Abstract
Sepsis is one of the leading causes of morbidity and mortality and a major cause of acute lung injury (ALI). carried by exosomes play a role in a variety of diseases. However,there are not many studies of exosomal miRNAs in sepsis and sepsis lung injury.miR-1298-5p and suppressor of cytokine signaling 6 (SOCS6) were silenced or overexpressed in human bronchial epithelial cells (BEAS-2B). PKH-67 Dye was used to trace exosome endocytosis. Cell permeability was evaluated by measuring trans-epithelial electrical resistance (TEER) and FITC dextran flux. ELISA kits were used for cytokine detection. Quantitative RT-PCR and western blots were used to evaluate gene expression. miR-1298-5p was elevated in exosomes from patients with sepsis lung injury (Sepsis_exo). Treatment of BEAS-2B cells using Sepsis_exo significantly inhibited cell proliferation, and induced cell permeability and inflammatory response. miR-1298-5p directly targeted SOCS6. Overexpressing SOCS6 reversed miR-1298-5p-induced cell permeability and inflammatory response. Inhibition of STAT3 blocked SOCS6-silencing caused significant increase of cell permeability and inflammation. Exosomes isolated from patients of sepsis lung injury increased cell permeability and inflammatory response in BEAS-2B cells through exosomal miR-1298-5p which targeted SOCS6 via STAT3 pathway. The findings highlight the importance of miR-1298-5p/SOCS6/STAT3 axis in sepsis lung injury and provide new insights into therapeutic strategies for sepsis lung injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Sepsis is a potentially life-threatening condition caused by the body's response to an infection with common signs and symptoms of fever, increased breathing rate, and confusion [1]. Sepsis is a leading cause of morbidity, with a mortality rate between 15 and 50% [2, 3]. It is estimated that more than 30 million people are affected by sepsis every year worldwide [4]. Sepsis also causes acute lung injury (ALI) and acute respiratory distress syndrome (ARDS) [5, 6]. Studies have shown that sepsis accounts for about 40% of ALI/ARDS cases [7, 8]. Cytokine-mediated inflammation has been shown to contribute to ALI by promoting dysfunction of the lungs and the injury of lung cells. Furthermore, inhibiting cytokine release to the lung has been shown to reduce the mortality of patients with ALI [9].
Cytokines activate intracellular signaling to exert their physiological effects including proliferation, differentiation, and survival [10]. The responses elicited by cytokines are regulated by various factors including suppressor of cytokine signaling (SOCS) family which comprises 8 proteins: SOCS1–7 and cytokine-inducible SH2-containing protein (CIS) [11]. SOCS negatively regulates cytokine receptor signaling [12]. SOCS6 is widely expressed in various tissues including ovary, uterus, and thyroid grand [13, 14] and is found to be downregulated in a variety of cancers [15,16,17]. SOCS protein has also been reported to be involved in the ALI secondary to sepsis in diabetic rats [18]. Zhang et al. suggested that miR-155 was involved in the inflammatory response in ALI by inhibiting the expression of SOCS protein [19].
Signal transducer and activator of transcription 3 (STAT3) is a transcription factor which regulates different biological processes [20]. Previous studies have shown that STAT3 is a key mediator inflammation [21]. Inhibiting the phosphorylation of STAT3 has been shown to increase the survival of sepsis rats, decrease histological damage of the lungs, and reduce inflammatory cytokines in serum and lung tissues of sepsis rats [22]. STAT3 also has been shown to regulate surfactant lipid synthesis in the lung [23]. Moreover, STAT3 regulates the neutrophil recruitment to decrease bacterial burdens during E. coli pneumonia via regulating of production of cytokines and chemokines [24].
Exosomes are extracellular vesicles (EVs) with a size range of ~ 40 to 160 nm in diameter. Intercellular communication via exosomes has been implicated in the pathogenesis of various disorders [25]. Studies have shown that microRNAs (miRNAs) carried by exosomes play a role in various diseases [26, 27]. Although the presence of miRNAs in plasma during sepsis has been previously confirmed [28, 29], few studies have evaluated the role of exosomes during sepsis.
Based on research findings that miR-1298-5p is highly expressed in exosomes of patients with sepsis [30], this study uses exosomes from sepsis patients to induce BEAS-2B cell injury, and investigated the role of miR-1298-5p/SOCS6/STAT3 in exosomes-induced lung epithelial cell damage and its underlying mechanism.
Material and methods
Cell culture
Human bronchial epithelial cells (BEAS-2B) were cultured in MEM medium (41500034, GIBCO) with 10% fetal bovine serum (FBS;16000-044, GIBCO, Carlsbad, CA) and 1% penicillin–streptomycin (P1400, Solarbio, Beijing, China) at 37 °C in an incubator with 5% CO2.
Plasmid construction
SOCS6 (NM_004232) coding sequence was cloned with the primers and inserted into pCDNA3.1( +) to elevate SOCS6 expression:
-
I.
SOCS6-F 5′-CCCAAGCTTATGAAGAAAATTAGTCTTAAAACCTTAC-3′ (Hind III).
-
II.
SOCS6-R 5′-CGGAATTCTCAGTAGTGCTTCTCCTGTAAATAATC-3′ (EcoR I).
SOCS6 siRNAs (Table 1) were used to knock down SOCS6 expression.
Cell transfection
BEAS-2Bcells in the logarithmic growth phase were trypsinized and counted to make 1 × 106 cells/ml suspension, and then 2 × 106 cells were inoculated into 6-well plates and cultured overnight at 37 °C in a 5% CO2 incubator. BEAS-2B cells (60–70% confluency) were transfected with WT + NC (negative control), WT + inhibitor, WT + mimic, Mut + NC, Mut + inhibitor and Mut + mimic, or control, vector and oeSOCS6, or control, shNC, shSOCS6-1, shSOCS6-2 and shSOCS6-3 using Lipo2000. Twenty four hours after transfection, complete medium was provided for 48 h. miR-1298-5p mimic/inhibitor was shown in Table 2.
Clinical samples
Venous blood from healthy controls and patients with sepsis lung injury was drawn into tubes without pro-coagulant, and spunat 3000 rpm for 10 min at room temperature to isolate serum. The protocol for the present study was approved by the Ethics Committee of Shanghai Pulmonary Hospital (Shanghai, China), and it conforms to the provisions of the Declaration of Helsinki in 1995. All participants have provided their written informed consent to participate in the study.
Isolation and identification of exosomes
Serum exosomes were extracted by centrifugation at 10,000 g for 30 min at 4 °C. Supernatants were spun twice at 17,000gfor 2 h. Pellet was re-suspended with PBS, filtered using 0.22 μm filters, and kept at − 80 °C. Serum exosomes were characterized by western blot with an antibody against Alix (ab88743, Abcam) or CD63 (ab271286, Abcam). The exosomes were quantified using a BCA protein quantitative kit(BCA1-1KT, Sigma), and the protein concentration > 100 ng/µl is suggested to use for subsequent experiments [31].
Exosome endocytosis tracing
Serum exosomes (100 μg/ml) extracted from healthy and patients with sepsis lung injury are co-cultured with BEAS-2B cells. PKH-67 (UR52303, Umibio) is used to monitor exosome endocytosis. PKH67 working solution was prepared according to the manufacturer’s protocol and used to stain exosomes for 10 min in the dark. A laser-scanning microscope was applied to take all images.
Cell proliferation analysis
Cell counting kit-8 (CCK-8) assay was performed using a Cell Proliferation and Cytotoxicity Assay Kit (SAB, CP002; College Park, MD, USA) [32]. Briefly, BEAS-2B cells (2 × 103, 100 µl) were added to each well of 96-w plates and cultured overnight. Cells were treated with Vector, Control_exo or Sepsis_exo (100 μg/ml). Next, CCK-8 (10 µl) (BioVision) was added and OD450 was measured to indicate cell proliferation.
Quantitative real-time PCR (qRT-PCR)
RNAs were isolated using TRIzol reagent (1596–026, Invitrogen) and then were converted to cDNA using High capacity cDNA reverse transcription kit (Bio-Rad) and amplified using SYBR Green Master Mix (Bio-Rad) according to the manufacturers’ instructions. The relative mRNA levels normalized to GAPDH were calculated using 2−△△Ct formula [33]. Primers were shown in Table 3 below:
Immunoblot analysis
Proteins were isolated using RIPA tissue cell rapid lysate and then resolved by SDS-PAGE, transferred to PVDF membranes, blocked in 3% BSA, incubated with optimally diluted first and second antibodies sequentially. Bands were analyzed using a chemiluminescent imager (Fuji film, Tokyo). Anti-Alix (ab88743, 1:1000), anti-CD63 (ab271286, 1:1000), anti-SOCS6 (ab197335, 1:500), anti-STAT3 (ab68153, 1:1000), anti-p-STAT3 (ab76315, 1:1000) supplied from Abcam, and anti-GAPDH (#5174, 1:2000) antibodies from CST, were used.
ELISA assay
Concentrations of IL-6 and TNF-α in supernatants were determined with commercial IL-6 and TNF-α ELISA kits according to the manufacturer’s instructions.
Cell permeability assay
Cell permeability was measured using two methods; trans-epithelial electrical resistance (TEER) and FITC dextran flux [34]. TEER was measured using a voltohmmeter (MillicellERS-2, Millipore). Resistance was calculated as follows: \(\mathrm{TEER }\left(\Omega \times \mathrm{cm}2\right)=\left(\mathrm{R}1-\mathrm{R}2\right)\left(\Omega \right)\times \mathrm{ Effective membrane area }\)(cm2), (R1: Experimental resistance; R2: Blank resistance). Dextran flux was measured by placing 10kD FITC-conjugated dextran (sc-263323, Santa cruz) in the upper chamber of the transwell for 5 min, and then the supernatants from the lower chamber were collected to measure the base value. Cells were supplemented with culture medium and incubated for 2 h. The supernatants from the lower chamber were then collected to detect FITC intensity using a microplate reader (E8051, Promega) to calculate permeability.
Luciferase reporter assays
SOCS6 3′-UTR was ligated into pGL3-Enhancer plasmid containing the firefly luciferase gene to get pGL3-wtSOCS6. Site-directed mutated SOCS6 3′-UTR was ligated into pGL3 to get pGL3-mutSOCS6. Cells were co-transfected with the pGL3-wtSOCS6 or pGL3-mutSOCS6 and pRL-TK-Renilla. Cells were then treated with NC, inhibitor, or mimic. Luminescence was monitored 24 h later using E1910 Kit (Promega, Madison, WI).
Statistical analysis
GraphPad Prism7.0 (San Diego, CA) was used. Each experiment was repeated three times. Data were shown as mean ± SD. One-way analysis of variance (ANOVA) with Tukey’s post hoc tests was used for comparison. P values less than 0.05 were defined as statistically significant.
Results
Isolation and identification of exosomes
We first collected serum from patients with sepsis lung injury and healthy controls to extract serum exosomes by ultra-high-speed centrifugation. Exosomes were successfully isolated from both patients with sepsis lung injury (Sepsis_exo, n = 10) and healthy controls (Control_exo, n = 10) as shown by TEM in Fig. 1a. The exosomes were further confirmed by measurement of exosomal markers Alix and CD63 (Fig. 1b). Then the exosomes were co-cultured with BEAS-2B cells. The endocytosis of the exosome was monitored using PKH-67 staining and results showed that exosomes could be endocytosed by BEAS-2B cells (Fig. 1c). The successful Isolation of exosomes laid the foundation of this study.
Isolation and identification of exosomes. Serum samples were collected, and serum exosomes were extracted by ultra-high-speed centrifugation. (a) Transmission electron microscope observation of exosomes. (b) Immunoblotting of exosomal markers Alix and CD63. (c) Exosomes from patients with sepsis lung injury and healthy controls were co-cultured with human lung bronchial epithelial cells BEAS-2B. Sepsis patients: n = 10; Healthy control: n = 10. PKH-67 was used to monitor endocytosis of exosomes by BEAS-2B cells
Sepsis_exo significantly suppressed proliferation and enhanced permeability and inflammation in BEAS-2B cells
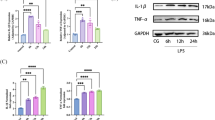
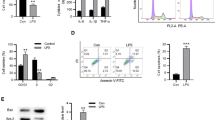
Next, BEAS-2B cells were treated by exosomes for 24 h to study the effect of exosomes on BEAS-2B cells. Sepsis_exo treatment significantly suppressed proliferation of BEAS-2B cells (Fig. 2a), increased cell permeability shown by the decrease of transmembrane resistance (Fig. 2b) and increase of FITC leakage (Fig. 2c). Sepsis_exo treatment also significantly enhanced TNF-α and IL-6 compared to that of controls (Fig. 2d). Q-PCR analysis indicated that Sepsis_exo treatment significantly decreased the expression of SOCS6 at mRNA level (Fig. 2e). Western blot results showed that Sepsis_exo treatment remarkably decreased the expression of SOCS6, sharply increased the expression p-STAT3, while had no significant effect on the expression of STAT3 (Fig. 2f). These findings suggested that Sepsis_exo significantly induced human lung bronchial epithelial cell injury.
Sepsis-exo suppressed proliferation, and enhanced permeability and inflammatory response in BEAS-2B cells. BEAS-2B cells were treated by exosomes (100 μg/ml) for 24 h. Sepsis patients: n = 10; Healthy control: n = 10. (a) Cell proliferation detected by CCK8 (0/12 h/24 h/48 h). (b, c) Transmembrane resistance (b) and FITC leakage test (c) to analyze cell permeability. (d) TNF-α and IL-6 levels. (e) Q-PCR analysis of the expression of SOCS6. (f) Western blot measurement of SOCS6, STAT3 and p-STAT3. At least 3independentrepeatdata. *p < 0.05, **p < 0.01, ***p < 0.001 vs. Control_exo
miR-1298-5p negatively regulated the activity of SOCS6 3′UTR promoter
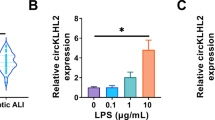
To investigate how Sepsis_exo treatment regulates SOCS6, we first checked exosomal miR-1298-5p level. Q-PCR indicated that miR-1298-5p was remarkably increased in Sepsis_exo compared to that of Control_exo (Fig. 3a). Then we did a bioinformatics analysis and found a potential binding site of miR-1298-5p in the 3′UTR of SOCS6. So, SOCS6 3′UTR-WT/3′UTR-Mut, and miR-1298-5p inhibitor/mimic were co-transfected into BEAS-2B cells. Luminescence assay indicated that inhibition of miR-1298-5p significantly increased SOCS6 promoter activity, which was sharply suppressed by overexpressing miR-1298-5p. Mutation of SOCS6′s miR-1298-5p binding site blocked miR-1298-5p’s effect on SOCS6 promoter (Fig. 3b). Then, miR-1298-5p was successfully overexpressed or silenced (Fig. 3c). Silencing miR-1298-5p up-regulated SOCS6, while overexpressing miR-1298-5p significantly suppressed SOCS6 at both mRNA and protein level (Fig. 3d, e). Next, different concentrations of Sepsis_exo (0, 50, 100, 200 μg/ml) were co-cultured with BEAS-2B cells. Q-PCR analysis indicated that miR-1298-5p increased along with the increase of Sepsis_exo concentration (Fig. 3f). In contrast, the levels of SOCS6 decreased along with the increased of Sepsis_exo concentration at both mRNA and protein levels (Figs. 3g, h). The findings indicated that miR-1298-5p negatively regulated SOCS6.
miR-1298-5p negatively regulated the activity of SOCS6 3′UTR promoter. (a) miR-1298-5p level in serum exosomes (n = 10, ***p < 0.001 vs. Control_exo). Sepsis patients: n = 10; Healthy control: n = 10. SOCS6 3′UTR-WT/3′UTR-Mut, miR-1298-5p inhibitor/mimic were used to transfect BEAS-2B cells. (b) The luciferase reporter assay of SOCS6 luciferase activity. *p < 0.05, ***p < 0.001 vs. WT + NC. (c) Q-PCR analysis of the expression of miR-1298-5p. (d) SOCS6 mRNA level. (e) SOCS6 protein level. *p < 0.05, **p < 0.01, ***p < 0.001 vs. NC. Different concentrations of Sepsis-exo (0, 50, 100, 200 μg/ml) were used to treat BEAS-2B cells. (f, g) miR-1298-5p and SOCS6 levels. (h) Western blot detection of the expression of SOCS6. At least 3 independent repeat data. *p < 0.05, **p < 0.01, ***p < 0.001 vs. Vehicle; #p < 0.05 vs. 50 μg/ml_exo; ++p < 0.01 vs. 100 μg/ml_exo
Overexpression of SOCS6 reversed miR-1298-5p-induced permeability and inflammatory response in BEAS-2B cells
To figure out how miR-1298-5p increased cell permeability and inflammatory response of BEAS-2B cells, we successfully overexpressed SOCS6 in BEAS-2B cells as indicated by Q-PCR (Supplementary Fig. 1a) and Western blot (Supplementary Fig. 1b). SOCS6-overexpressing BEAS-2B cells were then treated by Sepsis_exo. Results showed that overexpressing SOCS6 abolished Sepsis_exo caused decrease of TEER (Fig. 4a), increase of FITC leakage (Fig. 4b), elevation of TNF-α and IL-6 (Fig. 4c), suppression of SOCS6 and increase of p-STAT3 (Fig. 4d). Likewise, overexpressing SOCS6 also ameliorated miR-1298-5p mimic caused decrease of TEER (Fig. 4e), increase of FITC leakage (Fig. 4f), elevation of TNF-α and IL-6 (Fig. 4g), and suppression of SOCS6 and increase of p-STAT3 (Fig. 4h). These findings demonstrated that SOCS6 overexpression reversed miR-1298-5p-caused cell permeability and inflammation.
Overexpression of SOCS6 reversed miR-1298-5p-induced cell permeability and inflammation. SOCS6-overexpressing cells were treated with Sepsis-Exo (100 μg/ml). (a) Transmembrane resistance and (b) FITC leakage test were used to analyze cell permeability. (c) ELISA measurement of TNF-α and IL-6 in supernatant. (d) Western blot analysis of SOCS6, STAT3, and p-STAT3.At least 3 independent repeat data. **p < 0.01, ***p < 0.001 vs. Vehicle; ##p < 0.01, ###p < 0.001 vs. exo + Vector. SOCS6-overexpressing cells were treated with miR-1298-5p mimic. (e) Transmembrane resistance and (f) FITC leakage test analysis of cell permeability. (g) ELISA measurement of TNF-α and IL-6 in supernatant. (h) Western blot analysis of SOCS6, STAT3, and p-STAT3. At least 3 independent repeat data. **p < 0.01, ***p < 0.001 vs. NC; ##p < 0.01, ###p < 0.001 vs. Mimic + Vector
SOCS6 regulated cell permeability and inflammatory response in BEAS-2B cells through STAT3 pathway
To further investigate how SOCS6 regulated cell permeability and inflammation, we silenced SOCS6 in BEAS-2B cells (Supplementary Fig. 2a, b). Results showed that SOCS6-silencing caused a significant decrease of transmembrane resistance and increase of FITC leakage, which were reversed by inhibition of STAT3 (Fig. 5a, b). SOCS6-silencing induced elevation of TNF-α and IL-6 was also blocked by inhibition of STAT3 (Fig. 5c). SOCS6-silencing significantly increased p-STAT3 level, which was blocked by inhibition of STAT3 (Fig. 5d). These findings suggested that STAT3 pathway mediated the effect of SOCS6 on cell permeability and inflammatory response in BEAS-2B cells.
SOCS6 regulated cell permeability and inflammation probably through STAT3 pathway. After silencing of SOCS6, BEAS-2B cells were treated STAT3 inhibitor. (a) Transmembrane resistance and (b) FITC leakage test were used to detect cell permeability. (c) ELISA measurement of TNF-α and IL-6 in supernatant. (d) Western blot analysis of STAT3 and p-STAT3. At least 3 independent repeat data.**p < 0.01, ***p < 0.001 vs. shNC; ##p < 0.01, ###p < 0.001 vs. shSOCS6 + Vehicle
Discussion
We demonstrated that miR-1298-5p was significantly increased in exosomes isolated from patients with sepsis. Sepsis_exo treatment of BEAS-2B cells inhibited cell proliferation, induced cell permeability and inflammatory response. Mechanism study showed that inhibition of miR-1298-5p attenuated sepsis_exo-induced cell permeability and inflammatory response by targeting SOCS6. Data also suggested that SOCS6 regulated cell permeability and inflammatory response in BEAS-2B cells through STAT3 signaling pathway.
miRNAs have been implicated in a variety of diseases [35]. miRNA dysregulation plays a crucial role in regulating cell proliferation, migration, apoptosis, and so on [36, 37]. Roderburg et al. have reported that miRNAs were presented in plasma and were useful in the prediction of survival in patients of sepsis [29]. Fan et al. further confirmed miRNA exsitence in exosomes during sepsis [38]. Real et al. showed that Sepsis_exo convey miRNAs including miR-1298, suggesting that exosomes are involved in intercellular communication during sepsis [39]. In this study, we further explored miR-1298. We found that miR-1298-5p was significantly increased in the exosomes isolated from patients of sepsis lung injury. Moreover, it was further proved that exosomal miR-1298-5p enhanced cell permeability and induced inflammatory responses, leading to human lung bronchial epithelial cell injury. These findings revealed a new role of miR-1298-5p in sepsis lung injury, showing that miR-1298-5p promoted BEAS-2B cell injury by enhancing cell permeability and promoting inflammatory responses.
Recent years, various targets of miR-1298-5p have been reported. For instance, Li et al. have shown that miR-1298 targeted Cx43 to regulate the progression of bladder cancer [35]. A study by Zhou et al. indicated that miR-1298 targeted tyrosine kinase FAK to inhibit mutant KRAS-driven tumor growth [40]. Qiu et al. have shown that lower miR-1298 expression was a risk factor for survival in gastric cancer (GC) patients and miR-1298 overexpression suppressed PI3K/AKT signaling pathway to inhibit cell proliferation [41]. Wu et al. has reported that miR-1298 was significantly decreased in glaucoma [42]. Besides, SOCS protein has been demonstrated to be involved in the inflammatory responses in ALI as a miRNA target [19]. Filgueiras et al. have reported that SOCS protein was involved in the ALI secondary to sepsis in diabetic rats [18]. In the current study, we showed that exosomal miR-1298-5p bound to 3′UTR of SOCS6 promoter to negatively regulated SOCS6 expression at both mRNA and protein levels. This was further confirmed by the findings that overexpression of SOCS6 reversed miR-1298-5p-induced cell permeability and inflammation in BEAS-2B cells. These findings not only increase our knowledge of miR-1298-5p/SOCS6 in human lung bronchial epithelial cell injury but also broaden our understanding of the pathogenesis of sepsis lung injury.
Furthermore, STAT3 has been shown to be a major mediator of inflammation [21]. Nguyen et al. showed that STAT3 played a key role in inflammation-induced tumor progression [43]. STAT3 has also been shown to be activated in actively inflamed colons from inflammatory bowel disease (IBD) patients [44]. Persistent activation of STAT3 has also been shown to mediate tumor-promoting inflammation [21]. Data also suggested that inhibiting p-STAT3 increased the survival of sepsis rats, decreased lungs injury, and reduced inflammation in sepsis rats [22]. In this study, we showed that inhibition of STAT3 abolished SOCS6-silencing caused increase of cell permeability and inflammatory responses in BEAS-2B cells, suggesting the important role of STAT3 in the regulation of SOCS6-mediated cell permeability and inflammation. These findings indicate a very important role of miR-1298-5p/SOCS6/STAT3 in the induction of lung epithelial cell damage, and thus, improve our understanding of the pathogenesis of sepsis lung injury. There are certainly some limitations in this study. For example, this study was mainly performed in cells. Future studies in animal models or using clinical samples will provide more relevant data. Although further studies are needed, the current study reports a new mechanism underlying sepsis lung injury.
In conclusion, the current study revealed a new role of miR-1298-5p/SOCS6/STAT3 signaling, showing that exosomes isolated from patients with sepsis lung injury caused human lung bronchial epithelial cell injury through miR-1298-5p and its target SOCS6 via regulating STAT3 signaling pathway. These results identified the important role of miR-1298-5p/SOCS6/STAT3 signaling which has great relevance to the pathogenesis of sepsis, and may facilitate the development of new drugs for sepsis, ALI and ARDS.
Data availability
All data generated or analyzed during this study are included in this published article.
Abbreviations
- ALI:
-
Acute lung injury
- miRNAs:
-
MicroRNAs
- SOCS6:
-
Suppressor of cytokine signaling 6
- TEER:
-
Trans-epithelial electrical resistance
- Sepsis_exo:
-
Exosomes from patients with sepsis lung injury
- CIS:
-
Cytokine-inducible SH2-containing protein
- STAT3:
-
Signal transducer and activator of transcription 3
- EVs:
-
Extracellular vesicles
- GC:
-
Gastric cancer
- IBD:
-
Inflammatory bowel disease
References
Singer M, Deutschman CS, Seymour CW, Shankar-Hari M, Annane D, Bauer M, Bellomo R, Bernard GR, Chiche JD, Coopersmith CM, Hotchkiss RS, Levy MM, Marshall JC, Martin GS, Opal SM, Rubenfeld GD, van der Poll T, Vincent JL, Angus DC (2016) The third international consensus definitions for sepsis and septic shock (sepsis-3). JAMA 315:801–810
Sakr Y, Jaschinski U, Wittebole X, Szakmany T, Lipman J, Namendys-Silva SA, Martin-Loeches I, Leone M, Lupu MN, Vincent JL, Investigators I (2018) Sepsis in intensive care unit patients: worldwide data from the intensive care over nations audit. Open Forum Infect Dis 5:ofy313
Clemente G, Tuttolomondo A, Colomba D, Pecoraro R, Renda C, Della Corte V, Maida C, Simonetta I, Pinto A (2015) When sepsis affects the heart: a case report and literature review. World J Clin Cases 3:743–750
Gyawali B, Ramakrishna K, Dhamoon AS (2019) Sepsis: the evolution in definition, pathophysiology, and management. SAGE Open Med 7:2050312119835043
Gajic O, Dabbagh O, Park PK, Adesanya A, Chang SY, Hou P, Anderson H 3rd, Hoth JJ, Mikkelsen ME, Gentile NT, Gong MN, Talmor D, Bajwa E, Watkins TR, Festic E, Yilmaz M, Iscimen R, Kaufman DA, Esper AM, Sadikot R, Douglas I, Sevransky J, Malinchoc M, Illness USC (2011) Injury Trials Group: lung injury prevention study I. Early identification of patients at risk of acute lung injury: evaluation of lung injury prediction score in a multicenter cohort study. Am J Respir Crit Care Med 183:462–470
Maybauer MO, Maybauer DM, Herndon DN (2006) Incidence and outcomes of acute lung injury. N Engl J Med 354:416–417
Iscimen R, Cartin-Ceba R, Yilmaz M, Khan H, Hubmayr RD, Afessa B, Gajic O (2008) Risk factors for the development of acute lung injury in patients with septic shock: an observational cohort study. Crit Care Med 36:1518–1522
Fein AM, Calalang-Colucci MG (2000) Acute lung injury and acute respiratory distress syndrome in sepsis and septic shock. Crit Care Clin 16:289–317
Goodman RB, Pugin J, Lee JS, Matthay MA (2003) Cytokine-mediated inflammation in acute lung injury. Cytokine Growth Factor Rev 14:523–535
Lotem J, Sachs L (2002) Cytokine control of developmental programs in normal hematopoiesis and leukemia. Oncogene 21:3284–3294
Sasi W, Sharma AK, Mokbel K (2014) The role of suppressors of cytokine signalling in human neoplasms. Mol Biol Int 2014:630797
Kabir NN, Sun J, Ronnstrand L, Kazi JU (2014) SOCS6 is a selective suppressor of receptor tyrosine kinase signaling. Tumour Biol 35:10581–10589
Lai RH, Wang MJ, Yang SH, Chen JY (2009) Genomic organization and functional characterization of the promoter for the human suppressor of cytokine signaling 6 gene. Gene 448:64–73
Yoon S, Yi YS, Kim SS, Kim JH, Park WS, Nam SW (2012) SOCS5 and SOCS6 have similar expression patterns in normal and cancer tissues. Tumour Biol 33:215–221
Wu Q, Luo G, Yang Z, Zhu F, An Y, Shi Y, Fan D (2014) miR-17-5p promotes proliferation by targeting SOCS6 in gastric cancer cells. FEBS Lett 588:2055–2062
Zhu JG, Dai QS, Han ZD, He HC, Mo RJ, Chen G, Chen YF, Wu YD, Yang SB, Jiang FN, Chen WH, Sun ZL, Zhong WD (2013) Expression of SOCSs in human prostate cancer and their association in prognosis. Mol Cell Biochem 381:51–59
Letellier E, Schmitz M, Baig K, Beaume N, Schwartz C, Frasquilho S, Antunes L, Marcon N, Nazarov PV, Vallar L, Even J, Haan S (2014) Identification of SOCS2 and SOCS6 as biomarkers in human colorectal cancer. Br J Cancer 111:726–735
Filgueiras LR Jr, Martins JO, Serezani CH, Capelozzi VL, Montes MB, Jancar S (2012) Sepsis-induced acute lung injury (ALI) is milder in diabetic rats and correlates with impaired NFkB activation. PLoS ONE 7:e44987
Zhang Y, Xie Y, Zhang L, Zhao H (2020) MicroRNA-155 participates in smoke-inhalation-induced acute lung injury through inhibition of SOCS-1. Molecules 25:1022
Wang H, Lafdil F, Kong X, Gao B (2011) Signal transducer and activator of transcription 3 in liver diseases: a novel therapeutic target. Int J Biol Sci 7:536–550
Yu H, Pardoll D, Jove R (2009) STATs in cancer inflammation and immunity: a leading role for STAT3. Nat Rev Cancer 9:798–809
Wang C, Zhou G, Zeng Z (2014) Effects of peroxisome proliferator-activated receptor-beta/delta on sepsis induced acute lung injury. Chin Med J (Engl) 127:2129–2137
Ikegami M, Falcone A, Whitsett JA (1985) STAT-3 regulates surfactant phospholipid homeostasis in normal lung and during endotoxin-mediated lung injury. J Appl Physiol 2008(104):1753–1760
Jones MR, Quinton LJ, Simms BT, Lupa MM, Kogan MS, Mizgerd JP (2006) Roles of interleukin-6 in activation of STAT proteins and recruitment of neutrophils during Escherichia coli pneumonia. J Infect Dis 193:360–369
Kalluri R, LeBleu VS (2020) The biology, function, and biomedical applications of exosomes. Science 367:eaau6977
Lv LL, Cao YH, Ni HF, Xu M, Liu D, Liu H, Chen PS, Liu BC (2013) MicroRNA-29c in urinary exosome/microvesicle as a biomarker of renal fibrosis. Am J Physiol Renal Physiol 305:F1220-1227
Valadi H, Ekstrom K, Bossios A, Sjostrand M, Lee JJ, Lotvall JO (2007) Exosome-mediated transfer of mRNAs and microRNAs is a novel mechanism of genetic exchange between cells. Nat Cell Biol 9:654–659
Benz F, Tacke F, Luedde M, Trautwein C, Luedde T, Koch A, Roderburg C (2015) Circulating microRNA-223 serum levels do not predict sepsis or survival in patients with critical illness. Dis Markers 2015:384208
Roderburg C, Luedde M, Vargas Cardenas D, Vucur M, Scholten D, Frey N, Koch A, Trautwein C, Tacke F, Luedde T (2013) Circulating microRNA-150 serum levels predict survival in patients with critical illness and sepsis. PLoS ONE 8:e54612
Wang C, Zhou G, Zeng Z (2014) Effects of peroxisome proliferator-activated receptor-β/δ on sepsis induced acute lung injury. Chin Med J (Engl) 127:2129–2137
Peng W, Jiang R, Li Y, Chen J, Shao Q, Qian K, Liu F (2021) Exosomes derived from human-induced pluripotent mesenchymal stem cells inhibit the pyrolysis of alveolar macrophages. Zhonghua Wei Zhong Bing Ji Jiu Yi Xue 33:43–48
Zheng JP, Dai YM, Chen Z, Chen Q, Zheng Y, Lin X, Cui TJ (2020) Circular RNA circ-ABCB10 promotes non-small cell lung cancer proliferation and inhibits cell apoptosis through repressing KISS1. Eur Rev Med Pharmacol Sci 24:2518–2524
Livak KJ, Schmittgen TD (2001) Analysis of relative gene expression data using real-time quantitative PCR and the 2(-Delta Delta C(T)) Method. Methods 25:402–408
Van Den Broucke S, Vanoirbeek J, Alfaro-Moreno E, Hoet P (2020) Contribution of mast cells in irritant-induced airway epithelial barrier impairment in vitro. Toxicol Ind Health 36:823–834
Li G, Sun L, Mu Z, Liu S, Qu H, Xie Q, Hu B (2020) MicroRNA-1298-5p inhibits cell proliferation and the invasiveness of bladder cancer cells via down-regulation of connexin 43. Biochem Cell Biol 98:227–237
Wang CM, Cheng BH, Xue QJ, Chen J, Bai B (2017) MiR-1298 affects cell proliferation and apoptosis in C6 cells by targeting SET domain containing 7. Int J Immunopathol Pharmacol 30:264–271
Cai G, Qiao S, Chen K (2015) Suppression of miR-221 inhibits glioma cells proliferation and invasion via targeting SEMA3B. Biol Res 48:37
Fan H, Goodwin AJ, Chang E, Zingarelli B, Borg K, Guan S, Halushka PV, Cook JA (2014) Endothelial progenitor cells and a stromal cell-derived factor-1alpha analogue synergistically improve survival in sepsis. Am J Respir Crit Care Med 189:1509–1519
Real JM, Ferreira LRP, Esteves GH, Koyama FC, Dias MVS, Bezerra-Neto JE, Cunha-Neto E, Machado FR, Salomao R, Azevedo LCP (2018) Exosomes from patients with septic shock convey miRNAs related to inflammation and cell cycle regulation: new signaling pathways in sepsis? Crit Care 22:68
Zhou Y, Dang J, Chang KY, Yau E, Aza-Blanc P, Moscat J, Rana TM (2016) miR-1298 inhibits mutant KRAS-driven tumor growth by repressing FAK and LAMB3. Cancer Res 76:5777–5787
Qiu ZK, Liu N, Zhao SF, Ding AP, Cheng G, Qiu WS, Qi WW (2018) MiR-1298 expression correlates with prognosis and inhibits cell proliferation and invasion of gastric cancer. Eur Rev Med Pharmacol Sci 22:1672–1679
Ruibin W, Zheng X, Chen J, Zhang X, Yang X, Lin Y (2018) Micro RNA-1298 opposes the effects of chronic oxidative stress on human trabecular meshwork cells via targeting on EIF4E3. Biomed Pharmacother 100:349–357
Nguyen AV, Wu YY, Liu Q, Wang D, Nguyen S, Loh R, Pang J, Friedman K, Orlofsky A, Augenlicht L, Pollard JW, Lin EY (2013) STAT3 in epithelial cells regulates inflammation and tumor progression to malignant state in colon. Neoplasia 15:998–1008
Lovato P, Brender C, Agnholt J, Kelsen J, Kaltoft K, Svejgaard A, Eriksen KW, Woetmann A, Odum N (2003) Constitutive STAT3 activation in intestinal T cells from patients with Crohn’s disease. J Biol Chem 278:16777–16781
Acknowledgement
We would like to thank TopEdit (www.topeditsci.com) for English language editing of this manuscript.
Author information
Authors and Affiliations
Contributions
J.M. designed this projected and wrote the manuscript; J.M., L.Y.X. performed the experiments; Q.H.S., X.Y.W., B.L. analyzed the data and edited diagrams. All authors have contributed to, read, and agreed upon the final contents of the manuscript for submission.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare that they have no conflict of interest.
Ethical approval
The protocol for the present study was approved by the Ethics Committee of Shanghai Pulmonary Hospital (Shanghai, China), and it conforms to the provisions of the Declaration of Helsinki in 1995. All participants have provided their written informed consent to participate in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Ma, J., Xu, LY., Sun, QH. et al. Inhibition of miR-1298-5p attenuates sepsis lung injury by targeting SOCS6. Mol Cell Biochem 476, 3745–3756 (2021). https://doi.org/10.1007/s11010-021-04170-w
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-021-04170-w