Abstract
Background Patients colonized with carbapenem-susceptible Pseudomonas aeruginosa (CSPA) strains upon admission to the intensive care unit (ICU) tend to be quickly followed by detected carbapenem-resistant P. aeruginosa strains after admission. Objective To assess the risk factors associated with the quick loss of carbapenem susceptibility and to identify time threshold of prior antimicrobial exposure for the loss during ICU stay. Setting A tertiary-care teaching hospital with 2560 beds located in the northwest region of China. Method A retrospective observational study was conducted between January 2013 and April 2016 at ICUs. Logistic regression analysis was used to assess risk factors, and receiver operating characteristic (ROC) analyses were constructed to identify the time threshold. Main outcome measure The time threshold and risk factors for the quick loss of carbapenem susceptibility. Results Among the 84 patients with CSPA initially, 32 (38.1%) patients were observed to have a loss of carbapenem susceptibility during ICU stay. Logistic regression analyses showed that previous carbapenem exposure was only independently associated with the loss of carbapenem susceptibility (odds ratio 13.16; 95% CI 3.13–55.24; p < 0.001). The optimal cut-off was 3.5 days on ROC curve, indicating the high risk for loss of susceptibility. Conclusion In order to alleviate selective pressure caused by antipseudomonal carbapenems exposure, continued research is needed to determine the most appropriate carbapenems treatment strategies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Impact of findings on pharmacy and clinical practice
-
The duration of carbapenem intake of more than 3.5 days in ICU patients, means a higher risk of the loss of susceptibility of P. aeruginosa.
-
Continued research is critically needed to determine the most appropriate carbapenem treatment strategies, such as dosing regimens, combination therapy.
-
In order to alleviate selective pressure caused by antipseudomonal carbapenem exposure, it may be necessary to consider ertapenem use in the context of institutional stewardship initiatives.
Introduction
Carbapenems are often used as the last line of defense against increasingly difficult-to-treat Gram-negative pathogens such as Pseudomonas aeruginosa [1]. However, patients colonized with carbapenem-susceptible Pseudomonas aeruginosa (CSPA) strains upon admission to the intensive care unit (ICU) tend to be quickly followed by detected carbapenem-resistant Pseudomonas aeruginosa (CRPA) strains after admission. In fact, preserving carbapenems available for P. aeruginosa infections is difficult to achieve because the path of emergence and dissemination of CRPA have not yet been fully elucidated.
There have been many updated epidemiological and resistance mechanisms studies on CRPA [2,3,4]. The carbapenem resistance rates in Canada (3.3%) was the lowest of all countries, with ratios lower than 10%. On the other hand, ratios in some countries (such as Brazil, Peru, and Russia) were higher than 50%. In most countries, the reported CRPA ratio ranged from 10 to 50% [5]. Reportedly, in China about 30.2 and 25.9% of the P. aeruginosa isolates were resistant to imipenem and meropenem in 2013, respectively [6]. A few reports and meta-analyses revealed that carbapenem use is one of the leading risk factors for CRPA [7]. However, the carbapenem exposure duration for changed susceptibility in ICU patients colonized with CSPA upon admission remain obscure. The present study was designed to explore the above clinical issue. It is anticipated that an improved understanding of carbapenem resistance in P. aeruginosa may help ensure appropriate empirical therapy whilst minimizing the potential development of resistance.
Aim of the study
The goal of the study was to determine the prevalence characterization and verify risk factors associated with loss of susceptibility in P. aeruginosa strains to carbapenems during ICU staying, more importantly, to identify time threshold of this phenomenon.
Ethics approval
The study was reviewed and approved by the hospital’s human ethics committee. The requirement for informed consent was waived because this was an observational and retrospective study and only de-identified data were used in the study.
Methods
Study design and patient population
This retrospective and observational study was performed at the First Affiliated Hospital of Xi’an Jiaotong University. This is a tertiary-care teaching hospital with 2560 beds located in the northwest region of China.
We identified all the hospitalized patients in ICU from January 2013 to April 2016, with ICU stay ≥3 days and age ≥18 years. Organisms isolated within 48 h of ICU admission were considered colonized upon admission and more than 48 h after ICU admission in patients with previous negative specimens were considered ICU-acquired. In order to analyze the risk factors associated with carbapenem susceptibility loss against P. aeruginosa, patients colonized with CSPA upon admission were divided into two groups. The first group was patients with CRPA (ICU-acquired CRPA strains), the second group was patients without CRPA (who did not acquire CRPA and always colonized with CSPA strains during ICU stay).
Bacterial identification and antimicrobial susceptibility test
The hospital’s clinical microbiology laboratory provided data of bacterial identification and antibacterial susceptibility testing. All positive clinical specimens (blood, sputum, urine, wound, or normally sterile body fluid positive for P. aeruginosa) were included. Antimicrobial susceptibilities were determined by minimum inhibitory concentration (MIC) using the micro-broth dilution method and interpreted according to the criteria suggested by the Clinical and Laboratory Standards Institute document (CLSI document M100-S22. Wayne, PA, USA: CLSI, 2012). In this study, CRPA was defined as an isolate with meropenem and/or imipenem MICs ≥ 8 mg/L. The other P. aeruginosa isolates were defined as CSPA. Compared to first test upon admission, the changed multiples (from ≤0.5 to ≥64) were recorded when repeated test for MICs of meropenem and imipenem against P. aeruginosa from the same individual patients.
Data collection
The following data of each patient was collected by two researchers respectively from medical records: sex, age, patients’ setting, comorbidities and underlying diseases, hospital admission date, ICU admission date, and ICU discharge date, APACHE II score on ICU admission, clinical signs and laboratory data, the reasons for admission, prior non-antibiotic/antibiotic exposures. Prior non-antibiotic/antibiotic exposure was defined as the non-antibiotic or antibiotic exposure for at least three consecutive days within 30 days before the P. aeruginosa detection and acquired resistance or ICU discharge date if the patient did not acquire CRPA. The following non-antibiotic exposure was recorded: central venous catheter, bladder catheter, drainage catheter, nasogastric tube, enteral/parenteral nutrition, orotracheal intubation/tracheostomy, endoscopy, surgery, renal replacement therapies, packed red blood cell transfusion. The following antibiotics were recorded: meropenem, imipenem–cilastatin, ceftazidime, piperacillin–tazobactam, cefoperazone–sulbactam, moxifloxacin, levofloxacin, ciprofloxacin, gentamicin, amikacin, tigecycline, minocycline, glycopeptides, vancomycin, norvancomycin, teicoplanin, linezolid, fluconazole, voriconazole, itraconazole, and caspofungin.
Statistical analysis
Logistic regression analyses were conducted to assess the risk factors for the carbapenem susceptibility loss against P. aeruginosa during ICU stay. A receiver operating characteristic (ROC) analysis was done to determine the diagnostic value of prior antibiotic exposure duration for predicting loss of carbapenem susceptibility. All analyses were performed using PASW Statistics (version 18.0, Chicago, IL, USA). Continuous variables were described as mean ± standard deviation (SD) and compared with the Student t test; if their distributions were not normal, they were described as the median as well as range and compared with the Wilcoxon rank-sum test. Categorical variables were compared with a Chi square test or Fisher exact test. To identify the independent risk factors, variables with p < 0.20 in the univariate analysis were included in multivariate logistic regression models. Odds ratio (OR) and 95% confidence interval (CI) were also calculated. All test results were considered statistically significant when the p value was <0.05.
Results
Descriptive epidemiology
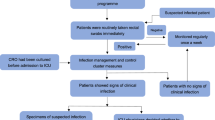
A total of 1077 P. aeruginosa strains from 386 patients in ICUs were obtained during the 40-month study period. Upon admission to ICU, resistant strains to piperacillin–tazobactam, meropenem, imipenem, ciprofloxacin, ceftazidime, and amikacin was observed in 55 (16.6%), 50 (15.0%), 40 (12.5%), 28 (9.8%), 25 (8.8%), and 12 (4.2%) patients, respectively. There were 84 patients colonized with CSPA strains upon admission. During ICU stay, among the 84 patients above-mentioned, 32 patients acquired CRPA strains. Carbapenems resistance against P. aeruginosa when first detected upon admission and acquired during ICU stay are shown in Fig. 1.
Schematic diagram of the number of patients: Pseudomonas aeruginosa resistance to carbapenems when first detected upon admission to ICU and acquisition cases during ICU stay. Note CSPA, carbapenem-susceptible Pseudomonas aeruginosa; CRPA, carbapenem-resistant Pseudomonas aeruginosa; ICU, intensive care unit
Table 1 respectively shows changed multiples with repeated MIC tests for meropenem and imipenem against P. aeruginosa collected from the same individual patients during ICU stay compared to first test upon admission. Notably, among the 84 patients with CSPA initially, MIC of meropenem in 32 (38.1%) patients was observed increased four times or more from the baseline MIC; likewise, in 30 (35.7%) patients, MICs of imipenem up to four times or more was observed. Among the 45 patients with carbapenem exposure, increased MICs of meropenem and imipenem were observed in 28 (62.2%) patients. Among the 39 patients without carbapenem exposure, only four (10.3%) and two (5.1%) patients respectively had decreased meropenem and imipenem susceptibility. Our study shows that in patients exposed to carbapenems during ICU stay, the MIC value distinctly increased in for meropenem and imipenem against P. aeruginosa.
Risk factors for the loss of susceptibility
We focused on those patients colonized upon admission as susceptible, who were evaluated to determine risk factors associated with ICU-acquired CRPA strain. The medical records of the 84 index patients were reviewed (32 patients acquired CRPA strains compared to 52 patients did not acquire CRPA). The mean age was 60.2 ± 17.2 years, and the mean APACHE II score was 15.5 ± 6.8 with a male to female ratio of 1.3:1. The most common causes for ICU admission were respiratory disease and infection.
Comparing patients in two groups by univariate logistic analysis, patients who acquired CRPA tended to have prior carbapenem, piperacillin–tazobactam, aminoglycosides, glycopeptides/linezolid exposure and more cumulative number of antibiotic treatments. Non-antibiotic exposures during ICU stay, such as central venous catheter and drainage catheter, tended to help with acquisition of CRPA. Beyond that, in other variables between the both groups, no significant differences were found (p > 0.20), as shown in Table 2. Using multivariate logistic analysis, carbapenem exposure was the only independent risk factor for colonized with CSPA upon admission whilst acquired CRPA isolates after admission (OR 13.16; 95% CI 3.13–55.24; p < 0.001), as shown in Table 3.
ROC curve and time threshold
As is shown in Table 3, carbapenems exposure was statistically significant in the drug resistance evolution. Duration of carbapenems intake, as test variable, was considered to construct a ROC curve. As were shown in Table 4 and Fig. 2, the ROC analysis determined the optimal cut-off value of carbapenems intake duration revealed a significantly higher risk of susceptibility loss at 3.5 days (sensitivity: 0.88, specificity: 0.75). The area under the ROC curve was 0.83 (95% CI 0.74–0.93) and the maximum Youden index was 0.63.
ROC curve of duration of carbapenems intake in days to identify time threshold for predicting risk of the loss of carbapenem susceptibility in patients colonized with CSPA strains upon admission to ICU. Note ROC curve, receiving operator characteristic curve; CSPA, carbapenem-susceptible Pseudomonas aeruginosa; ICU, intensive care unit; CI, confidence interval
Discussion
In the present study, exposure to carbapenems, the most commonly reported risk factor in previous studies [8, 9] was considered to be the only independent risk factor for the loss of carbapenem susceptibility in ICU patients colonized with CSPA upon admission. In previously studies, prior antibiotics exposure is considered an imperative risk factor for the acquisition of P. aeruginosa [10,11,12,13]. Resistance acquisition driven by antipseudomonal agents exposure can be reached by either selecting mutants in patients previously colonized or infected by susceptible phenotypes or promoting selection of an already resistant strain [14, 15]. For patients colonized by P. aeruginosa in previous studies, fluoroquinolones may have a greater tendency to select resistant mutants than other agents [16,17,18]. However, this tendency was not found in our study. Likewise, the role of aminoglycosides and piperacillin–tazobactam as a risk factor for acquiring CRPA strains was reported in other studies [19,20,21]. In multivariate logistic analysis of our study they were excluded (p > 0.05), and significant association with acquiring of CRPA were not observed.
Our prior study based on hospital-wide population-level data have revealed that antipseudomonal carbapenems consumption was strongly correlated with the monthly resistance rate of P. aeruginosa to imipenem [6]. The present study shows that on individual patient level, carbapenem exposure also closely correlated with evolution of resistance. Going even further, what is the minimal duration of prior antimicrobial exposure forecasting risk for the loss of carbapenem susceptibility? The threshold of P. aeruginosa exposed to carbapenems remains obscure in previous studies. In the previous study [12, 22, 23], carbapenems had the shortest duration of prior antibiotic exposure for piperacillin–tazobactam-resistant P. aeruginosa (3 days). In the present study, we firstly tried to build ROC curve for identify the time threshold of prior antimicrobial exposure. If the duration is longer than 3.5 days, it may suggest high-risk of ICU-acquired CRPA isolates. In clinical practice, physicians may predict resistance development in accordance with previous carbapenem exposure, including the duration. In fact, the widely used practice is to consider monotherapy until cultures grow a resistant organism [24]. This result encourages us to talk about and question what we did in practice. At what point after admission into the ICU should combinations with other antipseudomonal antimicrobial agents be initiated? Should combined medicine be started before detecting a resistant organism or not? In an in vitro hollow fiber infection and a murine model against P. aeruginosa, the combination of meropenem and levofloxacin was validated to be promising because of good bacterial kill and resistance suppression [25]. Without doubt, this combination treatment still needs clinical evaluation.
Avoiding collateral damage and preserving the effectiveness of the carbapenem class are priorities in the context of widespread resistance to often-used antibiotics. In this study, loss of P. aeruginosa susceptibility is fast after carbapenem exposure (meropenem and imipenem–cilastatin) such that more attention must be paid to carbapenem stewardship in order to delay the emergency of resistance. Available ecological data suggest that, between group 1 and group 2 carbapenems, there are significant variations in the effects on CRPA. Use of the group 2 carbapenems (imipenem, meropenem, and doripenem, that is, antipseudomonal carbapenems) may lead to emergence of P. aeruginosa resistance. The group 1 carbapenem ertapenem has limited activity against P. aeruginosa and does not adversely impact hospital ecology, and even can benefit with improved P. aeruginosa susceptibility [26,27,28,29]. Next, based on further argument, it is possible to consider prescribing ertapenem more instead of antipseudomonal carbapenems in suitable patients when clinically appropriate in ICU settings, e.g., against non-pseudomonad, non-Acinetobacter Gram-negative pathogens.
There are a few limitations to our study. First, this was a retrospective study. The retrospective nature may preclude accurate comparisons because of many confounding factors, and our study results need further investigation for verification. Second, the number of cases was small, which may have been underpowered to analyze some risk factors. Third, the present study was not involved in discussing pharmacodynamic profiles of individual exposure (e.g., time that the concentration exceeds the MIC, or minimum concentration/MIC Ratio) to differentiate the exposure degree associated with resistance, or detecting the presence of resistance genes, and further prospective study should involve these issues.
Conclusion
Our results revealed that previous carbapenem exposure is strongly and independently correlated with the quick loss of carbapenem susceptibility to P. aeruginosa isolates in ICU patients. If there has been more than 3.5 days of carbapenem intake, there is a higher risk of susceptibility loss in ICU. In order to alleviate selective pressure caused by antipseudomonal carbapenems exposure, continued research is critically needed to determine the most appropriate treatment strategies, such as dosing regimens, combination therapy. Furthermore, it may be necessary to consider ertapenem use in the context of institutional stewardship initiatives.
References
Nicolau DP, Carmeli Y, Crank CW, Goff DA, Graber CJ, Lima AL, et al. Carbapenem stewardship: does ertapenem affect Pseudomonas susceptibility to other carbapenems? A review of the evidence. Int J Antimicrob Agents. 2012;39:11–5.
Walkty A, Lagace-Wiens P, Adam H, Baxter M, Karlowsky J, Mulvey MR, et al. Antimicrobial susceptibility of 2906 Pseudomonas aeruginosa clinical isolates obtained from patients in Canadian hospitals over a period of 8 years: results of the Canadian Ward surveillance study (CANWARD), 2008–2015. Diagn Microbiol Infect Dis. 2017;87:60–3.
Ferreira ML, Dantas RC, Faria AL, Gonçalves IR, Silveira de Brito C, Queiroz LL, et al. Molecular epidemiological survey of the quinolone- and carbapenem-resistant genotype and its association with the type III secretion system in Pseudomonas aeruginosa. J Med Microbiol. 2015;64:262–71.
Rojo-Bezares B, Estepa V, Cebollada R, de Toro M, Somalo S, Seral C, et al. Carbapenem-resistant Pseudomonas aeruginosa strains from a Spanish hospital: characterization of metallo-β-lactamases, porin OprD and integrons. Int J Med Microbiol. 2014;304:405–14.
Hong DJ, Bae IK, Jang IH, Jeong SH, Kang HK, Lee K. Epidemiology and characteristics of metallo-β-lactamase-producing Pseudomonas aeruginosa. Infect Chemother. 2015;47:81–97.
Zou YM, Ma Y, Liu JH, Shi J, Fan T, Shan YY, et al. Trends and correlation of antibacterial usage and bacterial resistance: time series analysis for antibacterial stewardship in a Chinese teaching hospital (2009–2013). Eur J Clin Microbiol Infect Dis. 2015;34:795–803.
Voor In’t Holt AF, Severin JA, Lesaffre EM, Vos MC. A systematic review and meta-analyses show that carbapenem use and medical devices are the leading risk factors for carbapenem-resistant Pseudomonas aeruginosa. Antimicrob Agents Chemother. 2014;58:2626–37.
Barron MA, Richardson K, Jeffres M, McCollister B. Risk factors and influence of carbapenem exposure on the development of carbapenem resistant Pseudomonas aeruginosa bloodstream infections and infections at sterile sites. Springerplus. 2016;5:755.
Harris AD, Johnson JK, Thom KA, Morgan DJ, McGregor JC, Ajao AO, et al. Risk factors for development of intestinal colonization with imipenem-resistant Pseudomonas aeruginosa in the intensive care unit setting. Infect Control Hosp Epidemiol. 2011;32:719–22.
Patterson JE. Antibiotic utilization: is there an effect on antimicrobial resistance? Chest. 2001;119:426S–30S.
Safdar N, Maki DG. The commonality of risk factors for nosocomial colonization and infection with antimicrobial-resistant Staphylococcus aureus, enterococcus, Gram-negative bacilli, Clostridium difficile, and Candida. Ann Intern Med. 2002;136:834–44.
Kollef MH, Chastre J, Fagon JY, François B, Niederman MS, Rello J, et al. Global prospective epidemiologic and surveillance study of ventilator-associated pneumonia due to Pseudomonas aeruginosa. Crit Care Med. 2014;42:2178–87.
Cobos-Trigueros N, Solé M, Castro P, Torres JL, Hernández C, Rinaudo M, et al. Acquisition of Pseudomonas aeruginosa and its resistance phenotypes in critically ill medical patients: role of colonization pressure and antibiotic exposure. Crit Care. 2015;19:218.
Riou M, Carbonnelle S, Avrain L, Mesaros N, Pirnay JP, Bilocq F, et al. In vivo development of antimicrobial resistance in Pseudomonas aeruginosa strains isolated from the lower respiratory tract of Intensive Care Unit patients with nosocomial pneumonia and receiving antipseudomonal therapy. Int J Antimicrob Agents. 2010;36:513–22.
Lipsitch M, Bergstrom CT, Levin BR. The epidemiology of antibiotic resistance in hospitals: paradoxes and prescriptions. Proc Natl Acad Sci. 2000;97:1938–43.
Ong DS, Jongerden IP, Buiting AG, Leverstein-van Hall MA, Speelberg B, Kesecioglu J, et al. Antibiotic exposure and resistance development in Pseudomonas aeruginosa and Enterobacter species in intensive care units. Crit Care Med. 2011;39:2458–63.
Lin KY, Lauderdale TL, Wang JT, Chang SC. Carbapenem-resistant Pseudomonas aeruginosa in Taiwan: prevalence, risk factors, and impact on outcome of infections. J Microbiol Immunol Infect. 2016;49:52–9.
Fortaleza CM, Freire MP, Filho Dde C, de Carvalho Ramos M. Risk factors for recovery of imipenem- or ceftazidime-resistant Pseudomonas aeruginosa among patients admitted to a teaching hospital in Brazil. Infect Control Hosp Epidemiol. 2006;27:901–6.
Harris AD, Smith D, Johnson JA, Bradham DD, Roghmann MC. Risk factors for imipenem-resistant Pseudomonas aeruginosa among hospitalized patients. Clin Infect Dis. 2002;34:340–5.
Gbaguidi-Haore H, Dumartin C, L’Hériteau F, Péfau M, Hocquet D, Rogues AM, et al. Antibiotics involved in the occurrence of antibiotic-resistant bacteria: a nationwide multilevel study suggests differences within antibiotic classes. J Antimicrob Chemother. 2013;68:461–70.
Onguru P, Erbay A, Bodur H, Baran G, Akinci E, Balaban N, et al. Imipenem-resistant Pseudomonas aeruginosa: risk factors for nosocomial infections. J Korean Med Sci. 2008;23:982–7.
Patel N, McNutt LA, Lodise TP. Relationship between various definitions of prior antibiotic exposure and piperacillin–tazobactam resistance among patients with respiratory tract infections caused by Pseudomonas aeruginosa. Antimicrob Agents Chemother. 2008;52:2933–6.
Hyle EP, Gasink LB, Linkin DR. BilkerWB, Lautenbach E. Use of different thresholds of prior antimicrobial use in defining exposure: impact on the association between antimicrobial use and antimicrobial resistance. J Infect. 2007;55:414–8.
Kmeid JG, Youssef MM, Kanafani ZA, Kanj SS. Combination therapy for Gram-negative bacteria: what is the evidence? Expert Rev Anti Infect Ther. 2013;11:1355–62.
Louie A, Liu W, VanGuilder M, Neely MN, Schumitzky A, Jelliffe R, et al. Combination treatment with meropenem plus levofloxacin is synergistic against Pseudomonas aeruginosa infection in a murine model of pneumonia. J Infect Dis. 2015;211:1326–33.
Lima AL, Oliveira PR, Paula AP, Dal-Paz K, Almeida JN Jr, Félix Cda S, et al. Carbapenem stewardship: positive impact on hospital ecology. Braz J Infect Dis. 2011;15:1–5.
Carmeli Y, Klarfeld Lidji S, Navon-Venezia S, Schwaber MJ. The effects of group 1 versus group 2 carbapenems on imipenem-resistant Pseudomonas aeruginosa: an ecological study. Diagn Microbiol Infect Dis. 2011;70:367–72.
Graber CJ, Hutchings C, Dong F, Lee W, Chung JK, Tran T. Changes in antibiotic usage and susceptibility among nosocomial Enterobacteriaceae and Pseudomonas isolates following the introduction of ertapenem to hospital formulary. Epidemiol Infect. 2012;140:115–25.
Goldstein E, Citron DM, Peraino V, Elgourt T, Meibohm AR, Lu S. Introduction of ertapenem into a hospital formulary: effect on antimicrobial usage and improved in vitro susceptibility of Pseudomonas aeruginosa. Antimicrob Agents Chemother. 2009;53:5122–6.
Funding
The authors gratefully acknowledge the support by the National Natural Science Foundation of China (Grant Nos. 81473177, 81672954) and Shaanxi Provincial Natural Science Foundation (Grant No. 2016JM8015).
Conflicts of interest
All authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zou, Y., Lian, J., Di, Y. et al. The quick loss of carbapenem susceptibility in Pseudomonas aeruginosa at intensive care units. Int J Clin Pharm 40, 175–182 (2018). https://doi.org/10.1007/s11096-017-0524-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11096-017-0524-5