Abstract
Purpose
Chronic kidney disease (CKD) patients on long-term dialysis present changes in pulmonary function and respiratory muscle strength, negatively influencing physical capacity.
Objective
To analyze the impact of a continuous positive airway pressure (CPAP) protocol on the respiratory capacity of CKD patients under hemodialysis.
Methods
A randomized clinical trial was conducted involving 40 CKD patients 19–83 years old divided into two groups: control (n = 20) and CPAP (n = 20). Subjects were assessed on the respiratory muscle function test, maximal respiratory pressures, peak flow and 6-min walk test, at baseline and again at the 2-month follow-up. CPAP group patients were submitted to CPAP protocol (PEEP: 5 cm H2O, flow: 15 L/min, FiO2: 33 %) three times per week during hemodialysis sessions.
Results
The CPAP group showed higher forced vital capacity, forced expiratory volume in one second, peak expiratory flow, maximal inspiratory pressure, peak flow, as well as lower systolic blood pressure, heart rate, respiratory rate and Borg scale, in addition to a longer distance travelled on the 6-min walk test, compared with the control group.
Conclusion
The introduction of a CPAP protocol during hemodialysis sessions had a positive impact on pulmonary function and physical capacity in CKD patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Chronic renal disease leads to changes in almost all organic systems. Pulmonary impairment may result directly from circulating uremic toxins or indirectly due to volume overload, anemia, acid–base balance changes and cardiac or musculoskeletal alterations, among others [1–3]. Signs and symptoms may vary according to degree of muscle compromise by reduced caloric-protein intake and deficient metabolism, both of which predominantly affect muscle fibers causing myopathy and muscular atrophy [4].
Patients at advanced stages of chronic kidney disease (CKD) undergoing hemodialysis have low tolerance to exercise and present physical deconditioning. This patient group also exhibits changes in pulmonary mechanics, muscle function and gas exchange [2, 4, 5]. Among other factors, the accumulation of interstitial fluid in the lungs plays an important role in respiratory dysfunction in these patients [1, 4, 6].
The traditional treatment for diseases associated with pulmonary edema is noninvasive ventilation (NIV) in the continuous positive airway pressure (CPAP) modality, aimed at improving ventilation/perfusion ratio and respiratory mechanics [7]. To the best of our knowledge, no protocols using CPAP in patients undergoing HD are available in the literature. Consequently, the impact of this modality of ventilatory support on respiratory function and functional capacity in this patient group remains unknown. This prompted the present study, analyzing the impact of a CPAP-based protocol on respiratory and functional capacity in CKD patients undergoing hemodialysis treatment.
Method
Study design/subjects
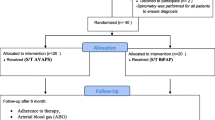
This prospective, consecutive, randomized controlled clinical trial involved clinically diagnosed CKD patients undergoing HD sessions at the Center for Dialysis at a tertiary teaching hospital. This study was previously approved by the Research Ethics Committee of the institution (protocol number 147/09), and the patients signed informed consent forms to participate in the study as summarized in Fig. 1.
Inclusion criteria were patients aged 18 years or older, undergoing HD for at least 6 months and hemodynamically stable. Exclusion criteria were individuals requiring urgent or elective surgical intervention during protocol application, present or past history of pulmonary, cardiac, and subjects with cognitive and/or physical impairments precluding performance of the tests in the assessments. The sample size was calculated for simple random sampling, using a confidence interval of 95 (95 %) and 5 % error for infinite sample.
All patients had been undergoing 4-h HD sessions, three times per week for over 6 months, using a polysulfone membrane (Fresenius) and bath containing sodium (138.0 mEq/L), potassium (2.0 mEq/L), calcium (3.5 mEq/L), magnesium (1.0 mEq/L), chloride (108.5 mEq/L), acetate (3.0 mEq/L) and bicarbonate (32.0 mEq/L).
Participants were randomized into two groups using a series of numbered, sealed, opaque envelopes; each envelope will contain a card stipulating to which group the subject will be allocated: control group (n = 20) and CPAP group (n = 20). Blinding will be maintained in all steps of the research for investigators, assessors and trial participants.
Respiratory evaluations
All evaluations were carried out prior to HD on the second, mid-week HD session. As patients received three HD sessions per week, there was a maximum of two-day interval between HD sessions. Follow-up assessments were performed in both control and CPAP groups after 2 months (when the CPAP group had already finished treatment).
Baseline and follow-up assessments included the following exams: laboratory parameters (Kt/V, hemoglobin, serum albumin and urea); pulmonary function test (PFT), forced vital capacity (FVC), volume expired in 1 s (FEV1), FEV1/FVC, peak expiratory flow (PEF); maximal respiratory pressures evaluating maximal inspiratory pressure and maximal expiratory pressure; peak flow and the 6-min walk test (6MWT).
The maximal respiratory pressures were evaluated with the manometer. Patients were instructed an expiration to residual volume followed by maximum inspiration to evaluate the maximum inspiratory pressure and inspiration to the inspiratory reserve volume followed by an expiration to residual volume to evaluate the maximum expiratory pressure.
For assessment of peak flow, patients were told to inspire deeply and using a nose clip, and expire on a portable device that measures the speed of expiration.
The 6MWT consists of a free walk during 6 min as fast as possible across a flat surfaced 30-m-long corridor graded by meter, including level of effort based on the Borg scale. At completion of the 6 min, the total distance walked was recorded [8].
CPAP protocol
Patients in the study group were submitted to a protocol involving continuous positive airway pressure (CPAP) applied during 24 HD sessions, therefore over a 2-month period. HD sessions were started as per the routine practiced by the sector, and, 1 h into the session, patients were assisted by the physiotherapist on placement of the facemask, which was secured using a head strap. Patients remained on CPAP for 30 min. Air pressure was produced by a flow generator setup with fraction of inspired oxygen (FiO2) at 33 %, continuous flow of 15 L/min and PEEP of 5 cm H2O.
Statistical analysis
Differences between groups were assessed with the unpaired Student’s t test or Mann–Whitney test, when appropriate. The paired Student’s t test was used to compare within-patient variations. Proportions of qualitative variables were compared using the Chi-square test. A p value lower than 5 % (p < 0.05) was considered statistically significant. The Statistical Package for the Social Sciences (version 13.0) statistical software was used for the data analysis.
Results
There were three losses of patients: two of these were from the control group, and they decided to drop out in the final respiratory evaluation. One patient in the treatment group had pneumonia, diagnosed in the third CPAP session, and this individual was excluded because the results in respiratory evaluations would be biased. Therefore, this study was completed with 40 patients, 20 in each group.
The etiology of CKD in the control group was distributed as follows: one case with chronic glomerulonephritis, seven patients with hypertensive nephrosclerosis and two with cystic disease of the kidneys. For the CPAP group, etiologies were as follows: eight cases of chronic glomerulonephritis, nine with hypertensive nephrosclerosis, two with diabetes mellitus and one patient with a tumor process. There was no statistically significant difference in etiology between the two groups.
At baseline assessment, no statistically significant difference between control and CPAP groups was evident for gender, with both groups comprising 55 % women and 45 % men. Similarly, no difference between the groups was found for mean age, height, body mass or time on HD (Table 1).
Groups were compared at baseline and follow-up for the following laboratory parameters: Kt/V, hemoglobin, serum albumin and urea. At baseline, a higher mean creatinine level was observed in the CPAP group, whereas at follow-up, the same group had greater serum albumin levels (Table 2).
On the PFT test, only the parameter PEF showed a statistically significant difference, with the CPAP group having a lower mean value compared with the control group (2.83 ± 0.51 versus 3.43 ± 1.00, respectively; p = 0.03). Conversely, no significant difference was found for baseline maximal respiratory pressures. PEF and 6MWT values between the control group and CPAP group.
Comparing PFT parameters at baseline and follow-up for the two groups revealed a decrease in forced expiratory volume in one second (FEV1) (p = 0.04) in the control group and increased FVC (p < 0.001), FEV1 (p < 0.001) and PEF (p < 0.001) in the CPAP.
Also in the CPAP group, mean maximal pressures and peak flow were increased at follow-up (p < 0.001), as were systolic blood pressure (SBP) (p = 0.01), heart rate (HR), respiratory rate (f) and distance walked (p < 0.001) in the 6MWT.
Comparing control and CPAP groups for values on the PFT revealed a significantly higher values in FVC (p < 0.001), FEV1 (p < 0.001) and PEF (p = 0.01) in the CPAP group. Maximal inspiratory pressure and peak flow were also different (p < 0.001 for both).
The 6MWT revealed a significant decrease in SBP, HR, f and Borg scale ratings as well as an increase in distance walked for the CPAP group after application of the protocol (Table 3).
Discussion
Patients with CKD undergoing HD show a decline in quality of life, with changes in a number of systems including cardiac, respiratory and musculoskeletal systems [1, 2, 8, 9]. The results of the present study showed that utilization of a CPAP program during hemodialysis sessions had a positive impact on pulmonary function and physical capacity among CKD patients.
Analysis of laboratory exams in patients on chronic HD should be carried with caution since variations are influenced by multiple factors resulting from the effect of HD among patients undergoing dialysis for more than 3 months [10–12]. Therefore, changes in serum creatinine and albumin observed in our study should be assessed in conjunction with assessments of nutritional and metabolic status (not performed).
On baseline assessments of the control and CPAP groups, values for the PFT were homogeneous and the reductions seen in FVC, FEV1, FEV1/FVC and PEF were in line with those reported by previous studies in CKD [4, 13, 14]. The PFT test allows the measurement of oxygen uptake capacity and gas exchange potential [15]. Other studies have noted that, although small, the variation in predicted values on spirometry in CKD leads to a significant impact on physical capacity [15, 16], an observation corroborated by the findings of our study.
The changes seen on the physical function and capacity tests indicate that CKD can alter arterial and venous capillaries as well as both enzymatic and mitochondrial activity, thereby affecting normal functioning of the structure of skeletal muscle fibers [17–19], evidenced by the low tolerance to physical activities seen in this patient group [19].
In our study, however, the group submitted to the CPAP program showed a significant increase in values for FVC, FEV and PEF, confirming a positive impact of the treatment. This increase may have been influenced by the CPAP protocol [14], although no similar studies are available in the literature for comparison. Inspired by findings of Siafakas et al. [5] we can say that limitation in airflow and reduced FVC are due to a generalized weakening of respiratory muscle strength and resultant delay in muscle fiber contraction. This clinical picture can be ameliorated through greater tissue oxygen delivery [11, 18] by improving the ventilation/perfusion ratio in patients submitted to NIV [20]. This was evidenced by higher FVC after treatment in our study.
Dujić et al. [6] also observed reductions in FEV, correlating these with reversible obstruction of the small airways and with air trapping caused by early closure of the bronchioles and bronchi due to fluid accumulation proximal to distal small airways. Our study showed this effect to be positively influenced by CPAP, owing to the greater recruitment of alveoli attained utilizing PEEP [7], and the procedure helps in reducing interstitial pulmonary edema [21, 22].
The impact of CKD in HD patients on the endothelium of pulmonary capillaries is an increase in permeability leading to interstitial edema and increased resistance of the airways, contributing to dyspnea and low capacity for physical exercise, as seen in these patients, given that progressive effort requires higher maximal oxygen consumption (VO2) [23].
Peak VO2 of patients on dialysis is approximately half the expected value for healthy sedentary individuals [24]. Although maximal oxygen consumption (maxVO2) was not directly assessed in our study, we noted a difference in performance on the 6MWT between baseline and follow-up assessments for control and CPAP groups. The 6MWT can be used as a proxy of maxVO2 with distance walked being positively correlated with maxVO2 values [24, 25].
Mehta and Hill (2001), studying the effects of NIV, confirmed reductions in cardiac pre- and after-loads as well as lower auto-PEEP among patients with hyperinflation, and optimization in respiratory effort [26], even when ventilation was applied for short periods [20]. With our protocol, patients remained under positive pressure for only 30 min per session yet showed improved PFT performance and maximal inspiratory pressure and peak flow values. This created favorable conditions for improvement in respiratory muscle strength through the ventilatory support by CPAP, and this strength is severely impaired in CKD due to changes in oxygen transport, extraction and consumption that trigger metabolic processes detrimental to ideal tensions for oxygenation of muscle fibers, particularly types I and II [1, 4, 12, 27, 28].
Maximal respiratory pressures and peak flow readings serve as an indicator of muscle strength behavior in patients under HD and invariably show lower values in CKD patients compared with expected values for age-matched healthy individuals [12, 29]. It is likely that the increased maximal inspiratory pressure and peak flow observed in our study were attributable to an increase in mitochondrial structures which were less impacted by the typical HD-related hypoxia [30–32] during the treatment period.
Variation in distance walked on the 6MWT is considered a valuable marker, since it is tightly correlated with morbidity and mortality in chronic diseases such as cardiac insufficiency [24, 33, 34]. A longer distance walked in the test is associated with lower morbidity [25, 35] and indirectly shows the beneficial effects of CPAC protocol, which has led to an increase in distance walked by patients from the CPAP group.
The 6MWT, in addition to measuring distance, also assesses blood pressure, heart rate, respiratory frequency, peripheral oxygen saturation and Borg rating (perceived exertion scale) [26]. Therefore, it constitutes an objective measure, verifying the positive impact of the therapeutic protocol. Besides the greater distance walked, the CPAP group also showed a significant decrease in HR, f and Borg scale ratings, with CPAP patients reporting lower levels of perceived exertion and fatigue.
The CPAP protocol had a positive impact on CKD patients undergoing HD and can be used as an instrument in physiotherapy for optimizing HD and providing patients with functional benefits.
Clinically, the method could still be reproduced during hemodialysis sessions by bringing the positive impact of improved physical performance that influence on implementing of routine every day activities of patients with CKD in addition to low cost and protocol security while the patient is this in renal unit optimizing the routine treatment that usually leads to physical disability of the patients.
References
Viana J, Kosmadakis GC, Watson EL, Bevington A, Feehally J, Bishop NC et al (2014) Evidence for anti-inflammatory effects of exercise in CKD. J Am Soc Nephrol 25:1–10
Gómez-Fernández P, Sánchez Agudo L, Calatrava JM, Escuin F, Selgas R, Martínez ME et al (1984) Respiratory muscle weakness in uremic patients under continuous ambulatory peritoneal dialysis. Nephron 36(4):219–223
Heiwe S, Jacobson SH (2011) Exercise training for adults with chronic kidney disease (Review). The Cochrane Collaboration 1–396
Pierson DJ (2006) Respiratory considerations in patient with renal failure. Respir Care 51(4):413–422
Siafakas NM, Argyrakopoulos T, Andreopoulos K, Tsoukalas G, Tzanakis N, Bouros D (1995) Respiratory muscle strength during continuous ambulatory peritoneal dialysis (CAPD). Eur Respir J 8(1):109–113
Dujic Z, Tocilj J, Ljutic D, Eterovic D (1991) Effects of hemodialysis and anemia on pulmonary diffusing capacity. Membrane diffusing capacity and capillary blood volume in uremic patients. Respiration 58:277–281
Huff JS, Whelan TV (1994) CPAP as adjunctive treatment of severe pulmonary edema in patients with ESRD. Am J Emerg Med 12:388–392
ATS Committee on Proficiency Standards for Clinical Pulmonary Function Laboratories (2002) ATS statement: guidelines for the six-minute walk test. Am J Respir Crit Care Med 166(1):111–117
Grassmann A, Gioberge S, Moeller S, Brown G (2005) ESRD patients in 2004: global overview of patient numbers treatment modalities and associated trends. Nephrol Dial Transplant 20:2587–2593
Zoccali C, Tripepi R, Torino C, Bellantoni M, Tripepi G, Mallamaci F (2013) Lung congestion as a risk factor in end-stage renal disease. Blood Purif 36:184–191
Palamidas AF, Gennimata SA, Karakontaki F, Kaltsakas F, Kaltsakas G, Papantoniou I et al (2014) Impact of hemodialysis on dyspnea and lung function in end stage kidney disease patients. Biomed Res Int 2014:212751
Adams GR, Vaziri ND (2006) Skeletal muscle dysfunction in chronic renal failure: effects of exercise. Am J Physiol Renal Physiol 290(4):753–761
Karacan Ö, Tutal E, Çolak T, Sezer S, Eyüboglu FÖ, Haberal M (2006) Pulmonary function in renal transplant recipients and end-stage renal disease patients undergoing maintenance dialysis. Transpl Proc 38:396–404
Karacan O, Tutal E, Uyar M, Eyüboğlu FO, Sezer S, Ozdemir FN (2004) Pulmonary function in uremic patients on long-term hemodialysis. Ren Fail 26(3):273–278
Tovbin D, Heimer D, Mashal A, Degtyar P, Avnon LS (2001) Intradialytic hypercapnic respiratory failure managed by noninvasive assisted ventilation. Am J Nephrol 21:383–385
Bush A, Gabriel R (1991) Pulmonary function in chronic renal failure: effects of dialysis and transplantation. Thorax 46:424–428
Kirkman DL, Roberts LD, Kelm M, Wagner J, Jibani MM, Macdonald JH (2013) Interaction between intradialytic exercise and hemodialysis adequacy. Am J Nephrol 38:475–482
Cupisti A, Licitra R, Chisari C, Stampacchia G, D’Alessandro C, Galetta F et al (2004) Skeletal muscle and nutritional assessment in chronic renal failure patients on a protein-restricted diet. J Intern Med 255:115–124
Clanton TL, Dixon GF, Drake J, Gadek JE (1985) Effects of breathing pattern on inspiratory muscle endurance in humans. J Appl Physiol 59(6):1834–1841
Wilson SH, Cooke NT, Edwards RH et al (1984) Predicted normal values for maximal respiratory pressures in caucasian adults and children. Thorax 39:535–538
Fu C, Caruso P, Lucato JJ, Souza R, Schettino GPP, Carvalho CRR (2005) Comparison of two flow generators with a noninvasive ventilator to deliver continuous positive airway pressure: a test lung study. Intensive Care Med 31:1587–1591
Koyner JL, Murray P (2010) Mechanical ventilation and the kidney. Blood Purif 29:52–68
Marquez JM, Douglas ME, Downs JB, Wu WH, Mantini EL, Kuck EJ et al (1979) Renal function and cardiovascular responses during positive airway pressure. Anesthesiology 50(5):393–398
Segura-Orti E (2010) Ejercicio en pacientes en hemodiálisis: revisión sistemática de la literatura. Nefrologia 30:236–246
Cahalin LP, Mathier MA, Semigran MJ, Dec GW, DiSalvo TG (1996) The six-minute walk test predicts peak oxygen uptake and survival in patients with advanced heart failure. Chest 10:325–332
Bersten AD, Holt AW, Vedig AE, Skowronski GA, Baggoley CJ (1991) Treatment of severe cardiogenic pulmonary edema with continuous positive airway pressure delivered by face mask. N Engl J Med 325(26):1825–1830
Mehta S, Hill NS (2001) Noninvasive ventilation. Am J Respir Crit Care Med 163:540–577
Bavbek N, Akay H, Uz B, Turgut F, Kanbay M, Senes M et al (2010) The effects of L-carnitine therapy on respiratory function test in chronic hemodialysis patients. Ren Fail 32:157–161
Koufaki P, Mercer TH, Naish PF (2002) Effects of exercise training on aerobic and functional capacity of end-stage renal disease patients. Clin Physiol Funct Imaging 22(2):115–124
Kemp GJ, Crowe AV, Anijeet HK, Gong QY, Bimson WE, Frostick SP et al (2004) Abnormal mitochondrial function and muscle wasting but normal contractile efficiency in haemodialysed patients studied non-invasively in vivo. Nephrol Dial Transplant 19:1520–1527
Schiffl H, Lang SM, Fischer R (2002) Daily hemodialysis and the outcome of acute renal failure. N Engl J Med 346:305–310
Rahgoshai R, Rahgoshai R, Khrosraviani AAN, Solouki M (2010) Acute effects hemodialysis on pulmonary patients with end-stage renal disease. IJKD 4:214–217
Neylon M, Marshall JM, Johns EJ (1997) The effects of chronic hypoxia on renal function in the rat. J Physiol 501(Pt 1):243–250
Enright PL, McBurnie MA, Bitter V, Tracy RP, McNamara R, Arnold A, Newman AB (2003) Cardiovascular Health Study: the 6-min walk test: a quick measure of functional status in elderly adults. Chest 123(2):387–398
Johansen KL, Painter P (2012) Exercise in individuals with CKD. Am J Kidney Dis 59:126–134
Conflict of interest
None.
Author information
Authors and Affiliations
Corresponding author
Additional information
Study conducted at: Dialysis Unit, Santa Casa de Misericórdia de São Paulo, São Paulo (SP)/Brazil.
Rights and permissions
About this article
Cite this article
Xavier, V.B., Roxo, R.S., Miorin, L.A. et al. Impact of continuous positive airway pressure (CPAP) on the respiratory capacity of chronic kidney disease patients under hemodialysis treatment. Int Urol Nephrol 47, 1011–1016 (2015). https://doi.org/10.1007/s11255-015-0988-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11255-015-0988-y