Abstract
Lung fibrosis is an ultimate consequence of bronchopulmonary dysplasia (BPD) which shows the excessive proliferation of lung fibroblasts (LFs). To find a better model for studying the role of LFs in hyperoxia-induced lung fibrosis at the cellular level, we isolated LFs from the lung tissue of hyperoxia- and normoxia-exposed rat lungs on postnatal days 7, 14 and 21 for primary culture to study their proliferative behavior. In the present study, the LF predominance was > 95% in our culture method. The LFs isolated from rats exposed to hyperoxia in vivo showed significantly greater proliferation than that from normoxia-exposed rats. Flow cytometry revealed that percentage of LFs in S and G2/M stage increased, and proportion in the G0/G1 stage declined at the same time. A greater presence of myofibroblasts in LFs isolated from rats exposed to hyperoxia compared with those exposed to normoxia. In addition, elevated collagen level, transforming growth factor-β and connective tissue growth factor protein expression in conditioned medium were also found in hyperoxia LFs. These data demonstrate that hyperoxia promotes LFs proliferation, myofibroblast transdifferentiation and collagen synthesis in a time-dependent manner. The primary culture of LFs from hyperoxia-exposed rats is a feasible method for studying the pathogenesis and treatment of lung fibrosis caused by BPD at the cellular level.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Although prenatal steroid use, surfactant treatment, gentle ventilation/nasal continuous positive airway pressure, and reduced oxygen concentrations have been suggested as beneficial agents for preventing bronchopulmonary dysplasia (BPD) (Keller and Ballard 2012), BPD remains a major cause of morbidity and mortality in preterm infants (Lemons et al. 2001). The pathogenesis of BPD is multifactorial, and researchers believe pulmonary oxygen toxicity may play an important role in the lung injury process, which leads to the development of BPD (Welty 2001). Lung fibrosis is a life threatening consequence of pulmonary oxygen toxicity in human and animal models (Weinberger et al. 2002; Qi et al. 2015; Huang et al. 2014). The mechanism by which hyperoxia ultimately leads to lung fibrosis is unclear, but the major contributor to lung fibrosis in this situation is the excessive proliferation of lung fibroblasts (LFs) (Crapo 1986; Rehan and Torday 2003). An improved understanding of the mechanisms of hyperoxia-induced excessive proliferation of LFs would be extremely helpful for formulating potential therapeutic strategies for ameliorating hyperoxia-induced lung injury.
Animal models and the in vitro exposure of lung cells to hyperoxia are the two classical models for studying the pathogenesis of BPD (Manji et al. 2001; Chen et al. 2007; Li et al. 2011; Lang et al. 2010). Animal models that expose the developing lung to hyperoxia leads to the changes in the lung that resemble human BPD (Manji et al. 2001; Chen et al. 2007), but this is not suitable for studies at the cellular level. The exposure of other lung cells to hyperoxia in vitro is extremely helpful for understanding the mechanisms of hyperoxia-induced cell injury and death (Li et al. 2011; Lang et al. 2010). However, there is a paradoxical phenomenon in LFs: the in vivo exposure of lungs to hyperoxia leads to increased fibroblast proliferation, but LFs undergo growth arrest and cell death when they are directly cultured under hyperoxia conditions (Hussain et al. 1997; Tzaki et al. 1988). These studies demonstrate that directly expose LFs to hyperoxia conditions is not the optimal method to study lung fibrosis at the cellular level.
Primary cultured cells are derived from tissues and cells that have just been isolated from the body. Compared with cell lines, their biological characteristics have changed very little, and they still have diploid genetic characteristics, which are close to and reflect the growth characteristics of the body. Primary cultured cells are very important for studying cell growth, and cell differentiation and for experimental studies of the effects of drug intervention. Therefore, the primary cell culture of LFs from BPD rats may be the only feasible method for understanding the molecular processes involved in this condition and defining therapeutic targets at the cellular level. The goal of the present study was to develop a reliable method for the isolation, purification and primary culture of LFs from BPD rats and to study the proliferative behavior of these cells for studies of the pathogenesis and treatment of interstitial lung fibrosis at the cellular level.
Materials and methods
Animals and oxygen exposure
All animal experiments were conducted in accordance with the principles stated in the Guide for the Care and Use of Laboratory Animals (NIH publication 8623, National Institutes of Health, Bethesda, MD, 1985). These experiments were approved by the China Medical University Animal Research Committee.
Time-dated pregnant Sprague-Dawley rats were obtained from the Centre for Animal Experiments, China Medical University. The rats were maintained on standard laboratory food and water ad libitum and at a 12:12-h light–dark cycle. Within 12 h of birth, the neonatal rats were randomly assigned to either the hyperoxia group or the normoxia group. The neonatal rats in the hyperoxia group were kept in standard cages placed inside 425-l capacity plexiglass isolation chambers with humidified O2 at ambient pressure with an oxygen concentration between 85 ± 2%, monitored continuously by an oxygen analyzer (OM-25 ME). The CO2 concentration was < 0.5%. The newborn rats in the normoxia group inhaled fresh air (21% oxygen). All other conditions and control factors were the same as those of the hyperoxia group. The nursing rats were exchanged between the 2 groups every 24 h to avoid oxygen toxicity.
Histologic examination
On postnatal days 7, 14 and 21, the rats were killed with an intraperitoneal injection of sodium pentobarbital and were exsanguinated by aortic transection. The right lungs were placed in 4% paraformaldehyde after washing in phosphate-buffered saline (PBS) and were serially dehydrated in increasing concentrations of ethanol before being embedded in paraffin. To standardize the analyses, the lung sections were taken from central areas of the right lower lobe. Five-micrometre tissue sections were stained with haematoxylin and eosin (H&E), examined with light microscopy, and assessed for the presence of intra-alveolar edema, inflammatory cell infiltration, and fibrosis. A quantitative analysis of the radial alveolar count (RAC) and the mean septal wall thickness (ST) was performed as previously described (Martin et al. 2014).
Isolation and culture of lung fibroblasts
Primary cultures of fibroblasts from rat lungs were obtained using a method that improved the method previously described by Kelleher et al. (1995). The left lungs of the rats were removed quickly from the chest under aseptic conditions and placed in a sterile petri dish with precooled D-Hanks solution. The lung tissues were repeatedly cleaned and dissected to free them from connective tissue and nonparenchymal pulmonary tissue. The lungs were then finely minced and digested in 0.25% trypsin (Sigma-Aldrich, St. Louis, MO, USA) for 30 min at 37 °C. When digestion was complete, the cell suspension was pipetted from the minced lung preparation and filtered through sterile gauze to remove particulate matter. Then, 10% fetal bovine serum (FBS, Sigma-Aldrich) was added to the filtered cell suspension to stop further digestion. The cell pellets obtained with centrifugation were then resuspended in Minimum Essential Medium (MEM, Sigma-Aldrich) with 10% FBS, 10,000 U/ml penicillin, and 10,000 µg/ml streptomycin (Sigma-Aldrich). The cells were incubated in 25-cm2 plastic culture flasks overnight. The medium and nonadherent cells were removed, and fresh MEM with 10% FBS was added. Fibroblast predominance was confirmed using immunocytochemical staining for vimentin (Santa Cruz Biotechnology, Inc, Santa Cruz, CA, USA). When they were passaged, the cells were seeded into 150-cm2 culture flasks at a density of 2.5 or 5 × 105 cells/flask and incubated in 95% air/5% CO2 at 37 °C. All experiments were performed using fibroblasts from passage number 2–4 (Kelleher et al. 1995).
Proliferation assay
While in the logarithmic phase, we inoculated 12-well tissue culture plates with 5 × 104 fibroblasts per well and started culturing the fibroblasts in MEM containing 10% FBS. From the second day, cells from 4 randomly selected wells were counted following digestion with 0.125% trypsin/0.01% EDTA and centrifugation. The cell counting was performed for 5 subsequent days. A Burker-Turk hemocytometer was used for cell counting. The growth curves were drawn.
When cells were passaged, they were seeded into cell culture plates, covered with a coverslip, and allowed to grow for 48 h. Then, the coverslip was removed, and the cells were fixed with Carnoy’s fixative (3:1 methanol–acetic acid). The coverslips were evaluated after being stained with Giemsa for 3 min. The labeled cells were counted on each coverslip. One thousand cells were examined from each coverslip to determine the mitotic index. Eight coverslips were calculated in each group.
Cell cycle test
The cell cycle phase distribution was evaluated using flow cytometry. After being harvested via trypsin release, the cells were washed twice with PBS and permeabilized with 70% ethanol overnight. The next day, the ethanol was discarded, and the cells were incubated for 15–20 min at 37 °C with 1 ml of a PI solution (0.1% Triton-100, 50 μg of PI and 200 μg of RNase A). The distribution of the cell cycle phases was determined with a flow cytometer (BD, San Jose, CA, USA).
Western blot analysis
The cells of the different groups were collected and washed with PBS, and then protein was extracted using RIPA Lysis Buffer (Beyotime Biotechnology, Haimen, Jiangsu, China) according to the manufacturer’s instructions. Then, 30 μg of protein was subjected to SDS–polyacrylamide gel (8%) electrophoresis (SDS–PAGE) followed by electrotransfer onto a polyvinylidenedifluoride membrane (Immobilon-P, Millipore Corporation, Billerica, MA, USA). This membrane was blocked for 2 h with 5% non-fat dry milk (NFDM) in Tris-buffered saline/Tween 0.05% (TBST) and then incubated with anti-proliferating cell nuclear antigen (PCNA) antibody (1:500), anti-α-SMA antibody (1:500) (Santa Cruz Biotechnology, Inc.) and anti-β-actin polyclonal antibody (1:1000) (Si Zhen Bai Biological Technology, Beijing, China) overnight at 4 °C. The membrane was washed three times with TBST at room temperature for 10 min and treated with a peroxide-conjugated secondary antibody (1:5000, Beyotime Biotechnology) for 2 h. The proteins in the membrane were revealed using the enhanced chemiluminescence system (ECL advance, Amersham Biosciences, Chalfont Saint Giles, UK), and the image was recorded and analyzed with the BIO-RAD ChemiDoc XRS system (BIO-RAD, Temecula, CA, USA).
Collection of conditioned medium
Lung fibroblasts at passage 2–4 were seeded into 100-cm dishes at a density of 5 × 105 cells/dish. Cells were allowed to grow in full medium for 1 day. At the end of the growth period full medium was aspirated and cells were rinsed with PBS and 10 ml of serum free medium was added to each dish. After 24 h the conditioned medium was collected, filter sterilized and stored at − 80 °C until further used.
Measurement of TGF-β1 and CTGF level
The levels of TGF-β1 and CTGF in conditioned medium were determined using a commercial enzyme-linked immunosorbent assay kit (Boster, Wuhan, China) according to the manufacturer’s protocol.
Collagen assay
Total soluble collagen was measured in the conditioned medium using the Sircol Collagen Assay Kit (Biocolor, Belfast, UK). Briefly, 0.3 ml of Sirius Red reagent was added to an equal volume of test sample and mixed for 30 min at room temperature. The collagen–dye complex was precipitated via centrifugation and dissolved in 0.5 M sodium hydroxide; the absorbance was measured at 540 nm.
Statistical analyses
Values were expressed as the mean ± SD. Statistical significance of the differences was analyzed by two-tail t test for comparison between two groups. P < 0.05 was considered statistically significant.
Results
Lung histology and morphometric analyses
Representative lung sections from normoxia- and hyperoxia-exposed rats are presented in Fig. 1a. While normal structure and alveolarization can be observed in the normoxia group, the lungs of the hyperoxia-exposed rats contained decreased alveolar septation, increased terminal air space size, and some lung fibrosis on postnatal day 7. On postnatal day 14, the lungs of the hyperoxia-exposed rats contained larger air spaces and thicker interstitium with fibrosis. Derangement of the pulmonary tissue with almost complete loss of the lung’s normal architecture associated with extensive interstitial and interalveolar fibrosis was observed on postnatal day 21.
Histological examination of lung tissues by Haematoxylin–eosin (H&E, × 200). Scale bar: 100 µm. Shown are photomicrographs from postnatal d 7, d 14, and d 21 rats exposed to normoxia and hyperoxia (a). In hyperoxia-exposed group, representative images show decreased alveolar septation, increased terminal air space size, and lung fibrosis on postnatal days 7 and 14; derangement of the pulmonary tissue with almost complete loss of the lung’s normal architecture associated with extensive interstitial and interalveolar fibrosis was observed on postnatal day 21. Normal development and alveolarization can be seen in normoxia-exposed group. RAC was lower than in the hyperoxia groups compared with normoxia groups on days 7, 14 and 21 (P < 0.01); ST was higher in the hyperoxia groups when compared with the normoxia groups on days 7, 14 and 21 (d 7, P < 0.05; d 14 and d 21, P < 0.01)
Two morphometric measures, RAC and ST were used to determine the effect of hyperoxia on lung development. RAC was lower than in the hyperoxia groups compared with normoxia groups on days 7, 14 and 21 (P < 0.01; Fig. 1b); ST was higher in the hyperoxia groups than in the normoxia groups on days 7, 14 and 21 (d 7, P < 0.05; d 14 and d 21, P < 0.01) (Fig. 1c).
Primary cell morphology and appraisal results
Inverted microscopy showed that the LFs were spindles and the cell bodies were bright. The cells had a radial or grating arrangement. The nuclei were ovoid and were located in the centre of the cell. There was no obvious difference in morphology between the normoxia and hyperoxia groups (Fig. 2a, b). The LF predominance was > 95%, as confirmed with immunocytochemical staining for vimentin (Fig. 2c).
Identification of lung fibroblasts. LFs were observed by inverted microscopy × 100 (a normoxia on day 21; b hyperoxia on day 21). Scale bar: 100 µm; Vimentin expression revealed by immunohistochemistry × 200. The LF predominance was > 95%, as confirmed with immunocytochemical staining for vimentin (c normoxia on day 21; e hyperoxia on dat 21); Cells in mitosis revealed by Giemsa × 200 (d normoxia on day 21; f hyperoxia on day 21). Scale bar: 200 µm
Effect of hyperoxia on LF proliferation
The LFs from individual normoxia- and hyperoxia-exposed rats were seeded into culture and allowed to grow for 5 days. The LFs isolated from the rats exposed to hyperoxia in vivo showed significantly greater proliferation than did the LFs isolated from normoxia-exposed animals (Fig. 3). As Table 1 shows, the mitotic index values increased from 1.82 to 2.36% at d 7, from 1.74 to 2.72% at d 14 and from 1.66 to 3.04% at d 21. The differences between the normoxia group and hyperoxia groups were significant (d 7, P < 0.05; d 14 and d 21, P < 0.01) (Table 1).
Effect of hyperoxia on cell cycle distribution (%)
To more closely examine the cellular events induced by hyperoxia, we evaluated the cell cycle distribution of the LFs at different days. Flow cytometry revealed that in the LFs isolated from rats exposed to hyperoxia, cell percentage in S and G2/M stage increased, and proportion in G0/G1 stage declined compared with the LFs isolated from normoxia-exposed rats. The cell cycle changes induced by hyperoxia were time dependent (Table 2): the longer the hyperoxia exposure, the more obvious the changes.
Effect of hyperoxia on PCNA and α-SMA protein expression
PCNA is an antigen characteristic of proliferating cells that is expressed in cell nuclei during the S phase of the cell cycle. Therefore, we examined the protein levels of PCNA in the cultured lung cells. The PCNA protein levels were significantly higher in the LFs isolated from the hyperoxia-exposed rats on postnatal days 14 and 21 compared with those isolated from normoxia-exposed rats (P < 0.01) (Fig. 4).
PCNA and α-SMA protein expression in LFs. (a) depicts representative bands for PCNA, α-SMA and β-actin protein. A: Normoxia 7d; B: Hyperoxia 7d; C: Normoxia 14d; D: Hyperoxia 14d; E: Normoxia 21d; F: Hyperoxia 21d. (b) PCNA, (c) α-SMA protein expression in LFs was measured by western blotting. Values are expressed as the mean ± SD with n = 3 for each experiment group, **P < 0.01
α-SMA is the antigen characteristic of myofibroblasts. The α-SMA protein levels in LFs indirectly reflect the proportion of myofibroblasts in the LFs. In this study, we found that the α-SMA protein levels in lung fibroblasts were significantly higher in the LFs isolated from hyperoxia-exposed rats on postnatal days 14 and 21 when compared with those isolated from normoxia-exposed rats (P < 0.01) (Fig. 4).
Effect of hyperoxia on collagen synthesis
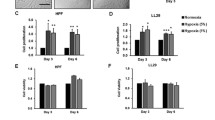
To investigate whether the fibroblast cultures used in this work responded to hyperoxia by increasing collagen production, the total soluble collagen in conditioned medium was analyzed. These data revealed that exposure to hyperoxia significantly increased the total collagen content in the conditioned medium of cultured fibroblasts compared with LFs isolated from normoxia-exposed rats during the same study period (d 14, P < 0.05; d 21, P < 0.01) (Fig. 5a).
Total collagen, TNF-β1 and CTGF levels in conditioned medium of LFs. Rats were exposed to hyperoxia or normoxia within 12 h of birth and primary cultures of LFs from rat lungs were performed from postnatal days 7, 14 and 21. Total soluble collagen (a), TNF-β1 (b) and CTGF (c) were measured in the conditioned media. Values are expressed as the mean ± SD with n = 5 for each experiment group, *P < 0.05; **P < 0.01
Effect of hyperoxia on TGF-β1 and CTGF levels
To define the effects of hyperoxia on the TGF-β1and CTGF protein production, ELISA assay was performed in conditioned medium. The level of TGF-β1and CTGF protein in conditioned medium in the hyperoxia group on days 14 and 21 were significantly enhanced compared with that of the normoxia group (TGF-β1, P < 0.01; CTGF, d 14, P < 0.05 and d 21, P < 0.01) (Fig. 5b, c).
Discussion
Lung fibrosis is the final result of hyperoxia-induced lung injury and is characterized by fibroblast proliferation and the differentiation of myofibroblast that are responsible for producing the extracellular matrix (Rehan and Torday 2003). In the in vivo model, we demonstrate that prolonged exposure of neonatal rats to hyperoxia resulted in decreased alveolar septation, increased terminal air space size and increased lung fibrosis. These changes were evident after 7 days and more pronounced by 21 days, a result consistent with the findings of Warner et al. (1998). However, when LFs were directly cultured in hyperoxia-exposed conditions, they underwent growth arrest and cell death. Therefore, the primary culture of LFs from BPD rats is the only feasible method for studying the mechanism of lung fibrosis at the cellular level.
In the present study, we demonstrated that LFs isolated from rats that were exposed to hyperoxia proliferated more rapidly than fibroblasts obtained from rats exposed to normoxia. This result was consistent with the pathological changes of LFs in the lung tissue during BPD. Kelleher et al. (1995) obtained the same result and explained that the fibroblasts isolated from hyperoxia-exposed rats were more sensitive to the proliferative effects of insulin-like growth factor I and that these cells had a higher expression of c-Ha-ras, which is an essential protein for progression through the cell cycle. To more closely examine the cellular events, the mitotic index, cell cycle distribution and PCNA expression of LFs were measured. Compared with those isolated from normoxia-exposed rats, the number of split phase LFs isolated from rats exposed to hyperoxia for 7 days was significantly higher, and flow cytometry showed a lower percentage of cells in the G0/G1 and a higher percentage of cells in the S and G2/M stage. With the extension of the hyperoxia exposure time, the trend became more obvious. This association illustrated that hyperoxia weakened the G1/S checkpoints and allowed more cells to cross the G1/S checkpoints from the G1 to the S and G2/M phase, complete DNA replication and eventually promote the proliferation of fibroblasts. PCNA was originally recognized as an antigen characteristic of proliferating cells that is expressed in cell nuclei during the S phase of the cell cycle (Celis et al. 1986). PCNA is a widely recognized cell proliferation marker, and there is a good correlation between PCNA and cell proliferation in high-oxygen lung injury (Albertine et al. 2010; Giordani et al. 2014). In this study, the increase in PCNA levels in LFs isolated from rats was detectable at 14 days of hyperoxia exposure and was more pronounced with increasing times of exposure, up to 21 days. This result is consistent with the protein levels of PCNA in neonatal rat lungs during the development of BPD (Xing et al. 2015).
Myofibroblasts are a type of LFs that has greater proliferative potency. They have a phenotype between fibroblasts and smooth muscle cells and are defined by the presence of α-SMA. As a special phenotype of fibroblasts, myofibroblasts play an important role in lung development and lung injury repair. The hyperoxia-increased presence of myofibroblasts has been implicated in the pathogenesis of BPD (Popova et al. 2010). There was a greater presence of myofibroblasts in LFs isolated from rats exposed to hyperoxia compared with those exposed to normoxia in this study. This suggests that hyperoxia induces myofibroblast transdifferentiation in LFs.
Collagen is the major extracellular matrix (ECM) component of the lungs and is vital for maintaining normal lung architecture. Total collagen levels are determined by a balance between synthesis and degradation. Kondrikov et al. (2011) found that the increase in the collagen content of lung tissues is correlated with changes in hyperoxia-induced lung fibrosis. However, the effect of hyperoxia on collagen synthesis of LFs in vitro, different conclusions were drawn. Hussain et al. (1997) demonstrated that hyperoxia reduced the expression levels of procollagens in fetal LFs; Lang et al. (2010) found that LF exposure to hyperoxia resulted in an increase in collagen synthesis. This discrepancy between the responses may be explained by the difference in the durations of hyperoxia exposure (120 vs. 48 h). Consequently, fibroblasts exposed to hyperoxia in vitro may not be suitable for studying collagen changes in BPD. In this study, the production of collagens instantly increased in LFs isolated from rats exposed to hyperoxia in vivo. The longer the hyperoxia exposure, the greater the collagen formation. We suggest that hyperoxia-induced collagen production is mainly caused by an increase in collagen synthesis rather than a decrease in collagen degradation.
It is widely believed that TGF-β1 plays a key role in the pathogenesis of hyperoxia-induced lung fibrosis, can induce fibroblast migration, proliferation and differentiation of myofibroblasts, and deposition of ECM (Petrov et al. 2002). Overexpression of TGF-β1 leads to structural changes, including proliferation α-actin-positive myofibroblasts within the alveolar septal walls and abnormal alveolar structure. CTGF is implicated in fibroblast proliferation, cellular adhesion, angiogenesis, and ECM synthesis, which functions as a downstream mediator of TGF-β1 (Chen et al. 2007). TGF-β1 and CTGF levels are increased in infants with BPD. In this study, hyperoxia upregulated the expression of both TGF-β1 and CTGF in conditioned medium. This finding suggests that both TGF-β1 and CTGF play important roles in the pathogenesis of hyperoxia-induced pulmonary fibrosis. The increase in TGF-β1 and CTGF is correlated with change in collagen content. These will help to increase the principal role of LFs which is to maintain the integrity of alveolar structure via the synthesis, secretion, maintenance, degradation and remodeling of ECM.
Conclusions
In this study, we demonstrated that hyperoxia promotes LFs proliferation, myofibroblast transdifferentiation and collagen synthesis in a time-dependent manner. These results were consistent with the pathological changes of LFs in the lung tissue of BPD. Therefore, we believe that the primary culture of LFs from BPD rats is a feasible method for studying the pathogenesis and treatment of interstitial lung fibrosis of BPD at the cellular level.
Abbreviations
- BPD:
-
Bronchopulmonary dysplasia
- LFs:
-
Lung fibroblasts
- TGF-β1:
-
Transforming growth factor-β
- CTGF:
-
Connective tissue growth factor
- PBS:
-
Phosphate-buffered saline
- RAC:
-
Radial alveolar count
- ST:
-
The mean septal wall thickness
- FBS:
-
Fetal bovine serum
- MEM:
-
Minimum essential medium
- NFDM:
-
Non-fat dry milk
- PCNA:
-
Proliferating cell nuclear antigen
References
Albertine KH, Dahl MJ, Gonzales LW, Wang ZM, Metcalfe D, Hyde DM et al (2010) Chronic lung disease in preterm lambs: effect of daily vitamin A treatment on alveolarization. Am J Physiol Lung Cell Mol Physiol 299:L59–L72
Celis JE, Madsen P, Nielsen S, Celis A (1986) Nuclear patterns of cyclin (PCNA) antigen distribution subdivide S-phase in cultured cells—some applications of PCNA antibodies. Leuk Res 10:237–249
Chen CM, Wang LF, Chou HC, Lang YD, Lai YP (2007) Up-regulation of connective tissue growth factor in hyperoxia-induced lung fibrosis. Pediatr Res 62:128–133
Crapo JD (1986) Morphologic changes in pulmonary oxygen toxicity. Annu Rev Physiol 48:721–731
Giordani VM, Debenedictus CM, Wang Y, Sanchez-Esteban J (2014) Epidermal growth factor receptor (EGFR) contributes to fetal lung fibroblast injury induced by mechanical stretch. J Recept Signal Transduct Res 34:58–63
Huang LT, Chou HC, Lin CM, Yeh TF, Chen CM (2014) Maternal nicotine exposure exacerbates neonatal hyperoxia-induced lung fibrosis in rats. Neonatology 106:94–101
Hussain N, Wu F, Christian C, Kresch MJ (1997) Hyperoxia inhibits fetal rat lung fibroblast proliferation and expression of procollagens. Am J Physiol 273:726–732
Kelleher MD, Naureckas ET, Solway J, Hershenson MB (1995) In vivo hyperoxic exposure increases cultured lung fibroblast proliferation and c-Ha-ras expression. Am J Respir Cell Mol Biol 12:19–26
Keller RL, Ballard RA (2012) Bronchopulmonary dysplasia. In: Gleason CA, Devaskar SU (eds) Avery’s diseases of the newborn, 9th edn. Elsevier Saunders, Philadelphia, pp 658–671
Kondrikov D, Caldwell RB, Dong Z, Su Y (2011) Reactive oxygen species-dependent RhoA activation mediates collagen synthesis in hyperoxic lung fibrosis. Free Radic Biol Med 50:1689–1698
Lang YD, Hung CL, Wu TY, Wang LF, Chen CM (2010) The renin-angiotensin system mediates hyperoxia-induced collagen production in human lung fibroblasts. Free Radic Biol Med 49:88–95
Lemons JA, Bauer CR, Oh W, Korones SB, Papile LA, Stoll BJ et al (2001) Very low birth weight outcomes of the National Institute of Child health and human development neonatal research network, January 1995 through December 1996. NICHD Neonatal Research Network. Pediatrics 107:E1
Li Z, Choo-Wing R, Sun H, Sureshbabu A, Sakurai R, Rehan VK et al (2011) A potential role of the JNK pathway in hyperoxia-induced cell death, myofibroblast transdifferentiation and TGF-β1-mediated injury in the developing murine lung. BMC Cell Biol 12:54. https://doi.org/10.1186/1471-2121-12-54
Manji JS, O’Kelly CJ, Leung WI, Olson DM (2001) Timing of hyperoxic exposure during alveolarization influences damage mediated by leukotrienes. Am J Physiol Lung Cell Mol Physiol 281:L799–L806
Martin CR, Zaman MM, Gilkey C, Salguero MV, Hasturk H, Kantarci A et al (2014) Resolvin D1 and lipoxin A4 improve alveolarization and normalize septal wall thickness in a neonatal murine model of hyperoxia-induced lung injury. PLoS ONE 9:e98773. https://doi.org/10.1371/journal.pone.0098773
Petrov VV, Fagard RH, Lijnen PJ (2002) Stimulation of collagen production by transforming growth factor-β1 during differentiation of cardiac fibroblasts to myofibroblasts. Hypertension 39:258–263
Popova AP, Bozyk PD, Bentley JK, Linn MJ, Goldsmith AM, Schumacher RE et al (2010) Isolation of tracheal aspirate mesenchymal stromal cells predicts bronchopulmonary dysplasia. Pediatrics. https://doi.org/10.1542/peds.2009-3445
Qi XJ, Ning W, Xu F, Dang HX, Fang F, Li J (2015) Fasudil, an inhibitor of Rho-associated coiled-coil kinase, attenuates hyperoxia-induced pulmonary fibrosis in neonatal rats. Int J Clin Exp Pathol 8:12140–12150
Rehan V, Torday J (2003) Hyperoxia augments pulmonary lipofibroblast-to-myofibroblast transdifferentiation. Cell Biochem Biophys 38:239–250
Tzaki MG, Byrne PJ, Tanswell AK (1988) Cellular interactions in pulmonary oxygen toxicity in vitro: II. Hyperoxia cause adult rat lung fibroblast cultures to produce apparently autocrine growth factors. Exp Lung Res 14:403–419
Warner BB, Stuart LA, Papes RA, Wispe JR (1998) Functional and pathological effects of prolonged hyperoxia in neonatal mice. Am J Physiol Lung Cell Mol Physiol 295:L110–L117
Weinberger B, Laskin DL, Heck DE, Laskin JD (2002) Oxygen toxicity in premature infants. Toxicol Appl Pharmacol 181:60–67
Welty SE (2001) Is there a role for antioxidant therapy in bronchopulmonary dysplasia? J Nutr 131:947S–950S
Xing Y, Fu J, Yang H, Yao L, Qiao L, Du Y et al (2015) MicroRNA expression profiles and target prediction in neonatal Wistar rat lungs during the development of bronchopulmonary dysplasia. Int J Mol Med 36:1253–1263
Author information
Authors and Affiliations
Corresponding author
Rights and permissions
About this article
Cite this article
Zhao, Sm., Wu, Hm., Cao, Ml. et al. Primary culture of lung fibroblasts from hyperoxia-exposed rats and a proliferative characteristics study. Cytotechnology 70, 751–760 (2018). https://doi.org/10.1007/s10616-017-0179-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10616-017-0179-z