [52]. A cohort study concluded that mildly increased hemoglobin was associated with subtle declines in GFR among a population with GFR ≥ 60 mL/min/1.73 m2 [53]. Another study indicated that as GFR decreased, the hemoglobin level climbed and then peaked at an eGFR of 60–89 mL/min/1.73 m2, followed by a decrease at an eGFR of < 60 mL/min/1.73 m2 [54]. In the univariate analysis, hemoglobin concentration was positively associated with CKD. Yet, the association turned negative in the multivariate analysis. Since the VIF values of the multivariate analysis were < 3, no collinearity existed in the final model and the reasons for opposite outcomes remained unclear. Cystatin C was seen as an alternative marker of kidney function apart from creatinine [55, 56]. A study conducted in the USA demonstrated that Cystatin C was greater in CKD groups [57]. In the present study, baseline Cystatin C and creatinine-based GFR were indicators for risk prediction of CKD, consistent with previous research [13, 58].
Hypertension and diabetes mellitus were among well-known causes of CKD [3, 5]. The greater the prevalence of hypertension and diabetes, the larger the amount of CKD patients [59]. Poorly controlled hypertension could lead to renal damage [60]. Two study conducted in China both found that hypertension and diabetes were independently associated with CKD [61, 62]. However, a community-based survey in Taiwan showed that hypertension was not significantly associated with CKD [63]. In the present study, there were significant association between hypertension and CKD. However, we did not found the association between diabetes mellitus and CKD. The results regarding the associations between diabetes mellitus/hypertension and CKD remained controversial among the Chinese population and further studies are required to figure out the actual associations.
Age was a conventional risk factor for CKD in the previous studies. Aging was known as the main risk factor for a sea of diseases, including cancer, impaired cardiovascular health, declining cognitive function, and so on [64,65,66,67]. Chronic kidney disease was no exception, and significant molecular, structural, and functional changes of the kidney were observed among the aging population even without any other chronic diseases [68, 69]. A cohort study found that older age was associated with prevalent CKD [70]. Another study brought age into the prediction model and took age as the biggest risk factor for CKD [22]. However, age was not a predictor for CKD in the final predictive model. In the univariate analysis, age was significantly associated with the risk of CKD, but age was excluded from the final model after applying stepwise multivariate logistic regression.
The nomogram had excellent value in clinical use. First, the nomogram performed well in the light of ROC, the calibration plots, and DCA. Second, the participants in the present study were from a nationally representative longitudinal survey, enabling the model applicable to Chinese populations. Additionally, all variables in the model are easily available as long as participants have done blood routine and liver and renal function tests, which are common and reasonable in regular physical examination. Billions of people across the globe perform a physical exam every year, and they can use the nomogram to predict the risk of CKD. When at higher risk of CKD, participants are supposed to take the first step of health self-management, such as managing blood pressure and anemia, to prevent from developing CKD or slowing renal function decline.
The present study had some limitations. Although CHARLS was a nationwide multi-center study, the study only included 3562 of 14,574 participants, mainly for the lack of key information. A large part of participants being excluded may have biased our findings. In addition, the nomogram was only internally validated, and further studies concerning external validation among other countries are needed.
Conclusions
In conclusion, we constructed and internally validated a nomogram to predict the 4-year risk of CKD among the Chinese elderly population, composed of gender, hypertension, eGFR, hemoglobin, and Cystatin C. The nomogram may be conducive to identifying individuals at increased risk for CKD given its remarkable performance in the evaluation.
Data availability
All data from the CHARLS are publicly available.
References
Webster AC, Nagler EV, Morton RL, Masson P (2017) Chronic kidney disease. Lancet 389:1238–1252. https://doi.org/10.1016/S0140-6736(16)32064-5
Hill NR, Fatoba ST, Oke JL, Hirst JA, O’Callaghan CA, Lasserson DS, Hobbs FDR, Remuzzi G (2016) Global prevalence of chronic kidney disease—a systematic review and meta-analysis. PLoS ONE 11:e158765. https://doi.org/10.1371/journal.pone.0158765
Zhang L, Wang F, Wang L, Wang W, Liu B, Liu J, Chen M, He Q, Liao Y, Yu X, Chen N, Zhang J, Hu Z, Liu F, Hong D, Ma L, Liu H, Zhou X, Chen J, Pan L, Chen W, Wang W, Li X, Wang H (2012) Prevalence of chronic kidney disease in China: a cross-sectional survey. The Lancet 379:815–822. https://doi.org/10.1016/S0140-6736(12)60033-6
Anderson S, Halter JB, Ashworth JR, Clayton CP, Parker RP, Tarver ED, Woolard NF, High KP, Hazzard WR, Himmelfarb J, Mcfarland Horne F, Kaysen GA, Kusek JW, Nayfield SG, Schmader K, Tian Y, Workshop P (2009) Prediction, progression, and outcomes of chronic kidney disease in older adults. J Am Soc Nephrol 20:1199–1209
Lv J, Zhang L, Liu BC, Lan HY, Lv LL (2019) Prevalence and disease burden of chronic kidney disease. Adv Exp Med Biol. https://doi.org/10.1007/978-981-13-8871-2_1
Wang Y, Ma S, Chen Y, Chen L, Liu B, Liu Q, Zhao Y (2019) Chronic kidney disease: biomarker diagnosis to therapeutic targets. Clin Chim Acta 499:54–63. https://doi.org/10.1016/j.cca.2019.08.030
Chen TK, Knicely DH, Grams ME (2019) Chronic kidney disease diagnosis and management: a review. JAMA 322:1294–1304. https://doi.org/10.1001/jama.2019.14745
Pugh D, Gallacher PJ, Dhaun N (2019) Management of hypertension in chronic kidney disease. Drugs 79:365–379. https://doi.org/10.1007/s40265-019-1064-1
Yamagata K, Ishida K, Sairenchi T, Takahashi H, Ohba S, Shiigai T, Narita M, Koyama A (2007) Risk factors for chronic kidney disease in a community-based population: a 10-year follow-up study. Kidney Int 71:159–166. https://doi.org/10.1038/sj.ki.5002017
Jadresic L, Silverwood RJ, Kinra S, Nitsch D (2019) Can childhood obesity influence later chronic kidney disease? Pediatr Nephrol 34:2457–2477. https://doi.org/10.1007/s00467-018-4108-y
Shen Y, Cai R, Sun J, Dong X, Huang R, Tian S, Wang S (2016) Diabetes mellitus as a risk factor for incident chronic kidney disease and end-stage renal disease in women compared with men: a systematic review and meta-analysis. Endocrine 55:66–76. https://doi.org/10.1007/s12020-016-1014-6
Fox CS, Gona P, Larson MG, Selhub J, Tofler G, Hwang SJ, Meigs JB, Levy D, Wang TJ, Jacques PF, Benjamin EJ, Vasan RS (2010) A multi-marker approach to predict incident CKD and microalbuminuria. J Am Soc Nephrol 21:2143–2149. https://doi.org/10.1681/ASN.2010010085
Halbesma N, Jansen DF, Heymans MW, Stolk RP, de Jong PE, Gansevoort RT (2011) Development and validation of a general population renal risk score. Clin J Am Soc Nephrol 6:1731–1738. https://doi.org/10.2215/CJN.08590910
O’Seaghdha CM, Yang Q, Wu H, Hwang S, Fox CS (2012) Performance of a genetic risk score for CKD stage 3 in the general population. Am J Kidney Dis 59:19–24. https://doi.org/10.1053/j.ajkd.2011.08.030
Zheng J, Zhang Y, Rasheed H, Walker V, Sugawara Y, Li J, Leng Y, Elsworth B, Wootton RE, Fang S, Yang Q, Burgess S, Haycock PC, Borges MC, Cho Y, Carnegie R, Howell A, Robinson J, Thomas LF, Brumpton BM, Hveem K, Hallan S, Franceschini N, Morris AP, Köttgen A, Pattaro C, Wuttke M, Yamamoto M, Kashihara N, Akiyama M, Kanai M, Matsuda K, Kamatani Y, Okada Y, Walters R, Millwood IY, Chen Z, Davey Smith G, Barbour S, Yu C, Åsvold BO, Zhang H, Gaunt TR (2021) Trans-ethnic Mendelian-randomization study reveals causal relationships between cardiometabolic factors and chronic kidney disease. Int J Epidemiol 50:1995–2010. https://doi.org/10.1093/ije/dyab203
Bundy JD, Mills KT, Chen J, Li C, Greenland P, He J (2018) Estimating the association of the 2017 and 2014 hypertension guidelines with cardiovascular events and deaths in US adults. Jama Cardiol 3:572. https://doi.org/10.1001/jamacardio.2018.1240
Wang Z, Chen Z, Zhang L, Wang X, Hao G, Zhang Z, Shao L, Tian Y, Dong Y, Zheng C, Wang J, Zhu M, Weintraub WS, Gao R (2018) Status of hypertension in China. Circulation 137:2344–2356. https://doi.org/10.1161/CIRCULATIONAHA.117.032380
Zheng Y, Ley SH, Hu FB (2018) Global aetiology and epidemiology of type 2 diabetes mellitus and its complications. Nat Rev Endocrinol 14:88–98. https://doi.org/10.1038/nrendo.2017.151
Regensteiner JG, Golden S, Huebschmann AG, Barrett-Connor E, Chang AY, Chyun D, Fox CS, Kim C, Mehta N, Reckelhoff JF, Reusch JEB, Rexrode KM, Sumner AE, Welty FK, Wenger NK, Anton B (2015) Sex differences in the cardiovascular consequences of diabetes mellitus. Circulation 132:2424–2447. https://doi.org/10.1161/CIR.0000000000000343
Lin J, Xu R, Yun L, Hou Y, Li C, Lian Y, Zheng F (1993) (2019) A risk prediction model for renal damage in a hypertensive Chinese Han population. Clin Exp Hypertens 41:552–557. https://doi.org/10.1080/10641963.2018.1523913
Wan EYF, Fong DYT, Fung CSC, Yu EYT, Chin WY, Chan AKC, Lam CLK (2017) Prediction of new onset of end stage renal disease in Chinese patients with type 2 diabetes mellitus - a population-based retrospective cohort study. Bmc Nephrol 18:257. https://doi.org/10.1186/s12882-017-0671-x
Chien KMP, Lin HM, Lee BMP, Hsu HP, Lee YMP, Chen MMP (2010) A Prediction model for the risk of incident chronic kidney disease. Am J Med 123:836–846. https://doi.org/10.1016/j.amjmed.2010.05.010
Zhao X, Jiang M, Zhang W (2022) The impact of environmental pollution and economic growth on public health: evidence from China. Front Public Health. https://doi.org/10.3389/fpubh.2022.861157
Chen W, Xia C, Zheng R, Zhou M, Lin C, Zeng H, Zhang S, Wang L, Yang Z, Sun K, Li H, Brown MD, Islami F, Bray F, Jemal A, He J (2019) Disparities by province, age, and sex in site-specific cancer burden attributable to 23 potentially modifiable risk factors in China: a comparative risk assessment. Lancet Glob Health 7:e257–e269. https://doi.org/10.1016/S2214-109X(18)30488-1
Zhang Z, Kattan MW (2017) Drawing nomograms with R: applications to categorical outcome and survival data. Ann Transl Med 5:211. https://doi.org/10.21037/atm.2017.04.01
Huang S, Xie X, Sun Y, Zhang T, Cai Y, Xu X, Li H, Wu S (2020) Development of a nomogram that predicts the risk for coronary atherosclerotic heart disease. Aging (Albany, NY.) 12:9427–9439
Wu J, Zhang H, Li L, Hu M, Chen L, Xu B, Song Q (2020) A nomogram for predicting overall survival in patients with low-grade endometrial stromal sarcoma: a population-based analysis. Cancer Commun 40:301–312. https://doi.org/10.1002/cac2.12067
Zhao Y, Hu Y, Smith JP, Strauss J, Yang G (2014) Cohort profile: the China health and retirement longitudinal study (CHARLS). Int J Epidemiol 43:61–68. https://doi.org/10.1093/ije/dys203
Iroegbu C, Lewis L, Matura LA (2021) An integrative review: chronic kidney disease awareness and the social determinants of health inequities. J Adv Nurs. https://doi.org/10.1111/jan.15107
Horio M, Imai E, Yasuda Y, Watanabe T, Matsuo S (2010) Modification of the CKD epidemiology collaboration (CKD-EPI) equation for Japanese: accuracy and use for population estimates. Am J Kidney Dis 56:32–38. https://doi.org/10.1053/j.ajkd.2010.02.344
KDIGO 2012 clinical practice guideline for the evaluation and management
Malyszko J, Tesarova P, Capasso G, Capasso A (2020) The link between kidney disease and cancer: complications and treatment. Lancet 396:277–287. https://doi.org/10.1016/S0140-6736(20)30540-7
Mok Y, Ballew SH, Matsushita K (2021) Chronic kidney disease measures for cardiovascular risk prediction. Atherosclerosis 335:110–118. https://doi.org/10.1016/j.atherosclerosis.2021.09.007
Gordon PL, Frassetto LA (2010) Management of osteoporosis in CKD Stages 3 to 5. Am J Kidney Dis 55:941–956. https://doi.org/10.1053/j.ajkd.2010.02.338
Gilligan S, Raphael KL (2017) Hyperkalemia and hypokalemia in CKD: prevalence, risk factors, and clinical outcomes. Adv Chron Kidney D 24:315–318. https://doi.org/10.1053/j.ackd.2017.06.004
Bello AK, Alrukhaimi M, Ashuntantang GE, Basnet S, Rotter RC, Douthat WG, Kazancioglu R, Köttgen A, Nangaku M, Powe NR, White SL, Wheeler DC, Moe O (2017) Complications of chronic kidney disease: current state, knowledge gaps, and strategy for action. Kidney Int Suppl 7:122–129. https://doi.org/10.1016/j.kisu.2017.07.007
Xiao J, Ding R, Xu X, Guan H, Feng X, Sun T, Zhu S, Ye Z (2019) Comparison and development of machine learning tools in the prediction of chronic kidney disease progression. J Transl Med 17:119. https://doi.org/10.1186/s12967-019-1860-0
Umesawa M, Sairenchi T, Haruyama Y, Nagao M, Yamagishi K, Irie F, Watanabe H, Kobashi G, Iso H, Ota H (2018) Validity of a risk prediction equation for CKD after 10 years of follow-up in a Japanese population: the Ibaraki prefectural health study. Am J Kidney Dis 71:842–850. https://doi.org/10.1053/j.ajkd.2017.09.013
Tangri NMPF, Inker LAMM, Hiebert BM, Wong JM, Naimark DMMF, Kent DMM, Levey ASM (2016) A dynamic predictive model for progression of CKD. Am J Kidney Dis 69:514–520. https://doi.org/10.1053/j.ajkd.2016.07.030
Tangri N, Stevens LA, Griffith J, Tighiouart H, Djurdjev O, Naimark D, Levin A, Levey AS (2011) A predictive model for progression of chronic kidney disease to kidney failure. JAMA 305:1553–1559. https://doi.org/10.1001/jama.2011.451
Nelson RG, Grams ME, Ballew SH, Sang Y, Azizi F, Chadban SJ, Chaker L, Dunning SC, Fox C, Hirakawa Y, Iseki K, Ix J, Jafar TH, Köttgen A, Naimark DMJ, Ohkubo T, Prescott GJ, Rebholz CM, Sabanayagam C, Sairenchi T, Schöttker B, Shibagaki Y, Tonelli M, Zhang L, Gansevoort RT, Matsushita K, Woodward M, Coresh J, Shalev V, CKD PC, For TCPC, (2019) Development of risk prediction equations for incident chronic kidney disease. JAMA 322:2104–2114. https://doi.org/10.1001/jama.2019.17379
Niu Y, Chen R, Kan H (2017) Air pollution, disease burden, and health economic loss in China. Adv Exp Med Biol 1017:233–242. https://doi.org/10.1007/978-981-10-5657-4_10
Al-Aly Z, Bowe B (2020) Air pollution and kidney disease. Clin J Am Soc Nephro 15:301–303. https://doi.org/10.2215/CJN.16031219
Tsai H, Wu P, Huang J, Chen S (2021) Environmental pollution and chronic kidney disease. Int J Med Sci 18:1121–1129. https://doi.org/10.7150/ijms.51594
Cobo G, Hecking M, Port FK, Exner I, Lindholm B, Stenvinkel P (1979) Carrero JJ (2016) sex and gender differences in chronic kidney disease: progression to end-stage renal disease and haemodialysis. Clin Sci 130:1147–1163. https://doi.org/10.1042/CS20160047
Carrero JJ, Hecking M, Chesnaye NC, Jager KJ (2018) Sex and gender disparities in the epidemiology and outcomes of chronic kidney disease. Nat Rev Nephrol 14:151–164. https://doi.org/10.1038/nrneph.2017.181
García GG, Iyengar A, Kaze F, Kierans C, Padilla-Altamira C, Luyckx VA (2022) Sex and gender differences in chronic kidney disease and access to care around the globe. Semin Nephrol 42:101–113. https://doi.org/10.1016/j.semnephrol.2022.04.001
Carrero J, Hecking M, Ulasi I, Sola L, Thomas B (2017) Chronic kidney disease, gender, and access to care: a global perspective. Semin Nephrol 37:296–308. https://doi.org/10.1016/j.semnephrol.2017.02.009
Brar A, Markell M (2019) Impact of gender and gender disparities in patients with kidney disease. Curr Opin Nephrol Hy 28:178–182. https://doi.org/10.1097/MNH.0000000000000482
Gong P, Zhang X, Gong Y, Liu Y, Wang S, Li Z, Chen W, Zhou F, Zhou J, Jiang T, Zhang Y (2020) A novel nomogram to predict early neurological deterioration in patients with acute ischaemic stroke. Eur J Neurol 27:1996–2005. https://doi.org/10.1111/ene.14333
Yang LB, Xu JY, Tantai XX, Li H, Xiao CL, Yang CF, Zhang H, Dong L, Zhao G (2020) Non-invasive prediction model for high-risk esophageal varices in the Chinese population. World J Gastroenterol 26:2839–2851. https://doi.org/10.3748/wjg.v26.i21.2839
Atkinson MA, Warady BA (2018) Anemia in chronic kidney disease. Pediatr Nephrol 33:227–238. https://doi.org/10.1007/s00467-017-3663-y
Shin N, Kim H, Kim HJ, Han M, Lee S, Jo H, Hyuk H, Chin HJ (2014) A mild decrease of renal function is related to increased hemoglobin level during 5-year follow-up period. Korean J Intern Med 29:341–351. https://doi.org/10.3904/kjim.2014.29.3.341
Han SY, Oh SW, Hong JW, Yi SY, Noh JH, Lee HR, Kim DJ (2016) Association of estimated glomerular filtration rate with hemoglobin level in Korean adults: the 2010–2012 Korea national health and nutrition examination survey. PLoS ONE 11:e150029. https://doi.org/10.1371/journal.pone.0150029
Ferguson TW, Komenda P, Tangri N (2015) Cystatin C as a biomarker for estimating glomerular filtration rate. Curr Opin Nephrol Hy 24:295–300. https://doi.org/10.1097/MNH.0000000000000115
Lassus J, Harjola VP (2012) Cystatin C: a step forward in assessing kidney function and cardiovascular risk. Heart Fail Rev 17:251–261. https://doi.org/10.1007/s10741-011-9242-6
Yassine HN, Trenchevska O, Dong Z, Bashawri Y, Koska J, Reaven PD, Nelson RW, Nedelkov D (2016) The association of plasma cystatin C proteoforms with diabetic chronic kidney disease. Proteome Sci 14:7. https://doi.org/10.1186/s12953-016-0096-7
Jardine MJ, Hata J, Woodward M, Perkovic V, Ninomiya T, Arima H, Zoungas S, Cass A, Patel A, Marre M, Mancia G, Mogensen CE, Poulter N, Chalmers J (2012) Prediction of kidney-related outcomes in patients With Type 2 diabetes. Am J Kidney Dis 60:770–778. https://doi.org/10.1053/j.ajkd.2012.04.025
Kramer H, Soyibo A, Forrester T, Boyne M, Markossian T, Durazo-Arvizu R, Luke A, Cooper R (2018) The burden of chronic kidney disease and its major risk factors in Jamaica. Kidney Int 94:840–842. https://doi.org/10.1016/j.kint.2018.07.025
Tannor EK, Sarfo FS, Mobula LM, Sarfo-Kantanka O, Adu-Gyamfi R, Plange-Rhule J (2019) Prevalence and predictors of chronic kidney disease among Ghanaian patients with hypertension and diabetes mellitus: a multicenter cross-sectional study. J Clin Hypertens 21:1542–1550. https://doi.org/10.1111/jch.13672
Duan J, Wang C, Liu D, Qiao Y, Pan S, Jiang D, Zhao Z, Liang L, Tian F, Yu P, Zhang Y, Zhao H, Liu Z (2019) Prevalence and risk factors of chronic kidney disease and diabetic kidney disease in Chinese rural residents: a cross-sectional survey. Sci Rep 9:10408. https://doi.org/10.1038/s41598-019-46857-7
Ji A, Pan C, Wang H, Jin Z, Lee JH, Wu Q, Jiang Q, Cui L (2019) Prevalence and associated risk factors of chronic kidney disease in an elderly population from eastern China. Int J Env Res Pub He 16:4383. https://doi.org/10.3390/ijerph16224383
Lin MY, Chiu YW, Lee CH, Yu HY, Chen HC, Wu MT, Hwang SJ (2013) Factors associated with CKD in the elderly and nonelderly population. Clin J Am Soc Nephrol 8:33–40. https://doi.org/10.2215/CJN.05600612
Chatsirisupachai K, Palmer D, Ferreira S, Magalhães JP (2019) A human tissue-specific transcriptomic analysis reveals a complex relationship between aging, cancer, and cellular senescence. Aging Cell 18:e13041. https://doi.org/10.1111/acel.13041
Dookun E, Passos JF, Arthur HM, Richardson GD (2020) Therapeutic potential of senolytics in cardiovascular disease. Cardiovasc Drugs Ther. https://doi.org/10.1007/s10557-020-07075-w
Glorioso CA, Pfenning AR, Lee SS, Bennett DA, Sibille EL, Kellis M, Guarente LP (2019) Rate of brain aging and APOE ε4 are synergistic risk factors for Alzheimer’s disease. Life Sci Alliance 2:e201900303
Buendia I, Michalska P, Navarro E, Gameiro I, Egea J, León R (2016) Nrf2-ARE pathway: an emerging target against oxidative stress and neuroinflammation in neurodegenerative diseases. Pharmacol Ther 157:84–104. https://doi.org/10.1016/j.pharmthera.2015.11.003
Hommos MS, Glassock RJ, Rule AD (2017) Structural and functional changes in human kidneys with healthy aging. J Am Soc Nephrol 28:2838–2844. https://doi.org/10.1681/ASN.2017040421
Fang Y, Gong AY, Haller ST, Dworkin LD, Liu Z, Gong R (2020) The ageing kidney: molecular mechanisms and clinical implications. Ageing Res Rev 63:101151. https://doi.org/10.1016/j.arr.2020.101151
Ferguson R, Leatherman S, Fiore M, Minnings K, Mosco M, Kaufman J, Kerns E, Amador JJ, Brooks DR, Fiore M, Parekh RS, Fiore L (2020) Prevalence and risk factors for CKD in the general population of southwestern Nicaragua. J Am Soc Nephrol 31:1585–1593. https://doi.org/10.1681/ASN.2019050521
Acknowledgements
The authors would like to thank the CHARLS team for their hard work and unselfish sharing of survey data.
Funding
This study was funded by The National Key R&D Program of China (2018YFC1311706). The funding body had no roles in study design, data collection and analysis, decision to publish, or preparation of the manuscript.
Author information
Authors and Affiliations
Contributions
LZ, LT, and BP contributed to the study conception and design. LZ, CC, SC, and BP participated to the data cleaning and statistical analysis. LZ drafted the manuscript. BP revised the article. All authors read and proved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that there is no conflict of interest related to this work.
Ethical approval
The Medical Ethics Board Committee of Peking University granted the study an exemption from review, and all the participants provided signed informed consent at the time of participation.
Consent to participate
All participants gave consent.
Consent for publication
Manuscript is approved by all authors for publication.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Zhang, L., Tang, L., Chen, S. et al. A nomogram for predicting the 4-year risk of chronic kidney disease among Chinese elderly adults. Int Urol Nephrol 55, 1609–1617 (2023). https://doi.org/10.1007/s11255-023-03470-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-023-03470-y