Abstract
The present study was designed to investigate the role of calpain and the proteasome in the removal of oxidized neuronal cytoskeletal proteins in myelin basic protein-induced experimental autoimmune encephalomyelitis (EAE). To this end, EAE rats received a single intrathecal injection of calpeptin or epoxomicin at the first sign of clinical disease. Forty-eight hours later, animals were sacrificed and lumbar spinal cord segments were dissected and used for biochemical analyses. The results show that calpain and proteasome activity is specifically, but partially, inhibited with calpeptin and epoxomicin, respectively. Calpain inhibition causes an increase in total protein carbonylation and in the amount of neurofilament proteins (NFPs), β-tubulin and β-actin that were spared from degradation, but no changes are seen in the oxidation of any of three NFPs. By contrast, proteasome inhibition has no effect on total protein carbonylation or cytoskeletal protein degradation but increases the amount of oxidized NFH and NFM. These results suggest that while the proteasome may contribute to removal of oxidized NFPs, calpain is the main protease involved in degradation of neuronal cytoskeleton and does not preferentially targets oxidized NFPs species in acute EAE. Different results were obtained in a cell-free system, where calpain inhibition rises the amount of oxidized NFH, and proteasome inhibition fails to change the oxidation state of the NFPs. The later finding suggests that the preferential degradation of oxidized NFH and NFM in vivo by the proteasome occurs via the 26S and not the 20S particle.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
A significant body of experimental evidence has accumulated recently demonstrating that oxidative stress is a major player in the pathogenesis of multiple sclerosis (MS) and its animal model experiment autoimmune encephalomyelitis (EAE) [1,2,3]. Carbonylation, the non-enzymatic addition of aldehydes or ketones to specific amino acid residues, is one of the primary modifications of proteins under severe or prolonged oxidative stress conditions [4,5,6]. Protein carbonyls are an irreversible form of protein damage [5] occurring in many neurodegenerative disorders including Alzheimer’s disease [7], Parkinson’s disease [8], amyotrophic lateral sclerosis [9] and MS [10].
Concentrations of carbonylated proteins in cells are normally very low, but even small changes in the percentage of oxidized proteins or the number of oxidative modifications on a molecule can lead to the formation of protein aggregates, alter their ability to function, or influence their metabolic stability. A number of proteolytic systems that preferentially degrade oxidized proteins operate in cells in order to keep the cellular levels of protein carbonylation low. The core 20S proteasome degrades oxidized proteins in an ATP- and ubiquitin-independent manner and is believed to be the chief mechanism clearing carbonylated proteins in cells [11]. Indeed, reduced activity of the 20S proteasome correlates with the accumulation of protein carbonyls in chronic EAE [12]. However, there is evidence that other proteases also hydrolyze oxidized proteins in a preferential manner. The calcium-dependent cysteine protease calpain has been shown to degrade oxidized neurofilaments at a higher rate than non-oxidized neurofilaments in a cell-free system [13]. Calpain has also been found to be an important proteolytic pathway for cytoskeletal proteins in the CNS [14] and its activity is elevated in both acute [15] and chronic EAE [16].
EAE shares a number of clinical and pathological features with MS and is routinely employed to study the mechanistic bases of disease and to test therapeutic approaches [17]. Myelin basic protein (MBP)-induced EAE in the Lewis rat, the animal model used in this study, is an acute monophasic clinical disease that resolves spontaneously within 5 days of onset. At the peak of disease there are perivenular infiltrates of inflammatory cells within the spinal cord. There is, however, no demyelination of CNS axons, making this an ideal model to study the neuroinflammatory aspects of MS. Previous studies in our laboratory have shown accumulation of protein carbonyls during the peak of neurological symptoms in acute EAE [18]. Protein carbonyl levels return to normal levels after neuroinflammation and neurologic deficits subside, indicating that proteolytic mechanisms are working to clear these damaged proteins from CNS tissue. The peak of neurologic disease in acute EAE also coincides with damage to the cytoskeletal protein network as seen by the significant degradation of all three neurofilament chains and β-tubulin [18].
The present study was designed to identify the proteolytic activity leading to cytoskeletal protein digestion in EAE and whether oxidative damage to those species targets them for specific degradation. Our focus was on neuronal cytoskeletal proteins because they are targets of oxidation in MS [19] and EAE [18, 20]. The specific oxidation of certain cytoskeletal proteins in acute EAE changes during the course of the disease, suggesting preferential targeting of the oxidized species for degradation [18]. Results presented herein show that calpain plays a critical role in the proteolysis of neurofilaments, β-tubulin and β-actin in EAE. Inhibition of calpain activity leads to accumulation of oxidized protein species but does not change the specific oxidation levels of any of the neurofilament proteins. Reducing proteasome activity does not affect total protein carbonylation or cytoskeletal protein levels but does lead to accumulation of oxidized NFM and NFH. These results suggest that while the proteasome may contribute to removal of oxidized proteins, calpain is the main protease involved in degradation of neuronal cytoskeleton and does not preferentially targets oxidized cytoskeletal protein species in acute EAE. To the best of our knowledge this is the first study using inhibition of calpain or the proteasome to investigate mechanisms of preferential degradation of oxidized proteins in vivo.
Materials and Methods
Induction of Experimental Autoimmune encephalomyelitis (EAE)
Housing and handling of the animals as well as the euthanasia procedure were in strict accordance with the NIH Guide for the Care and Use of Laboratory Animals and were approved by the Institutional Animal Care and Use Committee. Seven-week-old male Lewis rats were purchased from Harlan Bioproducts (Indianapolis, IN) and housed in the UNM-animal resource facility. EAE was induced with MBP in complete Freund’s adjuvant as described previously [18]. Rats were weighed and examined daily for the presence of neurological signs. Animals were euthanized by decapitation 48 h after an intrathecal (i.t.) injection of inhibitors (see below). Spinal cords segments L1–L3 were dissected and homogenized in HEN buffer (25 mM hepes pH 7.5, 1 mM EDTA and 0.1 mM neocuproine) containing 2 mM 4,5 dihydroxy-1,3 benzene disulfonic acid and 1 mM dithiothreitol. Protein homogenates were stored at − 80 °C until use. Protein concentration was assessed with the Bio-Rad DC™ protein assay (Bio-Rad Laboratories; Hercules, CA) using bovine serum albumin as standard.
Acute Lumbar Puncture and Intrathecal Drug Delivery
I.t. drug injections were conducted when rats displayed the first signs of clinical disease as previously described [21]. An injection catheter was inserted under brief isoflurane anesthesia (1–2% in oxygen). Here, a 25 cm PE-10 catheter (attached by a 30-gauge sterile needle to a sterile, 50 µl glass Hamilton syringe) was marked 7.7 cm from the open end. Under light anesthesia, the dorsal pelvic area was shaved and cleaned with 70% alcohol. An 18-gauge sterile needle with the plastic hub removed was inserted between lumbar vertebrae L5 and L6. The open end of the PE-10 catheter was inserted via the 18-gauge needle and threaded to the 7.7 cm mark allowing for intrathecal PE-10 catheter-tip placement at the T12-L1 junction. Injections consisted of 4 µl of dimethyl sulfoxide (DMSO) containing either 4 µg of calpeptin (Enzo Life Sciences, Plymouth Meeting, PA), 4 µg of epoxomicin (Cayman Chemical Co., Ann Arbor, MI) or no drug (vehicle), with a 5 µl post 0.9% sterile, isotonic saline flush. The PE-10 catheter was immediately withdrawn and the 18-gauge needle was removed from the L5–L6 inter-vertebral space. Rats were then placed in their home cage and observed during recovery from anesthesia.
Protease Activity Assay
Calpain activity was determined in EAE spinal cords homogenates using a fluorescence assay [22]. Spinal cord homogenates (100 µg protein) were diluted to 2 mg/ml in HEN buffer and membrane-bound calpain was removed prior to the assay by centrifugation at 10,000×g for 25 min. An aliquot of the soluble fraction (25 µl) was incubated with the substrate 7-aminomethyl-4-coumarin (AMC)-labeled peptide Suc-Leu-Leu-Val-Tyr-AMC (Enzo) in 100 mM KCl, 10 mM CaCl2, 25 mM hepes buffer pH 7.5. The incubation was carried out in the absence and presence of 0.4 µg/µl calpeptin. Calpain activity was calculated as the difference in fluorescence intensity at 460 nm between the samples with and without inhibitor using an excitation wavelength of 380 nm.
The proteasome chymotrypsin-like activity was determined in EAE spinal cord homogenates using a similar fluorescence assay [23]. Briefly, 50 µg of protein were incubated for 1 h at 25 °C with 50 µM Suc-Leu-Leu-Val-Tyr-AMC in the absence or presence of 10 µM clasto-lactacystin-β-lactone (Enzo). Enzyme activity was determined by fluorescence intensity as above.
Cathepsin B activity was also measured fluorometrically by incubating aliquots of the spinal cord homogenates with 50 µM z-Phe-Arg-AMC (Enzo) in 100 mM sodium acetate (pH 5.5) for 2 h at 37 °C [24].
Assessment of Protein Carbonylation by Western Blotting
Protein carbonyl groups were measured with the oxyblot procedure [18]. In brief, proteins (5 µg) were incubated with 2,4-dinitrophenyl-hydrazine to form the 2,4-dinitrophenyl (DNP) hydrazone derivatives. Proteins were separated by sodium dodecyl sulfate–polyacrylamide gel electrophoresis (SDS-PAGE) and blotted to polyvinylidene difluoride (PVDF) membranes. DNP-containing proteins were then immunostained using rabbit anti-DNP antiserum (1:500; Sigma, St Louis, MO) and goat anti-rabbit IgG conjugated to horseradish peroxidase (HRP) (1:2000; Sigma). Blots were developed by enhanced chemiluminescence (ECL) using the Western Lightning ECL™ kit from Perkin-Elmer (Boston, MA). The developed films were scanned in a Hewlett Packard Scanjet 4890 and the images quantified using the NIH image analysis program version 1.63. Lane intensities in the oxyblot were normalized by the corresponding coomassie brilliant blue staining.
Assessment of Cytoskeletal Protein Levels by Western Blotting
Aliquots (5 µg) from spinal cord homogenates were separated by SDS-PAGE on 10% polyacrylamide gels and blotted against PVDF membranes. Blots were probed with antibodies against NFH (1:1000, rabbit polyclonal; Chemicon, Temecula, CA), NFM (1:4000, rabbit polyclonal; Chemicon), NFL (1:1000, mouse monoclonal; Chemicon), β-tubulin (1:1000, mouse monoclonal; Sigma) and β-actin (1:1000, mouse monoclonal; Abcam, Cambridge, MA) followed by incubation with the appropriate HRP-conjugated secondary antibody. Blots were developed by ECL and analyzed as described above. Band intensities were normalized by the corresponding coomassie brilliant blue staining of the entire lane.
Quantification of Carbonylation Levels of Individual Proteins
Tissue proteins (1 mg), dissolved in 200 µl of 2% SDS, were incubated at room temperature with 5 mM biotin-hydrazide (Sigma). After 60 min, proteins were precipitated with 1 ml of acetone at -20 °C and collected by centrifugation at 10,000×g for 10 min. Pellets were washed three times with 1 ml of acetone–water (3:1, v/v) and dissolved in 100 µl of 50 mM hepes buffer pH 7.5 containing 1% SDS and 100 mM NaCl. The solutions were diluted 20-fold with 100 mM NaCl and centrifuged at 10,000×g for 10 min to remove any aggregated material. The supernatants were then incubated for 1 h at 20 °C with 50 µl of streptavidin-agarose (EMD Biosciences, San Diego, CA) previously equilibrated in 50 mM hepes buffer pH 7.5 containing 0.05% SDS and 100 mM NaCl (buffer A). The resin was washed five times with 500 µl of buffer A, 4-times with buffer A containing 1 M NaCl, and once with buffer A without NaCl. Bound-proteins were eluted from the resin with 100 µl of SDS-sample buffer containing 1% 2-mercaptoethanol. Aliquots from the total and bound fractions were separated by SDS-PAGE on 10% polyacrylamide gels and blotted against PVDF membranes. Blots were probed with antibodies against NFH, NFM, NFL, β-tubulin and β-actin, followed by incubation with the appropriate HRP-conjugated secondary antibody. Blots were developed by ECL, and band intensities in the streptavidin-bound and total fraction were used to calculate the percentage of oxidized protein.
Proteolysis of Carbonylated Cytoskeletal Proteins in a Cell-Free System
To determine the role of calpain at removing oxidized protein in vitro, spinal cord homogenates from EAE animals (1 mg of protein), suspended in HEN buffer containing 10 mM CaCl2, 1 mM dithiothreithol and 2 µM epoxomicin, were incubated for 10 min at 25 °C with or without calpeptin (2 µM). To assess the role of proteasomes at removing oxidized protein in vitro, spinal cord homogenates from EAE animals (1 mg of protein), suspended in HEN buffer containing 5 mM EGTA and 2 µM calpeptin, were incubated for 1 h at 25 °C with or without epoxomicin (2 µM). After incubation, reaction was stopped by addition of 5 µl of protease inhibitor cocktail I (RPI Corp., Mt Prospect, IL). Proteins were then derivatized with biotin-hydrazide and the percentage of carbonylated NFH, NFM, NFL, β-tubulin and β-actin was determined using the pull-down/western blotting procedure.
Statistical Analysis
Results were analyzed for statistical significance with Student’s unpaired t-test or one-way ANOVA and post-hoc multiple comparison test GraphPad Prism® (version 4) program (GraphPad Software Inc., San Diego, CA).
Results
Neurological Symptoms of EAE Rats are not Altered by Intrathecal Administration of Calpeptin or Epoxomicin
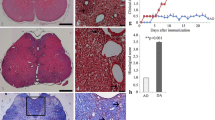
Following immunization with MBP, Lewis rats experience an acute and monophasic inflammation of the spinal cord resulting in clinical disability. Symptoms were graded according to the following scale: 0, no symptoms; 1, tail weakness; 1.5, clumsy gait; 2, hind limb paresis; 2.5, partial hind limb dragging; 3, hind limb paralysis; 3.5, hind limb paralysis with fore limb paresis; 4, complete paralysis; 5, moribund. As in our previous study, the onset of neurological symptoms began at 9–11 days post-immunization (dpi) [18]. The first day animals started exhibiting neurological disease, clinical score 1 or greater, an i.t. injection was performed as described in “Materials and Methods.” Animals injected with antigen that did not show symptoms by 11 dpi were excluded from our analysis. EAE rats were treated with DMSO (vehicle), the calpain inhibitor calpeptin, or the proteasome inhibitor epoxomicin. Animals were monitored for clinical disease for 48 h after i.t. injection and then sacrificed. As shown in Fig. 1, clinical disease in the three groups continues to progress at the same rate after injection. Furthermore, using one-way ANOVA, we found that there is no statistical difference in the clinical scores of the three groups at the time of injection (p = 0.466) and at the time of euthanasia (p = 0.554).
Intrathecal injection of calpeptin or epoxomicin does not affect the clinical course of EAE. Upon the first signs of clinical disease (9–11 dpi), EAE rats received a single i.t. injection of calpeptin (Clp, n = 11), epoxomicin (Epo, n = 9) or the vehicle DMSO (Veh, n = 15). Clinical disability scores were measured at the time of injection and the time of euthanasia (i.e. 48 h later) using the scale described in the “Results” section. The average clinical scores are expressed as mean ± SEM. Unpaired t-test was used to determine statistical significance between scores at time of injection and time of euthanasia for each group. One-way ANOVA was employed to compare statistical significance between scores of the three groups at the time of injection and time of euthanasia
Intrathecal Inhibitor Treatment Reduces Calpain or Proteasome Activity in Spinal Cords of EAE Rats
As shown in Fig. 2a, calpain activity is reduced in calpeptin-treated animals to 78.3% ± 8.3% of the levels of vehicle-treated EAE animals, while epoxomicin treatment does not affect calpain activity (106.3% ± 12.4%). Calpeptin has been shown to inhibit lysosomal proteases [25]. However, in our system we found that calpeptin treatment does not change the activity of the thiol protease cathepsin B (data not shown). It is important to note that we chose a dose of 4 µg of calpeptin (20–23 µg/kg) per animal based on preliminary studies in our laboratory showing that i.t. injections of this dosage inhibit calpain activity by 29–33% in non-EAE animals. Inhibition levels are reached 4 h after i.t. injection and remain steady up to 48 h post-injection. A 2 µg/kg dose does not reduce calpain activity while a 200 µg/kg dose does not offer significantly higher inhibition than the chosen dose (data not shown).
Specific inhibition of calpain and proteasome activity by intrathecal injection of calpeptin and epoxomicin in EAE rats. After 48 h of a single i.t. injection of calpeptin (Clp, n = 11), epoxomicin (Epo, n = 9) or the vehicle DMSO (Veh, n = 15), animals were euthanized and spinal cord segments L1 - L3 were dissected and homogenized in HEN buffer. Aliquots of the homogenates were used to determine calpain activity (a) and the proteasome chymotrypsin-like activity (b) as described in “Materials and Methods”. Values are expressed as a percentage of those obtained in vehicle-treated animals and represent the mean ± SEM of the number of animals indicated above. Proteasome and calpain activity were analyzed for statistical significance to determine difference from vehicle-injected EAE animals using one-way ANOVA. Dotted lines represent the average calpain or proteasome activity from 4 age-matched untreated non-EAE Lewis rats
Figure 2b shows that proteasome activity in the spinal cord of epoxomicin-treated EAE rats is significantly reduced to 76.4% ± 8.7% (mean ± SEM) of that in the vehicle-treated animals, while calpeptin treatment has no effect on proteasome activity (111.8% ± 21.5%). As in the case of calpeptin, a dose of 4 µg epoxomicin yields a constant inhibition of proteasome activity from 4 to 48 h post injection. A 10× higher dose does not produce significantly higher proteasome inhibition (data not shown).
Calpain Inhibition Increases the Accumulation of Oxidized Proteins in EAE
An oxyblot analysis of spinal cord proteins was carried out to ascertain whether calpain and/or the proteasome play a role in the elimination of carbonylated proteins in acute EAE. A representative western blot detecting carbonylated spinal cord proteins (i.e. oxyblot) of 4 vehicle-, 3 calpeptin-, and 3 epoxomicin-injected EAE mice is presented in Fig. 3a, b. The results show that the carbonyl content of several protein bands in the calpeptin injected EAE animals is higher than those in vehicle treated EAE. Quantitative analysis of the oxyblots reveals that total protein carbonyl levels in calpeptin treated EAE spinal cords is ~ 64% higher than that in vehicle treated EAE spinal cords (Fig. 3c). No significant increase in total protein carbonyls is seen in epoxomicin treated EAE, although the intensity of some bands is clearly higher. The above findings suggest that calpain acts as a main clearance mechanism to eliminate these damaged proteins in the disease tissue.
Calpain inhibition increases the amount of carbonylated proteins in EAE. Spinal cord proteins (5 µg) from EAE animals i.t. injected with calpeptin (Clp, n = 11), epoxomicin (Epo, n = 9) or vehicle (Veh, n = 15) for 48 h were derivatized with dinitrophenyl hydrazide and separated by SDS-PAGE. Carbonylated proteins were detected by western blotting using an anti-DNP antibody as described in “Materials and Methods”. a, b Representative oxyblot and coomassie blue stained PVDF membrane of spinal cord proteins from four vehicle-, three calpeptin-, and three epoxomicin-injected EAE animals. c Protein carbonyl levels in the three treatment groups was determined as described in “Materials and Methods”. Values are expressed as a percentage of the average carbonylation in vehicle-injected EAE spinal cords and represent the mean ± SEM of the number of animals indicated above. Dotted lines represent the average protein carbonylation from 4 age-matched uninjected non-EAE Lewis rats. Data were analyzed for statistical significance from that of vehicle-injected EAE animals using one-way ANOVA
Intrathecal Injection of Calpeptin, but not Epoxomicin, Reduces the Degradation of Cytoskeletal Proteins in EAE
We have previously shown that the integrity of the neuronal cytoskeletal network in the spinal cord of EAE rats is greatly compromised, with a significant reduction in the levels of NFPs and β-tubulin compared to CFA-treated controls [18]. To determine whether calpain and/or the proteasome are responsible for removal of the proteins, we carried out a western blot analysis of spinal cord proteins from calpeptin and epoxomicin injected EAE rats. Figure 4 shows that a single i.t. injection with the calpain inhibitor calpeptin at the onset of neurologic symptoms partially prevents the degradation of all NFPs, β-tubulin and β-actin in the spinal cord of EAE animals. In contrast, proteasome inhibition with epoxomicin does not prevent the clearance of these proteins.
Inhibition of calpain, but not the proteasome, reduces the degradation of NFPs and β-tubulin and β-actin in EAE. Spinal cord proteins (5 µg) from EAE animals i.t. injected with calpeptin (Clp, n = 11), epoxomicin (Epo, n = 9) or vehicle (Veh, n = 15) for 48 h were analyzed by western blotting as described in “Materials and Methods”. Blots were developed with antibodies against NFH (a), NFM (b), NFL (c), β-tubulin (d) and β-actin (e). Band intensities were normalized by the corresponding coomassie blue staining of the entire lane. Values are expressed as percentage of the average in vehicle-injected EAE spinal cords and represent the mean ± SEM of the number of animals indicated above. Data were analyzed for statistical significance from that of vehicle-injected EAE animals using one-way ANOVA. f Representative western blot samples from 3 vehicle-, 3 calpeptin- and 3 epoxomicin-treated EAE rats
Oxidation Levels of Some Cytoskeletal Proteins are Altered by Partial Inhibition of Proteasome or Calpain
We next investigated whether there are changes in the specific oxidation of cytoskeletal proteins (i.e. the percentage of total protein that is modified by carbonylation) in EAE animals treated with calpain or epoxomicin. An increase in specific oxidation upon treatment with an inhibitor would support previous in vitro studies that suggest calpain [13] or the proteasome [11, 26] preferentially target oxidized proteins for degradation. Quantification of the extent of carbonylation of individual proteins was performed using a pull-down/western blot procedure. To this end, protein carbonyl moieties from control and EAE spinal cord homogenates were first converted into biotinylated residues by reaction with biotin-hydrazide. Biotin-containing proteins were then isolated with streptavidin-agarose and analyzed by western blotting employing antibodies against the three NFPs, β-tubulin and β-actin. Figure 5 depicts the % oxidation of each NFP in the three injection groups expressed as relative to the average vehicle-injected EAE animals. The results show no significant differences in the specific oxidation of the three NFPs after treatment with calpeptin compared to vehicle-injected EAE animals. Epoxomicin inhibition of the proteasome, on the other hand, leads to an increase in the percentage of oxidized NFM and NFH. Thus, although calpain is the major degradation pathway for NFPs in EAE, these in vivo studies do not support the idea that oxidized forms of these proteins are preferentially targeted toward degradation by calpain. Conversely, while the proteasome is not the chief pathway for the removal of cytoskeletal proteins, it appears to contribute to the degradation of oxidized NFM and NFH. As shown in Fig. 6, carbonylated β-tubulin and carbonylated β-actin are preferentially degraded by calpain in EAE, while proteasome inhibition has no effect on the oxidation status of these proteins.
Proteasome, but not calpain, inhibition increases the amount of carbonylated NFH and NFM in EAE. Spinal cord proteins from EAE animals i.t. injected with calpeptin (Clp, n = 11), epoxomicin (Epo, n = 9) or vehicle (Veh, n = 15) for 48 h were derivatized with biotin hydrazide and carbonylated proteins were isolated with streptavidin-agarose as described in “Materials and Methods”. Total and bound fractions were analyzed by SDS-PAGE followed by western blotting for the three NFPs. The percentage of NFH (a), NFM (b) and NFL (c) that is modified by carbonylation (i.e. % oxidized protein) was calculated in the three experimental groups. Values are expressed as relative to the average in vehicle-injected EAE spinal cords and represent the mean ± SEM of the number of animals indicated above. Data were analyzed for statistical significance from that of vehicle-injected EAE animals using one-way ANOVA
Calpain, but not proteasome, inhibition increases the amount of carbonylated β-tubulin and β-actin in EAE. Spinal cord proteins from EAE animals i.t. injected with calpeptin (Clp, n = 10), epoxomicin (Epo, n = 9) or vehicle (Veh, n = 15) for 48 h were derivatized with biotin hydrazide and carbonylated proteins were isolated with streptavidin-agarose as described in “Materials and Methods”. Total and bound fractions were analyzed by SDS-PAGE followed by western blotting for β-tubulin and β-actin. The percentage of β-tubulin (a) and β-actin (b) that is modified by carbonylation (i.e. % oxidized protein) was calculated in the three experimental groups. Values are expressed as relative to the average in vehicle-injected EAE spinal cords and represent the mean ± SEM of the number of animals indicated above. Data were analyzed for statistical significance from that of vehicle-injected EAE animals using one-way ANOVA
Differential Susceptibility of Carbonylated Cytoskeletal Proteins to Calpain Digestion in a Cell-Free System
Finally, we studied the susceptibility of the oxidized cytoskeletal proteins to endogenous calpain or proteasomes in a cell-free system. To find out if calpain is involved in the removal of carbonylated cytoskeletal proteins, spinal cord homogenates from EAE rats (pre-treated with epoxomicin to inhibit endogenous proteasome activity and with 10 mM CaCl2 to activate calpain) were incubated in the absence or presence of calpeptin. After 10 min, the proportion of carbonylated NFPs, β-tubulin and β-actin was determined using the pull-down/western blot procedure described above. The results clearly show that calpain preferentially removes the carbonylated forms of NFH (Fig. 7), β-tubulin and β-actin in vitro (Fig. 8). Carbonylated NFM and NFL are apparently degraded at the same rate as the non-carbonylated species, but the disappearance of these two proteins from the homogenate is so rapid that it is difficult to ascertain if that is indeed the case. To determine if the proteasome 20S particle also participates in the removal of carbonylated cytoskeletal proteins, spinal cord homogenates (pre-treated with calpeptin and EGTA to inhibit endogenous calpain) were incubated for 1 h in the absence or presence of epoxomicin. As shown in Figs. 7 and 8, degradation of the carbonylated forms of NFPs, β-tubulin and β-actin is unaffected by epoxomicin, indicating that the endogenous 20S proteasome activity does not preferentially removes oxidized cytoskeletal proteins in this cell-free system.
Carbonylated NFH is preferentially degraded by calpain in a cell-free system. Spinal cord homogenates from EAE rats were incubated at 25 °C under various conditions as described in “Material and Methods”. After incubation, proteins were derivatized with biotin hydrazide and carbonylated proteins were isolated with streptavidin-agarose. Total and bound fractions were analyzed by SDS-PAGE followed by western blotting for the three NFPs. The percentage of NFH (a), NFM (b) and NFL (c) that is modified by carbonylation (i.e. % oxidized protein) was calculated in the four experimental groups. Values are expressed as relative to their respective controls and represent the mean ± SEM of 3–6 separate experiments. Data were analyzed for statistical significance using unpaired t-test
Carbonylated β-tubulin and β-actin are also substrates of calpain in a cell-free system. Spinal cord homogenates from EAE rats were incubated at 25 °C under various conditions as described in “Material and Methods”. After incubation, proteins were derivatized with biotin hydrazide and carbonylated proteins were isolated with streptavidin-agarose. Total and bound fractions were analyzed by SDS-PAGE followed by western blotting. The percentage of β-tubulin (a) and β-actin (b) that is modified by carbonylation (i.e. % oxidized protein) was calculated in the four experimental groups. Values are expressed as relative to their respective controls and represent the mean ± SEM of 3–8 separate experiments. Data were analyzed for statistical significance using unpaired t-test
Discussion
Cytoskeletal proteins are established carbonylation targets in several CNS disorders [7, 27], including MS [19] and EAE [18, 20]. More importantly, carbonylation of cytoskeletal proteins is known to have deleterious effects on the macromolecule structures. For example, actin filaments and microtubules both destabilize and disassemble upon oxidation of their protein components [28,29,30,31]. The secondary structure of neurofilaments is also altered when the individual proteins become carbonylated [32], often leading to the formation of dense aggregates [33]. Thus, it is important to investigate the mechanism underlying the removal of the damaged forms of these proteins, especially in pathological conditions.
The present study is a direct continuation of our previous work on carbonylation of cytoskeletal proteins in acute MBP-induced EAE in Lewis rats [18], and it was aimed to identify the proteolytic system(s) responsible of eliminating oxidized cytoskeletal proteins in vivo. The approach selected was to inhibit separately the two major degradation pathways for oxidized proteins: the calcium-dependent cysteine protease calpain and the proteasome. Calpeptin, a membrane permeable inhibitor that targets both m-calpain and µ-calpain [34], was used to inhibit calpain activity in the EAE spinal cord. Calpeptin was delivered directly into the spinal cord at the T12-L1 junction using an i.t. injection. Pilot studies proved this drug delivery method to be far superior to intraperitoneal injections at inhibiting calpain for a sustained period after a single injection. Using this method, we were able to reduce calpain activity by ~ 22%, as measured with a fluorescence-based protease activity assay. Although systemic administration of calpain inhibitors has been shown to improve clinical disease in EAE Lewis rats [22, 35], we found that a single i.t. injection with the inhibitor starting at the first sign of clinical disease does not alter the disease course. This was critical to our experimental paradigm, so differences seen in protein oxidation and cytoskeletal degradation could be attributed to changes in enzyme activity and not disease severity. To inhibit the proteasome, we chose epoxomicin, a naturally occurring and highly potent peptidyl epoxyketone. This agent is quite specific for the proteasome, inhibiting the chymotrypsin-like activity and reducing the trypsin-like and caspase-like catalytic rates [36], and has been used successfully for proteasome inhibition in the spinal cord in a chronic pain model [37]. Although systemic administration of protesome inhibitors is known to decrease inflammation and reduce neurological symptoms in EAE [38, 39], we found that a single i.t. injection of epoxomicin does not interfere with the progression of EAE.
Our results show that the partial inhibition of calpain for 48 h leads to increased accumulation of total protein carbonyls, as measured by oxyblot. Degradation of the NFPs, β-tubulin and β-actin are also significantly reduced in the animals with inhibited calpain activity. However, we were unable to detect significant changes in the specific carbonylation of NFPs. Thus, we conclude that while calpain is an important degradation mechanism for cytoskeletal proteins, it does not remove carbonylated NFPs in this animal model of MS. In contrast, oxidized β-tubulin and β-actin are removed by calpain at a higher rate than their non-oxidized forms. Thus, the increase in the amount of protein cabonyls observed in the oxyblots after treatment with calpeptin is probably due to (i) a preferential degradation of some oxidized proteins by calpain (e.g. β-tubulin and β-actin), and (ii) a decreased proteolysis of certain proteins (e.g. NFPs) that are major oxidized species. We also found that, in a cell-free system, the carbonylated forms of NFH, β-tubulin and β-actin are more susceptible to calpain degradation than their non-oxidized forms. Results for NFM and NFL were less clear as these proteins are almost completely digested within the 10 min-incubation. The higher resistance of NFH to digestion by calpain in the presence of calcium has been already described and seems to be due to its binding to calmodulin [40].
Partial inhibition of the proteasome with epoxomicin was found to cause the accumulation of carbonylated NFM and NFH but has no effect on the substantial degradation of cytoskeletal proteins that takes place in EAE. In a cell-free system, epoxomicin does not lead to accumulation of the oxidized forms of any of the cytoskeletal proteins studied. This could be due to the short incubation period (1 h) or to the absence of ATP, which is necessary to remove proteins by a ubiquitin-dependent mechanism via the 26S proteasome. The latter possibility would suggest that the 26S proteasome rather than the 20S particle alone mediates the removal of oxidized NFH and NFM in vivo. Interestingly, it has been shown that degradation of NFPs in vitro is stimulated by addition of ATP and ubiquitin [41].
Taken as a whole, our findings suggest that carbonylation is not a contributing factor to cytoskeleton removal by calpain in EAE. However, it is important to consider that after the i.t. injection we achieved only a 22% and 24% decrease in calpain and proteasome activity, respectively. These reductions in enzyme activity are significant and cause considerable biochemical changes in protein oxidation and cytoskeletal degradation. Yet, it could be argued that the remaining calpain or proteasome activity might be sufficient to preferentially remove some oxidized proteins. The major strength of the present study is that it was conducted in an animal model of a human disease. This is important since previous studies designed to identify the proteolytic system responsible for removal of carbonylated proteins have been carried out in cultured cells or in cell-free free systems under oxidative stress conditions that may differ from those taking place in disease states.
Abbreviations
- AMC:
-
7-Aminomethyl-4-coumarin
- DMSO:
-
Dimethyl sulfoxide
- DNP:
-
Dinitrophenyl
- dpi:
-
Days post-immunization
- EAE:
-
Experimental autoimmune encephalomyelitis
- ECL:
-
Enhanced chemioluminescence
- HRP:
-
Horseradish peroxidase
- i.t.:
-
Intrathecal
- MBP:
-
Myelin basic protein
- MS:
-
Multiple sclerosis
- NFH:
-
Neurofilament heavy (200 kDa) protein
- NFL:
-
Neurofilament light (69 kDa) protein
- NFM:
-
Neurofilament medium (150 kDa) protein
- NFPs:
-
Neurofilament proteins
- PAGE:
-
Polyacrylamide gel electrophoresis
- PVDF:
-
Polyvinylidene difluoride
- SDS:
-
Sodium dodecyl sulfate
References
Gilgun-Sherki Y, Melamed E, Offen D (2004) The role of oxidative stress in the pathogenesis of multiple sclerosis: the need for effective antioxidant therapy. J Neurol 251:261–268
LeVine SM (1992) The role of reactive oxygen species in the pathogenesis of multiple sclerosis. Med Hypotheses 39:271–274
Bizzozero OA (2009) Protein carbonylation in neurodegenerative and demyelinating CNS diseases. In: Lajtha A, Banik N, Ray S (eds) Handbook of neurochemistry and molecular neurobiology. Springer, New York, pp. 543–562
Berlett BS, Stadtman ER (1997) Protein oxidation in aging, disease, and oxidative stress. J Biol Chem 272:20313–20316
Dalle-Donne I, Giustarini D, Colombo R, Rossi R, Milzani A (2003) Protein carbonylation in human diseases. Trends Mol Med 9:169–176
Nystrom T (2005) Role of oxidative carbonylation in protein quality control and senescence. EMBO J 24:1311–1317
Aksenov MY, Aksenova MV, Butterfield DA, Geddes JW, Markesbery WR (2001) Protein oxidation in the brain in Alzheimer’s disease. Neurosci 103:373–383
Floor E, Wetzel MG (1998) Increased protein oxidation in human sustantia nigra pars compacta in comparison with basal ganglia and prefrontal cortex measured with an improved dinitrophenylhydrazine assay. J Neurochem 70:268–275
Ferrante RJ, Browne SE, Shinobu LA, Bowling AC, Baik MJ, MacGarvey U, Kowall NW, Brown RH, Beal MF (1997) Evidence of increased oxidative damage in both sporadic and familial amyotrophic lateral sclerosis. J Neurochem 69:2064–2074
Bizzozero OA, DeJesus G, Callahan K, Pastuszyn A (2005) Elevated protein carbonylation in the brain white matter and gray matter of patients with multiple sclerosis. J Neurosci Res 81:687–695
Grune T, Reinheckel T, Davies KJ (1997) Degradation of oxidized proteins in mammalian cells. FASEB J 11:526–534
Zheng J, Bizzozero OA (2010) Reduced proteasomal activity contributes to the accumulation of carbonylated proteins in chronic experimental autoimmune encephalomyelitis. J Neurochem 115:1556–1567
Troncoso JC, Costello AC, Kim JH, Johnson GV (1995) Metal-catalyzed oxidation of bovine neurofilaments in vitro. Free Radic Biol Med 18:891–899
Banik NL, Shields DC (2000) The role of calpain in neurofilament protein degradation associated with spinal cord injury. Methods Mol Biol 144:195–201
Shields DC, Banik NL (1998) Upregulation of calpain activity and expression in experimental allergic encephalomyelitis: a putative role for calpain in demyelination. Brain Res 794:68–74
Hassen GW, Feliberti J, Kesner L, Stracher A, Mokhtarian F (2008) Prevention of axonal injury using calpain inhibitor in chronic progressive experimental autoimmune encephalomyelitis. Brain Res 1236:206–215
Gold R, Hartung HP, Toyka KV (2000) Animal models for autoimmune demyelinating disorders of the nervous system. Mol Med Today 6:88–91
Smerjac SM, Bizzozero OA (2008) Cytoskeletal protein carbonylation and degradation in experimental autoimmune encephalomyelitis. J Neurochem 105:763–772
Hilgart AA, Bizzozero OA (2008) Carbonylation of major cytoskeletal proteins in multiple sclerosis. J Neurochem 104(Suppl.1):PTW06–P03
Zheng J, Bizzozero OA (2010) Accumulation of protein carbonyls within cerebellar astrocytes in murine experimental autoimmune encephalomyelitis. J Neurosci Res 88:3376–3385
Milligan ED, Sloane EM, Langer SJ, Cruz PE, Chacur M, Spataro L, Wieseler-Frank J, Hammack SE, Maier SF, Flotte TR, Forsayeth JR, Leinwand LA, Chavez R, Watkins LR (2005) Controlling neuropathic pain by adeno-associated virus driven production of the anti-inflammatory cytokine, interleukin-10. Mol Pain 1:9–22
Hassen GW, Feliberti J, Kesner L, Stracher A, Mokhtarian F (2006) A novel calpain inhibitor for the treatment of acute experimental autoimmune encephalomyelitis. J Neuroimmunol 180:135–146
Rodgers KJ, Dean RT (2003) Assessment of proteasome activity in cell lysates and tissue homogenates using peptide substrates. Int J Biochem Cell Biol 35:716–727
Sitte N, Huber M, Grune T, Ladhoff A, Doecke W, Von Zglinicki T, Davies JA (2000) Proteasome inhibition by lipofuscin/ceroid during postmitotic aging of fibroblasts. FASEB J 14:1490–1498
Siklos M, BenAissa M, Thatcher GRJ (2015) Cysteine proteases as therapeutic targets: does selectivity matters? A systematic review of calpain and cathepsin inhibitors. Acta Pharm Sin B 5:506–519
Poppek D, Grune T (2006) Proteasomal defense of oxidative protein modifications. Antioxid Redox Signal 8:173–184
Muntane G, Daldo E, Martinez A, Rey MJ, Avila J, Perez M, Portero M, Pamplona R, Ayala V, Ferrer I (2006) Glial fibrillary acidic protein is a major target of glycoxidative and lipoxidative damage in Pick’s disease. J Neurochem 99:177–185
Dalle-Donne I, Rossi R, Giustarini D, Gagliano N, Lusini L, Milzani A, Di Simplicio P, Colombo R (2001) Actin carbonylation: from a simple marker of protein oxidation to relevant signs of severe functional impairment. Free Radic Biol Med 31:1075–1083
Ozeki M, Miyagawa-Hayashino A, Akatsuka S, Shirase T, Lee WH, Uchida K, Toyokuni S (2005) Susceptibility of actin to modification by 4-hydroxy-2-nonenal. J Chromatogr 827:119–126
Banan A, Fitzpatrick L, Zhang Y, Keshavarzian A (2001) OPC-compounds prevent oxidant-induced carbonylation and depolymerization of the F-actin cytoskeleton and intestinal barrier hyperpermeability. Free Radic Biol Med 30:287–298
Neely MD, Boutte A, Milatovic D, Montine TJ (2005) Mechanisms of 4-hydroxynonenal-induced neuronal microtubule dysfunction. Brain Res 1037:90–98
Gelinas S, Chapados C, Beauregard M, Gosselin I, Martinoli MG (2000) Effect of oxidative stress on stability and structure of neurofilament proteins. Biochem Cell Biol 78:667–674
Smith MA, Rudnicka-Nawrot M, Richey PL, Praprotnik D, Mulvihill P, Miller CA, Sayre LM, Perry G (1995) Carbonyl-related posttranslational modification of neurofilament protein in the neurofibrillary pathology of Alzheimer’s disease. J Neurochem 64:2660–2666
Saito K, Nixon RA (1993) Specificity of calcium-activated neutral proteinase (CANP) inhibitors for human mu CANP and mCANP. Neurochem Res 18:231–233
Guyton MK, Das A, Samantaray D, Wallace GC, Butler JT, Ray SK, Banik NL (2010) Calpeptin attenuated inflammation, cell death, and axonal damage in an animal model of multiple sclerosis. J Neurosci Res 88:2398–2408
Meng L, Mohan R, Kwok BH, Elofsson M, Sin N, Crews CM (1999) Epoxomicin, a potent and selective proteasome inhibitor, exhibits in vivo antiinflammatory activity. Proc Natl Acad Sci USA 96:10403–10408
Ossipov MH, Bazov I, Gardell LR, Kowal J, Yakovleva T, Usynin I, Ekstrom TJ, Porreca F, Bakalkin G (2007) Control of chronic pain by the ubiquitin proteasome system in the spinal cord. J Neurosci 27:8226–8237
Hosseini H, Andre P, Lefevre N, Viala L, Walzer T, Peschanski M, Lotteau V (2001) Protection against experimental autoimmune encephalomyelitis by a proteasome modulator. J Neuroimmunol 118:233–244
Vanderlugt CL, Rahbe SM, Elliott PJ, Dal Canto MC, Miller SD (2000) Treatment of established relapsing experimental autoimmune encephalomyelitis with the proteasome inhibitor PS-519. J Autoimmun 14:205–211
Johnson VWG, Greewood JA, Costello AC, Troncoso JC (1991) The regulatory role of calmodulin in the proteolysis of individual neurofilament proteins by calpain. Neurochem Res 16:869–873
Gao JP, Letterier JF (1995) Possible involvement of ubiquitination in neurofilament degradation. Biochem Biophys Res Commun 217:528–539
Acknowledgements
The authors wish to thank Dr. Erin Milligan from the Department of Neurosciences at UNM-SOM for helping with the i.t. injections. This work was supported by PHHS Grant NS057755 from the National Institutes of Health.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Smerjac, S.M., Zheng, J., Hu, CL. et al. The Role of Calpain and Proteasomes in the Degradation of Carbonylated Neuronal Cytoskeletal Proteins in Acute Experimental Autoimmune Encephalomyelitis. Neurochem Res 43, 2277–2287 (2018). https://doi.org/10.1007/s11064-018-2648-y
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11064-018-2648-y