Abstract
Correctional workers form a high-priority group for tuberculosis control measures because of their high exposure and risk. This cross-sectional study conducted in April and May 2022 included 71 criminal police officers from the State Penitentiary of Francisco Beltrão-PR, Brazil. Their sociodemographic and laboratory data were collected. Latent tuberculosis infection (LTBI) was assessed using a QuantiFERON-TB Gold Plus in-tube test kit. Binary logistic regression was applied to calculate the odds ratios (ORs) and 95% confidence intervals (CI) of the LTBI predictors. The prevalence of LTBI was 22.6% (95% CI, 12.8–32.2%). Factors associated with LTBI were age > 43 years (OR, 0.18; 95% CI, 0.04–0.70; p < 0.014) and the use of medications (OR, 5.13; 95% CI, 1.40–18.87; p < 0.014). The prevalence was close to that estimated worldwide for LTBI in correctional workers, reinforcing the need for occupational health control measures consisting of regular screening and treatment of positive cases of latent infection among correctional workers to reduce the risk of illness and spread of infection in the penitentiary system and community.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Tuberculosis (TB) has historically been associated with poverty, malnutrition, overcrowding, immunosuppression, and insufficient access to health care [1]. TB is among the leading causes of morbidity and mortality from a single infectious agent worldwide, ranking above human immunodeficiency virus (HIV)/acquired immunodeficiency syndrome [2, 3]. It is estimated that in 2021, 10.6 million people (95% confidence interval [CI], 9.9–11 million) became ill with TB, a 4.5% increase compared to 2020, and the burden of drug-resistant TB has increased during this period [3], generating economic losses for patients, their families, and the country due to the reduction of the national productive force [4].
Considering the Brazilian commitment to eliminate TB by 2035 [3], it is essential to identify and treat cases of latent TB infection (LTBI) in occupational environments and workplaces that present a greater risk to occupational health [5, 6], such as correctional facilities. These environments are responsible for an increase of approximately 5% per year in cases of latent infection among inmates and may be responsible for the transmission of Mycobacterium tuberculosis to the community [2, 7, 8] as well as to correctional workers [9,10,11,12].
Globally, high rates of TB are frequently observed among incarcerated people [13,14,15,16,17]. In Brazil, the incidence of TB in prisons is approximately 20 times higher than in the general population, with the prevalence of active and latent TB among incarcerated persons is estimated at 2–9% and 40–73%, respectively [18].
The work activity of prison officers in correctional facilities, where they have close and prolonged contact with detainees, exposes them to M. tuberculosis and makes them possible facilitators of the spread of TB in the community [8]. Many studies of LTBI in prisoners have been conducted in Brazil [18, 19] versus few in correctional workers [10,11,12]; such studies are also scarce internationally [2, 9, 20, 21].
Despite the high prevalence of LTBI among inmates and evidence of continued transmission within prisons [22], correctional workers are not routinely screened. To move toward TB elimination, it is imperative to focus on high-risk populations as well as populations with direct contact. Thus, this investigation aimed to estimate the prevalence of and factors associated with LTBI among correctional workers in Paraná.
Methods
This cross-sectional prospective study performed in April and May 2022 included correctional workers at the State Penitentiary of Francisco Beltrão-PR. The reported 29.1% prevalence of LTBI in correctional unit workers was used as reference [11]. The sample size was calculated in Epi Info [23], using a population of 104 professionals, with an expected prevalence of 29.1%, variation of 1%, power of 80%, and alpha of 5%. An extra 10% of professionals were included to account for anticipated loss due to refusal to participate, resulting in a final sample of 85 employees. Only workers in direct contact with inmates participated in the study. Workers with at least 1 year of experience of either sex or any age and on a work schedule were included, and a sample of biological material was obtained from each. Workers on leave or with a medical certificate, who had returned to the sector for less than 1 year, who were pregnant, or who were previously diagnosed with or treated for TB were excluded.
The participants were informed about the purpose and stages of the research, after which they signed an informed consent form and answered a self-administered questionnaire that contained questions about personal characteristic data, work information, and TB. Subsequently, 4 mL of blood was collected from each participant. All samples were sent to Hermes Pardini Laboratory, processed with a QuantiFERON-TB Gold Plus in-tube test kit (lot no. 56,907,193; expiration date, 02/03/2024; Qiagen, Hilde, Germany), using enzyme-linked immunosorbent assay. The results were interpreted according to the manufacturer’s instructions. The cut-off value for a positive test was 0.35 UI/mL of interferon-γ in the plasma after stimulation regardless of the nitrogen control result. The test result was considered indeterminate if an antigen-stimulated sample tested negative and the positive control value was < 0.5 IU/mL after subtraction of the negative control value.
All correctional workers were informed through an orientation letter about the results and mechanism of the disease. For those with a positive Interferon Gamma Release Assay (IGRA) result, an appointment was scheduled with a pulmonologist, and a chest computed tomography scan was performed. A rapid test for HIV due to its correlation with TB, an HIV1/2/O Tri-line test (Hangzhou Economic & Technological Development Area, Hangzhou, 310,018, P.R. China), and other complementary tests were also performed to confirm the diagnosis. The medical professional established the conduct based on the Ministry of Health protocols for LTBI [24], and a return visit was scheduled for all positive cases for a 6-month new evaluation.
After collection, the data were tabulated in Excel software and analyzed in the SPSS program (version 25.0; IBM, Arlington, NY, USA). First, the database was inspected for typographical errors and edge cases. Descriptive statistical analyses were performed, including mean, standard deviation, range, frequency (%) and CI. Fisher’s exact test and Pearson’s chi-squared test were used to identify bivariate associations. The independent variables that presented values of p < 0.20 in that stage were entered into the logistic regression models. Finally, the independent variables that presented values of p < 0.05 after the adjustment for the other variables remained in the final multivariable model. The variables were manually inserted to define the final model.
The study complied with the ethical precepts of research involving human beings as established by Resolution 466/2012 of the National Health Council and was approved by the Research Ethics Committee of the University of Western Paraná (opinion no. 5.346.101).
Results
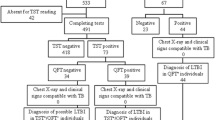
Of the calculated sample of 85 workers from correctional units, 71 agreed to participate, with losses and refusals comprising 16.47% (n = 14). Among the 71 correctional workers, the mean age was 42.91 ± 6.07 years (range, 30–59 years). The average income was R$11,591.50 ± 5,558.98 (range, R$2,000.00–24,000.00). Of the interviewees, the average time in the profession was 8.57 ± 3.01 years (range, 1–14 years), while the average working time in the investigated penitentiary was 6.77 ± 2.73 years (range, 1–10 years). Of the interviewees, nine (12.7%) claimed to have arterial hypertension, six (8.5%) had dyslipidemia, five (7%) had hyperthyroidism, four (5.6%) had viral hepatitis B or C, and one each (1.4%) had diabetes mellitus and osteoporosis.
The criminal police work schedules are 24 × 48 and 12 × 60 h, with 3% working at 24 × 48 and 24 × 72 h. The mean body mass index of male correctional workers was 28.35 ± 3.60 (range, 21.38–38.51), while that of female correctional workers was 26.44 ± 4.98 (range, 21.05–34.63). Officers of both sexes had high percentages of overweight and obesity (84.1% of men, 50% of women); that is, 80% (95% CI, 71.0–89.5%) of the participants were overweight or obese (n = 57).
Regarding LTBI, the highest frequency of criminal police officers were ≤ 43 years of age, were White, had > 9 years of schooling, were married or had a stable partner, were overweight or obese, had been immunized for hepatitis B, had > 9 years’ experience working in a penitentiary unit, had a history of transfer from correctional units, and had serological scarring for Bacillus Calmette-Guérin. All workers with a positive LTBI result had contact with inmates with symptoms of active TB, but the results were not statistically significant (Table 1).
The prevalence of LTBI in the study population was 22.6% (95% CI, 12.8–32.2%). We did not observe any indeterminate QuantiFERON-TB Gold Plus in-tube test kit results among the correctional workers in our study.
Table 2 presents the crude and adjusted binary logistic regression models after the bivariate analyses. Of all variables considered in the model, only two remained significant and were independently associated with LTBI. We observed that age > 43 years decreased the risk of a positive LTBI test result by 82%, while medication use increased the likelihood of LTBI by 413%.
Discussion
There are few studies of correctional workers diagnosed with latent M. tuberculosis infection using the IGRA test with an interferon-γ release assay [25], and most have used the tuberculin skin prick test [2, 9,10,11, 20, 21, 26, 27].
The prevalence identified in our study (22.6%) was close to that calculated in a systematic review of 110,192 correctional workers from five countries in 1986–2015 of 26% (95% CI, 12–42%) [2], lower than that of the Brazilian study in 12 prison units in the municipality of Franco da Rocha, SP of 33.7% (95% CI, 30.8–36.5%) [11] and the estimated prevalence in Colombia of 39.1% in two prisons and 55.8% in one prison [27]. These estimates are worrisome, as the disease can reactivate at any time in approximately 5% of people infected with M. tuberculosis, although this is usually within the first 5 years after infection or by being exposed to new sources of infection [28, 29]. It is estimated that, in the prison population, the working environment of the correctional worker, the incidence is up to 28 times higher [2, 30] than in the general population [2, 19, 30] and responsible for the increase of 8.5% and 6.3% of all TB cases in community settings in high-income countries, respectively [9]. Given this risk, the latency of the bacillus is a main challenge preventing TB eradication and prevention, especially in high-risk groups [31].
Other studies presented contradictory findings that describe older age as a factor associated with LTBI [2], which we identified as a protective factor. We identified that the correctional workers in our study were younger and had a history of transferring between correctional units in the previous year, which corroborates the plausibility of the nature of occupational transmission [5, 6], especially in Brazil, a country with a high TB burden whose environment prison environment is favorable for increasing the prevalence of LTBI among inmates [9, 10, 12, 19, 20, 26].
Correctional workers who use medication are more likely to have a positive LTBI result; among them, most worked long hours in an environment with unhealthy conditions, stress, and work overload, demonstrating the extent to which the work environment influences health [32] and makes them more susceptible to contracting TB [33].
The limitations of this study are the fact that it was cross-sectional and the data collection of exposure and outcomes occurred simultaneously, making it difficult to understand the temporal relationship between them. The small number of national and international studies using the same diagnostic method with the same target population limits the comparability of our findings with those of other studies.
The prevalence observed in the present study was close to that estimated worldwide for LTBI among correctional workers, reinforcing the need for occupational health control measures with regular screening and treatment of positive cases of LTBI among them [2, 6, 27] to reduce the risk of illness and the spread of TB in the penitentiary system and community.
Data Availability
The datasets generated during and/or analyzed during the current study are available from the corresponding author on reasonable request.
References
Mahara, G., Yang, K., Chen, S., Wang, W., & Guo, X. (2018). Socio-Economic Predictors and distribution of tuberculosis incidence in Beijing, China: a study using a combination of spatial statistics and GIS technology. Medical Sciences, 6(2), 26. https://doi.org/10.3390/medsci6020026.
Grenzel, M. L., Grande, A. J., Paniago, A. M. M., Pompilio, M. A., de Oliveira, S. M. do V. L., & Trajman, A. (2018). Tuberculosis among correctional facility workers: A systematic review and meta-analysis. PloS One, 13(11), e0207400. https://doi.org/10.1371/journal.pone.0207400
World Health Organization, W (2022). Global tuberculosis report 2022. Retrieved from https://www.who.int/teams/global-tuberculosis-programme/tb-reports
da Moreira, S. R., Lineu Kritski, A., A., & Calçada Carvalho, A. C. (2020). Social determinants of health and catastrophic costs associated with the diagnosis and treatment of tuberculosis. Jornal Brasileiro de Pneumologia, 46(5), e20200015–e20200015. https://doi.org/10.36416/1806-3756/e20200015.
Chaw, L., Chien, L. C., Wong, J., Takahashi, K., Koh, D., & Lin, R. T. (2020). Global trends and gaps in research related to latent tuberculosis infection. Bmc Public Health, 20(1), 352. https://doi.org/10.1186/s12889-020-8419-0.
Montecucco, A., Dini, G., Rahmani, A., Sticchi, L., & Durando, P. (2020). The seedbeds of tuberculosis: is it time to target congregate settings and workplaces? Journal of Preventive Medicine and Hygiene, 61(3), E324–E330. https://doi.org/10.15167/2421-4248/jpmh2020.61.3.1759.
Carbone, A. da S. S., Paião, D. S. G., Sgarbi, R. V. E., Lemos, E. F., Cazanti, R. F., Ota, M. M., … Croda, J. (2015). Active and latent tuberculosis in Brazilian correctional facilities: a cross-sectional study. BMC infectious diseases, 15, 24. https://doi.org/10.1186/s12879-015-0764-8
Sacchi, F. P. C., Praça, R. M., Tatara, M. B., Simonsen, V., Ferrazoli, L., Croda, M. G., … Croda, J. (2015). Prisons as Reservoir for Community Transmission of Tuberculosis, Brazil. Emerging Infectious Diseases, 21(3), 452–455. https://doi.org/10.3201/eid2103.140896
Al-Darraji, H. A. A., Tan, C., Kamarulzaman, A., & Altice, F. L. (2015). Prevalence and correlates of latent tuberculosis infection among employees of a high security prison in Malaysia. Occupational and Environmental Medicine, 72(6), 442–447. https://doi.org/10.1136/oemed-2014-102695.
Busatto, C., Nunes, L. de S., Valim, A. R. de M., Valença, M. S., Krug, S. F., Becker, D., … Possuelo, L. G. (2017). Tuberculosis among prison staff in Rio Grande do Sul. Revista Brasileira de Enfermagem, 70(2), 370–375. https://doi.org/10.1590/0034-7167-2016-0012
Nogueira, P. A., Abrahão, R. M. C., de Galesi, M., V. M. N., & López, R. V. M. (2018). Tuberculose e infecção latente em funcionários de diferentes tipos de unidades prisionais. Revista de Saúde Pública, 52, 13. https://doi.org/10.11606/S1518-8787.2018052007127.
Valle, S. M. do, de Oliveira, L., Lemos, E. L., Castro, L., Motta-Castro, A. R. C., Bandeira, L. M., … Maciel, E. L. N. (2017). Infecção Latente por Tuberculose em Trabalhadores do Sistema Prisional. Retrieved from https://proceedings.science/proceedings/60/_authors/204718
Soltobekova, N., Kozukeev, T., Yiehdego, G., Labib, F., Hovhannesyan, A., & Rossi, R. (2022). Time to start of tuberculosis treatment in penitentiary system of Kyrgyz Republic: a retrospective cohort study. PLOS ONE, 17(3), e0264252. https://doi.org/10.1371/journal.pone.0264252.
Dara, M., Chadha, S. S., Melchers, N. V., van den Hombergh, J., Gurbanova, E., Al-Darraji, H., & van der Meer, J. B. W. (2013). Time to act to prevent and control tuberculosis among inmates [Official Statement of the International Union against Tuberculosis and Lung Disease]. The International Journal of Tuberculosis and Lung Disease, 17(1), 4–5. https://doi.org/10.5588/ijtld.12.0909.
Izzo, C., Monica, A., De Matteis, G., De Biasi, S., De Chiara, A., Pagano, A. M.,… Maiese, A. (2022). Not Only COVID-19: Prevalence and Management of Latent Mycobacterium Tuberculosis Infection in Three Penitentiary Facilities in Southern Italy. Healthcare (Basel, Switzerland), 10(2), 386. https://doi.org/10.3390/healthcare10020386
López de Goicoechea-Saiz, M. E., Sternberg, F., & Portilla-Sogorb, J. (2018). Prevalence and associated risk factors of latent tuberculosis infection in a spanish prison. Revista Espanola De Sanidad Penitenciaria, 20(1), 4–10.
Agostinis, A., Heffernan, C., Long, R., Beckon, A., Cockburn, S., & Ahmed, R. (2021). Interferon-gamma release assays for latent tuberculosis infection screening in canadian federal correctional facilities. The International Journal of Tuberculosis and Lung Disease: The Official Journal of the International Union Against Tuberculosis and Lung Disease, 25(6), 447–452. https://doi.org/10.5588/ijtld.20.0801.
Carbone, A. da S. S., Sgarbi, R. V. E., Lemos, E. F., Paião, D. S. G., Simionatto, S., Castro, A. R. C. M. de, … Croda, J. (2018). Estudo multicêntrico da prevalência de tuberculose e HIV na população carcerária do Estado do Mato Grosso do Sul. Comunicação em Ciências da Saúde, 28(01), 53–57. https://doi.org/10.51723/ccs.v28i01.116
de Navarro, P. D., de Almeida, I. N., Kritski, A. L., Ceccato, M. G., Maciel, M. M. D., Carvalho, W. da S., & de Miranda, S. S. (2016). Prevalence of latent Mycobacterium tuberculosis infection in prisoners. Jornal Brasileiro de Pneumologia, 42(5), 348–355. https://doi.org/10.1590/S1806-37562016000000001
Jochem, K., Tannenbaum, T. N., & Menzies, D. (1997). Prevalence of tuberculin skin test reactions among prison workers. Canadian Journal of Public Health = Revue Canadienne De Sante Publique, 88(3), 202–206.
Steenland, K., Levine, A. J., Sieber, K., Schulte, P., & Aziz, D. (1997). Incidence of tuberculosis infection among New York State prison employees. American Journal of Public Health, 87(12), 2012–2014. https://doi.org/10.2105/AJPH.87.12.2012.
Mabud, T. S., de Lourdes Delgado Alves, M., Ko, A. I., Basu, S., Walter, K. S., Cohen, T.,… Andrews, J. R. (2019). Evaluating strategies for control of tuberculosis in prisons and prevention of spillover into communities: An observational and modeling study from Brazil. PLoS medicine, 16(1), e1002737. https://doi.org/10.1371/journal.pmed.1002737
CDC. (n.d.). EPI Info: pacote estatístico gratuito desenvolvido pelo CDC. Retrieved from Plataforma Renast Online. Epi Info: https://www.cdc.gov/epiinfo/index.html.
Brasil, M., & da Saúde, S. (2019). de V. em Saúde. D. de V. das D. T. Manual de Recomendações para o controle da tuberculose no Brasil. Retrieved from http://www.saude.sp.gov.br/resources/cve-centro-de-vigilancia-epidemiologica/areas-de-vigilancia/tuberculose/manuais-tecnicos/tb19_manual-2edrecomendacoes.pdf
Oliveira, S. M. do V. L. de, Lemos, E. F., Motta-Castro, A. R. C., Bandeira, L. M., Puga, M. A. M., Rezende, G. R. de, … Maciel, E. L. N. (2017). Infecção Latente por Tuberculose em Trabalhadores do Sistema Prisional. ANais Do Congresso da Sociedade Brasileira de Medicina Tropical presented at the Congresso da Sociedade Brasileira de Medicina Tropical, Campinas, Galoá. Retrieved from https://proceedings.science/medtrop/papers/infeccao-latente-por-tuberculose-em-trabalhadores-do-sistema-prisional.
Nogueira, P. A., de Abrahão, R. M. C. M., & Galesi, V. M. N. (2011). Infecção tuberculosa latente em profissionais contatos e não contatos de detentos de duas penitenciárias do estado de São Paulo, Brasil, 2008. Revista Brasileira de Epidemiologia, 14(3), 486–494. https://doi.org/10.1590/S1415-790X2011000300013.
Arroyave, L., Keynan, Y., Sanchez, D., López, L., Marin, D., Posada, M., & Rueda, Z. V. (2019). Guards in prisons: a Risk Group for latent tuberculosis infection. Journal of Immigrant and Minority Health, 21(3), 578–585. https://doi.org/10.1007/s10903-018-0746-1.
Aguiar, F. S., & de Mello, F. C. Q (2019). Latent tuberculosis and the use of immunomodulatory agents. Jornal Brasileiro de Pneumologia, 45(6), e20190361. https://doi.org/10.1590/1806-3713/e20190361.
Zellweger, J. P., Sotgiu, G., Corradi, M., & Durando, P. (2020). The diagnosis of latent tuberculosis infection (LTBI): currently available tests, future developments, and perspectives to eliminate tuberculosis (TB): the diagnosis of latent tuberculosis infection (LTBI). La Medicina del Lavoro | Work Environment and Health, 111(3), 170–183. https://doi.org/10.23749/mdl.v111i3.9983.
de Júnior, A. M. F., & Sá, A. M. M. (2019). Prevalência da infecção latente tuberculosa em comunicantes de portadores de tuberculose pulmonar. Revista Eletrônica Acervo Saúde, (30), e851. https://doi.org/10.25248/reas.e851.2019.
Anton, C., Machado, F. D., Ramirez, J. M. A., Bernardi, R. M., Palominos, P. E., Brenol, C. V., … Silva, D. R. (2019). Latent tuberculosis infection in patients with rheumatic diseases. Jornal Brasileiro de Pneumologia, 45(2), e20190023. https://doi.org/10.1590/1806-3713/e20190023.
Pauli, F. B., Follador, F. A. C., Wendt, G., Lucio, L. C., Pascotto, C. R., & Ferreto, L. E. D. (2022). Condiciones de trabajo y salud de los funcionarios de prisiones en Paraná (Brasil). Rev Esp Sanid Penit, 24(3), 85–92.
Mennoial, N. V., Napoli, P., Battaglia, A., & Candura, S. M. (2014). [Occupational risk factors and medical prevention in corrections officers]. Giornale Italiano Di Medicina Del Lavoro Ed Ergonomia, 36(4), 405–409.
Acknowledgements
To the Araucária Foundation of the State of Paraná (ARAUCÁRIA) for the financial assistance (Term of Agreement nº 289/2022).
Author information
Authors and Affiliations
Contributions
All authors contributed to the study conception and design. Material preparation, data collection and analysis were performed by Maico Trevisol, Thiago Poss Moreira, Gustavo Henrique Baraca Sanvezzo and Lirane Elize Defante Ferreto. The first draft of the manuscript was written by Maico Trevisol and all authors commented on previous versions of the manuscript. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of Interest
The authors have no competing interests to declare that are relevant to the content of this article.
Ethical Approval
The study was approved by the Institutional Review Board at the Western Paraná State University [opinion number. 5.346.101]. All participants provided their informed consent to participate in the study.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Trevisol, M., Moreira, T.P., Sanvezzo, G.H.B. et al. Latent Tuberculosis Infection Diagnosis Using QuantiFERON-TB Gold Plus Kit Among Correctional Workers: A Cross-Sectional Study in Francisco Beltrão-PR, Brazil. J Community Health 48, 600–605 (2023). https://doi.org/10.1007/s10900-023-01201-z
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10900-023-01201-z