Abstract
Previous studies reported that microRNA-1298 was abnormally expressed in the myocardium of rat hearts after hypoxia/normoxia injury. This study aims to investigate the function and specific mechanism of miR-1298 in myocardial ischemia/reperfusion (IR) injury. Neonatal rat cardiomyocytes (NRCMs) were isolated from neonatal rat hearts and subjected to oxygen/glucose deprivation/reperfusion (OGD/R) to induce I/R injury. The rat model with I/R injury was induced by ligating the proximal left anterior descending artery (LAD). MiR-1298 expression was detected by qRT-PCR. The levels of PP2A, Bcl-2, Bax, and AMPK signaling members (p-AMPK, p-GSK3β) was detected by Western blot. Cell apoptosis was evaluated by TUNEL staining assay and flow cytometry. The infarct size of rat hearts was assessed by TTC staining assay. Premature and mature MiR-1298 were significantly downregulated while PP2A was significantly upregulated during I/R injury both in vitro and in vivo. The prediction of Starbase suggested that PP2A was a potential target of miR-1298. MiR-1298 overexpression significantly reduced cardiomyocyte apoptosis in vitro, and its protective effect was obviously attenuated by PP2A overexpression. Luciferase reporter assay showed that miR-1298 targeted PP2A directly. In addition, miR-1298 overexpression significantly reduced infarct size and cardiomyocyte apoptosis in the hearts of rats received with I/R injury in vivo. Moreover, miR-1298 overexpression significantly elevated the levels of Bcl-2 and AMPK signaling members (p-AMPK, p-GSK3β) while decreased Bax level, and these effects were partially reversed by PP2A overexpression. MiR-1298 participated in myocardial I/R injury by targeting the PP2A/AMPK/GSK3β signaling pathway, suggesting that miR-1298 might be a potential therapeutic target for myocardial I/R injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Highlights
-
MiR-1298 overexpression significantly increased the levels of p-AMPK, p-GSK3β, and Bcl-2.
-
MiR-1298 overexpression decreased Bax level.
-
PP2A overexpression reversed the effects of MiR-1298.
-
MiR-1298 affected the development of myocardial I/R injury by inhibiting PP2A-mediated activation of the AMPK/GSK3β signaling pathway.
-
MiR-1298 might be a potential therapeutic target for myocardial I/R injury.
Introduction
Acute myocardial infarction has become a major leading cause of death and disability worldwide [1]. Recently, timely myocardial reperfusion is the effective therapeutic strategy for reducing acute myocardial ischemic injury and limiting myocardial infarct size [2]. However, ischemia–reperfusion (I/R) may cause serious clinical manifestations, including myocardial hibernation, acute heart failure, cerebral dysfunction, gastrointestinal dysfunction, systemic inflammatory response syndrome, and multiple organ dysfunction syndrome [3]. One of the common pathological characteristics caused by I/R injury is myocardial apoptosis [4], which has become a promising therapeutic target for myocardial I/R injury [5]. Therefore, identifying effective targets that are closely involved in myocardial apoptosis might help develop new therapeutic strategies for myocardial I/R injury.
MicroRNAs (miRNAs) have emerged as a class of small endogenous RNAs with approximately 19 to 25 nucleotides in length, regulating post-transcriptional silencing of target genes [6, 7]. Increasing evidences have demonstrated that miRNAs participate in numerous biological processes such as cell invasion, migration, apoptosis, and differentiation [8]. More and more miRNAs have been observed to be abnormally expressed and associated with myocardial apoptosis during myocardial I/R injury [9], suggesting the essential involvement of miRNAs in the development of myocardial I/R injury. For example, miR-145 protects against myocardial I/R injury by modulating CaMKII-mediated anti-apoptotic and anti-inflammatory pathways [10]. miR-138 attenuates myocardial I/R injury via inhibiting mitochondria-mediated apoptosis by directly targeting HIF1-alpha [11]. MiR-24-3p reduced cardiomyocyte apoptosis during I/R injury by regulating Keap1-Nrf2 signaling pathway [12]. MiR-1298 is a newly identified miRNA that is significantly associated with the malignant phenotypes of tumor cells [13, 14]. Recently, miR-1298 is found to be abnormally expressed in the myocardium of rat hearts during hypoxia/normoxia injury [15], suggesting that miR-1298 may be potentially involved in the development of myocardial I/R injury.
AMP-activated protein kinase (AMPK) is a widely distributed, highly conserved hetero-trimetric complex consisted of a catalytic α (62KDa) subunit and non-catalytic β and γ subunits, which are responsible for regulating its kinase activity, enzyme stability, and localization [16]. AMPK plays a major role in regulating cellular energy balance. Its activation attenuates MI/R injury and improves cardiac performance [17, 18]. AMPK could phosphorylate glycogen synthase kinase-3 beta (GSK3β), leading to nuclear accumulation of Nrf2, a key antioxidant transcription factor in maintaining cellular redox homeostasis [19, 20]. Protein phosphatase 2A (PP2A) is a serine/threonine phosphatase and functions as an antagonist of many signaling pathways involved in cell growth, proliferation, and apoptosis [21]. Zhong et al. found that PP2A effectively inhibited AMPK activation by downregulating AMPK phosphorylation [22], suggested that PP2A might also be associated with the development of myocardial I/R injury.
In the present study, we demonstrated that miR-1298 was significantly downregulated during myocardial I/R injury both in vitro and in vivo. MiR-1298 overexpression effectively reduced apoptosis of OGD/R-treated NRCMs in vitro and myocardial apoptosis and infarct size of hearts of I/R-stimulated rats. Meanwhile, the inhibitory effect of miR-1298 overexpression on cell apoptosis in vitro was attenuated by PP2A overexpression. In addition, miR-1298 overexpression significantly activated AMPK and GSK3β signaling by inhibiting PP2A. Taken together, our results revealed a novel function of the miR-1298/PP2A/AMPK-GSK3β signaling pathway in myocardial I/R injury and contributed to our understanding of the pathogenesis of myocardial I/R injury and developing new therapeutic strategies for diseases caused by myocardial I/R injury.
Materials and methods
Experimental animals
All Sprague Dawley (SD) rats were purchased from Shanghai Experimental Animal Center of Chinese Academy of Sciences and adaptively kept at specific pathogen‐free (SPF) conditions for 5 days before the experimental procedure. Of them, neonatal SD rats of < 3 days old were used to isolate neonatal rat cardiomyocytes (NRCMs) and neonatal SD rats of 3 months old were used to establish the in vivo animal model. All animal experiments were approved by the Animal Research Ethics Committee of Peking University Shenzhen Hospital.
Cell culture and the construction of oxygen/glucose deprivation/reperfusion (OGD/R) model
NRCMs were isolated from 3-day-old neonatal SD rats as previously described [23]. NRCMs were cultured in Dulbecco’s modified Eagle’s media (DMEM; GIBCO, Grand Island, NY, USA) supplemented with 10% fetal bovine serum (FBS, GIBCO, Grand Island, NY, USA) at 37 °C with 5% CO2. To mimic the ischemia–reperfusion (I/R) injury in vivo, NRCMs were cultured in serum-free DMEM medium in a hypoxic incubator (95% N2 and 5% CO2) for 4 h. Afterward, cells were cultured in fresh media with 10% FBS in an incubator with 5% CO2 for different times (4, 12, 24, 48, and 72 h) for re-oxygenation to establish the cardiomyocyte OGD/R model.
Cell transfection
miR-1298 (GenBank No.: rnomiR-1298, NR_031850) mimics and inhibitor, as well as their corresponding negative controls (NC-mimics and NC-inhibitor) were designed and synthesized by GenePharma Co. Ltd. The sequences were miR-1298 mimics sense 5′-UUCAUUCGGCUGUCCAGAUGUA-3′ and antisense 5′-CAUCUG GACAGCCGAAUGAAUU-3′; miR-1298 inhibitor 5′-UACAUCUGGACAGCCGA AUGAA-3′; NC-inhibitor 5′-CAGUACUUUUGUGUAGUACAA-3′; NC mimic: 5′-UUCUCCGAACGUGUCACGUTTA-3′; and miR-1298-TSB: 5′-AAGTAAGCCGAC AGGTCTACAT-3′. To overexpress PP2A, the full length of PP2A was amplified and cloned into pcDNA3.1 expression vector to generate PP2A-OS. 100 nM mimics/inhibitor, 100 nM NC-mimics/inhibitor or 10 ng plasmid were transfected into NRCMs using Lipofectamine 2000 (Thermo Fisher) according to the manufacturer’s instructions. All transfected cells were cultured for 48 h followed by OGD/R treatment for 12 h.
Flow cytometry
The apoptotic rate of NRCMs with different treatments was detected using Annexin V/Propidium Iodide (PI) Apoptosis Detection Kit (BD, San Jose, CA) following the manufacturer’s instructions. Briefly, approximately 5 × 104 cells were collected, washed twice with PBS, and subjected to Annexin V-FITC/PI double staining at room temperature for 20 min in the dark. The percentage of apoptotic NRCMs was analyzed by flow cytometry (BD Bioscience, San Jose, CA).
Animal model
SD rats were randomly divided into four groups: Sham group (Sham-operated rats), I/R group, I/R + NC mimics, and I/R + miR-1298 mimics (n = 6 in each group). For the transfection of miR-1298 mimic/NC-mimics in vivo, 5 mg miR-1298 mimic/NC mimics was mixed with 8 mL Entranster™ in vivo reagent (Engreen Biosystem, Beijing, China) and hydrated with PBS at a final concentration of 50 mg/mL. When the rat chest was opened, the miR-1298 mimic/NC mimics complex was equally injected into the myocardium of the left ventricle anterior wall. After 48 h for injection, rats were subjected to in vivo ischemia–reperfusion (I/R) treatment or sham operation followed by reperfusion for 24 h. The I/R treatment in vivo ischemia–reperfusion (I/R) model was constructed by ligating the proximal left anterior descending artery (LAD) as previously described [24]. Briefly, after anesthesia by intraperitoneally injecting 300 mg/kg chloral hydrate, a left thoracotomy was performed, and myocardial ischemia was induced for 45 min using a 5–0 polypropylene suture with a medical latex tube placed between the ligature and the LAD. Ischemic injury was confirmed by balanced regional color and weakened regional contraction. Sham-operated rats underwent the same procedures without ligating the LAD. Then the latex tube was removed to restore coronary circulation for 12, 24, 48, 72, or 96 h. After that, rats were anesthetized. After measuring their cardiac blood flow parameters, rats were sacrificed by cervical dislocation and the hearts were collected for the subsequent experiments.
Color Doppler echocardiography
After anesthesia, cardiac blood flow parameters of rats from different groups including left ventricular end-diastolic dimension (LVEDD), left ventricular end-systolic diameter (LVESD), left ventricular ejection fraction (LVEF), left ventricular fraction shortening (LVFS), left ventricular systolic pressure (LVSP), and left ventricular end-diastolic pressure (LVEDP) were detected using ultrasound Doppler examination as previously described [25].
Cell apoptosis
Cardiomyocyte apoptosis in the heart tissues or NRCMs was evaluated by terminal deoxynucleotidyl transferase-mediated dUTP nick end labeling (TUNEL) assay according to the instructions of the in situ cell death detection kit (Roche, Indianapolis, IN) as previously described [26, 27]. Briefly, in vivo, the hearts of different groups were embedded in paraffin and cut into 5 μm thick sections. The sections were stained with TUNEL reaction mixture for 60 min and then immersed into 4’,6-diamidino2-phenylindole (DAPI; Sigma-Aldrich) to stain nuclei for 30 min. In vitro, NRCMs received different treatments were fixed in 4% paraformaldehyde and stained with TUNEL reaction mixture for 60 min followed by DAPI for 30 min. TUNEL-positive (green) and DAPI-positive (blue) staining patterns in six randomly selected fields (× 200 magnification) were observed under a fluorescence microscope (Olympus IX71; Olympus Corporation, Tokyo, Japan). The apoptosis index was calculated as TUNEL-positive cells/total cells × 100%.
Detection of myocardial infarct size
For myocardial infarct size evaluation, the heart tissues were embedded in paraffin and cut into 1 mm thick sections. The sections were incubated with 1% 2, 3,5-triphenyl tetrazolium chloride (TTC, TGC, Shanghai, China) at 37 °C for 15 min. The infarct area (INF, pale white) and the area at risk (AAR, brick red) were detected using Image-Pro Plus 6.0 software, and the infarct size was calculated as INF/AAR × 100%.
RNA isolation and qRT-PCR
Total RNA of the cultured NRCMs or heart tissues was extracted using TRIzol Reagent (Life Technologies). To measure PP2A expression, RNA was reversely transcribed into cDNA using a Prime Script TM RT Reagent kit (Takara Biotechnology) and subjected to PCR reaction using SYBR Green Master Mix kit (Takara, Japan) on an ABI 7500 system (Applied Biosystems, USA). The levels of mature and premature miR-1298 were determined using All-in-One™ miRNA qRT-PCR Reagent Kits (Genecopoeia). Prior to the analysis of mature miR-1298 expression, addition of poly (A) was first performed. Mature miR-1298 level was determined using poly (T) as reverse the primer while premature miR-1298 level analyzed using sequence-specific primers. β-actin and U6 were used as the internal references for mRNAs and miRNA, respectively. The primers used for qRT-PCR were PP2A forward 5′-CATCCCTGGGG TTGACAAGAA-3′ and reverse 5′-TTTGTGCCCCTAAGCTGGG-3′, miR-1298 forward 5′-TTCGGCTGTCCAGATGTACC-3′ and reverse 5′-GCGAAAAGTTCAA TCAGTTGCC-3′, U6 forward 5′-GCTTCGGCACATATACTAAAAT-3′ and reverse 5′-CGCTTCACGAATTTGCGTGTCAT-3′, and β-actin forward 5′-CCCAGCACAA TGAAGATCAAGATCAT-3′ and reverse 5′-ATCTGCTGGAAGGTGTACAGCGA-3′. The relative expression changes of targets were calculated using the 2−ΔΔCt method.
Western blot
Total protein samples of cells or heart tissues were extracted using RIPA lysis buffer (Solarbio, Beijing, China). A total of 50 μg of proteins were separated by 12% SDS-PAGE and transferred onto polyvinylidene fluoride (PVDF) membranes (Millipore, USA). After blocking in 5% non-fat milk, the membranes were incubated with primary antibodies at 4 °C overnight. On the next day, the membranes were incubated with horseradish peroxidase-conjugated second antibody for 2 h at room temperature. The blots were visualized using an enhanced chemiluminescence kit (Thermo, Fisher Scientific) and the comparison of gray value was determined by ImageJ software. These primary antibodies included anti-PP2A (ab32104, 1:1000, Abcam, USA), anti-p-AMPK (ab133448, 1:1000, Abcam, USA), anti-AMPK (ab32047, 1:1000, Abcam, USA), anti-p-GSK3β (ab75814, 1:1000, Abcam, USA), anti-GSK3β (ab32391, 1:1000, Abcam, USA), anti-Bax (ab32503, 1:1000, Abcam, USA), anti-cleaved-caspase 3 (ab32042, 1:1000, Abcam, USA), and anti-β-actin (internal reference, ab179467, 1:10,000, Abcam, USA).
Luciferase reporter assay
The sequence of PP2A was obtained from Pubmed (https://www.ncbi.nlm.nih.gov/pubmed). HEK293T cell line was purchased from American Type Culture Collection (Manassas, VA, USA) and cultured in DMEM media with 10% FBS. The 3′ UTR sequences of PP2A with wild-type or mutated miR-1298 binding sites were subcloned into the pGL3 vector (#E1751, Promega, WI, USA) and named as PP2A-wt and PP2A-mut, separately. The PP2A-wt /PP2A-mut plasmid and miR-1298 mimics/negative control were co-transfected into HEK293T cells using Lipofectamine 2000 (#11668019, Invitrogen, CA, USA) according to the manufacturer’s protocol. Subsequently, cells were transfected with 0.1 μg PRL-TK (TK-driven Renilla luciferase expression vector) as an internal control. Luciferase activities were measured with a dual-luciferase reporter assay kit (#E1910, Promega, WI, USA) 48 h after transfection.
In situ hybridization
Whole-mount in situ hybridization (WIMISH) was performed as previously described. T7 labeled-full length miR-1298 cDNA was purchased from Invitrogen (CA, USA). Antisense probe for miR-1298 was made with fluorescence-labeled UTPs (Roche, Basel, Switzerland) using T7 labeled-full length cDNA as templates for RNA synthesis with T7 RNA polymerases (Takara). The stained rat hearts were dehydrated in glycerol and photographed with a Nikon SMZ1500 stereomicroscope (Nikon, Tokyo, Japan).
Statistical analysis
All data were analyzed using SPSS 18.0 software (SPSS, Inc., Chicago, IL, USA) and presented as mean ± standard deviation (mean ± SD). Differences between two groups were analyzed using two-tailed Student’s t-test and among multiple groups were tested using one-way analysis of variance (ANOVA). A p < 0.05 was considered statistically significant.
Results
MiR-1298 was downregulated, and PP2A was upregulated in NRCMs with I/R injury
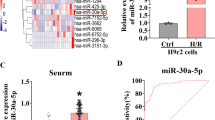
To explore the function of miR-1298 in myocardial I/R injury, we first detected the levels of premature and mature miR-1298 during I/R injury. The results indicated that both premature and mature miR-1298 were significantly downregulated in NRCMs after OGD/R treatment for 12, 24, 48 and 72 h except for 4 h compared with NRCMs without any treatment (p < 0.05, Fig. 1A and suppl Fig. 1A). Moreover, the levels of premature and mature miR-1298 were also significantly downregulated in heart tissues of rats that received I/R induction at different time points except for 12 h (p < 0.05, Fig. 1B and suppl Fig. 1B). In situ hybridization analysis also showed that miR-1298 was downregulated in heart tissues of rats that received I/R induction (suppl Fig. 3). To further investigate the specific mechanism of miR-1298 during I/R injury, the target genes of miR-1298 were predicted by Starbase 3.0 and the prediction showed that PP2A might be a potential target of miR-1298 (Fig. 1C). Then we extracted total RNA and protein samples from NRCMs after OGD/R for 12 h and from heart tissues of rats after I/R treatment for 24 h and detected PP2A expression. We found that PP2A expression was significantly upregulated in both OGD/R-treated NRCMs (p < 0.05, Fig. 1D and E) and heart tissues of I/R induced rats (p < 0.01, Fig. 1F and G). These results confirmed that miR-1298 might be closely associated with I/R injury.
MiR-1298 was downregulated and PP2A was upregulated in NRCMs with I/R injury. A NRCMs were treated with OGD/R for different times, and the expression of miR-1298 was detected by qRT-PCR. B Rats were treated with I/R for different times, and the expression of miR-1298 in heart tissues was detected by qRT-PCR (n = 6 in each group). C The putative binding site between miR-1298 and PP2A was predicted by Starbase. D, E NRCMs were treated with OGD/R for 12 h, the expression of PP2A was detected by qRT-PCR (D) and Western blot (E). F, G Rats were treated with I/R for 24 h, and the expression of PP2Ain heart tissues was detected by qRT-PCR (F) and Western blot (G) (n = 6 in each group). I/R = ischemia followed by reperfusion, OGD/R = oxygen/glucose deprivation followed by reperfusion. Each experiment was repeated for three times. *P < 0.05, **P < 0.01, ***P < 0.001 vs control group
MiR-1298 overexpression attenuated apoptosis of OGD/R-simulated NRCMs
To further determine the role of mIR-1298 during I/R injury, NRCMs were transfected with miR-1298 mimics to overexpress miR-1298 and miR-1298 inhibitor to block its expression. The transfection efficiency was evaluated by qRT-PCR and the results showed that miR-1298 expression was significantly enhanced in NRCMs by miR-1298 mimic transfection (p < 0.001) and decreased by miR-1298 inhibitor transfection (p < 0.001, Fig. 2A). There was no obvious change in miR-1298 expression between the NC mimics + NC inhibitor group and the control group (Fig. 2A). As expected, miR-1298 overexpression inhibited PP2A expression (p < 0.01) while miR-1298 suppression upregulated PP2A (p < 0.01, Fig. 2B and C) in NRCMs. To further explore the effect of miR-1298 on I/R injury-induced cell apoptosis, NRCMs were transfected with miR-1298 mimics/inhibitor or negative control followed by OGD/R treatment for 12 h. We found that compared with the OGD/R treatment group, TUNEL-positive cells were significantly decreased in the miR-1298 mimics-transfected NRCMs (p < 0.05) while markedly increased in miR-1298 inhibitor-transfected NRCMs (p < 0.05, Fig. 3A and B). Similarly, flow cytometry analysis of apoptosis revealed that miR-1298 overexpression significantly decreased the apoptotic rate of OGD/R-treated NRCMs (p < 0.05) while miR-1298 downregulation obviously enhanced the apoptotic rate of OGD/R-treated NRCMs (p < 0.05, Fig. 3C and D). In addition, we found that miR-1298 overexpression significantly increased Bcl-2 expression (p < 0.01) while decreased the levels of Bax and c-caspase-3 in OGD/R-treated NRCMs (p < 0.05). By contrast, miR-1298 downregulation exhibited an opposite effect on the expression of apoptosis-related proteins (p < 0.05, Fig. 3E and F). These results indicated that miR1298 overexpression effectively inhibited OGD/R-simulated NRCMs apoptosis in vitro and miR-1298 might affect I/R injury through modulating cell apoptosis.
PP2A expression was affected by transfection of miR-1298 mimic or inhibitor into NRCMs. NRCMs were transfected with miR-1298 mimics/inhibitor or negative controls. A The expression of miR-1298 was detected by qRT-PCR. B, C The expression of PP2A was detected by qRT-PCR (B) and Western blot (C). Each experiment was repeated three times. **P < 0.01, ***P < 0.001 vs control or NC mimics + NC inhibitor group. No mark indicates no significant difference
MiR1298 overexpression effectively inhibited OGD/R-simulated NRCMs apoptosis in vitro. NRCMs were transfected with miR-1298 mimics/inhibitor or negative control followed by OGD/R treatment for 12 h. A Representative microphotographs of NRCMs stained by TUNEL (green = TUNEL-positive cells). B Percentage of TUNEL-positive NRCMs. C NRCM apoptosis was detected by flow cytometry. D Quantitative analysis of flow cytometry. E The levels of Bax, c-caspase-3 and Bcl-2 were detected by Western blot. F Quantitative analysis of Western blot. Each experiment was repeated three times. *P < 0.05, **P < 0.01 vs OGD/R or OGD/R + NC group. No mark indicates no significant difference
MiR-1298 overexpression reduced apoptosis of OGD/R simulated NRCMs by activating PP2A/AMPK/GSK3β signaling pathway
To further determine whether the effect of miR-1298 was mediated by PP2A, PP2A was overexpressed in miR-1298 mimics-transfected NRCMs by transfecting pcDNA3.1-PP2A (PP2A-OS). The results of qRT-PCR (Fig. 4A) and Western blot (Fig. 4B) indicated that miR-1298 overexpression significantly decreased PP2A expression in OGD/R treated NRCMs (p < 0.01) while co-transfection of miR-1298 mimics and PP2A-OS markedly reversed the inhibitory effect of miR-1298 mimics on PP2A expression (p < 0.001). Meanwhile, miR-1298 overexpression significantly decreased the apoptosis rate of OGD/R-treated NRCMs (p < 0.05), and co-transfection of miR-1298 mimics and PP2A-OS enhanced the apoptosis rate compared with miR-1298 mimics group in OGD/R-treated NRCMs (p < 0.05, Fig. 4C). Similarly, miR-1298 overexpression significantly elevated Bcl-2 level while decreased Bax and c-caspase-3 levels in OGD/R-treated NRCMs (p < 0.05). Moreover, these effects were obviously reversed by co-transfection of miR-1298 mimics and PP2A-OS (p < 0.01, Fig. 4E). In addition, we investigated the effects of miR-1298 on AMPK/GSK3β signaling and found that miR-1298 overexpression significantly increased the levels of phosphorylated-AMPK (p-AMPK) and phosphorylated-GSK3β (p-GSK3β) in OGD/R-treated NRCMs (p < 0.01), while the elevations of p-AMPK and p-GSK3β were attenuated by co-transfection of miR-1298 mimics and PP2A-OS (p < 0.01, Fig. 4E). Luciferase assay showed that miR-1298 could directly target PP2A (Fig. 3A, B). We also performed the target site blocker (TSB) assay to block the binding site of miR-1298 on PP2A. The results indicated that after transfecting TSB, miR-1298 overexpression failed to inhibit PP2A expression and the apoptosis of OGD/R-treated NRCMs (suppl Fig. 2). To explore whether miR-1298 targeted PP2A directly, luciferase reporter assay was performed in cells co-transfected with miR-1298 mimic and 3’ UTR sequence of PP2A with wild-type or and mutated miR-1298 binding sites. The results suggested that miR-1298 targeted PP2A directly (Fig. 5A, B). Together, these results suggested that miR-1298 overexpression reduced apoptosis of OGD/R-simulated NRCMs by activating PP2A/AMPK/GSK3β signaling pathways.
MiR-1298 overexpression reduced apoptosis of OGD/R-simulated NRCMs by activating PP2A/AMPK/GSK3β signaling pathway. NRCMs were transfected with miR-1298 mimics/NC or co-transfected with miR-1298 mimics and PP2A-OS (PP2A overexpression plasmid). Then cells were treated with OGD/R for 12 h. A, B PP2A expression was detected by qRT-PCR (A) and Western blot (B). C Cell apoptosis was evaluated by flow cytometry. D The levels of Bax, c-caspase-3 and Bcl-2 were detected by Western blot. E The levels of PP2A and AMPK pathway members (p-AMPK, AMPK, p-GSK3β, and GSK3β) were detected by Western blot. Each experiment was repeated three times. *P < 0.05, **P < 0.01 vs OGD/R or OGD/R + NC group; #P < 0.05, ##P < 0.01, ###P < 0.001 vs OGD/R + miR-1298 mimic group. No mark indicates no significant difference
MiR-1298 overexpression improved I/R injury in vivo
To confirm the role of miR-1298 in I/R injury, rats were injected with miR-1298 mimics or NC mimics, and then stimulated by I/R for 24 h. The results of color Doppler echocardiography showed that LVEDD, LVESD, and LVEDP were greatly enlarged in the rats received with I/R treatment compared with that of the sham group (p < 0.05). By contrast, LVED, LVFS, and LVSP were significantly decreased in the rats received with I/R treatment compared with that of the sham group (p < 0.05). Furthermore, these damages induced by I/R treatment were obviously attenuated by injecting miR-1298 mimics compared with injecting NC mimics (p < 0.05, Fig. 6A–F). Myocardial infarct size was also evaluated, and the results indicated that I/R treatment significantly increased infract size of rats compared to the sham treatment (p < 0.001). Moreover, miR-1298 overexpression obviously decreased the I/R-induced infarct size compared with NC mimics (p < 0.001, Fig. 6G and H). Meanwhile, the apoptosis of myocardial cells in heart tissues was detected by TUNEL staining, and the results revealed that I/R treatment significantly enhanced the apoptosis of myocardial cells compared with sham treatment (p < 0.001), and miR-1298 overexpression decreased apoptosis of myocardial cells in the heart tissues of I/R rats compared with NC mimics (p < 0.001, Fig. 6I and J). These results indicated that miR-1298 overexpression effectively improved I/R injury in vivo.
MiR-1298 overexpression improved I/R injury in vivo. Rats were injected with miR-1298 mimics or NC mimics, and then treated with I/R for 24 h. A–F The LVEDD (A), LVESD (B), LVEF (C), LVFS (D), LVSP (E), and LVEDP (F) were assessed by color Doppler echocardiography. G The representative images of TTC staining in heart tissues of rats. H Infarct size was evaluated by Image-Pro Plus 6.0 software. I The apoptosis of myocardial cells in heart tissues was detected by TUNEL staining. J Quantitative analysis of TUNEL staining. n = 6 in each group. Each experiment was repeated for four times. *P < 0.05, **P < 0.01, and ***P < 0.001 vs Sham group; #P < 0.05, ##P < 0.01, ###P < 0.001 vs I/R + NC mimics group
MiR-1298 overexpression inhibited anti-apoptotic capacity of the heart by activating AMPK signaling pathway in vivo
We also detected the changes of proteins in AMPK signaling pathway in vivo. The results showed that I/R treatment significantly decreased the levels of p-AMPK, p-GSK3β, and Bcl-2, while increased the level of Bax in heart tissues of rats (p < 0.05). Moreover, miR-1298 overexpression obviously elevated the levels of p-AMPK, p-GSK3β, and Bcl-2, while decreased Bax level in the heart tissues of rats treated by I/R compared with NC mimics (p < 0.05, Fig. 7A–E). These results revealed that miR-1298 overexpression effectively reduced the apoptosis of myocardial cells in rat heart by activating AMPK signaling pathway in vivo.
MiR-1298 overexpression inhibited heart apoptosis by activating AMPK signaling pathway in vivo. Rats were injected with miR-1298 mimics or NC mimics, and then treated with I/R for 24 h. A The levels of AMPK signaling pathway-related proteins were detected by Western blot. B–E Quantitative analysis of p-AMPK (B), p-GSK3β (C), Bcl-2 (D), and Bax (E). n = 6 in each group. Each experiment was repeated four times. *P < 0.05, **P < 0.01 vs Sham group; ##P < 0.01, ###P < 0.001 vs I/R + NC mimics group
Discussion
Ischemia–reperfusion (I/R) injury can cause structural and functional damages at the cellular, tissue, and organ levels and even result in cell death [28]. Apoptosis is the main leading cause of cell death following I/R injury [29]. Hence, identifying potential targets involved in cell apoptosis is urgent to protect against myocardial I/R injury. In this study, we demonstrated that miR-1298 protected against myocardial I/R injury via reducing myocardial apoptosis through regulating PP2A/AMPK-GSK3β signaling pathway.
In the past decades, a series of miRNAs involved in the development of myocardial I/R injury have been found and studied in detail, and some of them are considered promising diagnostic and therapeutic targets [30, 31]. MiR-1298, a newly identified miRNA, has been reported to be closely associated with the malignant phenotypes of different types of tumor cells. For example, mIR-1298 expression was downregulated in gastric cancer tissues and cell lines, and miR-1298 overexpression inhibited cell proliferation and invasion capacity of gastric cancer cells [13]. MiR-1298 expression was significantly downregulated in bladder cancer tissues, and miR-1298 overexpression inhibited cell proliferation, migration, and invasiveness of two bladder cancer cell lines by targeting connexin 43 (Cx43) [32]. MiR-1298 was downregulated in non-small cell lung cancer and suppresses tumor progression [14]. In addition, miR-1298 was also significantly downregulated in the neocortex of 12 patients with mesial temporal lobe epilepsy and negatively correlated with the age of patients [33]. These reports suggest that miR-1298 may play a potential protective role in human diseases. Previous studies have reported that miR1298 was abnormally expressed in the myocardium of rat hearts after hypoxia/normoxia injury [15]. However, its specific function in regulating myocardial ischemia/reperfusion (IR) injury remains unclear. In this study, we found that miR-1298 was significantly downregulated in OGD/R-treated NRCMs and the heart tissues of I/R-stimulated rats. Moreover, miR-1298 overexpression effectively improved I/R injury by reducing myocardial apoptosis. Our study revealed a new myocardial protective role of miR-1298 in I/R injury.
MiRNAs have been found to play regulatory functions in human diseases by directly binding to the 3′ UTR (untranslated regions) of target mRNAs as competitive endogenous RNA (ceRNA) to inhibit their transcription [34]. Here, to explore the specific mechanism of miR-1298, we predicted the potential targets of miR-1298 using Starbase. The prediction revealed a putative binding site between miR-1298 and the 3′ UTR of PP2A. PP2A has been shown to regulate vital cellular processes, including cell cycle, growth, metabolism, and apoptosis. PP2A dysregulation is observed in many diseases such as neurodegenerative disorders, cardiovascular pathologies, and cancers [35]. Meanwhile, PP2A functions as a direct target of miRNAs to participate in the development of human diseases, such as miR-21 in nonalcoholic fatty liver [36], miR-19b in non-small cell lung cancer [37], and miR-155 in systemic lupus erythematosus [38]. One previous study found that PP2A expression was markedly upregulated in the infarct area of rats after ischemia [39]. However, the specific roles and regulatory axis in I/R myocardial injury have not been well studied. Here, our results confirmed that PP2A was significantly upregulated in OGD/R-treated NRCMs and heart tissues of rats after I/R stimulation and PP2A expression was negatively regulated by miR-1298. Moreover, the protective effect of miR-1298 overexpression on apoptosis of OGD/R-treated NRCMs was partially eliminated by PP2A overexpression.
Previous studies demonstrated that AMPK activation effectively improves cardiac functions and attenuates I/R injury by reducing myocardial apoptosis [40]. The crucial involvement of AMPK in cardioprotection has been persistently confirmed by the severe heart contractile dysfunction under AMPK inactivation or deletion [41]. Bcl-2 and Bax are two crucial apoptotic factors in the Bcl-2 family and are classified into two groups based on their functions and structures: Bcl-2 is an anti-apoptotic factor while Bax is a pro-apoptotic factor [42]. Abnormal expression of Bax and Bcl-2 is closely associated with cell apoptosis during myocardial dysfunction [43]. In the present study, we demonstrated that miR-1298 overexpression significantly increased p-AMPK, p-GSK3β, and Bcl-2 levels while decreased Bax level, and these effects were obviously reversed by PP2A overexpression. These results revealed that miR-1298 affected the development of myocardial I/R injury through inhibiting PP2A followed by the activation of AMPK/GSK3β signaling pathway.
Conclusion
Our study demonstrated that miR-1298 overexpression attenuated myocardial I/R injury by targeting PP2A and activating AMPK signaling pathway, suggesting that miR-1298 might be a potential therapeutic target for myocardial I/R injury.
Data availability
The data that support the findings of this study are not publicly available due to their containing information that could compromise the privacy of research participants but are available on request from the corresponding author.
References
Toldo S, Mauro AG, Cutter Z et al (2018) Inflammasome, pyroptosis, and cytokines in myocardial ischemia-reperfusion injury. Am J Physiol Heart Circ Physiol 315(6):H1553–H1568. https://doi.org/10.1152/ajpheart.00158.2018
Hausenloy DJ, Yellon DM (2013) Myocardial ischemia-reperfusion injury: a neglected therapeutic target. J Clin Investig 123(1):92–100. https://doi.org/10.1172/jci62874
Wu MY, Yiang GT, Liao WT et al (2018) Current mechanistic concepts in ischemia and reperfusion injury. Cell Physiol Biochem 46(4):1650–1667. https://doi.org/10.1159/000489241
Burke AP, Virmani R (2007) Pathophysiology of acute myocardial infarction. Med Clin North Am 91(4):553–572. https://doi.org/10.1016/j.mcna.2007.03.005
Dong Y, Chen H, Gao J et al (2019) Molecular machinery and interplay of apoptosis and autophagy in coronary heart disease. J Mol Cell Cardiol 136:27–41. https://doi.org/10.1016/j.yjmcc.2019.09.001
Lu TX, Rothenberg ME (2018) MicroRNA. J Allergy Clin Immunol 141(4):1202–1207. https://doi.org/10.1016/j.jaci.2017.08.034
Mohr AM, Mott JL (2015) Overview of microRNA biology. Semin Liver Dis 35(1):3–11. https://doi.org/10.1055/s-0034-1397344
Chen C, Zhou Y, Wang J et al (2018) Dysregulated MicroRNA involvement in multiple sclerosis by induction of T helper 17 cell differentiation. Front Immunol 9:1256. https://doi.org/10.3389/fimmu.2018.01256
Ong SB, Katwadi K, Kwek XY et al (2018) Non-coding RNAs as therapeutic targets for preventing myocardial ischemia-reperfusion injury. Expert Opin Ther Targets 22(3):247–261. https://doi.org/10.1080/14728222.2018.1439015
Liu Z, Tao B, Fan S et al (2019) MicroRNA-145 protects against myocardial ischemia reperfusion injury via CaMKII-mediated antiapoptotic and anti-inflammatory pathways. Oxid Med Cell Longev 2019:8948657. https://doi.org/10.1155/2019/8948657
Liu Y, Zou J, Liu X et al (2019) MicroRNA-138 attenuates myocardial ischemia reperfusion injury through inhibiting mitochondria-mediated apoptosis by targeting HIF1-α. Exp Ther Med 18(5):3325–3332. https://doi.org/10.3892/etm.2019.7976
Xiao X, Lu Z, Lin V (2018) MicroRNA miR-24-3p reduces apoptosis and regulates keap1-Nrf2 pathway in mouse cardiomyocytes responding to ischemia/reperfusion injury. Oxid Med Cell Longev 2018:7042105. https://doi.org/10.1155/2018/7042105
Qiu ZK, Liu N, Zhao SF et al (2018) MiR-1298 expression correlates with prognosis and inhibits cell proliferation and invasion of gastric cancer. Eur Rev Med Pharmacol Sci 22(6):1672–1679. https://doi.org/10.26355/eurrev_201803_14579
Du Z, Wu J, Wang J et al (2019) MicroRNA-1298 is downregulated in non-small cell lung cancer and suppresses tumor progression in tumor cells. Diagn Pathol 14(1):132. https://doi.org/10.1186/s13000-019-0911-4
Joshi SR, Dhagia V, Gairhe S et al (2016) MicroRNA-140 is elevated and mitofusin-1 is downregulated in the right ventricle of the Sugen5416/hypoxia/normoxia model of pulmonary arterial hypertension. Am J Physiol Heart Circ Physiol 311(3):H689-698. https://doi.org/10.1152/ajpheart.00264.2016
Young LH (2009) A crystallized view of AMPK activation. Cell Metab 10(1):5–6. https://doi.org/10.1016/j.cmet.2009.06.008
Morrison A, Chen L, Wang J et al (2015) Sestrin2 promotes LKB1-mediated AMPK activation in the ischemic heart. FASEB J 29(2):408–417. https://doi.org/10.1096/fj.14-258814
Wang J, Yang L, Rezaie AR et al (2011) Activated protein C protects against myocardial ischemic/reperfusion injury through AMP-activated protein kinase signaling. J Thrombosis Haemostasis: JTH 9(7):1308–1317. https://doi.org/10.1111/j.1538-7836.2011.04331.x
Jain AK, Jaiswal AK (2007) GSK-3beta acts upstream of Fyn kinase in regulation of nuclear export and degradation of NF-E2 related factor 2. J Biol Chem 282(22):16502–16510. https://doi.org/10.1074/jbc.M611336200
Salazar M, Rojo AI, Velasco D et al (2006) Glycogen synthase kinase-3beta inhibits the xenobiotic and antioxidant cell response by direct phosphorylation and nuclear exclusion of the transcription factor Nrf2. J Biol Chem 281(21):14841–14851. https://doi.org/10.1074/jbc.M513737200
Kauko O, Westermarck J (2018) Non-genomic mechanisms of protein phosphatase 2A (PP2A) regulation in cancer. Int J Biochem Cell Biol 96:157–164. https://doi.org/10.1016/j.biocel.2018.01.005
Zhong Y, Tian F, Ma H et al (2020) FTY720 induces ferroptosis and autophagy via PP2A/AMPK pathway in multiple myeloma cells. Life Sci 260:118077. https://doi.org/10.1016/j.lfs.2020.118077
Wang JX, Jiao JQ, Li Q et al (2011) miR-499 regulates mitochondrial dynamics by targeting calcineurin and dynamin-related protein-1. Nat Med 17(1):71–78. https://doi.org/10.1038/nm.2282
Li YM, Sun JG, Hu LH et al (2019) Propofol-mediated cardioprotection dependent of microRNA-451/HMGB1 against myocardial ischemia-reperfusion injury. J Cell Physiol 234(12):23289–23301. https://doi.org/10.1002/jcp.28897
Tan H, Qi J, Fan BY et al (2018) MicroRNA-24-3p attenuates myocardial ischemia/reperfusion injury by suppressing RIPK1 expression in mice. Cell Physiol Biochem 51(1):46–62. https://doi.org/10.1159/000495161
Zhang W, Li Y, Wang P (2018) Long non-coding RNA-ROR aggravates myocardial ischemia/reperfusion injury. Braz J Med Biol Res 51(6):6555. https://doi.org/10.1590/1414-431x20186555
Li B, Tao Y, Huang Q (2015) Effect and mechanism of miR-126 in myocardial ischemia reperfusion. Genet Mole Res 14(4):18990–18998. https://doi.org/10.4238/2015.December.29.6
Kalogeris T, Baines CP, Krenz M et al (2016) Ischemia/reperfusion. Compr Physiol 7(1):113–170. https://doi.org/10.1002/cphy.c160006
Wu D, Wang J, Wang H et al (2017) Protective roles of bioactive peptides during ischemia-reperfusion injury: from bench to bedside. Life Sci 180:83–92. https://doi.org/10.1016/j.lfs.2017.05.014
Fan ZX, Yang J (2015) The role of microRNAs in regulating myocardial ischemia reperfusion injury. Saudi Med J 36(7):787–793. https://doi.org/10.15537/smj.2015.7.11089
Makhdoumi P, Roohbakhsh A, Karimi G (2016) MicroRNAs regulate mitochondrial apoptotic pathway in myocardial ischemia-reperfusion-injury. Biomed Pharmacother 84:1635–1644. https://doi.org/10.1016/j.biopha.2016.10.073
Li G, Sun L, Mu Z et al (2020) MicroRNA-1298–5p inhibits cell proliferation and the invasiveness of bladder cancer cells via down-regulation of connexin 43. Biochem Cell Biol 98(2):227–237. https://doi.org/10.1139/bcb-2019-0137
Organista-Juárez D, Jiménez A, Rocha L et al (2019) Differential expression of miR-34a, 451, 1260, 1275 and 1298 in the neocortex of patients with mesial temporal lobe epilepsy. Epilepsy Res 157:106188. https://doi.org/10.1016/j.eplepsyres.2019.106188
Thomson DW, Dinger ME (2016) Endogenous microRNA sponges: evidence and controversy. Nat Rev Genet 17(5):272–283. https://doi.org/10.1038/nrg.2016.20
O’Connor CM, Perl A, Leonard D et al (2018) Therapeutic targeting of PP2A. Int J Biochem Cell Biol 96:182–193. https://doi.org/10.1016/j.biocel.2017.10.008
Albadrani M, Seth RK, Sarkar S et al (2019) Exogenous PP2A inhibitor exacerbates the progression of nonalcoholic fatty liver disease via NOX2-dependent activation of miR21. Am J Physiol Gastrointest Liver Physiol 317(4):G408-g428. https://doi.org/10.1152/ajpgi.00061.2019
Baumgartner U, Berger F, HashemiGheinani A et al (2018) miR-19b enhances proliferation and apoptosis resistance via the EGFR signaling pathway by targeting PP2A and BIM in non-small cell lung cancer. Mol Cancer 17(1):44. https://doi.org/10.1186/s12943-018-0781-5
Lashine YA, Salah S, Aboelenein HR et al (2015) Correcting the expression of miRNA-155 represses PP2Ac and enhances the release of IL-2 in PBMCs of juvenile SLE patients. Lupus 24(3):240–247. https://doi.org/10.1177/0961203314552117
Penna C, Tullio F, Perrelli MG et al (2011) Ischemia/reperfusion injury is increased and cardioprotection by a postconditioning protocol is lost as cardiac hypertrophy develops in nandrolone treated rats. Basic Res Cardiol 106(3):409–420. https://doi.org/10.1007/s00395-010-0143-y
Potenza MA, Sgarra L, Nacci C et al (2019) Activation of AMPK/SIRT1 axis is required for adiponectin-mediated preconditioning on myocardial ischemia-reperfusion (I/R) injury in rats. PLoS ONE 14(1):e0210654. https://doi.org/10.1371/journal.pone.0210654
Russell RR 3rd, Li J, Coven DL et al (2004) AMP-activated protein kinase mediates ischemic glucose uptake and prevents postischemic cardiac dysfunction, apoptosis, and injury. J Clin Investig 114(4):495–503. https://doi.org/10.1172/jci19297
Edlich F (2018) BCL-2 proteins and apoptosis: recent insights and unknowns. Biochem Biophys Res Commun 500(1):26–34. https://doi.org/10.1016/j.bbrc.2017.06.190
Biala AK, Kirshenbaum LA (2014) The interplay between cell death signaling pathways in the heart. Trends Cardiovasc Med 24(8):325–331. https://doi.org/10.1016/j.tcm.2014.08.002
Funding
This work was supported by Shenzhen Scientific Innovation Committee (Grant No. JCYJ20170412150405310) and Shenzhen Municipal Health and Family Planning Commission (Grant No. SZFZ2018071).
Author information
Authors and Affiliations
Contributions
CO, ZH: study concepts, literature research, clinical studies, data analysis, experimental studies, manuscript writing and review; MR: study design, literature research, experimental studies and manuscript editing; LH: definition of intellectual content, clinical studies, data acquisition and statistical analysis; XY: data acquisition, manuscript preparation and data analysis. All authors have read and approve the submission of the manuscript.
Corresponding authors
Ethics declarations
Conflict of interest
All other authors declare that we have no conflicts of interest and do not have any commercial or associative interest that represents a conflict of interest in connection with the work submitted.
Ethical approval
All procedures were approved by the Animal Research Ethics Committee of Peking University Shenzhen Hospital. Procedures operated in this research were completed in keeping with the standards set out in the Announcement of Helsinki and Laboratory Guidelines of Research in China.
Consent to participate
Informed consent was obtained from all individual participants.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
11239_2021_2540_MOESM1_ESM.tif
Supplementary file1 Mature miR-1298 was downregulated in NRCMs with I/R injury. (A) NRCMs were treated with OGD/R for different times, and the expression of mature-miR-1298 was detected by qRT-PCR. (B) Rats were treated with I/R for different times, and the expression of mature-miR-1298 in heart tissues was detected by qRT-PCR (n =6 in each group). Each experiment was repeated 3 times. * P < 0.05, ** P < 0.01, *** P < 0.001 (TIF 6257 kb)
11239_2021_2540_MOESM2_ESM.tif
Supplementary file2 MiR-1298 mostly functions towards PP2A in regulating myocardial ischemia-reperfusion injury. (A) MiR-1298-TSB blocked the inhibiting function of miR-1298 on PP2A expression. (B-D) MiR-1298-TSB blocked the inhibitory effect of miR-1298 on cell apoptosis. Each experiment was repeated 3 times. * P < 0.05, ** P < 0.01, *** P < 0.001 (TIF 3572 kb)
11239_2021_2540_MOESM3_ESM.tif
Supplementary file3 MiR-1298 expression in the rat myocardial cells was downregulated after IR injury. MiR-1298 was expressed both in the plasma and nucleus of rat myocardial cells (TIF 4714 kb)
Rights and permissions
About this article
Cite this article
Ouyang, C., Huang, L., Ye, X. et al. Overexpression of miR-1298 attenuates myocardial ischemia–reperfusion injury by targeting PP2A. J Thromb Thrombolysis 53, 136–148 (2022). https://doi.org/10.1007/s11239-021-02540-1
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11239-021-02540-1