Abstract
Abnormal expression of high-mobility group box-1 (HMGB1) protein occurs in many tumors and is closely associated with tumor invasion and metastasis. However, a role for HMGB1 in epithelial–mesenchymal transition (EMT) in hypopharyngeal carcinoma has not been previously reported. We cultured cells of the hypopharyngeal carcinoma cell line FaDu in vitro and then treated them with 5 ng/ml TGF-β1 for 48 h to induce EMT. Vimentin, Snail, and HMGB1 expression patterns were then detected using immunofluorescence staining; HMGB1 mRNA and protein expression were verified by RT-PCR and western blot analyses. HMGB1 was then silenced in FaDu cells using RNAi, followed by detection of Vimentin, Snail, and HMGB1 expressions by immunofluorescence staining. The mRNA expression levels of Vimentin, Snail, HMGB1, and E-cadherin were verified by RT-PCR, while protein expression of HMGB1 and receptor for advanced glycation end products (RAGE) were detected by western blot analysis. The biological behavior of FaDu cells was observed before and after HMGB1 silencing using wound healing and cell invasion assays. Following culture with 5 ng/ml TGF-β1 for 48 h, the morphology of FaDu cells changed from a regular cobblestone-like appearance into a spindle-like shape. Expression levels of Vimentin, Snail, and HMGB1 were upregulated at both mRNA and protein levels as determined by RT-PCR, immunofluorescence, and western blotting. After HMGB1 silencing, mRNA expression levels of the epithelial cell marker E-cadherin were upregulated. Meanwhile, expression levels of the mesenchymal markers Vimentin and Snail were decreased. Western blotting revealed that HMGB1 and RAGE were downregulated. RNAi-mediated inhibition of HMGB1 expression decreased the capacities of FaDu cells for invasion and metastasis as determined by wound healing and cell invasion assays. HMGB1 is essential for maintaining the interstitial cell phenotype in TGF-β1-induced EMT of FaDu cells, and silencing HMGB1 greatly inhibits the invasive and metastatic ability of these cells.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hypopharyngeal squamous cell carcinoma originates from mucosal cells of the upper gastrointestinal tract and has a high degree of malignancy [1]. The early symptoms of hypopharyneal squamous cell carcinoma are variable, and the tumor has poor biological characteristics which often cause lymph node metastases and lead to difficulties in early diagnosis and ultimately a poor prognosis. While there has been great progress in treating hypopharyngeal carcinoma, the 5-year survival rate remains at 25–40% [2]. Therefore, further study of the mechanisms underlying the occurrence and development of hypopharyngeal carcinoma is needed to aid discovery of new and effective therapeutic strategies.
Yu et al. [3] recently demonstrated that TNFα promotes epithelial–mesenchymal transition (EMT) in hypopharyngeal carcinoma through increased expression of the transcription factor Twist. Elevated levels of Twist induce EMT-like changes in cell morphology, result in intercellular junction disappearance, and promote the invasion and metastasis of hypopharyngeal carcinoma FaDu cells. The concept of EMT was first proposed by Greenberg et al. in 1982, and refers to the transition of polarized epithelial cells to mesenchymal-like cells capable of migration under special physical and pathological conditions. Cells that have undergone EMT exhibit a loss of intercellular polarity, adopt a spindle-shaped fibroblast-like morphology, and have decreased expression of epithelial cell markers such as epithelial cadherin (E-cadherin). Additionally, the expression levels of mesenchymal markers including Vimentin and N-cadherin are upregulated, as are levels of EMT-activating transcription factors such as Snail, Twist, ZEB1, ZEB2, and FOXC2. EMT endows cancer cells with an invasive and metastatic ability [5]. The EMT phenomenon has been observed in head and neck squamous cell carcinoma [6], breast cancer [7], ovarian cancer [8], colon cancer [9], and many other cancers.
The high-mobility group (HMG) comprises three families of highly conserved chromosomal proteins—HMGA, HMGB, and HMGN [10]. The HMGB family member HMG box-1 (HMGB1), also known as amphoterin, is a non-histone chromatin-binding protein found in eukaryotic cells which is involved in maintaining nucleosome structure and dynamics, DNA repair, and DNA recombination [11, 12].Prior studies have predominately focused on the role of HMGB1 in inflammatory and autoimmune diseases [13]. However, recent years have seen more attention given to the role of HMGB1 in cancer occurrence and development. Lynch et al. [14] found that HMGB1 is a key mediator of immune-mediated EMT in human proximal tubular epithelial cells, while high expression of HMGB1 is present in multiple malignant tumors [15]. HMGB1 is released into the extracellular matrix by tumor cells [16], where it can immediately bind to cell-surface receptors and activate downstream signaling pathways. Receptor for advanced glycation end products (RAGE), Toll-like receptor (TLR)-2, and TLR4 are the main receptors for HMGB1 [17–19]. RAGE expression is low in normal cells, and it is expressed at high levels after HMGB1 binds to the cell surface [17]. The role of the HMGB1–RAGE interaction in cancer development has been widely reported, with HMGB1 inducing cancer cell invasion, metastasis, tumor growth, and distant metastases via binding to RAGE [20, 21]. Zhu et al. [9] showed that HMGB1 can activate MMP-7 through the RAGE/Snail/NF-κB signaling pathway, eventually inducing EMT in colon cancer cells. However, whether HMGB1 plays a role in EMT in hypopharyngeal carcinoma cells is unknown.
In this study, we measured HMGB1 expression levels in a hypopharyngeal carcinoma cell line. We then used these cells to explore the role of HMGB1 in EMT and tumor invasion by RNA interference (RNAi).
Materials and method
Cells and antibody
The hypopharyngeal carcinoma cell line FaDu was obtained from Guangzhou Jinibio Biotechnology Co., Ltd. (Guangzhou, China). Antibodies targeting HMGB1, Vimentin, and Snail were purchased from Bioss (Beijing, China). Rabbit anti-human RAGE antibody was obtained from Abcam (Cambridge, UK). Mouse anti-GAPDH was purchased from Peprotech (Rocky Hill, NJ, USA). HRP-labeled goat anti-rabbit IgG and HRP-labeled goat anti-mouse IgG were from Santa Cruz Biotechnology, Inc (Santa Cruz, CA, USA).
Cell culture and establishment of the EMT model
FaDu cells were cultured in RPMI 1640 medium supplemented with 10% fetal bovine serum in an incubator at 37 °C with a 5% CO2 atmosphere. Cells were passaged every 2–3 days to ensure maintenance of an exponential growth phase. TGF-β1 was diluted with complete medium to a concentration of 5 ng/ml, and FaDu cells were cultured with 5 ng/ml TGF-β1 for 48 h. Cell morphology was observed and photographed with phase contrast microscopy.
siRNA transfection
siRNA interference vectors targeting the human HMGB1 gene sequence (NM-002128) were designed and synthesized by Shanghai Genechem Co., Ltd. The target sequence was AGATGACAAGCAGCCTTAT. The shRNA sequences were 5′-GATCCCgcAGATGACAAGCAGCCTTATCTCGAGATAAGGCTGCTTGTCATCTGCTTTTTGGAT-3′ and 5′-AGCTATCCAAAAAgcAGATGACAAGCAGCCTTATCTCGAGATAAGGCTGCTTGTCATCTGCGG-3′. The shRNA-coding oligonucleotides were inserted into the multiple cloning site of the GV102 vector, which contains hU6-MCS-CMV-GFP-SV40-Neomycin cis-action elements. A scrambled siRNA sequence was used as a control vector. FaDu cells were seeded into a 35-mm-diameter culture dish, and, upon reaching 75% confluence, were transfected with HMGB1 or control siRNA vectors according to the manufacturer’s instructions. HMGB1 mRNA and protein expression levels were measured using qPCR and western blot analysis, respectively.
Immunofluorescence staining
Cells were seeded onto glass slides and after 24 h were washed with phosphate-buffered saline (PBS), fixed with 4% paraformaldehyde at room temperature for 30 min, permeabilized in 0.1% Triton X-100, blocked in 5% goat serum for 1 h, and then incubated with primary antibody (1:100) overnight at 4 °C. The next day, cells were washed three times with PBS, incubated with secondary antibody (1:200) for 1 h at room temperature in dark, and washed three times with PBS. Cells were mounted in 50% glycerol and then observed and photographed using laser confocal microscopy (Fluo-View FV1000; Olympus, Japan).
Real-time qPCR assay
Total RNA was extracted from FaDu cells using TRIzol reagent and then reverse-transcribed to cDNA using the Quantscript reverse transcription kit (Tiangen, Beijing) according to the manufacturer’s instructions. Amplification was conducted using a SYBR Green I PCR kit (Roche, Indianapolis, IN, USA). Primer sequences are shown in Table 1. The PCR reaction conditions used were as follows: initial denaturation at 95 °C for 10 min, followed by 35 amplification cycles of 95 °C for 10 s, 55 °C for 10 s, 72 °C for 15 s, and a final extension at 72 °C for 10 min. GAPDH was used as an internal reference gene. Relative values for mRNA levels were calculated using the formula: Fold change = 2−△△CT.
Western blotting
FaDu cells grown on 6-well plates were lysed in 200 μl of Cell Lysis Buffer (5 mM EDTA, 150 mM NaCl, 50 mM Tris–HCl, and 1% TritonX-100 in ddH20). Total protein concentration was determined using a Beyotime Institute of Biotechnology bicinchoninic acid protein assay Kit (Nantong, Jiangsu, China). Proteins were subjected to 10% sodium dodecyl sulfate polyacrylamide gel electrophoresis and then electrically transferred to polyvinylidene fluoride membranes using constant current of 200 mA. The membrane was blocked with 5% non-fat milk powder for 1 h and then incubated with anti-HMGB1 or anti-RAGE antibody overnight at 4 °C, washed three times with TBST, and then incubated with HRP-labeled secondary antibody at room temperature for 1.5 h. ECL reagent (Thermo Fisher Scientific, Waltham, MA, USA) was used to visualize protein bands, and images were obtained using a Dolphin‑C hemi Mini image system (Wealtec Corp., Sparks, NV, USA). Gray values for each protein band were analyzed using Image J analysis software, and relative protein levels were calculated using GAPDH as an internal control.
Wound healing assay
Approximately 2 × 105 FaDu cells were plated in each well of a 6-well plate, and 5 ng/ml TGF-β was added. When cell confluency reached 90%, three scratches were gently made in straight lines across the well using a sterile pipette tip. Cells were then washed with serum-free medium and transfected with HMGB1 or control siRNA vectors. At 0, 24, and 48 h, cell migration to injury sites was recorded using photography.
Cell invasion assay
Cell invasion capacity was determined using a Matrigel-coated Transwell chamber (Costar Co., Cambridge, MA) containing 8 μm pore size polycarbonate microporous membranes between the upper and lower chambers. Membranes were coated with 90 μl artificial Matrigel, and FaDu cells were treated with 5 ng/ml TGF-β and then pre-transfected with shHMGB1 or control vector for 48 h. Approximately 4 × 104 cells in 200 μl of serum-free medium were then seeded into the upper chambers, while NIH3T3 cell supernatant was added to the lower chambers. After 20 h incubation, cells were observed using an FV 1000 laser confocal fluorescence microscope and five fields from each chamber were randomly selected and photographed.
Statistical analysis
All data were collected from at least three independent experiments. Results were analyzed using SPSS17.0 statistical software and are expressed as means ± standard deviation (SD). Student’s t-test, one-way analysis of variance, and multivariate analysis of variance were used to analyze data as appropriate. A value of P < 0.05 was considered statistically significant.
Results
TGF-β1 induces EMT in FaDu hypopharyngeal carcinoma cells
As shown in Fig. 1a–f, phase contrast microscopy revealed that FaDu cell morphology changed from a regular cobblestone-like shape into a spindle-like appearance following treatment with TGF-β1 for 48 h. Immunofluorescence staining showed that expression levels of the mesenchymal markers Vimentin and Snail were higher in TGF-β1-treated cells compared with untreated normal cells.
TGF-β1 induces EMT in FaDu cells. FaDu cells were treated with or without 5 ng/ml TGF-β1 for 48 h. Cell morphology and immunofluorescence analyses were performed. a, d Micrographs depicting cell morphology as seen by light microscopy (scale bar 50 μm). b, c, e, f Immunofluorescence staining of Vimentin and Snail, green fluorescence indicates positive expression; blue fluorescence indicates Hoechst33342-labeled nuclei. Scale bar 10 μm
HMGB1 expression is associated with EMT in hypopharyngeal carcinoma cells
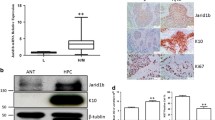
Strong fluorescent intensity for HMGB1 staining was present in TGF-β1-treated FaDu cells (Fig. 2a). We next determined the expression levels of HMGB1 mRNA (Fig. 2b) and protein (Fig. 2c, d) in FaDu cells following TGF-β1 treatment, finding that both were increased (P < 0.01). These findings indicate that HMGB1 is involved in the regulation of EMT in hypopharyngeal carcinoma cells.
HMGB1 expression is associated with EMT in hypopharyngeal carcinoma. FaDu cells were treated with or without 5 ng/ml TGF-β1 for 48 h, and after immunofluorescence analysis, total RNA and protein were extracted and subjected to RT-PCR and western blot analyses. a Green fluorescence indicates HMGB1, blue fluorescence indicates Hoechst33342-labeled nuclei. Bar 10 μm. b Quantitative analysis of HMGB1 mRNA expression, GAPDH served as an internal reference. **P < 0.01 versus untreated group. c, d Detection of HMGB1 protein expression by western blot analysis, GAPDH served as an internal reference, **P < 0.01 versus untreated group
HMGB1 gene silencing reverses the TGF-β1-induced EMT phenotype in hypopharyngeal carcinoma cells
In view of the close relationship between HMGB1 expression and EMT in FaDu cells, we next used RNAi to silence the HMGB1gene. TGF-β1-treated FaDu cells were transfected with shHMGB1 recombinant vector, with the transcription and expression levels of HMGB1 mRNA and protein decreased (Fig. 3a, d). Levels of Vimentin and Snail were significantly decreased in FaDu cells transfected with shHMGB1 vector compared with those transfected with control shRNA vector (Fig. 4a, b). These results indicate that HMGB1 gene silencing can reverse EMT in hypopharyngeal carcinoma cells. Furthermore, E-cadherin mRNA expression was upregulated (P < 0.05), while levels of Vimentin (P < 0.01) and Snail (P < 0.05) mRNA were downregulated in FaDu cells transfected with siHMGB1 (Fig. 4c). These results indicate that HMGB1 plays an important role in maintaining mesenchymal features of hypopharyngeal carcinoma cells.
Silencing of HMGB1 expression reverses EMT in hypopharyngeal carcinoma. HMGB1 or control shRNA vectors were transfected into FaDu cells followed by treatment with 5 ng/ml TGF-β1 for 48 h. Cells were divided into control siRNA group and HMGB1 siRNA groups, and HMGB1 expression was detected. a Red fluorescence indicates HMGB1-positive expression; blue fluorescence indicates Hoechst33342-labeled nuclei; green represents green fluorescent protein indicating transfected cells. Bar 20 μm. b Quantitative analysis of HMGB1 mRNA expression, GAPDH served as an internal reference. *P < 0.05 versus control siRNA group. c, d Western blot analysis of the expression of HMGB1 protein after transfection with siRNA, GAPDH served as an internal reference. **P < 0.01 versus control siRNA group
Immunofluorescence staining for expression of Vimentin and Snail in FaDu cells after transfection with siHMGB1. Red fluorescence indicates Vimentin (a) or Snail (b) expression. Scale bar 10 μm. c Quantitative analysis of E-cadherin, Vimentin, and Snail mRNA expression, GAPDH served as an internal reference. # P < 0.05, ## P < 0.01 versus Control siRNA group
HMGB1 silencing inhibits the invasive capacity of hypopharyngeal carcinoma cells
We next explored whether HMGB1 could influence the invasion and metastasis capacities of hypopharyngeal carcinoma cells by performing a wound healing assay to evaluate the effect of HMGB1 gene silencing on cell migration. Scratch wound healing was observed at 0, 24, and 48 h, with wounds exhibiting a higher healing rate in FaDu cells transfected with control shRNA compared with cells transfected with HMGB1 shRNA (Fig. 5a, b). Evaluation of cell invasion capability revealed that the number of FaDu cells capable of migrating through Matrigel was significantly decreased following silencing of HMGB1 by shRNA (P < 0.01) (Fig. 5c, d).
HMGB1 silencing inhibits the invasive ability of hypopharyngeal carcinoma. a Wound healing assay: FaDu cells were treated with 5 ng/ml TGF-β1 and then transfected with HMGB1 shRNA or control shRNA vector and scratches were made on the well surface. Cells were observed at 0, 24, and 48 h, and photographed. b The percentages of unhealed wound area compared with the initial wound area were calculated using ImageJ software. **P < 0.01. c Cell invasion assay was performed after FaDu cells were cultured with 5 ng/ml TGF-β1 and then transfected with HMGB1 shRNA or control shRNA vector for 48 h. d The number of cells that migrated through the Matrigel was calculated 20 h after cells were seeded. ## P < 0.01
HMGB1 downregulation inhibits expression of RAGE
HMGB1 is involved in the EMT process in hypopharyngeal carcinoma cells, and silencing of HMGB1 inhibits cellular invasion and metastasis, but the underlying mechanisms remain unclear. RAGE is the receptor of HMGB1, so we next used western blotting to measure RAGE expression in HMGB1-depleted FaDu cells that had undergone EMT. RAGE expression was obviously decreased (P < 0.01) (Fig. 6). These findings suggest that RAGE expression is downregulated by gene silencing of HMGB1.
Downregulation of HMGB1 expression inhibits RAGE expression. FaDu cells were transfected with HMGB1 siRNA or control siRNA and cultured with 5 ng/ml TGF-β1 for 48 h. Total protein was extracted from cells and RAGE expression levels determined using western blot analysis; GAPDH served as an internal reference. shRNA HMGB1-transfected groups were compared with the control shRNA group. **P < 0.01
Discussion
The molecular characteristics of EMT include the downregulation of epithelial cell markers and upregulation of mesenchymal markers [22]. While various growth factors and cytokines can induce EMT, TGF-β1 plays an important role in the EMT process [23, 24]. Cellular morphology analysis revealed that FaDu cell morphology changed from a regular cobblestone-like shape to a spindle-like configuration after treatment with TGF-β1. Furthermore, the expression of mesenchymal markers Vimentin and Snail was upregulated in TGF-β1-treated cells, suggesting that TGF-β1 induces EMT in hypopharyngeal carcinoma cells. Moreover, HMGB1 was highly expressed in TGF-β1-treated FaDu cells, consistent with previous reports that high levels of HMGB1 are found in multiple cancer types, including nasopharyngeal carcinoma [25], melanoma [26], colorectal cancer [27], and prostate cancer [28]. However, there are no prior reports investigating the role of HMGB1 in the occurrence and development of hypopharyngeal carcinoma. We used RT-PCR and western blotting analyses to verify the expression of HMGB1 in a hypopharyngeal cell line, and obtained results indicating that HMGB1 expression is associated with EMT in hypopharyngeal carcinoma.
We explored the role of HMGB1 in EMT and the invasion and metastasis processes in hypopharyngeal carcinoma. We used RNAi technology to silence HMGB1 expression, with subsequent immunofluorescence staining and RT-PCR analyses showing that HMGB1 depletion downregulates expression of Vimentin and Snail. Additionally, E-cadherin mRNA expression was upregulated following HMGB1 silencing. E-cadherin is important for maintaining epithelial cell polarity and cell–cell adhesion, and a reduction in E-cadherin expression is an important characteristic of EMT. Therefore, HMGB1 gene silencing may reverse the EMT phenomenon in hypopharyngeal carcinoma.
Evidence suggests that HMGB1 promotes cancer development by enhancing the capacity of cancer cells for proliferation and invasion [29]. Our wound healing and cell invasion assays showed that transfection with HMGB1 siRNA can significantly inhibit hypopharyngeal carcinoma cell invasion.
Previous studies have showed that HMGB1 and its receptor RAGE play important roles in the occurrence, development, and metastasis of various cancers [30, 31]. Kuniyasu et al. [32] reported that RAGE provides a system that can enhance gastric cancer cell invasion and metastasis in vitro, and that this system is associated with metastasis in gastric cancer patients. Moreover, Bhawal et al. [33] found that RAGE protein expression was significantly decreased in metastatic oral squamous cell carcinoma cells following treatment with antisense S-oligodeoxynucleotide. We used western blotting to measure RAGE expression in FaDu cells following RNAi-mediated HMGB1 depletion. FaDu cells transfected with siHMGB1 had significantly reduced levels of RAGE compared with those transfected with control siRNA. These findings suggest that RAGE activation by HMGB1 is involved in the regulation of FaDu cell invasion and metastasis. Yan et al. [34] found that HMGB1 can induce caspase-1 activation by activating TLR4 and RAGE signaling pathways in hepatocellular carcinoma cells exposed to hypoxia. This HMGB1-mediated signaling then promotes tumor invasion and metastasis.
In summary, we have demonstrated for the first time that silencing of HMGB1 can reverse EMT and inhibit invasion and metastasis in a hypopharyngeal carcinoma cell line. Furthermore, HMGB1 regulates hypopharyngeal carcinoma cell invasion and metastasis by signaling through RAGE. Together, these findings suggest that HMGB1 has potential clinical value as a biomarker and therapeutic target in the early diagnosis, treatment, and prognosis of hypopharyngeal carcinoma. Our current findings are at the cellular level, and further animal experiments at the tissue level are warranted to explore the precise molecular mechanism responsible for HMGB1-mediated regulation of invasion and metastasis of hypopharyngeal carcinoma.
References
Hall SF, Groome PA, Irish J, O’Sullivan B (2008) The natural history of patients with squamous cell carcinoma of the hypopharynx. Laryngoscope 118:1362–1371
Wycliffe ND, Grover RS, Kim PD, Simental A Jr. Hypopharyngeal cancer (2007) Top Magn Reson Imaging 18:243–258
Yu L, Lu S, Tian J, Ma J, Li J, Wang H, Xu W (2012) TWIST expression in hypopharyngeal cancer and the mechanism of TWIST-induced promotion of metastasis. Oncol Rep 27:416–422
Mjaatvedt CH, Markwald RR (1989) Induction of an epithelial-mesenchymal transition by an in vivo adheron-like complex. Dev Biol 136:118–128
Fuxe J, Vincent T, Garcia de Herreros A (2010) Transcriptional crosstalk between TGF-β and stem cell pathways in tumor cell invasion: role of EMT promoting Smad complexes. Cell Cycle 9:2363–2374
Liu S, Ye D, Guo W, Yu W, He Y, Hu J et al (2015) G9a is essential for EMT-mediated metastasis and maintenance of cancer stem cell-like characters in head and neck squamous cell carcinoma. Oncotarget 6:6887–6901
Zhang YQ, Wei XL, Liang YK, Chen WL, Zhang F, Bai JW, Qiu SQ, Du CW, Huang WH, Zhang GJ (2015) Over-expressed twist associates with markers of epithelial mesenchymal transition and predicts poor prognosis in breast cancers via ERK and Akt activation. PLoS One 10:e0135851
Wang YL, Zhao XM, Shuai ZF, Li CY, Bai QY, Yu XW, Wen QT (2015) Snail promotes epithelial-mesenchymal transition and invasiveness in human ovarian cancer cells. Int J Clin Exp Med 8:7388–7739
Zhu L, Li X, Chen Y, Fang J, Ge Z (2015) High-mobility group Box 1: A novel inducer of the epithelial–mesenchymal transition in colorectal carcinoma. Cancer Lett 357:527–534
Reeves R (2010) Nuclear functions of the HMG proteins. Biochim Biophys Acta 1799:3–14
Kang R, Zhang Q, Zeh HJ 3rd, Lotze MT, Tang D (2013) HMGB1 in cancer: good, bad, or both? Clin Cancer Res 19:4046–4057
Yan HX, Wu HP, Zhang HL, Ashton C, Tong C, Wu H, Qian QJ, Wang HY, Ying QL (2013) p53 promotes inflammation-associated hepatocarcinogenesis by inducing HMGB1 release. J Hepatol 59:762–768
Yanai H, Ban T, Wang Z, Choi MK, Kawamura T, Negishi H et al (2009) HMGB proteins function as universal sentinels for nucleic-acid-mediated innate immune responses. Nature 462:99–103
Lynch J, Nolan S, Slattery C, Feighery R, Ryan MP, McMorrow T (2010) High-mobility group box protein 1:a novel mediator of inflammatory-induced renal epithelial-mesenchymal transition. Am J Nephrol 32:590–602
Tang D, Kang R, Zeh HJ 3rd, Lotze MT (2010) High-mobility group box 1 and cancer. Biochim Biophys Acta 1799:131–140
Buoncervello M, Borghi P, Romagnoli G, Spadaro F, Belardelli F, Toschi E, Gabriele L (2012) Apicidin, docetaxel combination treatment drives CTCFL expression and HMGB1 release acting as potential antitumor immune response inducers in metastatic breast cancer cells. Neoplasia 14:855–867
Kokkola R, Andersson A, Mullins G, Ostberg T, Treutiger CJ, Arnold B, Nawroth P, Andersson U, Harris RA, Harris HE (2005) RAGE is the major receptor for the proinflammatory activity of HMGB1 in rodent macrophages. Scand J Immunol 61:1–9
Park JS, Svetkauskaite D, He Q, Kim JY, Strassheim D, Ishizaka A, Abraham E (2004) Involvement of toll-like receptors 2 and 4 in the cellular activation by high mobility group box 1 protein. J Biol Chem 279:7370–7377
Bianchi ME (2009) HMGB1 loves company. J Leukoc Biol 86:573–576
Degryse B, de Virgilio M (2003) The nuclear protein HMGB1, a new kind of chemokine? FEBS Lett 553:11–17
Rauvala H, Rouhiainen A (2010) Physiological and pathophysiological outcomes of the interactions of HMGB1 with cell surface receptors. Biochim Biophys Acta 1799:164–170
Janda E, Litos G, Grünert S, Downward J, Beug H (2002) Oncogenic Ras/Her-2 mediate hyperproliferation of polarized epithelial cells in 3D cultures and rapid tumor growth via the PI3K pathway. Oncogene 21:5148–5159
Katsuno Y, Lamouille S, Derynck R (2013) TGF-β signaling and epithelial-mesenchymal transition in cancer progression. Curr Opin Oncol 25:76–84
Wendt MK, Allington TM, Schiemann WP (2009) Mechanisms of the epithelial-mesenchymal transition by TGF-beta. Future Oncol 5:1145–1168
Wu D, Ding Y, Wang S, Zhang Q, Liu L (2008) Increased expression of high mobility group box 1 (HMGB1) is associated with progression and poor prognosis in human nasopharyngeal carcinoma. J Pathol 216:167–175
Poser I, Golob M, Buettner R, Bosserhoff AK (2003) Upregulation of HMG1 leads to melanoma inhibitory activity expression in malignant melanoma cells and contributes to their malignancy phenotype. Mol Cell Biol 23:2991–2998
Kuniyasu H, Yano S, Sasaki T, Sasahira T, Sone S, Ohmori H (2005) Colon cancer cell-derived high mobility group 1/amphoterin induces growth inhibition and apoptosis in macrophages. Am J Pathol 166:751–760
Gnanasekar M, Kalyanasundaram R, Zheng G, Chen A, Bosland MC, Kajdacsy-Balla A (2013) HMGB1: a promising therapeutic target for prostate cancer. Prostate Cancer 2013:157103
Lotze MT, Tracey KJ (2005) High-mobility group box 1 protein (HMGB1): nuclear weapon in the immune arsenal. Nat Rev Immunol 5:331–342
Srinivasan M, Banerjee S, Palmer A, Zheng G, Chen A, Bosland MC, Kajdacsy-Balla A, Kalyanasundaram R, Munirathinam G (2014) HMGB1 in hormone-related cancer: a potential therapeutic target. Hormon Cancer 5:127–5139
Diener KR, Al-Dasooqi N, Lousberg EL (2013) Hay-ball JD. The multifunctional alarmin HMGB1 with roles in the pathophysiology of sepsis and cancer. Immunol Cell Biol 91:443–450
Kuniyasu H, Oue N, Wakikawa A, Shigeishi H, Matsutani N, Kuraoka K, Ito R, Yokozaki H, Yasui W (2002) Expression of receptors for advanced glycation end-products (RAGE) is closely associated with the invasive and metastatic activity of gastric cancer. J Pathol 196:163–170
Bhawal UK, Ozaki Y, Nishimura M, Sugiyama M, Sasahira T, Nomura Y et al (2005) Association of expression of receptor for advanced glycation end products and invasive activity of oral squamous cell carcinoma. Int Soc Cell 69:246–255
Yan W, Chang Y, Liang X, Cardinal JS, Huang H, Thorne SH, Monga SP, Geller DA, Lotze MT, Tsung A (2012) High-mobility group box 1 activates caspase-1 and promotes hepatocellular carcinoma invasiveness and metastases. Hepatology 55:1863–1875
Acknowledgements
The authors would like to thank Dr. Xinrui Wang and Li Yang for their technical help in confocal photograph collection. This study was supported by grants from Jilin Province Technique-Development Plan (20160101051JC).
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors have declared no conflict of interest.
Additional information
Yanmei Li and Ping Wang contributed equally to this work.
Rights and permissions
About this article
Cite this article
Li, Y., Wang, P., Zhao, J. et al. HMGB1 attenuates TGF-β-induced epithelial–mesenchymal transition of FaDu hypopharyngeal carcinoma cells through regulation of RAGE expression. Mol Cell Biochem 431, 1–10 (2017). https://doi.org/10.1007/s11010-017-2968-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-017-2968-2