Abstract
This study aimed to (i) explore the association between perceptions of negative social relationships in childhood with significant others, including peers, guardians and teachers, symptoms of depression and OCD, and suicide behaviors, and (ii) examine whether depression and OCD severity meditated the association between these perceptions and suicide experiences. In total, 783 individuals from the community were invited to complete self-report measures. There were strong associations between perceptions of adverse social relationships in childhood, severity of depression and OCD, and suicide behaviors. Furthermore, depression and OCD partially mediated the association between perceptions of adverse social relationships, especially with peers, and suicide behaviors. These results provide strong evidence for the importance of developing clinical interventions that directly target negative experiences of social relationships in childhood, and for raising public and scientific awareness that everyday adverse social interactions with significant others can impact negatively on mental health including suicide behaviors.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Childhood maltreatment is broadly defined as the use of violent behaviors targeted at children and adolescents up until the age 18 [1]. There are five major forms of childhood maltreatment, namely, sexual, physical, and emotional abuse, and physical and emotional neglect. Within the extant literature, it is well established that there is a strong association between experiences of childhood abuse and/or neglect, and the development and maintenance of both physical and mental health problems which can have long-lasting consequences [2, 3]. In particular, experiences of different forms of childhood maltreatment can affect neurological, emotional, and psychosocial functioning. Examples include difficulties with working memory [4]; having heart problems [5]; and having an increased probability of engaging in risk taking behaviors. Such behaviors may result in contracting sexually transmitted infections, smoking tobacco, and excessive use of legal and illegal substances [6,7,8]. The mental health consequences of childhood maltreatment include experiencing depressed mood states which can be severe [9]; having a range of anxiety related mental health problems, for example, social phobia, obsessive-compulsive disorder, and post-traumatic stress disorder [10]; and experiencing suicide thoughts and behaviors [11].
Of note, leading contemporary psychological theories of suicide thoughts and behaviors have highlighted that problems with social relationships, such as perceptions of not belonging to communities or networks [12] and appraisals of social isolation, may be key components in the pathways leading to suicide thoughts, acts and deaths [12,13,14]. Although death by suicide is complicated, it is often preventable [15]. Yet, globally, suicide fatalities account for one death every 40 s [16]. Experiencing abuse and/or neglect as a child is a high-risk factor for suicide thoughts and behaviors later in life [17,18,19], even though the exact mechanisms remain under-studied. Experiences of childhood maltreatment, particularly within social relationships may be particularly salient, and can occur in different contexts, for example, from family members, peers, care givers and schools [11, 20, 21]. Furthermore, childhood maltreatment may be experienced on a continuum from less severe to more severe [22].
At the most severe end of this type of continuum, children may have been subjected to extreme physical, emotional and sexual abuse, all of which often co-occur and interact [23]. Childhood maltreatment and abuse may also be experienced in a less severe form which is, nevertheless, potentially highly damaging to mental health. For example, maltreatment within myriad social contexts can be characterized by negative social interactions with one or more significant others, namely, peers, guardians and/or teachers [24]. These types of unpleasant and negative social relationships include experiencing unsupportive social interactions emotionally and physically [25]; being bullied in both face-to-face and on-line communities [26]; dealing with frequent pejorative and/or criticizing comments from friends, guardians, and family members [27, 28]; being belittled [29]; and feeling unfairly treated by significant others [30].
Negative social relationships are common, with nearly one out of five schoolchildren reporting experiences of being either bullied or cyberbullied, and feeling unsupported by their parents, guardians and/or teachers [31, 32]. However, to date there is scant evidence examining the impact of negative social relationships experienced as a child with peers [33, 34], guardians [35], and teachers [36] on psychological well-being, and suicide thoughts and behaviors experienced in adulthood. Hence, the first aim of the current study was to redress this gap. In particular and in accord with the extant literature, we sought to examine the frequency of the perceptions of adverse social relationships in childhood with significant others and their association with common mental health problems, including depression [37] and suicide thoughts and behaviors [17, 18]. We also extended this association to include symptoms of obsessive-compulsive disorder for two main reasons. First, OCD is a very prevalent mental health problem, with an estimated lifetime prevalence of between 2.3 to 13% in European countries and the Unites States of America [38, 39]. Second, although current evidence suggests a strong relationship between adverse events in childhood and obsessive-compulsive behaviors [40, 41], this association has received mixed support within the extant literature [42]. Therefore, we aimed at redressing this important research gap.
It is plausible that certain types of adverse social relationships may be more distressing and more strongly linked with mental health problems experienced in adulthood than others, in particular suicide ideation and behaviors. Although previous research has suggested that adverse experiences from peers are more strongly associated with symptoms of depression and OCD, followed by adverse experiences from guardians and teachers [24, 32], these findings need to be extended within different types of social contexts. Notably, no prior research has fully examined the differential impact of perceptions of different types of negative social relationships formed during childhood on suicide thoughts and behaviors experienced as an adult. Specifically, we were interested in the relationships between perceptions of social interactions with (i) peers, (ii) guardians and (iii) teachers, and suicide thoughts and behaviors. Therefore, this formed the second aim of the current study.
Finally, although there is strong evidence that depression is related to suicide thoughts and behaviors [43], the evidence that anxiety and obsessive-compulsive disorders is associated with suicide thoughts and behaviors is, currently, under-researched [44]. Whilst it must be acknowledged that anxiety and obsessive-compulsive disorders are complex and multi-faceted, recent meta-analytic reviews found that both body-dysmorphic disorder [45] and obsessive-compulsive disorder [46] were associated with heightened suicide thoughts and behaviors. Hence, obsessive-compulsive disorder may be an important precursor to suicide thoughts and behaviors in those who have experienced childhood maltreatment because there is evidence which indicates that experiences of childhood abuse may contribute to the development of obsessive-compulsive, and related, mental health problems [47, 48]. Indeed, one study conducted in Northern Ireland found that any anxiety disorder, including obsessive-compulsive disorder, partially mediated the association between adverse childhood experiences, such as family violence, conflict, and sexual abuse, and suicide thoughts and behaviors [49]. It is, clearly, important to examine pathways to suicide thoughts and behaviors from adverse social events in childhood which are mediated by obsessive-compulsive related problems. Therefore, as adverse social events are frequently experienced during day-to-day interactions with significant others [31], the third aim of this study was to investigate the extent to which a range of perceptions of negative social relationships of differing levels of severity experienced during childhood predicted suicide thoughts and behaviors in adulthood both directly and indirectly via depressed mood states and OCD.
There were three key predictions. First, that self-reported experiences of childhood negative or adverse social events would be associated with mental health problems, in particular, depression, OCD and suicide thoughts and behaviors in adulthood.
The second prediction was related to the first which was that perceptions of negative social experiences in childhood from peers would be a stronger predictor of mental health problems in adulthood than perceptions of negative experiences from guardians and teachers. This prediction was based on current evidence suggesting that individuals who were both bullied by their peers and maltreated by adults in childhood were not more adversely affected in adulthood than those who were bullied by peers alone [50].
The third prediction was that symptoms of both depression and OCD would mediate any associations between perceptions of adverse childhood social experiences and suicide thoughts and behaviors in adulthood.
Method
Participants
A total of 783 adults over 18 years old took part in the study (93% participation rate). Participants’ mean age was 33.02 (SD = 11.06, range: 18–73), and 31.2% of the sample were male. Most of the participants were born (79.2%) or resided (89.8%) within the United Kingdom, whereas fewer participants were either born (20.8%) or resided (10.2%) in European countries or in the United States of America (U.S.A.). Employed participants comprised 69.7% of the sample; university students comprised 19.0% of the sample; and 11.2% were unemployed at the time of data collection. With regard to education, 88.3% of the total sample had a university education, whereas 11.2% had secondary education and 0.5% had not received any education. More than half of the participants (59.9%) reported a monthly household income that ranged between 500 and 2000 British pounds (which indicated a low or middle socioeconomic class), whereas the rest, i.e., 40.1% reported a monthly income higher than 2000 British pounds (indicating a middle to high socioeconomic class) [51]. Participants were recruited from the University of South Wales (via on-campus recruitment forums and through email), from the larger community within the United Kingdom (UK) by visiting local businesses (e.g., coffee places), and on-line through social media platforms, including Facebook, Twitter, and Instagram. Participation was voluntarily and anonymous. Participants had to be i) fluent in English and ii) over 18 years old to take part in the study. No other exclusion criteria were applied. The study was prepared in accord with the guidelines by the British Psychological Association and was approved by the ethics committee of the University of South Wales before commencement (Ref number: 1.905.172.1).
Design
A cross-sectional design was used. This means that all assessments were completed only once by all participants. The predictor variables were symptoms of depression and OCD, and self-reported perceptions of social adverse events experienced during childhood. Furthermore, the measure that assessed perceptions of adverse social experiences in childhood was broken down into sub-scales and formed three predictor variables of negative social relationships with i. peers, ii. guardians and iii. teachers. Suicide ideation and behaviors were the outcome variable. In the mediational analyses, depression and OCD scores were used as parallel mediators. Age and gender were used as control variables based on current evidence suggesting that (i) older participants were more adversely affected by negative childhood experiences [17] and (ii) males reported more adverse social experiences than females [24].
Measures
Centre for Epidemiologic Studies Depression Scale (CES-D) [52]
This is a 20-item self-report questionnaire that assesses the severity of depressive symptoms during the past week. Examples include “I felt depressed”, “I had crying spells”, and “I felt sad”. The measure uses a 4-point scale which range from 1 = rarely to 4 = most of the time. The overall scale has been found to have very good psychometric properties, with the Cronbach’s alpha index being as high as 0.95. The alpha coefficient for the current sample was 0.95.
Obsessive-Compulsive Inventory Revised (OCI-R) [53]
This is an 18-item self-report scale that evaluates the OCD symptom clusters that have been found to be present in those individuals experiencing obsessive-compulsive disorder. These symptoms are grouped around six sub-categories, namely, washing (e.g., “I wash my hands more often and longer than necessary”), checking (e.g., “I check things more often than necessary”), orderliness (e.g., “I get upset if objects are not arranged properly”), hoarding (e.g., “I have saved up so many things that they get in the way”), neutralizing (e.g., “I feel compelled to count while I am doing things”) and obsessions (e.g., “I am upset by unpleasant thoughts that come into my mind against my will”). The measure utilizes a 5-point scale to rate responses, which range from 1 = never to 5 = very much. The OCI-R has been found to be a reliable tool for measuring symptoms of obsessive-compulsive disorder, with the Cronbach’s alpha index reported to be 0.89 for the overall scale. The alpha coefficient for the current sample was 0.90.
Suicidal Behaviors Questionnaire Revised (SBQ-R) [54]
This is a 4-item self-report questionnaire that measures levels of lifetime suicidality (item 1; e.g., “Have you ever thought about or attempted to kill yourself ?”), frequency of suicide ideation in the past year (item 2; e.g., “How often have you thought about killing yourself in the past year ?”), communication of the intention to die by suicide (item 3; e.g., “Have you ever told someone that you were going to commit suicide, or that you might do it ?”), and the likelihood of death by suicide in the future (item 4; e.g., “How likely is it that you will attempt suicide someday?”). Osman et al. (2001) reported Cronbach’s alpha indices of 0.76 and 0.88 in non-clinical and clinical samples respectively. The alpha coefficient for the current sample was 0.87.
History of Social Punishment (HoSP) [40]
This is a 11-item self-report scale that assesses an individual’s perceived history of adverse social interactions during childhood with peers (“I have been bullied by my peers”), guardians, (“My parents could often be quite bossy”) and teachers (“My teachers usually underestimated me”). The HoSP employs a 5-point scale that ranges between 1 = never to 5 = very much. The HoSP was found to have very good to excellent convergent and divergent validity, test–retest reliability and internal consistency [24, 40]. To further examine the factor-structure of the newly developed English version of the HoSP, we conducted a series of confirmatory factor analyses based on the data of the current sample. We found that the 11-item three-factor solution [x2(41) = 114.39, p < 0.001; CFI = 0.97; TLI = 0.96; RMSEA = 0.05; SRMR = 0.04], demonstrated a very good model fit. The alpha coefficient was 0.86 for the overall scale; 0.81 for the peer sub-scale, which comprised 4 items; 0.87 for the guardian sub-scale scale comprising 4 items; and 0.77 for the teacher sub-scale, which comprised 3 items.
Procedure
Prospective participants were asked to complete the assessments for the study. After reading the Participation Information Sheet, they signed the consent form and were subsequently requested to provide their e-mail addresses to facilitate the logistics of future study participation if desirable. All data were collected online via the JISC Survey® platform and the order of the assessments was randomized. Participants were also requested to provide information about demographic characteristics, including, age, gender, occupation, and socio-economic status. All participants were fully debriefed regarding the full purposes of the study and were also provided with mental health resources that included contact details for Suicide Helplines (e.g., Samaritans, Hopeline UK, Calm), and the general emergency phone number for the UK (999 or 111). Furthermore, participants were advised to contact these services if they felt distressed about their participation in the study. None of the participants received money or other incentives and were debriefed at the end of their participation regarding the objectives of the study.
Data Analyses Strategy
All statistical analyses were conducted using Stata 15® (StataCorp LP, USA). First, all the variables to be analyzed were tested for univariate normality using the mvtest normality command. If the data was not normally distributed, to examine the relationship between the overall perceptions of adverse social relationships in childhood, the perceptions of adverse social events as experienced from peers, guardians, and teachers, the symptoms of depression, OCD, and suicide thoughts and behaviors, we used Spearman correlation coefficients. Conversely, if the data was normally distributed we used Pearson’s Product Moment correlation coefficients to evaluate associations between key variables. To examine the frequency of perceptions of different adverse social experiences in our sample, we calculated the percentages of these experiences based on the participants’ scores on each individual item of the HoSP scale. To examine differences between the correlation coefficients, we calculated Fisher’s z scores [55]. We conducted two hierarchical regression analyses with 5,000 bootstrapped iterations, which corrects biased standard errors, to test whether social adversities were associated with suicide ideation and behaviors after accounting for age, gender, depression and OCD. In the first regression model, age and gender was entered into step 1, symptoms of OCD and depression were entered into step 2, and overall perceptions of social adversities were entered into step 3. In the second regression model, the variables entered into steps 1 and 2 were the same as for model 1, but the components of social adversities i.e., adversity from (i) peers, (ii) guardians, and (iii) teachers were entered into step 3. To identify whether perceptions of adverse social events as experienced in childhood contributed to pathways to suicide thoughts/behaviors directly, indirectly via symptoms of depression and OCD, and/or both, we ran bootstrapped mediational analyses with 5000 iterations. The overall perceptions of adverse social relationships in childhood served as the predictor variable, depression and obsessive-compulsive scores were the parallel mediating variables, and suicide thoughts and behaviors were the outcome variable whilst controlling for age and gender differences [56, 57]. Subsequently, a second set of 5000 bootstrapped mediational analyses were conducted using the perceptions of adverse social events experienced from each of peers, guardians, or teachers as the predicting variables, depression and obsessive–compulsive scores were parallel mediating variables, and suicide thoughts and behaviors was the outcome variable whilst controlling for both age and gender. Finally, we ran an a priori power analysis to determine the minimum sample size for performing multiple linear regression analyses with at least 4 covariates, a small effect size (R-squared = 0.1) and an alpha of 0.05.
Results
The results from the power analysis showed that a total number of 113 participants was required to achieve a power of 0.80. However, we greatly increased our sample to include a representative community sample (see Participants section).
Experiences of Adverse Social Relationships
As detailed in Table 1, perceptions of adverse social interactions in childhood with peers were disclosed from between 21.1% and 33.1% of the sample who reported that they either agreed or strongly agreed with the items assessing adverse experiences from peers sub-scale of the HoSP. The most common experience was having received negative comments concerning a person’s face or body part (33.1%), followed by experiences of being bullied (29.0%). Between 13.67% and 27.2% of the sample reported having received adverse experiences from their guardians. Having bossy/authoritarian parental figures was the most frequent experience. Only a small proportion of the sample ranging between 4.6% and 10.5% either agreed or strongly agreed with having experienced adverse events from their teachers. The most common experience was perceptions of being underestimated by their teachers.
The Association Between Perceptions of Adverse Social Relationships with Significant Others in Childhood, and Depression, OCD, and Suicide Thoughts and Behavior in Adulthood
The first prediction was that overall perceptions of adverse social experiences in childhood would be associated with depression, OCD and suicide thoughts and behaviors in adulthood. In accord with this prediction, there were significant positive, strong, correlations between perceptions of adverse social experiences, symptoms of depression, OCD, and suicide thoughts and behaviors (see Table 2). Perceptions of overall social adversities were most strongly associated with depression, followed by suicide ideation/behaviors and then OCD. Whilst the correlation coefficient between adversities and depression was significantly stronger than that between adversities and OCD (zDifference = 2.77, p = 0.01), the correlation coefficient between adversities and suicide ideation/behaviors was not significantly different than that between adversities and depression (zDifference = 1.06, p = 0.15) nor between adversities and OCD (zDifference = 1.20, p = 0.12).
The second, and related prediction, was that negative social experiences in childhood from peers would be stronger predictors of depression, OCD, and suicide ideation and behaviors than the negative social events experienced in childhood from guardians and teachers. Our results showed that, indeed, perceptions of adverse social interactions in childhood with peers were correlated more strongly with depression, OCD, and suicide experiences than adverse social interactions with guardians (zDifference = 5.91, p < 0.001; zDifference = 4.23, p < 0.001; zDifference = 4.66, p < 0.001), and teachers (zDifference = 4.67, p < 0.001; zDifference = 3.34, p < 0.001; zDifference = 4.27, p < 0.001). No significant differences in the correlation coefficients were identified between perceptions of adverse social interactions in childhood from guardians, and depression, OCD and suicide experiences, and between perceptions of adverse social interactions in childhood from teachers, and depression, OCD and suicide experiences (zDifference = -1.04, p = 0.15; zDifference = -0.26, p = 0.40; zDifference = -0.76, p = 0.22).
As detailed in Table 3, the contribution of the perceptions of adverse social experiences in childhood on suicide ideation and behaviors was further explored by running two hierarchical regression analyses. In model 1, age and gender, which were control variables, were entered at step 1, symptoms of OCD and depression were entered at Step 2, and perceptions of overall adverse social experiences were entered at Step 3. Overall, adverse social experiences in childhood made a unique contribution to the prediction of suicide ideation and experiences (b = 0.08, t(777) = 5.42, p < 0.001) and explained a significant proportion of variance in suicide experiences, R2 = 0.38, F (5, 777) = 93.32, p < 0.001.
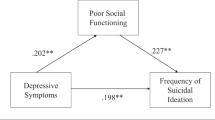
In model 2, we repeated the first three steps of model 1 and entered the perceptions of adverse social events as experienced independently from peers, guardians, and teachers at step 3. Adverse social events from peers significantly predicted suicide ideation and behaviors (b = 0.15, t(775) = 4.41, p < 0.001) which was in accord with our predictions, and also explained a significant proportion of variance in suicide experiences, R2 = 0.38, F (7, 775) = 67.54, p < 0.001 (Fig. 1).
The Direct and Indirect Effects of the Perceptions of Adverse Social Relationships in Childhood with Significant Others on Suicide Ideation and Behaviors in Adulthood
The third prediction was that symptoms of both depression and OCD would mediate any links between adverse social experiences in childhood and suicide thoughts and behaviors. The results of the first set of the analyses, which are presented in Table 4, demonstrated that perceptions of overall adverse social experiences in childhood were significantly associated with suicide thoughts/behaviors both directly and indirectly, via symptoms of depression and OCD. This means that symptoms of both depression and OCD partially mediated the relationship between perceptions of overall adverse social experiences in childhood, and suicide ideation and behaviors in adulthood. Furthermore, the results of the second set of the analyses showed that although perceptions of negative social relationships in childhood with peers were both directly and indirectly linked with suicide thoughts and behaviors, via depression and OCD, the perceptions of adverse social events in childhood from guardians and teachers were only linked with suicide experiences in adulthood through an indirect pathway via symptoms of depression or OCD, but not via a direct pathway. Although depression and OCD partially mediated the relationship between perceptions of adverse social events from peers and suicide ideation and behaviors, they fully mediated the relationships between perceptions of adverse social events from guardians or teachers, and suicide experiences.
Discussion
There were three major findings from the current study which have important clinical implications. First, our results confirmed the predicted strong associations between perceptions of common-place adverse social relationships in childhood with significant others and symptoms of depression, OCD, and suicide thoughts and behaviors in adult life. It is worth noting that studies examining the association between OCD and myriad adverse childhood events, including experiences of abuse and/or neglect, has been limited and inconclusive [58]. However, our findings suggested a moderate to strong association between perceptions of negative social experiences and OCD corroborating recent evidence suggesting that individuals who had experienced adversities during childhood may develop symptoms of OCD in adulthood [24, 40, 59]. Second, the pattern of results demonstrated that perceptions of adverse social interactions in childhood with peers were more strongly associated with depression, OCD, and suicide experiences compared to the perceptions of adverse social interactions from guardians and teachers. Consistent with this, perceptions of adverse social relationships with guardians and teachers did not predict suicide thoughts and behaviors above and beyond adverse social relationships with peers. Overall, these findings are important for two key reasons. First, perceptions of such ‘common-place’ adverse social experiences (e.g., criticism of someone’s face or body, bullying) may serve as risk factors for experiencing harsher forms of maltreatment [60]. Second, these results build upon a limited but growing literature indicating that peer victimization, which includes experiences of physical, emotional/verbal abuse and/or social isolation, may lead to mental health problems, such as depression [61, 62] and OCD [63], suicide experiences, and deaths by suicide [64]. Of note, the current study expands upon this line of research by investigating the impact of the perceptions of adverse childhood relationships with the significant others, including peers, guardians, and teachers and confirmed that perceptions of such unpleasant and negative social relationships have pernicious consequences on mental health [50]. Our findings are also consistent with recent meta-analyses which have shown that core forms of childhood maltreatment by adults, especially sexual and physical abuse, is strongly linked with mental health problems, involving mood, anxiety, substance use [65, 66], suicide experiences [17, 18], and non-suicide self-harm [67]. However, it must be stressed that current evidence suggests that experiences of peer victimization may have worse long-term effects on mental health in adulthood than having experienced any forms of abuse and/or neglect in childhood by adults, which is in accord with our findings [50].
One of the main objectives of this study was to examine whether symptoms of depression and OCD comprised key mediators in the pathways to suicide ideation and behaviors in those reporting adverse social relationships with significant others in childhood. In accord with our prediction, the third important finding of this study, again from both theoretical and clinical perspectives, was that perceptions of adverse social relationships in childhood, particularly with peers, were associated with suicide ideation and behaviors, both directly but also indirectly, and partially mediated by depression and OCD. However, it should be noted that perceptions of adverse relationships with both guardians and teachers were fully mediated by depression and OCD. This means that although such adverse events were not directly linked with suicide experiences, they were associated with common mental health problems, which, in turn, were associated with suicide ideation and behaviors. This finding corroborates a recent study showing that a number of mental health problems mediated associations between childhood maltreatment and suicide acts [49]. It is also consistent with a broad literature indicating that adverse parental and/or school practices in childhood may result in mental health problems in adult life [68,69,70,71]. Interestingly, this is the first study to link the perceptions of adverse social interactions in childhood from peers, guardians and teachers which are common-place (e.g., negative comments about people’s bodies; bullying) to suicide thoughts and behaviors experienced as an adult, via depression and OCD also experienced as an adult.
Although we speculate that these effects may be accentuated if similar models are tested within those with a clinically diagnosed mental health problems who most likely have experienced more pronounced adverse social childhood interactions and manifest more severe symptoms of psychological mental health problems [72], the important point is that mental health professionals should explore with their clients experiences of less extreme childhood social adversities and the consequences of these types of adversities on depression, different types of anxiety, and suicide experiences. Recent studies have proposed a myriad of factors, some of which are somewhat general, that may be important in understanding suicide experiences and could, therefore, influence the association between childhood adversities, mental health problems and suicide thoughts and behaviors. These factors include socio-economic deprivation [73], gene alterations [74]; neuropsychiatric problems in late-life [75]; functional impairment in older age [76]; less adaptive coping strategies [77]; emotional dysregulation [78], impaired decision making [79] and, relatedly, low social support [80]. To progress, it is essential to develop testable biopsychosocial models of the specific pathways arising from a continuum of negative adverse social interactions in childhood which affect the development of suicide thoughts and behaviors experienced as a consequence of those adversities. Currently, contemporary psychological models of the psychosocial pathways to suicide thoughts, plans and acts do not focus specifically on the different roles that a diverse range of adverse social interactions in childhood may have on the development and amplification of suicide experiences [81,82,83,84]. The work presented in the current study was quantitative in nature and cross-sectional. We encourage future work to use convergent methodologies to examine such pathways with cross-sectional [85], prospective [62], micro-longitudinal (e.g., experience sampling, diaries) [86], qualitative [87], and mixed methods designs [88].
Limitations
These findings should be interpreted within the context of four main limitations. First, all data were collected concurrently, at one time point. This prohibits us from drawing causal conclusions or those based on temporal relationships because it was not possible to test whether adverse social relationships were formed before the development of the symptoms of depression, OCD or engagement in suicide ideation and behaviors. Although it seems plausible for experiences of childhood adversities to have preceded the development of mental health problems and suicide ideation and behaviors, this should be investigated explicitly. Qualitative work which explores people’s experiences of suicide thoughts, plans and acts in relation to perceptions of childhood adverse social interactions seem particularly germane. Indeed, qualitative work with those who have suicide experiences can be particularly insightful, from pragmatic, clinical and theoretical perspectives [89,90,91]. Second, and based on the argument that suicide may be depicted as a continuum, albeit a dynamic one, ranging from suicide ideation, to urges, plans and attempts, and then suicide fatalities [92], the overall scores of the suicide behaviors’ questionnaire-revised (SBQ-R) were utilized. Future work should focus on disentangling distinct modes of suicide experiences, for example, thoughts, plans, urges, attempts, frequency and severity, in relation to the effects of childhood adverse social interactions on these different types of suicide experiences. Third, our sample size was well powered. However, it was not well balanced in terms of demographic characteristics such as the nuances of gender identity and sexual orientation [93]. Issues concerning gender identity and sexual orientation have been associated with mental health problems and suicide experiences arising from experiences of harassment and bullying from parents or carers, peers, and schools [94]. We recommend that future studies attempt to characterize gender identity and sexual orientation using terms chosen by participants themselves. A fourth limitation relates to a potential recall bias which refers to the lack of accuracy or correctness of the recollections of the participants’ adverse social relationships in childhood. However, there is evidence suggesting that recall biases do not significantly affect the links between self-reporting childhood experiences and mental health problems [95].
There were two key strengths of this study with associated important clinical implications. First, based on recent findings that people from the general population residing in the community can be severely affected by experiences of childhood abuse and/or neglect [17, 18], we endeavored to examine the association of the perceptions of adverse social relationships in childhood with suicide experiences in a large, representative, community sample. Participants were not selectively recruited who were under the care of mental health professionals. Our findings, that social adversities in childhood were, indeed, associated with suicide thoughts and acts in adulthood in such a diverse sample may be helpful in encouraging the development of efficient interventions targeted at those who are not under the care of mental health services. Second, we conducted two separate mediational analyses, which are considered to be powerful multivariate techniques [49], to examine the direct and indirect pathways to suicide experiences from perceived childhood social adversities. We focused on depression and OCD. Depression and OCD are both common mental health problems which affect people across society [96, 97]. However, the association between OCD and suicide experiences is under-studied [46]. Therefore, that OCD was found to be a mediator in the relationship between childhood social adversities and suicide experiences highlights the importance of examining the role of a range of anxiety problems in the pathways to suicide thoughts and behaviors.
Clinically, these results emphasize the need for targeted suicide prevention priorities with a particular focus on ameliorating the negative impact of adverse everyday social relationships with significant others, including peers, guardians and teachers experienced as a child. Furthermore, and in accord with the extant literature [17, 18, 98], our findings suggest that addressing depression and OCD, especially in those who have experienced social disapproval, criticism and/or lack of social support, constitutes an important step in an effort to prevent and/or attenuate suicide ideation and behaviors.
Summary
This is the first study to examine the link between perceptions of adverse social relationships in childhood with significant others, and common mental health conditions and suicide experiences in later life. Our analyses demonstrated that there were direct, strong associations between the perceptions of overall adverse social relationships, especially with peers, and suicide thoughts and behaviors, which also linked indirectly, via depression and obsessive-compulsive disorder, to suicide experiences. These findings have important implications for clinical practice, the development of appropriate interventions, as well as for raising public and scientific awareness regarding the negative outcomes of experiencing distressing social relationships with significant others as a child.
References
Finkelhor D, Turner HA, Ormond R, Hamby SL (2013) Violence, crime, and abuse exposure in a national sample of children and youth: an update. JAMA Pediatr 167:614–621
Min M, Minnes S, Kim H, Singer L (2013) Pathways linking childhood maltreatment and adult physical health. Child Abuse Negl 37:361–373
Springer K, Sheridan J, Kuo D, Carnes M (2007) Long-term physical and mental health consequences of childhood physical abuse: results from a large population-based sample of men and women. Child Abuse Negl 31:517–530
Cromheeke S, Herpoel L, Mueller S (2014) Childhood abuse is related to working memory impairment for positive emotion in female university students. Child Maltreat 19:38–48
Fuller-Thomson E, Brennenstuhl S, Frank J (2010) The association between childhood physical abuse and heart disease in adulthood: findings from a representative community sample. Child Abuse Negl 34:689–698
Girardet R, Lahoti S, Howard L, Fajman N, Sawyer M, Driebe E, Lee F, Sautter RL, Greenwald E, Beck-Sagué CM, Hammerschlag MR, Black CM (2009) Epidemiology of sexually transmitted infections in suspected child victims of sexual assault. Pediatrics 124:79–86
Hamburger M, Leeb R, Swahn M (2008) Childhood maltreatment and early alcohol use among high-risk adolescents. J Stud Alcohol Drugs 69:291–295
Lewis T, Kotch J, Wiley T, Litrownik A, English D, Thompson R, Zolotor AJ, Block SD, Dubowitz H (2011) Internalizing problems: a potential pathway from childhood maltreatment to adolescent smoking. J Adolesc Health 48:247–252
Kessler R, Mclaughlin K, Green J, Gruber M, Sampson N, Zaslavsky A, Aguilar-Gaxiola S, Alhamzawi AO, Alonso J, Angermeyer M, Benjet C, Bromet E, Chatterji S, De Girolamo G, Demyttenaere K, Fayyad J, Florescu S, Gal G, Gureje O, Haro JM, Hu CY, Karam EG, Kawakami N, Lee S, Lépine JP, Ormel J, Posada-Villa J, Sagar R, Tsang A, Ustün TB, Vassilev S, Viana MC, Williams D (2010) Childhood adversities and adult psychopathology in the WHO World Mental Health Surveys. Br J Psychiatry 197:378–385
Norman R, Byambaa M, De R, Butchart A, Scott J, Vos T, Tomlinson M (2012) The long-term health consequences of child physical abuse, emotional abuse, and neglect: a systematic review and meta-analysis. Plos Med 9:e1001349
Duve SR, Felitti VJ, Dong M, Giles WH, Anda RF (2003) The impact of adverse childhood experiences on health problems: evidence from four birth cohorts dating back to 1900. Prev Med 37:268–277
van Orden KA, Witte TK, Cukrowicz KC, Braithwaite S, Selby EA, Joiner TE Jr (2010) The interpersonal theory of suicide. Psychol Rev 117:575–600
Johnson J, Gooding P, Wood A, Tarrier N (2010) Resilience as positive coping appraisals: testing the schematic appraisals model of suicide (SAMS). Behav Res Ther 48:179–186
O’Connor RC, Nock MK (2014) The psychology of suicidal behaviour. Lancet Psychiatry 1:73–85
Tarrier N, Haddock G, Lewis S, Drake R, Gregg L (2006) Suicide behaviour over 18 months in recent onset schizophrenic patients: the effects of CBT. Schizophr Res 83:15–27
World Health Organization (2018) Preventing suicide: a global imperative. https://www.who.int/mental_health/prevention/suicide/suicideprevent/en/
Angelakis I, Gillespie EL, Panagioti M (2019) Childhood maltreatment and adult suicidality: a comprehensive systematic review with meta-analysis. Psychol Med 49:1057–1078
Angelakis I, Austin JL, Gooding P (2020) Association of childhood maltreatment with suicide behaviors among young people: a systematic review and meta-analysis. JAMA Netw Open 3(8):e2012563
Angelakis I, Austin J, Gooding P (2019) Childhood maltreatment and suicide attempts in prisoners: A systematic meta-analytic review. Psychol Med 50:1–10
Faust J, Runyon M, Kenny M (1995) Family variables associated with the onset and impact of intrafamilial childhood sexual abuse. Clin Psychol Rev 15:443–456
Li Q (2006) Cyberbullying in schools: a research of gender differences. Sch Psychol Int 27:157–170
Gelles RJ (1991) Physical violence, child abuse, and child homicide. Hum Nat 2:59–72
Dong M, Anda R, Felitti V, Dube S, Williamson D, Thompson T, Loo CM, Giles W (2004) The interrelatedness of multiple forms of childhood abuse, neglect, and household dysfunction. Child Abuse Negl 28:771–784
Angelakis I, Austin JL, Slater C, Roderique-Davies G (2018) Experiencing adverse social relationships: the development and validation of a self-report scale that measures individuals’ histories of social punishment (HoSP). J Psychopathol Behav Assess 40:355–365
Ingram KM, Betz EB, Mindes EJ, Schmitt MM, Smith NG (2001) Unsupportive responses from others concerning a stressful life event: development of the unsupportive social interactions inventory. J Soc Clin Psychol 20:173–207
Arseneault L, Bowes L, Shakkor S (2010) Bullying victimization in youths and mental health problems: “Much ado about nothing”? Psychol Med 40:717–729
Faith MS, Leone MA, Ayers TS, Heo M, Pietrobelli A (2002) Weight criticism during physical activity, coping skills, and reported physical activity in children. Pediatrics 110:e23
Holm KE, Bowler RP, Make BJ, Wamboldt FS (2009) Family relationship quality is associated with psychological distress, dyspnea, and quality of life in COPD. COPD 6:359–368
Frank E, Carrera JS, Stratton T, Bickel J, Nora LM (2006) Experiences of belittlement and harassment and their correlates among medical students in the United States: longitudinal survey. BMJ 333:682
Baldwin DC, Daugherty SR, Eckenfels EJ (1991) Student perceptions of mistreatment and harassment during medical school: a survey of ten United States schools. West J Med 155:140–145
Hawker DS, Boulton MJ (2000) Twenty years’ research on peer victimization and psychosocial maladjustment: a meta-analytic review of cross-sectional studies. J Child Psychol Psychiatry 41:441–455
Modecki K, Minchin J, Harbaugh A, Guerra N, Runions K (2014) Bullying prevalence across contexts: a meta-analysis measuring cyber and traditional bullying. J Adolesc Health 55:602–611
Gini G, Espelage D (2014) Peer victimization, cyberbullying, and suicide risk in children and adolescents. JAMA Psychiatry 312:545–546
Sweeting H, Young R, West P, Der G (2006) Peer victimization and depression in early–mid adolescence: a longitudinal study. Br J Educ Psychol 76:577–594
Topol P, Reznikoff M (1982) Perceived peer and family relationships, hopelessness and locus of control as factors in adolescents and suicide attempts. Suicide Life Threat Behav 12:141–150
Baker J, Grant S, Morlock L (2008) The teacher-student relationship as a developmental context for children with internalizing or externalizing behaviour problems. Sch Psychol Q 23:3–15
Merrick M, Ports K, Ford D, Afifi T, Gershoff E, Grogan-Kaylor A (2017) Unpacking the impact of adverse childhood experiences on adult mental health. Child Abuse Negl 69:10–19
Fullana MA, Vilagut G, Rojas-Far-Reras S, Mataix-Cols D, De Graff R, Demyt-Tenaere K et al (2000) Obsessive-compulsive symptoms dimensions in the general population: results from an epidemiological study in six European countries. J Affect Disord 124:291–299
Kessler R, Chiu W, Demler O, Merikangas K, Walters E (2005) Prevalence, severity, and comorbidity of 12-month DSM-IV disorders in the National Comorbidity Survey Replication. Arch Gen Psychiatry 62:617–627
Angelakis I, Gooding P (2020) A novel tool showing that perceptions of adverse social relationships in childhood were linked with mental health problems and suicidal experiences: validation of the English version of the history of social punishment (HoSP) scale. Psychiatry Res 285:112807
Barcaccia B, Tenore K, Mancini F (2015) Early childhood experiences shaping vulnerability to obsessive-compulsive disorder. Clin Neuropsychiatry 12:141–147
Briggs E, Price I (2009) The relationship between adverse childhood experience and obsessive-compulsive symptoms and beliefs: the role of anxiety, depression, and experiential avoidance. J Affect Disord 23:1037–1046
Bernal M, Haro J, Bernert S, Brugha T, de Graaf R, Bruffaerts R, Lépine JP, de Girolamo G, Vilagut G, Gasquet I, Torres JV, Kovess V, Heider D, Neeleman J, Kessler R, Alonso J (2007) Risk factors for suicidality in Europe: results from the ESEMED study. J Affect Disord 101:27–34
Kanwar A, Malik S, Prokop LJ, Sim LA, Feldstein D, Wang Z, Murad MH (2013) The association between anxiety disorders and suicidal behaviors: a systematic review and meta-analysis. Depress Anxiety 30:917–929
Angelakis I, Gooding P, Panagioti M (2016) Suicidality in body dysmorphic disorder (BDD): A systematic review with meta-analysis. Clin Psychol Rev 49:55–66. https://doi.org/10.1016/j.cpr.2016.08.002
Angelakis I, Gooding P, Tarrier N, Panagioti M (2015) Suicidality in obsessive compulsive disorder (OCD): A systematic review and meta-analysis. Clin Psychol Rev 39:1–15. https://doi.org/10.1016/j.cpr.2015.03.002
Lochner C, du Toit P, Zungu-Dirwayi N, Marais A, van Kradenburg J, Seedat S, Niehaus DJ, Stein DJ (2002) Childhood trauma in obsessive-compulsive disorder, trichotillomania, and controls. Depress Anxiety 15:66–68
Mathews C, Kaur N, Stein M (2008) Childhood trauma and obsessive-compulsive symptoms. Depress Anxiety 25:742–751
McKenna AE, Gillen AMC (2016) Direct and indirect effects of maltreatment typologies on suicidality in a representative Northern Irish sample: psychopathology only partially mediates the relationship. J Psychiatr Res 72:82–90
Lereya S, Copeland W, Costello E, Wolke D (2015) Adult mental health consequences of peer bullying and maltreatment in childhood: two cohorts in two countries. Lancet Psychiatry 2:524–531
Office for National Statistics (2018) Effects of taxes and benefits on the UK household income – flash estimate: FINANCIAL year ending 2018. Office for National Statistics, London
Radloff LS (1977) The CES-D Scale: A self-report depression scale for research in the general population. Appl Psychol Meas 1:385–401
Foa EB, Huppert JD, Leiberg S, Langner R, Kichic R, Hajcak G et al (2002) The obsessive-compulsive inventory: development and validation of a short version. Psychol Assess 14:485–496
Osman A, Bagge CL, Gutierrez PM, Konick LC, Kopper BA, Barrios FX (2001) The suicidal behaviors questionnaire-revised (SBQ-R): validation with clinical and nonclinical samples. Assessment 28:443–454
Thorndike RM (1994) Correlational procedures in data analysis. In: Husen T, Postlethwaite N (eds) International encyclopedia of education, 2nd edn. Pergamon, New York, pp 1107–1117
MacKinnon DP (2008) Introduction to statistical mediation analysis. Lawrence Erlbaum Associates, Mahwah
Preacher KJ, Hayes AF (2008) Asymptotic and resampling strategies for assessing and comparing indirect effects in multiple mediator models. Behav Res Methods 40:879–891
Selvi Y, Besiroglu L, Aydin A et al (2012) Relations between childhood traumatic experiences, dissociation, and cognitive models in obsessive compulsive disorder. Int J Psychiatry Clin Pract 16:53–59
Someshwar A, Bharath H, Preeti A, Thomas A, Jose A, Joseph B, Birudu R, et al (2019) Adverse childhood experiences in families with multiple members diagnosed to have psychiatric illnesses. BioRxiv. http://search.proquest.com/docview/2392879848/
Goldsmith RF, Freyd JJ, DePrince AP (2009) To add insight to injury: Childhood abuse, abuse perceptions, and the emotional and physical health of young adults. J Aggress Maltreatment Trauma 18:350–366
Stapinski L, Bowes L, Wolke D, Pearson R, Mahedy L, Button K, Lewis G, Araya R (2014) Peer victimization during adolescence and risk for anxiety disorders in adulthood: a prospective cohort study. Depress Anxiety 31:574–582
Zwierzynska K, Wolke D, Lereya T (2013) Peer victimization in childhood and internalizing problems in adolescence: a prospective longitudinal study. J Abnorm Child Psychol 41:309–323
Storch EA, Ledley DR, Lewin AB, Murphy TK, Johns NB, Goodman WK, Geffken GR (2006) Peer victimization in children with obsessive–compulsive disorder: relations with symptoms of psychopathology. J Clin Child AdolescPsychol 35:446–455
Klomek A, Sourander A, Niemelä S, Kumpulainen K, Piha J, Tamminen T, Almqvist F, Gould M (2009) Childhood bullying behaviors as a risk for suicide attempts and completed suicides: a population-based birth cohort study. J Am Acad Child Adolesc Psychiatry 48:254–261
Carr CP, Martins CMS, Stingel AM, Lemgruber VB, Juruena MF (2013) The role of early life stress in adult psychiatric disorders: a systematic review according to childhood trauma subtypes. J Nerv Ment Dis 201:100–1020
Lindert J, von Ehrenstein OS, Grashow R, Gal G, Braehler E, Weisskofp MG (2014) Sexual and physical abuse in childhood is associated with depression and anxiety over the life course: systematic review and meta-analysis. Int J Public Health 59:359–372
Liu RT, Scopelliti KM, Pittman SK, Zamora AS (2018) Childhood maltreatment and non-suicidal self-injury: a systematic review and meta-analysis. Lancet Psychiatry 5:51–64
Hyman I (1990) Reading, writing and the hickory stick: the appalling story of physical and psychological abuse of American school children. Lexington Books, Lexington, MA
Hyman IA, Perone DC (1998) The other side of school violence: educator policies and practices that may contribute to student misbehavior. J Sch Psychol 36:7–27
Hyman I, Clarke J, Erdlen R (1987) An analysis of physical abuse in American schools. Aggress Behav 13:1–7
Nickerson A, Bryant RA, Aderka IM, Hinton DE, Hofmann SG (2013) The impacts of parental loss and adverse parenting on mental health: findings from the National Comorbidity Survey-Replication. Psychol Trauma 5:119–127
Martin M, Dykxhoorn J, Afifi T, Colman I (2016) Child abuse and the prevalence of suicide attempts among those reporting suicide ideations. Soc Psychiatry Psychiatr Epidemiol 51:1477–1484
Wickham S, Taylor P, Shevlin M, Bentall RP (2014) The impact of social deprivation on paranoia, hallucinations, mania and depression: the role of discrimination social support, stress and trust. Plos One 9:e105140
Bani-Fatemi A, Howe AS, De Luca V (2014) Epigenetic studies of suicidal behaviour. Neurocase 21:134143
Gershon A, Sudheimer K, Tirouvanziam R, Williams L, O’Hara R (2013) The long-term impact of early adversity on late-life psychiatric disorders. Curr Psychiatry Rep 15:19
Draper BM (2014) Suicidal behaviour and suicide prevention in later life. Maturitas 79:179183
Valle LA, Silovsky JF (2002) Attributions and adjustment following child sexual and physical abuse. Child Maltreat 7:924
Palmier-Claus JE, Taylor PJ, Gooding P, Dunn G, Lewis SW (2012) Affective variability predicts suicidal ideation in individuals at ultra-high risk of developing psychosis: an experience sampling study. Br J Clin Psychol 51:72–83
Jollant F, Guillaume S, Jaussent I, Castelnau D, Malafosse A, Courtet P (2007) Impaired decision-making in suicide attempters may increase the risk of problems in affective relationships. J Affect Disord 99:59–62
Panagioti M, Gooding P, Taylor P, Tarrier N (2014) Perceived social support buffers the impact of PTSD symptoms on suicidal behaviour: implications into suicide resilience research. Compr Psychiatry 55:104–112
Johnson J, Gooding P, Tarrier N (2008) Suicide risk in schizophrenia: explanatory models and clinical implications. Psychol Psychother 81:55–77
Klonsky ED, May AM (2015) The three-step theory (3ST): a new theory of suicide rooted in the “Ideation-to-Action” framework. Int J Cogn Ther 8:114–129
O’Connor RC, Kirtley OJ (2018) The integrated motivational-volitional model of suicidal behaviour. Philos Trans R Soc Lond B Biol Sci 373:20170268
O’Connor RC, Portzky G (2018) Looking to the future: a synthesis of new developments and challenges in suicide research and prevention. Front Psychol 9:2139
Klumparendt A, Nelson J, Barenbrügge J, Ehring T (2019) Associations between childhood maltreatment and adult depression: a mediation analysis. BMC Psychiatry 19:1–11
Dautovich ND, Dzierzewski JM, Gum AM (2014) Older adults display concurrent but not delayed associations between life stressors and depressive symptoms: a micrologitudinal study. Am J Geriatr Psychiatry 22:1131–1139
Owen R, Gooding P, Dempsey R, Jones SH (2017) The reciprocal relationships between social factors and the experience of bipolar disorder: a qualitative investigation. Clin Psychol Psychother 24:911–918
Holland K, Vivolo-Kantor A, Logan J, Leemis R (2017) Antecedents of suicide among youth aged 11-15: a multistate mixed methods analysis. J Youth Adolesc 46:1598–1610
Awenat YF, Moore C, Gooding PA, Ulph F, Mirza A, Pratt D (2018) Improving the quality of prison research: a qualitative study of ex-offender service user involvement in prison suicide prevention research. Health Expect 21:100–109
Littlewood D, Gooding P, Kyle SD, Pratt D, Peters S (2016) Understanding the role of sleep in suicide risk: qualitative study of patient perspectives. BMJ 6:e012113
Owen R, Gooding P, Dempsey R, Jones S (2015) A qualitative investigation into the relationships between social factors and suicidal thoughts and acts experienced by people with a bipolar disorder diagnosis. J Affect Disord 176:133–140
Mann JJ, Waternaux C, Haas GL, Malone KM (1999) Toward a clinical model of suicide behaviour in psychiatric patients. Am J Psychiatry 156:181–189
Diamond LM, Butterworth M (2008) Questioning gender and sexual identity: dynamic links over time. Sex Roles 59:365–376
Mustanski B, Garofalo R, Emerson E (2010) Mental health disorders, psychological distress, and suicidality in a diverse sample of lesbian, gay, bisexual, and transgender youths. Am J Public Health 100(12):2426–2432
Fergusson DM, Horwood LJ, Boden JM (2011) Structural equation modeling of repeated retrospective reports of childhood maltreatment. Int J Methods Psychiatr Res 20:93–104
Richards D (2011) Prevalence and clinical course of depression: a review. Clin Psychol Rev 31:1117–1125
Ruscio AM, Stein DJ, Chiu WT, Kessler RC (2010) The epidemiology of obsessive-compulsive disorder in the national comorbidity survey replication. Mol Psychiatry 15:53–63
Rihmer Z (2001) Can better recognition and treatment of depression reduce suicide rates? A brief review. Eur Psychiatry 16:406–409
Acknowledgements
The authors would like to thank Matilda Angelaki for comments that greatly improved the manuscript
Funding
No financial support has been received.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
All authors declare no conflict of interest.
Ethical Approval
All procedures performed in this study were in accordance with the ethical standards of the institutional (REF No: 1905172.1) and/or national research committee and with the 1964 Helsinki declaration and its later amendments or comparable ethical standards.
Informed Consent
Informed consent was obtained from all individual participants included in the study.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Angelakis, I., Gooding, P. Adverse Social Relationships in Childhood: Are there Links with Depression, Obsessive-Compulsive Disorder and Suicidality in Adulthood?. Child Psychiatry Hum Dev 52, 945–956 (2021). https://doi.org/10.1007/s10578-020-01077-3
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10578-020-01077-3