Abstract
Accountable care organizations (ACO) in the United States show promise in controlling health care costs while preserving patients’ choice of providers. Understanding the effects of patient choice is critical in novel payment and delivery models like ACO that depend on continuity of care and accountability. The financial, utilization, and behavioral implications associated with a patient’s decision to forego local health care providers for more distant ones to access higher quality care remain unknown. To study this question, we used an agent-based simulation model of a health care market composed of providers able to form ACO serving patients and embedded it in a conditional logit decision model to examine patients capable of choosing their care providers. This simulation focuses on Medicare beneficiaries and their congestive heart failure (CHF) outcomes. We place the patient agents in an ACO delivery system model in which provider agents decide if they remain in an ACO and perform a quality improving CHF disease management intervention. Illustrative results show that allowing patients to choose their providers reduces the yearly payment per CHF patient by $320, reduces mortality rates by 0.12 percentage points and hospitalization rates by 0.44 percentage points, and marginally increases provider participation in ACO. This study demonstrates a model capable of quantifying the effects of patient choice in a theoretical ACO system and provides a potential tool for policymakers to understand implications of patient choice and assess potential policy controls.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
1 Introduction
Empowering patients and preserving their freedom to choose providers remains a fundamental aspect of health care delivery in the United States. However, accountability for the patient’s overall health dissipates in the complex transactions and provider disintegration of the traditional U.S. health care system [1]. Therefore, health care costs are on the rise in part due to the fragmentation of traditional health delivery outlets and misaligned incentives in the prominent payment model [2]. Novel health care delivery and payment models attempt to reconcile the freedom of choice for patients and provider accountability. The Affordable Care Act promotes accountable care organizations (ACO), which feature a comprehensive payment model and organizational structure for a more aligned care delivery system. An ACO is composed of health care providers and specialists who deliver coordinated, continuous care and are held accountable for patient outcomes and costs. ACO have shown promise in reducing health care costs and improving health outcomes in demonstration projects [3]. In 2011, the Centers for Medicare and Medicaid Services (CMS) published rules for its Medicare Shared Savings ACO Program [4] that specify how ACO savings are to be shared between providers and the CMS. The growth of public and private ACO and novel approaches to accountability require additional research to study the financial, operational, and behavioral impact of such models.
The appeal to providers of forming ACO has been studied and modeled in previous research. Liu and Wu [5] developed an agent-based model in which providers decide whether to participate in an ACO. The context is a dynamic market with active provider decision-making serving 5000 Medicare patients with congestive heart failure (CHF). Providers with different quality and profit orientations engage in an evolving environment and react based on an intention-driven decision module. The model presented valuable insights regarding the relationship between shared saving rates and provider behavior, as well as population outcomes [5]. However, the model did not allow patients to be active decision-makers; patients in this model did not have the freedom to pick providers or decide where to receive inpatient and outpatient care.
As with other markets, health care delivery markets are more likely to perform better when customers (i.e., patients) are empowered to choose their providers [6]. In the context of accountable health care delivery, some tension exists between preserving patient choice and continuity of care. On one hand, informed patients who consistently choose better quality providers are likely to motivate providers to invest in quality investments. On the other hand, ACO enable patient choice of providers, which may make it difficult to deliver continuous care, measure quality, and estimate savings when patients utilize non-ACO providers. The implications of patient choice in the context of ACO remain unclear. In wake of recent health care initiatives to promote provider accountability, understanding the power and effects of patient choice in an ACO health care delivery market is critical for policymakers to identify success factors and optimize implementations.
In rural areas, patients often go to urban hospitals for care rather than use the local hospital, a practice referred to as patient bypass. In part due to patient bypass, about three fourths of California rural hospitals are losing money and many have discontinued services, including emergency departments and inpatient services [7]. The resulting failure to provide access to care in a timely manner is likely to cause higher institutional costs [8]. Studies have analyzed patterns in numerous countries (including the United States, Netherlands, and Chad) and on various segments (e.g., older adults) and specialties [9, 10]. Although research has investigated patient choice and what hospitals can do to retain patients locally [11], we found no literature quantifying the financial and utilization effects of patient choice.
The dynamics in the health care market make it difficult to assess effects mathematically or empirically. Such investigations call for the use of modern engineering tools, particularly agent-based simulation, to explore and model complex patient–provider interactions and pertinent system outcomes. The goal of our research was to construct and run an agent-based simulation model to understand the effects of patient bypass. By designing the appropriate simulation scenarios, we may gain insights that will allow researchers and policymakers to understand and quantify the impacts of patient bypass and to draw closer to quantifying the degree to which patient choice drives quality in ACO.
2 Agent-based patient choice simulation
The advantages of agent-based modeling make it a well-suited tool to develop and understand the heterogeneity and complexity of patient choice behavior and its implications on financial and health outcomes. Therefore, we expanded and modified Liu and Wu’s [5] ACO agent-based simulation model (Fig. 1) to build and test a patient choice decision-making module and quantify the effects of bypass.
Modified agent-based simulation model. The structure shows the different layers of the simulation system and the different agents—payer, provider, and patient—and their key components. This research quantifies the impact of patient choice by adding the highlighted patient choice decision module. (Note: PCP = primary care physician clinic)
2.1 The patient agent
Each patient agent represents a Medicare beneficiary who is at least 65 years old. Every patient is generated with seven variables: three health condition variables (diabetes, hypertension, and CHF) and four demographic variables (age, race, gender, and income). The health condition and the gender variables are binary variables. For example, for the diabetes variable, 1 indicates a patient was diagnosed with diabetes, 0 indicates otherwise. Four race categories and three income categories were used. Refer to Liu and Wu [5] for an additional description of the patient attributes. According to the literature, demographic variables are predictors of patient preferences of providers and a patient’s readiness to travel farther to receive care [8]. In addition, the same seven patient-specific variables predict a patient’s likelihood of developing CHF and progressing through the condition and treatment stages [5]. The distributions of the seven patient attributes are based on the National Health and Nutrition Examination Survey from 1999 to 2010 for individuals aged 65 years old or older; a joint distribution was employed to relate the seven variables according to survey data to generate patients from a population with the same characteristics [5].
2.1.1 Patient alternatives
We randomly assigned individual patients to a preferred (local) primary care physician clinic (PCP) and hospital. Each patient was also assigned to an alternative (nonlocal) clinic and hospital. For modeling purposes, hospitals and clinics were assumed to provide identical services and have unlimited capacity. The model counted patient bypass occurrence when a patient sought care at the alternative providers [12].
We used a distance parameter to control the fixed distance between providers in each pair, measured in minutes between providers. A higher distance parameter indicates less dense, more dispersed delivery outlets that decrease the likelihood that a patient will bypass the closest providers. A lower distance parameter indicates more compact distribution of delivery outlets; hypothetically, patients in this scenario are more likely to bypass local providers. For modeling purposes, the distance between any pair of preferred and alternative providers was assumed to be the same (60 min) to mimic a typical rural–urban setting. In other words, should patients choose to receive care from the alternative provider, they must travel 60 min. Essentially, this model controlled the effect of distance, but future versions can be adapted for a thorough spatial representation of existing health care setting upon establishing model validity.
2.1.2 Patient decision-making module
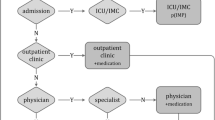
For modeling purposes, patients made the bypassing decision at their first contact with their assigned providers in the model based on the factors depicted in Fig. 2. Predictors of patient bypass include provider attributes, patient attributes [8], and distance [12]. The provider attributes that influence a patient’s bypassing decisions include limited technology, resources, services, and quality of care [8]. Four other studies have derived model variables from Medicare patient data, including discharge data, phone survey data, and Medicare hospital service area data [7, 12–14]. All four models predicted patient bypass behavior using conditional logit models, the accepted standard modeling framework for hospital choice studies [7]. The four models varied in the number of provider attributes, patient attributes, and comparators. For our ACO model, we selected a subset of variables from the most relevant study [12]. The selected variables that predict the probability of bypass are categorized in Fig. 2.
Variables that predict the probability of patient bypass in the agent-based simulation model. The figure groups the input variables into the corresponding categories: patient, provider, and environment. Table 1 presents more details on the categories of each variable and the odds of bypass
Patient attributes are considered case-specific regressors; they vary across patients and not across alternatives. Provider attributes are alternative-specific regressors; they vary across alternatives and not across patients. Some variables in the relevant models may not be applicable in our model. For example, severity of a condition is a significant predictor in some models, because severely ill patients would require a hospital with more resources and services [15].
The estimates of coefficients of regression model used are from the conditional logit model by Tai et al. [12]. Their study examined how patient and hospital attributes influence choices among rural Medicare beneficiaries. The researchers used a conditional logit model and provided odds ratios, intercepts, and compelling fit statistics in their study report. Our study adapted the applicable odds ratios to derive the model coefficients for our patient variables. We used a subset of the patient variables and a subset of the categories for some variables. Refer to the Remarks column in Table 1 for more details on the patient variables used. In our model, we did not account for degree of severity of CHF and assumed hospitals provided identical services but varied in the probability of service outcomes (based on their disease management program). Therefore, the regressors relating to service types were averaged and added to the intercept term. The odds ratios and the coefficients for every variable are listed in Table 1.
Effects of the quality of services provided, or perceptions of quality, on patient choice were not reported in the aforementioned study. This might be partly explained by the fact that perception of provider quality is often difficult to obtain, assess, and aggregate. Because of our interest in studying the effects of provider quality on patient choice, we introduced several contrived odds ratios to account for the effect of provider quality on patient choice. We assigned hypothetical odds ratio of patient bypass for mortality rate difference, hospitalization rate difference, and disease management, and we considered the assumed values to be simulation parameters that can be examined in the sensitivity analysis and updated if estimates become available. Naturally, we chose coefficients such that patients were more likely to bypass if the alternative provider provided disease management services and had lower mortality rates and hospitalization rates.
We assumed the odds ratio of patient bypass for a 1 percentage point increase in mortality rate to be 0.90. This means that patients favored lower mortality rates and were less likely (10 % decrease in odds) to decide to go to the alternative provider when the alternative provider had a mortality rate that is 1 % higher than the preferred provider. Similarly, for a 1 percentage point increase in hospitalization rate, we assigned an odds ratio of patient bypass of 0.95. We also assumed that the odds ratio for a patient seeking care at the alternative provider was equal to 2 when the preferred provider did not offer a disease management program and the alternative did. This means that a patient favored disease management services; the odds that a patient would bypass a local provider with no disease management intervention and choose an ACO alternative provider offering disease management programs were double the odds compared to a case in which both providers offered similar services.
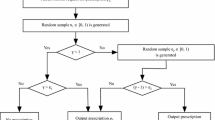
For modeling purposes, we assumed that patients were fully aware of yearly provider performance: mortality rates, hospitalization rates, and disease management programs. Although this research assumed perfect information and action around perfect information, it is possible to build information and action discrepancies in future expansions of this model. For every patient, the vector of patient and provider variables was multiplied by the vector of coefficients, yielding a value (y). This value was then placed in the logit function, such that:
The resulting value was then used as the probability of bypass for the corresponding patient at the time of decision making.
2.2 The provider agents
Providers in the simulation model delivered CHF care to patients and chose to be a member in the ACO network. Members of the ACO network shared cost savings with Medicare (50 % shared savings rate) and provided comprehensive disease management programs. Disease management programs involve engaging patients in increasing self-management behaviors, comprehensive discharge planning and support during hospitalizations, scheduling post-discharge follow-up visits to ensure medication reconciliation and treatment plan, and other preventive measures to reduce conditions that lead to a hospitalization. For the provider, this requires additional investments to enhance existing electronic record systems and increase the staff. The costs of implementing a disease management intervention were assumed to be in the form of monthly costs per CHF patient obtained from a meta-analysis on CHF disease management interventions [16]. Liu and Wu obtained the distribution of costs of CHF hospitalization from 2013 CMS estimates [17], whereas estimates of effects were extracted from a meta-analysis of CHF disease management interventions [16].
In this model, a cost target to obtain the net savings was acquired by running an identical model with no ACO network formation and comparing per patient payments [5]. Provider agents were either hospitals or PCPs. The model initiated with three hospitals and 15 PCPs. Each provider placed different weights on quality and profitability. The key aspect of the provider agent is the capability to decide whether to participate in the ACO by implementing disease management programs. Provider agents influenced other provider agents’ perceptions of participation, but each had individual attitudes concerning investments and returns.
The decision-making process was a three-step process that included perception, intention, and implementation. The decisions providers made affected reimbursements and two patient outcomes: mortality and hospitalization rates. The decision-making module has been published and validated as part of the ACO agent-based simulation model [5]. Additional details of the provider decision-making mechanism and other ACO components are beyond the scope of this research but can be found in the Liu and Wu study [5]. To allow for patient bypass, we modified the ACO model developed by Liu and Wu by refitting hospital and clinic provider agents to handle bypass patients as described below.
3 Research methods
The goal of this research was to construct a patient bypass decision model, develop scenarios for understanding and quantifying the effects of patient bypass, and draw insights regarding the power of patient choice to achieve more desirable outcomes. We used AnyLogic version 6.9 to develop the agent-based model. We retrofitted the new patient agent to the ACO agent-based model developed by Liu and Wu (2014) [5]. The patient agent code was developed to accommodate multiple health care providers and enable patient choice, along with the original modules (refer to Fig. 1). The code implemented the logic involved in patients’ choice of providers devised in Fig. 2 using the odds ratios listed in Table 1 and Section 2.1.2. Verifying and validating techniques, as described in Section 3.2, were employed to test the model, and different scenarios were tested and compared using a defined set of system outcomes. This section describes the approach to designing and testing the model.
3.1 Constructing patient agent
We designed the patient agent to be an active agent in the ACO simulation model originally developed by Liu and Wu [5], in which the patient agent was passive and made no choice. First, we studied and analyzed all aspects of the model by referring to original model documentation, variables, and parameters. A patient agent was constructed by defining new agent state charts, functions, and data arrays to handle the additional data. It was necessary to initiate and update existing sets, variables, methods, and data charts to handle bypassing patient data in other agents and modules, too. The aim was to allow for separate processing of bypass-related data. We propagated newly defined objects throughout the different classes of the model to ensure full compatibility and verify that we made appropriate modifications. In reference to Fig. 1, the highlighted module corresponding to the patient bypass decision making was new code relative to the original model. In the same figure, the boxes corresponding to all other modules were expanded to accommodate the enhanced patient capability.
3.2 Verifying and validating the model
Verifying refers to ensuring the model correctly implements its intended conceptual framework. The verifying process includes individually designed steps and occurs throughout and after building the model. Tests are considered successful if we exaggerate parameters in the simulation and the model reacts as expected. For example, setting the patient quality sensitivity to extremely high (or low) values should have predictable effects on the outcomes. This test verifies the fundamental relationship among costs, patient bypass, and provider behavior.
Validating refers to ensuring the model correctly represents the system specified in the objective. We validated the model by checking that financial and population outcomes are close to ACO studies at predetermined model settings. Bypass rates from the model should be comparable to bypass rates from studies performed on Medicare patients (30 % to 45 %) [7, 12, 18, 19]. Additionally, per-patient payments should be consistent with current Medicare CHF patient estimates [20, 21].
3.3 Outcome measures and simulation settings
Understanding system outcomes and agent behaviors requires defining a set of observable outcome measures that are consistent across the various settings of this study. The outcome measures were chosen to test hypotheses defined to meet the objective. The set of analyzed outcomes are categorized and listed in Table 2.
Yearly bypass rates refer to the percentage of CHF patients that choose to receive care at the alternative provider in a given year. Yearly hospitalization rate refers to the percentage of CHF patients that are hospitalized. Yearly hospitalization rates can be reduced by implementing disease management interventions, which are described in Section 2.2. Similarly, yearly mortality rate refers to CHF-related deaths in a given year, which occur with CHF hospitalization. Therefore, lower mortality and lower hospitalization rates indicate higher quality of care and better outcomes. Average yearly Medicare payment refers to the yearly payout Medicare makes to providers divided by the total number of CHF patients. These payments can also be referred to as costs from Medicare’s standpoint. Lastly, we also measured the rate of ACO participation among clinics and hospitals in the simulation.
We replicated each simulation 600 times and computed a confidence interval on the mean for each outcome variable. We chose the number of replicates to enable meaningful statistical comparisons between outcomes of different simulation parameters using hypothesis testing.
3.4 Scenario testing
We identified six scenarios to generate insights regarding how different aspects of the system influence outcomes and decision making (Table 3). To attain the objectives of this study, we devised a scenario structure that represented a design-of-experiments setup with two variables: ACO setting and patient decision capability. The ACO setting featured three levels: (1) no ACO, (2) ACO choice for providers to participate in or opt out of the ACO, and (3) full ACO in which every provider is a participant in the ACO. Meanwhile, patients were either permitted to visit their alternative providers or assigned a random provider with no choice (two levels). We ran a full design to test the effects of different capabilities by switching agent capabilities to various levels as show in Table 3, with each combination replicated 600 times.
The baseline system is one in which providers were not able to participate in an ACO nor were patients able to pick their preferred provider. In reference to Fig. 1, the baseline scenario corresponded to both modules in the dashed box being inactive. In Scenarios 1 and 4, all providers started as members of the ACO network to develop an impression on participation, then were allowed to opt out or in during subsequent years [5]. Scenario 1 allowed providers in the ACO network to decide whether they wanted to remain in the ACO and implement a disease management intervention or opt out, whereas patients had no choice of providers. Scenario 2 forced all providers to participate in the ACO network, whereas patients had no choice of providers. Last, Scenarios 3 through 5 are repeats of the first three scenarios but patients were given the freedom of choice by having an alternative provider. The effect of patient bypass on a traditional care (non-ACO) network can be observed as the difference between Scenario 3 and the baseline.
We expected that increased ACO participation and patient choice would be associated with improved outcomes: lower mortality and hospitalization rates and lower per patient costs. It is possible that patient choice would affect the efficacy of the ACO, influencing the amounts of savings generated and outcomes achieved. We also hypothesized that in scenarios in which agents are allowed to optimize based on their preferences (Scenario 4), we would observe the tradeoff between quality and profitability.
4 Results
After designing the patient agent and integrating it into the ACO model, we verified the various capabilities using the approaches described in the Methods section. When the patients were able to make bypass decisions, 39.5 % of patients chose to do so in the simulation model. The modeled patient bypass is consistent with estimates for Medicare patients in the literature. Tai et al. [12] reported an average patient bypass frequency of 40.5 % and Escarse et al. [7] reported a 45 % bypass rate. We observed consistent outcomes relating to per patient payments, bypass rates, and hospitalization [20, 21]. For each scenario, we estimated means and standard deviations for outcomes listed in Table 2. The results are graphically represented in Figs. 3 and 4.
Average yearly payment per CHF patient made to providers across scenarios. The graphs, generated in Microsoft Excel, depict the magnitude of the difference between the scenarios. There was a statistically significant decrease in payments received by providers when patients were permitted to bypass across all scenarios (p < .001)
Average mortality rates and hospitalization rates by scenario. The graphs, generated in Microsoft Excel, depict the improvements in quality outcomes attributed to patient bypass and provider ACO participation. Patient bypass produced statistically significant improvements in the ACO choice setting for both quality measures but not in the other two ACO settings
As shown in Fig. 3, allowing patient bypass consistently reduced yearly per patient payments across all ACO settings. On average, there was a $320 reduction in yearly per CHF patient payment (YPPP; p < .0001). The difference in payment induced by patient choice was greatest when providers had ACO choice ($337 YPPP), compared to non-ACO ($321 YPPP) and full ACO ($302 YPPP) scenarios. We attribute these savings in yearly payments per CHF patient to enabling patient choice, regardless of the ACO environment. Specifically, savings were more salient when providers had ACO choice. Furthermore, we observed that the savings generated by ACO were not statistically influenced by patient choice (p = .12). It is also noticeable that provider participation in ACO consistently reduced YPPP. When providers had the choice of participating in an ACO, there was savings of $823 YPPP; a full ACO generated savings of $1248 YPPP (p < .0001). For perspective, a recent cost estimate for Medicare beneficiaries with CHF is around $12,719.04 per patient per year [20].
Figure 4 shows the quality outcomes for each of the tested scenarios. Based on these results, patient choice statistically significantly improved mortality and hospitalization rates in the scenario when providers had the choice of ACO participation. In the ACO choice settings, patient choice reduced mortality rates by 0.13 percentage points (p = .038) and reduced hospitalization rates by 0.44 percentage points (p = .0069). In the other two scenario settings, patient choice did not produce statistically significant changes in either quality outcomes. Increased provider participation in the ACO statistically reduced mortality rates and CHF hospitalization rates; both reductions are visible moving rightward on the charts in Fig. 4 (p < .0001).
Patient bypass affected provider ACO participation decisions. Providers increased their ACO participation at a marginally significant level (p < .10) when patients were allowed to bypass. A 3 % increase in hospital participation in the ACO was attributable to patient choice (p = .071). In addition, patient choice drove an additional 1.4 % of the PCPs to participate in the ACO (p = .065). In other words, empowered and informed patients influenced a small fraction of providers that choose to participate in the ACO and provide a coordinated quality improving intervention.
Different ACO settings slightly altered the rate of patient bypass. Bypass rates were highest when providers had ACO choice and were allowed to differentiate themselves at 40.11 % patient bypass rate. When providers were forced to join an ACO or were forced outside of the ACO, patients were less likely to seek care at the alternative provider with 39.39 % bypassing in no ACO setting and 39.16 % bypassing at full ACO setting (p < .0001).
Running a sensitivity analysis on key parameters identified aspects of the model outcomes that varied when changing some of the model assumptions. The distance parameter was varied among the following values: {45, 60, 75} minutes. The odds ratios of patient bypass for differences in mortality rates {0.90, 0.95, 1} per percentage point change, hospitalization rates {0.90, 0.95, 1} per percentage point change, and disease management programs {1.25, 1.75, 2} were tested with 100 replicates for each combination of previously listed values. It is important to note that setting the odds ratio to 1 indicated that patients were indifferent to or unaware of changes in provider quality.
A design-of-experiments approach was used to assess the sensitivity of the model to key parameters. Distance and patient sensitivity to provider mortality rates, hospitalization rates, and disease management offerings were independent variables that were set at the aforementioned levels, each with two extreme values and a center point. The analysis was run on a comprehensive dataset that included the full model output along with sensitivity analysis output (4200 replicates in total). See Appendix A for more details regarding the effects of varying the aforementioned parameters on key measurable model outcomes. As expected, varying the distance parameter altered the average bypassing rate in the sensitivity analysis. A higher distance parameter led to a lower patient bypass rate (p < .0001). Furthermore, changing patient bypass sensitivity toward provider mortality rates and hospitalization rates had the expected effect on bypass tendencies. More sensitive patients were more likely to bypass (p < .05). The patient agent’s response to changes in the previous parameters verified that the patient bypass module functioned as intended. Varying model parameters did not have a significant impact on key model outcomes. However, the directionality of changes induced by changing the model parameters might generate valuable insights. For example, understanding the effect of patient sensitivity to provider quality on long-term average yearly payments would be useful. Increased patient sensitivity to differences in hospitalization rates increased average YPPP, albeit not at statistically significant levels in the tested range.
5 Discussion
By specifying key outcomes and the appropriate analysis approach, this research showed the technical feasibility of quantifying effects attributed to individual agents and their interactions in a health care market. The study demonstrated that patient bypass decisions have several financial and health implications. The estimated net effect of allowing patient choice reduced yearly payments by $320 for CHF patients consistently across all ACO settings without sacrificing the quality of care. Given that as of 2012, 5.1 million Medicare beneficiaries had CHF [21], savings of $320 per CHF patient constitute a substantial amount. In addition, we observed that patient choice did not have a significant impact on ACO effectiveness to generate savings. From such findings we may imply that even in rural settings, where there are fewer provider alternatives for patients to choose from, ACOs would still be effective. Regarding quality of care, findings suggest that patient choice that is driven by perfect information is associated with improvements in quality of care when providers are allowed to participate in an ACO. Although we recognize that the results of this model at this stage should be interpreted only as a simulation demonstration and not actual quantitative figures in practice, the magnitude and directionality of the effects found in the patient choice modeling provide useful insights.
This study allowed us to observe the tradeoff that providers make between optimizing profits and improving patient outcomes when they can decide whether to participate in an ACO and implement a disease management intervention. In other words, we witnessed the tension involved in profit maximization between cost reduction and creating value to attract patient volume (through investing in quality interventions such as disease management). When providers are allowed to opt out of an ACO network, they optimize their profits; consequently, they opt out of implementing the disease management intervention to reduce costs. This may result in lower quality of care, which might drive patients to the alternative provider. Therefore, patient expectations may act as an incentive to increase provider investments in quality interventions. This investment may then yield costs savings by reducing utilization, which generates ACO savings, and increasing patient volume. As a result, we observed a net savings effect induced by patient choice. It is worth noting that CMS currently allows Medicare patients to choose their health care providers. The findings of this model suggest that if CMS restricts patient choice, it may increase per-patient spending for Medicare CHF patients.
Patient choice marginally increases the number of hospitals and clinics that remain in an ACO. Three percent more hospitals and 1.4 % more clinics participated in the ACO when patients were allowed to pick providers in the simulated scenario. Hence, empowering patients to choose providers appears to make ACO participation more appealing for providers in the simulated health care system. Those differences quantify the pressure patients place on providers to meet their quality demands, when patients have perfect information. Furthermore, under different ACO conditions, patient bypass behaviors differed. When providers had the choice to participate in the ACO, we saw more patient bypass compared to a full ACO or non-ACO setting. Naturally, when providers are allowed to differentiate themselves, patients are expected to be more active in picking the most suitable provider. This research demonstrated the potential of studying emerging provider and patient behaviors to influence policy decisions, as well as the possibility of understanding the effects of imperfect information on provider and patient behavior. Furthermore, the sensitivity analysis demonstrated the influence of key model parameters on model outcomes. All of the outcomes seemed to be fairly stable to changes in the patient choice module and distance between providers. The results of the sensitivity analysis also verified the patient bypass decision module and the sensitivity of patients to provider quality and distance.
The study successfully demonstrates a simulation model capable of quantifying and assessing changes induced by patient choice. The results underscore the importance of patient choice in changing provider behavior and payments. Patient choice compelled more providers to participate in ACO, with slightly more salient improvements in quality outcomes given perfect information and providers’ ability to invest in quality improving interventions. Although patient choice is very important in the health care delivery system, the sensitivity analysis suggested that varying patient sensitivity towards provider attributes did not significantly alter the model outcomes.
6 Limitations and future research
This study established an approach for modeling the effects of patient choice using an agent-based simulation. Upon establishing face validity, the model can be extended to a more accurate reflection of actual health care delivery settings to obtain predictive and quantitative results, rather than exploratory and qualitative insights. Furthermore, the model was constrained by assumptions related to the patient and provider agents. These limitations can be addressed in future work by designing the model with additional capabilities for actively studying patient choice and its pertinent implications.
The model presented in this study assumed equal geographical distances and identical services among providers. Future research could utilize geographic information systems to aid in modeling existing systems, populations, and hospital types. By modeling different specializations and services for providers, researchers could account for capacity and assess its influence on different medical systems (e.g., urban, rural, teaching hospitals). Even though several of these factors may not be critical when studying CHF, it would be necessary to account for when studying other comorbidities. All of the aforementioned aspects are important in understanding patient choice behavior [15]. Analyzing them would allow us to better understand capacity implications in provider and patient decision models and also provide an additional validating pathway to compare model outcomes with existing systems outcomes.
Patient agents in the model can also be improved by increasing the complexity of the decision-making module. Patients typically interact socially with other patients and their providers, and the impact of this interaction can be represented in the model. With these improvements, the social aspect of patient choice can be better represented and understood.
The capability of introducing bypass control initiatives to the modeled system would allow us to study potential emergent behavior patterns and system outcomes. It would permit researchers to optimize particular outcomes and test proposed designs. Information availability and provider transparency could also be modified to reflect patient perception and model the effects of different policies on public reporting of quality of care. For example, patients who have updated information about the quality of possible providers are more likely to seek care from a provider that delivers better quality of care [22].
7 Conclusion
Patient choice affected health care payments, quality of care, and provider ACO participation. The effects of patient choice were most salient in scenarios in which providers had a choice regarding ACO participations. Therefore, the results suggest that the effects of patient choice, as an instrument in health care delivery, may not be fully realized without providers’ ability to differentiate themselves. In addition, the effects of patient choice were minuscule in terms of population health and quality outcomes. These findings, which are consistent with existing theories on the effects of patient choice, are critical in the wake of recent health care initiatives and reforms [23].
This research exhibited the potential for using complex systems modeling to generate insights regarding the dynamic, adaptive, and heterogeneous health care systems. By building a patient agent capable of making a bypass decision and fitting the agent into an existing ACO agent-based simulation model, this study successfully provided an approach capable of quantifying the effects of several aspects of patient choice on an ACO system. This model is a step in the right direction to decipher the complex interplay among various aspects of health care delivery and payment. As health care models converge toward accountability in payment and delivery, tools and approaches to understand the effects of key components are invaluable. The versatility of this approach, once further validated, will allow for testing of various policies to understand implications of patient bypass behavior and its impact on the system. This version of the model may be the first step in building a computational laboratory for researchers to test policy approaches to understanding and optimizing patient choice for more effective health care delivery.
References
England M (1994) From fee-for-service to accountable health plans. In: Schreter R, Sharfstein S. Schreter C Allies Advers. American Psychiatric Association Press, Washington DC, pp. 3–5
Enthoven AC (2009) Integrated delivery systems: the cure for fragmentation. Am J Manag Care 15:S284–S290
Nyweide DJ, Lee W, Cuerdon TT et al (2015) Association of pioneer accountable care organizations vs traditional Medicare fee for service with spending, utilization, and patient experience. J Am Med Assoc 313:2152–2161. doi:10.1001/jama.2015.4930
Centers for Medicare & Medicaid Services (2011) Shared Savings Program, Section 1899 of the Social Security Act (as amended by Affordable Care Act Section 3022 Medicare Shared Saving Program)
Liu P, Wu S (2014) An agent-based simulation model to study accountable care organizations. Health Care Manag Sci. doi:10.1007/s10729-014-9279-x
Dixon A, Ruth R, Appleby J, et al. (2010) Patient choice: how patients choose and how providers respond. http://www.kingsfund.org.uk/publications/patient-choice
Escarce JJ, Kapur K (2009) Do patients bypass rural hospitals? Determinants of inpatient hospital choice in rural California. J Health Care Poor Underserved 20:625–644. doi:10.1353/hpu.0.0178
Basu J, Mobley LR (2010) Impact of local resources on hospitalization patterns of Medicare beneficiaries and propensity to travel outside local markets. J Rural Health 26:20–29. doi:10.1111/j.1748-0361.2009.00261.x
Gauthier B, Wane W (2011) Bypassing health providers: the quest for better price and quality of health care in Chad. Soc Sci Med 73:540–549. doi:10.1016/j.socscimed.2011.06.008
Varkevisser M, van der Geest S a (2007) Why do patients bypass the nearest hospital? An empirical analysis for orthopaedic care and neurosurgery in the Netherlands. Eur J Health Econ 8:287–295. doi:10.1007/s10198-006-0035-0
Liu, J Jason, Bellamy GR, McCormick M (2007) Patient bypass behavior and critical access hospitals: Implications for patient retention. J. Rural Heal.
Tai W-TC, Porell FW, Adams EK (2004) Hospital choice of rural Medicare beneficiaries: patient, hospital attributes, and the patient-physician relationship. Health Serv Res 39:1903–1922. doi:10.1111/j.1475-6773.2004.00324.x
Buczko W (2001) Rural Medicare beneficiaries’ use of rural and urban hospitals. J Rural Health 17:53–58
Liu JJ, Bellamy G, Barnet B, Weng S (2008) Bypass of local primary Care in Rural Counties: effect of patient and community characteristics. Ann Fam Med 6:124–130. doi:10.1370/afm.794.introduction
Basu J (2005) Severity of illness, race, and choice of local versus distant hospitals among the elderly. J Health Care Poor Underserved 16:391–405. doi:10.1353/hpu.2005.0023
Phillips CO, Wright SM, Kern DE et al (2004) Comprehensive discharge planning with postdischarge support for older patients with congestive heart failure: a meta-analysis. JAMA 291:1358–1367. doi:10.1001/jama.291.11.1358
lefts for Medicare and Medicaid Services (CMS) H (2012) Hospital inpatient prospective payment Systems for Acute Care Hospitals and the long-term care hospital prospective payment system and fiscal year 2013 rates; hospitals’ resident caps for graduate medical education payment purposes. Quality Reporting, Requ
Roh C, Lee K (2005) Hospital choice by rural Medicare beneficiaries: does hospital ownership matter? - a Colorado case. J Health Hum Serv Adm 28:346–365
Radcliff TA, Brasure M, Moscovice IS, Stensland JT (2002) Understanding rural hospital bypass behavior. J Rural Health 19:252–259. doi:10.1111/j.1748-0361.2003.tb00571.x
Whellan DJ, Greiner MA, Schulman KA, Curtis LH (2010) Costs of inpatient care among Medicare beneficiaries with heart failure, 2001 to 2004. Circ. Cardiovasc Qual Outcomes 3:33–40. doi:10.1161/ciroutcomes.109.854760
Fitch K, Pelizzari PM (2015) Pyenson B. The High Cost of Heart Failure for the Medicare Population, An Actuarial Cost Analysis
Porell FW, Adams EK (1995) Hospital choice models: a review and assessment of their utility for policy impact analysis. Med Care Res Rev 52:158–195. doi:10.1177/107755879505200202
Gaynor M, Town RJ (2011) Competition in Health Care Markets. National Bureau of Economic Research. doi:10.3386/w17208
Acknowledgments
We would like to thank Dr. Pai Liu for sharing with us the ACO agent-based simulation model he developed as part of his dissertation project in the Health Systems Engineering Lab directed by Dr. Shinyi Wu at the University of Southern California. Dr. Wu is sponsored by the Roybal Institute on Aging at the School of Social Work, University of Southern California.
We would also like to thank Dr. Michael Nichol from the Department of Health Policy and Management at the University of Southern California. Dr. Nichol helped develop the original model by Liu and Wu and was vital in developing and interpreting the results of this expansion.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Appendix A. Sensitivity Analysis
Appendix A. Sensitivity Analysis
The sensitivity analysis was performed on one scenario; providers had a choice of participating in an ACO and patients had a choice between local and alternative providers. In total, 4200 replicates were analyzed, with each set of 100 replicates corresponding to a combination of values for the distance coefficient, mortality rate odds ratio (OR), hospitalization rate OR, and disease management OR. The results are presented in a matrix of plots for each outcome measure and model parameter, along with a standard least squares regression fit for each outcome.
The tables below represent the relationship between four key model parameters (horizontal axis) and measurable simulation outcomes (vertical axis) developed using JMP Pro v12. The vertical dashed line in every plot corresponds to the original values of the model parameters. The horizontal dashed line in every plot corresponds to the value of the key outcome at the original value of the model parameter. Note that ORs that are farther from 1 indicate higher sensitivity. Therefore, the columns corresponding to the ORs of CHF patient bypass for differences in mortality rates and hospitalization rates (Columns 1 and 2) are decreasing in sensitivity from left to right, because the right-most value is an OR of 1. Meanwhile, in the column corresponding to odds ratio for patient bypass for a difference in offering disease management (Column 3), the patient bypass decision becomes more sensitive from left to right.
Table a1. Payment Outcomes Sensitivity:
Shared Savings ($):
Term | Coefficient | Std. Error | T-ratio | Prob > |t| |
|---|---|---|---|---|
Intercept | 1126.6108 | 227.3818 | 4.95 | <.0001* |
Mortality Rate OR | -0.087882 | 0.454684 | -0.19 | 0.8467 |
Hospitalization rate OR | 8.0887695 | 156.7177 | 0.05 | 0.9588 |
Disease management OR | -278.5397 | 167.0616 | -1.67 | 0.0955 |
Distance Parameter | -22.54507 | 22.49653 | -1.00 | 0.3163 |
This model suggests that within the tested ranges, none of the model parameters significantly influenced savings realized in an ACO.
Per CHF Patient Payment in ACO ($):
Term | Coefficient | Std. Error | T-ratio | Prob > |t| |
|---|---|---|---|---|
Intercept | 15,819.445 | 205.4774 | 76.99 | <.0001* |
Mortality rate OR | 0.2231381 | 0.410883 | 0.54 | 0.5871 |
Hospitalization rate OR | -122.2252 | 141.6206 | -0.86 | 0.3882 |
Disease management OR | -121.2628 | 150.968 | -0.80 | 0.4219 |
Distance parameter | -49.12623 | 20.32937 | -2.42 | 0.0157* |
Total per patient payment was significantly influenced by the distance parameter in this sensitivity analysis.
Table a2. ACO Participation Sensitivity:
Number of ACO Hospitals:
Term | Coefficient | Std. Error | T-ratio | Prob > |t| |
|---|---|---|---|---|
Intercept | 1.6351875 | 0.284487 | 5.75 | <.0001* |
Mortality rate OR | 0.0004861 | 0.000569 | 0.85 | 0.3929 |
Hospitalization rate OR | -0.329667 | 0.196076 | -1.68 | 0.0928 |
Disease management OR | 0.0604167 | 0.209018 | 0.29 | 0.7726 |
Distance parameter | 0.0076333 | 0.028146 | 0.27 | 0.786 |
The results of this model suggest that none of the key model parameters tested within the ranges of this sensitivity analysis influenced hospitals’ decisions to remain in the ACO.
Number of ACO Clinics:
Term | Coefficient | Std. Error | T-ratio | Prob > |t| |
|---|---|---|---|---|
Intercept | 7.0897083 | 0.622143 | 11.40 | <.0001* |
Mortality rate OR | -0.000366 | 0.001244 | -0.29 | 0.7688 |
Hospitalization rate OR | -0.192833 | 0.428798 | -0.45 | 0.6529 |
Disease management OR | 0.0541667 | 0.4571 | 0.12 | 0.9057 |
Distance parameter | 0.0872556 | 0.061553 | 1.42 | 0.1564 |
The results of this model suggests that none of the key model parameters tested within the ranges of this sensitivity analysis influenced clinics’ decisions to remain in the ACO.
Table a3. Quality Outcome Sensitivity:
Tables a4. Model fits for sensitivity analysis parameters.
Bypass:
Term | Coefficient | Std. Error | T-ratio | Prob > |t| |
|---|---|---|---|---|
Intercept | 51.567674 | 1.069226 | 48.23 | <.0001* |
Mortality Rate OR | -0.043628 | 0.002138 | -20.41 | <.0001* |
Hospitalization Rate OR | -3.648671 | 0.736939 | -4.95 | <.0001* |
Disease Management OR | -7.87512 | 0.78558 | -10.02 | <.0001* |
Distance Parameter | 1.0145 | 0.105786 | 9.59 | <.0001* |
The results of this model suggest that increasing the mortality rate OR and hospitalization rate OR (decreasing sensitivity) significantly decreased the probability of bypassing. In addition, increasing disease management preference (increasing sensitivity) significantly increased the probability of bypassing. Furthermore, increasing the distance parameter (the assumed distance between providers) significantly decreased the probability of CHF patient bypass.
Hospitalization Rates:
Term | Coefficient | Std. Error | T-ratio | Prob > |t| |
|---|---|---|---|---|
Intercept | 0.8127582 | 0.016531 | 49.16 | <.0001* |
Mortality Rate OR | 1.1125e-5 | 0.000033 | 0.34 | 0.7365 |
Hospitalization Rate OR | 0.0020345 | 0.011394 | 0.18 | 0.8583 |
Disease Management OR | -0.015552 | 0.012146 | -1.28 | 0.2005 |
Distance Parameter | -0.001855 | 0.001636 | -1.13 | 0.2569 |
The results of this model suggest that varying the distance between providers and the desirability of lower mortality rates and hospitalization rates did not influence the actual hospitalization rates for the simulated CHF population.
Mortality Rates:
Term | Coefficient | Std. Error | T-ratio | Prob > |t| |
|---|---|---|---|---|
Intercept | 0.2267616 | 0.006633 | 34.18 | <.0001* |
Mortality Rate OR | -6.438e-8 | 1.326e-5 | -0.00 | 0.9961 |
Hospitalization Rate OR | 0.0053993 | 0.004572 | 1.18 | 0.2377 |
Disease Management OR | 0.001215 | 0.004874 | 0.25 | 0.8031 |
Distance Parameter | -0.000685 | 0.000656 | -1.04 | 0.2969 |
The results of this model suggest that varying the distance between providers and the desirability of lower mortality rates and hospitalization rates did not influence the actual mortality rates for the simulated CHF population.
Rights and permissions
About this article
Cite this article
Alibrahim, A., Wu, S. An agent-based simulation model of patient choice of health care providers in accountable care organizations. Health Care Manag Sci 21, 131–143 (2018). https://doi.org/10.1007/s10729-016-9383-1
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10729-016-9383-1