Abstract
Background
Circulating endotoxin (lipopolysaccharide, LPS) increases the gut paracellular permeability. We hypothesized that glucagon-like peptide-2 (GLP-2) acutely reduces LPS-related increased intestinal paracellular permeability by a mechanism unrelated to its intestinotrophic effect.
Methods
We assessed small intestinal paracellular permeability in vivo by measuring the appearance of intraduodenally perfused FITC-dextran 4000 (FD4) into the portal vein (PV) in rats 1–24 h after LPS treatment (5 mg/kg, ip). We also examined the effect of a stable GLP-2 analog teduglutide (TDG) on FD4 permeability.
Results
FD4 movement into the PV was increased 6 h, but not 1 or 3 h after LPS treatment, with increased PV GLP-2 levels and increased mRNA expressions of proinflammatory cytokines and proglucagon in the ileal mucosa. Co-treatment with a GLP-2 receptor antagonist enhanced PV FD4 concentrations. PV FD4 concentrations 24 h after LPS were higher than FD4 concentrations 6 h after LPS, reduced by exogenous GLP-2 treatment given 6 or 12 h after LPS treatment. FD4 uptake measured 6 h after LPS was reduced by TDG 3 or 6 h after LPS treatment. TDG-associated reduced FD4 uptake was reversed by the VPAC1 antagonist PG97-269 or L-NAME, not by EGF or IGF1 receptor inhibitors.
Conclusions
Systemic LPS releases endogenous GLP-2, reducing LPS-related increased permeability. The therapeutic window of exogenous GLP-2 administration is at minimum within 6–12 h after LPS treatment. Exogenous GLP-2 treatment is of value in the prevention of increased paracellular permeability associated with endotoxemia.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Lipopolysaccharide (LPS, endotoxin) is a lipophilic pathogenic factor derived from gut Gram-negative bacteria. Translocation of LPS or Gram-negative bacteria across the gut causes endotoxemia, associated with sepsis and severe acute illness, which triggers systemic inflammation. Systemic inflammation also increases intestinal paracellular permeability, associated with endotoxemia, further increasing systemic inflammation. Severe systemic inflammation associated with acute pancreatitis, fulminant hepatitis, burns, trauma, and severe infections is often complicated by endotoxemia [1]. Increased entry of LPS from the intestinal lumen enhances multiple organ injury. Chemically induced dextran sulfate sodium (DSS) colitis increases portal vein LPS levels, increasing liver injury [2]. Reduction of intestinal luminal LPS by antibiotics reduces ischemia-induced lung injury [3]. Therefore, therapeutics that decreases “secondary” endotoxemia that is aimed at reducing intestinal LPS transport may prevent the morbid complications of critical illness [4].
Glucagon-like peptide-2 (GLP-2) is an intestinotrophic hormone released from enteroendocrine L cells [5]. Chronic treatment with GLP-2 (twice a day for 14 days) prevents LPS translocation into the circulation [6], attributed to its pro-proliferative effects with increased expression of tight junction proteins. The intestinotrophic effects of GLP-2 are mediated by the release of growth factors, insulin-like growth factor-1 (IGF1), or epidermal growth factor (EGF) [7, 8], mostly from the peri-epithelial mesenchymal syncytium that expresses GLP-2 receptors (GLP2Rs) [9, 10]. Furthermore, GLP2Rs are also expressed on the enteric neurons of the myenteric and submucosal plexuses that express nitric oxide synthase (NOS) and vasoactive intestinal peptide (VIP) [11], suggesting that GLP-2 acutely affects mucosal responses via NO and VIP release. NO and VIP increase mucosal blood flow, increase epithelial anion secretion, and reduce gut paracellular permeability [12,13,14,15,16,17]. Therefore, we hypothesized that GLP-2 acutely affects small intestinal paracellular permeability following the induction of systemic inflammation via NO and VIP pathways, rather than via the growth factor pathway.
Systemic LPS treatment releases GLP-1 from enteroendocrine L cells directly or indirectly. In mice, a single dose of LPS time-dependently increased serum GLP-1 levels at ~ 2 h accompanied by hyperinsulinemia and hypoglycemia in an interleukin (IL)-6-dependent manner [18]. Another group also reported that a single ip LPS injection increased plasma GLP-1 levels at 6 h in mice [19]. Plasma GLP-1 levels are higher in critically ill patients in an intensive care unit (ICU) compared with healthy control subjects and higher in sepsis patients in an ICU cohort than in non-septic patients [18]. LPS directly stimulates GLP-1 release from L cells via Toll-like receptor-4 (TLR4) activation at 3 h in mice and at 1–24 h in the L cell model cell lines, GLUTag cells, and secretin tumor cell (STC)-1 cells [20]. Since equimolar amounts of GLP-1 and GLP-2 are released from stimulated L cells [21], LPS treatment may increase endogenous release of GLP-2 from L cells as well. Therefore, we also hypothesized that endogenous GLP-2 alters small intestinal paracellular permeability under systemic inflammation.
Here, we examined the effects of endogenous and exogenous GLP-2 on increased small intestinal paracellular permeability induced by systemic LPS treatment as a simple and reproducible model of acute inflammation [22, 23]. We used fluorescein isothiocyanate (FITC)-conjugated dextran 4 kDa (FD4) as a model paracellular permeability marker [24] measuring FD4 appearance in the portal vein (PV) in rats in vivo in order to assess the dynamics of FD4 movement across the small intestinal mucosa after LPS treatment. We further examined the effects of a stable GLP-2 analog teduglutide (TDG) on FD4 permeability during LPS-induced systemic inflammation.
Materials and Methods
Animals
Male Sprague–Dawley rats weighing 200–250 g (Harlan, San Diego, CA, USA) were fed a pellet diet and water ad libitum. All studies were performed with approval of the Veterans Affairs Institutional Animal Care and Use Committee. Some rats were fasted overnight with free access to water before the experiments, but some were fed ad libitum. Animals were euthanized by terminal exsanguination under deep isoflurane anesthesia, followed by thoracotomy.
Chemicals
Teduglutide (TDG, Shire Pharmaceuticals USA, Lexington, MA, USA) was provided by the Pharmacy Service of the West Los Angeles Veterans Affairs Medical Center. Rat GLP-2, NVP-728, NVP-AEW-541 (AEW541), and PD153035 were obtained from Tocris Bioscience (Ellisville, MO, USA). Rat GLP-2(3-33) was synthesized by Bachem Americas, Inc. (Torrance, CA). The VIP/pituitary adenylate cyclase-activating peptide (PACAP) receptor 1 (VPAC1) antagonist PG97-269, [Ac-His1, D-Phe2, Lys15, Arg16, Leu27]-VIP(1-7)-GRF(8-27) [25], was synthesized using solid-phase methodology according to the Fmoc strategy using an automated peptide synthesizer (Model Pioneer, Thermo Fisher Scientific, Waltham, MA, USA). The crude peptide was purified using reverse-phase high-performance liquid chromatography (HPLC, Delta 600 HPLC System, Waters, MA, USA) on a column of Develosil ODS-HG-5 (2 × 25 cm, Nomura Chemical Co., Ltd, Seto, Japan). The purity of each peptide was confirmed by analytical HPLC and matrix-assisted laser desorption/ionization time of flight and mass spectrometry (MALDI-TOF MS) analysis. FD4, LPS (from E. coli O55:B5), Nω-nitro-l-arginine methyl ester (L-NAME), and other chemicals were purchased from Sigma Chemical (St. Louis, MO, USA). NVP-AEW-541 and PD153035 were dissolved in dimethyl sulfoxide (DMSO) for stock solution. All other chemicals were dissolved in distilled water in order to prepare a stock solution.
LPS Treatment
Animals were treated with LPS (5 mg/kg, ip) once at 9 am. For the acute experiments, the animals were fasted overnight and were treated with LPS 1, 3, or 6 h before the anesthesia for small intestinal perfusion of FD4 as described below. For the 24-h experiments, the animals fed ad libitum were treated with LPS 24 h before anesthesia induction used for the perfusion study. As a control, saline was injected ip at the corresponding time before the experiments. The animal groups were expressed as control, LPS 1 h, LPS 3 h, LPS 6 h, and LPS 24 h.
Small Intestinal Perfusion
The small intestinal perfusion from the duodenum and portal vein (PV) cannulation were prepared by the modified methods as previously reported [26, 27]. Under isoflurane anesthesia (2%), the animal was placed spine on a recirculating heating block system (Summit Medical Systems, Bend, OR, USA) in order to maintain body temperature at 36–37 °C. Prewarmed saline was infused via the right femoral vein at 1.08 ml/h using a Harvard infusion pump (Harvard Apparatus, Holliston, MA, USA). The abdomen was incised, and the PV was cannulated with a polyethylene (PE)-50 tube attached with 23G needle and fixed by methacrylate adhesive at the insertion site. The tube was filled with heparinized saline enabling repeated blood sampling. Samples of 0.2 ml PV blood were collected every 15 min, followed by flushing with 0.2 ml heparinized saline. A polyethylene tube (diameter 5 mm) filled with PBS was inserted through the forestomach and tied at 0.5 cm caudal from the pyloric ring. After bolus perfusion of 2-ml phosphate buffer saline (PBS, 10 mM, pH 7.4) into the duodenum from the tube, followed by stabilization for ~ 30 min, the time was set as t = 0. FD4 (0.1 mM) in 10-ml PBS was slowly perfused at t = 0 min for 30 s. Blood samples were collected into 0.5-ml tubes containing 1 µl each of EDTA (0.5 M) and the dipeptidyl peptidase-4 (DPP4) inhibitor NVP-728 (1 mM) and immediately centrifuged at 5000×g for 5 min, after which the plasma was stored on ice or at − 80 °C until use. At 90 min, after collection of PV samples, arterial blood was taken from abdominal aorta, followed by euthanasia by thoracotomy.
Appearance of FD4 into the PV and arterial plasma was assessed by fluorescence intensity measurement using a multi-mode microplate reader (Synergy-2, BioTek Instruments, Inc., Winooski, VT, USA). Fluorescence intensity in t = 0 sample as background was subtracted from the fluorescence values measured in other time point samples. FD4 content was calculated according to the standard curve generated each time of measurement.
Drug Treatment for the Intestinal Perfusion Study
The following drugs were administered at the time after LPS treatment: The GLP2R partial agonist/antagonist GLP-2(3-33) (1 mg/kg; 280 nmol/kg, ip) [21, 28] was given immediately after LPS treatment (0 h after LPS treatment); GLP-2 (380 µg/kg; 100 nmol/kg, ip) was given 6 h after LPS treatment; a stable GLP-2 analog TDG (50 µg/kg; 13.3 nmol/kg) [29] was ip injected 0, 3, 6, or 12 h after LPS treatment or iv injected at t = 0 min just before the perfusion of FD4 solution (6 or 24 h after LPS treatment). In acute experiments, TDG was iv injected at t = 0 min (6 h after LPS treatment) with or without the pretreatment of the selective IGF1 receptor (IGF1R) tyrosine kinase inhibitor AEW541 (0.1 mg/kg, iv) [30], the selective EGF receptor (EGFR) tyrosine kinase inhibitor PD153035 (10 µg/kg, iv) [31] or PG97-269 (1 mg/kg, iv) at = − 10 min, or the co-perfusion of L-NAME (0.1 mM, pf) with FD4 solution.
GLP-2 Measurement in PV Plasma
GLP-2 content in PV plasma at t = 0 min of control (overnight fasted), control (fed ad libitum), and LPS 6 h or LPS 24 h group was measured using a GLP-2 ELISA kit (Phoenix Pharmaceuticals, Burlingame, CA) according to the manufacturer’s protocol.
Real-Time PCR
The mid-ileum (10–15 cm proximal from ileocecal junction) was removed from the animals of overnight fasted control and LPS 6 h groups and kept in a RNA stabilization solution (RNAlater, Qiagen, Valencia, CA, USA) at 4 °C until use. The ileal mucosa was separated from muscle layers using sharp dissection under a stereomicroscope. RT-PCR was performed as previously described [27] with primers for rat proglucagon (Gcg), GLP2R, cyclooxygenase-2 (COX2), tumor necrosis factor-α (TNF-α), interleukin 6 (IL-6), EGF, IGF1, IGF1R, and IGF2R and for β-actin as internal control. The expression level was presented as fold induction per 103 copies of β-actin by ΔCt method.
Immunofluorescence Staining
Small pieces of intestine were immersed in Zamboni’s fixative containing 2% paraformaldehyde and 0.2% picric acid in 0.1 M phosphate buffer (pH 7.4) overnight for 4 °C. The fixed tissues were then submerged in 20% sucrose in PBS (pH 7.4) overnight at 4 °C and embedded in optimum cutting temperature compound. Frozen sections of 8-μm thickness were cut and placed on aminosilane-coated glass slides (Matsunami Glass USA Inc., Bellingham, WA, USA). Sections were pretreated with 5% normal donkey serum in PBS, followed by incubation with primary antibodies: goat anti-GLP2R (Santa Cruz Biotechnology Inc., Santa Cruz, CA, USA), rabbit anti-VIP (RayBiotech, Inc., Peachtree Corners, GA, USA), or mouse anti-neuronal NOS (nNOS, Santa Cruz) overnight at 4 °C. After rinsing in PBS, fluorescence-conjugated secondary antibodies (Molecular Probes, Eugene, OR) were reacted for 2 h at room temperature. The sections were counterstained with 4’,6-diamidino-2-phenylindole (DAPI) and covered with the mounting medium (Invitrogen, Carlsbad, CA). Immunofluorescence was imaged and captured using a confocal laser microscope (LSM710; Carl Zeiss GmbH, Jena, Germany).
Statistics
Values are expressed as mean ± SEM. The number of animals in each experimental group was n = 6. Statistical analysis was performed using GraphPad® Prism 6 (La Jolla, CA, USA) using one-way ANOVA or two-way ANOVA followed by Dunnett’s test or Tukey’s multiple comparisons. Unpaired Student’s t test was also used for two-group comparison. Differences were considered significant when P values were < 0.05.
Results
Small Intestinal FD4 Permeability After LPS Treatment
First, we measured time-dependent changes in small intestinal FD4 permeability from the lumen to the PV after LPS treatment (5 mg/kg, ip), reflecting intestinal paracellular permeability. There was no change in FD4 appearance into the PV in the control group. Compared with the control group, LPS treatment had no effect on PV FD4 levels 1 or 3 h after LPS treatment, whereas PV FD4 levels were increased 6 h after LPS treatment (Fig. 1a). Arterial FD4 levels at t = 90 min (the end of experiments) also mirrored PV FD4 levels (Fig. 1b). Therefore, we used the LPS 6 h model (6 h after LPS treatment) to study the effects of acute drug treatment in the following experiments.
Effect of LPS treatment on small intestinal paracellular permeability (6 h study). FITC-dextran 4 kDa (FD4) solution (0.1 ml, 10 ml) was intraduodenally perfused at t = 0 min under anesthesia in rats of 1, 3, or 6 h after LPS treatment (5 mg/kg, ip), or 6 h after saline treatment (control). a FD4 concentration in portal venous (PV) plasma (PV FD4) collected every 15 min. Background fluorescent intensity at t = 0 was subtracted from the value at each time point, and calculated FD4 concentration is expressed as PV FD4 (nM) (mean ± SEM, n = 6). *p < 0.05 versus control group, †p < 0.05 versus LPS 1 h group, ‡p < 0.05 versus LPS 3 h group. b Arterial FD4 concentration at t = 90 min (mean ± SEM, n = 6). *p < 0.05 versus control, †p < 0.05 versus LPS 1 h, ‡p < 0.05 versus LPS 3 h
To test our hypothesis that endogenous GLP-2 is involved in LPS-induced increased intestinal paracellular permeability, the animals were treated with the GLP2R antagonist, GLP-2(3–33) (1 mg/kg, ip) immediately after LPS ip injection. PV FD4 levels were increased at t = 30 min, sustained to t = 90 min in the LPS 6 h group (Fig. 2a), accompanied by increased arterial FD4 levels at t = 90 min at the end of the experiments (Fig. 2b), the latter possibly reflecting the accumulated FD4 transported from the small intestinal lumen. GLP-2(3–33) treatment further increased PV FD4 levels at t = 60–90 min (Fig. 2a) and arterial FD4 levels at t = 90 min (Fig. 2b), suggesting that endogenous GLP-2 released in response to LPS treatment reduces intestinal paracellular permeability and FD4 transport.
Effect of a GLP-2 receptor antagonist on LPS-induced increases in FD4 permeability. A GLP-2 receptor antagonist GLP-2(3–33) (1 mg/kg, ip) was given immediately (0 h) after LPS treatment. FD4 solution was perfused as indicated in Fig. 1. a PV FD4 concentration (mean ± SEM, n = 6). *p < 0.05 versus control group, †p < 0.05 versus LPS 6 h group. b Arterial FD4 concentration at t = 90 min (mean ± SEM, n = 6). *p < 0.05 versus control, †p < 0.05 versus LPS 6 h
Next, we examined FD4 permeability 24 h after LPS treatment (LPS 24 h group). PV FD4 levels were increased 24 h after LPS treatment (Fig. 3a) with increased arterial FD4 levels (Fig. 3b), higher than that in the LPS 6 h group (LPS 6 h 24.5 ± 2.5 vs. LPS 24 h 54.5 ± 16.0, p < 0.05 by unpaired Student’s t-test). Exogenous GLP-2 treatment given 6 h after LPS treatment (380 µg/kg, ip) reduced PV and arterial FD4 levels (Fig. 3a, b), suggesting that exogenous GLP-2 reduces LPS-induced intestinal paracellular permeability, even when given 6 h after LPS treatment.
FD4 permeability 24 h after LPS treatment; effect of GLP-2 treatment. LPS was injected (5 mg/kg, ip) 24 h before the experiments, and FD4 solution was perfused as indicated in Fig. 1. Rat GLP-2 (380 µg/kg, ip) was injected 6 h after LPS treatment. a PV FD4 concentration (mean ± SEM, n = 6). *p < 0.05 versus control group, †p < 0.05 versus LPS 24 h group. b Arterial FD4 concentration at t = 90 min (mean ± SEM, n = 6). *p < 0.05 versus control, †p < 0.05 versus LPS 24 h
To clarify whether arterial FD4 levels reflect accumulated FD4 absorbed from the intestinal lumen to the PV, area under the curve (AUC) of PV FD4 levels during the 90-min period (µM min) from Figs. 1, 2, and 3 was plotted against arterial FD4 levels at t = 90 min (Fig. 4). Our analysis demonstrated that PV FD4 AUC and arterial FD4 levels were well correlated (r2 = 0.7113), suggesting that arterial FD4 levels reflect the total transported FD4 amount into the PV.
Correlation between FD4 transported into the PV and arterial FD4 concentration. Area under the curve (AUC) of PV FD4 concentration (µM min) (PV FD4 AUC) calculated by the trapezoidal rule, and arterial FD4 concentration (nM) at t = 90 min (arterial FD4) from the data in Figs. 1, 2, and 3 was plotted. Linear regression was calculated by GraphPad® Prism 6 statistics software
To confirm the involvement of endogenous GLP-2 during LPS-induced increased intestinal paracellular permeability, we measured PV GLP-2 levels of the animals 6 and 24 h after LPS treatment. Compared with the corresponding control conditions (overnight fasted or fed ad libitum), LPS treatment increased PV GLP-2 levels 6 h and 24 h after LPS treatment (Fig. 5a, b), suggesting that LPS directly or indirectly stimulates GLP-2 release from L cells of the intestine.
Effect of LPS treatment on PV GLP-2 levels. a Plasma GLP-2 content was measured in the PV blood in overnight fasted control and 6 h after LPS treatment (LPS 6 h). Each column is expressed as mean ± SEM (n = 6). *p < 0.05 versus control (fasted). b Plasma GLP-2 content was measured in the PV blood in fed ad libitum control and 24 h after LPS treatment (LPS 24 h). Each column is expressed as mean ± SEM (n = 6). *p < 0.05 versus control (fed)
We also measured mRNA expression levels of proglucagon (Gcg) and proinflammatory mediators in the ileal mucosa by real-time PCR. Compared with the control group, expression of Gcg was increased in the ileal mucosa of the group treated with LPS at 6 h (Fig. 6a), suggesting that LPS directly or indirectly upregulates Gcg expression in the ileal L cells, presumably to restore and further release GLP-2 and other proglucagon products. Expression of COX-2 and the proinflammatory cytokines TNF-α and IL-6 in the ileum was also upregulated by LPS treatment (Fig. 6c–e). Furthermore, the expression of the growth factors EGF, IGF1, and IGFR1 that are believed to be downstream of GLP-2 receptor activation [7, 8] (Fig. 6f–h), but not GLP2R (Fig. 6b) or IGFR2 (Fig. 6i), was also upregulated, suggesting that GLP2R activation during LPS-induced inflammation upregulates its downstream signals.
Effect of LPS treatment on expressions of GLP-2-related proteins and proinflammatory mediators. mRNA expressions in the ileal mucosa of overnight fasted control and 6 h after LPS treatment (LPS 6 h group) were assessed by real-time PCR using β-actin as internal control with ΔCT method. Each column is expressed as mean ± SEM (n = 6). *p < 0.05 versus control (fasted). a Proglucagon (Gcg), b GLP-2 receptor (GLP2R), c cyclooxygenase-2 (COX2), d tumor necrosis factor-α (TNF-α), e interleukin-6 (IL-6), f epidermal growth factor (EGF), g insulin-like growth factor 1 (IGF1), h IGF1 receptor (IGF1R), i IGF2R
Effects of Teduglutide (TDG) Treatment on LPS-Induced Intestinal FD4 Permeability
Next, we examined the effects of TDG treatment on FD4 permeability in LPS 6 h model. TDG (50 µg/kg) was given 3 h after LPS treatment (ip) or 6 h after LPS treatment (iv at t = 0 min), after which PV FD4 levels were measured 6 h after LPS treatment. Compared with the non-treated LPS 6 h group, TDG treatment at 3 h (ip) or 6 h (iv) after LPS treatment reduced PV FD4 levels (Fig. 7a), suggesting that TDG acutely improves LPS-induced increased intestinal FD4 permeability.
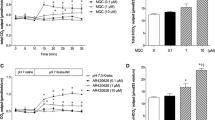
Effect of teduglutide on LPS-induced small intestinal FD4 permeability (6 h model). LPS was given 6 h before the experiments. Teduglutide (TDG, 50 µg/kg) was injected 3 h (ip) or 6 h (iv at t = 0 min) after LPS treatment. The FD4 solution was perfused as indicated in Fig. 1. Test drugs were iv injected at t = − 10 min, or co-perfused (pf) with FD4 solution. a PV FD4 concentration (mean ± SEM, n = 6) of control, LPS 6 h, LPS 6 h + TDG 3 h, and LPS 6 h + TDG 6 h group. *p < 0.05 versus control group, †p < 0.05 versus LPS 6 h group. b Effect of IGF1R inhibitor NVP-AEW541 (AEW541) (0.1 mg/kg, iv) on the inhibitory effect of TDG on LPS-induced PV FD4 increase (mean ± SEM, n = 6). *p < 0.05 versus LPS 6 h. c Effect of EGF receptor inhibitor PD153035 (10 µg/kg, iv) on the inhibitory effect of TDG on LPS-induced PV FD4 increase (mean ± SEM, n = 6). *p < 0.05 versus LPS 6 h. d Effect of VPAC1 antagonist PG97-269 (1 mg/kg, iv) on the inhibitory effect of TDG on LPS-induced PV FD4 increase (mean ± SEM, n = 6). *p < 0.05 versus LPS 6 h, †p < 0.05 versus LPS 6 h + TDG 6 h. e Effect of NO synthase inhibitor L-NAME (0.1 mM, pf) on the inhibitory effect of TDG on LPS-induced PV FD4 increase (mean ± SEM, n = 6). *p < 0.05 versus LPS 6 h, †p < 0.05 versus LPS 6 h + TDG 6 h. f Arterial FD4 concentration at t = 90 min (mean ± SEM, n = 6). *p < 0.05 versus control, †p < 0.05 versus LPS 6 h. ‡p < 0.05 versus LPS 6 h + TDG 6 h. g Effect of L-NAME (0.1 mM, pf) on LPS-induced PV FD4 increase (mean ± SEM, n = 6). *p < 0.05 versus LPS 6 h
Furthermore, using the LPS 6 h model treated with TDG 6 h after LPS treatment, we assessed the downstream mediators involved in the inhibitory effect of TDG on FD4 permeability. Pretreatment with the selective IGF1R tyrosine kinase inhibitor AEW541 (0.1 mg/kg, iv) (Fig. 7b) or EGFR tyrosine kinase inhibitor PD153035 (10 µg/kg, iv) (Fig. 7c) had no effect on TDG-induced inhibitory effect on PV FD4 levels, whereas the selective VPAC1 antagonist PG97-269 (1 mg/kg, iv) (Fig. 7d) and an NOS inhibitor L-NAME (0.1 mM, pf) (Fig. 7e) reversed the TDG effect on PV FD4 levels. Arterial FD4 levels were reduced by PG97-269 and L-NAME, but were not affected by AEW541 or PD153035 (Fig. 7f), in agreement with the TDG-induced inhibitory effect on LPS-augmented PV FD4 levels. These results suggest that acute TDG effects on LPS-induced FD4 permeability are mediated by VIP and NO, but not by the growth factors IGF1 or EGF. Since NO derived from inducible NOS (iNOS) contributes to the LPS-induced intestinal permeability increase [32, 33], we also examined the effect of L-NAME alone on LPS-induced FD4 permeability. Luminal co-perfusion of L-NAME with FD4 had no effect on LPS-induced increases in PV FD4 levels at 6 h (Fig. 7g), suggesting that luminal application of L-NAME may not affect iNOS activity in the small intestinal tissues or acute inhibition of iNOS may not reverse LPS-induced FD4 permeability.
We also tested the effects of TDG on FD4 permeability in an LPS 24 h model. The increased PV FD4 levels 24 h after LPS treatment (LPS 24 h group) were reduced by TDG treatment 6 and 12 h after LPS treatment (LPS 24 h + TDG 6 h group and + TDG 12 h group), whereas TDG treatment immediately after LPS treatment (LPS 24 h + TDG 0 h group) or 24 h after LPS treatment (LPS 24 h + TDG 24 h group) had little effect on the increased PV FD4 levels (Fig. 8a), suggesting that TDG given immediately or 24 h after LPS treatment is ineffective, whereas TDG given at 6–12 h after LPS treatment is effective in reducing inflammation-increased paracellular permeability. Increased arterial FD4 levels in the LPS 24 h group were inhibited by TDG treatment 6 h and 12 h after LPS treatment (LPS 24 h + TDG 6 h, and + TDG 12 h), whereas TDG treatment 0 or 24 h after LPS treatment (LPS 24 h + TDG 0 h, or + TDG 24 h) had no significant effect (Fig. 8b), mirrored by PV FD4 levels. These results suggest that the therapeutic window of TDG treatment is at minimum 6–12 h after LPS treatment.
Effect of teduglutide on LPS-induced small intestinal FD4 permeability (24 h model). LPS was given 24 h before the experiments. TDG (50 µg/kg) was injected 0, 6, 12 h (ip), or 24 h (iv at t = 0 min) after LPS treatment. The FD4 solution was perfused as indicated in Fig. 1. a PV FD4 concentration (mean ± SEM, n = 6). *p < 0.05 versus control group, †p < 0.05 versus LPS 24 h group. B: Arterial FD4 concentration at t = 90 min (mean ± SEM, n = 6). *p < 0.05 versus control, †p < 0.05 versus LPS 24 h
Colocalization of GLP2R with VIP and nNOS in the Myenteric Plexus
Immunostaining revealed that GLP2R was colocalized with nNOS (Fig. 9a–c) and VIP (Fig. 9d–f) in the myenteric plexus neurons and intramuscular nerve fibers in rat duodenum. We also confirmed colocalization of nNOS and VIP in the myenteric neurons and nerve fibers (Fig. 9g–i). These results suggest that downstream of GLP2R activation involves VIP and NO release, consistent with a prior report [11].
Colocalization of the GLP-2 receptor with nNOS and VIP in the enteric neurons in rat duodenum. Cryostat sections of rat duodenum were immunostained with primary antibodies for GLP-2 receptor (a, d green), nNOS (b, red; g, green), and VIP (e, h red). c, f, i: merged images. Internal bar = 50 µm. Nuclei were counterstained with DAPI (blue)
Discussion
We examined the dynamics of small intestinal FD4 permeability into the PV after systemic LPS treatment in vivo in order to test whether endogenous or exogenous GLP-2 acutely improves LPS-induced FD4 permeability and to ascertain optimal timing of treatment. We demonstrated that PV FD4 levels increased 30–90 min after FD4 perfusion into the small intestinal lumen 6 h after LPS treatment and further increased 24 h after LPS treatment and that endogenous GLP-2 release was involved in LPS-induced increased FD4 permeability at least 6 h after LPS treatment, whereas exogenous GLP-2 or the stable GLP-2 analog TDG reduced LPS-induced FD4 permeability when given 3 and 6 h after LPS treatment when FD4 uptake was measured 6 h after LPS injection and 6–12 h after LPS treatment when FD4 uptake was measured 24 h after LPS injection. We also confirmed that total FD4 movement into the PV is closely related to arterial FD4 levels 90 min after FD4 perfusion. This is the first study showing that parenteral LPS treatment acutely releases GLP-2, which defends against LPS-induced increased small intestinal paracellular permeability via the NO and VIP pathways (Fig. 10).
Proposed mechanisms by which endogenous or exogenous GLP-2 prevents LPS-induced small intestinal paracellular permeability increase. Systemic administration of LPS induces small intestinal inflammation via stimulation of resident immune cells such as macrophages (Mϕ) through Toll-like receptor 4 (TLR4) activation, which produce proinflammatory cytokines such as tumor necrosis factor-α (TNF-α), interleukin-6 (IL-6), that injure epithelial cells, in turn increasing paracellular permeability to the solute FITC-dextran 4000 (FD4), increasing transmucosal uptake of luminal LPS, the latter which may worsen LPS-related inflammation. LPS releases GLP-2 from L cells directly or indirectly via cytokine generation, which prevents the increase in paracellular permeability observed at early time points following LPS treatment. Exogenous GLP-2 or the stable GLP-2 analog teduglutide (TDG) prevents LPS from increasing paracellular permeability when given 3 and 6 h after LPS injection when FD4 is measured 6 h after LPS administration or 6–12 h after LPS injection when FD4 is measured 24 h after LPS administration. The effects of GLP-2 on the LPS-induced paracellular permeability increase are mediated by vasoactive intestinal peptide (VIP) release and nitric oxide (NO) production from the myenteric nerves expressing GLP-2 receptors (GLP2R)
There are several reasons why we perfused the FD4 solution intraduodenally and measured FD4 levels in the PV, rather than gavaged FD4 into conscious animals, followed by blood collection at one time point in order to assess FD4 permeability. One is that FD4 distribution into the small intestinal lumen following gavage of FD4 into the stomach is affected by gastric emptying and small intestinal motility, that are prolonged during endotoxemia due to gastroparesis and paralytic ileus, potentially confounding the measurements [34]. Another is that the dynamics of PV FD4 levels is the most direct measurement of FD4 transport from the small intestinal lumen to the blood stream. Last is that GLP-2 treatment may affect FD4 movement through the stomach and small intestine, since GLP-2 relaxes gastric smooth muscle in mice and reduces antral motility in pigs [35, 36], although GLP-2 or TDG has lesser or no effect on gastric emptying in humans [37, 38]. Therefore, we believe that our method provides the most accurate quantification available of small intestinal paracellular permeability of FD4 during LPS-induced systemic inflammation.
We found that FD4 permeability was increased 6 h, but not 1 or 3 h after LPS injection. A detailed histological study of mouse small intestine demonstrated that LPS injection (10 mg/kg) increased fluid exudation and villous shortening 1.5 h after injection with increased apoptosis and cell shedding via TLR4- and TNF receptor 1-dependent mechanisms, followed by plasma FD4 increase at 5 h, not at 1.5 or 3 h after injection [22], consistent with our results. We also observed the upregulation of TNF-α in the ileal mucosa 6 h after LPS treatment. These observations suggest that LPS-induced induction and release of TNF-α damage villous cells with resultant epithelial gap formation and increased FD4 permeability. Upregulation of growth factors that are downstream of GLP2R activation such as EGF, IGF1, and IGF1R in the ileal mucosa of the LPS 6 h group also suggests that endogenous GLP-2/GLP2R signaling is involved in rapid mucosal repair from LPS-induced inflammation. Since LPS treatment rapidly induces villous and crypt cell apoptosis and epithelial cell shedding, followed by the increased FD4 permeability from the small intestine in mice [22], activation of the GLP2R–growth factor signal may contribute to rapid restitution of the intestinal epithelium. Interestingly, LPS-induced increased FD4 permeability at 6 h was reversible. TDG treatment 3 and 6 h after LPS treatment inhibited FD4 movement into the PV, suggesting that TDG acutely reverses LPS-induced FD4 permeability. GLP-2 increases release of the growth factors IGF1 and EGF. EGF, but not IGF1, promotes restitution of damaged epithelial cells within 3 h [39]. IGF1 stimulates crypt expansion by increasing the rate of proliferation and promotes epithelial repair from enteritis in 5 days [40]. Therefore, IGF1 or EGF may be involved in the acute inhibitory effects of TDG on FD4 permeability. Nevertheless, inhibition of IGF1 or EGF tyrosine kinase failed to affect, whereas L-NAME and PG97-269 reversed the effects TDG on permeability, suggesting that the acute inhibitory effects of TDG on LPS-induced FD4 permeability are mediated by NO and VIP pathways, and not by growth factor pathways.
VIP modulates epithelial paracellular permeability via regulation of the expression and function of epithelial tight junction proteins. VIPergic pathways increase the expression of the tight junction protein zonula occludens-1 (ZO-1) peaking at 15 h in human polarized colonic epithelial monolayers co-cultured with human submucosa containing the submucosal plexus, associated with reduced epithelial paracellular permeability [16]. VIP likely reduces FD4 flux through the epithelial monolayer in 30 min [16], suggesting that VIP rapidly regulates FD4 permeability without altering the expression of tight junctional proteins. Daily treatment with exogenous VIP also ameliorates bacterial infection-induced intestinal barrier disruption by preventing the translocation of the tight junction proteins ZO-1, occludin, and claudin-3 10 days post-infection in a Citrobacter rodentium-induced colitis model [41]. Mucosal inflammation increases epithelial paracellular permeability primarily due to the disruption of the epithelial tight junction complex by TNF-α and interferon (IFN)-γ derived from activated macrophages and T cells [42]. VIP and PACAP equally reduce TNF-α release from activated macrophages induced by LPS [43], suggesting that VIP–VPAC signaling modifies epithelial paracellular permeability changes during intestinal inflammation via inhibition of inflammatory cytokine release. Nevertheless, these studies addressed the relatively long-term effect of VIP signals rather than acute effect of VIP-VPAC signaling, which we observed as the inhibitory effects of TDG on LPS-induced FD4 permeability that was acutely reversed by VPAC1 antagonism. The acute effect of VIP on FD4 permeability through the compromised small intestinal mucosa remains to be clarified.
NO is involved in the increase of intestinal paracellular permeability that occurs in inflammation. Excessive NO production derived from iNOS contributes to the increase of paracellular permeability 24 h after LPS treatment (5 mg/kg) in rats, as assessed by the three doses of iNOS inhibitor 2, 6, and 8 h after LPS treatment [32]. Increased FD4 flux through everted ileal sacs of LPS-treated mice at 12 h with reduced ZO-1 expression was inhibited by the iNOS inhibition and in iNOS knockout mice, whereas iNOS gene ablation likely increases FD4 flux and reduces ZO-1 expression without LPS treatment [33], suggesting the involvement of compensatory mechanisms in iNOS knockout mice. In contrast, we observed that luminal co-perfusion of L-NAME acutely blunted the inhibitory effect of TDG on LPS-induced increased FD4 permeability at 6 h, suggesting that NO derived from enteric nNOS by TDG treatment reduces LPS-augmented FD4 permeability, independently of iNOS-derived NO. Furthermore, luminal perfusion of L-NAME had no effect on the LPS-induced FD4 permeability increase, suggesting that the effect of L-NAME on the reversal of permeability due to TDG effect results from the inhibition of enteric nNOS rather than inhibition of iNOS. Direct and dose-dependent effects of NO on epithelial paracellular permeability remain to be determined.
The LPS 24 h model provides a clinical correlate for the therapeutic potency of TDG. Our results showed that TDG treatment inhibited LPS-induced increased FD4 permeability at 6 and 12 h, but not 0 or 24 h after LPS treatment, suggesting that the reversal of LPS-induced small intestinal paracellular permeability by TDG occurs within or somewhat outside of a 6–12-h timeframe after LPS treatment. Since the serum t1/2 of TDG is ~ 2 h [44], much longer than the ~ 7 min t1/2 of exogenous GLP-2 [45], the acute effect of TDG as observed in the LPS 6 h model may contribute to the TDG-related reversal of LPS-mediated increased intestinal permeability. These data imply that TDG may be beneficial only when administered early in the course of severe inflammatory diseases such as acute pancreatitis, fulminant hepatitis, burns, and other diseases complicated by the systemic inflammatory response syndrome (SIRS), assuming that increased intestinal paracellular permeability is related to the pathogenesis of SIRS, and not merely an inflammatory biomarker [46].
In conclusion, systemic treatment with LPS releases endogenous GLP-2, which acutely preserves LPS-induced FD4 permeability in the small intestine associated with increased Gcg expression and increased GLP-2 release. Furthermore, TDG inhibits LPS-induced FD4 permeability acutely via NO and VIP-VPAC1 pathways rather than via growth factor pathways. TDG treatment may prevent the progression of intestinal barrier disruption during endotoxemia, if given at the optimal time point after the induction of systemic inflammation. Exogenous GLP-2 treatment is of value in the prevention of the paracellular permeability increase associated with endotoxemia.
Abbreviations
- DPP4:
-
Dipeptidyl peptidase-4
- GLP-2:
-
Glucagon-like peptide-2
- GLP2R:
-
GLP-2 receptor
- LPS:
-
Lipopolysaccharide
- GPCR:
-
G protein-coupled receptor
- PV:
-
Portal vein
- IGF-1:
-
Insulin-like growth factor-1
- EGF:
-
Epidermal growth factor
- NO:
-
Nitric oxide
- NOS:
-
NO synthase
- VIP:
-
Vasoactive intestinal peptide
- L-NAME:
-
Nω-nitro-l-arginine methyl ester
- PACAP:
-
Pituitary adenylate cyclase-activating peptide
- TDG:
-
Teduglutide
- VPAC1:
-
VIP/PACAP receptor-1
References
Ammori BJ, Leeder PC, King RF, et al. Early increase in intestinal permeability in patients with severe acute pancreatitis: correlation with endotoxemia, organ failure, and mortality. J Gastrointest Surg. 1999;3:252–262.
Gäbele E, Dostert K, Hofmann C, et al. DSS induced colitis increases portal LPS levels and enhances hepatic inflammation and fibrogenesis in experimental NASH. J Hepatol. 2011;55:1391–1399.
Sorkine P, Szold O, Halpern P, et al. Gut decontamination reduces bowel ischemia-induced lung injury in rats. Chest. 1997;112:491–495.
Cohen J, Vincent JL, Adhikari NK, et al. Sepsis: a roadmap for future research. Lancet Infect Dis. 2015;15:581–614.
Drucker DJ, Erlich P, Asa SL, Brubaker PL. Induction of intestinal epithelial proliferation by glucagon-like peptide 2. Proc Natl Acad Sci U S A. 1996;93:7911–7916.
Cani PD, Possemiers S, Van de WT, et al. Changes in gut microbiota control inflammation in obese mice through a mechanism involving GLP-2-driven improvement of gut permeability. Gut. 2009;58:1091–1103.
Rowland KJ, Trivedi S, Lee D, et al. Loss of glucagon-like peptide-2-induced proliferation following intestinal epithelial insulin-like growth factor-1-receptor deletion. Gastroenterology. 2011;141:2166–2175.
Bahrami J, Yusta B, Drucker DJ. ErbB activity links the glucagon-like peptide-2 receptor to refeeding-induced adaptation in the murine small bowel. Gastroenterology. 2010;138:2447–2456.
Orskov C, Hartmann B, Poulsen SS, Thulesen J, Hare KJ, Holst JJ. GLP-2 stimulates colonic growth via KGF, released by subepithelial myofibroblasts with GLP-2 receptors. Regul Pept. 2005;124:105–112.
Kaunitz JD, Akiba Y. Control of intestinal epithelial proliferation and differentiation: the microbiome, enteroendocrine L cells, telocytes, enteric nerves, and GLP, too. Dig Dis Sci. 2019;64:2709–2716. https://doi.org/10.1007/s10620-019-05778-1.
Guan X, Karpen HE, Stephens J, et al. GLP-2 receptor localizes to enteric neurons and endocrine cells expressing vasoactive peptides and mediates increased blood flow. Gastroenterology. 2006;130:150–164.
Sugamoto S, Kawauch S, Furukawa O, Mimaki TH, Takeuchi K. Role of endogenous nitric oxide and prostaglandin in duodenal bicarbonate response induced by mucosal acidification in rats. Dig Dis Sci. 2001;46:1208–1216. https://doi.org/10.1023/A:1010603026913.
Eklund S, Jodal M, Lundgren O, Sjoqvist A. Effects of vasoactive intestinal polypeptide on blood flow, motility and fluid transport in the gastrointestinal tract of the cat. Acta Physiol Scand. 1979;105:461–468.
Yao B, Hogan DL, Bukhave K, Koss MA, Isenberg JI. Bicarbonate transport by rabbit duodenum in vitro: effect of vasoactive intestinal peptide, prostaglandin E2, and cyclic adenosine monophosphate. Gastroenterology. 1993;104:732–740.
Nylander O, Hällgren A, Holm L. Duodenal mucosal alkaline secretion, permeability, and blood flow. Am J Physiol. 1993;265:G1029–G1038.
Neunlist M, Toumi F, Oreschkova T, et al. Human ENS regulates the intestinal epithelial barrier permeability and a tight junction-associated protein ZO-1 via VIPergic pathways. Am J Physiol Gastrointest Liver Physiol. 2003;285:G1028–G1036.
Takeuchi K, Kagawa S, Mimaki H, Aoi M, Kawauchi S. COX and NOS isoforms involved in acid-induced duodenal bicarbonate secretion in rats. Dig Dis Sci. 2002;47:2116–2124. https://doi.org/10.1023/A:1019601702559.
Kahles F, Meyer C, Mollmann J, et al. GLP-1 secretion is increased by inflammatory stimuli in an IL-6-dependent manner, leading to hyperinsulinemia and blood glucose lowering. Diabetes. 2014;63:3221–3229.
Nguyen AT, Mandard S, Dray C, et al. Lipopolysaccharides-mediated increase in glucose-stimulated insulin secretion: involvement of the GLP-1 pathway. Diabetes. 2014;63:471–482.
Lebrun LJ, Lenaerts K, Kiers D, et al. Enteroendocrine L cells sense LPS after gut barrier injury to enhance GLP-1 secretion. Cell Rep. 2017;21:1160–1168.
Wang JH, Inoue T, Higashiyama M, et al. Umami receptor activation increases duodenal bicarbonate secretion via glucagon-like peptide-2 release in rats. J Pharmacol Exp Ther. 2011;339:464–473.
Williams JM, Duckworth CA, Watson AJ, et al. A mouse model of pathological small intestinal epithelial cell apoptosis and shedding induced by systemic administration of lipopolysaccharide. Dis Model Mech. 2013;6:1388–1399.
Yue C, Wang W, Tian WL, et al. Lipopolysaccharide-induced failure of the gut barrier is site-specific and inhibitable by growth hormone. Inflamm Res. 2013;62:407–415.
Volynets V, Reichold A, Bardos G, Rings A, Bleich A, Bischoff SC. Assessment of the intestinal barrier with five different permeability tests in healthy C57BL/6J and BALB/cJ mice. Dig Dis Sci. 2016;61:737–746. https://doi.org/10.1007/s10620-015-3935-y.
Gourlet P, Vandermeers A, Vertongen P, et al. Development of high affinity selective VIP1 receptor agonists. Peptides. 1997;18:1539–1545.
Mizumori M, Meyerowitz J, Takeuchi T, et al. Epithelial carbonic anhydrases facilitate PCO2 and pH regulation in rat duodenal mucosa. J Physiol. 2006;573:827–842.
Akiba Y, Inoue T, Kaji I, et al. Short-chain fatty acid sensing in rat duodenum. J Physiol. 2015;593:585–599.
Thulesen J, Knudsen LB, Hartmann B, et al. The truncated metabolite GLP-2 (3-33) interacts with the GLP-2 receptor as a partial agonist. Regul Pept. 2002;103:9–15.
Drucker DJ, DeForest L, Brubaker PL. Intestinal response to growth factors administered alone or in combination with human [Gly2]glucagon-like peptide 2. Am J Physiol. 1997;273:G1252–G1262.
García-Echeverría C, Pearson MA, Marti A, et al. In vivo antitumor activity of NVP-AEW541-A novel, potent, and selective inhibitor of the IGF-IR kinase. Cancer Cell. 2004;5:231–239.
Bos M, Mendelsohn J, Kim YM, Albanell J, Fry DW, Baselga J. PD153035, a tyrosine kinase inhibitor, prevents epidermal growth factor receptor activation and inhibits growth of cancer cells in a receptor number-dependent manner. Clin Cancer Res. 1997;3:2099–2106.
Unno N, Wang H, Menconi MJ, et al. Inhibition of inducible nitric oxide synthase ameliorates endotoxin-induced gut mucosal barrier dysfunction in rats. Gastroenterology. 1997;113:1246–1257.
Han X, Fink MP, Yang R, Delude RL. Increased iNOS activity is essential for intestinal epithelial tight junction dysfunction in endotoxemic mice. Shock. 2004;21:261–270.
Buchholz BM, Chanthaphavong RS, Bauer AJ. Nonhemopoietic cell TLR4 signaling is critical in causing early lipopolysaccharide-induced ileus. J Immunol. 2009;183:6744–6753.
Amato A, Baldassano S, Serio R, Mule F. Glucagon-like peptide-2 relaxes mouse stomach through vasoactive intestinal peptide release. Am J Physiol Gastrointest Liver Physiol. 2009;296:G678–G684.
Wøjdemann M, Wettergren A, Hartmann B, Holst JJ. Glucagon-like peptide-2 inhibits centrally induced antral motility in pigs. Scand J Gastroenterol. 1998;33:828–832.
Nagell CF, Wettergren A, Pedersen JF, Mortensen D, Holst JJ. Glucagon-like peptide-2 inhibits antral emptying in man, but is not as potent as glucagon-like peptide-1. Scand J Gastroenterol. 2004;39:353–358.
Berg JK, Kim EH, Li B, Joelsson B, Youssef NN. A randomized, double-blind, placebo-controlled, multiple-dose, parallel-group clinical trial to assess the effects of teduglutide on gastric emptying of liquids in healthy subjects. BMC Gastroenterol. 2014;14:25.
Riegler M, Sedivy R, Sogukoglu T, et al. Epidermal growth factor promotes rapid response to epithelial injury in rabbit duodenum in vitro. Gastroenterology. 1996;111:28–36.
Van Landeghem L, Santoro MA, Mah AT, et al. IGF1 stimulates crypt expansion via differential activation of 2 intestinal stem cell populations. FASEB J. 2015;29:2828–2842.
Conlin VS, Wu X, Nguyen C, et al. Vasoactive intestinal peptide ameliorates intestinal barrier disruption associated with Citrobacter rodentium-induced colitis. Am J Physiol Gastrointest Liver Physiol. 2009;297:G735–750.
Clayburgh DR, Barrett TA, Tang Y, et al. Epithelial myosin light chain kinase-dependent barrier dysfunction mediates T cell activation-induced diarrhea in vivo. J Clin Invest. 2005;115:2702–2715.
Delgado M, Pozo D, Martinez C, et al. Vasoactive intestinal peptide and pituitary adenylate cyclase-activating polypeptide inhibit endotoxin-induced TNF-alpha production by macrophages: in vitro and in vivo studies. J Immunol. 1999;162:2358–2367.
Marier JF, Mouksassi MS, Gosselin NH, Beliveau M, Cyran J, Wallens J. Population pharmacokinetics of teduglutide following repeated subcutaneous administrations in healthy participants and in patients with short bowel syndrome and Crohn’s disease. J Clin Pharmacol. 2010;50:36–49.
Hansen L, Hare KJ, Hartmann B, et al. Metabolism of glucagon-like peptide-2 in pigs: role of dipeptidyl peptidase IV. Regul Pept. 2007;138:126–132.
Hollander D, Kaunitz JD. The “Leaky Gut”: tight junctions but loose associations? Dig Dis Sci. 2019. https://doi.org/10.1007/s10620-019-05777-2. (in press).
Acknowledgment
This work was supported by a Department of Veterans Affairs Merit Review Award (Grant No. 5I01BX001245-08), NIH R01 DK54221, and an investigator-initiated Grant from Shire Pharmaceuticals/Takeda Pharmaceuticals USA (Grant Nos. IIR-USA-001851, IIR-USA-000857).
Author information
Authors and Affiliations
Contributions
Y.A. and J.D.K. were responsible for the study concept and design and for drafting article. K.M., T.T., Y.A., H.S., and E.I. were responsible for collection, assembly, and analysis of data. I.K and A.K provided the essential chemicals for the experiments. Y.A. and J.D.K. were responsible for data interpretation.
Corresponding author
Ethics declarations
Conflict of interest
All authors declare that they have no conflicts of interest.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Maruta and Takajo have equally contributed to this work.
Rights and permissions
About this article
Cite this article
Maruta, K., Takajo, T., Akiba, Y. et al. GLP-2 Acutely Prevents Endotoxin-Related Increased Intestinal Paracellular Permeability in Rats. Dig Dis Sci 65, 2605–2618 (2020). https://doi.org/10.1007/s10620-020-06097-6
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-020-06097-6