Abstract
Lupinus albus seeds contain conglutin gamma (Cγ) protein, which exerts a hypoglycemic effect and positively modifies proteins involved in glucose homeostasis. Cγ could potentially be used to manage patients with impaired glucose metabolism, but there remains a need to evaluate its effects on hepatic glucose production. The present study aimed to analyze G6pc, Fbp1, and Pck1 gene expressions in two experimental animal models of impaired glucose metabolism. We also evaluated hepatic and renal tissue integrity following Cγ treatment. To generate an insulin resistance model, male Wistar rats were provided 30% sucrose solution ad libitum for 20 weeks. To generate a type 2 diabetes model (STZ), five-day-old rats were intraperitoneally injected with streptozotocin (150 mg/kg). Each animal model was randomized into three subgroups that received the following oral treatments daily for one week: 0.9% w/v NaCl (vehicle; IR-Ctrl and STZ-Ctrl); metformin 300 mg/kg (IR-Met and STZ-Met); and Cγ 150 mg/kg (IR-Cγ and STZ-Cγ). Biochemical parameters were assessed pre- and post-treatment using colorimetric or enzymatic methods. We also performed histological analysis of hepatic and renal tissue. G6pc, Fbp1, and Pck1 gene expressions were quantified using real-time PCR. No histological changes were observed in any group. Post-treatment G6pc gene expression was decreased in the IR-Cγ and STZ-Cγ groups. Post-treatment Fbp1 and Pck1 gene expressions were reduced in the IR-Cγ group but increased in STZ-Cγ animals. Overall, these findings suggest that Cγ is involved in reducing hepatic glucose production, mainly through G6pc inhibition in impaired glucose metabolism disorders.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lupin seeds have high protein content (35–45% of protein), specially the domesticated species such as L. albus, L. angustifolius, and L. luteus, making them a useful protein source for enriched food products, such as bread, pasta, crisps, and cakes [1–3]. Lupin protein consumption has favorable effects on lipid and carbohydrate metabolism and, thus, enriching foods with lupin flour may promote cardiovascular benefits [4]. Consumption of lupin protein positively regulates plasma LDL cholesterol [5], confers protection against hepatic steatosis development [6], and lowers serum cholesterol in vivo [7]. However, the hypocholesterolemic effects of lupin proteins may be slightly reduced by thermal treatment [8].
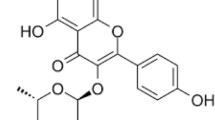
Lupin consumption also has hypoglycemic effects that have been proven in vitro, in vivo, and in clinical trials, and that are reportedly conferred by the protein conglutin gamma (Cγ) [9, 10]. Cγ is a glycoprotein with a relative mass of ~50 kDa, which comprises two subunits of 17 and 29 kDa [1]. It is suggested that Cγ has insulin-mimetic activity, allowing it to activate kinases involved in the insulin signaling pathway, promote GLUT4 translocation, participate in muscle cell differentiation, and increase HepG2 cell glucose consumption [11, 12]. Moreover, Cγ reportedly increases the pancreatic insulin content in beta cells and the Ins-1 gene expression in an animal model of type two diabetes mellitus (T2D) [13]. Based on these hypoglycemic effects, Cγ represents an alternative for glucose level control in impaired glucose metabolism disorders, such as metabolic syndrome and T2D [11].
To better understand the mechanism of action of Cγ, we must evaluate its effects on key enzymes of glucose hepatic production as a target for glucose homeostasis. The present study aimed to evaluate the effects of Cγ on the gene expressions of glucose-6-phosphatase (G6pc), fructose-bisphosphatase 1 (Fbp1), and phosphoenolpyruvate carboxykinase 1 (Pck1) in experimental models of IR and T2D. We additionally evaluated the histological changes in hepatic and renal tissue.
Materials and Methods
Plant Material
Lupin albus seeds were provided by E. van Santen (College of Agriculture, Auburn University, Alabama, USA).
Cγ Purification and Characterization by PAGE
Dehulled Lupin albus seeds were ground to obtain flour, which was then defatted using hexane. Cγ protein was extracted following a previously described method [13, 14]. First, we added double-distilled water (ddH2O) to the lupin flour to separate the albumin fraction. This solution was stirred for 2 h at 4°C and then centrifuged, and the supernatant was removed. The pellet was resuspended in 10% NaCl solution (pH 7), stirred for 12 h at 4°C, and then centrifuged at 8000 rpm for 30 min at 4°C. The supernatant was recovered (globulins fraction), precipitated with 85% saturated ammonium sulfate, and then centrifuged under the above-described conditions. The pellet was dissolved in 0.1 M phosphate buffer (pH 6.8), dialyzed for 18 h in 0.2 M acetate buffer (pH 4.8), and centrifuged. The resulting conglutin α pellet was discarded, and the supernatant was dialyzed for 48 h against ddH2O at 4°C. Finally, the solution was centrifuged and the Cγ-containing supernatant was lyophilized at −50°C, 0.040 mbar, for 8 h (Freeze Drying 4.5, LABCONCO).
Cγ Characterization by SDS-PAGE
The extracted Cγ was evaluated by 12% SDS-polyacrylamide gel electrophoresis (SDS-PAGE) [15]. The protein samples (2 μg) were mixed with Laemmli sample buffer (Bio-Rad, Milan, Italy) with and without 1% ß-mercaptoethanol (denaturing and non-denaturing conditions, respectively). These samples were incubated at 90°C for 2 min, and then centrifuged at 10,000 rpm for 10 min at 4°C. Polyacrylamide electrophoresis was performed using the Protean® Tetra cell minigel kit (Bio-Rad, Milan, Italy). Gels were stained with Coomassie brilliant blue G-250 (BioRad, Milan, Italy). A BenchMark ™ Pre-stained protein ladder (Invitrogen, UK) was included to verify the relative molecular masses of native and denaturated Cγ.
Animals
Male Wistar rats were obtained from the University of Guadalajara Bioterium. Animals were maintained under standard laboratory conditions, at 24 ± 2°C and 55 ± 5% humidity, with a 12-h light/dark cycle. They were provided a standard rodent diet (Purina LabDiet® 5001) and water ad libitum. Animal experiments were performed according to the Mexican Official Standard 062 (NOM-062-ZOO-1999) and were approved by the institutional ethics committee.
Insulin Resistance Experimental Model
To induce insulin resistance, adult male Wistar rats (body weight, 200 g) were given a 30% sucrose solution instead of drinking water ad libitum for 20 weeks, along with standard rat chow. After 20 weeks of IR induction, blood glucose levels were measured with a glucometer (One Touch® Ultra®, Johnson & Johnson), and serum triglycerides levels were measured using the glycerol phosphate/peroxidase method (BioSystems, Barcelona, Spain). The IR experimental group included animals with blood glucose values of 150–199 mg/dL and serum triglycerides levels of >145 mg/dL [16].
Type 2 Diabetes Experimental Model
To induce type 2 diabetes (T2D), five-day-old male Wistar rats (body weight, 9–11 g) were separated from their mothers and fasted overnight. Next, the animals were intraperitoneally injected with a fresh solution of STZ (150 mg/kg; Sigma, St. Louis, MO, USA) diluted in citrate buffer (10 mmol/L sodium citrate, pH 4.5) [17]. The rats were weaned at 21 days of age, and were housed in normal cages (five animals per cage). Glycemia was tested at 20 weeks post-induction. Animals with blood glucose levels of >200 mg/dL were considered diabetic [18].
Treatment Groups
The insulin resistance group (IR) and type 2 diabetes group (STZ) were each randomly divided into three subgroups: the negative control subgroups (IR-Ctrl, n = 5; STZ-Ctrl, n = 5) received normal saline solution (0.90% w/v NaCl, vehicle); the positive control subgroups (IR-Met, n = 5; STZ-Met, n = 5) received standard treatment (metformin, 300 mg/kg); and the experimental subgroups (IR-Cγ, n = 5; STZ-Cγ, n = 5) were treated with Cγ (120 mg/kg) [9]. All treatments were administrated by oral gavage, once daily, for one week.
Sample Collection
Blood samples from the retro-orbital plexus were collected at the beginning (pre-treatment values) and end (post-treatment values) of the treatment period. Animals were fasted overnight, and then anesthetized by intraperitoneal (i.p.) injection of 80 mg/kg of Zoletil ® 50 (Tiletamine-Zolazepam; Virbac, Carros, France). Blood samples were centrifuged at 3500 rpm for 10 min at 4°C, and serum was stored at −70°C until use.
Determination of Biochemical Parameters
Serum insulin levels were measured by enzyme-linked immunosorbent assay (ELISA) using the DRG® rat insulin ELISA kit (Marburg, Germany) following the manufacturer’s instructions. A semi-quantitative spectrophotometer (BTS-330; BioSystems, Spain) was used to quantify serum glucose, urea, creatinine, aspartate aminotransferase (AST), and alanine aminotransferase (ALT). Biochemical parameters were assessed using commercial reagents purchased from BioSystems (Barcelona, Spain).
Histological Assessment of Liver and Kidney
At the end of treatments, all rats were anesthetized as described above. Fragments of liver and kidney tissue were excised, separately fixed in 4% paraformaldehyde in 1× phosphate-buffered saline (PBS), and embedded in paraffin. Afterwards, paraffin-embedded serial 4-μm-thick sections were stained with hematoxylin and eosin, Masson’s trichrome stain, or periodic acid-Schiff (PAS) stain. A certified pathologist evaluated histological morphology.
RNA Extraction, Retro-Transcription, and Quantification of G6pc, Pck1, Fbp1 Gene Expression
RNA was isolated from hepatic tissue using the RNeasy® Protect Mini Kit (QIAGEN, USA), and 2 μg total RNA was used to synthesize cDNA. Reverse transcription was performed using the transcriptor first strand cDNA synthesis kit (Roche, Germany) following the manufacturer’s instructions. G6pc, Fbp1, and Pck1 gene expressions were quantified by real-time PCR using the LightCycler® FastStart (Roche, Germany), with Actb used as a housekeeping gene. The primers sequences were as follows: G6pc forward (F) 5′-CCCATCTGGTTCCACATTCAA-3′, reverse (R) 5′-CGCTGTCCAAAAAGAATCCAC-3′; Pck1 F 5′-CAGAGAGACACCGTGCCCATCC-3′, R 5′-AAGTCCTCTTCTGACATCCAGC-3′; Fbp1 F 5′- CCATCATAATAGAGCCCGAGAAGA-3′, R 5′-CTTTCTCCGAAGGCTCATTAGC-3′; and Actb F 5′-ACCCACACTGTGCCCATCTA-3′, R 5′-GCCACAGGATTCCATACCCA-3′. All amplification reactions were performed in triplicate using a 2.0 LightCycler® (Roche, Germany). The reaction conditions were as follows: 95°C for 10 min, followed by 45 cycles of 95°C for 10 s, 60°C for 10 s, and 72°C for 18 s. Negative controls included sterile water instead of cDNA. The Actb threshold cycle (Ct) values were used to normalize the target gene Ct values. The 2-ΔΔCT method was used to calculate the relative gene expressions of G6pc, Fbp1, and Pck1 [19]. Single product amplification for each gene was confirmed by melting curve analysis.
Statistical Analysis
Serum biochemical values are expressed as the mean ± standard error of the mean (SEM). The paired t-test was used to analyze intra-group differences in the pre- and post-treatment concentrations of biochemical parameters. Mean expressions of G6pc, Pck1, and Fbp1 were expressed in relative light units (RLU). Between-group differences in G6pc, Pck1, and Fbp1 gene expressions were assessed using the Mann-Whitney test, and changes were compared with the Wilcoxon test. Data analysis was performed using PASW statistical software, version 18 (Chicago, IL, USA).
Results and Discussion
The liver plays an important role in the physiological control of hepatic glucose production (HGP). In insulin resistance and T2D, HGP suppression is impaired, increasing hepatic glucose output [20, 21]. In the present study, we evaluated how the hypoglycemic protein Cγ influenced the key enzymes involved in HGP. Metformin treatment, which reduces HGP, was used as a control.
First, Cγ was extracted and characterized by SDS-PAGE as described above. Under non-reducing conditions, we identified one 50-kDa band, representing native Cγ. Under reducing conditions, we observed a 17- and a 29-kDa band, corresponding to the two Cγ subunits.
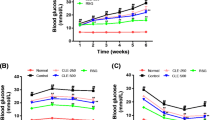
Blood’s biochemical parameters were quantified pre- and post-treatment in all groups. Changes in serum glucose and insulin concentrations, in each group, were calculated as a percentage of pre-treatment levels. Serum glucose levels were reduced by 41.89% in the IR-Met group (p < 0.001), 27.36% in the IR-Cγ group (p < 0.01), 23.23% in the STZ-Met group (p < 0.05), and 16.46% in the STZ-Cγ group (p < 0.05) (Table 1).
As expected, both Cγ [9] and metformin reduced glucose levels in the STZ and IR groups. However, the reduction in glucose concentration was notably higher in the treated IR groups than in the STZ treated animals. In a previous study, Lovati et al. [12] found that Cγ administration (28 mg/kg body weight) to Sprague-Dawley rats for three weeks while being fed a 10% glucose water solution lowered blood glucose levels as compared to the control animals (without Cγ). In the study they only compared glucose levels between groups, but did not consider the within groups biological variability [22]. In contrast, our present study included intra-group comparisons to account for normal biological variations.
One advantage of Cγ treatment is that it does not appear to produce hypoglycemia, even when the initial glucose level is close to the normal range [9, 10, 12].
Both metformin and Cγ treated groups showed a reduction in serum insulin. Serum insulin concentrations in the IR-Met and IR-Cγ groups decreased by 36.07 and 37.57%, respectively (Fig. 1a). This is likely due to the sensitizing action that both metformin and Cγ have on tissues, which lowers serum insulin levels in the IR treated groups. In contrast, serum insulin concentrations increased significantly in the T2D groups (STZ). Insulin levels were found to increase by 109.25 and 46.15% in the STZ-Met and STZ-Cγ groups, respectively (Fig. 1b). Higher insulin levels in the diabetic groups could be explained by a compensatory mechanism that is trying to reduce the high glucose levels found in these groups [23].
Pre- and post-treatment serum insulin measured in insulin resistance groups (a) and diabetic groups (b). Values represent the mean ± standard error of the mean. *p < 0.05, compare to pre-treatment; statistical analysis paired t-test. Abbreviations: IR-Ctrl insulin resistance control group, IR-Cγ insulin resistance group treated with conglutin gamma, IR-Met insulin resistance group treated with metformin, STZ-Ctrl streptozotocin control group, STZ-Cγ streptozotocin group treated with conglutin gamma, STZ-Met streptozotocin group treated with metformin
Neither serum insulin nor glucose levels in the IR-Ctrl and STZ-Ctrl groups changed after treatment (data not shown).
The use of any drug for the treatment of glucose disorders can result in some kind of kidney and/or liver damage [24, 25]. Cγ potential, as an alternative treatment for glucose disorders, justifies the evaluation of potential kidney and liver damage. The biochemical and histological evaluations revealed no renal or hepatic damage or lesions in the Cγ treated groups. Serum creatinine and urea concentrations did not change, after treatment, in any of the groups. Post-treatment serum AST and ALT concentrations were reduced only in the IR-Cγ group (Table 2). Finally, treated and control groups showed normal liver and kidney tissue architecture demonstrating that Cγ has no deleterious effects on these tissues.
G6Pase, a key enzyme in hepatic glucose production, catalyzes the final step of gluconeogenesis and glycogenolysis. In T2D, G6Pase overexpression increases the rate of endogenous glucose production [26]. In the present study, G6pc gene expression was reduced by 0.2-fold in the IR-Met group, 0.8-fold in the IR-Cγ group, 0.2-fold in the STZ-Met group, and 0.4-fold in the STZ-Cγ group compared with their respective control groups (Fig. 2a). In liver and muscle tissue, metformin inhibits G6Pase through stimulation of AMP-activated protein kinase (AMPK) [27]. It is possible that Cγ reduces G6pase activity in a similar manner. It has also been reported that metformin inhibits PEPCK gene expression through AMPK-dependent regulation of the small heterodimer partner (SHP). SHP is an orphan nuclear receptor that represses the transcription factors for G6Pase and PEPCK expression [27]. Here, we observed that metformin reduced Pck1 expression in both IR-Met and STZ-Met groups. In contrast, Cγ only diminished Pck1 gene expression in the IR-Cγ group, while the STZ-Cγ group showed a slight increase (Fig. 2c).
Expression levels of G6pc (a), Fbp1 (b), and Pck1 (c) in insulin resistance and diabetic groups. Data represent the mean ± standard error of the mean in relative light units (RLU). Actb was used as a housekeeping gene. *p < 0.05, **p < 0.01. Abbreviations: Actb beta actin gene, Fbp1 Fructose-bisphosphatase 1 gene, G6pc Glucose-6-phosphatase gene, IR-Ctrl insulin resistance control group, IR-Cγ insulin resistance group treated with conglutin gamma, IR-Met insulin resistance group treated with metformin, Pck1 Phosphoenolpyruvate carboxykinase 1 gene, SEM standard error of the mean, STZ-Ctrl streptozotocin control group, STZ-Cγ streptozotocin group treated with conglutin gamma, STZ-Met streptozotocin group treated with metformin
PEPCK gene regulation is a complex process where several transcription factors and molecules are involved [28]. The apparent discrepancy, in the diabetic treated groups, could be explained by the fact that in diabetes, insulin, glucagon, cAMP, and glucocorticoids levels are involved in PEPCK expression [28]. It can be speculated that Cγ can modify some of the molecules involved in the regulation of PEPCK expression. However, the results of this study are not enough to ascertain that Cγ mechanism of action is the same as that of metformin. Additional studies are required to elucidate Cγ mode of action.
Fbp1 gene expression increased by 2-fold in the IR-Met group, 1.6-fold in the STZ-Met group, and 2.5-fold in the STZ-Cγ group (Fig. 2b), but was reduced by 0.5-fold in the IR-Cγ group. This reflects the differences in gene regulation between PEPCK, G6Pase, and FBP1. While PEPCK and G6Pase are regulated at the transcriptional level, FBP1 is regulated through inhibition of fructose-2,6-bisphosphate (F-2,6-BP) [29]. Under hyperglycemic conditions, F-2,6-BP levels are reduced, leading to augmentation of fructose-1,6-bisphosphatase levels [20, 30]. In this respect, Fbp1 gene expression in the treated groups could be influenced by F-2,6-BP levels; however, this hypothesis must be confirmed with further experiments.
Conclusions
Overall, our present findings indicate that Cγ treatment reduced G6pc gene expression and diminishes GHP, representing one of the diverse processes involved in the hypoglycemic effect of Cγ. This study also provides evidence that the consumption of L. albus Cγ is a beneficial alternative to manage patients with glucose metabolic disorders. Further studies are necessary to investigate other potential Cγ targets.
Abbreviations
- Cγ:
-
Gamma conglutin
- Fbp1 :
-
Fructose-bisphosphatase 1 gene
- G6pc :
-
Glucose-6-phosphatase gene
- IR:
-
Insulin resistance
- Pck1 :
-
Phosphoenolpyruvate carboxykinase 1 gene
- STZ:
-
Streptozotocin
- T2D:
-
Type 2 diabetes
References
Duranti M, Consonni A, Magni C, Sessa F, Scarafoni A (2008) The major proteins of lupin seed: characterisation and molecular properties for use as functional and nutraceutical ingredients. Trends Food Sci Technol 19:624–633
Lucas MM, Stoddard FL, Annicchiarico P, Frías J, Martínez-Villaluenga C, Sussmann D, Duranti M, Seger A, Zander PM, Pueyo JJ (2015) The future of lupin as a protein crop in Europe. Front Plant Sci 6:705. doi:10.3389/fpls.2015.00705
Kohajdová Z, Karovičová J, Schmidt Š (2011) Lupin composition and possible use in bakery – a review. Czech J Food Sci 29(3):203–211
Belski R, Mori TA, Puddey IB, Sipsas S, Woodman RJ, Ackland TR, Beilin LJ, Dove ER, Carlyon NB, Jayaseena V, Hodgson JM (2011) Effects of lupin-enriched foods on body composition and cardiovascular disease risk factors: a 12-month randomized controlled weight loss trial. Int J Obes 35(6):810–819
Bähr M, Fechner A, Krämer J, Kiehntopf M, Jahreis G (2013) Lupin protein positively affects plasma LDL cholesterol and LDL:HDL cholesterol ratio in hypercholesterolemic adults after four weeks of supplementation: a randomized, controlled crossover study. Nutr J 12:107. doi:10.1186/1475-2891-12-107
Fontanari GG, Batistuti JP, da Cruz RJ, Saldiva PHN, Areas JAG (2012) Cholesterol-lowering effect of whole lupin (Lupinus albus) seed and its protein isolate. Food Chem 132:1521–1526
Radtke J, Schutkowski A, Brandsch C, Hirche F, Hasenkopf K, Stangl GI (2015) Isolated conglutin γ from lupin, but not phytate, lowers serum cholesterol without influencing vascular lesion development in the ApoE-deficient mouse model. Plant Foods Hum Nutr 70(2):113–118
Brandsch C, Kappis D, Weisse K, Stangl GI (2010) Effects of untreated and thermally treated lupin protein on plasma and liver lipids of rats fed a hypercholesterolemic high fat or high carbohydrate diet. Plant Foods Hum Nutr 65(4):410–416
Magni C, Sessa F, Accardo E, Vanoni M, Morazzoni P, Scarafoni A, Duranti M (2004) Conglutin gamma, a lupin seed protein, binds insulin in vitro and reduces plasma glucose levels of hyperglycemic rats. J Nutr Biochem 15(11):646–650
Bertoglio JC, Calvo MA, Hancke JL, Burgos RA, Riva A, Morazzoni P, Ponzone C, Magni C, Duranti M (2011) Hypoglycemic effect of lupin seed γ-conglutin in experimental animals and healthy human subjects. Fitoterapia 82(7):933–938
Terruzzi I, Senesi P, Magni C, Montesano A, Scarafoni A, Luzi L, Duranti M (2011) Insulin-mimetic action of conglutin-γ, a lupin seed protein, in mouse myoblasts. Nutr Metab Cardiovasc Dis 21(3):197–205
Lovati MR, Manzoni C, Castiglioni S, Parolari A, Magni C, Duranti M (2012) Lupin seed γ-conglutin lowers blood glucose in hyperglycaemic rats and increases glucose consumption of HepG2 cells. Br J Nutr 107(1):67–73
Vargas-Guerrero B, García-López PM, Martínez-Ayala AL, Domínguez-Rosales JA, Gurrola-Díaz CM (2014) Administration of Lupinus albus gamma conglutin (Cγ) to n5 STZ rats augmented ins-1 gene expression and pancreatic insulin content. Plant Foods Hum Nutr 69(3):241–247
Martínez-Ayala AL, Paredes-López O (2001) Molecular characterization of the β-conglutin of lupin seeds. J Food Biochem 25(1):15–31
Schägger H, von Jagow G (1987) Tricine-sodium dodecyl sulfate-polyacrylamide gel electrophoresis for the separation of proteins in the range from 1 to 100 kDa. Anal Biochem 166(2):368–379
Car BD, Eng VM, Everds NE et al (2006) Clinical pathology of the rat. In: Suckow MA, Weisbroth SH, Franklin CA (eds) The laboratory rat, 2nd edn. Academic Press, San Diego, p 133
Takada J, Machado MA, Peres SB, Brito LC, Borges-Silva CN, Costa CE, Fonseca-Alaniz MH, Andreotti S, Lima FB (2007) Neonatal streptozotocin-induced diabetes mellitus: a model of insulin resistance associated with loss of adipose mass. Metabolism 56(7):977–984
Matteucci E, Giampietro O (2008) Proposal open for discussion: defining agreed diagnostic procedures in experimental diabetes research. J Ethnopharmacol 115(2):163–172
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(−Delta Delta C(T)) method. Methods 25(4):402–408
Guo X, Li H, Xu H, Woo S, Dong H, Lu F, Lange AJ, Wu C (2012) Glycolysis in the control of blood glucose homeostasis. Acta Pharm Sin B 2(4):358–367
Wu C, Okar DA, Newgard CB, Lange AJ (2002) Increasing fructose 2,6-bisphosphate overcomes hepatic insulin resistance of type 2 diabetes. Am J Physiol Endocrinol Metab 282(1):E38–E45
Widjaja A, Morris RJ, Levy JC, Frayn KN, Manley SE, Turner RC (1999) Within- and between-subject variation in commonly measured anthropometric and biochemical variables. Clin Chem 45(4):561–566
Tripathy D, Chavez AO (2010) Defects in insulin secretion and action in the pathogenesis of type 2 diabetes mellitus. Curr Diab Rep 10(3):184–191
Chitturi S, George J (2002) Hepatotoxicity of commonly used drugs: nonsteroidal anti-inflammatory drugs, antihypertensives, antidiabetic agents, anticonvulsants, lipid-lowering agents, psychotropic drugs. Semin Liver Dis 22(2):169–183
Choudhury D, Ahmed Z (2006) Drug-associated renal dysfunction and injury. Nat Clin Pract Nephrol 2(2):80–91
Van Schaftingen E, Gerin I (2002) The glucose-6-phosphatase system. Biochem J 362:513–532
Kim YD, Park KG, Lee YS, Park YY, Kim DK, Nedumaran B, Jang WG, Cho WJ, Ha J, Lee IK, Lee CH, Choi HS (2008) Metformin inhibits hepatic gluconeogenesis through AMP-activated protein kinase-dependent regulation of the orphan nuclear receptor SHP. Diabetes 57(2):306–314
Croniger CM, Chakravarty K, Olswang Y, Cassuto H, Reshef L, Hanson RW (2002) Phosphoenolpyruvate carboxykinase revisited: II. Control of PEPCK-C gene expression. Biochem Mol Biol Educ 30(6):353–362
Barthel A, Schmoll D (2003) Novel concepts in insulin regulation of hepatic gluconeogenesis. Am J Physiol Endocrinol Metab 285(4):E685–E692
van Poelje PD, Potter SC, Erion MD (2011) Fructose-1, 6-bisphosphatase inhibitors for reducing excessive endogenous glucose production in type 2 diabetes. Handb Exp Pharmacol 203:279–301
Acknowledgements
The authors thank Ing. Rogelio Troyo-Sanromán for statistical advice and Dr. van Santen for the lupin seeds. This study was supported by a CONACyT grant (number 60283) given to CMGD. AEGS and BVG received fellowships from CONACyT (fellowship numbers 204929 and 225001, respectively). Also, partial financial support was received from University of Guadalajara REC/747/2016.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare no potential conflicts of interest or financial disclosures.
Additional information
Ana E. González- Santiago and Belinda Vargas-Guerrero contributed equally to this work.
Rights and permissions
About this article
Cite this article
González-Santiago, A.E., Vargas-Guerrero, B., García-López, P.M. et al. Lupinus albus Conglutin Gamma Modifies the Gene Expressions of Enzymes Involved in Glucose Hepatic Production In Vivo . Plant Foods Hum Nutr 72, 134–140 (2017). https://doi.org/10.1007/s11130-016-0597-7
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11130-016-0597-7