Abstract
Osteoporosis, a systemic bone disorder, is prevalent in postmenopausal woman. Bone mesenchymal stem cells (BMSCs), precursors of osteogenic cells, may contribute to prevention or treatment of bone frustrate in osteoporosis. Recently, two studies suggested a role of calcitonin gene-related peptide (CGRP) in promoting osteogenesis of BMSCs under physiological conditions. However, the role of CGRP on BMSCs, which are derived from osteoporotic tissues, is unclear. Here, we investigated the role of CGRP on BMSCs isolated from female osteoporotic rats. Data showed that CGRP stimulated cell proliferation and inhibited cell apoptosis for short-term culture of BMSCs. Instead, CGRP induced BMSCs differentiation into the osteoblasts and promoted formation of calcified nodules after long-term culture. Moreover, CGRP gradually up-regulated expression levels of osteoporotic differentiation-related genes including alkaline phosphatase, Collagen type I, Bmp2, Osteonectin, and Runx2 during osteogenic differentiation. In conclusion, CGRP promoted proliferation and induced osteogenic differentiation and mineralization during female osteoporotic rat-derived BMSC differentiation. These findings support a potential role of CGRP on the prevention or treatment of osteoporotic fracture.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoporosis, a progressive bone disease, is characterized by a decrease of bone mass and bone density [1]. Osteoporosis usually leads to an increased risk of bone fracture because of reduction of the bone mineral density (BMD) and deteriorates of bone microarchitecture [2]. Primary osteoporosis can be classified as two different types [3]. The postmenopausal osteoporosis is primary type 1 osteoporosis commonly happened in female after menopause [3]. The senile osteoporosis is primary type 2 osteoporosis, which frequently occurs in elder people in both male and female [3]. In osteoporotic bone fracture, the osteoblast differentiation and osteogenesis potential are reduced, while the differentiation of adipocytes is increased [4]. These alterations may result in poor effects for therapy of bone fracture in osteoporotic patients. Bone mesenchymal stem cells (BMSCs) are the common precursors for both osteoblasts and adipocytes [5]. To improve efficiency of therapy of bone fracture in osteoporotic patients, it’s important to stimulate BMSC proliferation and differentiation into osteoblasts but not to adipocytes in osteoporotic patients.
It has been reported that metabolism, resorption, and performance of bone tissues are frequently regulated by nervous system [6]. First, the nervous fibers innervate bone tissues [7]. Second, nervous fibers secret neurotransmitters such as calcitonin gene-related peptide (CGRP), neuropeptide, and substance P to regulate the performance of bone tissues [8, 9]. Third, peptides secreted from nervous fibers are highly associated with the regulation of osteoclast and osteoblast activities [9, 10]. Among those peptides, CGRP is an attractive candidate, which may play a role in promoting bone healing in fracture patients with osteoporosis [11].
CGRP is a member of the calcitonin family of peptides distributed in both peripheral and central nervous [12, 13]. In bone tissues, CGRP-positive nerve fibers are abundantly distributed and play an essential role in the regulation of bone formation and bone resorption [14, 15]. The CGRP receptors are expressed on the surface membrane of BMSCs [16], suggesting a potential role of CGRP on modulating BMSCs. Recently, two studies implicated that exogenous CGRP promoted BMSC proliferation and osteogenic potential in physiological conditions [11, 17]. However, the role of CGRP in proliferation and differentiation of BMSCs derived from pathological environment such as osteoporosis is unclear.
In this study, we employed ovariectomy female rats as an osteoporotic model and isolated BMSCs from these osteoporotic rats. During ex vivo culture of BMSCs, we found that CGRP stimulated cell growth for short-term culture (with CGRP for 7 days). Rather, CGRP promoted BMSCs differentiation into the osteoblasts and formation of calcified nodules after long-term culture (with CGRP longer than 14 days). In addition, gene expression mapping suggests that CGRP gradually up-regulated expression of osteoporotic differentiation-related genes including Alkaline phosphatase (Alp), Collagen type I (Coll-I), Bmp2, Osteonectin, and Runx2 during differentiation. Protein levels of Osteonectin and RUNX2 were also consistently increased after CGRP stimulation during differentiation. These findings reveal the role of CGRP in BMSCs derived from osteoporotic tissues and might give an insight into the prevention or treatment of osteoporotic fracture.
Materials and methods
Animal model
This experimental study was approved by the Animal Research Ethical Committee in The Fourth Affiliated Hospital, Guangxi Medical University. In this study, 12 female Sprague Dawley rats aged 3 months, weighing between 200 and 250 g were used. The Animals were randomly assigned to control group or experimental group after measurement of bone density. Rats in the experimental group were subjected to ovariectomy (OVX). Rats in the control group were performed the same surgical procedure but only some adipose tissues were removed in these rats. Rats in both groups were grown for 6 months with a low calcium diet after surgery.
Measure of bone density
At the beginning and 6 months later, BMD of all rats in both groups was measured in vivo with a micro-CT. In all measurements, the animals were under ketamine anesthesia and placed in a supine position with a complete abduction of the hind limbs. The instrument was calibrated daily. The scan images were analyzed and BMD (in grams per square centimeter) (g/cm2) of the metaphyseal zone of proximal femurs were determined.
Isolation and culture of BMSCs
BMSCs were collected from femoral and tibial bone marrow of six OVX mice by inserting a 26-gage syringe at bone cavity. Cells were washed with 10 ml of DMEM (Gibco, #11320-033), and then centrifuging at 1,500 rpm for 5 min. BMSCs were re-suspended in 1 ml DMEM supplied with 10 % FBS (Gibco, #16000-044). Cells were plated with 6 × 105 cells/60-mm dish. Cultures were maintained in an incubator at 37 °C with 5 % CO2. Medium was replaced every 3 days and cells were passaged with 0.25 % trypsin (Gibco, #25200-072) when they reached to 80 % confluence.
Flow cytometry analysis
One million BMSCs were incubated with FITC/PE/APC-conjugated mouse anti-rat antibodies (anti- CD29, CD34, CD45, and anti- CD90 from BD bioscience) for 15 min at room temperature. Then, cells were washed twice with PBS, centrifuged at 1,000 rpm for 10 min and resuspended in 0.5 ml PBS. Cells with antibody binding were then analyzed by a detector (FC500, Beckman Coulter). Cells incubated with PBS were used as control. Triplicated experiments were performed.
Hematoxylin and eosin staining (H&E staining)
BMSCs at passage 3 (P3) were dissociated and plated into 6-well plate at density 5 × 104 cells/well for 24 h. After that, different doses of CGRP (Sigma, #C2806) or corresponding volume of control vehicle were added to cultures for 3 days following by standard H&E staining. The images were taken with microscopy (Olympus DP71X).
MTT assay
BMSCs at P3 were dissociated and plated into 96-well plate at density 2.5 × 104 cells/well for 24 h. Then, different doses of CGRP or corresponding volume of control vehicle were added to cultures for 7 days. Each day, MTT assay was performed according to MTT assay protocol (Life technologies, #V13154). Triplicated experiments were performed.
EdU and propidium iodide (PI) assay
BMSCs were treated with vehicle or CGRP (10−10 mol/L or 10−7mol/L) for 7 days. Then, 10 µM EdU (Ribobio, Cat. No. C10310) were added to cultured cells for 2 h. Cells were then washed with PBS, followed by 4 % paraformaldchyde fixation. Then, cells were incubated with 2 mg/ml glycine, washed with PBS twice. After permeabilization with PBS containing 0.5 % triton X-100 and extensive washing with PBS, cells were incubated with staining solution for 30 min. Next, cells were washed with PBS containing 0.5 % triton X-100 for three times, followed by 10 min incubation with Hoechst 33342. Images of the staining were captured with a fluorescent microscope (Olympus DP71X).
The apoptosis of cells during differentiation in vehicle or CGRP-treated cells was identified by PI staining using cell apoptosis PI detection kit (Cat. No. Loo311, Genscript). The staining was performed according to technical manual from Genscript. Images of the staining were taken with a fluorescent microscope (Olympus DP71X).
Calcified nodule staining
BMSCs at P3 were dissociated and plated into 6-well plate at density 5 × 104 cells/well for 24 h. After that, different doses of CGRP or corresponding volume of control vehicle were added to cultures for 14 or 21 days. Then, cells were fixed with 10 % formalin (Sigma, #HT501128) for 30 min and stained with Alizarin Red S(Sigma, #122777) for another 30 min. Cells were then washed with distilled water and mounted on slides. The images were taken with microscopy.
Alkaline phosphatase staining
Cells were plated into 24-well plate at density 5 × 104 cells/well for 24 h. Then, different doses of CGRP or corresponding volume of control vehicle were added to cultures for 14 days. Each day, alkaline phosphatase staining was performed according to protocol provided by Life technologies (#A14153). Triplicated experiments were performed.
Real-time PCR
BMSCs with or without CGRP cultured for 1, 3, 7, or 14 days were subjected to RNA extraction using TRIzol reagent (Invitrogen, #15596-066). Quantitative PCR was performed in accordance with previous report [18]. PCR primers were listed as follow:
Western blot analysis
Western blotting analysis was used to determine the protein levels of RUNX2 and Osteonectin. Protein was isolated from BMSCs with CGRP (10−10 mol/L or 10−7 mol/L) treatment for 3, 7, and 14 days or from untreated cells using a Protein Isolation Kit (Tiangen Biotech Co. Ltd). Then, 20 μgof each protein sample was subjected for SDS-PAGE gel electrophoresis. The following antibodies were used: anti-RUNX2 (1:1,000, Cat No: ab76956, abcam), mouse anti-human Osteonectin (1:1,000, Cat No: LS-C25800, LifeSpan BioSciences), and anti-GAPDH (1:5,000, ab9485, abcam). The protein bands were digitally scanned and analysed using Adobe Photoshop, version CS4 (Adobe, USA).
Statistical analysis
All experiments were repeated at least three times independently. Graphs were drawn using the SPSS®statistical software, version 19.0 (SPSS, Chicago, IL, USA). Data for MTT assay were expressed as means ± SD, and data for real-time PCR were represented as means ± SEM. Student’s t test was used for statistical analysis. The value of p less than 0.05 was considered as significance.
Results
Molecular characteristics of female osteoporotic rat-derived BMSCs
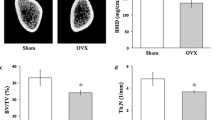
To evaluate the influence of CGRP on BMSCs that were derived from osteoporotic tissues, we generated the female osteoporotic rat model using OVX. The control and osteoporotic rats were maintained with a low calcium diet after surgery. Six months later, BMD of all rats in both groups was measured. The BMD of those adolescent rats was significantly increased from 0.11232 ± 0.0102 to 0.33259 ± 0.01001 (g/cm2) in control group, but not in OVX group (BMD: 0.182904 ± 0.00856 g/cm2) after surgery for 6 months, indicating osteoporotic problem to those OVX surgery rats. The result suggests that the osteoporotic model was established successfully according to previous reports [19, 20]. To obtain BMSCs in those osteoporotic rats, cells were collected from femoral and tibial bone marrow and cultured in DMEM with 10 % FBS. Then, flow cytometry was performed to validate the characteristics of BMSCs. The isolated cells presented molecular identities of BMSCs: with CD29 and CD90-positive (98.8 and 99.4 %, respectively) and CD34-negative (98.7 %) (Fig. 1). In addition, the isolated cells displayed spindle-shaped morphology (Fig. 2), which is a typical morphology of BMSCs.
CGRP promotes cell growth during culture
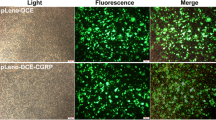
To measure the effects of CGRP on BMSCs during culture, H & E staining was performed 3 days after CGRP treatment. The data showed that the number of BMSCs with typical spindle-shaped morphology was increased in CGRP group as compared to control group (Fig. 2). This result implicate that CGRP may stimulate cell growth during BMSC culture ex vivo. To confirm that, MTT assay was used. With this assay, we measured the absorbance values (optical density, OD), which indicate number of viable cells, in control and CGRP-stimulated groups. Because the physiological concentration of circuitry CGRP is in range 10−10–10−8 mol/L [21–23] and studies widely used concentration of CGRP between 10−10 to 10−8 mol/L for BMSC treatment in vitro [11, 16], we chose concentration of CGRP in range 10−12–10−5 mol/L for our MTT assay. After one-day stimulation with CGRP, there was no significant difference between treated groups and control group. After 2 days’ treatment, CGRP-treated groups, except 10−12 mol/L group, significantly improved cell viability (p < 0.05, student’s t test, n = 3 independent cultures). After CGRP continuously treated for 7 days, CGRP-treated groups significantly promoted cell viability in a dose-dependent manner (Fig. 3a, p < 0.05, student’s t test, n = 3 independent cultures). Based on the physiological concentration of CGRP in vivo (10−10–10−8 mol/L), we chose concentration of CGRP in range 10−10–10−7 mol/L for our further experiments. To confirm the effects of CGRP, we performed EdU and PI staining. Our data showed that CGRP treatment gradually increased number of EdU-positive cells (Fig. 3b) and decreased number of PI-positive cells (Fig. 3c) in a dose-dependent manner. Taken together, CGRP promotes cell growth and inhibits cell apoptosis during culture ex vivo.
CGRP promotes cell proliferation and inhibits cell death during BMSC culture. a BMSCs without or with different doses of CGRP (10−12–10−5 mol/L) continuous stimulation for 7 days were collected for MTT assay. The OD value (Y axis) at different time points as indicated in X axis was used to generate growth curve of the cells. b Representative images of EdU (red) and corresponding Hoechst (blue) staining of cells treated with different concentrations of CGRP for 7 days as indicated. Scale bar = 75 μm for all images. c Representative images of propidium iodide (PI, red) and corresponding Hoechst (blue) staining of cells treated with different concentrations of CGRP for 7 days as indicated. Scale bar = 75 μm for all images. (Color figure online)
CGRP induces osteogenic differentiation
Next, we want to measure the effects of CGRP on BMSCs during long-term culture. After treatment with CGRP or vehicle for 14 days, cells were harvested for measurement of alkaline phosphatase (ALP) activity, which is an early marker of osteogenic differentiation. ALP staining showed heavy positive signals in cells with CGRP but not with vehicle treatment (Fig. 4). This result strongly suggests that CGRP induces differentiation of osteoblasts to generate ALP activities.
CGRP induces generation of ALP-positive osteoblasts. BMSCs after treatment with 10−8 mol/L CGRP (a and c) or vehicle (b and d) for 14 days, were harvested for ALP activity assay. Cells were visualized under microscopy with 100× object (CGRP group: c, control group: d). Scale bar = 75 μm in d (apply to c)
To further confirm the effects of CGRP on osteogenic terminal differentiation, alizarin red staining, which is used to indicate formation of bone nodules, was performed in cells cultured for 14 or 21 days ex vivo. Alizarin red staining showed that CGRP obviously promoted formation of calcium nodules as compared to vehicle group at 14 days (Fig. 5a–c). The Alizarin red staining became more apparent after stimulation with CGRP for 21 days (Fig. 5d–f). After CGRP-treated for 21 days, 90.5 % area were stained with Alizarin red, but only 10.1 and 8.5 % area were positive for Alizarin red staining in vehicle group and untreated group, respectively. CGRP treatment showed significant higher area coverage stained by Alizarin red as compared with vehicle or untreated group (p < 0.05, student’s t test, n = 4 independent cultures). There was no significant difference of Alizarin red staining coverage between vehicle and untreated groups (p < 0.05, student’s t test, n = 4 independent cultures).
Collectively, CGRP induced BMSC differentiation into osteoblasts and promoted osteogenic terminal differentiation.
Expression of osteogenic differentiation-related genes are increased after CGRP treatment
To validate the inductive role of CGRP during osteogenic differentiation, genes associated with osteoblast differentiation were examined. Cells stimulated with CGRP or vehicle for 1, 3, 7, and 14 days, were collected to generate mRNA. The real-time PCR results showed that CGRP significantly increased expression levels of genes in early stage of osteogenic differentiation (Alp and Coll-I), as well as expression levels of genes in late stage of osteogenic differentiation (Bmp2, osteonectin and Runx2) during differentiation for 14 days (Fig. 6). Notably, Coll-I, a gene expressed in early stage of osteogenic differentiation, was increased dramatically at first and then decreased after terminal differentiation (Fig. 6c). To further validate the real-time PCR results, Western blot analysis was employed to examine protein levels of RUNX2 and Osteonectin in control and CGRP-treated cells. The data showed that different dose of CGRP stimulation for 3, 7, or 14 days up-regulated protein levels of RUNX2 and Osteonectin as compared to untreated control (Fig. 7). Therefore, CGRP induced osteogenic differentiation-related gene expression during differentiation.
CGRP up-regulates expression levels of osteogenic differentiation-related genes. BMSCs without or with different concentration of CGRP (10−10 mol/L or 10−7 mol/L) stimulation for 1, 3, 7, or 14 days were harvested for gene expression analysis. The osteogenic differentiation-related genes including Alp (a), Bmp2 (b), Coll-I (c), Osteonectin (d), and Runx2 (e) were examined. *p < 0.05 for a–e
CGRP up-regulates protein expression levels of RUNX2 and Osteonectin. BMSCs without or with different concentrations of CGRP (10−10 mol/L or 10−7 mol/L) stimulation for 3, 7, or 14 days were harvested for protein expression analysis. The osteogenic differentiation-related genes including Runx2 and Osteonectin were examined. GAPDH was probed as loading control
Discussion
CGRP,a peptide with 37 amino acid residues, is mainly synthesized in small sensory neurons in the dorsal root ganglion [24]. CGRP-positive nerve fibers are abundantly distributed in bone tissue [7, 25]. CGRP generated from these fibers plays important roles in the regulation of growth, repair, and performance of bone tissues [14, 15, 26]. During healing of bone fracture, the number of CGRP-positive nerve fibers is increased in the periosteum as well as in new-formed bone [27]. CGRP may act on CGRP receptor expressing in BMSCs [16]. Recently, the roles of CGRP were implicated in BMSC cell line and BMSCs derived from healthy human [11, 17]; however, its function in BMSCs generated from osteoporotic tissues is unknown. In this study, we generated BMSCs from osteoporotic tissues in OVX rat model and confirmed their cell and molecular characteristics (Fig. 1 and Table 1). Interestingly, we noticed that there were two populations of CD90 and CD29-positive fractions based on FACS results (Fig. 1). This special feature may belong to BMSCs generated from osteoporotic tissues. However, it’s unclear what’s different between those two fractions. In this study, we also discovered the positive effects of CGRP in stimulation of cell growth and induction of osteogenic differentiation (Figs. 2, 3, 4, 5, 6, 7). These findings demonstrated the role of CGRP in BMSCs derived from osteoporosis. Upon these data, it’s interesting to know whether CGRP has a similar function on BMSCs and osteogenic differentiation in osteoporotic rats in future.
In our study, we found CGRP promoted cell growth at early stage (Figs. 2, 3) and induced osteoblast differentiation late on (Figs. 4, 5, 6, and 7). These results are consistent with findings in BMSC cell line and primary cultured BMSCs under physiological conditions [11, 17]. Together with previous reports, it’s reasonable to propose that CGRP has different roles in different stages of osteogenic differentiation. At first, CGRP stimulates cell proliferation to generate enough precursor cells. Then, CGRP induces cell differentiation into osteoblasts after long-term stimulation. However, the detailed mechanisms that mediate the roles of CGRP at different stages of osteogenic differentiation are unclear and should be explored in next study.
Although the detailed mechanisms are not explored in this study, we found some implications. We revealed that several osteogenic differentiation-related genes (Alp, Coll-I, Bmp2, Osteonectin, and Runx2) were responded to CGRP stimulation (Figs. 6, 7). Coll-I, a specific type of collagen synthesized by osteoblasts in bone tissues, plays an important role in osteoblastic differentiation of BMSCs [28]. CGRP may regulate expression of Coll-I to promote osteogenic differentiation. In addition to Coll-I, BMP signaling is another important player for osteogenic differentiation [29–31]. Consistent with previous report [32], our study suggests that CGRP increases expression levels of Bmp2 thereby potentially activating BMP2 signaling pathway to promote osteoblast differentiation. BMP signaling pathway can up-regulate Runx2, one of the key transcription factors involved in osteoblast differentiation [33]. Runx2 has a positive regulatory effect on bone formation by inhibiting adipogenic differentiation and promoting osteogenic differentiation of BMSCs [34, 35]. Thus, it’s possible that CGRP activates BMP2 pathway to up-regulate Runx2 and other bone-related genes during stimulation of osteogenesis. To validate this possibility, microarray approach will be employed to explore global gene expression changes in cells with and without CGRP stimulation and pathways including BMP pathway responding to CGRP stimulation will be analyzed.
References
Kanis JA, Melton LJ, Christiansen C, Johnston CC, Khaltaev N (1994) The diagnosis of osteoporosis. J Bone Miner Res 9:1137–1141. doi:10.1002/jbmr.5650090802
Kanis JA (2002) Diagnosis of osteoporosis and assessment of fracture risk. Lancet 359:1929–1936. doi:10.1016/S0140-6736(02)08761-5
Soen S (2014) Diagnostic criteria for primary osteoporosis: year 2012 revision. Clin Calcium 24:323–329. doi: CliCa1403323329
Pino AM, Rosen CJ, Rodriguez JP (2012) In osteoporosis, differentiation of mesenchymal stem cells (MSCs) improves bone marrow adipogenesis. Biol Res 45:279–287. doi:10.4067/S0716-97602012000300009
Takada I, Kouzmenko AP, Kato S (2009) Molecular switching of osteoblastogenesis versus adipogenesis: implications for targeted therapies. Expert Opin Ther Targets 13:593–603. doi:10.1517/14728220902915310
Togari A, Arai M (2008) Pharmacological topics of bone metabolism: the physiological function of the sympathetic nervous system in modulating bone resorption. J Pharmacol Sci 106:542–546
Serre CM, Farlay D, Delmas PD, Chenu C (1999) Evidence for a dense and intimate innervation of the bone tissue, including glutamate-containing fibers. Bone 25:623–629
Irie K, Hara-Irie F, Ozawa H, Yajima T (2002) Calcitonin gene-related peptide (CGRP)-containing nerve fibers in bone tissue and their involvement in bone remodeling. Microsc Res Tech 58:85–90. doi:10.1002/jemt.10122
Imai S, Matsusue Y (2002) Neuronal regulation of bone metabolism and anabolism: calcitonin gene-related peptide-, substance P-, and tyrosine hydroxylase-containing nerves and the bone. Microsc Res Tech 58:61–69. doi:10.1002/jemt.10119
Goto T, Nakao K, Gunjigake KK, Kido MA, Kobayashi S, Tanaka T (2007) Substance P stimulates late-stage rat osteoblastic bone formation through neurokinin-1 receptors. Neuropeptides 41:25–31. doi:10.1016/j.npep.2006.11.002
Xu G, Jiang D (2014) The role and mechanism of exogenous calcitonin gene-related peptide on mesenchymal stem cell proliferation and osteogenetic formation. Cell Biochem Biophys 69:369–378. doi:10.1007/s12013-013-9809-z
Ma W, Chabot JG, Powell KJ, Jhamandas K, Dickerson IM, Quirion R (2003) Localization and modulation of calcitonin gene-related peptide-receptor component protein-immunoreactive cells in the rat central and peripheral nervous systems. Neuroscience 120:677–694
Lennerz JK, Ruhle V, Ceppa EP, Neuhuber WL, Bunnett NW, Grady EF, Messlinger K (2008) Calcitonin receptor-like receptor (CLR), receptor activity-modifying protein 1 (RAMP1), and calcitonin gene-related peptide (CGRP) immunoreactivity in the rat trigeminovascular system: differences between peripheral and central CGRP receptor distribution. J Comp Neurol 507:1277–1299. doi:10.1002/cne.21607
Villa I, Dal Fiume C, Maestroni A, Rubinacci A, Ravasi F, Guidobono F (2003) Human osteoblast-like cell proliferation induced by calcitonin-related peptides involves PKC activity. Am J Physiol Endocrinol Metab 284:E627–E633. doi:10.1152/ajpendo.00307.2002
Lerner UH (2006) Deletions of genes encoding calcitonin/alpha-CGRP, amylin and calcitonin receptor have given new and unexpected insights into the function of calcitonin receptors and calcitonin receptor-like receptors in bone. J Musculoskelet Neuronal Interact 6:87–95
Wang L, Shi X, Zhao R, Halloran BP, Clark DJ, Jacobs CR, Kingery WS (2010) Calcitonin-gene-related peptide stimulates stromal cell osteogenic differentiation and inhibits RANKL induced NF-kappaB activation, osteoclastogenesis and bone resorption. Bone 46:1369–1379. doi:10.1016/j.bone.2009.11.029
Li J, Wang Y, Li Y, Sun J, Zhao G (2014) The effect of combined regulation of the expression of peroxisome proliferator-activated receptor-gamma and calcitonin gene-related peptide on alcohol-induced adipogenic differentiation of bone marrow mesenchymal stem cells. Mol Cell Biochem 392:39–48. doi:10.1007/s11010-014-2016-4
Xie Z, Chen Y, Li Z, Bai G, Zhu Y, Yan R, Tan F, Chen YG, Guillemot F, Li L, Jing N (2011) Smad6 promotes neuronal differentiation in the intermediate zone of the dorsal neural tube by inhibition of the Wnt/beta-catenin pathway. Proc Natl Acad Sci U S A 108:12119–12124. doi:10.1073/pnas.1100160108
Jee WS, Yao W (2001) Overview: animal models of osteopenia and osteoporosis. J Musculoskelet Neuronal Interact 1:193–207
Kalu DN (1991) The ovariectomized rat model of postmenopausal bone loss. Bone Miner 15:175–191
Stevenson JC, Macdonald DW, Warren RC, Booker MW, Whitehead MI (1986) Increased concentration of circulating calcitonin gene related peptide during normal human pregnancy. Br Med J (Clin Res Ed) 293:1329–1330
Wimalawansa SJ (1996) Calcitonin gene-related peptide and its receptors: molecular genetics, physiology, pathophysiology, and therapeutic potentials. Endocr Rev 17:533–585. doi:10.1210/edrv-17-5-533
Mikami N, Miyagi Y, Sueda K, Takatsuji M, Fukada S, Yamamoto H, Tsujikawa K (2013) Calcitonin gene-related peptide and cyclic adenosine 5′-monophosphate/protein kinase A pathway promote IL-9 production in Th9 differentiation process. J Immunol 190:4046–4055. doi:10.4049/jimmunol.1203102
van Rossum D, Hanisch UK, Quirion R (1997) Neuroanatomical localization, pharmacological characterization and functions of CGRP, related peptides and their receptors. Neurosci Biobehav Rev 21:649–678
Hara-Irie F, Amizuka N, Ozawa H (1996) Immunohistochemical and ultrastructural localization of CGRP-positive nerve fibers at the epiphyseal trabecules facing the growth plate of rat femurs. Bone 18:29–39
Rosenfeld MG, Mermod JJ, Amara SG, Swanson LW, Sawchenko PE, Rivier J, Vale WW, Evans RM (1983) Production of a novel neuropeptide encoded by the calcitonin gene via tissue-specific RNA processing. Nature 304:129–135
Wang XY, Guo X, Cheng JC, Mi YL, Lai PY (2010) Involvement of calcitonin gene-related peptide innervation in the promoting effect of low-intensity pulsed ultrasound on spinal fusion without decortication. Spine (Phila Pa 1976) 35:E1539–E1545. doi:10.1097/BRS.0b013e3181cde89d
Mizuno M, Fujisawa R, Kuboki Y (2000) Type I collagen-induced osteoblastic differentiation of bone-marrow cells mediated by collagen-alpha2beta1 integrin interaction. J Cell Physiol 184:207–213. doi:10.1002/1097-4652(200008)184:2<207:AID-JCP8>3.0.CO;2-U
Gruber R, Mayer C, Schulz W, Graninger W, Peterlik M, Watzek G, Luyten FP, Erlacher L (2000) Stimulatory effects of cartilage-derived morphogenetic proteins 1 and 2 on osteogenic differentiation of bone marrow stromal cells. Cytokine 12:1630–1638. doi:10.1006/cyto.2000.0760
Huang W, Carlsen B, Wulur I, Rudkin G, Ishida K, Wu B, Yamaguchi DT, Miller TA (2004) BMP-2 exerts differential effects on differentiation of rabbit bone marrow stromal cells grown in two-dimensional and three-dimensional systems and is required for in vitro bone formation in a PLGA scaffold. Exp Cell Res 299:325–334. doi:10.1016/j.yexcr.2004.04.051
Wang L, Huang Y, Pan K, Jiang X, Liu C (2010) Osteogenic responses to different concentrations/ratios of BMP-2 and bFGF in bone formation. Ann Biomed Eng 38:77–87. doi:10.1007/s10439-009-9841-8
Tian G, Zhang G, Tan YH (2013) Calcitonin gene-related peptide stimulates BMP-2 expression and the differentiation of human osteoblast-like cells in vitro. Acta Pharmacol Sin 34:1467–1474. doi:10.1038/aps.2013.41
Rosen V (2009) BMP2 signaling in bone development and repair. Cytokine Growth Factor Rev 20:475–480. doi:10.1016/j.cytogfr.2009.10.018
James AW (2013) Review of signaling pathways governing MSC osteogenic and adipogenic differentiation. Scientifica (Cairo) 2013:684736. doi:10.1155/2013/684736
Shakibaei M, Shayan P, Busch F, Aldinger C, Buhrmann C, Lueders C, Mobasheri A (2012) Resveratrol mediated modulation of Sirt-1/Runx2 promotes osteogenic differentiation of mesenchymal stem cells: potential role of Runx2 deacetylation. PLoS ONE 7:e35712. doi:10.1371/journal.pone.0035712
Acknowledgments
We thank all other members in the laboratory for their technical supports and helpful discussions. This study is supported by National Natural Science Foundation of China (No: 81260273).
Conflict of interest
The authors declare that they have no conflict of interests.
Author information
Authors and Affiliations
Corresponding author
Additional information
Wei Liang and Xianglong Zhuo contributed equally to this study.
Rights and permissions
About this article
Cite this article
Liang, W., Zhuo, X., Tang, Z. et al. Calcitonin gene-related peptide stimulates proliferation and osteogenic differentiation of osteoporotic rat-derived bone mesenchymal stem cells. Mol Cell Biochem 402, 101–110 (2015). https://doi.org/10.1007/s11010-014-2318-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s11010-014-2318-6