Abstract
Increasing evidence has indicated that glutaredoxin 1 (GRX1) is a potent antioxidant protein that promotes cell survival under conditions of oxidative stress. Oxidative stress-induced neuronal injury contributes to cerebral ischemia/reperfusion injury. However, the role of GRX1-mediated antioxidant defense against neuronal damage during cerebral ischemia/reperfusion injury has not been thoroughly investigated. Thus, the objective of this study was to evaluate whether GRX1 protects neurons against oxygen-glucose deprivation/reoxygenation (OGD/R)-evoked oxidative stress injury in an in vitro model of cerebral ischemia/reperfusion injury. Our data revealed that GRX1 was induced by OGD/R treatment in neurons. Functional assays indicated that loss of GRX1 exacerbated OGD/R-induced apoptosis and the generation of reactive oxygen species (ROS), while GRX1 up-regulation protected against OGD/R-evoked neuronal injury. Further investigation revealed that GRX1 promoted the nuclear expression of nuclear factor erythroid 2-related factor 2 (Nrf2) and enhanced transcription of the Nrf2/antioxidant response element (ARE) in GOD/R-exposed neurons. Furthermore, GRX1 promoted the activation of Nrf2/ARE associated with the modulation of glycogen synthase kinase-3β (GSK-3β). GSK-3β inhibition blocked GRX1 knockdown-mediated suppression of Nrf2 activation. Notably, the suppression of Nrf2 partially reversed GRX1-mediated anti-oxidative stress injury in OGD/R-exposed neurons. In summary, these findings indicate that GRX1 protects neurons against OGD/R-induced oxidative stress injury by enhancing Nrf2 activation via the modulation of GSK-3β. Our study suggests that GRX1 is a potential neuroprotective protein that protects against cerebral ischemia/reperfusion injury.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Cerebral ischemia/reperfusion injury is a life-threatening pathological process that has been the leading cause of disability and mortality for the last few years (Benjamin et al. 2018). Insufficient blood supply caused by blood vessel occlusion in the brain leads to irreversible ischemic damage that can be further exacerbated by blood reperfusion. The process is called cerebral ischemia/reperfusion injury (Lo et al. 2003). The pathological effects of cerebral ischemia/reperfusion injury are accompanied by the excessive production of reactive oxygen species (ROS), which causes oxidative stress in neurons and contributes to brain damage (Saito et al. 2005). Thus, enhancing our understanding of the mechanisms involved in neuronal death and oxidative stress could provide novel therapeutic strategies for the management of cerebral ischemia/reperfusion injury.
Glutaredoxin 1 (GRX1), a member of the sulfhydryl disulfide oxidoreductases, catalyzes the removal of glutathione from cysteine residues, which helps to maintain steady-state protein functioning (Gravina and Mieyal 1993; Allen and Mieyal 2012). GRX1 modulates various cell functions, including cell survival, apoptosis, differentiation and transcription (Sun et al. 2017; Yang et al. 2018; Madusanka et al. 2020). The dysregulation of GRX1 contributes to the pathogenesis of numerous disorders, including cancer, osteoarthritis and cardiovascular disease (Qi et al. 2016; Chen et al. 2017; Sun et al. 2017). Notably, GRX1 plays a vital role in maintaining the cellular redox state (Zhu et al. 2017). The overexpression of GRX1 prevented hydrogen peroxide-induced apoptosis and oxidative stress in retinal pigment epithelial cells (Liu et al. 2015). The up-regulation of GRX1 inhibited oxidative stress and apoptosis in osteoarthritis chondrocytes (Sun et al. 2017). A deficiency of GRX1 enhanced the excessive accumulation of intracellular oxidants, including ROS in HeLaS3 cells with exposure to γ-ray irradiation, heat shock and hydrogen peroxide (Zhao and Zhang-Akiyama 2020). Therefore, GRX1 represents an attractive target for the modulation of cellular protection in response to oxidative stress.
Cellular redox homeostasis is principally maintained by nuclear factor erythroid 2-related factor (Nrf2) (Itoh et al. 1997). Nrf2 is a Cap ‘n’ Collar basic leucine zipper transcription factor that is activated in response to oxidative stress (Kensler et al. 2007). Generally, Nrf2 translocates from the cytoplasm to the nucleus, where it interacts with anti-oxidant response element (ARE) within the promoter region of target genes. This up-regulates the transcription of a group of cytoprotective genes (Ma and He 2012). Nrf2/ARE activation is controlled by multiple regulators at different levels (Silva-Islas and Maldonado 2018). Glycogen synthase kinase-3β (GSK-3β) modulates Nrf2/ARE activation (Rada et al. 2012; Cuadrado 2015). The activation of GSK-3β results in Nrf2 degradation, and blocks the activation of Nrf2/ARE (Rada et al. 2012; Cuadrado 2015). Importantly, the GSK-3β/Nrf2 axis regulates oxidative stress during cerebral ischemia/reperfusion injury (Cai et al. 2017; Rana and Singh 2018). Moreover, multiple studies have reported that the GSK-3β/Nrf2 axis is regulated by various factors and mechanisms during cerebral ischemia/reperfusion injury (Liu et al. 2018; Park et al. 2018; Bao and Gao 2020). Thus, elucidating the molecular mechanism by which the GSK-3β/Nrf2 axis is activated has the potential to facilitate the development of promising approaches for preventing the oxidative stress-induced cerebral ischemia/reperfusion injury.
GRX1 is capable of protecting against oxidative stress and enhancing cell survival under various conditions of stress (Li et al. 2014; Liu et al. 2015, 2016). Emerging evidence revealed that GRX1 plays a crucial role in maintaining neuronal survival under different destructive stresses (Johnson et al. 2015). Interestingly, a recent study reported that GRX2, another member of GRX protein family, is also capable of preventing OGD/R-induced neuronal injury (Wen et al. 2020), indicating that the GRX protein family may have critical roles in cerebral ischemia/reperfusion injury. Moreover, GRX1 plays a key role in mediating myocardial ischemia/reperfusion injury (Burns et al. 2020). To date, whether GRX1 participates in the modulation of neuronal survival and oxidative stress during cerebral ischemia/reperfusion injury remains unknown. Thus, the objective of this study was to evaluate whether GRX1 protects neurons against oxygen-glucose deprivation/reoxygenation (OGD/R)-evoked injury in an in vitro model of cerebral ischemia/reperfusion injury. We demonstrated that GRX1 was induced by OGD/R treatment in neurons, and that a loss of GRX1 exacerbated OGD/R-induced apoptosis and ROS generation. Notably, the up-regulation of GRX1 protected against OGD/R-evoked neuronal injury. Further investigation revealed that GRX1 enhanced the nuclear expression of Nrf2 and enhanced the transcription of Nrf2/ARE in GOD/R-exposed neurons. Moreover, GRX1 promoted Nrf2/ARE activation via the modulation of GSK-3β phosphorylation. The suppression of Nrf2 partially reversed GRX1-mediated protective effects in OGD/R-exposed neurons. In summary, these findings indicate that GRX1 protected neurons from OGD/R-induced injury through the modulation of GSK-3β/Nrf2 signaling.
Materials and methods
Neuron culture
HT22 hippocampal neurons were provided by the BeNa Culture Collection (Kunshan, Jiangsu Province, China) and cultured using recommended methods. Briefly, HT22 neurons were plated on Dulbecco’s modified Eagle’s medium (DMEM) (Thermo Fisher Scientific, Waltham, MA, USA) supplemented with 10 % fetal bovine serum and cultivated in 95 % air/5 % CO2 at 37 °C. Cells at the second passage were utilized for the experiments.
Induction of OGD/R injury in HT22 neurons
HT22 neurons were washed with phosphate-buffered saline (PBS), plated in glucose-free medium and cultured under a hypoxic conditions (5 % CO2/3 % O2/92 % N2 at 37 °C) for 8 h, which stimulated ischemic-like conditions in vitro. Then, media was replaced with fresh media supplemented with 4.5 g/l glucose, and neurons were cultured for 24 h under normoxic conditions (95 % air/5 % CO2).
Real-time quantitative RCR (RT-qPCR)
HT22 neurons were collected and homogenized in TRIzol Reagent (Thermo Fisher Scientific) for total RNA extraction. The purified RNA was converted to cDNA using the EasyScript First-Strand cDNA Synthesis SuperMix (TransGen, Beijing, China). RT-qPCR was performed to quantify transcript levels using PerfectStartT Green qPCR SuperMix (TransGen). The recommended thermal cycle program was used, as follows: 94°C for 30 s and 45 cycles of 94°C for 5 s and 60°C for 30 s. RT-qPCR data were assessed using the 2−ΔΔCt method, and gene expression was determined using β-actin as a reference gene. The primer sequences were as follows: GRX1 sense: 5’-GCTCAGGAGTTTGTGAACTGC-3’ and antisense: 5’-AGAAGACCTTGTTTGAAAGGCA-3’; β-actin sense: 5’-GGCTGTATTCCCCTCCATCG-3’ and anti-sense: 5’-CCAGTTGGTAACAATGCCATGT-3’.
Western blot
HT22 neurons were collected and homogenized in Western Lysis Buffer (Beyotime, Shanghai, China) containing a proteinase inhibitor cocktail and phenylmethanesulfonyl fluoride for protein extraction. After determination of protein concentration by the bicinchoninic acid (BCA) method, equivalent amounts of proteins were resolved via sodium dodecyl sulfate polyacrylamide gel electrophoresis. Separated proteins were transferred to polyvinylidene difluoride (PVDF) membranes using an Electrophoretic Blotting System (Bio-Rad Laboratories, Shanghai, China). PVDF membranes were blocked with 5 % nonfat milk, and incubated with appropriate antibodies including rabbit polyclonal anti-GRX1 (1:500), rabbit polyclonal anti-β-actin (1:1000), rabbit polyclonal anti-Nrf2 (1:500), rabbit polyclonal anti-Histone H3 (1:1000), mouse monoclonal anti-phospho-GSK-3β (1:1000) (Sanying Biotech, Wuhan, China). Immunoreactive proteins were developed by ECL Western Blotting Substrate (Thermo Fisher Scientific) after incubation with goat anti-rabbit or goat anti-mouse secondary antibodies (Sanying Biotech). Protein expression was determined by measuring band intensities using Image-Pro Plus 6.0.
Cell transfection
The siRNA sequences targeting GRX1 were designed and synthesized by GenePharma (Shanghai, China). GRX1 coding sequences were subcloned into a pcDNA3.1 vector to construct a GRX1 expression vector. Lipofectamine 3000 Reagent (Thermo Fisher Scientific) was used to transfect siRNAs or vectors into HT22 neurons in accordance with the manufacturer’s recommendations. In brief, cells were grown to 70 % confluence at the time of transfection. The vectors or siRNAs were mixed with Lipofectamine 3000 Reagent and then added to cells. Transfected cells were incubated for 48 h at 37 °C before subsequent detections.
Cell viability assay
Cell counting kit-8 (CCK-8) which can be converted into orange formazan by intracellular dehydrogenase was utilized to measure the viability of cells. HT22 neurons were seeded into a ninety-six-well plate (1 × 104) and cultivated overnight prior to transfection. After transfection and OGD/R exposure, 10 µl per well CCK-8 reagent was added to cells. After an incubation period of 2 h, cell viability was determined by measuring the absorbance of each solution at 450 nm with a Microplate Reader (Bio-Tek Instruments, Winooski, VA, USA).
Cell apoptosis assay
Apoptosis in HT22 neurons was assessed by flow cytometry using an Annexin V-FITC/PI Apoptosis Detection Kit (Beyotime, Shanghai, China) in accordance with the manufacturer’s protocols. In brief, cells were digested by trypsin to obtain single cell suspension. A total of 5 × 104 cells were collected and suspended into 195 µl of Annexin V-FITC binding buffer. Then, 5 µl of Annexin V-FITC and 10 µl of PI reagents were added to the cells. Cells were incubated for 10 min in the dark. Afterwards, cells were detected by flow cytometry.
ROS assay
Intracellular ROS levels were quantitatively determined using a ROS-sensitive DCFH-DA probe that was capable of being converted to fluorescent DCF when oxidized. DCFH-DA (Beyotime) was diluted in serum-free medium to produce a final concentration of 10 µmol/l. HT22 neurons were harvested after they were treated appropriately, and were resuspended using DCFH-DA-containing media. Cells were cultivated for 20 min in an incubator at 37 °C. Thereafter, cells were washed with serum-free medium to completely remove DCFH-DA that had not entered cells. Fluorescence was quantitatively determined using flow cytometry.
Nrf2 transcriptional activity assay
Nrf2 transcriptional activity was evaluated using an Nrf2/ARE luciferase reporter vector. The Nrf2/ARE luciferase reporter vector (Beyotime, Shanghai, China), Ranilla luciferase reporter vector, and GRX1 siRNA or the GRX1 expression vector were co-transfected into HT22 neurons and cultivated for 48 h. After OGD/R exposure, cells were collected and analyzed using a Dual Luciferase Reporter Gene Assay Kit (Beyotime) to measure luciferase activities within cells.
Statistical analysis
Each individual experiment was repeated at least three times. The means and standard deviations of the data were obtained by using GraphPad Prism 8 (GraphPad Software Inc., San Diego, CA, USA). All of the data were expressed as means ± standard deviations. Differences were determined using the Student’s t test or one-way analysis of variance (ANOVA) followed by Bonferroni’s post-hoc test. Values of p < 0.05 were considered significant.
Results
GRX1 was an OGD/R-responsive factor in neurons
To evaluate whether GRX1 modulates OGD/R-induced neuronal injury, we assessed changes in the expression of GRX1 in response to OGD/R exposure in HT22 neurons. RT-qPCR findings indicated that OGD/R exposure induced GRX1 mRNA expression in HT22 neurons (Fig. 1a). Moreover, protein expression of GRX1 was also induced by OGD/R exposure (Fig. 1b and c). These data imply that GRX1 acts as an OGD/R-responsive factor in neurons.
Effect of OGD/R exposure on GRX1 expression. a Relative mRNA expression of GRX1 was examined using RT-qPCR (n = 3). b Protein expression of GRX1 was determined via Western blot, and c the quantification data (n = 3). Data were expressed as means ± standard deviation. Differences were assessed by the Student’s t test. **p < 0.01
Loss of GRX1 increased the sensitivity of neurons to OGD/R-induced injury
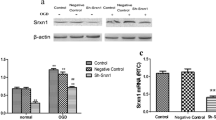
To elucidate the potential function of GRX1 in the regulation of OGD/R-induced injury, loss-of-function experiments involving GRX1 silencing were carried out in HT22 neurons using GRX1-specific siRNA expression. The transfection of GRX1 siRNA markedly depleted GRX1 expression in HT22 neurons in an OGD/R-exposure-independent manner (Fig. 2a–c). HT22 neuron viability, which was significantly impaired by OGD/R exposure, was further decreased by GRX1 knockdown (Fig. 2d). The OGD/R-induced apoptosis of neurons was markedly exacerbated by GRX1 knockdown (Fig. 2e and f). In addition, the loss of GRX1 also enhanced OGD/R-mediated ROS generation (Fig. 2g and h). Therefore, these data reveal that the loss of GRX1 enhances the sensitivity of neurons to OGD/R-induced injury.
GRX1 knockdown exacerbated OGD/R-induced neuronal injury. HT22 neurons were transfected with either negative control (NC) siRNA or GRX1 siRNA for 48 h and subjected to OGD/R exposure. a Relative mRNA expression of GRX1 was examined via RT-qPCR (n = 3). b Protein expression of GRX1 was determined via Western blot, and c the quantification data (n = 3). (D) Cell viability was assessed using a CCK-8 assay (n = 5). e, f Apoptosis was evaluated using an Annexin V-FITC/PI apoptosis assay (n = 3). Data in the Annexin V-FITC+/PI- and Annexin V-FITC+/PI + were quantified. g, h ROS generation was monitored using a ROS detection assay (n = 3). Data were expressed as means ± standard deviation. Differences were assessed by ANOVA followed by Bonferroni’s post-hoc test. **p < 0.01
GRX1 overexpression protects against OGD/R-induced neuronal injury
To verify whether GRX1 has neuroprotective effects on OGD/R-exposed neurons, gain-of-function experiments involving GRX1 overexpression in HT22 neurons were performed. Transfection HT22 neurons with the GRX1 expression vector markedly up-regulated the expression of GRX1 in an OGD/R exposure-independent manner (Fig. 3a and b). Interestingly, the up-regulation of GRX1 restored the viability of OGD/R-exposed neurons (Fig. 3c). Notably, GRX1 up-regulation markedly alleviated OGD/R-induced apoptosis (Fig. 3d and e) and ROS generation (Fig. 3f and g) in HT22 neurons. Collectively, these results reveal that GRX1 has neuroprotective effects on OGD/R-exposed neurons.
GRX1 overexpression ameliorated OGD/R-induced neuronal injury. HT22 neurons were transfected with either an empty vector (EV) or GRX1 expression vector for 48 h and subjected to OGD/R exposure. a Protein expression of GRX1 was determined via Western blot, b the quantification data (n = 3). c Cell viability was determined using a CCK-8 assay (n = 5). d, e Apoptosis was assessed using an Annexin V-FITC/PI apoptosis assay (n = 3). Data in the Annexin V-FITC+/PI− and Annexin V-FITC+/PI+ were quantified. f, g ROS levels were measured using a ROS detection assay (n = 3). Data were expressed as means ± standard deviation. Differences were assessed by ANOVA followed by Bonferroni’s post-hoc test. **p < 0.01
GRX1 overexpression enhanced the activation of Nrf2 antioxidant signaling
To reveal the molecular mechanism responsible for GRX1-mediated neuroprotection, we explored the effect of GRX1 expression on Nrf2 antioxidant signaling. We found that GRX1 knockdown markedly decreased OGD/R-mediated nuclear translocation of Nrf2 in HT22 neurons (Fig. 4a and b). Moreover, GRX1 knockdown down-regulated the transcriptional activity of Nrf2/ARE (Fig. 4c). In contrast, GRX1 overexpression markedly up-regulated the OGD/R-induced nuclear translocation of Nrf2 (Fig. 4d and e) and increased transcriptional activity of Nrf2/ARE (Fig. 4f). These results indicate that GRX1 modulates Nrf2 antioxidant signaling in OGD/R exposed neurons.
GRX1 is involved in the modulation of Nrf2 antioxidant signaling. a The effect of GRX1 knockdown on Nrf2 nuclear expression was assessed via Western blot, and (b) the quantification data (n = 3). c The effect of GRX1 knockdown on Nrf2/ARE transcriptional activity was assessed using a luciferase reporter assay (n = 5). d The effect of GRX1 overexpression on Nrf2 nuclear expression was examined via Western blot, and (e) the quantification data (n = 3). f The effect of GRX1 overexpression on Nrf2/ARE transcriptional activity was assessed using a luciferase reporter assay (n = 5). Data were expressed as means ± standard deviation. Differences were assessed by ANOVA followed by Bonferroni’s post-hoc test. **p < 0.01
GRX1 regulates Nrf2 signaling associated with modulation of GSK-3β phosphorylation
To further explore the molecular basis of GRX1-mediated modulation of Nrf2 signaling, we assessed the effect of activating GSK-3β, a vital regulator of Nrf2. The results showed that GRX1 knockdown markedly decreased GSK-3β phosphorylation, which indicated that GRX1 knockdown enhanced GSK-3β activation (Fig. 5a and b). To confirm whether GSK-3β contributes to the regulation of GRX1 knockdown-induced suppression of Nrf2 signaling, we detected the effect of GSK-3β inhibition on GRX1 knockdown-mediated effects. We utilized SB216763, a chemical inhibitor of GSK-3β (Coghlan et al. 2000), to decrease the activity of GSK-3β. Notably, the inhibition of GSK-3β by SB216763 markedly abolished GRX1 knockdown-induced suppressive effects on Nrf2/ARE activation (Fig. 5c). Furthermore, GSK-3β inhibition reversed the GRX1 knockdown-mediated exacerbation of OGD/R-induced neuronal apoptosis (Fig. 5d and e) and ROS generation (Fig. 5f and g). Taken together, these data suggest that GRX1 regulates Nrf2 activation via the modulation of GSK-3β.
GSK-3β inhibition reversed GRX1 knockdown-mediated modulation of Nrf2 signaling. a The effect of GRX1 knockdown on GSK-3β phosphorylation was determined via Western blot, and (b) the quantification data (n = 3). HT22 neurons were transfected with GRX1 siRNA and incubated for 48 h with or without SB216763 (3 µM), a GSK-3β inhibitor, prior to OGD/R exposure (n = 3). c The effect of GSK-3β inhibition on Nrf2/ARE transcriptional activity was monitored using a luciferase reporter assay (n = 5). d, e The effect of GSK-3β inhibition on neuronal apoptosis was assessed using an Annexin V-FITC/PI apoptosis assay (n = 3). Data in the Annexin V-FITC+/PI− and Annexin V-FITC+/PI+ were quantified. f, g The effect of GSK-3β inhibition on intracellular ROS generation was evaluated using a ROS detection assay (n = 3). Data were expressed as means ± standard deviation. Differences were assessed by ANOVA followed by Bonferroni’s post-hoc test. **p < 0.01
Suppression of Nrf2 reversed GRX1-mediated neuroprotective effect
To verify whether Nrf2 modulates GRX1-mediated neuroprotective effects, we investigated whether Nrf2 inhibition altered GRX1 overexpression-mediated effects on OGD/R-exposed neurons. We utilized ML385, a chemical inhibitor of Nrf2 (Singh et al. 2016), to suppress the activity of Nrf2. The inhibition Nrf2 by ML385 markedly decreased Nrf2/ARE-mediated transcriptional activity and blocked GRX1 overexpression-mediated Nrf2 activation (Fig. 6a). Notably, the suppressive effect of GRX1 overexpression on OGD/R-induced neuronal apoptosis and ROS generation was markedly reversed by Nrf2 inhibition (Fig. 6b and c). Collectively, these results confirm that GRX1 exerts neuroprotective effects against OGD/R-induced injury by enhancing Nrf2 activation.
GRX1 protects against OGD/R-induced neuronal injury via Nrf2. HT22 neurons were transfected with GRX1 expression vectors and incubated for 48 h either with or without ML385 (5 µM), an Nrf2 inhibitor, before OGD/R exposure. a Nrf2/ARE transcriptional activity was monitored using a luciferase reporter assay (n = 5). b Neuronal apoptosis was assessed using an Annexin V-FITC/PI apoptosis assay (n = 3). Data in the Annexin V-FITC+/PI− and Annexin V-FITC+/PI+ were quantified. c Intracellular ROS levels was monitored using ROS detection assay (n = 3). Data were expressed as means ± standard deviation. Differences were assessed by ANOVA followed by Bonferroni’s post-hoc test. **p < 0.01. d A graphical model of GRX1-mediated regulation of Nrf2 activation and its role in the regulation of OGD/R-induced neuronal injury
Discussion
In the present research, we report that GRX1 acts as a pro-survival protein in neurons. Our data showed that GRX1 facilitated neuronal survival under conditions of OGD/R exposure in vitro. The protective effect of GRX1 was associated with the activation of Nrf2 antioxidant signaling. We demonstrated that GRX1 inactivated GSK-3β by increasing GSK-3β phosphorylation, which enhanced the nuclear translocation of Nrf2 and Nrf2/ARE activation. These processes exert anti-apoptotic and anti-oxidant effects on OGD/R-exposed neurons (Fig. 6d). Collectively, these findings indicate that GRX1/GSK-3β/Nrf2 signaling plays a key role in regulating oxidative stress in neurons, which may modulate cerebral ischemia/reperfusion injury in vivo.
GRX1 has previously been reported to have a key role in the regulation of cell survival. The up-regulation of GRX1 protected cardiomyocytes from nitric oxide-induced apoptosis (Inadomi et al. 2012). Moreover, GRX1 protects cardiomyocytes and coronary artery endothelial cells against high glucose level-induced damage (Li et al. 2014; Qi et al. 2016). Notably, GRX1 participates in the modulation of ischemia/reperfusion injury (Godoy et al. 2011). The up-regulation of GRX1 ameliorates adverse ventricular remodeling induced by myocardial ischemia/reperfusion injury (Bubb et al. 2017). Furthermore, GRX1 overexpression attenuates OGD-induced injury in kidney epithelial cells in vitro, indicating the protective role of GRX1 in kidney ischemia (Yin et al. 2019). Interestingly, in this study, we determined that the loss of GRX1 enhanced OGD/R-induced apoptosis in neurons, while GRX1 overexpression protected neurons from OGD/R-induced apoptosis. In accordance with previous findings, our study confirms a cytoprotective role for GRX1, and suggests that GRX1 may participate in the regulation of cerebral ischemia/reperfusion injury. Interestingly, a recent study reported that GRX2, another member of the GRX protein family, is also capable of preventing OGD/R-induced apoptosis in neurons (Wen et al. 2020), indicating that the GRX protein family may have critical roles in cerebral ischemia/reperfusion injury. GRX1 and GRX2 have a significant Cys-X-X-Cys active site motif and these two cysteine residues act as redox sensors and allow for a monothiol mechanism using the N-terminal cysteine to reduce the reduced sulfhydryl groups of the cysteines of proteins (Holmgren 1979; Lundberg et al. 2001). However, these two protein have different cellular localizations (Holmgren 1979; Lundberg et al. 2001). These two proteins have shown similar effects on OGD/R injury of neurons. However, whether these proteins functions interactively in mediating OGD/R injury is unknown. Therefore, further studies should be performed to determine their specific different roles in mediating OGD/R injury of neurons.
Emerging evidence has revealed that GRX1 has a notable neuroprotective function (Johnson et al. 2015). It has been reported that GRX1 mRNA and protein expression are both up-regulated in mouse brain cells in response to chemical insult (Kenchappa and Ravindranath 2003). The treatment of neurons with 6-hydroxydopamine significantly enhanced GRX1 expression, and GRX1 knockdown exacerbated 6-hydroxydopamine-induced cytotoxic effects (Arodin et al. 2014). The up-regulation of GRX1 protected neurons from MPTP- or copper-induced apoptosis (Kenchappa et al. 2004; Cater et al. 2014). These findings indicate that GRX1 is induced in response to stress in neurons. Consistent with these findings, our results demonstrated that GRX1 was induced by OGD/R exposure in HT22 neurons and GRX1 overexpression protected against OGD/R-induced neuronal injury. Therefore, our study confirms that GRX1 is essential for neuronal survival and may participate in the modulation of ischemia/reperfusion-induced neuronal injury.
GRX1 confers resistance to oxidative stress. The up-regulation of GRX1 attenuates oxidative stress injury induced by hydrogen peroxide in retinal pigment epithelial cells (Liu et al. 2015, 2016). The steady laminar flow-induction of GRX1 protected endothelial cells from oxidative stress-induced apoptosis (Li et al. 2017). Moreover, GRX1 overexpression alleviated oxidative stress and apoptosis in osteoarthritic chondrocytes (Sun et al. 2017). Therefore, GRX1 functions as a potent antioxidant protein. Considering that OGD/R-evoked oxidative stress contributes to neuronal injury, we evaluated whether GRX1 was involved in regulating OGD/R-mediated oxidative stress in neurons. Herein, we found that the loss of GRX1 enhanced OGD/R-induced ROS production, while GRX1 overexpression suppressed ROS production in OGD/R-exposed neurons. Our findings suggest that GRX1 also participates in the regulation of OGD/R-associated oxidative stress in neurons and may serve as a promising target for neuroprotective therapy.
It has been reported that GRX1 regulates cell survival by affecting multiple signaling pathways (Li et al. 2017; Sun et al. 2017). It has been reported that GRX1 prevents the myocardial ischemia/reperfusion-induced reduction of cardioprotective proteins including Akt and HO-1(Lekli et al. 2010), which are key mediators in Nrf2 signaling. In this study, we identified GRX1 as a novel regulator of Nrf2 antioxidant signaling. Our data showed that GRX1 promoted Nrf2 activation through the inactivation of GSK-3β. The phosphorylation of GSK-3β by Akt inactivates GSK-3β (Golpich et al. 2015; Lee et al. 2020). Interestingly, GRX1 has been reported to be a critical regulator of Akt. GRX1 can prevent the oxidative modification of Akt, which leads to increased Akt phosphorylation (Ahmad et al. 2014; Liu et al. 2015). However, whether GRX1 regulates GSK-3β/Nrf2 axis via Akt requires further investigation. Nevertheless, our work showed that GRX1 may contribute to Nrf2 activation through the inactivation of GSK-3β.
Certain limitations of this work should be noted. The effects of GRX1 were mainly investigated in vitro using a cellular model. However, the precise effects of GRX1 in vivo are unknown. Therefore, further investigation using animal models of cerebral ischemia/reperfusion injury is required. It would be better to see the in vivo effects of GRX1 overexpression by virus vector mediated gene transfer on cerebral ischemia/reperfusion-induced infarct size, neurological dysfunction, neuronal apoptosis and oxidative stress in rodent models. Only through these studies can the neuroprotective effect of GRX1 in cerebral ischemia/reperfusion injury be further confirmed.
In conclusion, our data demonstrate that GRX1 is induced by OGD/R exposure in neurons and that the up-regulation of GRX1 alleviates OGD/R-induced neuronal apoptosis and oxidative stress by enhancing the activation of Nrf2/ARE. Moreover, we revealed that GRX1 contributes to Nrf2/ARE activation via the inactivation of GSK-3β. Thus, our study suggests that GRX1 is a novel regulator of the GSK-3β/Nrf2 axis and suggests that the GRX1/GSK-3β/Nrf2 axis may represent a novel mechanism modulating the oxidative stress response induced by cerebral ischemia/reperfusion injury.
Data availability
The data and material used to support the findings of this study are available from the corresponding author upon request.
Code availability
Not applicable.
References
Ahmad F, Nidadavolu P, Durgadoss L, Ravindranath V (2014) Critical cysteines in Akt1 regulate its activity and proteasomal degradation: implications for neurodegenerative diseases. Free Radic Biol Med 74:118–128
Allen EM, Mieyal JJ (2012) Protein-thiol oxidation and cell death: regulatory role of glutaredoxins. Antioxid Redox Signal 17:1748–1763
Arodin L, Miranda-Vizuete A, Swoboda P, Fernandes AP (2014) Protective effects of the thioredoxin and glutaredoxin systems in dopamine-induced cell death. Free Radic Biol Med 73:328–336
Bao H, Gao M (2020) Overexpression of lemur tyrosine kinase-2 protects neurons from oxygen-glucose deprivation/reoxygenation-induced injury through reinforcement of Nrf2 signaling by modulating GSK-3beta phosphorylation. Biochem Biophys Res Commun 521:964–970
Benjamin EJ, Virani SS, Callaway CW, Chamberlain AM, Chang AR, Cheng S, Chiuve SE, Cushman M, Delling FN, Deo R, de Ferranti SD, Ferguson JF, Fornage M, Gillespie C, Isasi CR, Jimenez MC, Jordan LC, Judd SE, Lackland D, Lichtman JH, Lisabeth L, Liu S, Longenecker CT, Lutsey PL, Mackey JS, Matchar DB, Matsushita K, Mussolino ME, Nasir K, O’Flaherty M, Palaniappan LP, Pandey A, Pandey DK, Reeves MJ, Ritchey MD, Rodriguez CJ, Roth GA, Rosamond WD, Sampson UKA, Satou GM, Shah SH, Spartano NL, Tirschwell DL, Tsao CW, Voeks JH, Willey JZ, Wilkins JT, Wu JH, Alger HM, Wong SS, Muntner P (2018) Heart disease and stroke statistics-2018 update: a report from the American Heart Association. Circulation 137:e67–e492
Bubb KJ, Kok C, Tang O, Rasko NB, Birgisdottir AB, Hansen T, Ritchie R, Bhindi R, Reisman SA, Meyer C, Ward K, Karimi Galougahi K, Figtree GA (2017) The NRF2 activator DH404 attenuates adverse ventricular remodeling post-myocardial infarction by modifying redox signalling. Free Radic Biol Med 108:585–594
Burns M, Rizvi SHM, Tsukahara Y, Pimentel DR, Luptak I, Hamburg NM, Matsui R, Bachschmid MM (2020) Role of Glutaredoxin-1 and Glutathionylation in cardiovascular diseases. Int J Mol Sci 21:6803
Cai L, Li Y, Zhang Q, Sun H, Yan X, Hua T, Zhu Q, Xu H, Fu H (2017) Salidroside protects rat liver against ischemia/reperfusion injury by regulating the GSK-3beta/Nrf2-dependent antioxidant response and mitochondrial permeability transition. Eur J Pharmacol 806:32–42
Cater MA, Materia S, Xiao Z, Wolyniec K, Ackland SM, Yap YW, Cheung NS, La Fontaine S (2014) Glutaredoxin1 protects neuronal cells from copper-induced toxicity. Biometals 27:661–672
Chen X, Lv Q, Hong Y, Chen X, Cheng B, Wu T (2017) IL-1beta maintains the redox balance by regulating glutaredoxin 1 expression during oral carcinogenesis. J Oral Pathol Med 46:332–339
Coghlan MP, Culbert AA, Cross DA, Corcoran SL, Yates JW, Pearce NJ, Rausch OL, Murphy GJ, Carter PS, Roxbee Cox L, Mills D, Brown MJ, Haigh D, Ward RW, Smith DG, Murray KJ, Reith AD, Holder JC (2000) Selective small molecule inhibitors of glycogen synthase kinase-3 modulate glycogen metabolism and gene transcription. Chem Biol 7:793–803
Cuadrado A (2015) Structural and functional characterization of Nrf2 degradation by glycogen synthase kinase 3/beta-TrCP. Free Radic Biol Med 88:147–157
Godoy JR, Oesteritz S, Hanschmann EM, Ockenga W, Ackermann W, Lillig CH (2011) Segment-specific overexpression of redoxins after renal ischemia and reperfusion: protective roles of glutaredoxin 2, peroxiredoxin 3, and peroxiredoxin 6. Free Radic Biol Med 51:552–561
Golpich M, Amini E, Hemmati F, Ibrahim NM, Rahmani B, Mohamed Z, Raymond AA, Dargahi L, Ghasemi R, Ahmadiani A (2015) Glycogen synthase kinase-3 beta (GSK-3beta) signaling: Implications for Parkinson’s disease. Pharmacol Res 97:16–26
Gravina SA, Mieyal JJ (1993) Thioltransferase is a specific glutathionyl mixed disulfide oxidoreductase. Biochemistry 32:3368–3376
Holmgren A (1979) Glutathione-dependent synthesis of deoxyribonucleotides. Characterization of the enzymatic mechanism of Escherichia coli glutaredoxin. J Biol Chem 254:3672–3678
Inadomi C, Murata H, Ihara Y, Goto S, Urata Y, Yodoi J, Kondo T, Sumikawa K (2012) Overexpression of glutaredoxin protects cardiomyocytes against nitric oxide-induced apoptosis with suppressing the S-nitrosylation of proteins and nuclear translocation of GAPDH. Biochem Biophys Res Commun 425:656–661
Itoh K, Chiba T, Takahashi S, Ishii T, Igarashi K, Katoh Y, Oyake T, Hayashi N, Satoh K, Hatayama I, Yamamoto M, Nabeshima Y (1997) An Nrf2/small Maf heterodimer mediates the induction of phase II detoxifying enzyme genes through antioxidant response elements. Biochem Biophys Res Commun 236:313–322
Johnson WM, Wilson-Delfosse AL, Chen SG, Mieyal JJ (2015) The roles of redox enzymes in Parkinson’s disease: Focus on glutaredoxin. Ther Targets Neurol Dis 2:e790
Kenchappa RS, Ravindranath V (2003) Glutaredoxin is essential for maintenance of brain mitochondrial complex I: studies with MPTP. FASEB J 17:717–719
Kenchappa RS, Diwakar L, Annepu J, Ravindranath V (2004) Estrogen and neuroprotection: higher constitutive expression of glutaredoxin in female mice offers protection against MPTP-mediated neurodegeneration. FASEB J 18:1102–1104
Kensler TW, Wakabayashi N, Biswal S (2007) Cell survival responses to environmental stresses via the Keap1-Nrf2-ARE pathway. Annu Rev Pharmacol Toxicol 47:89–116
Lee MJ, Jin N, Grandis JR, Johnson DE (2020) Alterations and molecular targeting of the GSK-3 regulator, PI3K, in head and neck cancer. Biochim Biophys Acta Mol Cell Res 1867:118679
Lekli I, Mukherjee S, Ray D, Gurusamy N, Kim YH, Tosaki A, Engelman RM, Ho YS, Das DK (2010) Functional recovery of diabetic mouse hearts by glutaredoxin-1 gene therapy: role of Akt-FoxO-signaling network. Gene Ther 17:478–485
Li S, Sun Y, Qi X, Shi Y, Gao H, Wu Q, Liu X, Yu H, Zhang C (2014) Protective effect and mechanism of glutaredoxin 1 on coronary arteries endothelial cells damage induced by high glucose. Biomed Mater Eng 24:3897–3903
Li Y, Ren M, Wang X, Cui X, Zhao H, Zhao C, Zhou J, Guo Y, Hu Y, Yan C, Berk B, Wang J (2017) Glutaredoxin 1 mediates the protective effect of steady laminar flow on endothelial cells against oxidative stress-induced apoptosis via inhibiting Bim. Sci Rep 7:15539
Liu X, Jann J, Xavier C, Wu H (2015) Glutaredoxin 1 (Grx1) protects human retinal pigment epithelial cells from oxidative damage by preventing AKT glutathionylation. Invest Ophthalmol Vis Sci 56:2821–2832
Liu X, Xavier C, Jann J, Wu H (2016) Salvianolic acid B (Sal B) protects retinal pigment epithelial cells from oxidative stress-induced cell death by activating Glutaredoxin 1 (Grx1). Int J Mol Sci 17:15539
Liu X, Li M, Hou M, Huang W, Song J (2018) MicroRNA-135a alleviates oxygen-glucose deprivation and reoxygenation-induced injury in neurons through regulation of GSK-3beta/Nrf2 signaling. J Biochem Mol Toxicol 32:e22159
Lo EH, Dalkara T, Moskowitz MA (2003) Mechanisms, challenges and opportunities in stroke. Nat Rev Neurosci 4:399–415
Lundberg M, Johansson C, Chandra J, Enoksson M, Jacobsson G, Ljung J, Johansson M, Holmgren A (2001) Cloning and expression of a novel human glutaredoxin (Grx2) with mitochondrial and nuclear isoforms. J Biol Chem 276:26269–26275
Ma Q, He X (2012) Molecular basis of electrophilic and oxidative defense: promises and perils of Nrf2. Pharmacol Rev 64:1055–1081
Madusanka RK, Tharuka MDN, Liyanage DS, Sirisena D, Lee J (2020) Role of rockfish (Sebastes schlegelii) glutaredoxin 1 in innate immunity, and alleviation of cellular oxidative stress: Insights into localization, molecular characteristics, transcription, and function. Comp Biochem Physiol B Biochem Mol Biol 243–244:110432
Park SY, Choi YW, Park G (2018) Nrf2-mediated neuroprotection against oxygen-glucose deprivation/reperfusion injury by emodin via AMPK-dependent inhibition of GSK-3beta. J Pharm Pharmacol 70:525–535
Qi X, Xu A, Gao Y, Shi Y, Sun X, Xu J, Liu J, Lan Q, Chang L, Zhang C, Yu H (2016) Cardiac damage and dysfunction in diabetic cardiomyopathy are ameliorated by Grx1. Genet Mol Res 15:3
Rada P, Rojo AI, Evrard-Todeschi N, Innamorato NG, Cotte A, Jaworski T, Tobon-Velasco JC, Devijver H, Garcia-Mayoral MF, Van Leuven F, Hayes JD, Bertho G, Cuadrado A (2012) Structural and functional characterization of Nrf2 degradation by the glycogen synthase kinase 3/beta-TrCP axis. Mol Cell Biol 32:3486–3499
Rana AK, Singh D (2018) Targeting glycogen synthase kinase-3 for oxidative stress and neuroinflammation: Opportunities, challenges and future directions for cerebral stroke management. Neuropharmacology 139:124–136
Saito A, Maier CM, Narasimhan P, Nishi T, Song YS, Yu F, Liu J, Lee YS, Nito C, Kamada H, Dodd RL, Hsieh LB, Hassid B, Kim EE, Gonzalez M, Chan PH (2005) Oxidative stress and neuronal death/survival signaling in cerebral ischemia. Mol Neurobiol 31:105–116
Silva-Islas CA, Maldonado PD (2018) Canonical and non-canonical mechanisms of Nrf2 activation. Pharmacol Res 134:92–99
Singh A, Venkannagari S, Oh KH, Zhang YQ, Rohde JM, Liu L, Nimmagadda S, Sudini K, Brimacombe KR, Gajghate S, Ma J, Wang A, Xu X, Shahane SA, Xia M, Woo J, Mensah GA, Wang Z, Ferrer M, Gabrielson E, Li Z, Rastinejad F, Shen M, Boxer MB, Biswal S (2016) Small molecule inhibitor of NRF2 selectively intervenes therapeutic resistance in KEAP1-deficient NSCLC tumors. ACS Chem Biol 11:3214–3225
Sun J, Wei X, Lu Y, Cui M, Li F, Lu J, Liu Y, Zhang X (2017) Glutaredoxin 1 (GRX1) inhibits oxidative stress and apoptosis of chondrocytes by regulating CREB/HO-1 in osteoarthritis. Mol Immunol 90:211–218
Wen J, Li X, Zheng S, Xiao Y (2020) Upregulation of Glutaredoxin 2 alleviates oxygen-glucose deprivation/reoxygenation-induced apoptosis and ROS production in neurons by enhancing Nrf2 signaling via modulation of GSK-3beta. Brain Res 1745:146946
Yang F, Yi M, Liu Y, Wang Q, Hu Y, Deng H (2018) Glutaredoxin-1 silencing induces cell senescence via p53/p21/p16 signaling axis. J Proteome Res 17:1091–1100
Yin J, Xu R, Wei J, Zhang S (2019) The protective effect of glutaredoxin 1/DJ-1/HSP70 signaling in renal tubular epithelial cells injury induced by ischemia. Life Sci 223:88–94
Zhao T, Zhang-Akiyama QM (2020) Deficiency of Grx1 leads to high sensitivity of HeLaS3 cells to oxidative stress via excessive accumulation of intracellular oxidants including ROS. Free Radic Res 54:585–605
Zhu J, Li X, Qi H, Gu Z, Song S, Yang X, Zhou G, Li C (2017) Oxidative and anti-oxidative status in muscle of young rats in response to six protein diets. Sci Rep 7:13184
Author information
Authors and Affiliations
Contributions
Zhengguo Qiu designed the work, performed the experiment, and drafted the article. Xu Li performed the experiment. Chongzhen Duan collected the data. Rui Li collected the data. Lifeng Ha designed the work and reviewed the article. The authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflicts of interest
The authors declare no conflict of interest.
Ethics approval
Not applicable.
Consent to participate
Not applicable.
Consent for publication
All authors have approved for the publication of this manuscript.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Qiu, Z., Li, X., Duan, C. et al. Glutaredoxin 1 protects neurons from oxygen‐glucose deprivation/reoxygenation (OGD/R)-induced apoptosis and oxidative stress via the modulation of GSK-3β/Nrf2 signaling. J Bioenerg Biomembr 53, 369–379 (2021). https://doi.org/10.1007/s10863-021-09898-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10863-021-09898-0