Abstract
The E2 promoter binding factor 1 (E2F1) and the Wnt/β-catenin signaling are crucial in regulating metabolic homeostasis including obesity. The β-catenin interacting protein 1 (CTNNBIP1), also known as the inhibitor of β-catenin and TCF4 (ICAT), is required for E2F1 to inhibit the activity of β-catenin. However, the role of ICAT in E2F1 regulating obesity-related metabolic disorders remains unknown. In the present study, male adipose tissue-specific ICAT knockout (ICATadi−/−) C57BL/6 J mice and control littermates aged 6–8 weeks were fed with high-fat diet (HFD) for 12 weeks to explore the effect of ICAT on lipid metabolism and obesity-related disorders. Results showed that the adipose tissue-specific ICAT knockout had negligible effect on lipid metabolism, reflected by no difference in body weight, fat mass, and the expression of proteins involved in lipid metabolism in white adipose tissue (WAT) and the liver between the ICATadi−/− mice and the control littermate (ICATfl/fl) mice. However, the knockout of ICAT reduced inflammatory response in WAT and the liver. Additionally, Sirius red staining results showed that deletion of ICAT attenuated fibrosis and reduced mRNA levels of transforming growth factor β1(TGF-β1), matrix metallopeptidase 2 (Mmp2), Mmp3, and collagen, type V, alpha 1 (Col5a1) in WAT and the liver. These results suggested that knockout of ICAT improved the metabolic abnormalities of obese mice through attenuating adipose tissue and the liver inflammation as well as fibrosis. Our findings may provide a new insight to understand the role of ICAT in inflammation and fibrosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Adipose tissue, composed of adipocytes, precursor adipose fibroblasts, blood vessels, neuronal cells, and immune cells, plays a central role in modulating energy homeostasis. Adipose tissue is also an endocrine organ involved in the immune response by secreting hormones such as adiponectin, leptin, cytokine, and chemokines [1,2,3]. Currently, more than 400 million adults and 100 million children worldwide are obese [4], according to the definition of individuals with a BMI ≥ 30 kg/m2 [5]. Unhealthy lifestyles, individual genetic variants, and excessive consumption of high-energy food contribute to energy accumulation in the body [4]. The imbalance of energy homeostasis leads to overweight, obesity and its comorbidities such as type II diabetes, cardiovascular disease, cancer, metabolic abnormalities (hyperglycemia and hyperlipidemia), and chronic inflammation, seriously impairing human health and well-being and increasing social and economic burdens worldwide [5, 6]. Accumulating evidence has demonstrated that obesity-induced inflammation is associated with the development of metabolic syndrome, diabetes, cancer, and so on [7]. Thus, strategies for inflammation control in obese individuals are greatly needed to improve obesity-associated metabolic disorders [8].
A variety of regulatory mechanisms or signal pathways have been reported to play key roles in the proliferation and differentiation of adipocytes, most of which are involved in activating or inhibiting the transformation of pluripotent stem cells (PSC) into adipocyte lines [9]. Several studies have demonstrated the critical role of Wnt/β-catenin signaling in the development of adipogenesis and obesity [10,11,12,13]. β-catenin signaling is essential for the commitment of early stem cells to the adipocyte lines [14]. Furthermore, β-catenin signaling contributes to restraining adipogenesis by inhibiting CAAT/enhancer binding protein α (C/EBPα) and peroxisome proliferators-activated receptor γ (PPARγ), two critical transcription factors involved in regulating adipogenesis, in the terminal differentiation stage [15]. E2 promoter binding factor 1 (E2F1), a crucial regulator involved in the cell cycle, DNA damage, apoptosis, and cancer, has been boosted in obesity [16]. In the occurrence of malignant tumors, the Wnt/β-catenin pathway is usually overactivated [17, 18], and mutations such as retinoblastoma (Rb) tumor suppressor protein often lead to the aberrant activation of E2F1 [19, 20]. By contrast, cyclin-dependent kinase-8 (CDK8) results in the overactivation of β-catenin by inhibiting E2F1 activity in colorectal cancers [21, 22]. Our previous study has shown that the β-catenin interacting protein 1 (CTNNBIP1), also known as the inhibitor of β-catenin and TCF4 (ICAT), is a direct target gene of E2F1 in colorectal cancers and activation of ICAT is required for inhibiting β-catenin activity by E2F1 [23]. Moreover, a previous study has revealed that E2F1 can bind to the promoter of C/EBPα but not PPARγ [24]. Accumulating evidence has indicated that E2F1 could regulate glucose and lipid metabolism via the CDK4-pRB-E2F1 signaling pathway by using E2F1−/− mice [25,26,27,28,29,30,31]. However, the exact mechanism by which E2F1 regulates adipocyte differentiation and affects metabolic diseases remains unclear.
To date, although the interplay between E2F1 and β-catenin has been demonstrated, whether the alleviation of obesity-associated metabolic disease, especially chronic inflammation, can be modulated by activating the Wnt/β-catenin through inhibition of ICAT activity is still unknown. Our previous study overexpressing or interfering with the expression of ICAT with siRNA in 3T3-L1 pre-adipocytes has proved that E2F1 can regulate lipogenesis by activating ICAT [32, 33]. Here, we constructed the adipose tissue-specific ICAT knockout mice to illustrate the effects of ICAT on body weight, fat mass, glucose homeostasis, lipid metabolism, and inflammatory response.
Methods
Reagents
Assay kits of triglycerides (TGs), total cholesterol (T-CHO), low density lipoprotein cholesterol (LDL-C), high density lipoprotein cholesterol (HDL-C), aspartate transaminase (AST), and alanine transaminase (ALT) were purchased from Nanjing Jiancheng Bioengineering Institute (Nanjing, China). Primary antibodies against PPARγ, C/EBPα, c-Myc, and β-catenin were obtained from Cell Signaling Technology (Beverly, MA, USA). Antibodies against HSL and E2F1 were purchased from Santa Cruz Biotechnology (Santa Cruz, CA, USA). Antibody against ICAT was purchased from Abcam (Cambridge, UK), and antibodies against UCP1, AMPK, p-AMPK, ATGL, ACC, FASN, Cyclin D1 were products of Proteintech (Chicago, IL, USA). Horseradish peroxidase (HRP)-conjugated GAPDH and β-actin were purchased from Yeasen Biotechnology (Shanghai, China). Horseradish peroxidase (HRP)-conjugated goat anti-rabbit, and rabbit anti-mouse secondary antibodies were purchased from Sangon Biotech Co (Shanghai, China). Fluorescein-labeled anti-bodies against CD68+ and F4/80+ in immunofluorescence staining were purchased from BioLegend (San Diego, CA, USA). TRIzol Reagent was purchased from Aidlab Biotechnologies (Beijing, China), FastQuant RT Kit was obtained from Yeasen Biotechnology (Shanghai, China). SYBR Premix EX Taq was obtained from Takara (Dalian, China). Hematoxylin and eosin (H&E) kit and Sirius red were products of Yeasen Biotechnology (Shanghai, China). The normal-fat diet (ND, D12450B) and high-fat diet (HFD, D12492) were purchased from Research Diets (New Brunswick, NJ, USA). Unless stated, all other chemicals were purchased from Sigma-Aldrich (St. Louis, MO, USA).
Animals and Diet
To generate adipose-specific ICAT knockout mice, the adiponectin-cre (Adipoq-cre) mice on a C57BL/6 J background (purchased from Jackson Laboratories) were used. Mice were crossed with homozygous for ICATflox/flox and heterozygous for Adipoq-cre to generate ICAT KO (ICATadi−/−) mice and control ICATfl/fl littermates. In the present study, the ICATadi−/− mice (6–8 weeks, male) were compared with the ICATfl/fl mice (6–8 weeks, male). In the first experiment, both the ICATadi−/− and ICATfl/fl mice were fed with a normal-fat diet (ND) for 12 weeks; mice were fed with a high-fat diet (HFD) for 12 weeks in the second experiment. At the end of the experiment, peripheral blood was obtained from retro-orbital the sinus of mice. Thereafter, the liver, spleen, kidney, inguinal WAT (iWAT), epididymal WAT (eWAT), perirenal WAT (pWAT), and brown adipose tissue (BAT) were collected and weighed. Small pieces of liver and adipose tissue were fixed in 4% formaldehyde solution for morphological examination, and the remaining tissue was immediately frozen in liquid nitrogen and stored at − 80℃ for later analysis.
Oral Glucose Tolerance Test (OGTT)
Mice in each group were fasted overnight with free access to water, and each mouse orally received a glucose load with 2 g glucose/kg body weight. The OGTT was carried out one week before the end of the whole trial. Blood collected from the tail vein was used to measure blood glucose concentration at 0, 30, 60, 90, and 120 min after the administration of glucose by using a glucometer (Johnson & Johnson, USA).
Serum Biochemical Analyses
Serum ALT, AST, TGs, TC, LDL-C, and HDL-C were measured by using commercial kits (Nanjing Jiancheng Bioengineering Institute), as the manufacturer instructed. The concentration of each index was calculated according to the formula provided in the instruction.
Adipose Tissue and Liver Histopathological Examination
Briefly, samples were fixed in paraformaldehyde for 24 h and then stored in 70% alcohol until analysis. After a series of steps of dehydration, the tissue was embedded in paraffin and then cut into thin slices with a thickness of 5–10 μm for eosin-hematoxylin (H&E) or Sirius red (fibrosis) staining. The adipocyte area was quantified by counting six visual fields of each slice.
Immunofluorescence Staining
Tissue embedded in the OCT compound was prepared into five-micrometer sections with a Cryotome FSE cryostat (Leica Company, Germany). Then, the tissue sections were immobilized with ice acetone for 20 min, and treated with 0.3% H2O2 for 30 min. After washing with phosphate buffered solution (PBS), sections were blocked by 5% BSA (diluted in PBS) for 30 min at room temperature. Tissue sections were stained with fluorescein-labeled primary antibodies (CD68+ or F4/80+) overnight at 4℃. Nuclei were visualized by counterstaining with Hoechst 33,342. Sections of each mouse (n = 6) were visualized and recorded by using a fluorescence microscope (Axio Vert.A1, Zeiss).
Quantitative Real-time PCR
According to the manufacturers’ instructions, total RNA of adipose tissue and the liver were extracted with TRIzol Reagent, and then were reverse-transcribed into cDNA, after which RT-qPCR was performed with 25 ng of cDNA with the ABI-Prism 7500 Sequence Detection System (Applied Biosystems). The 2−∆∆Ct method was used to measure the fold-change of gene expression levels, and the Gapdh was used for the normalization of target genes. The primer sequences are listed in Supplementary Table 1.
Western Blotting Analysis
Adipose tissue and the liver were homogenized with radio-immunoprecipitation assay (RIPA) buffer added with protease and phosphatase inhibitors (MedChemExpress LLC, Shanghai, China) on ice for 30 min. Then, the homogenates were centrifuged at 12,000 × g for 20 min at 4 °C and supernatants were collected as the total protein. As the adipose tissue contained a mass of fat, it should be centrifuged three times to remove fat from the supernatant. Total protein abundance was quantified using the BCA method. Identical amounts of proteins (50 μg) were used to analyze the abundance of target proteins as described previously [34]. Protein bands were measured by the Image Quant LAS 4000 mini system (GE Healthcare, NJ, USA), and the density of protein bands was analyzed by the ImageJ software.
Statistical Analysis
Data are presented as means ± SEM using the GraphPad Prism 7.0 software (GraphPad Software, San Diego, CA, USA). The statistical analysis was carried out in SPSS (Version 19.0) (SPSS, Inc., Chicago, IL, USA) and significance was determined by Unpaired Student’s t-test with ∗ p < 0.05, ∗∗ p < 0.01, and ∗∗∗ p < 0.001.
Results
Effects of ICAT on Body Weight and Tissue Weight in Mice Fed Normal-Fat Diet
To investigate the role of ICAT in regulating adipogenesis, the adipose tissue-specific ICAT knockout (ICATadi−/−) mice were constructed by crossing ICATflox/flox (ICATfl/fl) mice with adiponectin-cre mice. Results showed that the adipose tissue-specific ICAT knockout mice were obtained (Supplementary Fig. 1). Furthermore, no differences on body weight, tissue weight, TG and T-CHO in serum, and blood glucose concentration were observed in ICATadi−/− mice when compared with the ICATfl/fl mice (Fig. 1). However, adipocyte area of iWAT in ICATadi−/− mice was enlarged as indicated by H&E staining (Supplementary Fig. 2a and b).
Body weight and tissue weight of ICATadi−/− mice fed with normal-fat diet for 12 weeks. a Representative photographs of mice body size and adipose tissue. b Body weight of ICATfl/fl and ICATadi−/− mice. c Organ and tissue weight. d Serum levels of blood glucose, TG, T-CHO, HDL-C, and LDL-C. e Glucose tolerance test. Data are means ± SEM, n = 6. eWAT, epididymal WAT; iWAT, inguinal WAT; pWAT, perirenal WAT; BAT, brown adipose tissue; HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; T-CHO, total cholesterol; TG, triglyceride.
Effects of ICAT on Body Weight and Tissue Weight in Mice Fed High-Fat Diet
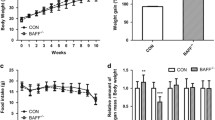
No differences were observed in body weight and fat mass of mice fed a normal diet. Next, mice were fed a high-fat diet to recapitulate lipogenesis to investigate the effect of ICAT on body weight and tissue weight. Nevertheless, the ablation of ICAT exerted no effects on the body weight, tissue weight, and TG and T-CHO in serum (Fig. 2). Additionally, enlarged adipocyte diameter of iWAT was found in ICATadi−/− mice fed high-fat diet (Fig. 2d and e), in line with the result observed in mice fed normal-fat diet. Furthermore, H&E staining results showed more crown-like structures in WAT in the ICATfl/fl mice than ICATadi−/− mice (Fig. 2d).
Body weight and tissue weight of ICATadi−/− mice fed with high-fat diet for 12 weeks. a Representative photographs of mice body size and adipose tissue. b Body weight of ICATfl/fl and ICATadi−/− mice. c Organ and tissue weight. d H&E staining of iWAT and eWAT. Classical crown-like structures surrounding individual adipocytes were pointed out by black arrow. e Adipocyte area of iWAT and eWAT. f Serum levels of blood glucose, TG, T-CHO, HDL-C, and LDL-C. g Glucose tolerance test. Data are means ± SEM, n = 6. eWAT, epididymal WAT; iWAT, inguinal WAT; pWAT, perirenal WAT; BAT, brown adipose tissue; HDL-C, high-density lipoprotein cholesterol; LDL-C, low-density lipoprotein cholesterol; T-CHO, total cholesterol; TG, triglyceride.
Effects of ICAT on Expression of Lipid Metabolism-Related Proteins in WAT
Our previous study on 3T3-L1 pre-adipocytes demonstrated that knocking down ICAT inhibited adipocyte differentiation [32]. As shown in Fig. 2, adipose tissue-specific knockout of ICAT did not affect adipogenesis (Fig. 2), which prompted us to explore the cause of this finding. Furthermore, expression of proteins involved in anabolic processes of lipid metabolism, such as C/EBPα, PPARγ, and fatty acid synthase (FASN), as well as expression of proteins (adipose triglyceride lipase, ATGL; hormone-sensitive lipase, HSL) involved in catabolic processes, were not obviously changed in the ICATadi−/− mice when compared with the ICATfl/fl mice (Fig. 3). However, ICAT knockout reduced the protein expression of acetyl-CoA carboxylase (ACC, lipid synthesis-related protein) and uncoupling protein 1 (UCP1, energy metabolism-related protein) in iWAT, and ACC in eWAT (Fig. 3a and c). ICAT is downstream of E2F1 and only affects the binding of β-catenin to TCF4, without inhibition of β-catenin activity [32]. Correspondingly, the abundance of E2F1 and β-catenin was similar between the ICATadi−/− mice and ICATfl/fl mice (Fig. 3b and d). Interestingly, the protein level of c-Myc (one of the target genes of Wnt/β-catenin signaling) was not changed, but the protein level of Cyclin D1 (another target gene of Wnt/β-catenin signaling) enhanced significantly both in the iWAT and eWAT of ICATadi−/− mice (Fig. 3b and d).
Adipose tissue-specific knockout of ICAT had no effect on the expression of lipid metabolism-related proteins. a Expression of proteins involved in adipogenesis (C/EBPα, PPARγ, FASN, and ACC), lipolysis (ATGL and HSL), and energy metabolism (AMPK and UCP1) of iWAT. b Expression of proteins related to the Wnt/β-catenin pathway of iWAT. c Expression of proteins involved in adipogenesis (C/EBPα, PPARγ, FASN, and ACC), lipolysis (ATGL and HSL), and energy metabolism (AMPK and UCP1) of eWAT. d Expression of proteins related to the Wnt/β-catenin pathway of eWAT. Data are means ± SEM, n = 6. eWAT, epididymal WAT; iWAT, inguinal WAT; ACC, acetyl-CoA carboxylase; AMPK, adenosine 5′-monophosphate-activated protein kinase; ATGL, adipose triglyceride lipase; β-actin, C/EBPα, CAAT/enhancer binding protein α; E2F1, E2 promoter binding factor 1; FASN, fatty acid synthase; GAPDH, glyceraldehyde-3-phosphate dehydrogenase; HSL, hormone-sensitive lipase; PPARγ, peroxisome proliferators-activated receptor γ; UCP1, uncoupling protein 1.
Effects of ICATadi−/− on Expression of Lipid Metabolism-Related Proteins in the Liver
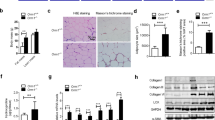
In addition to adipose tissue, the liver also plays a central role in lipid homeostasis. The H&E staining result showed lipid accumulation in the liver of mice fed with HFD (Fig. 4a). However, no difference in liver lipid accumulation was observed between the ICATadi−/− mice and ICATfl/fl mice (Fig. 4a). Furthermore, activities of ALT and AST (markers of liver injury) (Fig. 4b and c) and expression levels of lipid metabolism-related proteins did not differ between the two groups (Fig. 4d and e).
Effect of ICATadi−/− on the liver lipid metabolism. a Representative photographs and H&E staining of the liver. Serum level of AST (b) and ALT (c). d Expression of proteins involved in lipid metabolism of the liver. e Expression of proteins related to the Wnt/β-catenin pathway of the liver. Data are means ± SEM, n = 6. ACC, acetyl-CoA carboxylase; ALT, alanine transaminase; AMPK, adenosine 5′-monophosphate-activated protein kinase; AST, aspartate transaminase; ATGL, adipose triglyceride lipase; E2F1, E2 promoter binding factor 1; FASN, fatty acid synthase; GAPDH, glyceraldehyde-3-phosphate dehydrogenase; HSL, hormone-sensitive lipase; PPARγ, peroxisome proliferators-activated receptor γ.
Effects of Deletion of ICAT on Adipose Tissue Fibro-inflammation
Obesity is usually accompanied by inflammation and fibrosis. Immunofluorescence staining results showed that deletion of ICAT reduced macrophage infiltration in adipose tissue caused by high-fat diet, indicated by the decreased CD68+ and F4/80+ positive macrophages in the ICATadi−/− mice (Fig. 5a). Notably, mRNA levels of proinflammatory cytokines (IL-6, TNF-α, and IL-1β) and chemokines (CCL2 and CCL3) in the iWAT and eWAT were remarkably reduced in the ICATadi−/− mice when compared with the ICATfl/fl mice (Fig. 5b). In addition, Sirius red staining showed that there was a certain degree of fibrosis around the adipocytes of iWAT and eWAT in the ICATfl/fl mice (Fig. 5c). However, ICAT knockout reduced the fiber and mRNA levels of fibrosis-related genes (TGF-β1, Mmp3 and Col5a1 in iWAT; TGF-β1, Mmp2, Mmp3 and Col5a1 in eWAT) (Fig. 5d). These results suggested that ablation of ICAT in adipose tissue could alleviate the inflammatory response caused by obesity, which might contribute to the reduction of fibrosis.
ICATadi−/− improved fibro-inflammation of WAT. a Immunofluorescent staining of CD68+ and F4/80+ macrophages (red) in WAT. Nuclei were stained with Hoechst 33,342 (blue). b Relative mRNA levels of inflammation-related genes. c Sirius red staining of iWAT and eWAT. d Relative mRNA levels of fibrosis-related genes. Data are means ± SEM, n = 6. eWAT, epididymal WAT; iWAT, inguinal WAT; CCL, chemokine (C–C motif) ligand; Col5a1, collagen, type V, alpha 1; IL-6, interleukin 6; IL-1β, interleukin 1β; Mmp2, matrix metallopeptidase 2; Mmp3, matrix metallopeptidase 2; TGF-β1, transforming growth factor β1; TNF-α, tumor necrosis factor α; Timp2, tissue inhibitor of metalloproteinase 2.
Effects of ICATadi−/− on Liver Fibro-inflammation
Under the stimulation of the high-fat diet, fibrosis appeared in the liver of mice (Fig. 6a). Interestingly, deletion of ICAT in adipose tissues also reduced the fibrosis of the liver and decreased the mRNA levels of TGF-β1, Mmp2, and Col5a1 (Fig. 6b). In addition, CD68+ and F4/80+ positive macrophages (Fig. 6c and d), and mRNA expressions of IL-6, IL-1β, and CCL2 (Fig. 6e) were also significantly reduced in ICATadi−/− mice. Of note, the fatty acid oxidation capacity of the liver in ICATadi−/− mice was improved and reflected by the increased mRNA levels of fatty acid oxidation-related genes (Fig. 6f). These results indicated that adipose tissue-specific knockout of ICAT could relieve liver fibrosis and inflammation.
ICATadi−/− alleviated the liver fibro-inflammation. a Sirius red staining of the liver. b Relative mRNA levels of fibrosis-related genes. c Immunofluorescent staining of CD68+ and F4/80+ macrophages in the liver. d Number of CD68+ and F4/80+ positive macrophages (red). Nuclei were stained with Hoechst 33,342 (blue). e Relative mRNA levels of inflammation-related genes. f Relative mRNA levels of genes related to fatty acid oxidation. Data are means ± SEM, n = 6. Acox1, acyl-Coenzyme A oxidase 1; CCL, chemokine (C–C motif) ligand; Col5a1, collagen, type V, alpha 1; Cpt1α, carnitine palmitoyl-transferase 1α; CytoC, cytochrome C; IL-6, interleukin 6; IL-1β, interleukin 1β; Mmp2, matrix metallopeptidase 2; Mmp3, matrix metallopeptidase 2; Pgc-1α, peroxisome proliferator-activated receptor-γ coactivator-1α; Pparα, peroxisome proliferator activated receptor α; TGF-β1, transforming growth factor β1; TNF-α, tumor necrosis factor α; Timp2, tissue inhibitor of metalloproteinase 2; a-SMA, actin alpha 2.
Discussion
The increasing population of obese subjects over the past several decades has been one of the most prevalent public health problems. Obesity and obesity-associated metabolic diseases have reduced life quality and life span and increased social and economic burdens [4, 5]. A growing number of researchers have devoted themselves to studying the mechanism of obesity and its comorbidities, and potential obesity-related target genes have been discovered. In our previous study on the effects of ICAT on differentiation and adipogenesis of 3T3-L1 cells, we suggested that ICAT may be a potential target gene in alleviating obesity and obesity-related diseases [23, 32]. To further investigate the exact role of ICAT on obesity, adipose tissue-specific ICAT knockout mice were generated in the present study regarding embryonic lethality of the global knockout of ICAT [33]. In the present study, deletion of ICAT in mice fed with HFD ameliorated fibrosis and inflammation in adipose tissue and the liver, but did not affect the BW, fat mass, and glucose tolerance. These findings might provide a new hint on E2F1 and the relationship between E2F1and ICAT.
The E2Fs family, an important transcription factor family, regulates apoptosis, DNA synthesis, and cell cycle progression [35]. A previous study revealed that E2F1, E2F2, and E2F3 directly stimulate adipogenesis by activating PPARγ, and E2F1−/− mice were resistant to obesity. Conversely, the E2F4 negatively regulates adipogenesis [36]. Accumulating studies documented that E2F1 play a key role in regulating oxidative metabolism of muscle and BAT [26], nonalcoholic fatty liver disease (NAFLD) [27], hepatic gluconeogenesis [28], liver fibrosis [29], and autophagy of adipose tissue [16, 31]. The CDK4-pRB is the upstream of E2F1 and is essential for E2F1 to exert its functions [19, 25, 30], but the downstream of E2F1 is largely unknown. Notably, the ICAT was identified as the direct target gene of E2F1 in our previous work [23].
Considering the importance of Wnt/β-catenin pathway in lipid metabolism and inhibition activity of ICAT on β-catenin and TCF4 [37], the functional role of ICAT on obesity was firstly validated in 3T3-L1 cells. Indeed, E2F1 promoted the differentiation of 3T3-L1 pre-adipocytes by inhibiting the activity of Wnt/β-catenin signaling through activating ICAT [32]. By contrast, adipose tissue-specific knockout of ICAT was found to be unable to reduce adipogenesis in the present study. The inconsistent results obtained between 3T3-L1 pre-adipocytes model and in vivo model is probably because the differentiation of 3T3-L1 pre-adipocytes can not fully represent the complex regulatory mechanism of adipogenesis in vivo. Additionally, β-catenin is phosphorylated in a destruction protein complex, composed of glycogen synthase kinase 3 (GSK3), scaffold protein Axin, tumor suppressor adenomatous polyposis coli (APC), glycogen synthase kinase and casein kinase 1a (CK1a), in the absence of Wnt ligands. Phosphorylated β-catenin is recognized and ubiquitinated by the β-TrCP E3 ligase and eventually is degraded by the proteasome [38]. Although ICAT was initially identified as an inhibitor of β-catenin signal, it was recently demonstrated that ICAT plays a positive role in regulating the Wnt/β-catenin signal by blocking APC-mediated β-catenin degradation [39]. Knockout of ICAT decreased β-catenin level in cytosolic but almost did not affect the expression of β-catenin target genes [39]. The reduced cytosolic β-catenin upon the knockout of ICAT was probably counterbalanced by enhanced capability of other β-catenin molecules to bind to TCF and to regulate downstream target gene transcription, which suggested that ICAT affected the final function of β-catenin signal in a context-dependent manner [39]. Hence, other β-catenin molecules might play a compensatory role after the knockout of ICAT in adipose tissue, resulting in no change in adipogenesis of mice.
As illustrated in Fig. 3, although adipogenesis seemed to be enhanced in the ICATadi−/− mice as reflected by the elevated protein expression of C/EBPα and UCP1 in iWAT and PPARγ in eWAT, and enlarged diameter of adipocytes in iWAT. However, the abundance of ACC was reduced in iWAT and eWAT, and Cyclin D1 abundance (a target of β-catenin signal) was enhanced, which was positive with adipogenesis inhibition [32]. The mutual restriction and balance between proteins with different functions might eventually lead to no difference between the ICATadi−/− and ICATfl/fl mice fed with HFD.
For decades, adipose tissue was regarded only as an energy store. In 2003, two articles highlighted the infiltration of macrophages in expanding adipose tissue [40, 41], which established the basis that adipose tissue is also an important endocrine organ and regulates immune metabolism and homeostasis [3, 42]. Macrophages are the most abundant immune cells in adipose tissue, accounting for 40% of stromal vascular cells [43]. As the severity of obesity increases, macrophages usually change from M2 to M1, and the secretion of TNF-α, IL-6, IL-1β and some other proinflammatory cytokines in adipose tissue increases [3, 42]. However, due to the limited techniques and methods for adipose tissue treatment, it is not clear whether the cytokine and chemokines secreted in adipose tissue are derived from adipocytes or macrophages. In 2013, at the single-cell level, Lindsey et al. concluded that TNF-α was derived from macrophages rather than adipocytes by using three-dimensional image analysis and confocal immunohistochemistry technology [44]. While IL-10, which was also reported to be elevated in obese individuals, was only marginally derived from macrophages. These results have demonstrated the tight and complex association between adipocytes and macrophages during the development of obesity. On other hand, it has been proved that E2F1 may be a new immunomodulatory factor [45,46,47]. In the present study, H&E results showed obvious crown-like structures surrounding some adipocytes, and there were more of them in ICATfl/fl mice than in ICATadi−/− mice, which prompted us to explore whether knockout of ICAT could affect inflammatory response. Indeed, results showed that macrophage markers CD68+ and F4/80+, and mRNA levels of proinflammatory cytokines (IL-6, IL-1β, and TNF-α) and chemokines (CCL2 and CCL3) in iWAT and eWAT were both significantly decreased in the ICATadi−/− mice when compared with the ICATfl/fl mice. The alleviation of inflammation was consistent with previous studies, which reported that the expression of E2F1 in the liver, spleen, and lung of mice was elevated when stimulated by systemic lipopolysaccharide (LPS) [47], while the inflammatory response was inhibited in E2F1−/− mice [46]. In addition, our study reported an elevated expression of E2F1 in HFD-fed mice (Supplementary Fig. 3a and b), which was consistent with a previous study suggesting inflammation stimulates E2F1 expression [16].
Excessive obesity often leads to fibrosis, which is characterized by the excessive deposition of components of the extracellular matrix (ECM). In obese subjects, excessive collagen accumulates around adipocytes, resulting in fibrosis and affecting the plasticity of adipose tissue [48]. The TGF-β1 signaling is one of the main pathways involved in regulating fibrosis. TGF-β1 modulates collagen, matrix metalloproteinases (MMPs), inhibitors of metalloproteinases (TIMPs), and integrin transmembrane proteins to perpetuate fibrosis through activating transcription factor SMAD2 and SMAD3 [49,50,51]. Interestingly, in the present study, both the Sirius red staining and related gene expression results showed that the fibrosis in ICATadi−/− mice was reduced, which suggested that E2F1/ICAT might be a new target for improving fibrosis during obesity.
In obesity, adipocyte hypertrophy usually means more dysfunctional effects on the body, such as insulin resistance and inflammation [42, 52]. However, results in the present study showed that inflammatory response of adipose tissue was reduced in ICATadi−/− mice when compared with the ICATfl/fl mice, despite the larger adipocyte size. This interesting result may be related to the more severe fibrosis in the ICATfl/fl mice. E2F1 has previously been shown to be associated with fibrosis [29], and ICAT is a target gene of E2F1, so knockout of ICAT may have an effect on fibrosis. Adipocytes need to expand to store excess energy, studies have indicated that fibrosis restricts adipose tissue plasticity and limits the expansion of adipocytes [53, 54]. Furthermore, fibrosis itself alters adipocyte metabolism, such as decreasing lipolysis, and in turn, further increasing the secretion of proinflammatory cytokines [48, 55]. Therefore, the improvement of adipose tissue inflammation may benefit from the reduction of fibrosis. Nevertheless, the role of ICAT and E2F1 in contributing to reducing fibrosis and inflammation needs to be further investigated.
Similarly, ICATadi−/− had no significant effect on liver lipid metabolism when compared with ICATfl/fl mice. Surprisingly, the mRNA level of ICAT in the liver of ICATadi−/− mice was significantly higher than in the ICATfl/fl mice when fed with HFD (Supplementary Fig. 3d). This variation may be a compensatory mechanism between different tissues, so liver fibrosis was also determined in the present study. During the progress of liver fibrosis, hepatic stellate cells are activated and lead to the overexpression of α-SMA and ECM secretion [56]. In the present study, we found that fibrosis was not particularly apparent and only collagen deposition was present in the liver because of the insufficient induction time by feeding the high-fat diet. However, the Sirius red result showed that deposition of collagen decreased in ICATadi−/− mice. Consistently, mRNA levels of TGF-β1, Col5a1, and Mmp2 were significantly reduced in the ICATadi−/− mice when compared with ICATfl/fl mice. Lai et al. found that the knockout of E2F1 induced liver fibrosis in mice [29]. Since ICAT is downstream of E2F1, the increased expression of ICAT might amplify the regulatory effect of E2F1 on the liver, thus reducing liver fibrosis. In addition, compared with ICATfl/fl mice, inflammatory cell infiltration and mRNA levels of IL-6, IL-1β, and CCL2 in the liver were also reduced in the ICATadi−/− mice, which indicated the high fat diet-induced inflammation in the liver was alleviated. The increase of free fatty acids (FAAs) in the liver may cause lipotoxicity, induce mitochondrial dysfunction, and aggravate liver inflammation and hepatocyte degeneration [57]. Our results showed that the mRNA levels of fatty acid oxidation-related genes were significantly reduced in the liver of the ICATadi−/− mice, which might help to suppress the inflammatory response of the liver. The liver-specific ICAT knockout mice and more advanced murine models are needed to further investigate the role of ICAT in inflammation and fibrosis.
Conclusion
Collectively, our study showed that adipose tissue-specific ICAT knockout had no effect on overall lipid metabolism. Moreover, the deletion of ICAT alleviated fibrosis and inflammation in white adipose tissue and the liver in obese mice. These findings might facilitate future investigations to reveal more accurate mechanism of ICAT in regulating fibrosis and inflammation.
Data Availability
Data that support the results of the present study are available from the corresponding author upon reasonable request.
Abbreviations
- eWAT:
-
Epididymal WAT
- iWAT:
-
Inguinal WAT
- ACC:
-
Acetyl-CoA carboxylase
- C/EBPα:
-
CAAT/enhancer binding protein α
- Col5a1 :
-
Collagen, type V, alpha 1
- E2F1:
-
E2 promoter binding factor 1
- ICAT:
-
β-Catenin interacting protein 1 (CTNNBIP1), inhibitor of β-catenin and TCF4
- Mmp2 :
-
Matrix metallopeptidase 2
- PPARγ:
-
Peroxisome proliferators-activated receptor γ
- TGF-β1 :
-
Transforming growth factor β1
- Timp2 (3) :
-
Tissue inhibitor of metalloproteinase 2 (3)
- WAT:
-
White adipose tissue
References
Cinti, S. 2018. Adipose organ development and remodeling. Comprehensive Physiology 8 (4): 1357–1431.
Backdahl, J., L. Franzen, L. Massier, Q. Li, J. Jalkanen, H. Gao, et al. 2021. Spatial mapping reveals human adipocyte subpopulations with distinct sensitivities to insulin. Cell Metabolism 33 (9): 1869–1882.
Rosen, E.D., and B.M. Spiegelman. 2014. What we talk about when we talk about fat. Cell 156 (1–2): 20–44.
Worldwide trends in body-mass index, and underweight, overweight, and obesity from. 1975. to 2016: A pooled analysis of 2416 population-based measurement studies in 128·9 million children, adolescents, and adults. Lancet 390 (10113): 2627–2642.
Hogan, P., T. Dall, and P. Nikolov. 2003. Economic costs of diabetes in the US in 2002. Diabetes Care 26 (3): 917–932.
Flier, J.S. 2004. Obesity wars: Molecular progress confronts an expanding epidemic. Cell 116 (2): 337–350.
Ellulu, M.S., I. Patimah, H. Khaza’ai, A. Rahmat, and Y. Abed. 2017. Obesity and inflammation: The linking mechanism and the complications. Archives of Medical Science 13 (4): 851–863.
Xu, L., N. Nagata, and T. Ota. 2018. Glucoraphanin: A broccoli sprout extract that ameliorates obesity-induced inflammation and insulin resistance. Adipocyte 7 (3): 218–225.
Tang, Q.Q., and M.D. Lane. 2012. Adipogenesis: From stem cell to adipocyte. Annual Review of Biochemistry 81: 715–736.
Cawthorn, W.P., F. Heyd, K. Hegyi, and J.K. Sethi. 2007. Tumour necrosis factor-alpha inhibits adipogenesis via a beta-catenin/TCF4(TCF7L2)-dependent pathway. Cell Death and Differentiation 14 (7): 1361–1373.
Chen, M., P. Lu, Q. Ma, Y. Cao, N. Chen, W. Li, et al. 2020. CTNNB1/β-catenin dysfunction contributes to adiposity by regulating the cross-talk of mature adipocytes and preadipocytes. Science Advance 6(2): eaax9605.
Christodoulides, C., A. Scarda, M. Granzotto, G. Milan, E. Dalla Nora, J. Keogh, et al. 2006. WNT10B mutations in human obesity. Diabetologia 49 (4): 678–684.
Mattei, J., Q. Qi, F.B. Hu, F.M. Sacks, and L. Qi. 2012. TCF7L2 genetic variants modulate the effect of dietary fat intake on changes in body composition during a weight-loss intervention. American Journal of Clinical Nutrition 96 (5): 1129–1136.
Bowers, R.R., and M.D. Lane. 2008. Wnt signaling and adipocyte lineage commitment. Cell Cycle 7 (9): 1191–1196.
Rosen, E.D., and O.A. MacDougald. 2006. Adipocyte differentiation from the inside out. Nature Reviews: Molecular Cell Biology 7 (12): 885–896.
Haim, Y., M. Bluher, N. Slutsky, N. Goldstein, N. Kloting, I. Harman-Boehm, et al. 2015. Elevated autophagy gene expression in adipose tissue of obese humans: A potential non-cell-cycle-dependent function of E2F1. Autophagy 11 (11): 2074–2088.
Julien, C., B. Le-Bail, K. Ouazzani Touhami, N. Frulio, J.F. Blanc, J.P. Adam, et al. 2021. Hepatocellular adenoma rrisk factors of hemorrhage: Size is not the only concern!: Single-center retrospective experience of 261 patients. Annals of Surgery 274 (5): 843–850.
Luke, J.J., R. Bao, R.F. Sweis, S. Spranger, and T.F. Gajewski. 2019. WNT/β-catenin pathway activation correlates with immune exclusion across human cancers. Clinical Cancer Research 25 (10): 3074–3083.
Mandigo, A.C., W. Yuan, K. Xu, P. Gallagher, A. Pang, Y.F. Guan, et al. 2021. RB/E2F1 as a master regulator of cancer cell metabolism in advanced disease. Cancer Discovery 11 (9): 2334–2353.
Chun, J.N., M. Cho, S. Park, I. So, and J.H. Jeon. 2020. The conflicting role of E2F1 in prostate cancer: A matter of cell context or interpretational flexibility? Biochimical et Biophysica Acta-Review on Cancer 1873 (1): 188336.
Morris, E.J., J.Y. Ji, F. Yang, L. Di Stefano, A. Herr, N.S. Moon, et al. 2008. E2F1 represses beta-catenin transcription and is antagonized by both pRB and CDK8. Nature 455 (7212): 552–556.
Zhao, J., R. Ramos, and M. Demma. 2013. CDK8 regulates E2F1 transcriptional activity through S375 phosphorylation. Oncogene 32 (30): 3520–3530.
Wu, Z., S. Zheng, Z. Li, J. Tan, and Q. Yu. 2011. E2F1 suppresses Wnt/beta-catenin activity through transactivation of beta-catenin interacting protein ICAT. Oncogene 30 (37): 3979–3984.
Wells, J., C.R. Graveel, S.M. Bartley, S.J. Madore, and P.J. Farnham. 2002. The identification of E2F1-specific target genes. Proceedings of the National Academy of Sciences of the United States of America 99 (6): 3890–3895.
Annicotte, J.S., E. Blanchet, C. Chavey, I. Iankova, S. Costes, S. Assou, et al. 2009. The CDK4-pRB-E2F1 pathway controls insulin secretion. Nature Cell Biology 11 (8): 1017–1023.
Blanchet, E., J.S. Annicotte, S. Lagarrigue, V. Aguilar, C. Clape, C. Chavey, et al. 2011. E2F transcription factor-1 regulates oxidative metabolism. Nature Cell Biology 13 (9): 1146–1152.
Denechaud, P.D., I.C. Lopez-Mejia, A. Giralt, Q. Lai, E. Blanchet, B. Delacuisine, et al. 2016. E2F1 mediates sustained lipogenesis and contributes to hepatic steatosis. Journal of Clinical Investigation 126 (1): 137–150.
Giralt, A., P.D. Denechaud, I.C. Lopez-Mejia, B. Delacuisine, E. Blanchet, C. Bonner, et al. 2018. E2F1 promotes hepatic gluconeogenesis and contributes to hyperglycemia during diabetes. Molecular Metabolism 11: 104–112.
Lai, Q., A. Giralt, C. Le May, L. Zhang, B. Cariou, P. D. Denechaud, et al. 2017. E2F1 inhibits circulating cholesterol clearance by regulating Pcsk9 expression in the liver. Junior Chamber International Insight 2(10).
Lu, Z., G. Marcelin, F. Bauzon, H. Wang, H. Fu, S.L. Dun, et al. 2013. pRb is an obesity suppressor in hypothalamus and high-fat diet inhibits pRb in this location. The EMBO Journal 32 (6): 844–857.
Xiong, M., W. Hu, Y. Tan, H. Yu, Q. Zhang, C. Zhao, et al. 2021. Transcription factor E2F1 knockout promotes mice white adipose tissue browning through autophagy inhibition. Frontiers in Physiology 12: 748040.
Chen, J., Y. Yang, S. Li, Y. Yang, Z. Dai, F. Wang, et al. 2020. E2F1 regulates adipocyte differentiation and adipogenesis by activating ICAT. Cells 9(4): 1024.
Satoh, K., M. Kasai, T. Ishidao, K. Tago, S. Ohwada, Y. Hasegawa, et al. 2004. Anteriorization of neural fate by inhibitor of beta-catenin and T cell factor (ICAT), a negative regulator of Wnt signaling. Proceedings of the National Academy of Sciences of the United States of America 101 (21): 8017–8021.
Jia, H., N. Liu, Y. Zhang, C. Wang, Y. Yang, and Z. Wu. 2021. 3-Acetyldeoxynivalenol induces cell death through endoplasmic reticulum stress in mouse liver. Environmental Pollution 286: 117238.
Kent, L.N., and G. Leone. 2019. The broken cycle: E2F dysfunction in cancer. Nature Reviews: Cancer 19 (6): 326–338.
Fajas, L., R.L. Landsberg, Y. Huss-Garcia, C. Sardet, J.A. Lees, and J. Auwerx. 2002. E2Fs regulate adipocyte differentiation. Developmental Cell 3 (1): 39–49.
Graham, T.A., W.K. Clements, D. Kimelman, and W. Xu. 2002. The crystal structure of the beta-catenin/ICAT complex reveals the inhibitory mechanism of ICAT. Molecular Cell 10 (3): 563–571.
Kim, S.E., H. Huang, M. Zhao, X. Zhang, A. Zhang, M.V. Semonov, et al. 2013. Wnt stabilization of β-catenin reveals principles for morphogen receptor-scaffold assemblies. Science 340 (6134): 867–870.
Ji, L., B. Lu, Z. Wang, Z. Yang, J. Reece-Hoyes, C. Russ, et al. 2018. Identification of ICAT as an APC inhibitor, revealing Wnt-dependent inhibition of APC-Axin interaction. Molecular Cell 72(1): 37–47 e34.
Xu, H., G.T. Barnes, Q. Yang, G. Tan, D. Yang, C.J. Chou, et al. 2003. Chronic inflammation in fat plays a crucial role in the development of obesity-related insulin resistance. Journal of Clinical Investigation 112 (12): 1821–1830.
Weisberg, S.P., D. McCann, M. Desai, M. Rosenbaum, R.L. Leibel, and A.W. Ferrante Jr. 2003. Obesity is associated with macrophage accumulation in adipose tissue. Journal of Clinical Investigation 112 (12): 1796–1808.
Skurk, T., C. Alberti-Huber, C. Herder, and H. Hauner. 2007. Relationship between adipocyte size and adipokine expression and secretion. Journal of Clinical Endocrinology and Metabolism 92 (3): 1023–1033.
Lee, Y.S., J. Wollam, and J.M. Olefsky. 2018. An integrated view of immunometabolism. Cell 172 (1–2): 22–40.
Ebke, L.A., A.L. Nestor-Kalinoski, B.D. Slotterbeck, A.G. Al-Dieri, S. Ghosh-Lester, L. Russo, et al. 2014. Tight association between macrophages and adipocytes in obesity: Implications for adipocyte preparation. Obesity (Silver Spring) 22 (5): 1246–1255.
Lim, C.A., F. Yao, J.J. Wong, J. George, H. Xu, K.P. Chiu, et al. 2007. Genome-wide mapping of RELA(p65) binding identifies E2F1 as a transcriptional activator recruited by NF-kappaB upon TLR4 activation. Molecular Cell 27 (4): 622–635.
Warg, L.A., J.L. Oakes, R. Burton, A.J. Neidermyer, H.R. Rutledge, S. Groshong, et al. 2012. The role of the E2F1 transcription factor in the innate immune response to systemic LPS. American Journal of Physiology: Lung Cellular and Molecular Physiology 303 (5): L391-400.
Yang, I.V., S. Alper, B. Lackford, H. Rutledge, L.A. Warg, L.H. Burch, et al. 2011. Novel regulators of the systemic response to lipopolysaccharide. American Journal of Respiratory Cell and Molecular Biology 45 (2): 393–402.
Marcelin, G., A.L.M. Silveira, L.B. Martins, A.V. Ferreira, and K. Clement. 2019. Deciphering the cellular interplays underlying obesity-induced adipose tissue fibrosis. Journal of Clinical Investigation 129 (10): 4032–4040.
Walton, K.L., K.E. Johnson, and C.A. Harrison. 2017. Targeting TGF-β mediated SMAD signaling for the prevention of fibrosis. Frontiers in Pharmacology 8: 461.
Bonnans, C., J. Chou, and Z. Werb. 2014. Remodelling the extracellular matrix in development and disease. Nature Reviews: Molecular Cell Biology 15 (12): 786–801.
Reed, N.I., H. Jo, C. Chen, K. Tsujino, T.D. Arnold, W.F. DeGrado, et al. 2015. The αvβ1 integrin plays a critical in vivo role in tissue fibrosis. Science Translational Medicine 7(288): ra79.
Jernås, M., J. Palming, K. Sjöholm, E. Jennische, P.A. Svensson, B.G. Gabrielsson, et al. 2006. Separation of human adipocytes by size: Hypertrophic fat cells display distinct gene expression. FASEB Journal 20 (9): 1540–1542.
Chun, T.H., K.B. Hotary, F. Sabeh, A.R. Saltiel, E.D. Allen, and S.J. Weiss. 2006. A pericellular collagenase directs the 3-dimensional development of white adipose tissue. Cell 125 (3): 577–591.
Kim, J.Y., E. van de Wall, M. Laplante, A. Azzara, M.E. Trujillo, S.M. Hofmann, et al. 2007. Obesity-associated improvements in metabolic profile through expansion of adipose tissue. Journal of Clinical Investigation 117 (9): 2621–2637.
Pellegrinelli, V., J. Heuvingh, O. du Roure, C. Rouault, A. Devulder, C. Klein, et al. 2014. Human adipocyte function is impacted by mechanical cues. Journal of Pathology 233 (2): 183–195.
Atzori, L., G. Poli, and A. Perra. 2009. Hepatic stellate cell: A star cell in the liver. International Journal of Biochemistry and Cell Biology 41 (8–9): 1639–1642.
Sano, A., E. Kakazu, S. Hamada, J. Inoue, M. Ninomiya, T. Iwata, et al. 2021. Steatotic hepatocytes release mature VLDL through methionine and tyrosine metabolism in a keap1-Nrf2-dependent manner. Hepatology 74 (3): 1271–1286.
Funding
This work was supported by the National Natural Science Foundation of China (No. 31625025 and No. 32000082), China Postdoctoral Science Foundation (No.2022M713405), and the 2115 Talent Development of China Agricultual University.
Author information
Authors and Affiliations
Contributions
All authors participated in the study and supported the publication. Zhenlong Wu designed and conducted the research. Material preparation, data collection, and analysis were performed by Zhuan Song, Ning Liu, Yu He, Jingqing Chen, and Jun Li. Fengchao Wang constructed the knockout mice. The draft of the manuscript was written by Zhuan Song.
Corresponding author
Ethics declarations
Ethics Approval
The experimental protocol was approved by the Protocol Management and Review Committee of China Agricultural University (Beijing, China). All mice were raised and conformed to the Institutional Animal Care and Use Committee of China Agricultural University (AW72602202-1–7).
Consent to Participate and Consent for Publication
Not applicable.
Conflict of Interest
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Song, Z., Liu, N., He, Y. et al. Knockout of ICAT in Adipose Tissue Alleviates Fibro-inflammation in Obese Mice. Inflammation 46, 404–417 (2023). https://doi.org/10.1007/s10753-022-01742-w
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-022-01742-w