Abstract
Electronic-cigarette (ECIG) use increased over the last decade as many find vaping as a safe alternative to cigarettes; however, the safety of ECIGs on biological functions are still not fully understood. The present study evaluated the effects of daily ECIG use on body weight, lung tissue, and inflammatory cytokines using a low vapor exposure design as many teenagers use ECIGs sporadically throughout the day rather than heavy consistent use found in the adult population. Mice were divided evenly into three groups: Control (no vapor treatment), vapor vehicle (nicotine-free vapor), and 30.0 mg/mL nicotine. Mice received two vapor inhalation sessions per day for 28 days in which mice received a 3-s vapor puff every 2 min for 10 min (6 puffs total). On day 29, mice were sacrificed after a final vapor administration session, and lungs were examined microscopically with hematoxylin & eosin stain and ten inflammatory cytokines were assessed. Mice in the vape groups failed to gain weight over the 28 days. Control mice significantly increased weight in a linear fashion. Deleterious lung morphologies were significantly higher in the vape groups as compared to controls (12 vs 3) with all of the vapor mice showing at least one deleterious lung morphology. IL-2 and IL-6 were significantly decreased in vape mice. This study found that vapor inhalation significantly hindered weight gain and damaged lungs of both nicotine and vehicle groups, suggesting that damage may be caused by vapor inhalation, rather than nicotine.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The use of electronic-cigarettes (ECIGs), also called vapes by the general population, has become increasingly popular in the United States, especially among teenagers. For example, 20.8% of high school students reported using ECIGs in the last 30 days as compared to 4.7% of adults [1]. The use of ECIGs in high school students significantly increased from 1.5% in 2011 to 20.8% in 2018. Additionally, ECIGs have created a significant shift in how nicotine and tobacco products are consumed. Since the introduction of ECIGs in 2007, adult use of combustible cigarettes decreased by 7% with many combustible cigarette users switching to ECIGs [1]. There is much contradiction regarding the safety of vaping as many posit that ECIGs must be safer than cigarette smoking or believe that ECIGs are not harmful [2,3,4]. However, recently many individuals have been presenting to emergency rooms with ECIG or vaping product use-associated lung injury (EVALI). Although ECIGs have been on the market since 2007, we do not have a clear understanding of the short- or long-term effects of oil vapor inhalation biological functions.
Recent autopsies have found acute lung injury, diffuse alveolar damage, lipid-laden macrophages, and numerous inflammatory cells in patients that have chronically used ECIGs [5,6,7,8,9]. Lung injury associated with ECIGs can be a challenging clinical diagnosis with overlapping symptoms with numerous other lung diseases as many adult ECIG users were previous combustible cigarette users [5, 10]. Preclinical animal studies can provide vital insight into the impact that vapor inhalation has on biological function, behavior, and abuse liability.
One problem that has plagued the preclinical vapor inhalation field is determining a vapor administration regimen (length of vapor puff, frequency of vapor puff, duration of vapor administration session, wattage, nicotine dose, etc.) that translates to the clinical population (see [11] for review). Vapor inhalation has been shown to cause significant lung damage in mice using vapor dosing regimens that are consistent with heavy daily ECIG user [12,13,14,15,16,17,18]. However, more recent studies have found that shorter puff durations and vapor administration sessions (i.e. low vapor exposure) produce abuse-related behavioral effects and nicotine blood/plasma concentrations similar to injected nicotine [19,20,21,22]. For example, a 3-s puff of 6 mg/ml produced reliable self-administration in mice [19]. Repeated treatment of 1 and 3 mg/ml vaporized nicotine delivered as a 3-s puff every 2 min for 10 min produced nicotine sensitization comparable to injected nicotine [20]. Moreover, we demonstrated that longer vapor puff durations (6–10 s) and longer vapor administration sessions (10 vs 20 min) produce significant behavioral disruption and anxiety-like behaviors in mice [11]. Taken together, these studies indicate a need to evaluate the effects of low vapor exposure (i.e. shorter puff durations and vapor administration sessions) on biological functions as many teenagers and young adults use ECIGs sporadically throughout the day and use a lower nicotine concentration rather than heavy consistent use found in the adult population [23].
The present study sought to evaluate the effects of daily chronic ECIG use on body weight, lung tissue, and inflammatory cytokines using a low vapor exposure design in mice. The vapor administration sessions used in the present study are consistent with the studies that found abuse-related effects in mice. Mice were chronically exposed to twice-a-day nicotine-free vapor inhalation or 30 mg/ml nicotine vapor inhalation for 28-days, in which mice received a 3-s puff every 2 min for 10 min (the control group had no vapor inhalation). Additionally, this dosing regimen allows us to determine if nicotine was required to produce significant weight change or lung injury. We hypothesized that chronic vapor inhalation, regardless of the presence of nicotine, would have a deleterious inflammatory effect on the lung parenchyma.
Materials & methods
Subjects
Eighteen adult male C57BL/6 mice were purchased from Charles River Laboratories (Raleigh-Durham, NC). Mice were eight weeks old at the start of the experiments and were group housed (n = 3–4) in standard shoebox cages (18.5 cm × 29.5 cm × 12.5 cm). The vivarium was temperature (20–22 °C) and light controlled (12-h light/dark cycle with lights on at 6:00 am). Mice had free access to food and water except during vapor inhalation sessions. Experiments were performed during the light cycle. All procedures were approved by the Institutional Animal Care and Use Committee at Weber State University and complied with federal guidelines (Institute of Laboratory and Animal Resources 2011).
Drugs and materials
Freebase nicotine obtained from Sigma-Aldrich (St. Louis, MO) was dissolved in the unflavored e-liquid. The e-liquid consisted of a nicotine-free unflavored 50:50 propylene glycol:vegetable glycerin (PG:VG) oil blend that was purchased from vaporvapes.com (Sand City, CA, USA). The hematoxylin & eosin (H&E) kit was obtained from Vector Laboratories (H-3502) and a custom mouse ProcartaPlex 10-plex cytokine panel was purchased from ThermoFisher Scientific.
Apparatus and dosing procedure
Mice were divided evenly into three groups (n = 6); control group (no vapor treatment), vehicle group received nicotine-free vaporized e-liquid, nicotine group received vaporized e-liquid with 30 mg/mL of nicotine. Vapor administration was based on published literature [11, 19, 20, 24]. An e-Vape™ delivery system (Model SVS200, La Jolla Alcohol Research, Inc.) equipped with a Cloud Beast tank (TFV8) and atomizer (0.15Ω) was used for vapor administration (SMOK, Nanshan District, Shenzhen, China). The battery wattage output was set at 125W based on tank specifications and airflow was maintained at 1 L/min. The vapor administration sessions were controlled by a preprogrammed digital interface that produced a 3-s vapor puff every 2 min for 10 min (6 puffs total). Mice were removed from the e-Vape™ chamber (29 cm × 20 cm × 15 cm) after the sixth and final puff of the session completely cleared the chamber, which took approximately 90 s [11]. Mice in the vehicle and nicotine groups received 28 days of chronic vapor inhalation treatment which consisted of two vapor inhalation sessions per day that were separated by at least 4 h (typically 8:00 am and 1:00 pm). In total, mice were exposed to 12 puffs daily (6 puffs in the morning and 6 puffs in the afternoon). Control mice were weighed and placed into the e-Vape™ chamber twice a day but did not receive vapor administration.
Weight gain and lung weight
To determine if vapor inhalation altered normal weight gain, mice were weighed each week in the morning before any experimental session (approximately 18 h after the last nicotine exposure). To determine if vapor inhalation increased the weight of the lungs as a result of fluid accumulation or another side effect, the right lung of each animal was weighed after the lung had been thawed on ice before cytokine analysis (see below).
Histology analysis
On day 29, mice received one morning vapor inhalation session. Two hours later, mice were sacrificed by cervical dislocation and the lungs were obtained by dissection. Hemostats were placed over the right bronchus and the superior portion of the trachea. The right lung was clipped off, immediately placed on dry ice, and stored at -80˚C for cytokine analysis. The left lung was insufflated with 10% formalin by inserting a needle into the trachea. After insufflation, the left lung was placed in 10% formalin and fixed overnight. The left lungs were made into slides at Utah State University and stained at Weber State University using a standard hematoxylin & eosin (H&E) kit following the manufacturer's protocol.
The slides were examined by a trained pathologist that was blind to treatment conditions and findings were recorded as being positive or negative for four nonspecific categories of pathology for this study; myxoid stroma, lymphocytic infiltration, hyaline membrane formation, and diffuse alveolar damage. Myxoid stroma consists of a mucoid-appearing tissue surrounding the cells in the tissue and is a nonspecific indicator of inflammation. Lymphocytic infiltration generally reflects chronic inflammation; the inflammatory state of each lung was also assessed using cytokine analysis. Hyaline membrane formation is defined as the presence of hyaline membranes in the alveolus. Diffuse alveolar damage is a complete disruption of the alveolar structure. A pathology score was calculated as a numerical frequency representation of each pathologic event observed by the treatment groups.
Cytokine analysis
The right lung tissue was thawed on ice, weighed, and added to the appropriate volume of T-PER containing Complete Mini Protease Inhibitor Cocktail at the manufacturer defined concentration. Each mouse lung was homogenized separately on ice using a glass tissue grinder with a minimum of twenty strokes. The homogenates were then centrifuged at 9,000 × g for ten minutes at 4 degrees Celsius. Supernatants were transferred to fresh microcentrifuge tubes and stored at -80 Celsius for cytokine testing [25]. A custom mouse ProcartaPlex 10-plex cytokine panel was used to quantify IL-1b, IL-2, IL-4, IL-5, IL-6, IL-10, IL-12 (p70), GM-CSF, TNF-α, and IFN-γ present in the lung supernatants. Reagents, standards, and controls were prepared in accordance with manufacturer instructions, and samples were thawed on ice. Assay standards, controls, and samples were run in triplicate. Briefly, 12.5 uL of the sample, control, or standard was mixed with 12.5 uL of antibody magnetic beads in the provided 96-well plate and incubated on a shaker for 24 h at room temperature. After incubation, detection antibodies and streptavidin PE were added, and data acquisition was performed on a MAGPIX System with xPONENT 4.2 software. Any zero/undetectable cytokine concentrations were replaced with the minimum detection limit of that analyte; this was done for TNF-α, IL-5, and IL-12p70 with the minimum detection level of 2.856, 1.953, and 1.599 pg/mL respectively. Any missing concentrations were replaced with the median value of the samples [25,26,27]. Cytokine concentrations for each sample were then averaged across the triplicate measurements.
Statistical analysis
Initial examination of the treatment groups displayed no difference in study outcomes between the vehicle vapor inhalation and nicotine vapor inhalation groups. To enhance the statistical power of further analysis, the vapor inhalation groups (nicotine-free and 30.0 mg/ml nicotine) were merged and will be referred to as the vapor inhalation group abbreviated “Vape” in the tables and figures. The supplemental material includes figures and tables for the data from the three treatment groups prior to merging vapor inhalation groups (Supplemental Figs. 1 and 2, Supplemental Tables 1 and 2). A two-way mixed factor analysis of variance (ANOVA) was used to analyze body weight with “treatment group” as the between-subject factor and “day” as the within-subject factor. The significant ANOVA was followed by a Holm-Sidak post hoc test. Lung weight was analyzed using a parametric Welch Two Sample t-Test to account for the comparison of groups with unequal sample sizes [25,26,27]. For the H&E staining experiments, a Fisher’s Exact Test for count data was used to compare the frequency of tissue morphologies between treatment groups. Cytokine concentrations were first log10 transformed, normality was confirmed using a Shapiro–Wilk test, and then compared across treatment groups using a parametric Welch Two Sample t-Test [25,26,27]. All data cleaning, graphical representations, and statistical comparisons were performed using R Statistical Computing Platform v3.6.3 (R Core Team 2020) and GraphPad Prism 7.0.
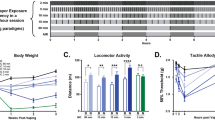
Effect of vapor inhalation on (A) body weight gain and (B) lung weights. A) Control mice significantly increased weight over the 28-day study; whereas the vape group failed to gain weight. B) There was a nonsignificant trend when comparing the lung weights of control and vape group mice with the group appearing to have enlarged lungs. The significant two-way ANOVA was followed by a Holm-Sidak post hoc test. All data show mean ± SD. ***p < 0.001 versus days 1 and 7
Observed lung morphologies in mice following chronic vapor inhalation. Representative images of H&E stains at 10X. A) Diffuse alveolar visible throughout the lung and hyaline membranes (light red, glassy, diffuse, material inside the alveoli). Within areas of Diffuse alveolar damage, there are disruptions of the alveolar structure, neutrophils, and hyaline membranes. Hyaline membranes are the light red, glassy, mucinous material inside the alveoli. B) Lymphocytic infiltration (numerous small round blue cells) and hyaline membranes. C) fibrinous exudates (darker red material inside airways) and chronic inflammation (lymphocytic infiltration) from a mouse in the vehicle group, D) normal architecture with occasional lymphocytes from a mouse in the control group. E) Observed morphologies were totaled for each mouse and displayed by treatment group, (red) circles are control mice, and (blue) circles are vapor inhalation (Vape) treated mice
Results
Weight gain and lung weight
Figure 1 shows the effects of vapor inhalation on body weight gain and lung weights. There was a significant interaction (time X treatment condition) (F (4, 64) = 6.40, p < 0.001) and a significant main effect of time (F (4, 64) = 15.62, p < 0.001); however, there was no main effect of treatment condition (F (1, 16) = 1.01, p = 0.33). The Holm-Sidak post hoc test revealed that the control mice significantly increase body weight on days 14, 21, and 28 as compared to days 1 and 7 (Fig. 1A). The vape mice failed to gain a significant body weight during the 28-day study. There was a nonsignificant trend when comparing the lung weights of control and vape group mice, t(12.86) = -1.61, p = 0.06) as mice in the vape group appear to have enlarged lungs (Fig. 1B).
Lung morphologies
Lung morphology data are summarized in Table 1 with representative images in Fig. 2. Overall, the number of mice in the vape group with lung morphologies was significantly higher than that controls as all vape mice showed at least one morphology (12 vs 3, p = 0.02; Table 1). The vape group displays a significantly higher occurrence of hyaline membrane formation as compared to the control group (p = 0.05). Lymphocytic infiltration was the most commonly found lung morphology in the vape group (75%); however, the control group had occasional mild inflammation. Incidentally, a lymph node of one of the vaping mice was observed on H&E staining, which revealed normal germinal centers with occasional mitotic figures but a lack of apparent malignant transformation. Enlarged follicles with frequent mitotic figures in the germinal centers were observed in the lymph node. Mice in the Vape group showed that vapor inhalation had substantial deleterious effects on the health of lung tissues.
Cytokine concentrations
The cytokine concentrations of individual mice stratified by treatment group are shown in Fig. 3. The vape group had significantly lower concentrations of IL-2 as compared to the control group (t(15.33) = 2.24, p = 0.04; Fig. 3, Table 2). The vape group mice had an almost sixty percent lower average of IL-5 concentrations as compared to control mice (t(15.87) = 2.20, p = 0.04; Fig. 3, Table 2). Although not significant, the vape mice appear to have a lower expression of most of the cytokines that were tested when compared to controls. In contrast to the other cytokines, TNF-alpha and IL-4 showed increased concentrations but were not statistically significant.
Discussion
The present study aimed to evaluate the effects of chronic vapor inhalation on mouse lungs by using a low vapor exposure dosing regimen that is consistent with teenagers and young adults. Overall, the results support the hypothesis of a link between vapor inhalation and increased health risks. We found that chronic vapor inhalation hinders normal developmental weight gain in mice, which is consistent with previous findings [13, 17, 28]. For example, vapor inhalation has been shown to block weight gain in mice comparable to cigarette smoke [13]. This reduction in weight gain does not appear to be a byproduct of the appetite-suppressant effects of nicotine as it occurs in mice exposed to nicotine-free e-liquid [28], the present study, suggesting that vapor inhalation can stunt growth but the mechanism for this effect is unknown.
We found that all mice in the vapor inhalation group had at least one deleterious lung morphology, if not several. The majority of vape mice had myxoid stroma, lymphocytic infiltration, and hyaline membranes formation morphologies, which are similar to those observed in patients with inflammatory lung disease and cases of EVALI [5,6,7,8,9, 29]. The lung morphologies found in the vape mice were not consistent across all mice which is similar to previous reports that found minimal, or no lung morphology changes when mice were exposed to PG:VG e-liquid vapor [13, 30]. We were unable to link our morphologic findings with the cytokine panel, likely due to our small sample size (an issue of power) but could also be due to a covert inflammatory response occurring in the control group, research technique, or something else entirely. Overall, we found a trend toward a decrease in the expression of cytokines, which is consistent with a previous study that found that two weeks of vapor inhalation produced a significant decrease in IL-6 [17]. However, a previous study found acute (3 days) vapor inhalation significantly increases IL-6, IL-1α, and IL-13 expression as well as a trend towards an increase in IL-10 and IL-1β [16]. There are major differences in the methodologies of these studies that might explain the differences in cytokine results. It is also possible that our study did not expose the mice to enough vapor inhalation to elicit a strong inflammatory response as we used a low vapor exposure dosing regimen or that the inflammatory response is downregulated after chronic exposure to vapor inhalation, which could explain the decreased IL-6 found after two weeks of exposure in a different study [17]. Overall, there have been mixed and non-consistent results on lung damage and inflammatory responses following vapor inhalation in mice, which is likely a result of the different dosing regimens and apparatus used for these studies.
One of the most appealing features of ECIGs, but also the most difficult feature for researchers, is the customizability for each user. First, there are several different types of e-cigs devices, which include vape pens, “mods”, e-cigs, and JUUL, that determine the customizability. Second, ECIG users can customize the e-liquid from the PG:VG oil blend ratio (ranges from 0:100 to 80:20) to flavor additives to nicotine concentration, which will determine the “smoothness” and “buzz” of each vape hit [31]. The present study used a “mod” device, a 50:50 oil blend that was not flavored. It is uncommon for ECIG users to use unflavored e-liquid; however, we wanted to reduce the confounding variables and decided that it was best to eliminate the flavoring solution as a variable. It is possible that changing the oil blend (e.g. 70:30 or 100:0) and/or adding flavor could result in a greater morphological and inflammatory response. Lastly, a “vape session” is much different from a traditional cigarette session because the user can control the wattage, duration of the puff, duration of the session, etc. Traditional cigarettes are typically smoked over a 7–10 min period because of the combustible nature of the cigarette; whereas, ECIGs do not have a combustible component and allow the user to take any number of puffs with little to no loss of nicotine between vapor puffs as compared to traditional cigarettes. Clinical data suggest that the typical vape sessions last approximately 10 min with a mean puff duration of ~ 4.5 s [32,33,34]. The vapor inhalation parameters used in this study are consistent with the clinical population (i.e. 10 min session with six 3-s puffs) and were adequate to produce an oxidative stress response in mouse brain and liver (lungs were not examined) [24].
In conclusion, these microscopic findings in these mice are significant and detrimental to overall health, which was demonstrated by the stunted weight gain, enlarged lungs, and significant lung damage in the vapor group. Vapor inhalation, not nicotine, appears to be responsible for the myxoid stroma, lymphocytic infiltration, hyaline membrane formation, and diffuse alveolar damage found in the vapor groups. Additionally, we only tested one set of vapor inhalation parameters (i.e. 50:50 PG:VG unflavored e-liquid, 10 min session with six 3-s puffs) to set a foundation for future testing. To fully understand EVALI, further studies should evaluate how oil blend ratios, flavors, session length, Vitamin E acetate, and nicotine might mediate EVALI. Taken together, these results do not support the claim that ECIGs are safe.
Data availability
The datasets generated during and/or analysed during the current study are available from the corresponding author on reasonable request.
References
National Center for Health Statistics. Health, United States, 2019. Hyattsville, MD. 2021. https://doi.org/10.15620/cdc:100685.
Cooper, M., Loukas, A., Case, K. R., Marti, C. N., & Perry, C. L. (2018). A longitudinal study of risk perceptions and e-cigarette initiation among college students: Interactions with smoking status. Drug and Alcohol Dependence, 186, 257-263. https://doi.org/10.1016/j.drugalcdep.2017.11.027
Ma, J. Z., Hart, J. L., Walker, K. L., Giachello, A. L., Groom, A., Landry, R. L., . . . Payne, T. J. (2019). Perceived health risks of electronic nicotine delivery systems (ENDS) users: The role of cigarette smoking status. Addict Behav, 91, 156–163. https://doi.org/10.1016/j.addbeh.2018.10.044
Pericot-Valverde, I., Gaalema, D. E., Priest, J. S., & Higgins, S. T. (2017). E-cigarette awareness, perceived harmfulness, and ever use among U.S. adults. Preventive Medicine, 104, 92-99. https://doi.org/10.1016/j.ypmed.2017.07.014
Acharya, S., Ali, S. I., Anwar, S., & Glaser, A. (2020). Do not fall to the vape trap! Respiratory Medicine Case Reports, 31, 101165. https://doi.org/10.1016/j.rmcr.2020.101165
Agustin, M., Yamamoto, M., Cabrera, F., & Eusebio, R. (2018). Diffuse alveolar hemorrhage induced by vaping. Case Reports in Pulmonology, 2018, 9724530. https://doi.org/10.1155/2018/9724530
Butt, Y. M., Smith, M. L., Tazelaar, H. D., Vaszar, L. T., Swanson, K. L., Cecchini, M. J., Braselton M, Brosius CR, Caron KT, Chambers D, Corstvet J, Cowan E, De Jesús VR, Espinosa P, Fernandez C, Holder C, Kuklenyik Z, Kusovschi JD, Newman C, Reis GB, Rees J, Reese C, Silva L, Seyler T, Song M-A, Sosnoff C, Spitzer CR, Tevis D, Wang L, Watson C, Wewers MD, Xia B, Heitkemper DT, Ghinai I, Layden J, Briss P, King BA, Delaney LJ, Jones CM, Baldwin GT, Patel A, Meaney-Delman D, Rose D, Krishnasamy V, Barr JR, Thomas J, Larsen, B. T. (2019). Pathology of vaping-associated lung injury. New England Journal of Medicine, 381(18), 1780-1781. https://doi.org/10.1056/NEJMc1913069
Jatlaoui T. C., Wiltz J. L., Kabbani S., et al. Update: Interim guidance for health care providers for managing patients with suspected E-cigarrette, or vaping, product use-associated lung injury – United States, November 2019. MMWR Morb Mortal Wkly Rep 2019;68:1081-1086
Marsden, L., Michalicek, Z. D., & Christensen, E. D. (2019) More on the pathology of vaping-associated lung injury. New England Journal of Medicine, 382(4), 387-390. https://doi.org/10.1056/NEJMc1914980
Maddock, S. D., Cirulis, M. M., Callahan, S. J., Keenan, L. M., Pirozzi, C. S., Raman, S. M., & Aberegg, S. K. (2019). Pulmonary lipid-laden macrophages and vaping. New England Journal of Medicine, 381(15), 1488-1489. https://doi.org/10.1056/NEJMc1912038
Garrett, P. I., Honeycutt, S. C., Marston, C., Allen, N., Barraza, A., Dewey, M., Turner B., Peterson A. M., Hillhouse, T. M. (2021). Nicotine-free vapor inhalation produces behavioral disruptions and anxiety-like behaviors in mice: Effects of puff duration, session length, sex, and flavor. Pharmacology Biochemistry and Behavior, 173207. https://doi.org/10.1016/j.pbb.2021.173207
Chun V., Moshensky A., Shin J., Alexander L. C., (2018). Chronic inhalation of unflavored nicotine and no‐nicotine containing electronic cigarette vapor leads to impaired lung function. Respirology 23:16-16.
Larcombe, A. N., Janka, M. A., Mullins, B. J., Berry, L. J., Bredin, A., & Franklin, P. J. (2017). The effects of electronic cigarette aerosol exposure on inflammation and lung function in mice. American Journal of Physiology-Lung Cellular and Molecular Physiology, 313(1), L67-L79. https://doi.org/10.1152/ajplung.00203.2016
Laube, B. L., Afshar-Mohajer, N., Koehler, K., Chen, G., Lazarus, P., Collaco, J. M., & McGrath-Morrow, S. A. (2017). Acute and chronic in vivo effects of exposure to nicotine and propylene glycol from an E-cigarette on mucociliary clearance in a murine model. Inhalation Toxicology, 29(5), 197-205. https://doi.org/10.1080/08958378.2017.1336585
Lee, H.-W., Park, S.-H., Weng, M.-w., Wang, H.-T., Huang, W. C., Lepor, H., Wu, X-R, Chen, L-C, Tang, M.-s. (2018). E-cigarette smoke damages DNA and reduces repair activity in mouse lung, heart, and bladder as well as in human lung and bladder cells. Proceedings of the National Academy of Sciences, 115(7), E1560. https://doi.org/10.1073/pnas.1718185115
Lerner, C. A., Sundar, I. K., Yao, H., Gerloff, J., Ossip, D. J., McIntosh, S., Robinson, R., Rahman, I. (2015). Vapors produced by electronic cigarettes and E-juices with flavorings induce toxicity, oxidative stress, and inflammatory response in lung epithelial cells and in mouse lung. PLOS ONE, 10, e0116732.
Sussan, T. E., Gajghate, S., Thimmulappa, R. K., Ma, J., Kim, J. H., Sudini, K., Consolini, N., Cormier, S. A., Lomnicki, S., Hasan, F., Pekosz, A., Biswal, S. (2015). Exposure to electronic cigarettes impairs pulmonary anti-bacterial and anti-viral defenses in a mouse model. PLOS ONE, 10(2), e0116861. https://doi.org/10.1371/journal.pone.0116861
Tang, M. S., Wu, X. R., Lee, H. W., Xia, Y., Deng, F. M., Moreira, A. L., Chen, L. C., Huang, W. C., Lepor, H. (2019). Electronic-cigarette smoke induces lung adenocarcinoma and bladder urothelial hyperplasia in mice. Proc Natl Acad Sci U S A, 116(43), 21727-21731. https://doi.org/10.1073/pnas.1911321116
Cooper, S. Y., Akers, A. T., & Henderson, B. J. (2020). Flavors enhance nicotine vapor self-administration in male mice. Nicotine & Tobacco Research. https://doi.org/10.1093/ntr/ntaa165
Honeycutt, S. C., Garrett, P. I., Barraza, A. G., Maloy, A. N., & Hillhouse, T. M. (2020). Repeated nicotine vapor inhalation induces behavioral sensitization in male and female C57BL/6 mice. Behav Pharmacol, 31(6), 583-590. https://doi.org/10.1097/fbp.0000000000000562
Lefever, T. W., Thomas, B. F., Kovach, A. L., Snyder, R. W., & Wiley, J. L. (2019). Route of administration effects on nicotine discrimination in female and male mice. Drug and Alcohol Dependence, 204, 107504. https://doi.org/10.1016/j.drugalcdep.2019.06.007
Montanari, C., Kelley, L. K., Kerr, T. M., Cole, M., & Gilpin, N. W. (2020). Nicotine e-cigarette vapor inhalation effects on nicotine & cotinine plasma levels and somatic withdrawal signs in adult male Wistar rats. Psychopharmacology (Berl), 237(3), 613-625. https://doi.org/10.1007/s00213-019-05400-2
Peterson M. L., Clark, C. T., Lynch, C. J., Coope,r J. T., Gelfman, N., Blumenstein, J., Hansen, R., Porter, J. H., Hillhouse, T. M. (2021) Preliminary assessment of the subjective effects of electronic-cigarettes in young-adult low-dose electronic-cigarette users: Effects of nicotine dose and e-liquid flavor. J Am Coll Health. 20:1-10. https://doi.org/10.1080/07448481.2021.1950162
Tyler, K., Geilman, S., Bell, D. M., Taylor, N., Honeycutt, S. C., Garrett, P. I., Hillhouse, T. M., Covey, T. M. (2021). Acyl Peptide Enzyme Hydrolase (APEH) activity is inhibited by lipid metabolites and peroxidation products. Chem Biol Interact, 348, 109639. https://doi.org/10.1016/j.cbi.2021.109639
McDuffie, E., Obert, L., Chupka, J., & Sigler, R. (2006). Detection of cytokine protein expression in mouse lung homogenates using suspension bead array. J Inflamm (Lond), 3, 15. https://doi.org/10.1186/1476-9255-3-15
Benjamini, Y., & Hochberg, Y. (1995). Controlling the false discovery rate: A practical and powerful approach to multiple testing. Journal of the Royal Statistical Society: Series B (Methodological), 57(1), 289-300. https://doi.org/10.1111/j.2517-6161.1995.tb02031.x
Siebert, J. C., Inokuma, M., Waid, D. M., Pennock, N. D., Vaitaitis, G. M., Disis, M. L., Dunne, J. F., Wagner, D. H. Jr., Maecker, H. T. (2008). An analytical workflow for investigating cytokine profiles. Cytometry A, 73(4), 289-298. https://doi.org/10.1002/cyto.a.20509
McGrath-Morrow, S. A., Hayashi, M., Aherrera, A., Lopez, A., Malinina, A., Collaco, J. M., Neptune, E., Klein, J. D., Winickoff, J. P., Breysse, P., Lazarus, P., Chen, G. (2015) The effects of electronic cigarette emissions on systemic cotinine levels, weight and postnatal lung growth in neonatal mice. PLoS One 10: e0118344.
Mukhopadhyay, S., Mehrad, M., Dammert, P., Arrossi, A. V., Sarda, R., Brenner, D. S., Maldonado, F., Choi, H., Ghobrial, M. (2020). Lung biopsy findings in severe pulmonary illness associated with E-Cigarette use (Vaping). Am J Clin Pathol, 153(1), 30-39. https://doi.org/10.1093/ajcp/aqz182
Glynos, C., Bibli, S.-I., Katsaounou, P., Pavlidou, A., Magkou, C., Karavana, V., Topouzis, S., Kalomenidis, I., Zakynthinos, S., Papapetropoulos, A. (2018). Comparison of the effects of e-cigarette vapor with cigarette smoke on lung function and inflammation in mice. American Journal of Physiology-Lung Cellular and Molecular Physiology, 315(5), L662-L672. https://doi.org/10.1152/ajplung.00389.2017
Etter, J. F. (2015). Explaining the effects of electronic cigarettes on craving for tobacco in recent quitters. Drug Alcohol Depend, 148, 102-108. https://doi.org/10.1016/j.drugalcdep.2014.12.030
Hiler, M., Breland, A., Spindle, T., Maloney, S., Lipato, T., Karaoghlanian, N., Shihadeh A, Lopez A, Ramôa C, Eissenberg, T. (2017). Electronic cigarette user plasma nicotine concentration, puff topography, heart rate, and subjective effects: Influence of liquid nicotine concentration and user experience. Experimental and Clinical Psychopharmacology, 25(5), 380-392. https://doi.org/10.1037/pha0000140
Spindle, T. R., Breland, A. B., Karaoghlanian, N. V., Shihadeh, A. L., & Eissenberg, T. (2014). Preliminary results of an examination of electronic cigarette user puff topography: The effect of a mouthpiece-based topography measurement device on plasma nicotine and subjective effects. Nicotine & Tobacco Research, 17(2), 142-149. https://doi.org/10.1093/ntr/ntu186
Spindle, T. R., Hiler, M. M., Breland, A. B., Karaoghlanian, N. V., Shihadeh, A. L., & Eissenberg, T. (2017). The Influence of a mouthpiece-based topography measurement device on electronic cigarette user's plasma nicotine concentration, heart rate, and subjective effects under directed and ad libitum use conditions. Nicotine & Tobacco Research, 19(4), 469-476. https://doi.org/10.1093/ntr/ntw174
Acknowledgements
We would like to thank the Office of Undergraduate Research, Office of Sponsored Projects, Academic Resources and Computing Committee (ARCC), and the Department of Medical Laboratory Sciences at Weber State University for funding this project. Additionally, we would like to thank Arnaud VanWettere, Ph.D., DVM, MS, Utah State University, Veterinary Pathology, for guidance and expertise in processing mouse tissue. Sarah C. Honeycutt was funded by National Institute on Alcohol Abuse and Alcoholism (NIAAA) (T32 AA007583).
Funding
Sarah C. Honeycutt is currently funded by National Institute on Alcohol Abuse and Alcoholism (NIAAA) (T32 AA007583), but was not funded at the time data was collected.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Declarations
All animal care and use were conducted in compliance with federal guidelines (National Research Council, 2011) and approved by the Institutional Animal Care and Use Committee (IACUC) at Weber State University. All authors have followed the COPE guidelines.
Conflict of interest
The authors report there are no competing interests to declare that are relevant to the content of this article.
Competing interests
The authors report there are no competing interests to declare.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Moore, S., Stanger, A., Langston, K. et al. Effects of chronic vapor inhalation on mouse body weight, lung morphology, and inflammatory cytokines using a low vapor exposure design. Neurosci Behav Physi 53, 929–938 (2023). https://doi.org/10.1007/s11055-023-01464-y
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11055-023-01464-y