Abstract
The purpose of our study was to identify primary care providers’ (PCPs’) practices in promoting childhood vaccination and their perceptions regarding barriers to vaccination in a primarily rural state. In January-May 2022, we conducted a mail and online survey of PCPs across Montana (n = 829). The survey included modules on routine immunizations in children 0–2 years old and COVID-19 vaccination in children 5–17 years old. The survey response rate was 36% (298/829). We categorized PCPs as working in rural (n = 218) or urban areas (n = 80), based on Rural-Urban Commuting Area codes. We then compared responses between rural and urban PCPs using chi-square tests. Urban PCPs (90–94%, depending on vaccine) stocked routinely recommended vaccines more frequently than rural PCPs (71–84%), but stocked the COVID-19 vaccine less often than rural PCPs (44% vs. 71%, respectively, p < 0.001). A higher percentage of rural providers reported parental beliefs that vaccine-preventable diseases are not severe enough to warrant vaccination (48% vs. 31%, p = 0.01) and concerns that vaccination will weaken their child’s immune system (29% vs. 6%, p < 0.001). More rural (74%) compared to urban (59%) PCPs identified a social media campaign from local health departments promoting early childhood vaccinations as an effective strategy to increase childhood vaccination rates (p = 0.01). We identified key differences in some childhood vaccination practices and barriers between rural and urban PCPs. Interventions to increase rural vaccination rates could include increasing the number of providers stocking all recommended vaccines, identifying strategies to address parents’ concerns regarding vaccine necessity, and collaborations with public health departments.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Background
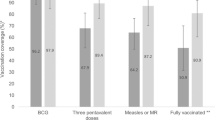
Routine childhood vaccinations have prevented millions of serious illnesses and thousands of premature deaths [1,2,3,4]. Data collected by the U.S. Centers for Disease Control and Prevention show that children living outside of a metropolitan statistical area (MSA) have lower vaccination rates than children living in an MSA (e.g., influenza, 48% vs. 62%), and non-MSA children have higher rates of not receiving any vaccines (1.4% vs. 0.9%) [5]. Additionally, COVID-19 vaccination coverage is lower in rural areas for children 5–11 years old (rural: 15%, urban: 31%) and 12–17 years old (rural: 39%, urban: 65%) [6].
One reason for low uptake of childhood vaccinations in rural communities is parental vaccine hesitancy, including concerns about the safety of vaccines routinely recommended to children, the number of vaccines administered at once, the necessity of vaccines, and potential side effects [7,8,9,10]. Furthermore, although research has been limited regarding COVID-19 vaccine-related concerns of parents residing in rural areas, recent non-rural focused studies reported that parents are hesitant to vaccinate their children against COVID-19 due to concerns about vaccine side effects and the safety of the COVID-19 vaccine [11, 12]. However, more research in rural communities is needed. While parental hesitancy is a driver of childhood undervaccination in rural and urban America, structural barriers to immunization services, such as transportation barriers [13], access to fewer pediatricians [14], and medical providers not stocking all recommended vaccines [15], are more prominent in rural areas.
There is a range of evidence-based strategies to address hesitancy and non-hesitancy barriers to routine childhood vaccinations. Primary care providers (PCPs) have consistently been shown to be the strongest influencers in parents’ vaccination decision-making [16,17,18,19,20], even among people who are hesitant about vaccines [17]. Additionally, clinic-level strategies like reminder-recall processes that inform parents that their children are due or overdue for vaccinations [21] and automated prompts at the point of care that guide providers in which vaccines to recommend, are associated with higher vaccination rates [16, 21, 22]. While there are multiple evidence-based strategies to increase vaccination coverage [16], there is a lack of data on how frequently such strategies are used, particularly in communities outside of urban areas.
We surveyed PCPs across Montana, a primarily rural state [23]. Rates of routine vaccinations in Montana in early childhood (0–2 years old) lag behind the national average, and 5- to 17-year-olds in Montana are about 15% points behind national levels for COVID-19 vaccination [5, 24,25,26]. Our objectives were to identify Montana PCPs’ practices in promoting routine and COVID-19 childhood vaccinations and their perceptions of vaccination barriers, and to compare the prevalence of practices and perceptions between rural and urban providers.
Methods
Participants
We sent a survey to all eligible PCPs in Montana (n = 829). PCPs were eligible for the survey if they were physicians, advanced practice registered nurses (APRNs), or physician associates (PAs) who administered childhood (less than 18 years old) vaccinations or referred children for immunization services and primarily worked in Montana with a specialty in family medicine or pediatrics. A complete list of Montana PCPs was identified using Wyoming, Idaho, Montana Health Workforce Data (WIM Tracking) [27]. This study was approved by the University of Montana Institutional Review Board under the exempt category of review.
Survey Design
We surveyed PCPs in January-May 2022 when COVID-19 vaccines were available for children 5–17 years old, but not for younger age groups. The survey included two distinct modules: routine childhood immunizations in children 0–2 years old and COVID-19 vaccination for children 5–17 years old. We adapted survey questions from previous provider and parent surveys [28,29,30,31,32,33,34]. Due to limited published studies of surveys specific to COVID-19 vaccination for children at the time of survey development, some questions were developed by the research team with assistance from a PCP specializing in family medicine. The PCP provided feedback about the design and flow of the survey and the validity of the survey questions. Additionally, 4 PCPs (3 Physicians, 1 PA) gave survey feedback through cognitive interviews, which were used to test and modify the survey tool [35]. Providers received a $30 Amazon gift card for participation in cognitive interviews.
The final survey tool had 21 content questions and four demographic questions. Comment boxes were available throughout the survey for participants to provide additional open-ended feedback. The survey included a cover page with information about the study and information that participation was voluntary. Participants could skip survey questions they did not wish to answer.
Survey Administration
We sent four survey mailings from January-May 2022, 4–6 weeks apart. Providers were not offered an incentive to participate in the survey. Each survey mailing contained a paper survey and a cover letter with information about the survey. All potential participants could either complete the survey via hard copy and return it by mail in a pre-paid envelope or take the survey online. The last survey mailing (mailing #4) contained a hand-addressed, larger (10” x 13”), and different-colored envelope than was previously used [36]. Study data were collected and managed using REDCap (Research Electronic Data Capture) [37, 38]. REDCap is a secure, web-based software platform that supports data capture for research studies. Each provider was given a unique code linked to their online survey response to (1) avoid replicated data if one provider completed a survey online and by hardcopy, and (2) so providers that participated were excluded from future survey mailings. For a subset of providers, the WIM Tracking provider dataset listed an email address for the provider (n = 31) or the practice manager (n = 425). We sent email invitations to these providers directly to complete the survey or to the practice manager to forward to the provider. The email invitations were sent about two weeks after the most recent survey mailout. Data collection was continuous from the first survey mailing until the online survey was inactivated in June 2022. The last accepted paper survey was received in July 2022.
Rurality
Rurality was categorized using 2010 Rural-Urban Commuting Area (RUCA) codes. RUCA codes classify U.S. census tracts by accounting for population, commuting patterns, and amount of urbanization [39, 40]. We matched RUCA codes with PCP address information from WIM Tracking at the census tract level using 2020 Census Bureau tract information for Montana [41]. To account for small sample sizes, we created an urban and a rural category from RUCA codes based on recommendations from previous research [42,43,44]. More details on the dichotomization of RUCA codes are provided in Table 1.
Analysis
Online surveys were completed in REDCap, and study personnel entered paper survey data into REDCap. Once an initial group of paper surveys was received (n = 25), two study team members developed data entry rules to ensure consistency with paper survey data entry and online surveys. We pooled paper and online survey entries for analyses [45, 46].
We completed descriptive analyses of responses to survey questions. For Likert scale responses, we combined response options: (1) ‘Barrier’ (major barrier + somewhat of a barrier), ‘Neutral or Not a barrier’ (neutral + not much of a barrier + definitely not a barrier), (2) ‘Factors that contributed a lot or somewhat to parental concerns’ (contributed a lot + contributed somewhat), ‘Factors that contributed a little or did not contribute to parental concerns’ (contributed a little + contributed not at all), (3) ‘Agreed’ (somewhat agreed + strongly agreed), ‘Neutral or disagreed’ (neutral + somewhat disagree + strongly disagree’), and (4) ‘Effective strategies’ (very effective + somewhat effective), ‘Not considered effective’ (neutral + somewhat ineffective + not at all effective). We used Chi-square tests of independence and Fisher’s exact test to compare characteristics of participants versus nonparticipants, and survey responses from PCPs practicing in urban versus rural areas. We conducted all analyses using SAS (version 9.4, The SAS Institute, Cary, NC), and figures were produced in R [47, 48].
Results
Provider Demographics
Survey Participants
Out of 829 eligible PCPs, 298 participated in the survey (36% response rate). Overall, 54.2% of eligible survey participants were physicians, 26.2% were APRNs, and 19.7% were PAs. Physicians and APRNs were more likely to participate in the survey than PAs (p = 0.006). About 81.5% of participating PCPs specialized in family medicine, and 18.5% specialized in pediatrics. PCPs with a pediatric specialty were more likely to participate than those specializing in family medicine (p < 0.001). Participants were predominately White (87.6%) and identified as female (67.1%). Age of participants included 30–40 years old (31.7%), 41–50 years old (25.9%), or 51–60 years old (22.5%). Experience as a provider varied from less than 5 years (20.9%), 5–10 years (17.9%), 11–20 years (26.9%), 21–30 years (20.5%), or more than 30 years (13.8%). There were no significant differences in participants and nonparticipants by urban/rural location (p = 0.05; Table 2). While 73.2% of participants worked in rural areas, 26.9% worked in urban areas. Providers represented 45 out of 56 counties in Montana. Participants reported working at a hospital or health-system owned private clinics (n = 85), private independent clinics (n = 72), federally qualified health centers (n = 59), clinics within critical access hospitals (n = 47), rural health clinics (n = 44), Indian Health Service-operated centers/Tribal health facilities/urban Indian health care facilities (n = 11), community health centers (n = 8), or other (ex. school-based health centers) (n = 5) (multiple settings could be selected).
Participant and Clinic Characteristics by RUCA Categorization
We did not find differences in provider roles when comparing urban participants (67.5% physicians, 22.5% APRNs, 10.0% PAs) to rural participants (54.1% physicians, 30.7% APRNs, 15.1% PAs, p = 0.11). Urban participants had a higher percentage of providers specializing in pediatrics (26.3%) than rural areas (15.6%, p = 0.04). Among all participants, 96.3% indicated their facility offered immunizations on site, 84.0% participated in the Vaccines for Children (VFC) program, and 96.6% reported vaccinations to the state’s centralized immunization information system (ImMTrax); there were no significant differences in these clinic characteristics by RUCA group (p-value range 0.30–0.97, Table 3).
Routine Early Childhood Vaccination (0–2 Years old)
The majority of PCPs (93.1%) agreed that giving all routine early childhood vaccines in the primary series at the recommended times was important, with no significant differences between rural and urban providers (p = 0.51). Overall, the majority of PCPs reported regularly stocking early childhood vaccines; however, we found that a higher proportion of urban providers indicated they stocked hepatitis A (91.3% vs. 81.2%, p = 0.04), poliovirus (88.8% vs. 76.6%, p = 0.02), and rotavirus (87.5% vs. 76.2%, p = 0.03) vaccines compared to rural providers (Table 3).
While 34.9% of providers reported using a process to identify and contact parents of children who are due or overdue for routine vaccinations (i.e., reminder/recall), 43.2% indicated their facility did not have a reminder/recall system, and 21.9% were unsure. No difference in the use of reminder/recall was found between rural and urban providers (p = 0.43). Among providers who did report having a reminder/recall process, 2.9% reported that reminder/recall occurred on a weekly basis, 14.7% reported that reminder/recall was conducted on a monthly basis, 33.3% reported that reminder/recall was conducted only when there was staff capacity to do so, and 38.2% were unsure how often reminder/recall was conducted.
The majority of providers reported that barriers to on-time vaccinations for children 0–2 years old included parents choosing to delay or refuse some or all vaccines for their children (84.5%) or parents not knowing when to bring their child in for routine well-care (50.0%, Fig. 1, Appendix Table 1). There were no significant differences in provider-reported barriers to vaccinations between participants working in urban or rural areas (p-value range: 0.15–0.98).
Most providers reported that based on their experiences, concerns that children receive too many vaccines (62.7%), concerns that their child will suffer long-term complications from vaccines (53.8%), and general worries about vaccines without a specific concern (52.8%) contributed a lot or somewhat to parents’ questions and concerns about vaccines. However, a higher percentage of rural providers reported that parental beliefs that vaccine-preventable diseases are not severe enough to warrant vaccination (47.8% vs. 31.0%, p = 0.01) and concerns that vaccination will weaken their child’s immune system (28.6% vs. 5.9%, p < 0.001) contributed a lot or somewhat to parental vaccine concerns. There were no other significant differences between rural and urban PCPs (p-value range = 0.12–0.91, Fig. 2, Appendix Table 2).
Regarding their perceptions of strategies to increase routine childhood vaccination rates, most PCPs supported having the local public health department use state immunization information systems data (ImMTrax) to contact parents when their child is due or overdue for immunizations (81.0%). Additionally, PCPs indicated that training non-PCP clinic staff (83.9%) and PCPs (73.1%) in strategies for effective vaccine conversations, increasing the capacity to deliver vaccinations at alternative immunization sites (63.5%), or mailing/emailing educational vaccine materials to parents before their child’s scheduled appointment (64.1%) would be very or somewhat effective strategies to increase routine childhood vaccination. The largest percentage (88.1%) of PCPs agreed that providing expecting parents with information about early childhood vaccines as part of prenatal care would be a very or somewhat effective strategy. Fewer urban (58.7%) compared to rural (73.9%) PCPs identified a social media campaign from state or local health departments promoting early childhood vaccinations as a potentially very or somewhat effective strategy to increase childhood vaccination rates (p = 0.01). No other differences between perceptions of strategy effectiveness were found between rural and urban PCPs (p-value range: 0.08–0.87, Fig. 3, Appendix Table 3).
Provider-reported barriers to early childhood vaccination (0–2 years old). aAll questions were voluntary. Sample size and percentages represent the providers that answered the question, therefore, sample sizes provided for each question may not add up to the total sample size of providers. bThe figure provided shows percentages for all response options. However, we completed analyses using the categories barrier and Neutral or not a barrier. ‘Barrier’ represents percentages from major barrier + somewhat of a barrier and ‘Neutral or not a barrier’ represents percentages from neutral + not much of a barrier + definitely not a barrier.
Abbreviations: Electronic health record (EHR).
Provider-reported factors that contribute to parental concerns for early childhood vaccination (0–2 years old). aAll questions were voluntary. Sample size and percentages represent the providers that answered the question, therefore, sample sizes provided for each question may not add up to the total sample size of providers. bThe figure provided shows percentages for all response options. However, analyses were completed using two categories, contributes a lot or somewhat and contributes a little or not at all. ‘Contributes a lot or somewhat’ indicates that the factor contributed either a lot or somewhat to parental concerns and ‘Contributes a little or not at all’ represents concerns that contributed a little or not at all to parents’ concerns about early childhood vaccines. *Significant finding, significance level p < 0.05.
Abbreviations: vaccine-preventable diseases (VPDs).
Providers’ opinions on the effectiveness of strategies for increasing early childhood vaccination rates. aAll questions were voluntary. Sample size and percentages represent the providers that answered the question, therefore, sample sizes provided for each question may not add up to the total sample size of providers. bThe figure provided shows percentages for all response options. However, analyses were completed using the categories effective and not considered effective. ‘Effective’ indicates PCPs that reported the strategy would be either very effective or somewhat effective. ‘Not considered effective’ represented PCPs that reported strategies would be somewhat ineffective, not at all effective, or they were neutral. *Significant finding, significance level p < 0.05.
Child and Adolescent COVID-19 Vaccination (5–17 Years old)
The majority of PCPs reported that they stocked COVID-19 vaccinations (64.1%). A higher proportion of rural PCPs (71.3%) reported stocking COVID-19 vaccines than urban providers (44.3%, p < 0.01). Of providers that reported not stocking COVID-19 vaccines, 86.4% did not plan to stock the vaccine in the future, and 9.7% were unsure if they would stock the vaccine. Of the providers that indicated they are not planning to stock the COVID-19 vaccine, their reasons were concerns about vaccine waste if all doses from the multi-dose vials were not used (60.7%), lack of appropriate cold storage for the vaccine (48.3%), not enough anticipated demand to stock the vaccine (29.2%), not enough staff to manage the vaccine inventory (28.1%), or not enough staff to administer vaccines (23.6%). In the open-feedback option, 15 PCPs wrote that they were not planning to stock the COVID-19 vaccine because COVID-19 vaccines were readily available at public health departments or pharmacies in their community.
Although 84.5% of providers somewhat or strongly agreed that their facility does a good job of routinely checking patients’ COVID-19 vaccine status if the patient is age-eligible, only 26.0% somewhat or strongly agreed that their clinic has been proactive in reaching out to parents to encourage them to get their child vaccinated against COVID-19. We did not find significant differences in these survey responses between rural and urban providers (p-value range: 0.21–0.98).
The most frequent provider-reported barriers to COVID-19 vaccination for children 5–17 years old were parents’ or patients’ concerns; specifically, their concerns that the COVID-19 vaccines were rapidly developed and authorized (96.2%), fears that getting the COVID-19 vaccine will lead to long-term health issues (92.3%), beliefs that the COVID-19 vaccine is being promoted for commercial gains of pharmaceutical companies (77.7%), or fears that getting the COVID-19 vaccine will cause short-term side effects/allergic reactions (76.3%). We did not find significant differences in reported barriers based on the urban/rural designation of the provider (p-value range: 0.09–0.97, Fig. 4, Appendix Table 4).
Provider-reported barriers to COVID-19 vaccination for children and adolescents 5–17 years old. aAll questions were voluntary. Sample size and percentages represent the providers that answered the question, therefore, sample sizes provided for each question may not add up to the total sample size of providers. bThe figure provided shows percentages for all response options. However, we completed analyses using the categories barrier and neutral or not a barrier. ‘Barrier’ represents percentages from major barrier + somewhat of a barrier and ‘Neutral or not a barrier’ represents percentages from neutral + not much of a barrier + definitely not a barrier.
Discussion
Our survey investigated Montana primary care providers’ experiences with and perceptions of routine early childhood vaccines for children 0–2 years old and COVID-19 vaccines for children and adolescents 5–17 years old. Participants overwhelmingly supported vaccinations for children in this large and primarily rural state, where most PCPs practice outside of urban areas. Our analysis of responses by whether providers worked in an urban or rural RUCA designation illuminated important differences in PCPs’ perceptions of parental concerns and immunization practices.
In Montana, fewer PCPs in rural areas reported stocking some routine childhood vaccines. These findings align with prior research that found providers practicing outside urban areas are less likely to stock all recommended vaccines [9, 15]. Similarly, prior studies have also reported that children and adolescents living in rural communities are more likely to be referred to local public health departments for vaccination services [9, 15] and are more likely to receive vaccinations at a public facility than urban or suburban children [15, 49,50,51]. However, because referring patients outside of primary care for immunization services is associated with lower vaccination coverage [15], efforts to increase childhood vaccination should include increasing the percentage of primary care clinics that stock all recommended childhood vaccines. Interestingly, our survey findings revealed an opposite trend for COVID-19 vaccination, with more rural PCPs reporting stocking COVID-19 vaccines, likely due to the availability of commercial pharmacies providing the vaccination in urban areas. Therefore, recommendations to public health practitioners should include stocking more COVID-19 vaccines in urban primary care facilities. However, it is also essential that rural PCPs continue stocking the COVID-19 vaccine in-house to ensure easy access to COVID-19 vaccination.
We also found significant differences by rurality in PCPs’ perceptions of contributing factors to parental concerns about early childhood vaccinations. More rural PCPs reported parental concerns that vaccine-preventable diseases (VPDs) are not severe enough to warrant vaccination. Individuals’ perceptions of greater disease severity are associated with increased intent to vaccinate and increased receipt of vaccinations [52,53,54]. Currently, there is limited evidence on how to effectively promote vaccination uptake among parents who have lower perceptions of disease severity. One randomized controlled trial found that providing vaccine-hesitant parents with details on the severity of VPDs did not improve intent to vaccinate [55]. Given our findings of higher provider-reported prevalence of parents questioning the necessity of vaccinations in rural areas, additional studies are needed to address this parental concern effectively. Misperceptions about lower disease risk in rural areas may be one reason for decreased parental concerns regarding disease severity. However, VPD outbreaks cluster geographically [56,57,58,59] in both urban [58] and rural environments [57, 60]. A recent study in Florida found that even though more pertussis cases were identified in urban areas, the risk of pertussis was higher in rural counties compared to urban counties. Indeed, given the ample evidence that lower vaccination coverage leads to higher VPD risk, it was suggested that rural counties in Florida had higher disease risk due to lower vaccination coverage [58]. Misperceptions that rurality is associated with less disease risk should be addressed in targeted community interventions.
Compared with urban providers, more rural providers agreed that a social media campaign from state or local health departments would be an effective strategy to promote childhood vaccinations. This finding was likely associated with the high reliance on public health departments in rural areas. Studies have demonstrated that rural children were more likely to be vaccinated at public facilities [49, 61] and county health departments or community health centers [15], compared to urban and suburban children. In Montana, over 12% of children born in 2015–2017 only received vaccinations in public clinics during their first two years of life [62]. Additionally, an earlier study in Colorado found that rural PCPs demonstrated a stronger preference for health department involvement in vaccination reminders than urban providers [28], and rural parents were more supportive than urban parents in receiving reminders to vaccinate their child from the local health department [32]. In our survey, a majority of urban (82%) and rural (78%) providers thought that having public health departments use a centralized immunization information system to conduct reminder-recall would be a somewhat or very effective strategy for increasing vaccination rates. Moving forward, targeted interventions for increasing vaccination rates in rural Montana should consider expanding the involvement of public facilities in promoting vaccination.
Our study had some limitations. Compared to the distribution of specialties in Montana, PCPs with pediatric specialties were more likely to participate in the survey than PCPs with family medicine specialties. Because children are just one portion of family medicine providers’ patient population, some family medicine PCPs may have been less inclined to take the survey as compared to pediatric PCPs. Additionally, there is evidence that providers with a pediatric specialty are more likely to provide all early childhood vaccinations [15]. Therefore, our results may overestimate the prevalence of current strategies used in Montana clinics to increase vaccine uptake. Finally, participants only represented Montana PCPs, so our findings may not represent other non-urban areas across the U.S. Rural communities are heterogenous and, therefore, experience unique barriers to childhood vaccination. However, state and local investigations of immunization service delivery are critical to establishing effective community-level intervention strategies that increase vaccination uptake.
Conclusion
The findings from our statewide survey with PCPs that predominantly serve a rural population revealed promising avenues for future initiatives to increase childhood vaccination rates. The focus of future interventions for PCPs in rural areas should include increasing the number of PCPs that stock all recommended childhood vaccines, targeting parent-provider vaccine conversations to include discussions about parental perceptions of disease severity and the effect of vaccines on the immune system, and collaborations with local health departments to promote childhood vaccination.
Data Availability
The data that support the findings of this study are available from the corresponding author upon request.
Code Availability
The code that supports the findings of this study is available from the corresponding author upon request.
References
Orenstein, W. A. (2006). The role of measles elimination in development of a national immunization program. Pediatr Infectious Disease Journal, 25, 1093–1101. https://doi.org/10.1097/01.inf.0000246840.13477.28.
Ozawa, S., Portnoy, A., Getaneh, H., Clark, S., Knoll, M., Bishai, D., Yang, H. K., & Patwardhan, P. D. (2016). Modeling the economic burden of adult vaccine-preventable diseases in the United States. Health Affairs (Millwood), 35(11), 2124–2132. https://doi.org/10.1377/hlthaff.2016.0462.
Roush, S. W., Murphy, T. V., & Vaccine-Preventable Disease Table Working Group. (2007). Historical comparisons of morbidity and mortality for vaccine-preventable diseases in the United States. Journal Of The American Medical Association, 298(18), 2155–2163. https://doi.org/10.1001/jama.298.18.2155.
Whitney, C. G., Zhou, F., Singleton, J., & Schuchat, A. (2014). Benefits from immunization during the vaccines for children program era - United States, 1994–2013. MMWR Morbidity and Mortality Weekly Report, 63(16), 352–355.
Hill, H. A., Yankey, D., Elam-Evans, L. D., Singleton, J. A., & Sterrett, N. (2021). Vaccination coverage by age 24 months among children born in 2017 and 2018 - National Immunization Survey-Child, United States, 2018–2020. MMWR Morbidity and Mortality Weekly Report, 70(41), 1435–1440. https://doi.org/10.15585/mmwr.mm7041a1.
Saelee, R., Zell, E., Murthy, B. P., Castro-Roman, P., Fast, H., Meng, L., Shaw, L., Gibbs-Scharf, L., Chorba, T., Harris, L. Q., & Murthy, N. (2022). Disparities in COVID-19 vaccination coverage between urban and rural Counties — United States, December 14, 2020–January 31, 2022. MMWR Morbidity and Mortality Weekly Report, 71(9), 335–340. https://doi.org/10.15585/mmwr.mm7109a2.
Ames, H. M., Glenton, C., & Lewin, S. (2017). Parents’ and informal caregivers’ views and experiences of communication about routine childhood vaccination: A synthesis of qualitative evidence. Cochrane Database of Systematic Reviews, 2, CD011787. https://doi.org/10.1002/14651858.CD011787.pub2Ames
Mical, R., Martin-Velez, J., Blackstone, T., & Derouin, A. (2021). Vaccine hesitancy in rural pediatric primary care. Journal of Pediatric Health Care, 35(1), 16–22. https://doi.org/10.1016/j.pedhc.2020.07.003.
Deutchman, M., Brayden, R., Siegel, C. D., Beaty, B., & Crane, L. (2000). Childhood immunization in rural family and general practices: Current practices, perceived barriers and strategies for improvement. Ambulatory Child Health, 6(3), 181–189. https://doi.org/10.1046/j.1467-0658.2000.00087.x2000.
Kettunen, C., Nemecek, J., & Wenger, O. (2017). Evaluation of low immunization coverage among the amish population in rural Ohio. American Journal of Infection Control, 45(6), 630–634. https://doi.org/10.1016/j.ajic.2017.01.032.
Ruggiero, K. M., Wong, J., Sweeney, C. F., Avola, A., Auger, A., Macaluso, M., & Reidy, P. (2021). Parents’ intentions to vaccinate their children against COVID-19. Journal of Pediatric Health Care, 35(5), 509–517. https://doi.org/10.1016/j.pedhc.2021.04.005.
Szilagyi, P. G., Shah, M. D., Delgado, J. R., Thomas, K., Vizueta, N., Cui, Y., Vangala, S., Shetgiri, R., & Kapteyn, A. (2021). Parents’ intentions and perceptions about COVID-19 vaccination for their children: Results from a national survey. Pediatrics, 148(4), e2021052335. https://doi.org/10.1542/peds.2021-052335.
Hicks, P., Tarr, G. A., & Hicks, X. P. (2007). Reminder cards and immunization rates among Latinos and the rural poor in northeast Colorado. Journal of the American Board of Family Medicine, 20(6), 581–586. https://doi.org/10.3122/jabfm.2007.06.060071.
Weigel, P. A., Ullrich, F., Shane, D. M., & Mueller, K. J. (2016). Variation in primary care service patterns by rural-urban location. Journal of Rural Health, 32(2), 196–203. https://doi.org/10.1111/jrh.12146.
Fagnan, L. J., Shipman, S. A., Gaudino, J. A., Mahler, J., Sussman, A. L., & Holub, J. (2011). To give or not to give: Approaches to early childhood immunization delivery in Oregon rural primary care practices. Journal of Rural Health, 27(4), 385–393. https://doi.org/10.1111/j.1748-0361.2010.00356.x.
Cataldi, J. R., Kerns, M. E., & O’Leary, S. T. (2020). Evidence-based strategies to increase vaccination uptake: A review. Current Opinnion in Pediatrics, 32(1), 151–159. https://doi.org/10.1097/MOP.0000000000000843.
Chung, Y., Schamel, J., Fisher, A., & Frew, P. M. (2017). Influences on immunization decision-making among U.S. parents of young children. Maternal and Child Health Journal, 21(12), 2178–2187. https://doi.org/10.1007/s10995-017-2336-6.
Edwards, K. M., Hackell, J. M., & Committee on Infectious Disease, The Committee on Practice and Ambulatory Medicine. (2016). Countering vaccine hesitancy. Pediatrics, 138(3), e20162146. https://doi.org/10.1542/peds.2016-2146.
Kennedy, A., Basket, M., & Sheedy, K. (2011). Vaccine attitudes, concerns, and information sources reported by parents of young children: Results from the 2009 HealthStyles survey. Pediatrics, 127(Supplement 1), S92–S99. https://doi.org/10.1542/peds.2010-1722n.
Smith, P. J., Kennedy, A. M., Wooten, K., Gust, D. A., & Pickering, L. K. (2006). Association between health care providers’ influence on parents who have concerns about vaccine safety and vaccination coverage. Pediatrics, 118(5), e1287–e1292. https://doi.org/10.1542/peds.2006-0923.
Jacobson Vann, J. C., Jacobson, R. M., Coyne-Beasley, T., Asafu-Adjei, J. K., & Szilagyi, P. G. (2018). Patient reminder and recall interventions to improve immunization rates. Cochrane Database of Systematic Reviews, 1(1), CD003941. https://doi.org/10.1002/14651858.CD003941.pub3d.
Kempe, A., Stockwell, M. S., & Szilagyi, P. (2021). The contribution of reminder-recall to vaccine delivery efforts: A narrative review. Academic Pediatrics, 21(4S), S17–S23. https://doi.org/10.1016/j.acap.2021.02.016.
U.S. Census Bureau (2023, January 3). Urban and rural. https://www.census.gov/programs-surveys/geography/guidance/geo-areas/urban-rural.html
American Academy of Pediatrics (AAP) (2022). Summary of data publicly reported by the Centers for Disease Control and Prevention. https://www.aap.org/en/pages/2019-novel-coronavirus-covid-19-infections/children-and-covid-19-vaccination-trends/
Centers for Disease Control and Prevention (CDC) (2022, October). COVID-19 vaccination coverage and vaccine confidence among children. COVIDVaxView. https://www.cdc.gov/vaccines/imz-managers/coverage/covidvaxview/interactive/children.html. Accessed October 13, 2022.
Montana.gov. Percent of Montanans fully vaccinated by county and by age group (updated monthly). https://dphhs.mt.gov/assets/publichealth/CDEpi/DiseasesAtoZ/2019-nCoV/Reports/MTUptakeGraphs2022-09-30.pdf
WIM Health Workforce Information Services. WIM (2022). https://wimtracking.com/
Albright, K., Saville, A., Lockhart, S., Racich, W., Beaty, K., B., & Kempe, A. (2014). Provider attitudes toward public-private collaboration to improve immunization reminder/recall: A mixed-methods study. Academic Pediatrics, 14(1), 62–70. https://doi.org/10.1016/j.acap.2013.09.003.
Ernst, K. C., Haenchen, S., Pinyerd, H., & Jacobs, B. (n.d.). Report on physician attitudes and practices regarding vaccine exemptions. https://www.azdhs.gov/documents/preparedness/epidemiology-disease-control/immunization/statistics-reports/personal-beliefs-exemption-study/physician-attitudes-and-practices-regarding-vaccine-exemptions.pdf
Kempe, A., O’Leary, S. T., Kennedy, A., Crane, L. A., Allison, M. A., Beaty, B. L., Hurley, L. P., Brtnikova, M., Jimenez-Zambrano, A., & Stokley, S. (2015). Physician response to parental requests to spread out the recommended vaccine schedule. Pediatrics, 135(4), 666–677. https://doi.org/10.1542/peds.2014-3474.
Leib, S., Liberatos, P., & Edwards, K. (2011). Pediatricians’ experience with and response to parental vaccine safety concerns and vaccine refusals: A survey of Connecticut pediatricians. Public Health Reports, 126, 13–26. https://doi.org/10.1177/00333549111260s203.
Saville, A. W., Beaty, B., Dickinson, L. M., Lockhart, S., & Kempe, A. (2014). Novel immunization reminder/recall approaches: Rural and urban differences in parent perceptions. Academic Pediatrics, 14(3), 249–255. https://doi.org/10.1016/j.acap.2014.02.003.
Day, P., Strenth, C., Kale, N., Schneider, F. D., & Arnold, E. M. (2021). Perspectives of primary care physicians on acceptance and barriers to COVID-19 vaccination. Family Medicine and Community Health, 9(4), e001228. https://doi.org/10.1136/fmch-2021-001228.
Kumari, A., Ranjan, P., Chopra, S., Kaur, D., Upadhyay, A. D., Kaur, T., Bhattacharyya, A., Arora, M., Gupta, H., Thrinath, A., Prakash, B., & Vikram, N. K. (2021). Development and validation of a questionnaire to assess knowledge, attitude, practices, and concerns regarding COVID-19 vaccination among the general population. Diabetes & Metabolic Syndrome, 15(3), 919–925. https://doi.org/10.1016/j.dsx.2021.04.004.
Ryan, K., Gannon-Slater, N., & Culbertson, M. J. (2012). Improving survey methods with cognitive interviews in small- and medium-scale evaluations. American Journal of Evaluation, 33(3), 414–430. https://doi.org/10.1177/1098214012441499.
Brtnikova, M., Crane, L. A., Allison, M. A., Hurley, L. P., Beaty, B. L., & Kempe, A. (2018). A method for achieving high response rates in national surveys of U.S. primary care physicians. PLOS One, 13(8), e0202755. https://doi.org/10.1371/journal.pone.0202755.
Harris, P. A., Taylor, R., Thielke, R., Payne, J., Gonzalez, N., & Conde, J. G. (2009). Research electronic data capture (REDCap) – a metadata-driven methodology and workflow process for providing translational research informatics support. Journal of Biomedical Informatics, 42(2), 377–381. https://doi.org/10.1016/j.jbi.2008.08.010.
Harris, P. A., Taylor, R., Minor, B. L., Elliott, V., Fernandez, M., O’Neal, L., McLeod, L., Delacqua, G., Delacqua, F., Kirby, J., Duda, S. N., & REDCap Consortium. (2019). Building an international community of software partners. Journal of Biomedical Informatics, 95,103208. https://doi.org/10.1016/j.jbi.2019.103208
U.S. Department of Agriculture (USDA) (2020, August 17). Rural-urban commuting area codes. https://www.ers.usda.gov/data-products/rural-urban-commuting-area-codes/
U.S. Department of Agriculture (USDA) (2020, August 17). 2010 Rural-urban commuting area codes documentation. https://www.ers.usda.gov/data-products/rural-urban-commuting-area-codes/documentation/
U.S. Census Bureau. Geocoding system (2020). https://geomap.ffiec.gov/FFIECGeocMap/GeocodeMap1.aspx.
WWAMI Rural Health Research Center (RHRC). (n.d.). RUCA data. https://depts.washington.edu/uwruca/ruca-uses.php
WWAMI Rural Health Research Center (RHRC). (n.d.). RUCA: maps. https://depts.washington.edu/uwruca/ruca-maps.php#:~:text=Map%20Classifications&text=Four%20category%20classification%2 C%20Census%20Division,%2 C%20small%20rural%2 C%20and%20isolated
Surbhi, S., Tolley, E. A., Cossman, R. E., Dashputre, A. A., & Bailey, J. E. (2021). Refining a traditional urban-rural classification approach to better assess heterogeneity of treatment effects in patient-centered outcomes research. MethodsX, 8(101299), 1–11. https://doi.org/10.1016/j.mex.2021.101299.
Atkeson, L. R., Adams, A. N., Bryant, L. A., Zilberman, L., & Saunders, K. L. (2011). Considering mixed mode surveys for questions in political behavior: Using the internet and mail to get quality data at reasonable costs. Political Behavior, 33:161–178. https://doi.org/0.1007/s11109-010-9121-1
Kempe, A., O’Leary, S. T., Markowitz, L. E., Crane, L. A., Hurley, L. P., Brtnikova, M., Beaty, B. L., Meites, E., Stokley, S., & Lindley, M. C. (2019). HPV vaccine delivery practices by primary care physicians. Pediatrics, 144(4), e20191475. https://doi.org/10.1542/peds.2019-1475.
R Core Team (2021). R: A language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria. https://www.R-project.org/
Wickham, H. (2009). ggplot2: Elegant graphics for data analysis. New York: Springer.
Stokley, S., Smith, P. J., Klevens, R. M., & Battaglia, M. P. (2001). Vaccination status of children living in rural areas in the United States: Are they protected? American Journal of Preventive Medicine, 20(4 Suppl), 55–60. https://doi.org/10.1016/s0749-3797(01)00280-x.
Walker, T. Y., Elam-Evans, L. D., Williams, C. L., Fredua, B., Yankey, D., Markowitz, L. E., & Stokley, S. (2020). Trends in human papillomavirus (HPV) vaccination initiation among adolescents aged 13–17 by metropolitan statistical area (MSA) status, National Immunization Survey - Teen, 2013–2017. Human Vaccines & Immunotherapeutics, 16(3), 554–561. https://doi.org/10.1080/21645515.2019.1671765.
Williams, C. L., Walker, T. Y., Elam-Evans, L. D., Yankey, D., Fredua, B., Saraiya, M., & Stokley, S. (2020). Factors associated with not receiving HPV vaccine among adolescents by metropolitan statistical area status, United States, National Immunization Survey-Teen, 2016–2017. Human Vaccines & Immunotherapeutics, 16(3), 562–572. https://doi.org/10.1080/21645515.2019.1670036.
Wilson, A. R., Hashibe, M., Bodson, J., Gren, L. H., Taylor, B. A., Greenwood, J., Jackson, B. R., She, R., Egger, M. J., & Kepka, D. (2016). Factors related to HPV vaccine uptake and 3-dose completion among women in a low vaccination region of the USA: An observational study. BMC Women’s Health, 16(1), 1–9. https://doi.org/10.1186/s12905-016-0323-5.
Coe, A. B., Elliott, M. H., Gatewood, S. B. S., Goode, J. R., & Moczygemba, L. R. (2022). Perceptions and predictors of intention to receive the COVID-19 vaccine. Research in Social and Adminstrative Pharmacy, 18(4), 2593–2599. https://doi.org/10.1016/j.sapharm.2021.04.023.
Reiter, P. L., Pennell, M. L., & Katz, M. L. (2020). Acceptability of a COVID-19 vaccine among adults in the United States: How many people would get vaccinated? Vaccine, 38, 6500–6507. https://doi.org/10.1016/j.vaccine.2020.08.043.
Nyhan, B., Reifler, J., Richey, S., & Freed, G. L. (2014). Effective messages in vaccine promotion: A randomized trial. Pediatrics, 133(4), e835–e842. https://doi.org/10.1542/peds.2013-2365.
Aloe, C., Kulldorff, M., & Bloom, B. R. (2017). Geospatial analysis of nonmedical vaccine exemptions and pertussis outbreaks in the United States. Proceedings of the National Academy of Sciences, 114(27), 7101–7105. https://doi.org/10.1073/pnas.1700240114
Medina-Marino, A., Reynolds, D., Finley, C., Hays, S., Jones, J., & Soyemi, K. (2013). Communication and mass vaccination strategies after pertussis outbreak in rural amish communities-Illinois, 2009–2010. Journal of Rural Health, 29(4), 413–419. https://doi.org/10.1111/jrh.12019.
Tandy, C. B., & Odoi, A. (2021). Geographic disparities and socio-demographic predictors of pertussis risk in Florida. PeerJ, 9, e11902. https://doi.org/10.7717/peerj.11902.
Patel, M., Lee, A. D., Clemmons, N. S., Redd, S. B., Poser, S., Blog, D., Zucker, J. R., Leung, J., Link-Gelles, R., Pham, H., Arciuolo, R. J., Rausch-Phung, E., Bankamp, B., Rota, P. A., Weinbaum, C. M., & Gastañaduy, P. A. (2019). National update on measles cases and outbreaks United States, January 1-October 1, 2019. MMWR Morbidity and Mortality Weekly Report, 68(40), 893–896. https://doi.org/10.15585/mmwr.mm6840e2.
Eshofonie, A. O., Lin, H., Valcin, R. P., Martin, L. R., & Grunenwald, P. E. (2015). An outbreak of pertussis in rural Texas: An example of the resurgence of the disease in the United States. Journal of Community Health, 40(1), 88–91. https://doi.org/10.1007/s10900-014-9902-2.
Kempe, A., Steiner, J. F., Renfrew, B. L., Lowery, E., Haas, K., & Berman, S. (2001). How much does a regional immunization registry increase documented immunization rates at primary care sites in rural Colorado? Ambulatory Pediatrics, 1(4), 213–216. https://doi.org/10.1367/1539-4409(2001)001<0213:hmdari>2.0.co;2.
Newcomer, S. R., Freeman, R. E., Wehner, B. K., Anderson, S. L., & Daley, M. F. (2021). Timeliness of early childhood vaccinations and undervaccination patterns in Montana. American Journal of Preventve Medicine, 61(1), e21–e29. https://doi.org/10.1016/j.amepre.2021.01.038.
Acknowledgements
This work was supported by a Center for Biomedical Research Excellence award from the National Institutes of Health, National Institute of General Medical Sciences [1P20GM130418]. The addition of the survey module related to COVID-19 vaccination was supported by an administrative supplement from the National Institutes of Health, National Institute of General Medical Sciences [3P20GM13041802S1]. The use of REDCap was supported by the National Center for Advancing Translational Sciences of the National Institutes of Health [UL1 TR002319, KL2 TR002317, TL1 TR002318]. The content is solely the responsibility of the authors and does not necessarily represent the official views of the National Institutes of Health.
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation and data collection were performed by Alexandria Albers, Sophia Newcomer, Kathrene Conway, and Juthika Thaker. Data analysis was completed by Alexandria Albers and Sophia Newcomer. The first draft of the manuscript was written by Alexandria Albers and all authors commented on previous versions of the manuscript. All authors have read and approved the final manuscript.
Corresponding author
Ethics declarations
Competing interests
The authors have no competing interests to declare that are relevant to the content of this article.
Ethical Approval
This project was reviewed by the University of Montana Institutional Review Board and was considered under the exempt category of review.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic Supplementary Material
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Albers, A.N., Wright, E., Thaker, J. et al. Childhood Vaccination Practices and Parental Hesitancy Barriers in Rural and Urban Primary Care Settings. J Community Health 48, 798–809 (2023). https://doi.org/10.1007/s10900-023-01226-4
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-023-01226-4