Abstract
Ulcerative colitis (UC) has been considered a Th2- and Th17-related disease. However, anti-IL-12/23 p40 antibody, which blocks Th1 and Th17 cell induction and maintenance, has shown efficacy in treating UC, suggesting that UC might not be a prototypical Th2 and Th17 cell-mediated autoimmune disease. To verify how the immune responses in UC patients interact with each other, we analyzed the cytokine expression and transcription factors involved in the Th1, Th2, and Th17 responses. The mucosal expression of 19 cytokines and transcription factors related to Th1, Th2, and Th17 cells, as well as Tregs, were measured by quantitative polymerase chain reaction using endoscopic biopsy specimens from inflamed colons of UC patients. A correlation analysis between the cytokines and transcription factors was conducted. The characteristic cytokine profile in UC patients has two immune response clusters: Th17-related responses and Th1-/Th2-related responses. IL-23 showed a weaker association with Th17 cell-related cytokines and transcription factor RORC and a much stronger correlation with T-bet and GATA3. In the high-IL-23-expression group, the rate of chronic continuous type was higher and the remission rate lower than in the low-IL-23-expression group. IL-23 may be a very important cytokine for evaluating the UC disease condition, as the expression of IL-23 is associated with certain clinical characteristics of UC patients. A unique association between IL-23 and T-bet/GATA3 might play a key role in the pathogenesis of UC.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
INTRODUCTION
Inflammatory bowel disease (IBD), which includes ulcerative colitis (UC) and Crohn’ disease (CD), is characterized by chronic relapsing inflammation of the gastrointestinal tract. Although its exact etiology remains unknown, IBD has been reported to result from an exaggerated immune response to gut microbiota and environmental factors in genetically predisposed hosts [1].
Among the various immune cells that respond excessively in the intestinal mucosa, CD4+ helper T (Th) cells, including effecter T cells (Th1, Th2, and Th17) and suppressor T cells (regulatory T cells; Tregs), play a particularly important role in acquired immunity [2]. Changes in the balance between effector and suppressor T cells are involved in the pathogenesis of IBD, with a significant difference in the subtype of the effecter T cells noted between UC and CD. Based on in vitro experiments, UC is considered a Th2- and Th17-related disease, while CD is a Th1- and Th17-related disease [3,4,5]. Accumulated basic studies have revealed that Th1 cells induced by interleukin (IL)-12 (IL-12 p40/IL-12 p35) express the transcription factor T-bet and secrete interferon (IFN)-γ. Th2 cells, under stimulation with IL-4 and IL-33, express the transcription factor GATA3 and secrete IL-4 and IL-13. Th17 cells induced and maintained by IL-6, transforming growth factor (TGF)-β and IL-23 (IL-12 p40/IL-23 p19) express the transcription factor retinoic acid receptor– related orphan receptor (ROR) C and secrete IL-17A, IL-17F, IL-21, and IL-22 [5,6,7].
Recently developed biologic agents have revealed that the concept of these immune responses based on the findings of experimental colitis and in vitro studies cannot necessarily be applied to the pathogenesis of UC patients. Given that ustekinumab (UST), an anti-IL-12/23 p40 antibody, works against the induction and maintenance of Th1 and Th17 cells, we can reasonably expect UST to be effective for treating CD, where both Th1 and Th17 cells are involved [8]. However, UST has also been proven effective for the treatment of UC, which is considered a Th2- and Th17-related disease [9]. Furthermore, it has been shown that the anti-IL-13 antibody has no therapeutic effect on UC patients [10, 11], and anti-IL-17A antibody does not ameliorate but actually exacerbates colitis in UC patients [12,13,14], although these antibodies were shown to be effective on experimental colitis. How UC conditions are relieved by UST treatment remains unclear, but UC is indeed exacerbated by anti-IL-17A antibody in actual clinical practice.
UC has been suggested to not be a prototypical Th2- and Th17 cell-mediated autoimmune disease. Apparently, the concept based on the findings of basic studies, such as experimental colitis and in vitro studies, might not be sufficient to explain the pathogenesis of UC. The inflamed mucosa in the experimental colitis animal model may differ from that in UC patients, where CD4+ T cell subsets coexist with other cytokine-secreting cells, including innate lymphoid cells (ILCs), macrophages, granulocytes, and fibroblasts [1, 7, 15]. An analysis of human samples from UC patients is thus indispensable for clarifying the actual pathogenesis of UC.
We therefore hypothesized that the pathogenesis of UC could be clarified by evaluating the correlation with each transcription factor and cytokine, including Th-induced factors, in UC patients. Furthermore, that analysis might lead to the elucidation of the mechanism underlying the effects of UST on UC patients. Therefore, we conducted a correlation analysis of the cytokine expression and transcription factors involved in the Th1, Th2, and Th17 responses.
MATERIAL AND METHODS
Patient Enrollment and Mucosal Sample Collection
Between May 2010 and September 2016, patients with clinically active UC who visited outpatient units for scheduled colonoscopy at Kyushu University Hospital and two other referral centers were invited to participate in this observational study. A total of 51 UC patients were initially enrolled, but 13 whose treatment period was over 10 years and 3 with right-sided UC were excluded because the expression pattern of cytokines can be affected by a long disease duration and specific disease phenotype. As a result, a total of 35 patients were evaluated in this study.
The biopsy samples were obtained from the inflamed areas of the rectum during colonoscopy and immersed in RNAlater (Ambion, Austin, TX, USA) immediately after collection before being transferred to a freezer (− 30 °C) and stored until further use.
Collection of Clinical Information
The age at enrollment, age at onset, sex, family history of IBD, history of smoking, disease duration, endoscopic activity index using the Rachmilewitz score at enrollment, disease activity based on the Japanese diagnostic criteria for UC, extraintestinal manifestation, disease type, previous treatment, treatment after enrollment, and clinical response were obtained from the patients’ medical records. At 8 weeks after treatment, a clinical activity index (CAI) of < 4 was defined as clinical remission.
Extraction of RNA and Quantitative Real-Time Polymerase Chain Reaction
The gene expression in biopsy samples was examined as previously described. In brief, total RNA was extracted from whole biopsy tissues using TRIzol reagent (Invitrogen, Carlsbad, CA, USA), and its concentration and purity were measured at 260 and 280 nm using the NanoDrop ND-1000 UV/Vis spectrophotometer. cDNA was synthesized from 1-μg aliquots of RNA using a QuantiTect Reverse Transcription Kit (Qiagen, Valencia, CA, USA). The expression of mRNAs encoding cytokines and transcription factors was determined by a quantitative polymerase chain reaction (PCR) using TaqMan Gene Expression Assay Reagent (Applied Biosystems, Foster City, CA, USA). The targets were cytokines and transcription factors related to Th1 cells (IFN-γ, IL-12 p35, TNF-α, and T-bet), Th2 cells (IL-4, IL-13, IL-33, and GATA3), Th17 cells (IL-17A, IL-17F, IL-21, IL-22, IL-23 p19, and RORC), and Tregs (IL-10, TGF-β, forkhead box P3 [FoxP3]), using the primer-probe sets listed in Table 1. The cDNA equivalent of 10 ng of the RNA, specific primers, and TaqMan Universal PCR Master Mix, No AmpErase UNG (Applied Biosystems), was added to each well, the volume was adjusted to 20 μL, and thermal cycling reactions were performed using a 7500 Real-Time PCR System (Applied Biosystems). The amplification protocol consisted of initial denaturation at 95 °C for 10 min, followed by 45 cycles of denaturation at 95 °C for 15 s and annealing and extension at 60 °C for 60 s. The internal control consisted of primers amplifying a sequence of glyceraldehyde-3-phosphate dehydrogenase (GAPDH). Data are expressed as log2 [relative expression] according to the following formula: relative expression = 45 – ΔCt, where 45 is the maximum number of cycles, and ΔCt is the difference in number of cycles of the gene of interest with the housekeeping gene. We attributed a relative expression of 45 to samples with an undetectable expression (threshold cycle ≥ 45); next, we estimated the relative expression as described above [16].
Data and Statistical Analysis
All calculations and statistical analyses and drawing of scatterplots were performed using the JMP Pro 14.0.0 software program (SAS Institute, Inc., Cary, NC, USA). All numerical data are expressed as the median (range). The chi-square test was used to compare categorical variables, and the Mann-Whitney U test was used to compare continuous variables between two groups. The target gene expression was compared between groups using the nonparametric Wilcoxon rank sum test. P value < 0.05 was considered statistically significant.
Pairwise Pearson’s correlation was used to generate the correlation matrix of the cytokines. To account for multiple testing, the P values were adjusted by Bonferroni correction. An adjusted P value < 0.01 was considered statistically significant.
Cluster Analyses
A variable cluster analysis, in which the variables are clustered so that ones with high correlation belong to the same cluster, was performed on the cytokine expression profiles. To identify groups of cytokines that correlate, as a complement to the cluster analysis, a factor analysis using a principal component analysis (PCA) analysis was performed. Using the correlation coefficient, high scores (factor loading) are given to similar variables. The coefficients generated with this procedure, linking the cytokines to the factors, are the correlation coefficients (Pearson’s correlation under Varimax rotation) between the cytokines and the factors [17].
K-Means Cluster Analyses
K-means clustering, which we applied to the data after the PCA, divides the n observations in a data set into k clusters. Each observation is assigned to the cluster whose mean is the nearest to that observation. The standard K-means clustering algorithm is based on two alternating procedures. The first involves the assignment of observations to clusters, and the second involves the calculation of new cluster means based on the assignments. The process stops when no reassignment of an observation to a cluster would minimize the within-cluster sum of distances between samples and the mean of each cluster. The Euclidean measure was used here to calculate the distance between observations [17].
RESULTS
Clinical Characteristics of the UC Patients
Table 2 shows the clinical characteristics of the patients in this study. The median (range) ages at enrollment and at onset were 37 (19–80) years old and 32 (16–80), respectively. Eighteen males and 17 females were enrolled. The Endoscopic Rachmilewitz score at the diagnosis was 8.0 (2–12). Disease activity at the diagnosis was mild in 14, moderate in 15, and severe in 6. The extent of UC was ulcerative proctitis in 7, left-sided UC in 10, and extensive UC in 18. The clinical course was first attack in 7, relapse-remitting in 15, and chronic continuous in 13. After registration, patients received medical treatments as shown in Table 2. At 8 weeks, clinical remission had been achieved in 45.7%.
Results of a Correlation Analysis of the Cytokines and Transcription Factors in UC Patients
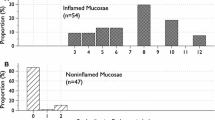
The levels of targeted cytokines and transcription factors were examined in the inflamed mucosa of the rectum. The log2 relative expression of each cytokine is shown in Fig. 1. IL-4 and IL-13, which tended to have a bimodal distribution, showed a relatively low expression, while other factors showed a high expression, including IL-23p19 and TGF-β, which showed a particularly high expression. This high expression of many cytokines and transcription factors suggests that the biopsy samples were obtained from active inflammation mucosa and are therefore worth examining.
A correlation analysis among all targeted cytokines and transcription factors was performed by calculating the Pearson’s correlation coefficient (Fig. 2a, b). The correlation coefficients among Th1-related cytokines, including IFN-γ, TNF-α, IL-6, and IL-12, ranged from 0.49 to 0.71; those among Th2-related cytokines, including IL-4, IL-13, and IL-33, ranged from 0.32 to 0.60; and that of the Treg-related cytokines IL-10 and TGF-β was r = 0.57. The correlation coefficients were reasonable values, but the correlation coefficients among the Th17-related cytokines (except for IL-23p19) ranged from 0.07 to 0.79. The wide range of the correlation coefficients for Th17-related cytokines was attributed to IL-23p19. Interestingly, IL-23p19 was found to be poorly correlated with other Th17-related cytokines, including IL-17A (r = − 0.06), IL-17F (r = 0.06), and IL-22 (r = 0.07).
The Pearson’s correlation coefficient was computed for all pairwise cytokines. a The correlation coefficients between each pair of cytokines and transcription factors. The dark gray areas indicate Th1, Th2, Th17, and Treg cell-related cytokines. The light gray areas indicate the cytokines which belonged to each of the Th cell transcription factors. Single asterisk indicates a significant correlation (P < 0.01) after Bonferroni correction. b Heat maps showing the correlation coefficients of a as color code. Color codes in each panel indicate red for a positive correlation and blue for a negative correlation. The area surrounded by black line indicates Th1, Th2, Th17, and Treg cell-related cytokines. c and d Correlation between the relative expression of mucosal IL23 and T-bet or GATA3 in UC patients. Values were normalized by the corresponding mRNA expression of the housekeeping gene GAPDH. The correlations were analyzed using Spearman’s correlation test.
After reviewing the results of the correlation analysis among all cytokines and transcription factors, the strongest correlation was observed between IL-23p19 and T-bet (r = 0.87) (Fig. 2a, c), and the second strongest was between IL-23p19 and GATA3 (r = 0.84) (Fig. 2a, d). FOXP3 was significantly correlated with several Th1-, Th2-, and Th17-related cytokines. There was also a strong correlation between each transcription factor and the transcription factor related-cytokines (Th1, r = 0.49–0.61; Th2, r = 0.31–0.50; Th17, r = − 0.48–0.05; Tregs, r = 0.38–076) (Fig. 2a), but importantly, those values were lower than those between IL-23p19 and T-bet (r = 0.87).
Results of a Cluster Analysis of Targeted Cytokines and Transcription Factors on Effector T Cells
Next, we performed a correlation hierarchical cluster analysis to identify groups of cytokines and transcriptome factors using the average linkage method. The Treg-related cytokines and transcriptional factors were excluded from this analysis, as they were reasonably and highly correlated with all effector T cells. This analysis revealed that there were two distinct groups in UC patients (Fig. 3a, b): consistent with the previous correlation analysis, the Th1-related factors (T-bet, IL-12, and IFN-γ) and Th2-related factors (GATA-3, IL-4, IL-13, and IL-33) formed one cluster with IL-23 p19, while the Th17-related factors (IL-17A, IL-17F, IL-22, and RORC) formed the other distinct cluster.
a A variable cluster analysis was performed on the cytokine expression profiles. Heat maps showing the correlation coefficients as color code. Color codes in each panel indicate red for a positive correlation and blue for a negative correlation. b The Varimax-rotated factors and their loadings are shown. The loading scores represent how well each cytokine correlates to the corresponding factors.
Results of an Analysis of Groups Characterized by IL-23, T-bet, and GATA3
Since the correlation analysis together with the cluster analysis showed that IL-23p19 is not correlated with Th17-related factors but is correlated with Th1- and Th17-related factors, especially T-bet and GATA3, a k-means cluster analysis was conducted using IL-23p19, T-bet, and GATA3. As a result, the UC patients were classified into two groups: the high-IL-23-expression group (n = 20) and the low-IL-23-expression group (n = 15, Fig. 4a, b).
a K-means clustering, which we applied to IL-23, T-bet, and GATA3, divided the 35 patients in the data set into 2 clusters. b The relative mRNA expression of IL-23 in mucosal specimens from group 1 and 2 patients was quantified by real-time reverse transcription-PCR, and the values were normalized to GAPDH. c and d The relative mRNA expression of IL-17A and IL-13 in mucosal specimens from patients in the high- and low-IL-23-expression groups was quantified by real-time reverse transcription-PCR, and the values were normalized to GAPDH.
Regarding the cytokines secreted by these groups, there were significant differences in the secretion of TNF-α (p = 0.03), IL-12 (p = 0.007), IL-4 (p = 0.004), IL-33 (p = 0.007), and IL-21 (p = 0.001) between the two groups. However, surprisingly, there were no significant differences in other cytokines, including the IL-17A and IL-13 expressions, between the two groups (Fig. 4c, d).
Next, we examined whether or not there were any marked differences in clinical characteristics between two groups (Table 3). The proportion of a chronic continuous clinical course was significantly higher and the clinical remission rate significantly lower in the high-IL-23p19-expression group than in the low-IL-23p19-expression group. There were no significant differences in other clinical characteristics between the two groups.
DISCUSSION
UC is considered to be a Th2- and Th17-related disease where IL-23 plays a crucial role in the induction and maintenance of Th17 cells. In the present study, we showed that IL-23 and TGF-β were highly expressed in the inflamed mucosa of UC patients compared with other cytokines and revealed for the first time that IL-23 is poorly associated with Th17 cell-related cytokines and the transcription factor RORC but is rather strongly associated with Th1- and Th2-related transcriptional factors (T-bet and GATA3) in UC patients. Furthermore, the proportion of chronic continuous type was higher and the remission rate was lower in the high-IL-23-expression group than in the low-IL-23-expression group. IL-23 is strongly associated with T-bet and GATA3 and may be a key cytokine of UC.
IL-23 is a heterodimeric cytokine composed of a unique p19 subunit and a common p40 subunit and is primarily secreted by activated dendritic cells (DCs), monocytes, and macrophages. Importantly, the p40 subunit is shared with IL-12, which has another specific subunit in p35 [18]. Basic research has shown that IL-23 is involved in the induction and maintenance of Th17 cells, which express the transcription factor RORC and secrete IL-17A, IL-17F, IL-21, and IL-22. In contrast, T-bet and GATA3 are transcription factors of Th1 and Th2 cells. Given the main findings of the present study, the IL-23-RORC axis may be changed to the IL-23-T-bet/GATA3 axis under UC conditions. In this context, it is not appropriate to consider UC as simply a Th2- and Th17-related disease; instead, we must consider that a Th1-related immune response is also present in UC patients.
Although the mechanisms underlying the transition to the IL-23-T-bet/GATA3 axis in UC are unclear at present, one possible mechanism may involve “plasticity.” It was recently reported that Th17 cells and Tregs can change their phenotype and repolarize towards different fates, which is referred as plasticity [19,20,21,22]. Indeed, several studies have revealed that IL-23 can induce T-bet in Th17 cells. Those cells, which are able to secret both IL-17A and IFN-γ and are referred to as Th17/Th1 cells, were furthermore transformed into IFN-γ-secreting Th1 cells by the downregulation of RORC [23]. Th17/Th1 cells are considered to be more closely associated with the pathogenesis of IBD than Th17 cells [24]. This plasticity might explain why IL-23 was strongly correlated with T-bet in the UC patients in the present study.
In contrast, with regard to the relationship between IL-23 and GATA3, although whether or not Th17 cells have plasticity to Th2 cells remains unclear, it was recently suggested that IL-23-IL-23R signaling might promote GATA3 expression and enhance the Th2 cytokine expression in allergic airway inflammation [25, 26]. Furthermore, it was also reported that IL-23 was able to modulate pathogenic Th2 immune responses independently of its original role in promoting Th17 cell development [26]. These findings suggest that IL-23 is associated with GATA3 independently of Th17 cells under certain disease conditions, such as UC and bronchial asthma.
It is often difficult to analyze the cytokine profile, since the involvement of not only the plasticity of the immune cells and other cytokine-secreting cell groups, like ILCs, but also the dual effects of secreted cytokines (termed “duality”) must be taken into account. Both IL-13 and IL-17A have demonstrated duality, showing both protective and pathogenetic aspects [27,28,29]. These molecules are reportedly important for maintaining homeostasis of the barrier function in the normal gut mucosa. In contrast, both Th2 cells and Th17 cells are involved in the pathogenesis of UC. As the condition of the inflamed mucosa in UC patients varies depending on both the severity and the duration from onset, it is difficult to interpret how IL-13 and IL-17A, which are secreted by not only Th cells but also ILCs, macrophages, granulocytes, and fibroblasts, contribute to the pathogenesis of UC.
Given such factors as the plasticity of immune cells and the duality of secreted cytokines, the result of our study which show Th1-, Th2-, and Treg-related cytokines to be comparatively closely related to each transcription factor, but not very strongly, might be acceptable. Furthermore, the result that both IL-17A and IL-17F were rarely related with RORC might thus also deem to be reasonable. Despite difficulty analyzing transcription factors and cytokines, the strong correlation of IL-23 with T-bet and GATA3 may be an important finding. At the risk of overstatement, T-bet and GATA3 might be located downstream of IL-23 in the active state of UC.
UC patients display substantial heterogeneity, showing a wide range of clinical characteristics, including the age of onset, clinical course, and response rate of biologic treatment. These clinical characteristics may be classified into some different groups by the immune reaction patterns evaluated based on the expression of cytokines, including IL-13 and IL-17A [30]. However, it remains to be determined which cytokine affects the clinical characteristics. Indeed, establishing such groups in the present study did not necessarily reflect the clinical characteristics (data not shown). This study showed that the groups based on the IL-23-T-bet/GATA3 axis might help to determine some of the typical clinical characteristics. The proportion of chronic continuous type was higher and the clinical remission rate lower in the high-IL-23-expression group than in the low-IL-23-expression group. Although further research is required, anti-IL23 antibody may be a good option for treating chronic continuous type UC, for which remission is difficult to achieve at present.
Several limitations associated with the present study warrant mention. First, this was a retrospective study with a relatively small number of patients enrolled. Second, IL-12/23 p40 was not measured in this study. However, since IL-12/23 p40 is common subunit of IL-12 and IL-23, IL-23p19 is considered sufficient to evaluate IL-23. Third, we did not evaluate isolated lamina propria mononuclear cells by FACS analysis. As ILC and natural killer T cells are also involved in IL-23, T-bet, and GATA3, these cells affect the mechanism of IL-23. However, results analyzed by FACS cannot reveal the correlation between IL23, T-bet, and GATA3. Therefore, the analysis of cytokine profile is considered to be more useful for identifying the correlation between IL23, T-bet, and GATA3 than FACS analysis. Fourth, we did not evaluate the association of IL-23-T-be/GATA3 in a mouse or rat model. However, as there is not a mouse and rat model which exactly reflects the pathogenesis of UC, we consider that the analysis of human samples, but not basic colitis model, contributed to the present results of IL23-T-bet/GATA3 axis. Fifth, UC patients receiving UST, an anti-IL-12/23 p40 antibody, were not enrolled in this study. How UST affects the treatment efficacy in UC patients in terms of the IL-23-T-bet/GAT3 axis would be interesting to explore. The findings of this study can be used to conduct prospective studies in the future with a larger sample size of UC patients receiving UST.
In conclusion, IL-23 may be a very important cytokine for evaluating the UC disease condition, as the expression of IL-23 is associated with certain clinical characteristics of UC patients. A unique association between IL-23 and T-bet/GATA3 might play a key role in the pathogenesis of UC. The IL-23-T-bet/GATA3 axis may be a viable target for the treatment of UC.
Data Availability
The authors confirm that the data supporting the findings of this study are available within the article and material.
References
Morrison, G., B. Headon, and P. Gibson. 2009. Update in inflammatory bowel disease. Australian Family Physician. 38: 956–961.
Geremia, A., P. Biancheri, P. Allan, G.R. Corazza, and A. di Sabatino. 2014. Innate and adaptive immunity in inflammatory bowel disease. Autoimmunity Reviews. 13: 3–10.
Xavier, R.J., and D.K. Podolsky. 2007. Unravelling the pathogenesis of inflammatory bowel disease. Nature. 448: 427–434.
Rosen, M.J., R. Karns, J.E. Vallance, R. Bezold, A. Waddell, M.H. Collins, Y. Haberman, P. Minar, R.N. Baldassano, J.S. Hyams, S.S. Baker, R. Kellermayer, J.D. Noe, A.M. Griffiths, J.R. Rosh, W.V. Crandall, M.B. Heyman, D.R. Mack, M.D. Kappelman, J. Markowitz, D.E. Moulton, N.S. Leleiko, T.D. Walters, S. Kugathasan, K.T. Wilson, S.P. Hogan, and L.A. Denson. 2017. Mucosal expression of type 2 and type 17 immune response genes distinguishes ulcerative colitis from colon-only Crohn’s disease in treatment-naive pediatric patients. Gastroenterology. 152: 1345–1357.
Hirahara, K., and T. Nakayama. 2016. CD4+ T-cell subsets in inflammatory diseases: beyond the Th1/Th2 paradigm. International Immunology 28: 163–171.
Imam, T., S. Park, M.H. Kaplan, and M.R. Olson. 2018. Effector T helper cell subsets in inflammatory bowel diseases. Frontiers in Immunology. 9: 1212.
Iboshi, Y., K. Nakamura, E. Ihara, T. Iwasa, H. Akiho, N. Harada, M. Nakamuta, and R. Takayanagi. 2014. Multigene analysis unveils distinctive expression pro files of helper T-cell – related genes in the intestinal mucosa that discriminate between ulcerative colitis and Crohn’s disease. Inflammatory Bowel Diseases 20: 967–977.
Feagan, B.G., W.J. Sandborn, C. Gasink, D. Jacobstein, Y. Lang, J.R. Friedman, M.A. Blank, J. Johanns, L.L. Gao, Y. Miao, O.J. Adedokun, B.E. Sands, S.B. Hanauer, S. Vermeire, S. Targan, S. Ghosh, W.J. de Villiers, J.F. Colombel, Z. Tulassay, U. Seidler, B.A. Salzberg, P. Desreumaux, S.D. Lee, Loftus EV Jr, L.A. Dieleman, S. Katz, P. Rutgeerts, and UNITI–IM-UNITI Study Group. 2016. Ustekinumab as induction and maintenance therapy for Crohn’s disease. New England Journal of Medicine. 375: 1946–1960.
Sands, B.E., W.J. Sandborn, R. Panaccione, C.D. O'Brien, H. Zhang, J. Johanns, O.J. Adedokun, K. Li, L. Peyrin-Biroulet, G. van Assche, S. Danese, S. Targan, M.T. Abreu, T. Hisamatsu, P. Szapary, C. Marano, and UNIFI Study Group. 2019. Ustekinumab as induction and maintenance therapy for ulcerative colitis. New England Journal of Medicine. 381: 1201–1214.
Reinisch, W., J. Panés, S. Khurana, G. Toth, F. Hua, G.M. Comer, M. Hinz, K. Page, M. O'Toole, T.M.D. Moorehead, H. Zhu, Y.H. Sun, and F. Cataldi. 2015. Anrukinzumab, an anti-interleukin 13 monoclonal antibody, in active UC: efficacy and safety from a phase IIa randomised multicentre study. Gut. 64: 894–900.
Danese, S., J. Rudziński, W. Brandt, J.L. Dupas, L. Peyrin-Biroulet, Y. Bouhnik, D. Kleczkowski, P. Uebel, M. Lukas, M. Knutsson, F. Erlandsson, M.B. Hansen, and S. Keshav. 2015. Tralokinumab for moderate-to-severe UC: A randomised, double-blind, placebo-controlled, phase IIa study. Gut. 64: 243–249.
Ehrlich, D., N. Jamaluddin, J. Pisegna, and D. Padua. 2018. A challenging case of severe ulcerative colitis following the initiation of secukinumab for ankylosing spondylitis. Case Reports in Gastrointestinal Medicine. 2018: 1–4.
Orrell, K.A., M. Murphrey, R.C. Kelm, H.H. Lee, D.R. Pease, A.E. Laumann, D.P. West, and B. Nardone. 2018. Inflammatory bowel disease events after exposure to interleukin 17 inhibitors secukinumab and ixekizumab: postmarketing analysis from the RADAR (“Research on Adverse Drug events and Reports”) program. Journal of the American Academy of Dermatology. 79: 777–778.
Lozano, M.J.F., R.S. Giménez, and M.C. Fernández. 2018. Emergence of inflammatory bowel disease during treatment with secukinumab. Journal of Crohn’s and Colitis. 12: 1131–1133.
Ogino, H., K. Nakamura, E. Ihara, H. Akiho, and R. Takayanagi. 2011. CD4+CD25+ regulatory T cells suppress Th17-responses in an experimental colitis model. Digestive Diseases and Sciences. 56: 376–386.
Fukaura, K., Y. Iboshi, H. Ogino, E. Ihara, K. Nakamura, Y. Nishihara, K. Nishioka, T. Chinen, T. Iwasa, A. Aso, A. Goto, K. Haraguchi, H. Akiho, N. Harada, and Y. Ogawa. 2019. Mucosal profiles of immune molecules related to T helper and regulatory T cells predict future relapse in patients with quiescent ulcerative colitis. Inflammatory Bowel Diseases. 25: 1019–1027.
Wallner, F.K., M. Hultqvist Hopkins, T. Lindvall, P. Olofsson, and A. Tilevik. 2017. Cytokine correlation analysis based on drug perturbation. Cytokine 90: 73–79.
Allocca, M., F. Furfaro, G. Fiorino, et al. 2018. Can IL-23 be a good target for ulcerative colitis? Best Practice and Research: Clinical Gastroenterology. 32–33: 95–102.
Ueno, A., L. Jeffery, T. Kobayashi, T. Hibi, S. Ghosh, and H. Jijon. 2018. Th17 plasticity and its relevance to inflammatory bowel disease. Journal of Autoimmunity. 87: 38–49.
Li, J., A. Ueno, M. Iacucci, M. Fort Gasia, H.B. Jijon, R. Panaccione, G.G. Kaplan, P.L. Beck, J. Luider, H.W. Barkema, J. Qian, X. Gui, and S. Ghosh. 2017. Crossover subsets of CD4+T lymphocytes in the intestinal lamina propria of patients with Crohn’s disease and ulcerative colitis. Digestive Diseases and Sciences. 62: 2357–2368.
Harrison, O.J., J.L. Linehan, H.-Y. Shih, et al. 2019. Commensal-specific T cell plasticity promotes rapid tissue adaptation to injury. Science. 363: 1–27.
Hirota, K., J.H. Duarte, M. Veldhoen, E. Hornsby, Y. Li, D.J. Cua, H. Ahlfors, C. Wilhelm, M. Tolaini, U. Menzel, A. Garefalaki, A.J. Potocnik, and B. Stockinger. 2011. Fate mapping of IL-17-producing T cells in inflammatory responses. Nature Immunology 12: 255–263.
Globig, A.M., N. Hennecke, B. Martin, M. Seidl, G. Ruf, P. Hasselblatt, R. Thimme, and B. Bengsch. 2014. Comprehensive intestinal T helper cell profiling reveals specific accumulation of IFN-γ+IL-17+coproducing CD4+ T cells in active inflammatory bowel disease. Inflammatory Bowel Diseases. 20: 2321–2329.
Kobayashi, T., S. Okamoto, T. Hisamatsu, N. Kamada, H. Chinen, R. Saito, M.T. Kitazume, A. Nakazawa, A. Sugita, K. Koganei, K. Isobe, and T. Hibi. 2008. IL23 differentially regulates the Th1/Th17 balance in ulcerative colitis and Crohn’s disease. Gut. 57: 1682–1689.
Wakashin, H., K. Hirose, Y. Maezawa, S.I. Kagami, A. Suto, N. Watanabe, Y. Saito, M. Hatano, T. Tokuhisa, Y. Iwakura, P. Puccetti, I. Iwamoto, and H. Nakajima. 2008. IL-23 and Th17 cells enhance Th2-cell-mediated eosinophilic airway inflammation in mice. American Journal of Respiratory and Critical Care Medicine. 178: 1023–1032.
Peng, Juan, Xuexian O. Yang, and Seon Hee Chang. 2010. Jiong Yang and CD. IL-23 signaling enhances Th2 polarization and regulates allergic airway inflammation. Cell Research 20: 62–71.
Gieseck, R.L., M.S. Wilson, and T.A. Wynn. 2018. Type 2 immunity in tissue repair and fibrosis. Nature Reviews Immunology. 18: 62–76.
Oeser, K., C. Schwartz, and D. Voehringer. 2015. Conditional IL-4/IL-13-deficient mice reveal a critical role of innate immune cells for protective immunity against gastrointestinal helminths. Mucosal Immunology. 8: 672–682.
O'Connor, W., Jr., M. Kamanaka, C.J. Booth, et al. 2009. A protective function for interleukin 17A in T cell–mediated intestinal inflammation. Nature Immunology 10: 603–609.
Butera, A., M. di Paola, F. Vitali, D. de Nitto, F. Covotta, F. Borrini, R. Pica, C. de Filippo, D. Cavalieri, A. Giuliani, A. Pronio, and M. Boirivant. 2020. IL-13 mRNA tissue content identifies two subsets of adult ulcerative colitis patients with different clinical and mucosa-associated microbiota profiles. Journal of Crohn’s and Colitis. 14: 369–380.
Acknowledgments
We sincerely thank the staff of the endoscopy unit at Kyushu Medical Center, Kitakyushu Municipal Medical Center, and Harasanshin Hospital for their valuable assistance in conducting this study. We appreciate the technical assistance received from The Research Support Center, Research Center for Human Disease Modeling, and Kyushu University Graduate School of Medical Sciences.
Funding
This study was supported in part by the Japan Society for the Promotion of Science KAKENHI (20K08389).
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
Eikichi Ihara belongs to an endowed course supported by companies including Ono Pharmaceutical Co., Ltd., Miyarisan Pharmaceutical Co. Ltd., Sanwa Kagaku Kenkyusho Co., Ltd., Otsuka Pharmaceutical Factory, Inc., Fujifilm Medical Co., Ltd., Terumo Corporation, Fancl Corporation, and Ohga Pharmacy. All other authors declare that they have no conflict of interest.
Ethics Approval, Consent to Participate, and Consent for Publication
The aim of the present study was explained to each patient during the interview before endoscopy. Patients were informed of the potential risk of bleeding from the biopsy sites although the risk was considered to be low. Only those who gave their written informed consent were included. This study was reviewed and approved by the institutional review boards of all of the study sites and was conducted in accordance with the ethical principles of the Declaration of Helsinki. The study is registered with the Kyushu university hospital under the identification number: 30-472.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Ogino, H., Fukaura, K., Iboshi, Y. et al. Role of the IL-23-T-bet/GATA3 Axis for the Pathogenesis of Ulcerative Colitis. Inflammation 44, 592–603 (2021). https://doi.org/10.1007/s10753-020-01358-y
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10753-020-01358-y