Abstract
Background/Aims
Epithelial-mesenchymal transition (EMT) plays an important role in hepatocellular carcinoma (HCC) dissemination. Bromodomain PHD-finger transcription factor (BPTF) could regulate embrogenesis and stem cell differentiation, and it may be involved in tumor progression and EMT. In this study, we aimed to determine BPTF, E-cadherin and vimentin expression in tumor tissues and the clinical significance in relation to HCC.
Methods
The BPTF, vimentin and E-cadherin expression of 106 HCC tissue samples was examined by immunohistochemical staining.
Results
BPTF and vimentin showed high expression and E-cadherin showed low expression in HCC. BPTF is associated with the tumor number, vascular invasion, Edmondson-Steiner grade, TNM stage and recurrence (P < 0.05). Vimentin is positively correlated with tumor size, tumor number, vascular invasion, Edmondson-Steiner grade, TNM stage and recurrence (P < 0.05). E-cadherin is negatively correlated with tumor number, Edmondson-Steiner grade, TNM stage and recurrence (P < 0.05). Survival analysis has shown that high expression of BPTF and vimentin indicates poorer overall and disease-free survival (P < 0.05). Multivariate analysis shows that BPTF is an independent marker for survival prediction (P = 0.015). Additionally, high BPTF expression is correlated with high vimentin expression and low E-cadherin expression (P < 0.05).
Conclusion
High BPTF expression may be an independent marker for survival prediction in HCC patients and is probably involved in EMT.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hepatocellular carcinoma (HCC) is the sixth most common neoplasm and the third most frequent cause of cancer death. More than 700,000 cases of this malignant disease are diagnosed each year, and 695,900 cancer deaths occurred worldwide in 2008 [1]. Despite the great gains in the treatment of HCC, the 5-year postoperative survival rate is only 30–40 %. The poor prognosis of patients with HCC is largely the result of tumor recurrence and metastasis [2]. Thus, there is an urgent need to understand the mechanism of invasion and metastasis in HCC.
Bromodomain PHD-finger transcription factor (BPTF) is the largest subunit of the nucleosome remodeling factor (NURF), located at chromosome 17q24.3 [3, 4]. The biological function of BPTF has been implicated in embryo development and morphogenesis and progenitor cell differentiation. BPTF participates in the malignant transformation of human embryonic lung fibroblasts and bladder cancer cell growth [4–9]. Several recent studies have indicated that increased BPTF expression is correlated with SMAD, TGF-β and BMP2, which are closely related with many human cancers, including bladder cancer, lung cancer, breast cancer, etc. [9–11]. Epithelial-mesenchymal transition (EMT) is a biological process in which cells lose their epithelial cell phenotype and acquire a mesenchymal cell phenotype, which could change their potential for development, fibrosis, differentiation, migration, invasiveness, metastasis and resistance to apoptosis [12]. EMT is often accompanied by the abnormal downregulation of expression of E-cadherin and upregulation of expression of vimentin, which are the most commonly used epithelial marker and mesenchymal marker, respectively. The EMT process is often regulated by a series of transcriptional factors (EMT-TFs) such as TGF-β, SMAD, Snail, ZEB, Slug, etc. [13] The function of BPTF in embryonic development, differentiation and cell migration and close correlation with EMT-TFs enable us to speculate that BPTF may be an important modulator of EMT.
However, to date, no studies have reported on the clinicopathological significance of BPTF in HCC. In this study, we present the first evidence that BPTF is correlated with a poor prognosis in HCC and has a close relationship with EMT. According to this research, these results reveal a novel role of BPTF, which may be an important regulatory transcription factor of EMT in HCC.
Materials and Methods
Patients and Tissue Specimens
Tissue specimens of 113 patients with HCC after curative hepatectomy were collected and retrieved from the Department of General Surgery, Affiliated Nanhua Hospital of University of South China, Hunan, China, from January 2003 to December 2008. None of the patients had received chemotherapy or radiotherapy before surgery. Seven patients were lost to follow-up or had insufficient clinicopathological data for analysis and were therefore excluded. Thus, a total of 106 cases of HCC were included in the study. Clinicopathological data on each case, including age, gender, tumor size, nodal status, histological grade, etc., were obtained from patient files. These patients included 81 (59.7 %) males and 25 (40.3 %) females, with a median age of 46 years (range, 19–80). The main clinical characteristics of the 106 patients selected for this study are detailed in Table 1. Each patient's diagnosis was confirmed by histopathology. All patients were staged according to the criteria of the seventh edition of the American Joint Committee on Cancer/International Union Against Cancer TNM classification system. This study was approved by the Research Ethics Committee of the Affiliated Nanhua Hospital of the University of South China. Written informed consent was obtained from all patients. All specimens were handled and made anonymous according to the ethical and legal standards.
Reagents and Antibodies
The primary antibodies used for immunohistochemical detection included rabbit polyclonal anti-human BPTF (sc-98404, Santa Cruz Biotechnology), mouse monoclonal anti-human vimentin (ZM-0260, Zhong-shan Goldenbridge Biotechnology) and mouse monoclonal anti-human E-cadherin (ZM-0092, Zhong-shan Goldenbridge Biotechnology). The PV-9000 Polymer Detection System, DAB and hematoxylin (Zhongshan Golden Bridge Biotechnology) were used for immunohistochemical staining according to the manufacturer’s recommendations.
Immunohistochemistry
The tissue specimens were fixed in 10 % formalin and embedded in paraffin; 4-mm sections were cut and placed on silane-coated slides for immunohistochemical studies. Some of the specimens were stained with H&E and microscopically examined to confirm the diagnosis. The paraffin sections were dewaxed and pretreated in 0.01 M sodium citrate buffer (pH 6.0) for 15 min at 95 °C for tissue antigen retrieval. These sections were then incubated with 3 % hydrogen peroxide for 20 min at room temperature to block endogenous peroxidase. After rinsing three times for 2 min with PBS, 50 µl of 10 % goat serum was added as a blocking liquid, and incubation was conducted for 15 min at room temperature. Then, the serum was removed, and 50 µl per slide of diluted primary antibody (BPTF, 1:150 dilution; E-cadherin, 1:300 dilution; vimentin, 1:200 dilution) was added to each section and incubated overnight at 4 °C. The sections were developed according to the manufacturer’s recommendations (PV-9000, Zhongshan Golden Bridge Biotechnology) and counterstained with hematoxylin; then ethanol dehydration was conducted by grade followed by the addition of xylene to make the sections transparent. Finally, mounting was performed with neutral balsam.
Evaluation of Immunostaining
The staining intensity of BPTF, vimentin and E-cadherin was evaluated on a four-step scale (0, no staining; 1+, weak intensity; 2+, moderate intensity; 3+, strongest intensity). The fraction of stained cells was scored according to the following criteria: 0, 0–10 % positive cancer cells; 1, 11–50 % positive cancer cells; 2, 51–80 % positive cancer cells; 3, >80 % positive cancer cells. The results of staining intensity and extent gave the overall staining score [14]. Negative control slides were probed with goat serum followed by the secondary antibody under the same conditions. Immunostaining was simultaneously evaluated by two pathologists on a multihead microscope without knowledge of the patients’ clinicopathological features and clinical follow-up data.
Patient Follow-Up and Prognostic Study
The follow-up period was from January 2009 to 31 December 2013. Follow-up of all surviving patients included estimation of serum α-fetoprotein levels, dynamic liver computed tomography (CT), liver ultrasonography and chest radiography every 1–2 months, especially during the first 2 years. For suspected recurrence, all available diagnostic modalities including hepatic angiography, magnetic resonance imaging, high-resolution chest CT and positron emission tomography were performed. The follow-up period was defined as the interval between the date of operation and the date of patient death or last follow-up. We censored survival at 5 years after the initial resection surgery. Deaths from other causes were treated as censored cases. The primary outcome was overall survival, defined as the interval between surgery and death regardless of etiology, and the secondary end point was disease-free survival defined by the interval between surgery and tumor recurrence.
Statistical Analysis
All data were analyzed using the SPSS statistical software, version 17.0, for Windows (SPSS, Chicago, IL). Fisher’s exact test was used for statistical analysis of categorical data, whereas independent t tests were used for continuous data. Survival curves were constructed using the Kaplan-Meier method and evaluated using the log-rank test. The Cox proportional hazards regression model was established to identify factors that were independently associated with the overall survival of HCC patients. P values <0.05 were considered statistically significant.
Results
Aberrant Expression of BPTF, E-Cadherin, and Vimentin in HCC
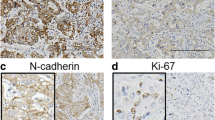
One hundred six paraffin-embedded samples from HCC patients were used to determine the expression of BPTF, E-cadherin and vimentin by immunohistochemistry. The protein expression pattern was categorized into two groups: high (IHC level 2–3) versus low (IHC level 0–1). Of the 106 samples, 75 (70.6 %) exhibited high expression levels of BPTF staining, and 59 samples (55.7 %) exhibited high expression levels of vimentin staining in the tumor. In contrast, only 39 samples (36.8 %) exhibited high expression levels of E-cadherin staining in the tumor. Representative samples of the three protein expressions in the tumor tissues are shown in Fig. 1. BPTF was positively identified in the cell nucleus and cytoplasm (Fig. 1a); E-cadherin was found to be majorly positive in the cell membranes (Fig. 1b); vimentin was found to be majorly positive in the cell cytoplasm (Fig. 1c). These results indicate that BPTF and vimentin are upregulated and E-cadherin downregulated specifically in HCC tissues. The results also showed that BPTF (Fig. 1d) and vimentin (Fig. 1f) had negative expression in adjacent normal liver tissues (ANLTs), but E-cadherin had positive expression in ANLTs (Fig. 1e).
Representative photomicrographs of BPTF, E-cadherin and vimentin expression in HCC tissues. a BPTF-positive expression in the nucleus of HCC cells. b E-cadherin-positive expression in the membrane of HCC cells. c Vimentin-positive expression in the cytoplasm of HCC cells. d, f BPTF- and vimentin-negative expression in adjacent normal liver tissue (ANLT). e E-cadherin-positive expression in ANLT. Magnification, ×100 and ×400
Correlations of BPTF, Vimentin, and E-Cadherin Expression with Clinicopathological Characteristics of HCC
Subsequently, we examined whether aberrant expressions of BPTF, vimentin and E-cadherin were correlated with the clinicopathological characteristics of HCC in our research. We found that high BPTF expression was positively correlated with tumor number, vascular invasion, intrahepatic metastasis, high Edmondson-Steiner grade, TNM stage and recurrence of HCC (P < 0.05, Table 2). High vimentin expression was significantly positively correlated with tumor size, tumor number, vascular invasion, intrahepatic metastasis, high Edmondson-Steiner grade, TNM stage and recurrence of HCC (P < 0.05, Table 2). High expression of E-cadherin was significantly negatively correlated with tumor number, high Edmondson-Steiner grade, TNM stage and recurrence of HCC (P < 0.05, Table 2). These results showed that BPTF, vimentin and E-cadherin expression may be correlated with the prognosis of HCC patients.
High BPTF and Vimentin Expression Is Correlated with a Poor Survival Outcome of HCC Patients
We further analyzed the association between the protein level of BPTF, vimentin and E-cadherin with the prognosis of HCC patients after hepatectomy. We found that high BPTF expression (P = 0.001) and high vimentin expression (0.008) were significantly associated with a poor overall survival (OS) (Fig. 2a, b). However, there was no significant association for E-cadherin expression (P = 0.093) in HCC patients’ OS (Fig. 2c). Furthermore, We found that high BPTF (P = 0.001) or vimentin (P = 0.019) expression indicated significantly poorer disease-free survival (DFS) in HCC patients. There was no significant association between E-cadherin expression and the DFS of HCC patients (P = 0.118). These results demonstrated that BPTF and vimentin expression may be prognostic markers in HCC patients.
BPTF Expression Is An Independent Risk Factor for Survival in HCC Patients
To assess the feasibility of using BPTF, vimentin and E-cadherin expression in HCC prognosis, univariate and multivariate Cox proportional hazards regression models were used. The univariate survival analysis showed that the hepatitis B status, AFP level, liver cirrhosis, Child-Pugh class, tumor number, capsulation formation, vascular invasion, intrahepatic metastasis, Edmondson-Steiner grade, TNM stage and BPTF expression affect the overall survival of HCC patients. Next, the multivariate analysis showed that liver cirrhosis, tumor number, vascular invasion, intrahepatic metastasis, TNM stage and BPTF expression are significant independent prognostic factors for overall survival (Table 3). For analysis of the disease-free survival time, the AFP level, liver cirrhosis, tumor number, vascular invasion, intrahepatic metastasis, TNM stage and BPTF expression reached significance in the univariate Cox proportional hazards regression model. Multivariate survival analysis showed that liver cirrhosis, tumor number, vascular invasion, intrahepatic metastasis, TNM stage and BPTF expression were independent prognostic factors for the disease-free survival time (Table 4). These results indicated that higher BPTF expression is an independent risk factor for survival in HCC patients.
BPTF Expression Correlated with EMT Markers Vimentin and E-Cadherin
We next detected the expression correlations between BPTF and vimentin and E-cadherin in HCC tissues. The Spearman rank correlation analysis showed that high expression of BPTF was significantly associated with evaluated vimentin expression (r = 0.462, P < 0.001) and reduced E-cadherin expression (r = −0.316, P = 0.008) (Table 5). We next detected BPTF, E-cadherin and vimentin expression in serial sections of the same HCC sample. The results indicated that lesions that had high BPTF expression showed low E-cadherin expression and high vimentin expression in HCC tumors (Fig. 3a–c). We also found that these three proteins had a complementary colocalization phenomenon in ANLT (Fig. 3d–f). These data suggest that BPTF may be an important regulator of EMT in HCC cells.
Representative photomicrographs of BPTF, E-cadherin and vimentin expression in serial sections of HCC tissues. a–c BPTF- and vimentin-positive expression, but E-cadherin-negative expression in similar lesions of HCC tumor tissues. d–f BPTF- and vimentin-negative expression, but E-cadherin-positive expression in similar ANLT lesions. Magnification, ×100 and ×400
Discussion
This study used immunohistochemistry to analyze expression patterns of BPTF, vimentin and E-cadherin in HCC cells in order to investigate the role of these molecules in HCC progression and their prognostic importance in HCC. To our knowledge, this is the first study to indicate that BPTF plays an important role in HCC and BPTF may be an EMT regulator. Moreover, based on the survival analysis, we revealed that BPTF and E-cadherin may be valuable independent prognostic factors.
BPTF is a chromatin-mediated regulation of transcription factor, which participates in gene regulation and embryonic development. In previous studies, researchers discovered that BPTF may regulate transcription via histone acetylation and could take part in cancer progression [4, 15]. Then, a study found BPTF-mediated ATP-dependent chromatin remodeling was directly coupled to H3K4 trimethylation to maintain Hox gene expression patterns during development [3]. Next, a series of studies showed that normal expression of BPTF played an important role in maintaining early mouse embryonic development and embryonic stem cell differentiation [7, 8]. The role of BPTF in the regulation of the development, morphogenesis, nervous system development, and cell death and proliferation is similar to cancer progression. This speculation echoed recent research finding that deregulation of BPTF may confer a cancer-promoting phenotype to the cells, and the gain of the BPTF locus is a frequent aberrancy in neuroblastomas, lung adenocarcinomas and various cancer cell lines [9, 11, 16]. In this role, BPTF may regulate TGF-β/Smad transcription signaling to achieve the function [7]. Taking the results of these studies together, we could conclude that BPTF may be an important regulative transcription factor in promoting cancer progression. The characteristic of BPTF in regulating migration, motion and differentiation and the involvement of Smad signaling suggest to us that BPTF may be associated with EMT [13, 17]. EMT plays a crucial role in the development and progression of HCC [18, 19]. HCC cells lose their cell-cell adhesion and cell polarity, and they acquire migratory and invasive properties during the EMT process. Loss of E-cadherin expression and gain of vimentin expression are very significant signs of EMT [20].
Therefore, we investigated the protein expression of BPTF, E-cadherin and vimentin in HCC by IHC. The results indicated that BPTF and vimentin expressions were high in HCC; in contrast, E-cadherein expression was low in HCC. High expression of BPTF and vimentin and low expression of E-cadherin were closely related to negative clinicopathological parameters such as tumor size, tumor numbers, vascular invasion, high Edmondson-Steiner grade, TNM stage and recurrence of HCC. Survival analysis likewise indicated that HCC patients with high expression of BPTF or vimentin had short overall survival and disease-free survival. These results suggested BPTF may be correlated with HCC progression. The univariate and multivariate Cox proportional hazards regression model revealed that high BPTF expression was an independent risk factor for HCC prognosis. We next investigated the relation between BPTF expression and the expression of E-cadherin and vimentin in HCC. Results showed that the expression of BPTF and vimentin had a positive correlation; in contrast, the expression of BPTF and E-cadherin had a negative correlation. Photomicrographs of IHC indicated that lesions with high BPTF expression showed low E-cadherin expression and high vimentin expression. These results, combined with those of the previous functional studies, suggested to us that BPTF may be involved in EMT and may be an important cancer-prompting transcription factor.
Taken together, our results suggest that high BPTF expression is significantly correlated with tumor progression and may be a potent prognostic marker of HCC. High vimentin expression and low E-cadherin expression were closely related with negative clinicopathological characteristics of HCC. Low E-cadherin expression could also be an independent prognostic risk factor. Moreover, BPTF may promote invasion and metastasis via the EMT program. Understanding the regulation mechanism further requires more in vitro and in vivo research.
References
Jemal A, Bray F, Center MM, Ferlay J, Ward E, Forman D. Global cancer statistics. CA Cancer J Clin. 2011;61:69–90.
de Lope CR, Tremosini S, Forner A, Reig M, Bruix J. Management of HCC. J Hepatol. 2012;56:S75–S87.
Wysocka J, Swigut T, Xiao H, et al. A PHD finger of NURF couples histone H3 lysine 4 trimethylation with chromatin remodelling. Nature. 2006;442:86–90.
Jones MH, Hamana N, Shimane M. Identification and characterization of BPTF, a novel bromodomain transcription factor. Genomics. 2000;63:35–39.
Jordan-Sciutto KL, Dragich JM, Caltagarone J, Hall DJ, Bowser R. Fetal Alz-50 clone 1 (FAC1) protein interacts with the Myc-associated zinc finger protein (ZF87/MAZ) and alters its transcriptional activity. Biochemistry. 2000;39:3206–3215.
Li H, Ilin S, Wang W, et al. Molecular basis for site-specific read-out of histone H3K4me3 by the BPTF PHD finger of NURF. Nature. 2006;442:91–95.
Landry J, Sharov AA, Piao Y, et al. Essential role of chromatin remodeling protein Bptf in early mouse embryos and embryonic stem cells. PLoS Genet. 2008;4:e1000241.
Goller T, Vauti F, Ramasamy S, Arnold HH. Transcriptional regulator BPTF/FAC1 is essential for trophoblast differentiation during early mouse development. Mol Cell Biol. 2008;28:6819–6827.
Buganim Y, Goldstein I, Lipson D, et al. A novel translocation breakpoint within the BPTF gene is associated with a pre-malignant phenotype. PLoS ONE. 2010;5:e9657.
Kim K, Punj V, Choi J, et al., Gene dysregulation by histone variant H2A.Z in bladder cancer. Epigenetics Chromatin. 2013;6:34.
Xiao F, Kim YC, Snyder C, et al. Genome instability in blood cells of a BRCA1+ breast cancer family. BMC Cancer. 2014;14:342.
Kalluri R, Weinberg RA. The basics of epithelial-mesenchymal transition. J Clin Invest. 2009;119:1420–1428.
Craene BD, Berx G. Regulatory networks defining EMT during cancer initiation and progression. Nat Rev Cancer. 2012;13:97–110.
Fan CC, Wang TY, Cheng YA, et al. Expression of E-cadherin, Twist, and p53 and their prognostic value in patients with oral squamous cell carcinoma. J Cancer Res Clin Oncol. 2013;139:1735–1744.
Mulder KW, Wang X, Escriu C, et al. Diverse epigenetic strategies interact to control epidermal differentiation. Nat Cell Biol. 2012;14:753–763.
Dai X, Deng S, Wang T, et al. Associations between 25 lung cancer risk-related SNPs and polycyclic aromatic hydrocarbon-induced genetic damage in coke oven workers. Cancer Epidemiol Biomarkers Prev. 2014;23:986–996.
Lim J, Thiery JP. Epithelial-mesenchymal transitions: insights from development. Development. 2012;139:3471–3486.
Maheswaran T, Rushbrook SM. Epithelial-mesenchymal transition and the liver: role in hepatocellular carcinoma and liver fibrosis. J Gastroenterol Hepatol. 2012;27:418–420.
Choi SS, Diehl AM. Epithelial-to-mesenchymal transitions in the liver. Hepatology. 2009;50:2007–2013.
Thiery JP, Acloque H, Huang RY, Nieto MA. Epithelial-mesenchymal transitions in development and disease. Cell. 2009;139:871–890.
Acknowledgments
The authors thank Fan Zheng for polishing the English in the revision.
Conflicts of interest
There are no conflicts of interest.
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Xiao, S., Liu, L., Fang, M. et al. BPTF Associated with EMT Indicates Negative Prognosis in Patients with Hepatocellular Carcinoma. Dig Dis Sci 60, 910–918 (2015). https://doi.org/10.1007/s10620-014-3411-0
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10620-014-3411-0