Summary
Macrocyclic compounds meso-(p-acetamidophenyl)-calix[4]pyrrole and meso-(m-acetamidophenyl)-calix[4]pyrrole have previously been reported to exhibit cytotoxic properties towards lung cancer cells. Here, we report pre-clinical in vitro and in vivo studies showing that these calixpyrrole derivatives can inhibit cell growth in both PC3 and DU145 prostatic cancer cell lines. We explored the impact of these compounds on programmed cell death, as well as their ability to inhibit cellular invasion. In this study we have demonstrated the safety of these macrocyclic compounds by cytotoxicity tests on ex-vivo human peripheral blood mononuclear cells (PBMCs), and by in vivo subcutaneous administration. Preliminary in vivo tests demonstrated no hepato-, no nephro- and no genotoxicity in Balb/c mice compared to controls treated with cisplatin. These findings suggest these calixpyrroles might be novel therapeutic tools for the treatment of prostate cancer and of particular interest for the treatment of androgen-independent castration-resistant prostate cancer.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Prostate cancer (PCa) is considered one of the ‘big killers’, accounting for 1.2 million cases and 359,000 deaths in 2018 [1]. According to GLOBOCAN 2018, PCa is the second most frequent cancer in men and the fifth cause of death worldwide. Its prevalence is higher in developed countries and its mortality rate is strongly correlated to age [1]. PCa affects mainly patients with significant comorbidities. These epidemiological features provide an estimate of the socioeconomic impact of this disease. Androgen deprivation therapy (ADT) represent the cornerstone of PCa treatment as the initial response rate is about 80%. During ADT, disease progresses and develops distant metastases in 35% of patients treated for local PCa, while 10–20% of the patients with advanced stage of the disease become refractory to ADT [2] evolving castration-resistant prostate cancer (CRPC). Notably, the development of CRPC is mostly associated with poor prognosis and overall survival time of about 14 months [3]. Although, by 2019 several clinical trials regarding the therapeutic management of PCa were concluded with positive results, to date the advanced and aggressive variants of CRPC remain incurable [4].
Calix[4]pyrroles (C4PYs) are macrocycles (heterocyclophanes) containing four pyrrole units linked by quaternary carbon atoms [5]. Unlike porphyrins, they do not have a planar shape and an extended delocalized electronic system. The pyrrole NH units provide an array of hydrogen-bond donors that can effectively interact with a variety of hydrogen-bond acceptors (anions as well as neutral molecules), thus forming supramolecular complexes in which the selectivity (towards different acceptors and their binding strengths) can be extensively modulated by decorating the calixpyrrole core-structure with ancillary chemical moieties [6,7,8,9,10,11,12,13].
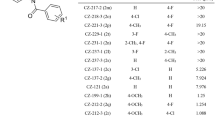
Although C4PYs are known since more than a century [Baeyer, A. (1886), Ueber ein Condensations product von Pyrrol mit Aceton. Ber. Dtsch. Chem. Ges., 19: 2184–2185. https://doi.org/10.1002/cber.188601902121], their use in medicinal chemistry has been pioneered by our group through a rather serendipitous approach. Looking for a novel nanovector to properly deliver cytotoxic drugs directly to cancer cells, we initially reported the ability of meso-p-aminophenylcalix[4]pyrrole to form a cytotoxic trans-Pt(II) complex (215 in Fig. 1) in which the calix unit appears to assist the delivery of the toxic metal to DNA via the preliminary binding of the phosphate residues [14]. Later on, it has been demonstrated how some C4PYs derivatives exhibit cytotoxic actions against selected cell lines by acting as ionophores capable of altering chloride transport across cell membranes [15]. In parallel, we reported that meso-octamethyl-calix[4]pyrrole (100 in Fig. 1) acts as an antagonist of the G-Protein Coupled Estrogen Receptor 30 (GPER/GPR30) in different model systems, such as breast tumour cells and cancer-associated fibroblasts [16] hence exhibiting a biological action that is associated with its ability to interact with specific proteins rather than acting just as ionophores. To our minds, these results indicated that C4PYs deserve additional investigation as potential drugs in their own right, rather than as merely vectors of biologically active species. In this context we showed that the C4PY derivatives 107 and 563 (Fig. 1) exhibit very different cytotoxicity towards different cell lines [17, 18]. All together, these observations prompted us to further investigate 107 and 563 searching for cancer types for which they could be useful drug candidates. Hereby, we report cytotoxic effects of 107 and 563 on two androgen-independent PCa cell lines (DU145 and PC3).
Materials and methods
Chemistry, cell lines and culture
Calixpyrrole derivatives 107 and 563 were prepared as previously reported [17] and their purity checked.
Prostate cancer (PCa: PC3, DU145 and LNCaP), small cell lung cancer (SCLC: DMS-79, IST-SL1, IST-SL2), ovarian serous adenocarcinoma (A2774) and glioblastoma (U251) cell lines were purchased from the ICLC (Biological Bank and Cell Factory, IRCCS Policlinico San Martino, Genoa, Italy), and cultured respectively in RPMI (Pan Biotech, Aidenbach, Germany) or DMEM (Sigma-Aldrich, Milan, Italy), both supplemented with 10% fetal calf serum (Euroclone, Milan, Italy), 2 mM L-glutamine (Euroclone, Milan, Italy), and 1% penicillin–streptomycin (Euroclone, Milan, Italy) at 37 °C in a 5% CO 2 incubator.
MTT assay
We evaluated cytotoxicity by MTT assay; cancer cell lines were seeded in 96-well plates and treated with various concentrations (up to 100 µM) of 107 or 563 for 48 h. Tests for each compound was conducted independently at least three times. The half maximal inhibitory concentration (IC50) values were determined using GraphPad Prism® software (GraphPad Prism® 6.01, GraphPad Software, Inc., CA, USA).
Annexin-V analysis of apoptotic cells
Apoptosis analysis was performed using Muse™ Annexin V & Dead Cell Assay. PC3 and DU145 cells were seeded at a density of 2 × 10 5 per well in 1 mL of culture medium DMEM (Sigma-Aldrich, Milan, Italy), and treated with 107 or 563 at IC50 concentrations for 48 h. Samples were stained at room temperature in the dark for 20 min using Muse™ Annexin V & Dead Cell Reagent (Millipore Merck, Vimodrone Milan, Italy).
Multicaspase assay
PC3 and DU145 cells (1 × 106 cells/well/2 mL culture media) were seeded at 37 °C in a 6-well plate and allowed to reach 70–80% confluence, then treated with 107 or 563 for 24 h at IC50 concentrations as previously described [19]. Muse™ multicaspase assay kit (Millipore Merck, Vimodrone Milan, Italy) was used for the detection of multiple caspase activation (caspase-1, -3, -4, -5, -6, -7, -8 and -9), following manufacturer’s instructions. The percentage of cells with multicaspase activity was subsequently examined using Muse™ cell analyzer (Millipore Merck, Vimodrone Milan, Italy) flow cytometer.
Cell invasion assays
Cell invasion assays were carried out in Matrigel chambers (BD Bio Coat) as previously described [20]. PC3 and DU145 cells were seeded (3 × 104 cell/well) in the Matrigel chamber in serum-free medium with 0.1% DMSO as control or with 1 µM solutions of 107, 563, or etoposide. Invasion assay was carried out using medium supplemented with 20% FBS as a chemo attractant for 48 h. PC3 and DU145 cells that invaded the lower chamber were fixed with 100% methanol and stained with 1% toluidine blue in 1% borax. The invasion index was determined by cell count as the ratio of cells treated with 107 or 563 compared to untreated cells that invaded the Matrigel chamber.
Ex-vivo toxicity of 107 and 563
The toxicity of 107 and 563 was examined against Peripheral Blood Mononuclear cells (PBMCs) from healthy volunteers (22–55 years). PBMCs were cultured in medium supplemented with interleukin-2 (IL-2) and seeded in a 96-well microplate (4 × 105 – 5 × 104 cells/200µL/well). The two compounds were added to the cell cultures at final concentrations ranging from 1–300 µM. For this purpose, 107 and 563 were added in identical volumes of DMSO solutions of appropriate concentrations in order to have a final concentration of DMSO 0.1% in the cell culture medium in all cases. The cells were incubated at 37 °C for 48 h in a humidified 5% CO2 incubator. Cell cytotoxicity was evaluated by the trypan blue dye exclusion technique.
Experimental design for the study on animals
After an acclimation period, Balb/c mice were randomly divided into 3 groups of 6 mice each. The first group received a subcutaneous injection with 50 mg/kg b.w. of 107 dissolved in an olive oil/DMSO mixture. The positive control group was treated with intraperitoneal injections of cisplatin (CDDP) (15 mg/kg b.w.) dissolved in a DMSO/PBS solution, the negative control group was administered with 5% DMSO in PBS. In all cases the amount of DMSO administered to the mice was below 0.01% of the body weight. Animals were killed 72 h after the injection. Body weight was measured before and after treatment with 107 and CDDP. The major organs (spleen, liver, lung, brain, and kidney) were harvested, inspected and weighed on an electronic balance after blotting the blood and body fluids on filter paper. The organ coefficient was calculated as the ratio of organ weight (in mg) per 10 g of animal weight. Blood samples were collected from the scarified animals and immediately placed in heparin anticoagulant tubes. Samples were then centrifuged at 1,500 rpm for 7 min. Plasma was obtained and stored at -20 °C for biochemical parameters analysis.
Genotoxic effect of 107
Alkaline comet assay was carried out as reported previously [21]. Spleens and kidneys of Balb/c mice treated with 107 or CDDP were individually homogenized with 10 mM Tris–HCl (pH 7.4) and centrifuged at 12,000 rpm at 4 °C for 25 min. The cellular supernatants were used to examine DNA damage. Cellular suspensions were embedded in agarose gel, lysed, and subjected to electrophoresis. The total score of DNA damage was calculated as reported [22].
Histopathology
For histological analysis, kidney sections were prepared as previously described [23]. Organs were collected from the 3 groups and: a) fixed with 10% phosphate-buffered neutral formalin; b) dehydrated in graded alcohol (75–95%), and c) embedded in paraffin. Slices (5 μm thick) were stained with hematoxylin and eosin (H & E) and analyzed by optical microscopy (Leica DMI 4000 B; Leica Microsystems, Wetzlar, Germany).
Determination of liver and kidney function indexes
Aspartate transaminase (AST), alanine transaminase (ALT), and creatinine (CR) levels in plasma were evaluated by clinical chemistry analyzer COBAS C × 72. 4.15.
Results
Cytotoxicity of C4PYs 107 and 563 in different human cancer cell lines
The viability of PCa (PC3 and DU145), SCLC (DMS-79, IST-SL1, IST-SL2), ovarian serous adenocarcinoma (A2774) and glioblastoma (U251) cell lines were evaluated by MTT assay after 48 h treatment with C4PYs 107 or 563. The highest cytotoxic activity was observed against PCa cell lines (Table 1). Dose–response curves for the cytotoxic effects of 107 and 563 against PC3 and DU145 are shown in Fig. 2. The IC50 for 107 and 563 were 4.9 µM and 10.8 µM for PC3 cell line and 9.0 µM and 9.9 µM for DU145, respectively. A lower anti proliferative potential was recorded for ovarian and glioblastoma cell lines. No significant cytotoxic effect was detected for SCLC cell lines.
Apoptosis induction in PC3 and DU145 cell lines
We analysed the apoptotic potential of 107 and 563 in PC3 and DU145 cell lines at the IC50 concentrations determined using MTT. The Annexin V/7-AAD assay confirmed the IC50 obtained through the MTT assays and the prevalent apoptotic mechanism of cell death in PC3 and DU145 (Supplementary Figs. S1 and S2 respectively).
We also used the Muse™ multicaspase (Millipore Merck, Vimodrone Milan, Italy) assay kit to gain an insight into the apoptosis mechanism of action. Caspase activation (caspase-1, 3, 4, 5, 6, 7, 8, and 9) was evaluated. After 24 h 107 (IC50) and 563 (IC50) were able to increase caspase activation in PC3 (19.47% and 20.52% respectively) and DU145 (32.15% and 10.99% respectively) (Supplementary Figs. S3 and S4). Thus, for DU145 cells, 107 induced a higher caspase activation than 563. All indicated values are referred to the DMSO negative control.
Invasion inhibition of PC3 and DU145 cell lines treated with 107 and 563
We evaluated the inhibitory effects of 107 and 563 on the invasive ability of PC3 and DU145 cells by Matrigel invasion assay. Based on previous results, this test was conducted using the C4PYs derivatives at 1 µM concentration. Compared to control cells treated with DMSO alone (0.1%), 107 and 563 displayed a remarkable inhibitory effect against PC3 and DU145 cell invasiveness. For PC3 33.6% and 43.9% respectively (Supplementary Fig. S5), and for DU145 14.6% and 80.7% respectively (Supplementary Fig. S6), in comparison to the negative control (100%). Notably, the inhibitory activity of 107 and 563 was found to be more effective than 1 μM etoposide, an antineoplastic agent used as the positive control [24]. This in vitro invasion assay suggests that C4PY 107 and 563 inhibit the metastatic potential of PCa cells.
Ex-vivo toxicity of 107 and 563
The toxicity of 107 and 563 were determined against PBMCs collected from healthy volunteers. The PBMCs were treated with 107 and 563 at 1–300 µM concentrations. After 48 h, the viability of both controls and treated cells was determined by trypan blue dye exclusion. The results showed no cytotoxic effect on lymphocytes compared to the negative control at any of the tested concentrations (Fig. 3).
Effect of C4PY 107 on mice weight organ coefficient and morphologies
The toxicity study was limited to 107 as this compound was found to be the most cytotoxic in cancer cells compared to 563. After 72 h from the cutaneous administration of 107 to Balb/c mice no significant changes in body weight, mental state, food, and water consumption could be detected compared to the negative control. In contrast, mice treated with CDDP appeared to suffer from exhaustion (behaviour), and showed a significant body weight loss (Supplementary Fig. S7). After CDDP administration, mice showed normal average weight for liver, lung, brain, and heart while we observed a significant reduction of spleen and kidney coefficients (Supplementary Table ST2). In contrast, the administration of 107 did not affect the organ coefficients nor spleen and kidney morphology (Fig. 4).
Effect of 107 on ALT, AST and creatinine serum levels
Transaminases and creatinine serum levels were measured in the three groups of mice treated with 107, CDDP, and DMSO controls after 72 h. While significantly increased functional biomarkers were observed in CDDP-treated mice, there was no statistically significant difference between the negative control and mice treated with 107, indicating no hepato- or nephro-toxicity induced by the tested compound (Supplementary Fig. S8). The effects of CDDP on these biochemical parameters, are consistent with those reported previously [25].
Genotoxic effect of C4PY 107: Comet assay
DNA damage induction was evaluated using the alkaline comet assay (Fig. 5). The total score of DNA damage showed no significant differences between spleen and kidney cells of mice treated with 107 and negative controls. However, we detected a significant increase in total DNA damage of spleen and kidney in mice treated only with CDDP.
a Photographs for the comet assay evaluation of DNA damage in mice kidney cells: NC negative control (DMSO 0.1%), CDDP-treated, 107-treated. b Histogram reports ex-vivo comet score of the spleen and kidney cells. ****P < 0.0001 compared to the negative control group that received equal dosage of DMSO; CDDP was used as positive control
Kidney histopathology
Histopathological analysis of the mice kidneys revealed normal glomerulus and tubules with regular morphology in both negative controls and 107-treated animals. By contrast, CDDP induced damage in the kidneys characterized by renal tubule necrosis (Fig. 6).
Histology of kidney samples: DMSO negative control; 107-treated mouse; and CDDP-treated mouse. Normal histological structure of the tubules (t) and glomeruli (g) are observed in the negative control and in 107-treated animals; necrosis in tubules (n) is evident in CDDP-treated mice (c); hematoxylin–eosin staining, magnifications: × 40
Discussion
Crucial steps in the development of a new drug include the determination of its toxicity and of the molecular mechanism of action (i.e. the biological target). For cancer drugs, which should impair or kill cancer cells, toxicity is a requirement that should be evaluated in relative terms with respect to non-targeted cells, hence selectivity is paramount. Indeed, our study indicates considerable selectivity of 107 and 563 towards different cancer cells lines: powerful cytotoxic action against non-small cell lung cancer A549 and PCa (PC3 and DU145), modest activity against ovarian cancer A2774 and SKOV3, and negligible activity against glioma U251, and SCLC (IST-SL1, IST-SL2, and DMS-79) cell lines. This selectivity of action leads us to the hypothesis that the formation of DNA adducts we have previously reported [17] might not be the primary mechanism of action. Data on the human apoptotic proteins array (checking expressions of 43 proteins) was followed by a qRT-PCR to investigate the apoptosis pathway (see Supplementary Information and Supplementary Fig. S9). We demonstrated that 107 and 563 modulate the apoptotic protein and gene expressions including Bcl-2 and caspase 3 in A549. These data triggered our interest in apoptosis including the abnormal expression of Bcl-2 that increases anti-apoptotic potency and chemoresistance.
We have also evaluated LNCaP cells, another PCa cell line that, unlike DU145 and PC3, express the AR receptor, and that was considered an in vitro PCa model for the phase prior to the establishment of anti-androgen resistance. Only modest activities (IC50 of approximately 30 μM) were observed for both compounds, probably due to the inherently lower proliferation rate of LNCaP cells with respect to DU145 and PC3 cells (data not shown). Indeed, some drugs which act on DNA or its repair mechanisms usually work better on faster replicating cells than on slower growing cells such as LNCaP. There is a great deal of documentation to support this, including our previous paper on 107 and 563 against A549 [17].
We considered various drugs commonly used in PCa treatment to be used as the ‘in house’ positive reference. Taking into account the above cited modulation of Bcl-2 and caspase 3 in A549 cells, we referred to a paper [26] in which the authors investigated the effects of Bcl-2 expression status on the susceptibility of DU145 cells to docetaxel (a taxane) and CDDP. Bcl-2 expression levels were unrelated to the susceptibility of DU145 cells to docetaxel. The sensitivity of DU145 cells to CDDP was reported. In a xenograft mouse model, over-expression of Bcl-2 drastically decreased the sensitivity of DU145 cells to CDDP. However, there was no change in the response to docetaxel. Interestingly, in this study docetaxel barely induced caspase-3/7 activation in controls or in Bcl-2-overexpressing DU145 cells. These findings indicate that the antitumor effects of docetaxel on DU145 cells are independent of both Bcl-2 and pro-apoptotic caspases. Therefore, although taxanes are first-line chemotherapeutic agents for PCa, in light of our previous study and that of Ogura, we were interested in using CDDP as a positive blank in our toxicity tests. Moreover, CDDP is a convenient reference compound because it is a conventional chemo-drug endowed with significant hepato- and nephro-toxicity [27].
We tested in vitro and ex-vivo toxicity of 107 and 563 on human PBMCs and on mice. There was no cytotoxic effect on lymphocytes compared to the negative control, at any of the concentrations tested. In vivo studies evidenced that 72 h after the subcutaneous administration of 107 at 50 mg/Kg dose there were no significant changes in Balb/c body weight, behavior, food and water consumption compared to the negative controls. In contrast, mice treated with 15 mg/kg of CDDP suffered from fatigue as well as exhibiting a significant loss of body weight. Transaminases (ALT and AST) and creatinine levels were not significantly different from negative controls, showing that 107 is neither hepato- nor nephro-toxic. Moreover, the comet assay showed no genotoxicity and histopathology of the kidney also exhibited normal glomerulus and tubule morphology.
The cell lines that derive from bone metastasis (PC3) and brain metastasis (DU145) are extensively used in research as a powerful tool for antitumoral drug discovery and for understanding the molecular pathways implicated in PCa anti-androgen resistance [28]. Both C4PY derivatives induced apoptosis after 48 h, as demonstrated by the Annexin V tests in both PCa cell lines.
The growth and survival of PCa cancers depend on androgens, male steroid hormones. The principal androgens are testosterone and dihydrotestosterone (DHT) which activate and bind to the androgen receptor (AR) [29]. High expression of AR is observed in most patients with castration resistant prostate cancer (CRPC). Moreover, the expression of AR-regulated genes that is restored in patients that received ADT implies that AR transcriptional activity is reactivated [29]. In particular, there is evidence that after ADT, a high concentration of DHT, the most potent AR agonist, can be produced by androgen precursors of adrenal origin [30, 31]. Consequently, molecular targets used to treat CRPC are not only AR antagonists but also androgen synthesis inhibitors. Other strategies in CRPC include targeting the mechanisms of survival (PI3K/AKT/mTOR), DNA repair, immune checkpoints, and stress-response.
In a previous study we demonstrated that C4PY 100 is a novel antagonist ligand of the Membrane Estrogen Receptor GPER [16] also providing an example for the binding of a calixpyrrole with a protein. The interaction of calixpyrrole derivatives with amino acids is also well documented [32]. Thus the observed selectivity, together with the numerous and considerable changes in miRNA expression determined in A549 cells point to a mechanism of action that is more specific than the exclusive formation of DNA adducts or a general impairment of cell homeostasis due to the transport of chloride ions across membranes, as previously suggested for other calix[4]pyrrole derivatives [15]. Recently, polymers capable of binding polyanionic proteins were reported to kill PCa cancer cells [33], and indeed 107 and 563 are anion binders.
The ability of 107 and 563 to inhibit PC3 and DU145 cell migration, at concentrations that are significantly lower than their IC50, is also an unprecedented discovery of this study with groundbreaking implications for the potential exploitation of the biological activity of calixpyrroles. The significance of this result lies in the invasiveness of PCa for which metastasis development is associated with poor prognosis and overall survival [34].
Conclusions
This work demonstrates that 107 and 563 are potentially useful new drugs or lead-compounds for the development of novel tools against CRPC. Despite the limitation that the details of their mechanism of action have still to be uncovered, a pragmatic observation of data presented here cannot but underscore this statement. All experiment conducted so far in order to uncover any significant toxicity (in vitro or in vivo) towards heathy cells or tissues, has given no indication of any adverse effects at the dosages that were effective against cell lines PC3, and DU145 in this study, and H727 and A549 in the previously reported one [17]. We are undertaking experiments by differential mass spectrometry on treated vs. non-treated cells to further characterize the genes and signaling pathways that are altered by 107 and 563 in different in vitro cancer models. The identification of specific alterations should allow us to define the cellular phenotype sensitive to these C4PY derivatives and pave the way to additional therapeutic options not only for CRPC patients but also for other neoplastic diseases.
Data availability statement
Any additional information will be made available by the authors, without undue reservation, to any qualified researcher upon request.
References
Bray F, Ferlay J, Soerjomataram I et al (2018) Global cancer statistics 2018: GLOBOCAN estimates of incidence and mortality worldwide for 36 cancers in 185 countries. CA Cancer J Clin 68:394–424. https://doi.org/10.3322/CAAC.21492
Arora K, Barbieri CE (2018) Molecular Subtypes of Prostate Cancer. Curr Oncol Rep 20:1–9
Kirby M, Hirst C, Crawford ED (2011) Characterising the castration-resistant prostate cancer population: a systematic review. Int J Clin Pract 65:1180–1192. https://doi.org/10.1111/J.1742-1241.2011.02799.X
Schmid S, Omlin A (2020) Progress in therapy across the spectrum of advanced prostate cancer. Nat Rev Urol 17:71–72
Gale PA, Anzenbacher P, Sessler JL (2001) Calixpyrroles II. Coord Chem Rev 222:57–102
Wagay SA, Rather IA, Ali R, Ali R (2019) Functionalized calix[4]pyrroles: Emerging class of ion-pair receptors in supramolecular chemistry. In: Materials Today: Proceedings. Elsevier, pp 657–678
Peng S, He Q, Vargas-Zúñiga GI et al (2020) Strapped calix[4]pyrroles: From syntheses to applications. Chem Soc Rev 49:865–907
Vargas-Zúñiga GI, Sessler JL (2017) Pyrrole N-H anion complexes. Coord Chem Rev 345:281–296
Saha I, Lee JT, Lee CH (2015) Recent Advancements in Calix[4]pyrrole-Based Anion-Receptor Chemistry. European J Org Chem 2015:3859–3885
Kim SK, Sessler JL (2014) Calix[4]pyrrole-based ion pair receptors. Acc Chem Res 47:2525–2536. https://doi.org/10.1021/ar500157a
Kim DS, Sessler JL (2015) Calix[4]pyrroles: Versatile molecular containers with ion transport, recognition, and molecular switching functions. Chem Soc Rev 44:532–546
Vargas Jentzsch A, Hennig A, Mareda J, Matile S (2013) Synthetic ion transporters that work with anion-π interactions, halogen bonds, and anion-macrodipole interactions. Acc Chem Res 46:2791–2800. https://doi.org/10.1021/ar400014r
Ballester P (2011) Supramolecular capsules derived from calixpyrrole scaffolds. Isr J Chem 51:710–724
Cafeo G, Carbotti G, Cuzzola A et al (2013) Drug delivery with a calixpyrrole-trans -Pt(II) complex. J Am Chem Soc 135:2544–2551. https://doi.org/10.1021/ja307791j
Ko SK, Kim SK, Share A et al (2014) Synthetic ion transporters can induce apoptosis by facilitating chloride anion transport into cells. Nat Chem 6:885–892. https://doi.org/10.1038/nchem.2021
Lappano R, Rosano C, Pisano A et al (2015) A calixpyrrole derivative acts as an antagonist to GPER, a G-protein coupled receptor: Mechanisms and models. DMM Dis Model Mech 8:1237–1246. https://doi.org/10.1242/dmm.021071
Geretto M, Ponassi M, Casale M et al (2018) A novel calix[4]pyrrole derivative as a potential anticancer agent that forms genotoxic adducts with DNA. Sci Reports 81(8):1–16. https://doi.org/10.1038/s41598-018-29314-9
Kohnke FH (2020) Calixpyrroles: from Anion Ligands to Potential Anticancer Drugs. European J Org Chem 2020:4261–4272
Parodi F, Carosio R, Ragusa M et al (2016) Epigenetic dysregulation in neuroblastoma: A tale of miRNAs and DNA methylation. Biochim Biophys Acta - Gene Regul Mech 1859:1502–1514. https://doi.org/10.1016/j.bbagrm.2016.10.006
Ferrari N, Granata I, Capaia M et al (2017) Adaptive phenotype drives resistance to androgen deprivation therapy in prostate cancer. Cell Commun Signal 15:51. https://doi.org/10.1186/s12964-017-0206-x
Singh NP, McCoy MT, Tice RR, Schneider EL (1988) A simple technique for quantitation of low levels of DNA damage in individual cells. Exp Cell Res 175:184–191. https://doi.org/10.1016/0014-4827(88)90265-0
Collins AR, Dobson VL, Dušinská M et al (1997) The comet assay: What can it really tell us? Mutat Res - Fundam Mol Mech Mutagen 375:183–193. https://doi.org/10.1016/S0027-5107(97)00013-4
Boubaker J, Ben Toumia I, Sassi A et al (2018) Antitumoral Potency by Immunomodulation of Chloroform Extract from Leaves of Nitraria retusa, Tunisian Medicinal Plant, via its Major Compounds β-sitosterol and Palmitic Acid in BALB/c Mice Bearing Induced Tumor. Nutr Cancer 70:650–662. https://doi.org/10.1080/01635581.2018.1460683
Siddiqui MF, Muqaddas M, Sarwar S (2015) BIOCHEMICAL MECHANISMS OF ETOPOSIDE; UPSHOT OF CELL DEATH. Int J Pharm Sci Res 6:4920. https://doi.org/10.13040/IJPSR.0975-8232.6(12).4920-39
Palipoch S, Punsawad C (2013) Biochemical and histological study of rat liver and kidney injury induced by cisplatin. J Toxicol Pathol 26:293–299. https://doi.org/10.1293/tox.26.293
Ogura T, Tanaka Y, Tamaki H, Harada M (2016) Docetaxel induces Bcl-2- and pro-apoptotic caspase-independent death of human prostate cancer DU145 cells. Int J Oncol 48:2330–2338. https://doi.org/10.3892/ijo.2016.3482
Tsang RY, Al-Fayea T, Au HJ (2009) Cisplatin overdose: Toxicities and management. Drug Saf 32:1109–1122
Sobel RE, Sadar MD (2005) Cell lines used in prostate cancer research: A compendium of old and new lines - Part 2. J Urol 173:360–372
Lian F, Sharma NV, Moran JD, Moreno CS (2015) The biology of castration-resistant prostate cancer. Curr Probl Cancer 39:17–28. https://doi.org/10.1016/j.currproblcancer.2014.11.004
Sharifi N (2013) Minireview: Androgen metabolism in castration- resistant prostate cancer. Mol Endocrinol 27:708–714
Simard J, Ricketts ML, Gingras S et al (2005) Molecular biology of the 3β-hydroxysteroid dehydrogenase/ Δ5-Δ4 isomerase gene family. Endocr Rev 26:525–582
Sessler JL, Gale PA, Genge JW (1998) Calix[4]pyrroles: New solid-phase HPLC supports for the separation of anions. Chem - A Eur J 4:1095–1099. https://doi.org/10.1002/(SICI)1521-3765(19980615)4:6%3c1095::AID-CHEM1095%3e3.0.CO;2-1
Takahashi H, Yumoto K, Yasuhara K et al (2019) Anticancer polymers designed for killing dormant prostate cancer cells. Sci Rep 9:1–11. https://doi.org/10.1038/s41598-018-36608-5
Smith MR, Mehra M, Nair S et al (2020) Relationship Between Metastasis-free Survival and Overall Survival in Patients With Nonmetastatic Castration-resistant Prostate Cancer. Clin Genitourin Cancer 18:e180–e189. https://doi.org/10.1016/j.clgc.2019.10.030
Funding
This work was partially supported by grants to C.R. from the Italian Ministry of Health (5 × 1000 funds 2018–2019 and Ricerca Corrente 2021). C.R. and F.H.K. acknowledge the support from COST Action CA16231 “ENOVA”—European Network of Vaccine Adjuvants. F.H.K. thanks Messina University for awarding the FFABR Unime PO 2019. C.R. wishes to thank the COST Action CA17104 “STRATAGEM”—New diagnostic and therapeutic tools against multidrug-resistant tumors”, for their support and funding an STSM to I.B.T. through an "STSM" fellowship. E.I. and G.C.V are supported by fellowships from the Italian Ministry of Health (5 × 1000 funds 2018–2019).
Author information
Authors and Affiliations
Contributions
C.R.., Conceptualization; I.B.T, M.P., P.B., F.H.K.., S.F., and B.B. Investigation; I.B.T, L.C.G., P.B., B.B. and A.I. Formal analysis; I.B.T, G.C.V. and C.R Writing—original draft; P.B., E.I., G.C.V. and C.R. Writing—review & editing; A.I. and C.R. Methodology and validation; C.R., Funding acquisition and Supervision.
Corresponding authors
Ethics declarations
Ethics statement
All experiments on Balb/c mice (22–26 g) were performed following the European Communities Council Directive (86/609/EEC; November 24, 1986) regulating the welfare of experimental animals, and experiments were approved by the Life Sciences and Health Research Ethics Committee (cer-svs) of the Institute of Biotechnology (University of Monastir, Tunisia; ethical approval no. 2019/02/I/CER-SVS/ISBM; 9 January, 2019). Mice were housed under standard conditions in an accredited pathogen-free facility. All animals were provided access to filtered water and standard rodent chow ad libitum.
Conflict of interest
C.R. is member of the Advisory Board of GIAM PHARMA International S.A.R.L., Monthey (CH). Other authors declare any conflict of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Toumia, I.B., Ponassi, M., Barboro, P. et al. Two calix[4]pyrroles as potential therapeutics for castration-resistant prostate cancer. Invest New Drugs 40, 1185–1193 (2022). https://doi.org/10.1007/s10637-022-01294-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10637-022-01294-8