Abstract
Parkinson Disease (PD) is one of the most common neurodegenerative disorders characterized by loss of dopaminergic neurons involved in motor functions. Growing evidence indicates that gut microbiota communicates with the brain known as the gut-brain axis (GBA). Mitochondrial toxin 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) is commonly used in animal studies to investigate the GBA in PD. Various MPTP administration regimens are performed in PD mouse models involving one to multiple injections in 1 day or one injection per day for several days. The aim of this study is to investigate if the impact of MPTP on gut microbiota differs depending on the administration regimen. C57BL/6 mice were treated with acute or subchronic regimens of MPTP. Motor functions were assessed by open-field, catalepsy, and wire hanging tests. The cecum and the brain samples were obtained for microbiota and gene expression analyses, respectively. MPTP administration regimens differed in their ability to alter the gut microbiota. Firmicutes and Bacteroidota were both increased in subchronic mice while did not change and decreased, respectively, in acute mice. Verrucomicrobiota was elevated in acute MPTP mice but dropped in subchronic MPTP mice. Muribaculaceae was the predominant genus in all groups but acute mice. In acute mice, Akkermansia was increased and Colidextribacter was decreased; however, they showed an opposite trend in subchronic mice. These data suggest that MPTP mouse model cause a gut microbiota dysbiosis in an administration regimen dependent manner, and it is important to take consideration of mouse model to investigate the GBA in neurodegenerative diseases including PD.
Graphical Abstract

Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Parkinson Disease (PD) is one of the rapidly growing neurological disorders which are the most common cause of disability in the world (Dorsey and Bloem 2018; Maserejian et al. 2020). Incidence of PD increases with age, and around 4% of the patients has been diagnosed even before age 50 (Foundation 2021; Medicine 2021). PD is described by loss of dopaminergic neurons, which causes motor dysfunction such as postural instability, bradykinesia, resting tremor, and rigidity (Taylor et al. 2013; Li et al. 2017). This neuronal degeneration is associated with several factors including increase in inflammatory cytokines, mitochondrial dysfunction, and oxidative stress.
Although PD is defined by motor impairments, non-motor symptoms such as sleep disorders, cognitive impairment, leaky gut syndrome, and defecation dysfunction have been observed in PD patients as well (Lindqvist et al. 2012; Schapira et al. 2017). Constipation is one of the non-motor manifestations reported the most frequently (Hopfner et al. 2017; Houser et al. 2018). Over 50% of the PD patients have been found to suffer from constipation and moreover, the gastrointestinal symptoms have found to be developed several years before onset of motor symptoms (Houser et al. 2018). Therefore, it has been thought that an early involvement of gastrointestinal dysfunction is a possible presymptomatic phase of PD (Schapira et al. 2017). PD treatments that mostly include dopamine supplementation targeting motor symptoms only provide a symptomatic relief and the effect is very short-lived. (Biju et al. 2018). They may lead to drug resistant-motor symptoms along with the drug side effects. Moreover, it has been reported that no pharmacologic agent delaying or preventing the disease progression has been approved yet (Armstrong and Okun 2020). Discovery and development of alternative therapeutic strategies, therefore, are need to be considered.
Emerging pieces of evidence suggest that gut microbiota communicates with the brain via the GBA (Pellegrini et al. 2018; Santos et al. 2019; Rani and Mondal 2021). Disruption of the gut-brain interaction has shown to be linked to several neurodegenerative disorders including PD (Morais et al. 2021). Studies with fecal samples collected from PD patients and matched controls reported that gut microbiota has been altered in the PD patients compared to the healthy individuals (Unger et al. 2016; Hill-Burns et al. 2017; Sun et al. 2018). Moreover, intestinal permeability increased in people with PD (Hasegawa et al. 2015; Schwiertz et al. 2018).
In-vivo studies demonstrated that gut microbial dysbiosis is not only found in human studies, but also in various animal models of neurodegenerative diseases (Ellett et al. 2016; Lai et al. 2018; Sun et al. 2018). PD rat model induced by rotenone revealed that microbial alterations in both small and large intestine are relatively consistent with the alterations in the gut microbial composition found in PD patients (Johnson et al. 2018). In a study where germ-free and α-syn overexpressing mice were received fecal microbiota transplantation (FMT) from PD patients, PD driven microbiota induced motor dysfunction in mice and intestinal microbiota was suggested to impact the movement disorders (Sampson et al. 2016). In another study with α-syn overexpressing mice, environment of the proinflammatory gut microbiota triggered PD pathogenesis (Gorecki et al. 2019). Furthermore, FMT from healthy donors in 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP)-induced mouse model of PD reduced gut dysbiosis and improved motor impairment and dopamine deficiency (Sun et al. 2018).
Animal models are commonly employed to explore the mechanisms of PD, to understand the GBA, and to screen potential therapeutics for PD progression. Since MPTP was discovered as a byproduct of a meperidine analog, producing similar symptoms as idiopathic PD in human, it has been reported as a neurotoxin for nigrostriatal dopaminergic neurons (Langston et al. 1983; Ko and Bezard 2017; Hwang et al. 2019). Among various animal models, MPTP model does not require surgery or experimental technology and yields a reproducible dopaminergic damage in nigrostriatal pathway. MPTP, therefore, provides one of the most purposive approaches to investigate critical aspects of PD in animal models and has been widely used as an agent to induce PD like symptoms to explore the progression of the disease as well as developing symptomatic and neuroprotective drugs (Lai et al. 2018; Fang et al. 2019; Liu et al. 2021). MPTP is a neurotoxin precursor of 1-methyl-4-phenylpyridinium (MPP +) that induces neurodopaminergic cell death mostly in striatum and SNc, similar to that seen in patients with PD (Prasad and Hung 2020). Since MPTP can crosses the blood–brain barrier after systemic administration due to its lipophilic nature, MPTP provides a big advantage to be used in animal studies (Jagmag et al. 2016). MPTP, after converted to MPP + , enters the dopaminergic neurons mediated by the dopamine transporter (Dat) and leads to neuronal damage. MPTP quickly kills dopaminergic neuronal cells at first, however can, over time, continue causing cell death. The number of reviews and research papers on MPTP mouse models for PD has steadily increased over the past decades. Recently in-vivo gut microbiota studies for PD also have been performed with MPTP; however, there have been conflicting reports for the alteration of bacterial populations in MPTP-induced mouse models including Firmicutes, Proteobacteria, Lachnospiraceae, Bacteroidetes, Akkermansia, Lactobacillus, and Bacteroides which were increased in some studies while decreased in others (Lai et al. 2018; Sun et al. 2018, 2021; Fang et al. 2019; Pu et al. 2019; Liao et al. 2020; Liu et al. 2021; Wang et al. 2021, 2022).
Various MPTP administration regimens are used ranging from acute intoxication, involving one to multiple injections in 1 day, to subchronic or chronic intoxication schedule corresponding to one injection per day for several days or weeks (Prasad and Hung 2020). In some studies, the toxin is delivered with a minipump for a month or longer (Fornai et al. 2005; Meredith and Rademacher 2011). It is known that procedures of MPTP administration to mice could yield different results varying in neurotoxic effect of MPTP, forming inclusion bodies, and recovery time, depending on timing and dose regimens (Kuroiwa et al. 2010; Meredith and Rademacher 2011; Huang et al. 2017).
Administration protocols differed in time and dose affect the magnitude of lesion and recovery rate and reveal different parkinsonian pathophysiological events (Kuroiwa et al. 2010; Meredith and Rademacher 2011; Huang et al. 2018). Moreover, several other factors including mouse strain, age, sex, and body weight impact the MPTP effectivity and sensitivity (Jackson-Lewis and Przedborski 2007; Kuroiwa et al. 2010; Huang et al. 2017). Studies on gut microbiota with MPTP-induced mouse model of PD also comprise different injection schedules varying from days to weeks and mice at different age (Lai et al. 2018; Fang et al. 2019; Pu et al. 2019; Sun et al. 2021).
This study aims to administer acute and subchronic MPTP to mice with same strain, sex, and age, receiving the same diet, and to determine regimen-induced alteration in the gut microbiota. To demonstrate the success of PD animal model, the expression of tyrosine hydroxylase (Th) which is involved in dopamine production and considered as a marker of dopaminergic neurons were evaluated as well as Dopamine receptor (Drd) and Dat genes taking role in dopamine binding and transport, respectively (Taylor et al. 2013; Liu et al. 2014; Li et al. 2017; Parashar and Udayabanu 2017).
The significance of the study lies in that a better understanding of the administration schedule of MPTP in PD mouse models will benefit studies developing microbiota-associated therapeutic strategies for PD.
Material and Methods
Animals
The procedures containing mice were reviewed and approved by the Local Ethics Committee for Animal Experiments with the protocol #311 (Kobay D.H.L. A.S., Ankara, Turkey). Eight to ten-week-old, healthy male C57BL/6 mice were received from and group housed at Kobay D.H.L. A.S facility. Mice were fed same water and mouse chow ad-libitum throughout the study and housed under a 12 h light/dark cycle with controlled temperature (22 ± 2 °C) and humidity (65–70%). A week after acclimation to their surroundings in testing room, mice (n:24) were randomly assigned to the following groups; Acute MPTP, Subchronic MPTP and their respective controls and housed as one in each cage.
MPTP Administration
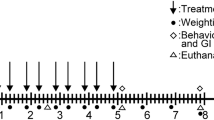
All mice except the control groups were administered an intraperitoneal injection of MPTP hydrochloride (MedChemExpr, USA, Cat# HY-15608) with two different procedures: acute dosing regimen or subchronic dosing regimen. Acute mice were injected (i.p.) 18 mg/kg MPTP-HCl four times at 2 h interval, while Subchronic mice were received (i.p.) 30 mg/kg MPTP-HCl daily for 5 consecutive days (Huang et al. 2018; Haque et al. 2021). Control group of the corresponding regimen was received equal volume of saline with the same procedure. No blinding was performed when the mice were injected. All mice were killed at the end of the experimental period, 7 days after the first injection (Supplementary Fig. 1).
Behavioral Tests for Motor Functions
After training and preadaptation, open-field, catalepsy, and wire hanging tests were performed every other day until they were killed. In order to be consistent, tests were applied at the same time with the same order. Each set up was cleared all mouse feces away and cleaned by 70% EtOH between each mouse.
Open Field
The open-field test was performed to test general locomotor activity and exploratory behavior of the mice (Biju et al. 2018; He et al. 2018). Briefly, each mouse was placed in the middle of a squared plexiglass box (40 × 40x40 cm) with white floor and allowed to freely move for 10 min while being monitored by an overhead camera. The records were analyzed using an animal tracking software (ToxTrac) (Rodriguez et al. 2018). Total distance traveled (mm) during the observation period and average speed (mm/s) were reported. Data of two mice on the day six are missing due to COVID-19 pandemic restrictions.
Catalepsy Bar Test
A standard bar test was performed to evaluate the catalepsy (Bhattacharjee et al. 2016). The mice were positioned individually with forelimbs on a 4 cm-high horizontal bar and the maintenance time of the posture with fore/hindlimbs was recorded in seconds. The cut-off time was 180 s.
Wire Hanging Test
A wire gripping test was performed to assess whole body force (Feng et al. 2018). Mice were suspended from a horizontal wire (30 cm high) by their forelimbs. Each mouse was scored from 1 to 4 based on the number of fore/hindlimbs used for gripping. Falling from the wire was scored as 0. The maximum time allowed was 60 s.
Sample Collection
After killing, the cecum content, as identified by its homogeneous characteristics, was immediately placed on ice, and then kept at − 20 °C until processed for microbial DNA isolation. Specimens of striatum were dissected rapidly and preserved in RNAlater (Ambion, CA, Cat# AM7020) at 4 °C overnight for RNA extraction. After the overnight treatment, the samples were stored at − 80 °C until processing.
Gene Expression Analysis
Weighed brain tissue samples were homogenized in ultra-pure-guanidine isothiocyanate (Sigma-Aldrich, Cat# 50,983) using innuSPEED Lysis Tubes P in SpeedMill Plus (Analytik Jena, Germany, Cat# 845-CS-1020250). RNA was isolated using Pure Link RNA mini kit (Invitrogen, Cat# 12183018A) as recommended by the manufacturer. DNA contamination was removed using PureLink™ DNase Set (Invitrogen, Cat# 10,977,035). RNA purity and the concentrations were determined using a NanoDrop spectrophotometer (Epoch, BioTek) and total RNA was converted into cDNA using High-Capacity cDNA Reverse Transcription Kit (Applied Biosystems, Cat# 4,368,814) according to supplier’s protocol. Quantitative PCR (qPCR) was performed using with the primers shown at Supplementary Table 1. AMPIGENE qPCR Green Mix Hi-ROX (Enzo Life Sciences, Cat# ENZ-NUC104) was used under the following conditions: 95 °C for 2 min for initial denaturation, followed by 5 s (40 cycles) at 95 °C and 30 s at 57 °C. Data were generated in the final step at 95 °C for 15 s and melting curves (65 to 95 °C) were acquired at the end for each primer set. Relative gene expression was calculated by 2−ΔΔCt method by normalizing gene expression to β-actin (Aktas et al. 2015). Data were generated for four mice per group and each biological replicate has four technical replicates.
DNA Extraction
After weighing, the cecum content was homogenized in Phosphate-buffered saline (PBS) and total DNA was extracted using the QIAamp Fast DNA Stool-Mini Kit (Qiagen Sciences, MD, Cat# 51,604) as described previously (Aktas et al. 2015). In brief, a mechanical cell-disruption step was performed using 0.1 mm glass-beads (Sigma-Aldrich, Cat# G8893) and samples were exposed to six 1 minute beating at maximum speed using the SpeedMill Plus (Analytik Jena, Germany) with intervals of 2 min on ice.
Afterward, a heat treatment step was performed at 95 °C for 5 min. The DNA was further isolated with the manufacturer’s instructions. DNA was quantified by NanoDrop spectrophotometer (Epoch, BioTek) and used to carry out 16S rRNA sequencing. Data were generated for five mice per group.
Sequencing and Microbiota Analysis
16S rRNA sequencing was performed using the Illumina NovaSeq 6000 at Bmlbosis (Ankara, Turkey). 16S rRNA gene consists of nine hypervariable regions and each region starts with a conserved sequence (Claesson et al. 2010; Yang et al. 2016; Zhang et al. 2018) For library preparation, the V3–V4 region was amplified using specific primers (F5ʹTCGTCGGCAGCGTCAGATGTGTATAAGAGACAGCCTACGGGNGGCWGCAG3ʹ,R-5ʹGTCTCGTGGGCTCGGAGATGTGTATAAGAGACAGGACTACHVGGGTATCTAATCC3ʹ). The Nextera XT index kit (Illumina, San Diego, CA, Cat# FC-131–10) was used to attach unique identifiers to both 5′ and 3′ ends. After PCR products were cleaned up using AMPure XP magnetic beads, the amplicons with equal quantities were pooled. Paired end reads sequenced on NovaSeq 6000 system underwent a quality-filtering and were trimed with quality cut-off of Phred score of 20 by Divisive Amplicon Denoising Algorithm 2 (DADA2). Operational Taxonomic Units (OTUs) were generated using DADA2. Data analysis was assessed in Quantitative Insights Into Microbial Ecology (QIIME2) framework. The sequences were submitted to the Sequence Read Archive (SRA) database with the accession number of PRJNA867416.
Statistical Analysis
Based on a sample size calculation (www.biomath.info/power/index.html) with 80% power (unpaired t-test; α = 0.05) to determine a significant difference between the control and the treatments in dopaminergic neural damage, the sample size in each group was estimated to be five (Du et al. 2001; Sun et al. 2018). Six mice per group were used in the study. Assumptions of normality and homogeneity of variances were tested by the Shapiro–Wilk test for small-sized samples (≤ 50) and Levene’s test, respectively (Supplementary Table 2). Student’s t test was performed for normally distributed values, otherwise, a Wilcoxon Mann–Whitney test was performed for nonparametric data using JMP Pro (SAS Institute Inc., Cary, NC). Data are introduced as the mean ± standard deviation (SD). Statistical difference was ascertained at a P value equal to or less than 0.05. Mauchly’s test was performed to assess the sphericity assumption. For microbiome, the statistical difference between groups was analyzed using the Mont Carlo test, a nonparametric test based on random permutations, in package ade4 generated by R 3.6.1 as described by de Carcer et al. (Chessel et al. 2004; Dray and Dufour 2007; Aguirre de Cárcer et al. 2011; TheRCoreTeam 2013). The statistical differences of the between groups were evaluated with the randtest.between function in package ade4 of R 3.6.1. The zero (0) values were replaced with the limit of detection, which is assessed by the ratio of one to the lowest number of read in the data set. The Benjamini–Hochberg procedure was applied to manage the false-discovery rate. The dominant genera that raised or diminished in abundance were identified by correspondence analysis in package ade4 of R 3.6.1 (Aguirre de Cárcer et al. 2011).
Results
MPTP Administration with Different Schedule Induced Behavioral Deficits
After training for preadaptation, behavioral tests were performed every other day until they were killed. General locomotor activity and exploratory behavior of the mice were tested by the open-field test. To evaluate the catalepsy and whole body force, a standard bar test and a wire gripping test were performed, respectively.
Behavioral deficits of the mice exposed to MPTP under acute or subchronic schedule were detected by open-field, catalepsy, and wire hanging tests. As shown in Fig. 1, MPTP administration with both regimens significantly decreased the locomotor activity in the open-field test with reduced average speed and overall traveled distance in 10 min (acute, t(10) = 2.14479, p = 0.004 for day 2, t(10) = 2.07961, p = 0.001 for day 4, and p = 0.1735 for day 6; subchronic, t(10) = 2.14479, p = 0.0004 for day 2; t(10) = 2.07961, p = < 0.0001 for day 4, and p = 0.0122 for day 6).
MPTP induced behavioral alteration of mice in the open-field locomotion test. Mice in acute regimen groups (A) were injected intraperitoneally (i.p.) 18 mg/kg MPTP-HCl four times at 2 h interval while the mice in subchronic regimen groups (B) were received (i.p.) 30 mg/kg MPTP-HCl daily for 5 consecutive days. Student’s t test for parametric data (day 0, day 2, and day 4 while Wilcoxon Mann–Whitney test was applied for nonparametric data (day 6) (C), representative examples of moving pattern from each group. White bar, Control; Patterned bar, MPTP *p < 0.05: significant differences from the control, (n: 6/group)
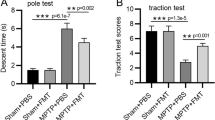
As seen in catalepsy test results, the total time was significantly increased for both acute and subchronic mice (acute, p = 0.0303 for day 2, p = 0.016 for day 4 and day 6; subchronic, p = 0.0055 for day 2, p = 0.0034 for day 4 and day 6) to maintain the posture after the first day of injection relative to their controls (Fig. 2). Meanwhile a large proportion of acute mice started to recover after the day 2, cataleptic symptoms for subchronic mice continued through the experiment.
MPTP induced behavioral alteration of mice in the catalepsy (A) and wire hanging (B) test. Mice in acute regimen groups were injected intraperitoneally (i.p.) 18 mg/kg MPTP-HCl four times at 2 h interval while the mice in subchronic regimen groups were received (i.p.) 30 mg/kg MPTP-HCl daily for 5 consecutive days. Wilcoxon Mann–Whitney test was applied. White bar, Control; Patterned bar, MPTP *p < 0.05: significant differences from the control, (n: 6/group)
In the wire hanging test, it was apparent that the total score of paw/limb placement and hanging time were significantly decreased in both acute and subchronic mice compared to the controls (acute, p = 0.0022 for day 2, p = 0.0025 for day 4, and p = 0.0246 for day 6; subchronic, p = 0.0013 for day 2, day 4, and day 6) (Fig. 2).
MPTP Administration with Different Schedule Affected Striatal Tyrosine Hydroxylase Depletion
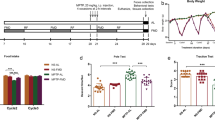
Total RNA was extracted from striatum to screen the alterations in the expression of genes involved in PD pathology resulting from MPTP administration with acute and subchronic regimens. Five genes associated with PD pathology due to MPTP administration were targeted, which are Tyrosine hydroxylase (Th), α-synuclein (α-syn), Dopamine Receptor 1 (Drd1), Dopamine Receptor 2 (Drd2), and Dopamine Transporter (Dat) (Fig. 3). These preliminary gene expression results showed that MPTP at both administration schedule reduced Th and Dat expression relative to the control. However, α-syn and Drd2 showed no differences from the control in the mice administered both acute and subchronic regimens of MPTP. The expression of Drd1 was increased in both regimens.
Fold change in gene expression of Tyrosine hydroxylase (Th), α-synuclein (α-syn), Dopamine Receptor 1 (Drd1), Dopamine Receptor 2 (Drd2), and Dopamine Transporter (Dat) in the striatum of mice administered MPTP or saline. Mice in acute regimen groups were injected intraperitoneally (i.p.) 18 mg/kg MPTP-HCl 4 times at 2 h interval while the mice in subchronic regimen groups were received (i.p.) 30 mg/kg MPTP-HCl daily for 5 consecutive days. Relative gene expression was calculated by 2−ΔΔCt method by normalizing gene expression to β-actin. White bar, Control; Patterned bar, MPTP.(n: 4/group)
MPTP Injection Altered the Cecal Microbiota Composition in an Administration Regimen-Dependent Manner
In this study, to evaluate the impact of MPTP administration with acute and subchronic regimens on the commensal microbiota of PD mice, 16S rRNA sequencing was performed with the cecum digesta sample collected from MPTP induced mice. A total of 1,865,972 filtered reads from cecum content samples of 20 mice were obtained with the number of reads varying from 55,811 to 220,728 and an average of 93,299 reads/sample. Assigning the each read to a taxonomic status resulted in 18 phyla, 25 classes, 59 orders, 95 families, and 212 genera. Chao1 and Shannon index was computed to assess taxonomic diversity (Supplementary Fig. 2). Additionally, a principal coordinate analysis (PCA) plots using weighted Unifrac distances were generated for beta diversity (Supplementary Fig. 3). The cecum microbiota of the mice injected with acute and subchronic regimen of MPTP were evaluated and the MPTP groups were compared with their corresponding controls as well as with each other. A Monte-Carlo test (with 10,000 replicates) was employed to identify the groups that were significantly (p = 0.035 at phylum level; p = 0.001 at genus level) different from each other. While the overall microbiota at phylum and genus level in the MPTP groups differed significantly from each other, the overall microbiota in the control groups did not differ significantly (p = 0.708 at phylum level; p = 0.334 at genus level) from each other (Fig. 4 and 5).
MPTP administration altered the composition of cecal microbiome in mice at phylum level. A Microbial communities of individual mouse cecum content. B Predominant phylum in the cecum microbiome of mice administered MPTP (n: 5 for each bar). C Pair wise comparison of each group. Statistical p-values were assessed using a Monte-Carlo test with 10,000 replicates
The dominant phyla of the cecum microbiota in all samples were Firmicutes and Bacteroidota in rank order, together these phyla comprise 73–92% of the total microbiota (Fig. 4, Supplementary Table 3). The percentage of phylum Firmicutes significantly (Z = − 2.1, p = 0.038) increased in the subchronic mice while did not change in the acute mice (Z = − 0.62, p = 0.23). Interestingly, the percentage of Bacteroidota increased significantly (Z = − 2.5, p = 0.004) in the subchronic MPTP mice while significantly (Z = − 3.5, p = 0.008) decreased in the acute MPTP mice. Similarly, opposite effect has been observed on the abundance of Verrucomicrobiota where increased significantly (Z = 4.6, p = 0.009) in the acute MPTP mice while decreased in the subchronic MPTP mice. Moreover, for both group of MPTP mice, the predominance of Campylobacterota decreased while Patescibacteria increased in abundance.
As shown in the petal diagram (Fig. 6A), 111 core OTUs at genus level were detected in all groups, and the number of unique OTUs in healthy control mice, acute MPTP, and subchronic MPTP mice were 31, 6, and 10, respectively. Muribaculaceae was the most dominant genus in the cecum microbiota of all groups except acute MPTP mice where Akkermansia was the most dominant (Fig. 6B, Supplementary Table 4).
MPTP administration altered the composition of cecal microbiome in an application schedule-dependent manner. A Petal diagram represents the number of core genera and unique genera detected in Control and MPTP mice. B The major microbial communities of mouse cecum content at genus level in the control group and MPTP group. Only genera with over 3% of the total bacteria are presented (n: 5 for each bar)
The dominant genera of the cecum microbiota at genus level in all samples were Muribaculaceae, Akkermansia, and Lachnospiraceae_NK4A136_group in rank order, together these genera comprise 39–49% of the total microbiota (Supplementary Table 4). While the predominance of Muribaculaceae was reduced significantly (Z = − 3.1, p = 0.001) in the mice administered acute regimen of MPTP, it did not change in the mice administered subchronic regimen of MPTP compared to their respective controls. However, the abundance of Akkermansia significantly (Z = 3.2, p = 0.009) increased in the acute MPTP mice while decreased in the subchronic MPTP mice. Similar impact has been observed in Prevotellaceae_NK3B31. The percent of Colidextribacter was changed in a like manner, where decreased in the acute MPTP mice while increased in the subchronic MPTP mice. The abundance of Candidatus_Saccharimonas, Clostridia_UCG-014, and Anaerotruncus increased significantly (Z = 1.7, p = 0.008) in the acute MPTP mice while did not change in the subchronic MPTP mice. In both MPTP groups, the predominance of Prevotellaceae_UCG-001, Intestinimonas, and Lactobacillus increased while Alistipes and Acinetobacter decreased.
Discussion
Here the current study investigated whether the impact of MPTP intoxication for PD mouse model on gut microbiota differs depending on the administration regimen, using acute and subchronic MPTP injected mice. The results demonstrated that MPTP application schedule differed in their ability to alter the gut microbiota. The abundance of Firmicutes and Bacteroidota increased in the subchronic mice while did not change and decreased, respectively, in the acute mice. The predominance of Verrucomicrobiota was lower in the subchronic MPTP mice but higher in the acute MPTP mice. Muribaculaceae was the predominant genus in all groups, however; not in acute mice. The abundance of Akkermansia was lower in the subchronic mice but higher in the acute mice. However, Colidextribacter was higher in the subchronic mice but lower in the acute mice.
The MPTP animal model is the most elaborate model among PD animal models (Dauer and Przedborski 2003; Jackson-Lewis and Przedborski 2007; Kuroiwa et al. 2010; Meredith and Rademacher 2011; Ko and Bezard 2017; Hwang et al. 2019) The MPTP-induced mouse is a valuable tool for studying PD, allowing us a better understanding of the mechanism of PD and the exploration of neurorestorative and neuroprotective strategies associated with the GBA. Studies performed various MPTP administration schedules and different administration procedures, doses, and application times of MPTP have found to produce different pathological conditions of PD (Fornai et al. 2005; Kuroiwa et al. 2010; Meredith and Rademacher 2011; Huang et al. 2017, 2018; Prasad and Hung 2020).
In acute model, MPTP is delivered systemically by repeated injections closely spaced, over a day while in subchronic model, the administration is spread out over multiple days (Fornai et al. 2005; Kuroiwa et al. 2010; Huang et al. 2018). In chronic model, MPTP is administered continuously for days or weeks, sometimes with a mini pump. When mice were treated with MPTP acutely or subchronically, formation of neither Lewy bodies nor inclusion was observed meanwhile α-syn aggregates in mice only treated chronically/continuously for weeks (Fornai et al. 2005; Meredith and Rademacher 2011). Acute and subchronic administration produce a quick loss of dopaminergic neurons and a reduction in striatal Th protein level and recovery time has found to be shorter than the chronic application (Kuroiwa et al. 2010; Meredith and Rademacher 2011; Lai et al. 2018). However, introducing the MPTP continuously leads to a progressive neurodegeneration and neurons continue to die after completing MPTP administration. For a quick dopamine depletion, acute and subchronic models are found to be useful for a cost and time effective trials as compared to the chronic models with continuous MPTP treatment.
Although microbiome studies in animal models of PD has only just began, the results clearly indicate that the gut microbiota in MPTP-induced mice is altered (Fang et al. 2019; Pu et al. 2019; Liu et al. 2021; Sun et al. 2021; Wang et al. 2021). MPTP mouse model of PD, therefore, has been extensively used to understand the GBA and to investigate possible therapeutics for PD. Taking into account the influence of different MPTP application regimens on PD pathology, this study aimed to investigate the impact of acute and subchronic MPTP administration regimens on gut microbiota.
Behavioral tests including open-field, catalepsy, and wire hanging tests were performed every other day until they were killed since the motor dysfunction is one of the significant characteristics of PD, reflecting the dopamine depletion (Taylor et al. 2013; Li et al. 2017). The injection of MPTP with both regimens impaired the ability of mice to show normal locomotor activity, exploratory behavior, and posture maintaining in a regimen-dependent manner. These behavioral findings are consistent with the motor symptoms in MPTP-induced PD mice models and indicate that mice responded to MPTP administration.
After the mice were killed, the brain tissues were collected for gene expression analysis. Depletion of dopamine is one of the most significant pathological changes in PD and Th, which is a rate-limiting enzyme of dopamine synthesis, takes an important role in this pathology (Taylor et al. 2013; Li et al. 2017). Th, therefore, has been considered as a marker of dopaminergic neurons and used to confirm the success of PD animal model in studies investigating PD pathology and developing potential therapeutics for PD progression (Lu et al. 2018; Jeon et al. 2021). Reduction in Th expression showed that both regimen impaired the dopamine synthesis and produced PD animal model. Dopamine transporter (Dat) is responsible for dopamine uptake and definitive in the clinical diagnosis of PD (Liu et al. 2014). Reduction in striatal Dat expression in MPTP mice indicates the pathophysiology of PD resulting from loss of dopaminergic neurons. Dopamine receptors are divided into two different groups as D1 like receptors including Drd1 and Drd5 and D2 like receptors including Drd2, Drd3, and Drd5 (Al Sweidi et al. 2013). The majority of dopamine receptors in the striatum consist of Drd1 and Drd2. In acute regimen, none of the dopamine receptors targeted in this study were modulated while in subchronic regimen, the expression of dopamine receptors tested was increased. The modulation in the level of dopamine receptors is reported to be controversial in PD model of animal as well as patients with PD and increase, decrease, or no change in MPTP induced animals were documented (Smith et al. 1997; Tanji et al. 1999; Al Sweidi et al. 2013; Liu et al. 2014; Rico et al. 2017; Yang et al. 2021).
Evidence suggests that alterations in the gastrointestinal microbiota play an important role in onset, progression, and risk of neurodegenerative diseases such as Alzheimer diseases and PD (Pellegrini et al. 2018; Santos et al. 2019; Morais et al. 2021; Rani and Mondal 2021). Recently the MPTP mouse models for PD studies have been commonly used to explore the GBA in PD and investigate possible gut microbiota-associated PD therapeutics (Fang et al. 2019; Pu et al. 2019; Liu et al. 2021; Sun et al. 2021; Wang et al. 2021). However, there have been conflicting reports for the alteration of bacterial populations in MPTP induced mouse models of PD likely due to different MPTP administration schedules as well as different mouse strain, age, sex, body weight which impact the MPTP effectivity and sensitivity (Lai et al. 2018; Sun et al. 2018; Fang et al. 2019; Pu et al. 2019; Liao et al. 2020; Liu et al. 2021; Wang et al. 2022). In this study cecum digesta was collected from same age and sex mice administered acute and subchronic regimens of MPTP to perform microbiota analysis and evaluate if the impact of MPTP on gut microbiota differs depending on the administration regimen.
When the samples were compared at both phylum and genus level using correspondence analysis, significant changes were observed between the groups. The abundance of Firmicutes and Bacteroidota, the most dominant phyla in all the samples, increased in the mice administered subchronic regimen of MPTP while decreased in the acute MPTP group of mice. The Firmicutes and Bacteroidota are two major phyla detected in human and murine gastrointestinal microbiome and the ratio of these two phyla has found to be relevant to human health (Nguyen et al. 2015). A previous study exploring neuroprotective effect of an engineered commensal bacterium on 20 mg/kg of MPTP induced mouse model of PD reported a decrease in Firmicutes and an increase in Bacteroidata in MPTP mice (Fang et al. 2019). On contrary, in a study examining the neurodegenerative impact of L. plantarum strain on PD mouse model where 30 mg/kg MPTP administered for 7 days, Firmicutes was found to be increased in MPTP mice (Wang et al. 2022). Although Keshavarzian et al. reported that the abundance of Firmicutes in PD patients was found to be lower and the level of Bacteroidata was higher in fecal samples, the ratio of Firmicutes and Bacteroidata was not significantly different from the healthy control (Keshavarzian et al. 2015). They also reported that the level of Verrucomicrobiota was higher in PD patients. The abundance of Bacteroidata was found to be significantly reduced in another study while Firmicutes was not significantly different (Unger et al. 2016). Moreover, Bedraf et al. reported a higher abundance of Firmicutes together with the abundance of Verrucomicrobiota in l-DOPA-naïve PD patients (Bedarf et al. 2017). The predominance of mucin degrading Verrucomicrobiota, found to be reduced in mice over-expressing wild-type human α-syn, was increased in the acute MPTP mice while decreased in the subchronic MPTP mice in this study (Rani and Mondal 2021). These results indicate that acute and subchronic administration schedule of MPTP is capable of altering the gut microbiota differently at the phylum level.
When the dominant genera that increased or decreased in abundance were identified by correspondence analysis, significant (p < 0.05) changes were observed between all samples. Muribaculaceae previously known as S24-7 was the most dominant genus in the cecum microbiota of all groups except acute MPTP mice. Its prevalence was decreased in acute MPTP mice while increased in the subchronic mice (Pereira et al. 2020). Muribaculaceae, a poorly characterized genus, was identified as mucin monosaccharide foragers. In a study exploring the significance of casein in the development of PD using 6 weeks-old mice administered 25 mg/kg/day MPTP for 5 days, microbiota of the fecal samples collected 24 days after MPTP administration was analyzed. Similar to the subchronic MPTP mice, Muribaculaceae was found to be increased in the MPTP mice used in the study (Liu et al. 2021). Besides, Muribaculaceae was reported to be decreased in a different PD animal model induced by rotenone (Rani and Mondal 2021).
Akkermansia was the most dominant genus in the acute MPTP mice, which distinctive from the other groups of mice. The prevalence of Akkermansia was increased in the acute MPTP mice, while it was decreased in the subchronic MPTP mice. Previously, Fang et al. reported a non-significant reduction in the abundance of Akkermansia in mice injected with 20 mg/kg MPTP for 7 days, while Jeon et al. reported a rise in the mice administered 30 mg/kg of MPTP for 5 days similar to the subchronic MPTP mice in this study (Fang et al. 2019; Jeon et al. 2021). Akkermansia shown to be associated with irritable bowel syndrome and PD with constipation was found to be increased in PD patients (Keshavarzian et al. 2015; Bedarf et al. 2017; Hill-Burns et al. 2017; Gorecki et al. 2019).
Colidextribacter which was decreased in the acute MPTP mice while was increased in the subchronic MPTP mice, was detected to increase in murine microbiota during aging along with the Clostridia UCG-014 which was higher in the acute MPTP mice (Ratto et al. 2022). Additionally, predominance of Candidatus_Saccharimonas which was higher in both acute and subchronic MPTP mice, has found to be associated with intestinal inflammation (Cruz et al. 2020). Similarly, proportion of Lactobacillus was higher in the microbiota of mice administered either regimen, which has been reported to be increased in PD patients previously (Hasegawa et al. 2015; Hill-Burns et al. 2017). Abundance of Alistipes was reduced in both regimen which was found to be lower in MPTP mouse models previously (Fang et al. 2019; Wang et al. 2022). These data indicate that acute and subchronic administration schedule of MPTP are capable of altering the gut microbiota differently at the genus level.
Although this study was not designed to evaluate the influence of the repeated injection stress on the composition of the cecum microbiota, the differences in some of the microbial populations in the control samples were compelling. Observed differences in the control samples could be due to mouse-to-mouse variation since the overall microbiota between the controls was not significantly different. Previously, it has been reported that different types of stress such as repeated injection and social isolation could impact systemic inflammation and anxiety-like behavior in mice (Du Preez et al. 2020). This suggests that repeated injection could have an impact on microbial composition as well. Meta-analysis and systematic reviews performed recently revealed that although gut microbial composition detected in PD patients may vary among different studies, shared alterations in gut microbiota of PD have been observed (Hill et al. 2021; Shen et al. 2021; Nowak et al. 2022). Abundance of Akkermansia, Verrucomicrobiota, and Alistipes have found to be increased in PD patients while decrease in level of Lachnospiraceae and Prevotellaceae have detected. Some of the microbial populations such as Firmicutes and Bacteroidetes vary in predominance. Heterogeneity of the results have been explained with various factors including difference in geographical regions, dietary habits, stage of PD, and age of matched-controls. However, common changes in the gut microbiota have been suggested to be used as biomarker in future studies (Nowak et al. 2022). As a conclusion, overall these results demonstrate that MPTP administration alters the gut microbiota in an administration regimen specific manner. These could imply an association with the time course of pathophysiological events in PD mice. Hence, MPTP administration schedule must be taken into consideration when designing experiments including MPTP induced mouse model of PD that follow microbiota composition as well as strain, age, sex, and body weight of the mice. Future studies evaluating the time course effect of MPTP administration on gut microbial composition would help to better understand the interaction between gut microbiota and PD pathophysiology.
Data Availability
The datasets generated during the current study are available in Sequence Read Archive (SRA) database with the accession number of PRJNA867416, https://www.ncbi.nlm.nih.gov/bioproject/PRJNA867416/.
References
Aguirre de Cárcer D, Cuív PO, Wang T et al (2011) Numerical ecology validates a biogeographical distribution and gender-based effect on mucosa-associated bacteria along the human colon. ISME J 5:801–809. https://doi.org/10.1038/ismej.2010.177
Aktas B, De Wolfe TJ, Tandee K et al (2015) The effect of Lactobacillus casei 32G on the mouse cecum microbiota and innate immune response is dose and time dependent. PLoS ONE. https://doi.org/10.1371/journal.pone.0145784
Al Sweidi S, Morissette M, Rouillard C, Di Paolo T (2013) Estrogen receptors and lesion-induced response of striatal dopamine receptors. Neuroscience 236:99–109. https://doi.org/10.1016/j.neuroscience.2012.12.058
Armstrong MJ, Okun MS (2020) Diagnosis and treatment of Parkinson disease: a review. JAMA 323:548–560. https://doi.org/10.1001/jama.2019.22360
Bedarf JR, Hildebrand F, Coelho LP et al (2017) Functional implications of microbial and viral gut metagenome changes in early stage L-DOPA-naïve Parkinson’s disease patients. Genome Med 9:1–13
Bhattacharjee N, Paul R, Giri A, Borah A (2016) Chronic exposure of homocysteine in mice contributes to dopamine loss by enhancing oxidative stress in nigrostriatum and produces behavioral phenotypes of Parkinson’s disease. Biochem Biophys Reports 6:47–53. https://doi.org/10.1016/j.bbrep.2016.02.013
Biju KC, Evans RC, Shrestha K et al (2018) Methylene blue ameliorates olfactory dysfunction and motor deficits in a chronic MPTP/probenecid mouse model of Parkinson’s disease. Neuroscience 380:111–122
Chessel D, Dufour AB, Thioulouse J (2004) The ade4 package - I : One-table methods. R News 4:5–10
Claesson MJ, Wang Q, O’Sullivan O et al (2010) Comparison of two next-generation sequencing technologies for resolving highly complex microbiota composition using tandem variable 16S rRNA gene regions. Nucleic Acids Res. https://doi.org/10.1093/nar/gkq873
Cruz BC, Conceição LL, Mendes TA et al (2020) Use of the synbiotic VSL#3 and yacon-based concentrate attenuates intestinal damage and reduces the abundance of Candidatus Saccharimonas in a colitis-associated carcinogenesis model. Food Res Int. https://doi.org/10.1016/j.foodres.2020.109721
Dauer W, Przedborski S (2003) Parkinson’s disease: mechanisms and models. Neuron 39:889–909
Dorsey ER, Bloem BR (2018) The Parkinson pandemic—A call to action. JAMA Neurol 75:9–10. https://doi.org/10.1001/jamaneurol.2017.3299
Dray S, Dufour A-B (2007) Journal of statistical software. J Stat Softw Sept 22:1–20
Du Preez A, Law T, Onorato D et al (2020) The type of stress matters: repeated injection and permanent social isolation stress in male mice have a differential effect on anxiety- and depressive-like behaviours, and associated biological alterations. Transl Psychiatr. https://doi.org/10.1038/s41398-020-01000-3
Du Y, Ma Z, Lin S et al (2001) Minocycline prevents nigrostriatal dopaminergic neurodegeneration in the MPTP model of Parkinson’s disease. Proc Natl Acad Sci 98:14669–14674. https://doi.org/10.1073/pnas.251341998
Ellett LJ, Hung LW, Munckton R et al (2016) Restoration of intestinal function in an MPTP model of Parkinson’s disease. Sci Rep 6:1–11. https://doi.org/10.1038/srep30269
Fang X, Tian P, Zhao X et al (2019) Neuroprotective effects of an engineered commensal bacterium in the 1-methyl-4-phenyl-1, 2, 3, 6-tetrahydropyridine Parkinson disease mouse model via producing glucagon-like peptide-1. J Neurochem 150:441–452. https://doi.org/10.1111/jnc.14694
Feng P, Zhang X, Li D et al (2018) Two novel dual GLP-1/GIP receptor agonists are neuroprotective in the MPTP mouse model of Parkinson’s disease. Neuropharmacology 133:385–394
Fornai F, Schlüter OM, Lenzi P et al (2005) Parkinson-like syndrome induced by continuous MPTP infusion: convergent roles of the ubiquitin-proteasome system and α-Synuclein. Proc Natl Acad Sci. https://doi.org/10.1073/pnas.0409713102
Foundation P (2021) Understanding Parkinson’s. In: Park. Found. Park. Preval. Proj. https://www.parkinson.org/Understanding-Parkinsons/Statistics
Gorecki AM, Preskey L, Bakeberg MC et al (2019) Altered gut microbiome in Parkinson’s disease and the influence of lipopolysaccharide in a human α-synuclein over-expressing mouse model. Front Neurosci 13:1–13
Haque ME, Azam S, Akther M et al (2021) The neuroprotective effects of GPR4 inhibition through the attenuation of caspase mediated apoptotic cell death in an MPTP Induced mouse model of Parkinson’s disease. Int J Mol Sci. https://doi.org/10.3390/ijms22094674
Hasegawa S, Goto S, Tsuji H et al (2015) Intestinal dysbiosis and lowered serum lipopolysaccharide-binding protein in Parkinson’s disease. PLoS ONE 10:1–15. https://doi.org/10.1371/journal.pone.0142164
He R, Huang W, Huang Y et al (2018) Cdk5 inhibitory peptide prevents loss of dopaminergic neurons and alleviates behavioral changes in an MPTP induced Parkinson ’ s disease mouse model. Front Aging Neurosci 10:1–9
Hill AE, Wade-Martins R, Burnet PWJ (2021) what is our understanding of the influence of gut microbiota on the pathophysiology of Parkinson’s disease? Front Neurosci 15:1–9. https://doi.org/10.3389/fnins.2021.708587
Hill-Burns EM, Debelius JW, Morton JT et al (2017) Parkinson’s disease and Parkinson’s disease medications have distinct signatures of the gut microbiome. Mov Disord 32:739–749
Hopfner F, Künstner A, Müller SH et al (2017) Gut microbiota in Parkinson disease in a northern German cohort. Brain Res 1667:41–45
Houser MC, Chang J, Factor SA et al (2018) Stool immune profiles evince gastrointestinal inflammation in Parkinson’s disease. Mov Disord 33:793–804
Huang D, Xu J, Wang J et al (2017) Dynamic changes in the nigrostriatal pathway in the MPTP mouse model of Parkinson’s disease. Neuroscience 2017:303–313. https://doi.org/10.1016/j.neuroscience.2017.11.041
Huang D, Wang Z, Tong J et al (2018) Long-term changes in the nigrostriatal pathway in the MPTP mouse model of Parkinson’s disease. Neuroscience 369:303–313. https://doi.org/10.1016/j.neuroscience.2017.11.041
Hwang D-J, Kwon K-C, Song H-K et al (2019) Comparative analysis of dose-dependent neurotoxic response to 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine in C57BL/6 N mice derived from three different sources. Lab Anim Res 35:1–9
Jackson-Lewis V, Przedborski S (2007) Protocol for the MPTP mouse model of Parkinson’s disease. Nat Protoc 2:141–151. https://doi.org/10.1038/nprot.2006.342
Jagmag SA, Tripathi N, Shukla SD et al (2016) Evaluation of models of Parkinson’s disease. Front Neurosci. https://doi.org/10.3389/fnins.2015.00503
Jeon H, Bae CH, Lee Y et al (2021) Korean red ginseng suppresses 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine-induced inflammation in the substantia nigra and colon. Brain Behav Immun 94:410–423. https://doi.org/10.1016/j.bbi.2021.02.028
Johnson ME, Stringer A, Bobrovskaya L (2018) Rotenone induces gastrointestinal pathology and microbiota alterations in a rat model of Parkinson’s disease. Neurotoxicology 65:174–185
Keshavarzian A, Green SJ, Engen PA et al (2015) Colonic bacterial composition in Parkinson’s disease. Mov Disord 30:1351–1360
Ko WKD, Bezard E (2017) Experimental animal models of Parkinson’s disease: a transition from assessing symptomatology to α-synuclein targeted disease modification. Exp Neurol 298:172–179
Kuroiwa H, Yokoyama H, Kimoto H et al (2010) Biochemical alterations of the striatum in an MPTP-treated mouse model of Parkinson’s disease. Metab Brain Dis 25:177–183. https://doi.org/10.1007/s11011-010-9195-9
Lai F, Jiang R, Xie W et al (2018) Intestinal pathology and gut microbiota alterations in a methyl-4-phenyl-1,2,3,6-tetrahydropyridine (MPTP) mouse model of Parkinson’s disease. Neurochem Res 43:1986–1999
Langston JW, Ballard P, Tetrud JW, Irwin I (1983) Chronic Parkinsonism in humans due to a product of meperidine-analog synthesis. Science. https://doi.org/10.1126/science.6823561
Li Y, Liu WZ, Li L, Hölscher C (2017) D-Ala2-GIP-glu-PAL is neuroprotective in a chronic Parkinson’s disease mouse model and increases BNDF expression while reducing neuroinflammation and lipid peroxidation. Eur J Pharmacol 797:162–172
Liao JF, Cheng YF, You ST et al (2020) Lactobacillus plantarum PS128 alleviates neurodegenerative progression in 1-methyl-4-phenyl-1,2,3,6-tetrahydropyridine-induced mouse models of Parkinson’s disease. Brain Behav Immun 90:26–46. https://doi.org/10.1016/j.bbi.2020.07.036
Lindqvist D, Kaufman E, Brundin L et al (2012) Non-motor symptoms in patients with Parkinson’s disease - correlations with inflammatory cytokines in serum. PLoS ONE. https://doi.org/10.1371/journal.pone.0047387
Liu J, Gao J, Tu S et al (2014) Neuroprotective effects of Jitai tablet, a traditional Chinese medicine, on the MPTP-induced acute model of Parkinson’s disease: involvement of the dopamine system. Evid-Based Complement Altern Med. https://doi.org/10.1155/2014/542383
Liu X, Liu S, Tang Y et al (2021) Intragastric administration of casein leads to nigrostriatal disease progressed accompanied with persistent nigrostriatal—intestinal inflammation activited and intestinal microbiota—metabolic disorders induced in MPTP mouse model of Parkinson’s disease. Neurochem Res. https://doi.org/10.1007/s11064-021-03293-2
Lu Y, Zhang X, Zhao L et al (2018) Metabolic disturbances in the striatum and substantia nigra in the onset and progression of MPTP-induced Parkinsonism model. Front Neurosci 12:1–10. https://doi.org/10.3389/fnins.2018.00090
Maserejian N, Vinikoor-Imler L, Dilley A (2020) Estimation of the 2020 Global Population of Parkinson’s Disease (PD). In: MDS Virtual Congress 2020. p 35 (suppl 1)
Medicine JH (2021) Young-Onset Parkinson’s Disease. In: Med. Johns Hopkins. https://www.hopkinsmedicine.org/health/conditions-and-diseases/parkinsons-disease/youngonset-parkinsons-disease
Meredith GE, Rademacher DJ (2011) MPTP mouse models of Parkinson’s disease: an update. J Parkinsons Dis 1:19–33. https://doi.org/10.3233/JPD-2011-11023
Morais LH, Schreiber HL, Mazmanian SK (2021) The gut microbiota–brain axis in behaviour and brain disorders. Nat Rev Microbiol 19:241–255
Nguyen TLA, Vieira-Silva S, Liston A, Raes J (2015) How informative is the mouse for human gut microbiota research? Dis Model Mech 8:1–16. https://doi.org/10.1242/dmm.017400
Nowak JM, Kopczyński M, Friedman A et al (2022) Microbiota dysbiosis in Parkinson disease—in search of a biomarker. Biomedicines 10:1–16. https://doi.org/10.3390/biomedicines10092057
Parashar A, Udayabanu M (2017) Gut microbiota: implications in Parkinson’s disease. Park Relat Disord 38:1–7
Pellegrini C, Antonioli L, Colucci R et al (2018) Interplay among gut microbiota, intestinal mucosal barrier and enteric neuro-immune system: a common path to neurodegenerative diseases? Acta Neuropathol 136:345–361
Pereira FC, Wasmund K, Cobankovic I et al (2020) Rational design of a microbial consortium of mucosal sugar utilizers reduces Clostridiodes difficile colonization. Nat Commun. https://doi.org/10.1038/s41467-020-18928-1
Prasad EM, Hung SY (2020) Behavioral tests in neurotoxin-induced animal models of parkinson’s disease. Antioxidants 9:1–50. https://doi.org/10.3390/antiox9101007
Pu Y, Chang L, Qu Y et al (2019) Antibiotic-induced microbiome depletion protects against MPTP-induced dopaminergic neurotoxicity in the brain. Aging. https://doi.org/10.18632/aging.102221
Rani L, Mondal AC (2021) Unravelling the role of gut microbiota in Parkinson’s disease progression: pathogenic and therapeutic implications. Neurosci Res 168:100–112
Ratto D, Roda E, Romeo M et al (2022) The many ages of microbiome–gut–brain axis. Nutrients 14:2937
Rico AJ, Dopeso-Reyes IG, Martínez-Pinilla E et al (2017) Neurochemical evidence supporting dopamine D1–D2 receptor heteromers in the striatum of the long-tailed macaque: changes following dopaminergic manipulation. Brain Struct Funct 222:1767–1784. https://doi.org/10.1007/s00429-016-1306-x
Rodriguez A, Zhang H, Klaminder J et al (2018) Toxtrac: a fast and robust software for tracking organisms. Methods Ecol Evol 9:460–464. https://doi.org/10.1111/2041-210X.12874
Sampson TR, Debelius JW, Thron T et al (2016) Gut microbiota regulate motor deficits and neuroinflammation in a model of Parkinson’s disease. Cell 167:1469–1480
Santos SF, De Oliveira HL, Yamada ES et al (2019) The gut and Parkinson’s disease—a bidirectional pathway. Front Neurol 10:1–8
Schapira AHV, Chaudhuri KR, Jenner P (2017) Non-motor features of Parkinson disease. Nat Rev Neurosci 18:435–450
Schwiertz A, Spiegel J, Dillmann U et al (2018) Fecal markers of intestinal inflammation and intestinal permeability are elevated in Parkinson’s disease. Park Relat Disord 50:104–107. https://doi.org/10.1016/j.parkreldis.2018.02.022
Shen T, Yue Y, He T et al (2021) The association between the gut microbiota and Parkinson’s disease, a meta-analysis. Front Aging Neurosci 13:1–12. https://doi.org/10.3389/fnagi.2021.636545
Smith TS, Trimmer PA, Khan SM et al (1997) Mitochondrial toxins in models of neurodegenerative diseases. II: Elevated zif268 transcription and independent temporal regulation of striatal D1 and D2 receptor mRNAs and D1 and D2 receptor-binding sites in C57BL/6 mice during MPTP treatment. Brain Res 765:189–197. https://doi.org/10.1016/S0006-8993(97)00430-7
Sun MF, Zhu YL, Zhou ZL et al (2018) Neuroprotective effects of fecal microbiota transplantation on MPTP-induced Parkinson’s disease mice: gut microbiota, glial reaction and TLR4/TNF-α signaling pathway. Brain Behav Immun 70:48–60
Sun J, Li H, Jin Y et al (2021) Probiotic Clostridium butyricum ameliorated motor deficits in a mouse model of Parkinson’s disease via gut microbiota-GLP-1 pathway. Brain Behav Immun 91:703–715. https://doi.org/10.1016/j.bbi.2020.10.014
Tanji H, Araki T, Nagasawa H, Itoyama Y (1999) Differential vulnerability of dopamine receptors in the mouse brain treated with MPTP. Brain Res 824:224–231. https://doi.org/10.1016/S0006-8993(99)01209-3
Taylor JM, Main BS, Crack PJ (2013) Neuroinflammation and oxidative stress: co-conspirators in the pathology of Parkinson’s disease. Neurochem Int 62:803–819
TheRCoreTeam (2013) R : A Language and Environment for Statistical Computing. 1
Unger MM, Spiegel J, Dillmann KU et al (2016) Short chain fatty acids and gut microbiota differ between patients with Parkinson’s disease and age-matched controls. Park Relat Disord 32:66–72. https://doi.org/10.1016/j.parkreldis.2016.08.019
Wang L, Li S, Jiang Y et al (2021) Neuroprotective effect of Lactobacillus plantarum DP189 on MPTP-induced Parkinson’s disease model mice. J Funct Foods 85:104635
Wang L, Zhao Z, Zhao L et al (2022) Lactobacillus plantarum DP189 reduces α-SYN aggravation in MPTP-induced Parkinson’s disease mice via regulating oxidative damage, inflammation, and gut microbiota disorder. J Agric Food Chem 70:1163–1173. https://doi.org/10.1021/acs.jafc.1c07711
Yang B, Wang Y, Qian PY (2016) Sensitivity and correlation of hypervariable regions in 16S rRNA genes in phylogenetic analysis. BMC Bioinform 17:1–8. https://doi.org/10.1186/s12859-016-0992-y
Yang P, Knight WC, Li H et al (2021) Dopamine D1 + D3 receptor density may correlate with Parkinson disease clinical features. Ann Clin Transl Neurol 8:224–237. https://doi.org/10.1002/acn3.51274
Zhang J, Ding X, Guan R et al (2018) Evaluation of different 16S rRNA gene V regions for exploring bacterial diversity in a eutrophic freshwater lake. Sci Total Environ 618:1254–1267. https://doi.org/10.1016/j.scitotenv.2017.09.228
Acknowledgements
This work was funded by the Scientific and Technological Research Institution of Turkey (TUBITAK) with grant number of 119S434.
Funding
This work was funded by the Scientific and Technological Research Institution of Turkey (TUBITAK) with Grant No. of 119S434.
Author information
Authors and Affiliations
Contributions
The author (BA) contributed to the study conception and design; material preparation, data collection and analysis, and manuscript writing.
Corresponding author
Ethics declarations
Competing Interests
The author has no relevant financial or non-financial interests to disclose.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Aktas, B. Gut Microbial Alteration in MPTP Mouse Model of Parkinson Disease is Administration Regimen Dependent. Cell Mol Neurobiol 43, 2815–2829 (2023). https://doi.org/10.1007/s10571-023-01319-7
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10571-023-01319-7