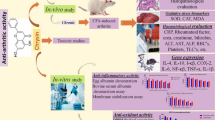
Abstract
Methyl gallate (MG) is a plant-derived phenolic compound known to present remarkable anti-inflammatory effect in different experimental models, such as paw oedema, pleurisy, zymosan-induced arthritis and colitis. Herein we investigated the effect of MG in the mice model of antigen-induced arthritis (AIA), a model with complex inflammatory response, driven primally by immune process and that cause bone and cartilage erosion similarly found in rheumatoid arthritis. Arthritis was induced by intra-articular injection of albumin methylated from bovine serum (mBSA) in C57BL/6 male mice previously immunized. The dose–response analysis of MG (0.7–70 mg/kg; p.o) showed that maximum inhibition was reached with the dose of 7 mg/kg on paw oedema and cell infiltration induced by AIA at 7 h. Treatment with MG (7 mg/kg; p.o) or with the positive control, dexamethasone (Dexa, 10 mg/kg, ip) reduced AIA oedema formation, leukocyte infiltration, release of extracellular DNA and cytokine production 7 and 24 h (acute response). Mice treated daily with MG for 7 days showed no significant weight loss or liver and kidney toxicity contrary to dexamethasone that induced some degree of toxicity. Prolonged treatment with MG inhibited the late inflammatory response (28 days) reducing oedema formation, cell infiltration, synovial hyperplasia, pannus formation and cartilage degradation as observed in histopathological analyses. Ultimately, MG reduced bone resorption as evidenced by a decrease in tartrate-resistant acid phosphate (TRAP)-positive cells number in femur histology. Altogether, we demonstrate that MG ameliorates the inflammatory reaction driven primarily by the immune process, suggesting a potential therapeutic application in arthritis treatment.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Rheumatoid arthritis (RA) is a systemic autoimmune disease characterized by chronic synovial inflammation, which can promote progressive cartilage and bone damage (Smolen et al. 2018; Giannini et al. 2020), ultimately leading to substantial disability in RA patients (Fardellone et al. 2020).
Pro-inflammatory mediators are released in the synovial compartment by resident and infiltrated cells, playing a crucial role in arthritis pathogenesis. Cytokines, including tumor necrosis factor-α (TNF-α), interleukin (IL)-1β, IL-6, IL-17, and IL-23, increase the recruitment of neutrophils into the joint and trigger chemokines release and degradative enzymes production (Brennan and McInnes 2008; Cecchi et al. 2018). Moreover, this pro-inflammatory milieu leads to an increase of macrophage colony-stimulating factor (M-CSF) levels and receptor activator of nuclear factor-κB ligand (RANKL) expression, which stimulates the differentiation and activity of osteoclasts, promoting cartilage destruction and bone erosion (Karmakar et al. 2010; Llorente et al. 2020).
The current therapy for RA includes non-steroidal anti-inflammatory drugs, disease-modifying anti-rheumatic drugs (DMARDs) of synthetic and of biological origin (Burmester and Pope 2017). However, traditional DMARDs such as glucocorticoids and methotrexate frequently present side-effects such as cytopenia, transaminase elevation, and poor tolerability. There are biological DMARDs that target tumour necrosis factor, IL-6 or IL-6 receptor, co-stimulatory molecules CD80 and CD86 or the molecule CD20, expressed in B cells. These drugs are usually administered in association with MTX but still, there is a high rate of unresponsive patients (Smolen et al. 2018). More recently, medications that suppress the Janus kinase (JAK) pathways have shown noticeable effects as RA treatments. Nevertheless, the JAK inhibitors, also often cause gastrointestinal side-effects, lymphopenia, neutropenia, elevated cholesterol, and more infections (Burmester and Pope 2017). Therefore, the investigation of alternatives to treat RA is still relevant. In the last decade studies have been trying to identify complementary therapies for RA from natural products with low toxicity (Sung et al. 2019). Polyphenols is one of the major classes of natural products that have been studied in this context. They are plant secondary metabolites and numerous studies have shown that polyphenol-rich diets exert cardioprotective, anti-cancer, anti-diabetic anti-inflammatory and anti-aging effects (Pandey and Rizvi 2009).
Methyl gallate (MG; Fig. 1) is a phenolic compound found in medicinal and food plants, such as Schinus terebinthifolius, Galla Rhois, Rosa rugosa e Givotia rottleriformis Griff. (Cho et al. 2004; Kang et al. 2009; Kamatham et al. 2015; Rosas et al. 2015), which presents pharmacological properties, such as antioxidant (Huang et al. 2021), antitumor (Lee et al. 2013), antimicrobial (Acharyya et al. 2015) and anti-inflammatory (Chae et al. 2010). MG attenuates osteoclastic differentiation in vitro and reduces the bone loss induced by lipopolysaccharide in mice (Baek et al. 2017). MG presented a potent anti-inflammatory effect inhibiting paw oedema, hyperalgesia and articular inflammation induced by the zymosan by decreasing cell accumulation and inflammatory mediators (Correa et al. 2016, 2020). This effect was associated with the modulation of NF-κB signaling and MAPK pathway triggered by TLRs (Correa et al. 2020). However, these studies have several limitations and are less representative of RA processes.
This study aimed to investigate a potential therapeutic effect of MG in mice under antigen-induced arthritis (AIA), a model with a complex inflammatory response, driven primally by immune process and that cause extensive bone and cartilage erosion similarly to the reaction found in rheumatoid arthritis.
Materials and methods
Animals
The experiments were performed in male C57BL/6 mice weighing between 20 and 25 g from the Science and Technology in Biomodel Institute (Fiocruz, Rio de Janeiro, Brazil). Mice were kept with free access to food and fresh water in a room with temperatures ranging from 22 to 24 °C and a 12-h light/dark cycle. All animal care and experimental procedures performed were approved by the institution's Committee of Ethics in Animal Care and Use (CEUA) (registered under the number CEUA LW-43/14).
Treatments
Animals were fasted overnight and then received oral administration (p.o.) of MG (98% purity; purchased from Fluka-Sigma-Aldrich) in doses ranging from 0.7 to 70 mg/kg diluted in filtered water in a final volume of 200 µL, 1 h before mBSA (albumin methylated from bovine serum; Sigma-Aldrich, St. Louis, MO, USA). The dose range was based on previous results on paw and articular oedema induced by zymosan published before (Correa et al. 2016, 2020). Dexamethasone (10 mg/kg, 100 µL) was administered intraperitoneally (i.p.) 1 h before stimulation and used as a positive control as described before (Correa et al. 2016). The same volume of water (200 μL) was administered orally to the control groups.
In another set of experiments, mice were treated daily with MG (7 mg/kg; p.o.) or dexamethasone (10 mg/kg; i.p.) for seven consecutive days. Treatment started on day 21, 1 h before mBSA challenge and was administered daily until day 28 when animals were euthanized.
Induction of experimental arthritis—antigen-induced arthritis
Mice were immunized as described previously (Oliveira et al. 2011; Kanashiro et al. 2016). C57BL/6 male mice were immunized with 500 µg of mBSA in 0.2 mL of an emulsion containing 0.1 mL phosphate-buffered saline (PBS) and 0.1 mL complete Freund's adjuvant (CFA; Sigma-Aldrich) by subcutaneous (s.c.) route at day 0. Booster injection of mBSA was given 7 days after the first immunization. On days 21 and 25, mice were challenged by intra-articular (i.a.) injection of mBSA (30 µg/cavity) or sterile saline (immunized saline group; [sal]) through the patellar ligament into the knee joint with an insulin syringe (BD Ultra-Fine). This protocol was used to prolong knee inflammation and to induce proteoglycan degradation. Non-immunized (NI) mice were given similar injections but without the antigen (mBSA) during the immunization process and challenged in the knee joint with mBSA (Fig. 2).
Immunoglobulins (IgG) specific for the antigen mBSA were determined in serum, obtained at 24 h of mBSA challenge (day 21) by ELISA. The serum levels of anti-mBSA specific total IgG antibodies were significantly higher in immunized mice than in non-immunized control mice (Supplemental Fig. 1).
Knee joint oedema evaluation
Articular oedema of the tibiofemoral joint was evaluated by measuring the transverse diameters of each knee joint with a digital caliper (Digmatic Caliper, Mitsutoyo Corporation, Japan) at different timepoints after challenge with mBSA. Values of knee joint thickness are expressed as the difference (Δ) between the diameters measured before (basal) and after the induction of articular inflammation in millimeters (mm).
Determination of joint leukocyte infiltration
Knee synovial cavities were washed twice with 150 µL of PBS containing EDTA (10 mM) by inserting a 21 G needle into mouse knee joints, and the synovial washes were recovered by aspiration. Total leukocyte counts were performed in an automatic particle counter Z2 (Coulter Z2, Beckman Coulter Inc., Brea, CA, USA). Differential counts of leucocytes were performed using May–Grunwald–Giemsa-stained cytospin smears (Cytospin 3, Shandon Inc., Pittsburgh, PA, USA), and the values are reported as the number of cells per cavity (× 105). After cellular counts, the synovial washes were centrifuged at 400× g for 10 min at 4 °C, and the supernatant was stored at −80 °C for further analysis.
Histological analysis
Whole knee joints obtained from C57BL/6 mice 7 days after i.a. administration of mBSA or saline were removed, dissected, and fixed in 10% formalin for 48 h. After that, the knees were kept in 10% EDTA in PBS solution for 2–3 weeks for decalcification. Tissue sections (5 µm) were stained with hematoxylin and eosin (H&E) or safranin O/fast green, mounted on permanent glass slides, and analyzed under an optical microscope (Olympus BX41, Olympus, Japan). To assess pathological changes in the synovial cavity, images were taken at 100 × and 200 × magnification to allow the visualization of the entire area of the synovial cavity. The following parameters were subjectively graded: synovial hyperplasia (pannus formation; from 0 = no hyperplasia to 3 = most severe hyperplasia); synovial infiltrate (from 0 = no inflammation to 3 = most severe inflammation), bleeding (from 0 = no bleeding to 3 = most severe bleeding). The safranin-O/fast green staining was used to assess cartilage protein loss, suggesting cartilage degradation, and was also included in the assessment (from 0 = no cartilage degradation to 3 = severe cartilage degradation). Scores for all parameters were subsequently summed to give an arthritis index (AI; expressed as the mean ± SEM).
Cytokine and chemokine measurements (ELISA)
Levels of IL-17, CCL-2, and CCL-3 were quantified in the knee joint washes, and TNF-α concentration was quantified in the tissue joint at 7 h after injection of mBSA. Briefly, joints were dissected out, frozen with liquid nitrogen, crushed in a mortar and pestle, then were homogenized in 500 µL of the appropriate buffer containing a cocktail of protease inhibitors (Sigma-Aldrich), centrifuged and the supernatants were used to determine TNF-α levels. According to the manufacturer's instructions, cytokines were measured using standard sandwich ELISA using matched antibody pairs (Quantikine, R&D Systems, Minneapolis, MN, USA). The results are expressed as picograms of each cytokine or chemokine per milliliter (pg/mL) or per mg of tissue.
Measurement of extracellular dsDNA
Synovial fluids from animals subjected to AIA were collected 7 and 24 h after i.a. challenge with mBSA. The washings were centrifuged to remove cells and 50 µL of the supernatant was added to 50 µL of Quanti-it ™ PicoGreen® dsDNA Assay kit (Thermo Fisher Scientific, Waltham, USA), and the reding determined at 485/538 nm emission/excitation according to (Gardinassi et al. 2017). The results were expressed in arbitrary units (AU).
Assess of acute oral toxicity of MG
To assess the potential toxic of MG, healthy mice were treated for 14 consecutive days with different concentrations of MG (5, 50, 300 and 1000 mg/kg) accordingly to OECD guideline 420. After oral administration, the animals were followed for 14 days to assess the following aspects: food intake, clinical signs (assessed daily) and assessment of body weight. The organs evaluated were: kidneys, liver, heart and spleen. The absolute weight was recorded from the direct weighing of each organ, and the relative weight was obtained by calculating the absolute weight of the organ divided by the animal weight, to obtain the proportion of organ weight (g) per gram of body weight. For the hematological and biochemical evaluation, abdominal aortic puncture was performed and samples were processed according to the manufacturer's instructions. The tests were performed using the dry chemistry methodology using the Vitros 250 equipment (Ortho clinical; Jonhson & Jonhson) and pocH-100iV Diff equipment (Sysmex Corporation) for hematological evaluation.
Evaluation of plasma enzyme activities after prolonged treatment with MG
Mice were treated daily with MG (7 mg/kg; p.o.) or dexamethasone (10 mg/kg; i.p.) for seven consecutive days. Treatment started on day 21, 1 h before mBSA challenge and was administered daily until day 28. Blood samples were collected by cardiac puncture (day 28) and added into microtubes containing anticoagulant (Heparin; Sigma-Aldrich) to determine enzymatic activities of aspartate aminotransferase (AST) and alanine aminotransferase (ALT) as indicators of hepatotoxicity and urea and creatinine kinase levels as indicators of nephrotoxicity. Plasma was separated by centrifugation (200× g, 10 min, 4 °C), samples processed according to the manufacturer's instructions and the tests were performed using the Vitros 250 equipment. Results were presented as U/mL (AST and ALT) and mg/dL (urea and creatinine kinase) of plasma. Bodyweight was monitored throughout the experiment from day 0 to 28.
Histochemical staining for TRAP
Sections of knee joints obtained from C57BL/6 mice at 7 days after i.a. mBSA administration were stained according to tartrate-resistant acid phosphate (TRAP) kit 387A (Sigma-Aldrich, St. Louis, MO, USA). TRAP was used as a histochemical marker of osteoclasts in 5 µm sections (Ballanti et al. 1997) and TRAP-positive cells appeared as dark purple. Osteoclasts were identified as TRAP-positive multinucleated cells and counted in the joint growth area (femur). The result was expressed as the number of TRAP-positive cells.
Osteoclast culture and in vitro TRAP analysis
Bone marrow cells (BMCs) from 8-week-old male C57BL/6 mice were obtained by flushing tibias and femurs with α-MEM (Thermo Fisher Scientific, Waltham, MA, USA) supplemented with 10% FBS, penicillin (100 U/mL), and streptomycin (100 µg/mL). Cells were transferred to 10 cm Petri dishes and then cultured in the presence of M-CSF (30 ng/mL; R&D Systems, Minneapolis, MN, USA) for 3 days. After that, floating cells were discarded, and the adhering cells were classified as BMMs (bone marrow macrophages). To generate osteoclasts, BMMs were cultured in 96-well plates (2 × 104 cells/well) at 37 °C/5% CO2 in the presence of osteoclastic media, which consists of M-CSF (30 ng/mL) and RANKL (10 ng/mL), with different concentrations of methyl gallate (0, 3, 10, 30 µM). After 3 days, the cells were stained according to TRAP kit 387A (Sigma-Aldrich, St. Louis, MO, USA). TRAP-positive multinucleated cells with more than three nuclei were identified as osteoclasts. Mature osteoclasts were counted and represented as multinucleated TRAP+ cells/well. To determine the osteoclast area, we analyzed the images using ImageJ software.
Cell viability
BMMs were seeded in 96-well plates (2 × 104 cells/well) and cultured with osteoclastic media and different concentrations of MG (0, 3, 10, 30 e 100 µM) as described above. On the third day, 5 mg/mL MTT solution (22.5 µL) was added to each well. After 3 h, the plate was centrifuged (200× g/5 min), the medium was removed, and DMSO (150 µL) was added to dissolve the formazan dye. The optical density (OD) was measured at 570 nm using a microplate reader. The mean OD of the control group (RANKL) was set as 100%, and the experimental groups were compared to RANKL.
RNA extraction and qRT-PCR
BMMs were seeded in 24-well plates (2 × 105 cells/well) and cultured with osteoclastic media and MG (30 µM) for 48 h. Total RNA was isolated from cell culture using the SV Total Isolation System kit (Promega) and quantified using NanoDrop with an A260/280 ratio of 1.9–2.1. Complementary DNA was synthesized using the High-Capacity synthesis kit (Applied Biosystems, Life Technologies, Carlsbad, CA, USA). Quantitative PCR (qPCR) was performed on a StepOnePlus system (Applied Biosystems, Carlsbad, CA, USA) using a predesigned TaqMan Universal master mix II (Applied Biosystems). The relative levels of mRNA expression were determined by the 2−∆∆ cycle threshold (2−∆∆CT) method using glyceraldehyde 3-phosphate dehydrogenase (GAPDH) as an endogenous control (reference gene). Specific primers for nuclear factor of activated T cells, calcineurin-dependent (Nfatc1; Mm00479445_m1), tartrate-resistant acid phosphatase (Trap/ACp5; Mm00475698_m1), integrin-β 3 (Itgb3; Mm00443980_m1), calcitonin receptor (CTR; Mm00432282_m1) and GAPDH (Mm99999915_g1) genes were employed (TaqMan® Gene Expression Assay). The graphs show the relative expression of the gene of interest normalized to the control population (RANKL).
Statistical analyses
In all experiments, values are expressed as means ± SEM. Differences between groups were tested for significance by one-way ANOVA followed by Tukey multiple comparison tests using GraphPad Prism 5 software. A p value of ≤ 0.05 was considered significant.
Results
Dose–response analysis of methyl gallate on oedema and cellular influx in the antigen-induced arthritis model
We investigated the anti-inflammatory effects of methyl gallate (MG) in a well-established model of antigen-induced arthritis (AIA) in mice, which involves adaptive immunity to generate the acute inflammatory response (Asquith et al. 2009; Benson et al. 2018).
Pretreatment with MG inhibit antigen-induced oedema formation at doses of 7 and 70 mg/kg, whereas no effect was observed for pretreatment with MG at 0.7 mg/kg (Fig. 3A). As shown in Fig. 3B–D, only the dose of 7 mg/kg inhibited significantly total leukocyte recruitment from 1.065 ± 0.093 to 0.628 ± 0.095 × 105 cells/cavity. Considering these results, further analysis was performed using a dose of 7 mg/kg.
Dose–response analysis for MG on antigen-induced arthritis. A–D Mice were treated with MG (0.7–70 mg/kg) orally 1 h before i.a. injection of mBSA (30 µg/25 µL). Control group was injected with the same volume of sterile saline. Knee joint diameter was evaluated with a digital caliper (A). The numbers of total leukocytes (B), neutrophils (C), and mononuclear cells (D) in the synovial cavity were assessed 7 h after mBSA challenge. The results are presented as the means ± SEM of seven mice per group [*p ≤ 0.05 compared to the vehicle group; +p ≤ 0.05 compared to the immunized mBSA group; #p ≤ 0.05 compared different doses of MG (one-way ANOVA followed by Tukey test)]
Methyl gallate inhibits acute articular inflammatory response in AIA model
The antigen injection in the knee joints of immunized C57BL/6 mice induced significant oedema formation and increased total leukocyte, mononuclear cells, and neutrophil count in its joint exudate 7 and 24 h after the challenge (Fig. 4). Treatment with dexamethasone (10 mg/kg; i.p.) or MG (7 mg/kg) was performed 1 h before the challenge, and the mice were euthanized 7 or 24 h after the challenge. Prior oral administration of MG significantly reduced the increase in joint diameter at both times evaluated to the same extent as the positive control, dexamethasone (Fig. 4A, B). Treatment with MG also decreased the number of total leukocytes accumulated in the joint at 7 h (56% of inhibition) and 24 h (62% of inhibition), compared with immunized and challenged mice (Fig. 4C, D). Treatment with MG also significantly reduced mononuclear cells and neutrophils accumulation into the synovial cavity (Fig. 4E–H). Inhibition in all parameters evaluated was statistically similar to that of the positive control, dexamethasone.
Effect of methyl gallate on oedema, leukocyte influx and DNA released in the synovial wash. Mice were treated with MG (7 mg/kg, po,—1 h) or dexamethasone (10 mg/kg, ip,—1 h) before i.a. injection of mBSA (30 µg/25 µL). Control group was injected with the same volume of sterile saline. Non-immunized mice also were challenged i.a. with mBSA. Knee joint diameter was evaluated with a digital caliper 7 and 24 h after mBSA challenge (A, B). The numbers of total leukocytes (C, D), mononuclear cells (E, F), and neutrophils (G, H) are plotted as the number of cells × 105. Knee synovial cells were recovered 7 and 24 h after mBSA challenge. Levels of DNA released in synovial wash induced by injection of antigen (I, J). The results are presented as the means ± SEM of seven mice per group per experiment and are representative of three separate experiments [*p ≤ 0.05 compared to the vehicle group; +p ≤ 0.05 compared to the immunized mBSA group (one-way ANOVA followed by Tukey test)]. NI not-immunized; IM immunized
An excessive formation of neutrophil extracellular traps (NETs) is one of the primary mechanisms by which neutrophils cause tissue damage and promote autoimmunity in RA (Apel et al. 2018). We evaluated the release of extracellular DNA in the synovial wash to infer MG's effect on NET formation. The i.a. injection of mBSA on joint of immunized mice induced an increase of DNA release on synovial wash 7 and 24 h after the challenge (Fig. 4I, J), suggesting NET formation in this model. MG treatment reduced the release of extracellular DNA similarly as dexamethasone at both times evaluated (Fig. 4I, J). These results collectively indicate that MG is efficient in modulating the inflammatory process involved in AIA.
Methyl gallate inhibited the production of pro-inflammatory cytokines in the AIA model
Chemokines and cytokines play a pivotal role in the recruitment of inflammatory cells and the development of arthritis. The levels of CCL-2, CCL-3, IL-17 and TNF-α were evaluated in the synovial wash and periarticular tissue by ELISA (Fig. 5). The chemokines CCL-2 and CCL-3, related to the recruitment of monocytes and polymorphonuclear leukocytes, were increased in the synovial wash of AIA mice compared to the control groups (non-immunized mice and immunized-saline group). Treatment with MG reduced CCL-2 and CCL-3 production (Fig. 5A, B). It was also observed an increase in cytokines IL-17 and TNF-α 7 h after the challenge with mBSA. Pretreatment with MG significantly reduced IL-17 and TNF-α production at 7 h, to a similar extent to the dexamethasone pretreatment effect (Fig. 5C, D). In this way, inhibition of pro-inflammatory chemokines and cytokines by MG correlates with reducing the inflammatory reaction in the AIA model.
Effect of methyl gallate on inflammatory mediators release. Mice were treated with MG (7 mg/kg, po,—1 h) or dexamethasone (10 mg/kg, ip,—1 h) before i.a. injection of mBSA (30 µg/25 µL). Control group was injected with the same volume of sterile saline. Non-immunized mice also were challenged i.a. with mBSA. Concentration of CCL-2 (A), CCL-3 (B) and IL-7 (C) were evaluated from synovial wash, TNF-α (D) was evaluated from periarticular tissue 7 h after the injection of mBSA. The results are presented as the means ± SEM of seven mice per group per experiment and are representative of two separate experiments [*p ≤ 0.05 compared to the vehicle group; +p ≤ 0.05 compared to the immunized mBSA group (one-way ANOVA followed by Tukey test)]. NI not-immunized; IM immunized
Effect of daily treatment with methyl gallate on liver and kidney enzymes
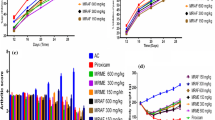
An important issue to be addressed is whether prolonged treatment with MG present toxicity effects. Accordingly, the acute oral toxicity assay showed no changes in hematological and biochemical patterns or in the size or morphology of vital organs, such as heart, liver, spleen and kidneys even after treatment with the highest MG dose (1000 mg/kg) (Table 1). Next, we evaluated a potential toxicity effect of prolonged treatment with MG in animals affected by AIA. Mice were treated daily with MG or dexamethasone for seven consecutive days after i.a. challenge with mBSA. During the disease's progression, the mice weight was monitored, and it was not observed a significant difference between non-immunized and immunized mice groups (Fig. 6A). However, daily treatment with dexamethasone, induced a significant weight loss. MG treatment did not cause weight loss, but the animals did not gain weight in the same proportion as the control groups (Fig. 6A). Next, plasma samples were collected to determine the concentrations of aspartate aminotransferase (AST), alanine aminotransferase (ALT), urea BUN and creatinine kinase (CK). Dexamethasone induced an increase in AST and ALT levels (Fig. 6B, C). Significantly, the treatment with MG did not alter the plasma concentration of AST (Fig. 6B), ALT (Fig. 6C), urea BUN (Fig. 6D) and CK (Fig. 6E) compared to control groups. These results suggest that prolonged treatment with MG does not interfere with mice liver or kidney function.
Effect of daily treatment with methyl gallate on liver and kidney enzymes. Mice were treated with MG (7 mg/kg, po) or dexamethasone (10 mg/kg, ip.) for seven consecutive days after i.a. injection of mBSA (30 µg/25 µL). Non-immunized mice also were challenged i.a. with mBSA. The weight of each animal was recorded from day 0 and day 28 (A). AST (B), ALT (C), urea BUN (D), and creatinine kinase (CK) (E) plasmatic levels were examined 7 days after the first challenge with mBSA. The results are presented as the means ± SEM of seven mice per group per experiment and are representative of two separate experiments [*p ≤ 0.05 compared to the vehicle group; +p ≤ 0.05 compared to the immunized mBSA group (one-way ANOVA followed by Tukey test)]. NI non-immunized; IM immunized
Daily treatment with methyl gallate inhibits late articular inflammatory response in the AIA model
AIA model presents several parameters of a chronic inflammatory process at day 28, after two challenges with mBSA. The daily treatment with MG for 7 days after the first injection of mBSA reduced significantly the antigen-induced oedema formation (Fig. 7A). The treatment was also able to reduce the arthritis index calculated with histopathological parameters: severity of synovial hyperplasia (pannus formation), intensity of the inflammatory infiltrate, bleeding and cartilage degradation (Fig. 7B). Figure 7C shows representative images of histological sections of mice femorotibial joints obtained 7 days after the i.a. challenge with mBSA stained with H&E or Safranin-O. Immunized-saline group exhibited a typical architecture of the femorotibial joint, with a normal appearance of the cartilage lining, without any inflammatory infiltrates in the synovial tissue (Fig. 7C). Non-immunized histological sections show moderate inflammatory infiltrate in the tissue. Histological sections from immunized-mBSA mice presented an abnormal histologic appearance of the joint, with pronounced synovial inflammation (black arrows) and severe decrease in fat cells, synovial hyperplasia and pannus formation (*) (Fig. 7C). The analysis of immunized group showed an increase in the overall arthritis score in comparison to control mice (Fig. 7B).
Effect of daily treatment with methyl gallate on histopathological parameters. Mice were treated with MG (7 mg/kg, po) or dexamethasone (10 mg/kg, ip.) for seven consecutive days after i.a. injection of mBSA (30 µg/25 µL). Non-immunized mice also were challenged i.a. with mBSA. A Knee joint diameter was evaluated with a digital caliper 7 days after first mBSA challenge. B Subjective classification for histopathological changes. The scores of all parameters were added to give the arthritis index (AI). C, D Longitudinal histological sections of the femorotibial joint were obtained 7 days after the antigen's challenge, a representative image of at least six different animals per group. The highlighted area (rectangle) was represented in greater amplification in the image below (200× ; bar = 100 µm). The results are presented as the means ± SEM of seven mice per group per experiment and are representative of two separate experiments [*p ≤ 0.05 compared to the vehicle group; +p ≤ 0.05 compared to the immunized mBSA group (one-way ANOVA followed by Tukey test)]. NI non-immunized; IM immunized
In contrast, the animals treated with dexamethasone showed significant inhibition in cell infiltration compared with vehicle-treated mice, leading to a reduction in the arthritis index (Fig. 7B). MG treatment was also effective in reducing all scores of histologic features analyzed and the arthritis index was decreased in a similar proportion to the observed with dexamethasone treatment (Fig. 7B, C). Safranin-O stain was used to assess the loss of cartilage protein. Histological sections from mBSA-immunized mice, suggest cartilage degradation as evidenced by loss of safranin staining (Fig. 7D). Treatment with MG or dexamethasone protected the cartilage from proteoglycans loss (Fig. 7D).
Methyl gallate attenuates osteoclastogenesis in vitro and bone resorption in the knee joint in the AIA model
Bone erosion during arthritis is primarily the result of activated osteoclasts that express bone-resorbing enzymes. The expression of TRAP enzyme is a marker of osteoclast function and bone resorption intensity. Methyl gallate was previously described to reduce in vitro RANKL-dependent osteoclastic differentiation (Baek et al. 2017). We confirmed this finding by evaluating the number and area of multinucleated TRAP-positive cells as well as the expression of osteoclastogenic marker genes. Bone marrow macrophages (BMMs) were cultured with M-CSF, RANKL and different concentrations of MG (3, 10, 30 or 100 µM). Figure 8A shows the cell viability using MTT assay. The concentration of 100 µM presents a cytotoxic effect; however, the other concentrations tested were not cytotoxic. Numerous large TRAP-positive cells were formed after 3 days of culture of BMMs stimulated with M-CSF and RANKL (Fig. 8B, C and Supplemental Fig. 2A). The number of multinucleated TRAP-positive cells decreased in the presence of MG at 30 µM (Fig. 8B). The area of multinucleated TRAP-positive cells decreased in the presence of MG in a concentration-dependent manner (Fig. 8C), reaching a maximum effect at the concentration of 30 µM. Gene expression analysis showed that stimulus with M-CSF and RANKL upregulated the expression of integrin-β3, calcitonin receptor (CTR) and NFATc1 (Supplemental Fig. 2B–D). MG downregulated the expression of integrin-β3 and CRT (Supplemental Fig. 2B, C) and also decreased the expression of NFATc1 which is a key regulator of osteoclast differentiation (Supplemental Fig. 2D).
Effect of MG on osteoclast differentiation in vitro and osteoclasts number in synovial tissue. A–E Mouse bone marrow macrophage (BMMs) were cultured with osteoclastic media in the presence of the indicated concentration of MG (3, 10, 30 or 100 µM). A Cell viability was assessed by MTT assay. B After 3 days, cells were fixed and stained for TRAP. C Multinucleated TRAP-positive cells containing more than three nuclei were considered mature osteoclast and were counted (osteoclasts per well). D Longitudinal histological sections of the femorotibial joint were obtained 7 days after the challenge with the antigen, a representative image of at least six different animals per group (100× ; bar = 100 µm). E Quantitative analysis of TRAP positive cells. The results are presented as the means ± SEM and are representative of two separate experiments [A–C, +p ≤ 0.05 compared to untreated and treated mice; #p ≤ 0.05 compared different doses of MG; E, *p ≤ 0.05 compared to the vehicle group; +p ≤ 0.05 compared to the immunized mBSA group (one-way ANOVA followed by Tukey test)]
Next, we investigated the effect of daily treatment with MG in the knee joint in AIA model. TRAP-positive cells were determined by histochemical staining in knee joint tissue samples. AIA-induced a significant TRAP-positive cells detection compared to the control groups (non-immunized mice and immunized mice challenge with saline). In turn, MG and dexamethasone treatment inhibit AIA-induced TRAP-positive cells (Fig. 8D). Quantitative analysis (Fig. 8E) of TRAP-positive cells confirmed that MG inhibited osteoclast activation. This result suggests that MG reduces in vivo osteoclast formation, and consequently, decreases the articular damage of murine antigen-induced arthritis model.
Discussion
Methyl gallate is a prevalent phenolic acid in the plant kingdom and is often found in herbs used in folk medicine to treat inflammatory conditions. In previous works, we already described that MG (0.7–70 mg/kg p.o.) inhibited in vivo inflammatory pain, edema, and cell migration in an acute inflammatory reaction induced by zymosan (Correa et al. 2016, 2020). This effect is related to the inhibition of neutrophil accumulation and inflammatory mediators, such as IL-1β, IL-6, TNF-α, CXCL-1, LTB4, and PGE2 which are relevant in the pathogenesis of rheumatoid arthritis (RA). Herein, we demonstrated the MG activity on the murine model of antigen-induced arthritis (AIA). This model is trigger primarily by immune processes and presents several characteristics of RA. Among others, a marked synovial-lining hyperplasia, proliferation of subliming cells, infiltration of inflammatory cells, local chemokine and cytokine production, pannus formation, hypernociception and articular cartilage destruction concomitant with prominent osteoclastogenesis (van Den Berg et al. 1981; Ferraccioli et al. 2010; Sachs et al. 2011).
Our data demonstrate that MG pretreatment significantly attenuates the development of AIA. This was evidenced by the reduction of clinical scores and synovial inflammation in treated animals. MG treatment also reduced the neutrophil influx into the joint cavity, oedema formation, articular cartilage damage, cytokines production, and osteoclasts number in the synovial tissue. The inhibition achieved with MG was equivalent to the obtained with dexamethasone, except for the number of osteoclasts in synovial tissue. Dexamethasone is a synthetic glucocorticoid with anti-inflammatory and immunosuppressant properties commonly used to manage RA (Fraenkel et al. 2021). Dexamethasone binds to coactivators to directly inhibit histone acetyltransferase (HAT) activity and recruits histone deacetylase (HDAC)-2, which reverses histone acetylation, leading to suppression of activated inflammatory genes (Dinarello 2010). Our studies focused on the evaluation of the main signs of the inflammatory process and the production of inflammatory mediators, that is the reason we have chosen a positive control that acts directly on these pathways, such as dexamethasone.
Neutrophils have been recognized as critical participants in the onset and progression of rheumatoid arthritis. The pathogenic role of neutrophils includes increased migratory capacity, increased ROS and cytokines production and apoptosis delay (Martelli-Palomino et al. 2017; Marchi et al. 2018). Moreover, an exacerbated release of neutrophil extracellular traps is also observed (Khandpur et al. 2013; Wright et al. 2021). Many studies have confirmed a high degree of spontaneous NETs formation in RA neutrophils, showing a strong correlation between free circulating DNA levels and inflammatory markers, such as C-reactive protein (CRP), erythrocyte sedimentation rate, ACPAs titers, and levels of TNF-α and IL-17 (Khandpur et al. 2013; Sur Chowdhury et al. 2014; Pérez-Sánchez et al. 2017). Accordingly, we demonstrated that MG pretreatment reduced the release of extracellular DNA in the AIA model at both times studied (36% and 39%, of inhibition, respectively). It was recently shown that NETs are released in the joints in the AIA model and mediate articular pain through activation of TLRs (Schneider et al. 2020). It is interesting to note that MG can also inhibit inflammatory pain and cell signaling induced by Toll‑like receptor ligands (Correa et al. 2020). However, we did not evaluate the effect of MG directly on NET release and we cannot rule out whether this reduction of circulating DNA on synovial wash is due to a direct decrease in the neutrophils number in the inflamed joint.
Several cytokines, including TNF-α and IL-17, play a fundamental role in the events that cause inflammation, joint destruction, and various comorbidities in RA (Tarner et al. 2007). MG inhibited AIA-induced pro-inflammatory cytokines production (TNF-α, IL-17, CCL-2 and CCL-3). We have recently demonstrated that MG (1–100 µM) is able to inhibit cytokines production induced by Toll‑like receptor ligands by inhibiting MAPK and NF‑Κb signaling impairing the ERK1/2, JNK and p38 MAPK phosphorylation as well as the IκB-α degradation (Correa et al. 2020). IL-17 and TNF-α are increased in RA serum and synovial fluid, and their elevated level predicts joint damage progression. IL-17 and TNF-α are also described to induce NETosis in neutrophils from RA patients (Khandpur et al. 2013). IL-17 has a widespread inflammatory effect on the joint, orchestrating bone and cartilage damage progression, and causes pro-inflammatory mediators' augmentation to the synovium (Maddur et al. 2012). Many chemokines are also increased in RA synovial fluid, including CCL-3 and CCL-2. These chemokines regulate the joint inflammatory response by recruiting and activating both innate and adaptative immune cells (Szekanecz and Koch 2016). Therefore, MG inhibition of mBSA-induced cytokine production may lead to reduced leukocyte recruitment reduction, oedema formation, and bone and cartilage damage.
RA patients commonly take corticosteroids; however, the induction of many side effects limits this therapy (Yasir and Sonthalia 2019). In this work, we investigated the action of MG and dexamethasone when administered in a prolonged treatment regimen, regarding weight gain and plasma enzymes. We observed a loss of weight and an increase in plasma levels of AST and ALT in mice treated daily with dexamethasone. On the other hand, treatment with MG did not cause any changes in plasma enzymes related to liver and kidney function. Our results showed that prolonged treatment with MG did not cause liver and kidney damage.
The histopathological study confirmed the effectiveness of the prolonged treatment with MG. We observed a reduction in cell infiltration, synovial inflammation, synovial hyperplasia and pannus formation at the same proportion as the prolonged treatment with dexamethasone. Treatment with MG or dexamethasone also protected cartilage degradation as observed with safranin-O stain.
Systemic bone loss in RA is a multifactorial and complex alteration in which chronic inflammation plays an important role. Osteoclast plays a critical role in bone loss and its differentiation and activation are mainly dependent on the presence of M-CSF and RANKL (Boyle et al. 2003). Pro-inflammatory cytokines such as TNF, IL-1 and IL-6 can enhance osteoclastogenesis by amplifying osteoclast function, inhibiting osteoblast function, and perpetuating an inflammatory response that can lead to tissue degradation (Redlich and Smolen 2012).
It was previous described that MG inhibits osteoclastogenesis in vitro, by diminishing mRNA expression of OSCAR (osteoclast-associated receptor) and TRAP through downregulation of c-Fos and NFATc1 genes (Baek et al. 2017). Macrophages differentiate into bone-resorbing osteoclasts under stimulation of two necessary factors, M-CSF and RANKL. These factors induce the expression of genes that characterize the osteoclast lineage, such as tartrate-resistant acid phosphatase (TRAP), cathepsin K (CATK), calcitonin receptor (CRT) and the integrin-β3, leading to the development of mature osteoclasts (Han et al. 1998; Udagawa et al. 2021). NFATc1 is a pivotal regulator of osteoclastogenesis, modulating the expression of several osteoclast-specific molecules involved in fusion, differentiation, maturation and bone remodeling (Matsuo et al. 2004; Huang et al. 2006; Park et al. 2017). We confirmed this effect, showing that MG can directly modulate osteoclastogenesis in vitro, diminishing the number and area of multinucleated TRAP-positive cells, as well as the expression of osteoclastogenic marker genes integrin-β3 and CRT and the expression of NFATc.
Importantly, we demonstrated that oral treatment with MG was able to reduce, the bone loss observed in the AIA model by quantifying the number of TRAP-positive cells. The number of TRAP-positive cells was decreased after prolonged treatment with dexamethasone or MG, reinforcing the in vivo effect on osteoclast differentiation.
Conclusions
The present data demonstrate that MG ameliorates antigen-induced arthritis. The reduction in the acute influx of neutrophils and cytokines and chemokines may be leading to cartilage degradation prevention. In addition, MG protected against bone erosion, possibly by its direct effect on osteoclast differentiation. These findings collectively demonstrate that MG exerts therapeutic effects on chronic inflammatory reactions driven primarily by an immune process characterized by extensive bone and cartilage erosion, such as in rheumatoid arthritis.
Data availability
All the data of this study are transparent.
Code availability
No applicable.
References
Acharyya S, Sarkar P, Saha DR et al (2015) Intracellular and membrane-damaging activities of methyl gallate isolated from Terminalia chebula against multidrug-resistant Shigella spp. J Med Microbiol 64:901–909. https://doi.org/10.1099/jmm.0.000107
Apel F, Zychlinsky A, Kenny EF (2018) The role of neutrophil extracellular traps in rheumatic diseases. Nat Rev Rheumatol 14:467–475
Asquith DL, Miller AM, McInnes IB, Liew FY (2009) Animal models of rheumatoid arthritis. Eur J Immunol 39:2040–2044. https://doi.org/10.1002/eji.200939578
Baek JM, Kim JY, Lee CH et al (2017) Methyl gallate inhibits osteoclast formation and function by suppressing Akt and Btk-PLCγ2-Ca. Int J Mol Sci. https://doi.org/10.3390/ijms18030581
Ballanti P, Minisola S, Pacitti MT et al (1997) Tartrate-resistant acid phosphate activity as osteoclastic marker: sensitivity of cytochemical assessment and serum assay in comparison with standardized osteoclast histomorphometry. Osteoporos Int 7:39–43
Benson RA, McInnes IB, Garside P, Brewer JM (2018) Model answers: rational application of murine models in arthritis research. Eur J Immunol 48:32–38
Boyle WJ, Simonet WS, Lacey DL (2003) Osteoclast differentiation and activation. Nature 423:337–342
Brennan FM, McInnes IB (2008) Evidence that cytokines play a role in rheumatoid arthritis. J Clin Invest 118:3537–3545. https://doi.org/10.1172/JCI36389
Burmester GR, Pope JE (2017) Novel treatment strategies in rheumatoid arthritis. Lancet 389:2338–2348. https://doi.org/10.1016/S0140-6736(17)31491-5
Cecchi I, de la Rosa I, Menegatti E et al (2018) Neutrophils: novel key players in rheumatoid arthritis. Current and future therapeutic targets. Autoimmun Rev 17:1138–1149. https://doi.org/10.1016/j.autrev.2018.06.006
Chae HS, Kang OH, Choi JG et al (2010) Methyl gallate inhibits the production of interleukin-6 and nitric oxide via down-regulation of extracellular-signal regulated protein kinase in RAW 264.7 cells. Am J Chin Med 38:973–983. https://doi.org/10.1142/S0192415X10008391
Cho EJ, Yokozawa T, Kim HY et al (2004) Rosa rugosa attenuates diabetic oxidative stress in rats with streptozotocin-induced diabetes. Am J Chin Med 32:487–496. https://doi.org/10.1142/S0192415X04002132
Correa LB, Pádua TA, Seito LN et al (2016) Anti-inflammatory effect of methyl gallate on experimental arthritis: inhibition of neutrophil recruitment, production of inflammatory mediators, and activation of macrophages. J Nat Prod 79:1554–1566. https://doi.org/10.1021/acs.jnatprod.5b01115
Correa LB, Seito LN, Manchope MF et al (2020) Methyl gallate attenuates inflammation induced by Toll-like receptor ligands by inhibiting MAPK and NF-Κb signaling pathways. Inflamm Res. https://doi.org/10.1007/s00011-020-01407-0
Dinarello CA (2010) Anti-inflammatory agents: present and future. Cell 140:935–950. https://doi.org/10.1016/j.cell.2010.02.043
Fardellone P, Salawati E, Le Monnier L, Goëb V (2020) Bone loss, osteoporosis, and fractures in patients with rheumatoid arthritis: a review. J Clin Med 9:3361. https://doi.org/10.3390/jcm9103361
Ferraccioli G, Bracci-Laudiero L, Alivernini S et al (2010) Interleukin-1β and interleukin-6 in arthritis animal models: roles in the early phase of transition from acute to chronic inflammation and relevance for human rheumatoid arthritis. Mol Med 16:552–557. https://doi.org/10.2119/molmed.2010.00067
Fraenkel L, Bathon JM, England BR et al (2021) 2021 American College of Rheumatology guideline for the treatment of rheumatoid arthritis. Rheumatology. https://doi.org/10.1002/art.41752
Gardinassi LG, DeSouza-Vieira TS, Da Silva NO et al (2017) Molecular signatures of neutrophil extracellular traps in human visceral leishmaniasis. Parasit Vectors. https://doi.org/10.1186/s13071-017-2222-5
Giannini D, Antonucci M, Petrelli F et al (2020) One year in review 2020: pathogenesis of rheumatoid arthritis. Clin Exp Rheumatol 38:387–397
Han Z, Boyle DL, Manning AM, Firestein GS (1998) AP-1 and NF-kappaB regulation in rheumatoid arthritis and murine collagen-induced arthritis. Autoimmunity 28:197–208. https://doi.org/10.3109/08916939808995367
Huang H, Chang EJ, Ryu J et al (2006) Induction of c-Fos and NFATc1 during RANKL-stimulated osteoclast differentiation is mediated by the p38 signaling pathway. Biochem Biophys Res Commun 351:99–105. https://doi.org/10.1016/j.bbrc.2006.10.011
Huang C-Y, Chang YJ, Wei PI et al (2021) Methyl gallate, gallic acid-derived compound, inhibit cell proliferation through increasing ROS production and apoptosis in hepatocellular carcinoma cells. PLoS ONE. https://doi.org/10.1371/JOURNAL.PONE.0248521
Kamatham S, Kumar N, Gudipalli P (2015) Isolation and characterization of gallic acid and methyl gallate from the seed coats of. Toxicol Rep 2:520–529. https://doi.org/10.1016/j.toxrep.2015.03.001
Kanashiro A, Talbot J, Peres RS et al (2016) Neutrophil recruitment and articular hyperalgesia in antigen-induced arthritis are modulated by the cholinergic anti-inflammatory pathway. Basic Clin Pharmacol Toxicol 119:453–457. https://doi.org/10.1111/bcpt.12611
Kang MS, Jang HS, Oh JS et al (2009) Effects of methyl gallate and gallic acid on the production of inflammatory mediators interleukin-6 and interleukin-8 by oral epithelial cells stimulated with Fusobacterium nucleatum. J Microbiol 47:760–767. https://doi.org/10.1007/s12275-009-0097-7
Karmakar S, Kay J, Gravallese EM (2010) Bone damage in rheumatoid arthritis: mechanistic insights and approaches to prevention. Rheum Dis Clin North Am 36:385–404. https://doi.org/10.1016/j.rdc.2010.03.003
Khandpur R, Carmona-Rivera C, Vivekanandan-Giri A et al (2013) NETs are a source of citrullinated autoantigens and stimulate inflammatory responses in rheumatoid arthritis. Sci Transl Med 5:178ra40. https://doi.org/10.1126/scitranslmed.3005580
Lee SH, Kim JK, Kim DW et al (2013) Antitumor activity of methyl gallate by inhibition of focal adhesion formation and Akt phosphorylation in glioma cells. Biochim Biophys Acta 1830:4017–4029. https://doi.org/10.1016/j.bbagen.2013.03.030
Llorente I, García-Castañeda N, Valero C et al (2020) Osteoporosis in rheumatoid arthritis: dangerous liaisons. Front Med 7
Maddur MS, Miossec P, Kaveri SV, Bayry J (2012) Th17 cells: biology, pathogenesis of autoimmune and inflammatory diseases, and therapeutic strategies. Am J Pathol 181:8–18
Marchi LF, Paoliello-Paschoalato AB, Oliveira RDR et al (2018) Activation status of peripheral blood neutrophils and the complement system in adult rheumatoid arthritis patients undergoing combined therapy with infliximab and methotrexate. Rheumatol Int 38:1043–1052. https://doi.org/10.1007/s00296-018-3997-1
Martelli-Palomino G, Paoliello-Paschoalato AB, Crispim CO et al (2017) DNA damage increase in peripheral neutrophils from patients with rheumatoid arthritis is associated with the disease activity and the presence of shared epitope. Clin Exp Rheumatol 35:247–254
Matsuo K, Galson DL, Zhao C et al (2004) Nuclear factor of activated T-cells (NFAT) rescues osteoclastogenesis in precursors lacking c-Fos. J Biol Chem 279:26475–26480. https://doi.org/10.1074/jbc.M313973200
Oliveira PG, Grespan R, Pinto LG et al (2011) Protective effect of RC-3095, an antagonist of the gastrin-releasing peptide receptor, in experimental arthritis. Arthritis Rheum 63:2956–2965. https://doi.org/10.1002/art.30486
Pandey KB, Rizvi SI (2009) Plant polyphenols as dietary antioxidants in human health and disease. Oxid Med Cell Longev 2:270–278. https://doi.org/10.4161/oxim.2.5.9498
Park JH, Lee NK, Lee SY (2017) Current understanding of RANK signaling in osteoclast differentiation and maturation. Mol Cells 40:706–713
Pérez-Sánchez C, Ruiz-Limón P, Aguirre MA et al (2017) Diagnostic potential of NETosis-derived products for disease activity, atherosclerosis and therapeutic effectiveness in rheumatoid arthritis patients. J Autoimmun 82:31–40. https://doi.org/10.1016/j.jaut.2017.04.007
Redlich K, Smolen JS (2012) Inflammatory bone loss: pathogenesis and therapeutic intervention. Nat Rev Drug Discov 11:234–250
Rosas EC, Correa LB, de Almeida PT et al (2015) Anti-inflammatory effect of Schinus terebinthifolius Raddi hydroalcoholic extract on neutrophil migration in zymosan-induced arthritis. J Ethnopharmacol. https://doi.org/10.1016/j.jep.2015.10.014
Sachs D, Coelho FM, Costa VV et al (2011) Cooperative role of tumour necrosis factor-α, interleukin-1β and neutrophils in a novel behavioural model that concomitantly demonstrates articular inflammation and hypernociception in mice. Br J Pharmacol 162:72–83. https://doi.org/10.1111/j.1476-5381.2010.00895.x
Schneider AH, Machado CC, Veras FP et al (2020) Neutrophil extracellular traps mediate joint hyperalgesia induced by immune inflammation. Rheumatology. https://doi.org/10.1093/rheumatology/keaa794
Smolen JS, Aletaha D, Barton A et al (2018) Rheumatoid arthritis. Nat Rev Dis Prim 4:18001. https://doi.org/10.1038/nrdp.2018.1
Sung S, Kwon D, Um E, Kim B (2019) Could polyphenols help in the control of rheumatoid arthritis? Molecules. https://doi.org/10.3390/molecules24081589
Sur Chowdhury C, Giaglis S, Walker UA et al (2014) Enhanced neutrophil extracellular trap generation in rheumatoid arthritis: analysis of underlying signal transduction pathways and potential diagnostic utility. Arthritis Res Ther 16:R122. https://doi.org/10.1186/ar4579
Szekanecz Z, Koch AE (2016) Successes and failures of chemokine-pathway targeting in rheumatoid arthritis. Nat Rev Rheumatol 12:5–13
Tarner IH, Müller-Ladner U, Gay S (2007) Emerging targets of biologic therapies for rheumatoid arthritis. Nat Clin Pract Rheumatol 3:336–345
Udagawa N, Koide M, Nakamura M et al (2021) Osteoclast differentiation by RANKL and OPG signaling pathways. J Bone Miner Metab 39:19–26
van Den Berg WB, Kruijsen MWM, van De Putte LBA et al (1981) Antigen-induced and zymosan-induced arthritis in mice: Studies on in vivo cartilage proteoglycan synthesis and chondrocyte death. Br J Exp Pathol 62:308–316
Wright HL, Lyon M, Chapman EA et al (2021) Rheumatoid arthritis synovial fluid neutrophils drive inflammation through production of chemokines, reactive oxygen species, and neutrophil extracellular traps. Front Immunol. https://doi.org/10.3389/fimmu.2020.584116
Yasir M, Sonthalia S (2019) Corticosteroid adverse effects. StatPearls Publishing, Florida
Acknowledgements
The authors are grateful to Erika Cunha for technical assistance and Ursula Raquel do C. F. da Silva for technical assistance in histopathological analysis.
Funding
The author Luana Barbosa Correa has received research support from Carlos Chagas Filho Foundation of Rio de Janeiro State (FAPERJ—E-26/201.946/2020). This work was supported by grants from the FAPERJ—Cientistas de Nosso Estado No. E-26/202.887/2018; Brazilian Council for Scientific and Technological Development (CNPq)—313443/2018-1; Oswaldo Cruz Foundation (FIOCRUZ) Projeto INOVA Geração do Conhecimento No. 1531.
Author information
Authors and Affiliations
Contributions
LBC: conceptualization, data curation, formal analysis, investigation, methodology, writing—original draft, writing—review & editing. PVGA: conceptualization, formal analysis, investigation, methodology. TAP: investigation, visualization, writing—review & editing. EMS: formal analysis, investigation. EBG: formal analysis, investigation. FCA: formal analysis, investigation; FKF: formal analysis, investigation. SYF: conceptualization, resources, supervision, Writing—review & editing. MGH: conceptualization, funding acquisition, project administration, resources, supervision, writing—original draft; writing—review & editing. ECR: conceptualization, funding acquisition, project administration, resources, supervision, writing—original draft; writing—review & editing. All authors read and approved the final manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no conflicts of interest to declare that are relevant to the content of this article.
Ethics approval
All animal care and experimental procedures performed were approved by the institution's Committee of Ethics in Animal Care and Use (CEUA) (registered under the number CEUA LW-43/14).
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Supplemental Fig. 1
Levels of antibody against mBSA in the serum of immunized and non-immunized mice 24 h after mBSA challenge. mBSA (30 µg in 25 µL) was injected into the left tibio-femural joint of immunized mice. Non-immunized mice also were challenged i.a. with mBSA. The results are presented as the means ± SEM of seven mice per group per experiment and are representative of two separate experiments [*p ≤ 0.05 compared to the saline group; +p ≤ 0.05 compared to the immunized mBSA group (one-way ANOVA followed by t-test)]. Supplementary file1 (TIF 88 KB)
Supplemental Fig. 2
Effect of MG on osteoclast differentiation and expression of osteoclastogenic markers. (A-D) Mouse bone marrow macrophage (BMMs) were cultured with osteoclastic media in the presence of the indicated concentration of MG (3, 10 or 30). (A) Multinucleated TRAP-positive cells containing more than three nuclei were considered mature osteoclast and were counted and the area was measured. The cells were photographed under a light microscope at the magnification (10 ×). The mRNA expression of NFATc1 (E), Itgb3 (F) and CTR (G) was analyzed by quantitative PCR (RT-PCR). The results are presented as the means ± SEM and are representative of two separate experiments [*p ≤ 0.05 compared to untreated and treated mice (one-way ANOVA followed by t-test)]. Supplementary file2 (TIF 2783 KB)
Rights and permissions
About this article
Cite this article
Correa, L.B., Pádua, T.A., Alabarse, P.V.G. et al. Protective effect of methyl gallate on murine antigen-induced arthritis by inhibiting inflammatory process and bone erosion. Inflammopharmacol 30, 251–266 (2022). https://doi.org/10.1007/s10787-021-00922-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10787-021-00922-8