Abstract
Purpose
To evaluate surgical resection with brachytherapy placement as a salvage treatment in patients with recurrent high-grade meningioma who exhausted prior external beam treatment options.
Methods
Single-center retrospective review of our institutional experience of brachytherapy implantation from 2012 to 2018. The primary outcome of the study was progression free survival (PFS). Secondary outcomes included overall survival (OS) and complications. A matched cohort of patients not treated with brachytherapy over the same time period was evaluated as a control group. All patients had received prior radiation treatment and underwent planned gross total resection (GTR) surgery.
Results
A total of 27 cases were evaluated. Compared with prior treatment, brachytherapy implantation demonstrated a statistically significant improvement in tumor control [HR 0.316 (0.101 − 0.991), p = 0.034]. PFS-6 and PFS-12 were 92.3% and 84.6%, respectively. Compared with the matched control cohort, brachytherapy treatment demonstrated improved PFS [HR 0.310 (0.103 − 0.933), p = 0.030]. Overall survival was not statistically significantly different between groups [HR 0.381 (0.073 − 1.982), p = 0.227]. Overall postoperative complications were comparable between groups, although there was a higher incidence of radiation necrosis in the brachytherapy cohort.
Conclusion
Brachytherapy with planned GTR improved PFS in recurrent high-grade meningioma patients who exhausted prior external beam radiation treatment options. Future improvement of brachytherapy dose delivery methods and techniques may continue to prolong control rates and improve outcomes for this challenging group of patients.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
Outcomes following retreatment for recurrence in high-grade meningiomas are poor [1]. Repeat treatment is associated with increased complication rates [2, 3], worsened progression-free (PFS) [4,5,6,7] and overall survival (OS) [2, 4, 5], and diminishing treatment options with each subsequent recurrence. While chemotherapy and immunotherapy clinical trials are actively being investigated, no systemic agent has proven efficacious to date in halting meningioma growth or preventing recurrence [1, 8, 9]. Consequently, there is a population of patients with recurrent meningioma with high-grade pathology (WHO grade II/III) who have undergone prior surgery, maximized external beam radiation treatment options, and may have failed trials of medical therapy.
Brachytherapy is an attractive alternative treatment strategy for select cases of recurrent high-grade meningioma, as it allows for delivery of substantial radiation doses to the margins of a resection cavity with high conformality, delivered over the lifespan of the radioactive seeds. This is particularly appealing following meningioma resection, as the incidence of local recurrence due to microscopic disease along the dura or at the tumor-brain interface is high [10]. Although brachytherapy has historically been used in neurosurgery following surgical resection or by stereotactic implantation for brain metastases [11,12,13,14,15,16,17,18,19,20,21,22], and gliomas [23,24,25,26], case reports and heterogeneous case series describing its use in meningioma have been published [27,28,29,30,31,32,33,34,35].
For meningioma patients undergoing brachytherapy seed placement, patient selection criteria, surgical technique, and the outcomes of brachytherapy placement have been mixed in the literature to date [28, 29, 33, 35]. In recent years, our institution has increasingly utilized brachytherapy seed placement as an adjunct to surgical resection for cases of recurrent high-grade meningioma that have proven refractory to prior treatment strategies. Specifically, we consider brachytherapy seed placement for cases that have maximized options for additional external beam radiation treatment yet remain amenable to surgical resection. Herein, we report the characteristics of our patient cohort, examine the safety and efficacy of brachytherapy implantation, and compare outcomes to a matched cohort of patients treated during the same time period.
Methods
Patient characteristics
A retrospective study of meningioma outcomes from 2012 to 2018 was performed with approval of the institutional review board [IRB: 2014P000427]. Given the retrospective nature of the study, informed consent was not obtained. For the treatment cohort, we identified all cases of brachytherapy seed implantation performed during this time. Patients with a recurrent high-grade meningioma that had maximized external beam radiation treatment options were considered for brachytherapy implantation. One patient who underwent brachytherapy seed placement was lost to follow-up immediately following surgery and subsequently suffered death of unknown cause; this patient was not included in the analysis.
Demographic, clinical, and radiation treatment variables were collected. WHO grade was reported according to the histopathological criteria at the time of the resection. Chromosomal copy number analyses were performed as previously described [36]. The Cytogenetic Abnormality Score (CAS) was calculated as the sum of a defined set of common chromosomal aberrations observed in meningiomas, as previously described [37].
Brachytherapy implantation
Our technique for brachytherapy seed implantation has been previously described [27]. Following planned gross total tumor resection (GTR, Simpson Grade 1–3) [10], brachytherapy seeds were implanted in conjunction with a radiation oncologist to determine dosage and distribution of the radiation source. A dosimetric goal of 100 Gy minimum peripheral dose to a 5 mm margin was planned for all cases, regardless of the isotope. Radioactive seeds (I-125 or Cs-131) were prepared into strands in an absorbable vicryl mesh with 1 cm spacing between seeds. Strands were lined along the contour of the resection cavity and dural margins, also with 1 cm spacing between each row of seeds. The seeds are fixed to the margins and cavity using fibrin glue. A postoperative computed-tomography (CT) scan is obtained to determine final seed placement and dose distribution.
Outcomes analyses
Treatment history including number of prior surgical resections, number and modality of prior radiation treatments (RTs), and any trials of medical treatment were recorded. The primary outcome of our study was PFS. Overall survival, patterns of recurrence, and complications were also assessed. Postoperative complications were reported based on the Common Terminology Criteria for Adverse Events (CTCAE; Version 4.0) [38].
In order to investigate the impact of brachytherapy on tumor behavior, we compared the brachytherapy cohort against two control arms. First, as all patients had a history of extensive pre-treatment and recurrence, patients were used as their own controls in order to capture tumor behavior. PFS was calculated from the intervention immediately before brachytherapy (surgery or RT) and compared with the PFS after brachytherapy, similar to other reports [33]. Second, a matched cohort of patients with recurrent high-grade meningiomas treated at our institution during the same time period without brachytherapy implantation was evaluated (matched control cohort). For the matched control cohort, all patients had histologically confirmed WHO grade II or III meningioma, a history of prior surgery and prior radiation treatment, and gross-total resection (GTR) of tumor at the recurrent operation.
PFS was calculated from the time of surgery to the time of local recurrence or death. Local recurrence was defined as the appearance or progression of nodular tumor growth on magnetic resonance imaging studies following treatment in the resection cavity or within 1.5 cm of the craniotomy. Dosimetry plans were merged with preoperative and postoperative imaging studies to evaluate the pattern of recurrence in relation to the radiation treatment field. Recurrences within the 100% isodose line were classified as in-field; recurrences outside of the 100% isodose line but within 1.5 cm of the craniotomy were classified as marginal. Classification of recurrence location was determined by an experienced neuroradiologist not involved in the treatment or study design (LH). Radiation necrosis was identified on serial postoperative imaging studies as gadolinium contrast enhancement surrounding the resection cavity and treatment field with associated T2-intense signal, when present. Severity of radiation necrosis was retrospectively categorized based on radiographic reports and clinical history.
The Strengthening the Reporting of Observational Studies in Epidemiology (STROBE) guidelines for cohort studies were utilized as the reporting guidelines for this study (https://www.strobe-statement.org).
Statistical analyses
All statistical analyses were performed using Stata Statistical Software (StataCorp., LLC, College Station, Texas). Chi-squared tests and independent-samples t tests were used when appropriate. Cox proportional hazard regression model was used to examine factors associated with recurrence in univariate and multivariate analyses. Statistical significance was defined as P < 0.05.
Results
Patient characteristics
Thirteen operations involving brachytherapy implantation were performed in eleven patients over the study period. Mean patient age at time of surgery was 63.5 years (range 34–89) and 69% of cases were in men (n = 9) (Table 1). The majority (77%, n = 10/13) of cases had WHO grade II pathology while the others (23%) were WHO grade III. Median follow-up from the time of first surgery was 10.4 years (mean 9.9 years, range 1.5–14.1 years); mean and median follow-up following brachytherapy implantation were both 36.9 months (range 7.4–80.5). Although GTR was intended for all cases, one case had a nodule of tumor noted at the edge of the resection on postoperative imaging (near-total resection, NTR).
Nearly all cases received the prescribed dose of 100 Gy (n = 10/13). The remaining cases received 75 Gy (n = 1), 80 Gy (n = 1), and 120 Gy (n = 1). Most operations were performed with implantation of I-125 seeds (n = 10/13); a subset of more recent cases was performed with Cs-131 seeds (n = 3). For I-125 patients, the median number of seeds used was 45 (range 9–80) with a median activity of 0.382 mCi per seed (range 0.287-0.454 mCi) and total activity of 12.84 mCi (range 4.1–29.7 mCi). For Cs-131 patients, the median number of seeds used was 50 (range 40–79) with a median activity of 3.77 mCi per seed (range 3.76–3.82 mCi) and total activity of 188 mCi (range 150.8–301.8 mCi). For the control cohort, 4 patients received adjuvant radiation treatment in the form of fractionated RT (30–59 Gy); the remainder did not receive additional adjuvant RT given their radiation history and concern for treatment-related toxicity secondary to additional external beam radiation.
Tumor control, survival, and complications following brachytherapy implantation
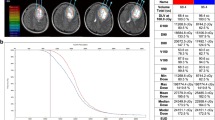
We sought to evaluate whether brachytherapy conferred any benefit to tumor control for these multiply treated high-grade meningioma patients. We first analyzed the time to recurrence for each patient for the tumor-directed treatment immediately preceding brachytherapy (surgery or RT) versus following brachytherapy. When PFS was compared, brachytherapy demonstrated a statistically significant improvement in tumor control (HR 0.316 (0.101–0.991), p = 0.034) (Fig. 1a). The PFS-6 and PFS-12 were 92.3% and 84.6%, respectively. Median PFS was not reached. For the five recurrences, the median time to recurrence was 14 months after brachytherapy implantation (range 6–31 months). Durability of control did not significantly differ between WHO grade II and III cases during the follow-up period (Fig. 1b).
Kaplan–Meier survival analyses. a PFS analysis before and after resection with brachytherapy placement demonstrating a statistically significant improvement in PFS following surgery with brachytherapy (P = 0.034). b PFS analysis of WHO Grade 2 versus Grade 3 tumors demonstrating no statistically significant difference (P = 0.885). c PFS analysis of the brachytherapy cohort compared to the matched control cohort demonstrating a statistically significant improvement in PFS in the brachytherapy group (P = 0.030). d Overall survival analysis of the brachytherapy cohort and matched control cohort demonstrating no statistically significant difference (P = 0.227). e Analysis of PFS considering in-field recurrences only, which demonstrates a statistically significant improvement in PFS compared to patients’ treatment prior to brachytherapy (P = 0.007). f Analysis of PFS considering in-field recurrences only, which demonstrates a statistically significant improvement in PFS compared to the matched control cohort (P = 0.002)
We then compared the PFS and OS of our brachytherapy cohort with 14 patients treated at our institution during the same period (matched control cohort). These control patients were matched by age, gender, number of prior surgeries, WHO grade, MIB-1 index, as well as cytogenetic signatures, compared to patients who underwent brachytherapy implantation (Table 1). Prior non-operative treatment history was also similar between groups (Table 2). Notably, all patients in both groups had received prior radiation treatment, with fractionated EBRT being the most common treatment modality in both groups. Brachytherapy treatment was associated with improved PFS [HR 0.310 (0.103–0.933), p = 0.030] (Fig. 1c). This did not retain statistical significance when patient age was included as a covariate [HR 0.354 (0.117–1.068), p = 0.065] (Table 3). There were two deaths in the brachytherapy cohort and five deaths in the control cohort. Overall survival was not statistically significantly different between groups [HR 0.381 (0.073–1.982), p = 0.227] (Fig. 1d).
A summary of complications in both cohorts according to CTCAE classification is summarized in Supplementary Table 1. Most notably, a higher incidence of radiation necrosis was observed in the brachytherapy cohort, with 3 patients requiring additional medical intervention beyond corticosteroids with the use of bevacizumab (CTCAE Class 3).
Patterns of recurrence following brachytherapy
We further investigated whether recurrence following brachytherapy related to failure to control disease within the treated area or inadequate field coverage by the distribution of brachytherapy seeds. Among the five recurrences in the brachytherapy-treated patients over the study period, two recurrences were classified as in-field (i.e. within the 100% isodose line) and three recurrences were marginal (i.e. within 1.5 cm of the craniotomy) (Fig. 2). Of the two in-field recurrences, one was the solitary case of NTR in our series. Considering in-field recurrences alone, PFS following brachytherapy implantation was significantly improved in the brachytherapy group compared to treatment before brachytherapy [HR 0.2097 (0.059–0.747), p = 0.007] and the matched control cohort [HR 0.147 (0.037-–0.578), p = 0.002] (Fig. 1e, f).
Illustrative case example of a marginal recurrence. a–c Post-operative CT-based dosimetry plan superimposed on 6-month follow-up MRI, axial (a), coronal (b), and sagittal (c), demonstrating the recurrent nodule anterior to the resection cavity. The recurrence was outside of the 50 Gy isodose line but within the limits of the craniotomy. d Three-dimensional representation of the radiation dose distribution with the recurrent nodule segmented (orange) and illustrated adjacent to the radiation field
Discussion
Rationale for brachytherapy
Outcomes of recurrent high-grade meningiomas are poor with high rates of re-recurrence, increased risk of subsequent intervention, and increased disease-related mortality [1,2,3,4,5,6,7]. For patients who have maximized external beam radiation options, surgery alone offers limited prolongation of PFS and OS. The addition of brachytherapy is an appealing option for these patients because of a number of factors. Namely: (1) its ability to be used as an adjunct to surgical resection, (2) the immediate delivery of radiation following maximal cytoreduction, (3) the administration of a high dose at the resection margin with a steep dose fall off, and (4) the ability to achieve a conformal, highly-targeted placement of radiation seeds to the areas at risk.
Efficacy of brachytherapy
In a cohort of heavily pretreated recurrent high-grade meningiomas, planned GTR followed by brachytherapy seed placement improved PFS. This was demonstrated in comparison to the cohort’s prior treatment history (Fig. 1a), as well as a matched cohort of patients treated at our institution during the same time period (Fig. 1c). Importantly, this was achieved with an acceptable complication profile despite the increased risks associated with retreatment in this challenging patient population (Supplementary Table 1).
Our results demonstrating brachytherapy efficacy and relatively high PFS-6 and PFS-12 rates compare favorably with prior reported series of meningioma patients [28,29,30,31, 33, 35]. We hypothesize this effect is attributable to several factors related to patient selection and treatment strategy. Most importantly, brachytherapy implantation was only pursued in cases amenable to GTR on preoperative evaluation. The radiation dose penetration to tissue adjacent to brachytherapy seed placement is limited, and thus brachytherapy seed placement adjacent to nodular tumor is known to have limited efficacy. Indeed, this was demonstrated in our series, as one of our cases of in-field recurrence occurred in the single case of NTR in our series.
The limited dose penetration of brachytherapy seeds may also explain the limited efficacy of brachytherapy in the literature. In a series of 49 patients wherein the majority of cases underwent subtotal resection (n = 31/49, 63%), the median time to progression was relatively poor (11.4 months) compared with our series, although their cohort did contain a higher proportion of WHO grade III tumors (n = 28/42, 67%) [28]. Similarly, a recent publication of 15 patients with recurrent high-grade meningioma and brachytherapy implantation reported a 47% subtotal resection rate (n = 7/15) and equally poor median time to progression (8.5 months for WHO grade 2 tumors, 4.5 months for WHO grade 3 tumors) [35].
The importance of extent of resection in meningioma brachytherapy cases is highlighted in another series of 19 patients with recurrent meningiomas who, as in our series, underwent planned GTR with placement of Cs-131 seeds [33]. Only two cases of local progression (within 1.5 cm of the operative bed) were observed in their series, and both recurrences occurred in patients who underwent near gross-total resection (> 90%). Similar to our study, when compared with time to local progression before brachytherapy, resection with brachytherapy implantation significantly improved local control. Although the median time to local progression was not reached, overall survival was poor, with only 58% of patients remaining alive at a median observation period of 19.7 months, and PFS was not reported in their study.
Taken together, the results of our study, as well as the studies above, highlight the importance of extent of resection in cases of planned brachytherapy treatment. At our institution, the goal of planned GTR is a major selection criterion when evaluating candidates for brachytherapy, and we hypothesize that this strategy strongly impacts the excellent local control achieved in our study.
Recurrences within versus outside of the brachytherapy treatment field
Importantly, measuring PFS may underestimate the impact of brachytherapy seed placement in recurrent high-grade meningioma patients. This is supported by the nature of the recurrences documented in our study. Over half of the recurrences in our study were marginal (i.e. within 1.5 cm of the craniotomy; n = 3/5), and all three marginal recurrences occurred along the convexity and parasagittal dura. Tumor control within the brachytherapy field was excellent, with only two recurrences observed within the brachytherapy field over the study period, as demonstrated in a subset analysis (Fig. 1e, f). We evaluated marginal recurrences separately since they may be considered a failure to achieve a wide treatment field at the time of surgery more than a failure of the treatment itself.
Furthermore, it should be noted that small recurrences adjacent to the resection cavity or at marginal locations may remain amenable to subsequent intervention. This is supported by two patients in our study who underwent repeat resection with additional brachytherapy seed placement after recurrence of disease. Thus, although patients with marginal recurrence were included as local failure in our study and the progression timepoint was reached, resection with brachytherapy seed placement may confer a greater benefit to the long-term outcomes in these challenging patients.
Continued follow-up and analysis of OS is essential to evaluate the potential long-term benefit of brachytherapy in these patients. A significant difference in OS was not observed in our study, although the OS in the brachytherapy cohort was promising (Fig. 1d). The statistical analysis of OS in our study is limited by the small number of deaths to date in the brachytherapy cohort (n = 2) and the limited follow-up in the retrospective control cohort.
Technical considerations
In addition to surgical technique refinements, such as maximizing the resection of gross disease and improving brachytherapy seed coverage, technical refinements in radiation delivery methods continue. Brachytherapy seed implantation carries theoretical benefit over low dose intraoperative radiation therapy (IORT) for meningiomas due to its delivery of the radiation dosage over time, as opposed to one isolated timepoint with IORT [2, 39]. Depending on the radiation isotope used, dose delivery occurs over the half life of 9.7 days (Cs-131 seeds) to 59 days (I-125 seeds). In recent years, there has been a shift to the Cs-131 isotope rather than I-125 due to Cs-131′s shorter half-life. This has been associated with decreased complication rates, particularly regarding wound complications and radiation necrosis [20], which have been a limiting factor in earlier reported series [28, 29, 35]. While the predominant application of Cs-131 seed implantation has been in the context of metastatic disease [19,20,21], it remains to be determined if the shorter half-life of Cs-131 will be of equal, greater, or lesser efficacy in meningioma cases. The longer half-life of I-125 carries theoretical benefit in a tumor that is not rapidly dividing, as may be true in meningioma. Alternatively, it may be true that these meningiomas have already become highly proliferative and Cs-131 is an appropriate and effective strategy. Although we have recently shifted to using Cs-131 in more recent cases of brachytherapy seed implantation, direct comparison of the efficacy of I-125 versus Cs-131 was not possible in our series at the time of this analysis. Further investigation of Cs-131 control rates with additional follow-up is underway.
Refinements in brachytherapy seed implantation methods continue to improve radiation delivery and limit the migration of seeds post-operatively. At our institution, we utilize brachytherapy seeds implanted in vicryl suture strands that are manually spaced 1 cm apart within the surgical resection cavity, as previously reported by our group and others [27, 34, 35]. In the series reported by Brachman et al., a collagen-based delivery system was used to improve the precision of implantation and to alter the dose distribution [33]. They report that this delivery system improves the surgeon’s ability to target high-risk regions of the resection cavity and limits seed migration following implantation. Despite these refinements, several barriers remain. Improved delivery methods that allow for safer posterior fossa and skull base implantation, as well as methods for protecting adjacent brainstem and cranial nerve structures, would further expand applications of brachytherapy in difficult-to-treat tumors. Our results demonstrate the efficacy of brachytherapy on tumor control in recurrent high-grade meningiomas, and improving the safety of implantation may allow for expanded indications for this strategy.
Limitations
Our results must be viewed in the context of several limitations. First, its retrospective design carries the inherent limitations and biases of any study of this nature. Future prospective cohort studies and registries will be more rigorous for evaluating and comparing the results of this treatment strategy in future patients. Second, patient selection criteria for brachytherapy seed placement were stringent and dependent on the evaluation of both the neurosurgeon and the radiation oncologist. Enrollment was based on their experience and expertise, which limits the number of patients enrolled and the generalizability of the results. Third, we compared the PFS before and after brachytherapy placement in the brachytherapy cohort, assuming similar biological activity of the tumors; future studies examining the underlying genetic and molecular profiles of these tumors before and after brachytherapy placement may provide additional insight into the impact of brachytherapy on tumor recurrence. Lastly, given the extensive treatment history and heterogeneous pathology of these patients, comparison to the cohort of control patients from our institution, as well as prior patients reported in the literature, is potentially limited in this complex population.
Conclusions
Brachytherapy after planned GTR improved PFS in recurrent high-grade meningioma patients who had maximized external beam radiation treatment options. This was achieved with an acceptable complication rate in comparison to a matched cohort of patients with recurrent meningiomas treated without brachytherapy at our institution. Future improvement of brachytherapy dose delivery methods and techniques may continue to prolong control rates and limit complications in this challenging group of patients.
References
Kaley T, Barani I, Chamberlain M, McDermott M, Panageas K, Raizer J, Rogers L, Schiff D, Vogelbaum M, Weber D, Wen P (2014) Historical benchmarks for medical therapy trials in surgery- and radiation-refractory meningioma: a RANO review. Neuro Oncol 16(6):829–840. https://doi.org/10.1093/neuonc/not330
Magill ST, Lee DS, Yen AJ, Lucas CG, Raleigh DR, Aghi MK, Theodosopoulos PV, McDermott MW (2018) Surgical outcomes after reoperation for recurrent skull base meningiomas. J Neurosurg 1:1–8. https://doi.org/10.3171/2017.11.JNS172278
Magill ST (2018) Surgical outcomes after reoperation for recurrent non-skull base meningiomas. J Neurosurg 1:1–9. https://doi.org/10.3171/2018.6.JNS18118
Chohan MO, Ryan CT, Singh R, Lanning RM, Reiner AS, Rosenblum MK, Tabar V, Gutin PH (2018) Predictors of treatment response and survival outcomes in meningioma recurrence with atypical or anaplastic histology. Neurosurgery 82(6):824–832. https://doi.org/10.1093/neuros/nyx312
Lin AJ, Hui C, Dahiya S, Lu HC, Kim AH, Campian JL, Tsien C, Zipfel GJ, Rich KM, Chicoine M, Huang J (2018) Radiologic response and disease control of recurrent intracranial meningiomas treated with reirradiation. Int J Radiat Oncol Biol Phys 102(1):194–203. https://doi.org/10.1016/j.ijrobp.2018.05.011
Wojcieszynski AP, Ohri N, Andrews DW, Evans JJ, Dicker AP, Werner-Wasik M (2012) Reirradiation of recurrent meningioma. J Clin Neurosci 19(9):1261–1264. https://doi.org/10.1016/j.jocn.2012.01.023
Kim M, Lee DH, Kim Rn HJ, Cho YH, Kim JH, Kwon DH (2017) Analysis of the results of recurrent intracranial meningiomas treated with re-radiosurgery. Clin Neurol Neurosurg 153:93–101. https://doi.org/10.1016/j.clineuro.2016.12.014
Brastianos PK, Galanis E, Butowski N, Chan JW, Dunn IF, Goldbrunner R, Herold-Mende C, Ippen FM, Mawrin C, McDermott MW, Sloan A, Snyder J, Tabatabai G, Tatagiba M, Tonn JC, Wen PY, Aldape K, Nassiri F, Zadeh G, Jenkinson MD, Raleigh DR, International Consortium on M (2019) Advances in multidisciplinary therapy for meningiomas. Neuro Oncology 21:i18–i31. https://doi.org/10.1093/neuonc/noy136
Gupta S, Bi WL, Dunn IF (2018) Medical management of meningioma in the era of precision medicine. Neurosurg Focus 44(4):E3. https://doi.org/10.3171/2018.1.FOCUS17754
Simpson D (1957) The recurrence of intracranial meningiomas after surgical treatment. J Neurol Neurosurg Psychiatry 20(1):22–39
Bernstein M, Laperriere N, Leung P, McKenzie S (1990) Interstitial brachytherapy for malignant brain tumors: preliminary results. Neurosurgery 26(3):371–379
Brahimaj B, Lamba M, Breneman JC, Warnick RE (2016) Iodine-125 seed migration within brain parenchyma after brachytherapy for brain metastasis: case report. J Neurosurg 125(5):1167–1170. https://doi.org/10.3171/2015.11.JNS151464
Heros DO, Kasdon DL, Chun M (1988) Brachytherapy in the treatment of recurrent solitary brain metastases. Neurosurgery 23(6):733–737
Huang K, Sneed PK, Kunwar S, Kragten A, Larson DA, Berger MS, Chan A, Pouliot J, McDermott MW (2009) Surgical resection and permanent iodine-125 brachytherapy for brain metastases. J Neurooncol 91(1):83–93. https://doi.org/10.1007/s11060-008-9686-2
Matsumoto K, Tada E, Tamesa N, Tomita S, Ohmoto T (1998) Stereotactic brachytherapy for a cystic metastatic brain tumor in the midbrain. Case report. J Neurosurg 88(1):141–144. https://doi.org/10.3171/jns.1998.88.1.0141
Pham A, Yondorf MZ, Parashar B, Scheff RJ, Pannullo SC, Ramakrishna R, Stieg PE, Schwartz TH, Wernicke AG (2016) Neurocognitive function and quality of life in patients with newly diagnosed brain metastasis after treatment with intra-operative cesium-131 brachytherapy: a prospective trial. J Neurooncol 127(1):63–71. https://doi.org/10.1007/s11060-015-2009-5
Raleigh DR, Seymour ZA, Tomlin B, Theodosopoulos PV, Berger MS, Aghi MK, Geneser SE, Krishnamurthy D, Fogh SE, Sneed PK, McDermott MW (2017) Resection and brain brachytherapy with permanent iodine-125 sources for brain metastasis. J Neurosurg 126(6):1749–1755. https://doi.org/10.3171/2016.4.JNS152530
Rogers LR, Rock JP, Sills AK, Vogelbaum MA, Suh JH, Ellis TL, Stieber VW, Asher AL, Fraser RW, Billingsley JS, Lewis P, Schellingerhout D, Shaw EG, Brain Metastasis Study G (2006) Results of a phase II trial of the GliaSite radiation therapy system for the treatment of newly diagnosed, resected single brain metastases. J Neurosurg 105(3):375–384. https://doi.org/10.3171/jns.2006.105.3.375
Wernicke AG, Yondorf MZ, Peng L, Trichter S, Nedialkova L, Sabbas A, Kulidzhanov F, Parashar B, Nori D, Clifford Chao KS, Christos P, Kovanlikaya I, Pannullo S, Boockvar JA, Stieg PE, Schwartz TH (2014) Phase I/II study of resection and intraoperative cesium-131 radioisotope brachytherapy in patients with newly diagnosed brain metastases. J Neurosurg 121(2):338–348. https://doi.org/10.3171/2014.3.JNS131140
Wernicke AG, Hirschfeld CB, Smith AW, Taube S, Yondorf MZ, Parashar B, Nedialkova L, Kulidzhanov F, Trichter S, Sabbas A, Ramakrishna R, Pannullo S, Schwartz TH (2017) Clinical outcomes of large brain metastases treated with neurosurgical resection and intraoperative cesium-131 brachytherapy: results of a prospective trial. Int J Radiat Oncol Biol Phys 98(5):1059–1068. https://doi.org/10.1016/j.ijrobp.2017.03.044
Wernicke AG, Smith AW, Taube S, Yondorf MZ, Parashar B, Trichter S, Nedialkova L, Sabbas A, Christos P, Ramakrishna R, Pannullo SC, Stieg PE, Schwartz TH (2017) Cesium-131 brachytherapy for recurrent brain metastases: durable salvage treatment for previously irradiated metastatic disease. J Neurosurg 126(4):1212–1219. https://doi.org/10.3171/2016.3.JNS152836
Ruge MI, Suchorska B, Maarouf M, Runge M, Treuer H, Voges J, Sturm V (2011) Stereotactic 125iodine brachytherapy for the treatment of singular brain metastases: closing a gap? Neurosurgery 68(5):1209–1218. https://doi.org/10.1227/NEU.0b013e31820b526a
Hood TW, McKeever PE (1989) Stereotactic management of cystic gliomas of the brain stem. Neurosurgery 24(3):373–378
Korinthenberg R, Neuburger D, Trippel M, Ostertag C, Nikkhah G (2011) Long-term results of brachytherapy with temporary iodine-125 seeds in children with low-grade gliomas. Int J Radiat Oncol Biol Phys 79(4):1131–1138. https://doi.org/10.1016/j.ijrobp.2009.12.040
Ruge MI, Kickingereder P, Simon T, Treuer H, Sturm V (2012) Stereotactic iodine-125 brachytherapy for treatment of inoperable focal brainstem gliomas of WHO grades I and II: feasibility and long-term outcome. J Neurooncol 109(2):273–283. https://doi.org/10.1007/s11060-012-0889-1
Kickingereder P, Hamisch C, Suchorska B, Galldiks N, Visser-Vandewalle V, Goldbrunner R, Kocher M, Treuer H, Voges J, Ruge MI (2014) Low-dose rate stereotactic iodine-125 brachytherapy for the treatment of inoperable primary and recurrent glioblastoma: single-center experience with 201 cases. J Neurooncol 120(3):615–623. https://doi.org/10.1007/s11060-014-1595-y
Abou Al-Shaar H, Almefty KK, Abolfotoh M, Arvold ND, Devlin PM, Reardon DA, Loeffler JS, Al-Mefty O (2015) Brachytherapy in the treatment of recurrent aggressive falcine meningiomas. J Neurooncol 124(3):515–522. https://doi.org/10.1007/s11060-015-1873-3
Magill ST, Lau D, Raleigh DR, Sneed PK, Fogh SE, McDermott MW (2017) Surgical resection and interstitial iodine-125 brachytherapy for high-grade meningiomas: a 25-year series. Neurosurgery 80(3):409–416. https://doi.org/10.1227/NEU.0000000000001262
Ware ML, Larson DA, Sneed PK, Wara WW, McDermott MW (2004) Surgical resection and permanent brachytherapy for recurrent atypical and malignant meningioma. Neurosurgery 54(1):55–64. https://doi.org/10.1227/01.Neu.0000097199.26412.2a
Gutin PH, Leibel SA, Hosobuchi Y, Crumley RL, Edwards MS, Wilson CB, Lamb S, Weaver KA (1987) Brachytherapy of recurrent tumors of the skull base and spine with iodine-125 sources. Neurosurgery 20(6):938–945
Kumar PP, Good RR, Patil AA, Leibrock LG (1989) Permanent high-activity iodine-125 in the management of petroclival meningiomas: case reports. Neurosurgery 25(3):436–441
Obasi PC, Barnett GH, Suh JH (2002) Brachytherapy for intracranial meningioma using a permanently implanted iodine-125 seed. Stereotact Funct Neurosurg 79(1):33–43. https://doi.org/10.1159/000069502
Brachman DG, Youssef E, Dardis CJ, Sanai N, Zabramski JM, Smith KA, Little AS, Shetter AG, Thomas T, McBride HL, Sorensen S, Spetzler RF, Nakaji P (2018) Resection and permanent intracranial brachytherapy using modular, biocompatible cesium-131 implants: results in 20 recurrent, previously irradiated meningiomas. J Neurosurg 1:1–10. https://doi.org/10.3171/2018.7.JNS18656
Shafiq AR, Wernicke AG, Riley CA, Morgenstern PF, Nedialkova L, Pannullo SC, Parashar B, Magge R, Schwartz TH (2019) Placement of cesium-131 permanent brachytherapy seeds using the endoscopic endonasal approach for recurrent anaplastic skull base meningioma: case report and technical note. J Neurosurg 1:1–6. https://doi.org/10.3171/2018.11.JNS181943
Koch MJ (2019) Brachytherapy as an adjuvant for recurrent atypical and malignant meningiomas. Neurosurgery. https://doi.org/10.1093/neuros/nyz115/5479423
Ramkissoon SH, Bi WL, Schumacher SE, Ramkissoon LA, Haidar S, Knoff D, Dubuc A, Brown L, Burns M, Cryan JB, Abedalthagafi M, Kang YJ, Schultz N, Reardon DA, Lee EQ, Rinne ML, Norden AD, Nayak L, Ruland S, Doherty LM, LaFrankie DC, Horvath M, Aizer AA, Russo A, Arvold ND, Claus EB, Al-Mefty O, Johnson MD, Golby AJ, Dunn IF, Chiocca EA, Trippa L, Santagata S, Folkerth RD, Kantoff P, Rollins BJ, Lindeman NI, Wen PY, Ligon AH, Beroukhim R, Alexander BM, Ligon KL (2015) Clinical implementation of integrated whole-genome copy number and mutation profiling for glioblastoma. Neuro Oncology 17(10):1344–1355. https://doi.org/10.1093/neuonc/nov015
Aizer AA, Abedalthagafi M, Bi WL, Horvath MC, Arvold ND, Al-Mefty O, Lee EQ, Nayak L, Rinne ML, Norden AD, Reardon DA, Wen PY, Ligon KL, Ligon AH, Beroukhim R, Dunn IF, Santagata S, Alexander BM (2016) A prognostic cytogenetic scoring system to guide the adjuvant management of patients with atypical meningioma. Neuro Oncology 18(2):269–274. https://doi.org/10.1093/neuonc/nov177
USDHHS (2009) Common terminology criteria for adverse events (CTCAE) Version 4.0. US Department of Health and Human Services, Bethesda.
Cifarelli CP, Brehmer S, Vargo JA, Hack JD, Kahl KH, Sarria-Vargas G, Giordano FA (2019) Intraoperative radiotherapy (IORT) for surgically resected brain metastases: outcome analysis of an international cooperative study. J Neurooncol. https://doi.org/10.1007/s11060-019-03309-6
Giordano FA, Brehmer S, Murle B, Welzel G, Sperk E, Keller A, Abo-Madyan Y, Scherzinger E, Clausen S, Schneider F, Herskind C, Glas M, Seiz-Rosenhagen M, Groden C, Hanggi D, Schmiedek P, Emami B, Souhami L, Petrecca K, Wenz F (2019) Intraoperative radiotherapy in newly diagnosed glioblastoma (intrago): an open-label, dose-escalation phase i/ii trial. Neurosurgery 84(1):41–49. https://doi.org/10.1093/neuros/nyy018
Acknowledgements
The authors would like to thank the Goss family for their generosity and support of meningioma research at the Brigham and Women’s Hospital.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declares that they have no conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Mooney, M.A., Bi, W.L., Cantalino, J.M. et al. Brachytherapy with surgical resection as salvage treatment for recurrent high-grade meningiomas: a matched cohort study. J Neurooncol 146, 111–120 (2020). https://doi.org/10.1007/s11060-019-03342-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11060-019-03342-5