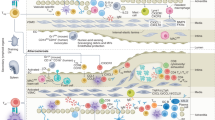
Abstract
Background and Aims
The long-term effect of immune tolerance has not been explored so far in atherosclerosis. In the present study, we assessed the effect of mucosal tolerance to a multi antigenic construct expressing three peptides from ApoB, HSP60, and outer membrane protein from Chlamydia pneumonia (AHC) for 30 weeks at every 6-week interval to understand the kinetics of immune modulation in disease progression. The safety profile of the molecule was also evaluated in mice.
Methods
Apobtm2SgyLdlrtm1Her/J mice (5–6 weeks) were orally dosed with multi antigenic construct (AHC) molecule on alternate days, followed by high-fat diet feeding to initiate atherosclerosis.
Results
Treated animals showed an efficient reduction in plaque growth and lipid accumulation at 6 weeks (49%, p < 0.01) and 12 weeks (42.3%, p < 0.01) which decreased to 29% (p = 0.0001) at 18 weeks and at later time points. Macrophage accumulation was significantly lower at all time points (53% at 12 weeks to 27% at 30 weeks). Regulatory T cells increased in the spleen following treatment until 12 weeks (week 0 (2.57 ± 0.18 vs. 6.36 ± 0.03, p = 0.02), week 6 (4.52 ± 0.2 vs. 8.87 ± 0.32, p = 0.02), and week 12 (8.74 ± 0.37 vs. 15.4 ± 0.27, p = 0.02)) but showed a decline later. A similar trend was observed with tolerogenic dendritic cells. We observed an increase in antibody levels to low-density lipoprotein and oxidized LDL at later stages. AHC molecule was found to be safe in acute and repeated dose toxicity studies.
Conclusions
Our results suggest that immune tolerance to AHC protein by oral administration is able to provide efficient atheroprotection up to 18 weeks and moderately at later stages. Apart from immune regulatory cells, protective antibodies may also have a role in controlling atherosclerosis.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Immune modulation to treat atherosclerosis has gained momentum in the past decade, and several studies have shown atheroprotective effects of restoring tolerance to auto-antigens [1,2,3]. Atherosclerosis is now considered as an autoimmune disease, wherein the oxidized low-density lipoprotein (Ox-LDL), HSP60, and molecular mimicry between pathogenic antigens and self-antigens induce an immune response and inflammation [4, 5]. Oxidation of LDL generates several new epitopes known as oxidation-specific epitopes which are not present in native LDL. These neo-epitopes are recognized by both innate and adaptive immune response [6, 7]. Naïve T lymphocytes differentiate into helper T cells (Th) and regulatory T cells (Treg) in response to cytokine and antigen stimulation. The Treg cells are critical for maintaining immune tolerance to self-antigens, and dysregulation of Treg activity is associated with several autoimmune diseases including atherosclerosis [8, 9].
Immune tolerance to self-antigens is mediated by antigen-specific Treg cells. These Tregs can suppress the inflammatory and proatherogenic adaptive immune response and shown to have a protective effect in several models of atherosclerosis [10, 11]. The role of Tregs in atherosclerosis has been studied extensively in animal models, wherein they reduce inflammation and induce protection against plaque development and stabilize the plaque [12, 13]. Treatment with ApoB- or HSP60-derived peptides was reported to reduce plaque inflammation in association with regulatory T cell (CD4+CD25+) response by us as well as several other groups [14,15,16,17]. Chyu et al. [18] in a series of studies showed that a P210—a peptide derived from ApoB100—activated CD8+ cells which could confer atheroprotective immunity. Immunization with P210 peptide was also associated with Treg response and increase in CD4+IL10+cells [15]. Other distinct peptides from ApoB protein (ApoB3501–3516 and ApoB978–993) were also reported to reduce atherosclerosis by an IL10-dependent mechanism [19]. Recently, ApoB100-specific T cell hybridoma expressing a single V beta chain has been identified. The peptide derived from this study was found to block T cell recognition of ApoB100 and significantly reduce atherosclerosis [20]. Similarly, treatment with HSP60 protein or peptides was reported to induce protection by inducing CD4+GARP+ regulatory T cells (Tregs) [21], type 1 regulatory T cell (Tr1) cells, or CD4+CD25+FoxP3+ Tregs [22].
In our previous studies, we have shown that the oral immunotherapy to atherosclerosis by a multi antigenic construct “AHC protein” expressing peptide epitopes from apolipoprotein (Apo B), heat shock protein (HSP60), and Chlamydia pneumonia outer membrane protein induces immune tolerance and has both protective and curative effects against atherosclerosis in animal models. The AHC recombinant molecule was generated by incorporating the ApoB peptide at the N-terminal, Cpn Peptide at the C-terminal, and the HSP60 peptide replacing the loop II of dendroaspin scaffold as described earlier [17]. Oral administration of AHC molecule was found to increase antigen-specific Treg response, reduce the inflammatory cells, and activate the tolerogenic dendritic cells, which was able to reduce both plaque development and progression in both mice and rabbits [17, 23,24,25].
Most of the studies on immune modulation are explored for a short duration of 10 to 12 weeks. The effect of tolerance induction has not been studied for any antigen for a long period of time to comprehend the long-lasting effect of immune modulation therapy. Moreover, understanding of preclinical toxicity is also an important aspect of any therapeutic model. In the present study, we explored the effect of tolerance to AHC protein in Apobtm2SgyLdlrtm1Her/J mice model for a period of 30 weeks and observed the disease progression and immune response at 6-week interval to understand the protection at different stages and evaluated the acute and repeated dose safety profile at escalated doses in Swiss albino mice.
Materials and Methods
Animals
Apobtm2SgyLdlrtm1Her/J-knockout mice on a C57BL/6 background (Jackson Laboratories) were used for all the experiments. All animal experiments were approved by the Institutional Animal Ethics Committee of the Thrombosis Research Institute (Registration Number: 1261/c/09/CPCSEA) in compliance with Government of India guidelines and conform to the Guide for the Care and Use of Laboratory Animals published by the US National Institutes of Health (NIH Publication, 8th Edition, 2011). Mice were kept under standard laboratory 12-h day and 12-h night cyclic conditions and fed on either a chow diet or a diet high in fat and cholesterol (21% fat and 1.25% cholesterol). Starting at 6 weeks of age, an equal number of males and females (6–8 animals per group) were used in each group.
Materials
Multi antigenic construct AHC (APOB, HSP60, and Chlamydia pneumonia outer membrane protein) was purified as described earlier [25]. High-fat diet (HFD) was purchased from Harlan, TD 96121 Indianapolis, USA, with 21% anhydrous milk fat and 1.25% cholesterol. Details of AHC construction and purification are included in the supplementary section.
Generation of Recombinant Construct AHC
The construction of multi antigenic construct and the detailed structural dendroaspin carrier for incorporating multi antigens was described earlier [17, 26]. The epitope derived from human ApoB100 (peptide sequence: I688EIGLEGKGFEPTLEALFGK707, numbered including signal peptide) was incorporated into the N-terminal of dendroaspin with a poly-glycine linker between ApoB peptide and dendroaspin. Epitope from hHSP60 (peptide sequence: A153ELKKQSKPVT163) was incorporated in dendroaspin loop III as a replacement of wild-type loop III sequence. Cpn sequence in a combination form was derived from the major outer membrane protein (MOMP) of the Cpn (peptide sequence: G67DYVFDRI74) and polymorphic outer membrane protein (OMP) 5 of Cpn (peptide sequence: Q283AVANGGAI291) at the C-terminal of dendroaspin.
Synthesis, Expression, and Purification of Multi Antigenic Protein
The genes were synthesized by Genescript, USA Inc. under confidential agreement and cloned into a PUC57 vector. The genes of constructs AHC were amplified by PCR and cloned in a pGEX-3X and used for the transformation of E.coli BL21 strain. Protein expression was induced by 0.1 mm IPTG and purified using glutathione-Sepharose affinity and ion exchange chromatography and analyzed by sodium dodecyl sulfate polyacrylamide gel electrophoresis (SDS-PAGE) and western blotting [17].
Experimental Design
Apobtm2SgyLdlrtm1Her/J double-knockout mice aged 5–6 weeks (N = 72) were orally dosed with multi antigenic construct AHC (1μg/dose/animal) or phosphate buffered saline on five alternate days (N = 36 each) through oral gavage. Animals were fed on HFD to induce atherosclerosis. Groups of 6 mice were sacrificed humanely by using an overdose of isoflurane inhalant anesthetic (15%) as per American Veterinary Medical Association guidelines (June 2007) immediately after the oral dosing schedule, considered as 0 week and at every 6-week interval at 6, 12, 18, 24, and 30 weeks, and organs collected for further evaluation. The experimental design is shown in Fig. 1a. The dose response was studied as described earlier.
Reduction in lesion size and necrotic core by AHC. a Experimental design: groups of 6 mice (5–6 weeks) were orally dosed 5 times with 1 μg of purified recombinant multi antigenic molecule (AHC) or PBS on alternate days and were fed on HFD for 6, 12, 18, 24, and 30 weeks. b Representative photomicrograph showing elastic Von Gieson staining of aortic sinus sections at different time points. The scale bar represents 200 μm. c Representative bar graph showing the comparative average lesion size at different time points for both control and AHC group. d Representative bar graph showing the percentage reduction in necrosis in AHC group compared with the control group. The scale bar represents 100 μm
Atherosclerotic Lesion Assessment and Immunohistochemistry on Aortic Sinus
Aortic sinuses from 6 animals per group were collected in either OCT (optimum cutting temperature) or paraffin. Minimum of 6 sections from each animal were stained with elastic Van Gieson (EVG) stain to measure the percentage of lesion area in the total aortic sinus, and Oil Red O was used to assess the total lipid deposition in the sinus. Images were processed using a confocal microscope (Leica DMI 4000 B, Germany) and quantified using Image-Pro Plus software (Media Cybernetics, Bethesda, USA).
Immunohistochemical Analysis of Atherosclerotic Lesions
The frozen sections were collected on slides coated with 5% amino-silane. Sections were permeabilized using 0.2% of Triton X 100 for 30 min and fixed with ice-cold acetone. Slides were incubated with primary antibodies, after blocking with 5% serum followed by the appropriate secondary antibody (Alexa-633 tagged Invitrogen). Sections were mounted in Vector Shield, imaged using a Leica DMI 4000 B confocal microscope, and then analyzed using the Image-Pro software.
Immunophenotyping
Immunophenotyping for enumerating the Th1, Th17, Tregs, monocytes, and dendritic cell population in the spleen at different time points was performed by FACS Canto II using FACS DIVA software (Becton Dickinson, New Jersey, USA). The antibodies used in the study were as follows: fluorescein isothiocyanate (FITC) conjugated CD4 (clone RM4-5), allophycocyanin (APC) anti CD25 (clone 3C7), phycoerythrin (PE) anti-fork head fox p3 (Foxp3) (clone NRRF-30), PE IFN-γ (clone XMG1.2), PE anti Ly6c (clone HK 1.4), FITC anti CD103 (clone 2E7), APC-anti CD11c (clone N418) (all from eBiosciences, San Diego, CA, USA), APC-Cy™7 IL-17A (clone TC11-18H10, BD Pharmingen, San Jose, USA), PE-Cy™7 anti CD11b (clone M1/70, BD Pharmingen, San Jose, USA). The intracellular cytokines and Foxp3 were assessed using the intracellular staining kit (eBiosciences San Diego, CA, USA) according to the manufacturer’s instructions. Surface staining was performed according to standard procedures at a density of 1 × 105 cells/100 μL, and volumes scaled up accordingly. The fluorescence minus one (FMO) controls were used along with tested samples from both AHC and HFD group for gating negative cell population. The results were analyzed by Flow Jo software (Tree Star Ltd., Oregon, USA). The gating strategy for both T cell and monocytes was given in Figures S1 and S2 respectively.
ELISA
ELISA was carried out for native LDL and Ox-LDL on plasma samples at different stages of disease development. LDL (Sigma Chemicals, St. Louis, USA) was oxidized overnight with CuSO4 (5 μM), as described earlier [27], and plates were coated with 10 μg/mL Cu-oxidized LDL or native LDL. Sera from control and AHC-treated animals (1:100) were added to coated plates for 90 min h at 37 °C. The plates were washed and developed by adding horseradish peroxidase (HRP) labeled anti-mouse IgG or IgM (Sigma Chemicals, St. Louis, USA) as secondary antibodies. Excess antibodies were washed, and the plate was developed by adding substrate for 30 min in dark. Absorbance was recorded at 450 nm.
Plasma Lipid Profile
Blood from overnight fasted animals was collected from the retro-orbital venous plexus under 3% isoflurane inhalant anesthesia in oxygen as per American Veterinary Medical Association guidelines (June 2007). Diluted plasma (10 times to get the values within the range) was used for measuring lipid concentrations by using Siemens Dimension® Xpand® plus following the manufacturer’ s instructions.
Safety Studies
Acute and sub-chronic toxicity was evaluated in Swiss albino mice to understand the safety profile of the AHC molecule. In the acute study, 20, 100, and 200 μg/mL concentration of AHC protein were orally administered to six animals (3M + 3F) once. Trypsin inhibitor neutralization of proteases in the gut was carried out in all the animals 10–20 min before the test item administration. The animals were observed for any adverse clinical symptoms for 14 days. At the completion of the study period, all the animals were humanely sacrificed and subjected to external and internal gross pathological observations. Repeated dose toxicity was conducted in two sets for 15 days and 30 days of repeated oral dosing with 1, 5, and 10 times the therapeutic dose with appropriate PBS control in a total of 10 animals (5M and 5F) per group. Animals were humanely sacrificed at the end of the study period and subjected to external and internal gross pathological observations. Hematological parameters; clinical biochemistry including albumin, glucose, alanine aminotransferase (ALT), aspartate aminotransferase (AST), alkaline phosphatase (ALP), blood urea nitrogen (BUN), creatinine, and calcium; and histopathology of internal organs were carried out to understand the safety data [27].
Real-time PCR
Total RNA was extracted from the ascending part of the aorta using TRIzol® Reagent from 6 control and 6 treated groups at each time point of disease progression (Invitrogen, Carlsbad, USA). Messenger RNA was reverse transcribed using Invitrogen cDNA synthesis kit, and polymerase chain reaction (RT-PCR) was performed using a two-step SYBR® Superscript® RT-PCR kit (Invitrogen, Carlsbad, USA) using an ABI PRISM 7900 qRT-PCR (Applied Biosystems, California, USA). The oligonucleotide sequences of primers used are presented in Table 1.
Statistical Analysis of Data
Data are expressed as mean ± SEM. Differences between control and treated groups at each time point were evaluated by Mann-Whitney test and were considered statistically significant at p < 0.05. Statistical analysis was performed using GraphPad Prism software version 6.01(GraphPad Software Inc., La Jolla, CA, USA).
Results
Effect of Oral Immunotherapy on the Progression of the Disease
Oral immunotherapy using the AHC protein was able to significantly control the progression of the lesion size and lipid accumulation in the aortic sinus of Apobtm2sgy/LDLrtm1Her/J mice as seen by elastic Van Gieson (EVG). The size of the lesion increased progressively as the disease progressed from 0 to 30 weeks. Significant reduction in the accumulation of atherosclerotic plaques was observed at 6 weeks (9.53 ± 1.0 vs. 3.55 ± 0.45, p = 0.0002, 62%) and 12 weeks (30.75 ± 0.78 vs. 16.5 ± 0.376, p = 0.0001, 46%) but decreased to 23% by 18 weeks (42.89 ± 1.26 vs. 33.18 ± 0.57, p = 0.0001) and 20% in later stages of atherosclerosis at 24 weeks (52.33 ± 0.49 vs. 40.7 ± 0.61, p = 0.0001) and 30 weeks (60.81 ± 0.56 vs. 50.28 ± 1.12, p = 0.0001) in the treated group of mice in comparison with HFD controls (Fig. 1b, c). Necrotic changes in the plaque were observed only by the 18th week, and the reduction in necrosis was 42% at 18 weeks (4.05 ± 0.20 vs. 2.32 ± 0.14, p = 0.0001), 30% at 24 weeks (8.17 ± 0.8 vs. 5.67 ± 0.26, p = 0.0001), and 25% by 30 weeks (9.88 ± 0.23 vs. 7.38 ± 0.20, p = 0.0001) (Fig. 1d).
Effect of Oral Immunotherapy on Aortic Lipid Accumulation, Plasma Lipids, and Macrophages
Lipid accumulation as a direct consequence of plaque growth studied at different weeks by ORO staining also showed a significant reduction of 49% at 6 weeks (8.42 ± 0.76 vs. 3.55 ± .59, p = 0.0003) and 42.3% at 12 weeks (30.73 ± 1.02 vs. 16.60 ± 1.15, p = 0.0006), and by 18 weeks the lipid accumulation decreased to 29% (41.4 ± 1.12 vs. 29.91 ± 0.4, p = 0.0001) whereas at 24 weeks (50.53 ± 0.86 vs. 37.81 ± 0.63, p = 0.0001) and 30 weeks (59.62 ± 0.71 vs. 46.12 ± 0.61, p = 0.0001) it was able to prevent around 22% when compared with the control group (Fig. 2a). Having observed the lower levels of lipid accumulation in the aortic sinus by ORO, we further measured the total cholesterol, triglyceride, and LDL levels in the plasma. The total cholesterol (TC) concentration of the treated group showed an insignificant difference in comparison with control, while the LDL levels were slightly lower in treated animals throughout at all the time points. Triglyceride levels were significantly lower only in the early stages of disease (Fig. 2b). In correlation with the total lesion area, the LDL and total cholesterol levels of HFD group were steadily increased whereas in AHC group the increase was lower when compared with the control group (Fig. 2c).
AHC reduces the lipid accumulation and plasma lipid levels in progressive atherosclerosis. a Representative photomicrographs of aortic sinus plaque area stained with Oil Red O for different weeks. The bar and line graphs show the comparative amount of lipid accumulation over a period of disease progression. The scale bar represents 200 μm. b Representative bar graphs showing plasma lipid profile of the AHC and control group. c Representative graph showing the comparative correlation of lipid progression in aortic sinus with respect to plasma total cholesterol and LDL
Oral Immunotherapy Reduces the Inflammation of the Aorta
The lipid-laden macrophages in the aortic sinus enumerated by immunohistochemistry using CD68 antibodies showed significantly lower levels in treated mice compared with the control group throughout the disease progression. The reduction in macrophage accumulation in the lesion was lower by 40% at 6 weeks (0.087 ± 0.012 vs. 0.147 ± 0.08), 12 weeks (0.337 ± 0.08 vs. 0.156 ± 0.03, p = 0.04), and 18 weeks (0.453 ± 0.10 vs. 0.210 ± 0.04) 53% up to 24 weeks (0.773 ± 0.12 vs. 0.371 ± 0.05, p = 0.02) which dropped to 27% at 30 weeks (0.998 ± 0.04 vs. 0.734 ± 0.03, p = 0.005) Fig. 3a, b.The quantitative expression levels of inflammatory and anti-inflammatory markers in the aortic sinus were normalized to GAPDH compared with the respective control group at each week. We observed a decrease in expression levels of inflammatory cytokines IFN-γ, IL-17, and arginase2, and increased anti-inflammatory cytokines like CTLA4, Foxp3, TGF-β, and arginase1 in the aorta of treated mice compared with control. The AHC therapy could control the expression of inflammatory cytokines IFN-γ and IL-17 in the early stages of disease up to 12 weeks, while at advanced stages of the disease no significant difference in expression could be observed in comparison with control (Fig. 3c). The expression of proteins associated with immune regulation, including Foxp3 (7fold), TGF-β (5.3 fold), and CTLA4 (9.3fold) was highest at 12 weeks and decreased by 18 weeks, while their expression was comparable to that of control by 30 weeks (Fig. 3e). A similar trend was observed for arginase 1, a marker of M2 macrophages. The ratio of arginase 1 to arginase 2 was skewed towards arginase 1 in the early stages of the disease, while at 24 and 30 weeks arginase 2 expression was higher (Fig. 3d).
Oral administration of AHC reduces inflammatory markers in the aorta. a Representative photomicrograph showing immunofluorescence staining of aortic sinus sections with CD68 (macrophage) at different time points. The scale bar represents 50 μm. b Percentage of CD68 positive area from several sections for each group (n = 6) were measured using Image-Pro Plus software and shown in bar. c mRNA expression levels of inflammatory IFN-γ and IL-17 in the ascending aorta were quantified using RT-PCR analysis and normalized with GAPDH. Fold changes in expression of the AHC immunized mice relative to control mice are shown. d mRNA expression levels of ARGINASE1and ARGINASE2 and the ratio of arginase I and arginase II in the ascending aorta. e mRNA expression levels of Foxp3, TGF-β, and CTLA 4 in the ascending aorta
Changes in CD4 T Cell Population and Monocytes in the Spleen
The change in T cell and monocyte population in the peripheral immune system as a consequence of oral immune therapy was studied by using flow cytometry. The CD4 cell population from both AHC and HFD group at different time points were comparable at all time points with a significant change only at 24 weeks (29.2 ± 2.3 vs. 35.8 ± 1.2, p = 0.04) (Fig. 4a). The gating strategy and representative dot plots for sample analysis for T cell and monocytes are given in Figure S1. Inflammation by CD4 positive IFN-γ-secreting cells at 12 weeks (6.22 ± 0.4 vs. 4.32 ± 0.07, p = 0.015), 18 weeks (9.47 ± 0.27 vs. 6.37 ± 0.14, p = 0.007), and 24 weeks (8.91 ± 0.37 vs. 6.78 ± 0.18, p = 0.015) was significantly lower in AHC treated group in contrast with the HFD control group (Fig. 4b). Th17 cells as seen by IL17-secreting CD4 positive cell were lower in AHC-treated mice at all time points but showed a statistical significance only at 12 (3.39 ± 0.22 vs. 2.65 ± 0.18, p = 0.02) and 24 weeks (2.30 ± 0.17 vs. 1.16 ± 0.05, p = 0.01) (Fig. 4c). We observed significantly higher proportion of Treg cells (CD25+Foxp3+) cells in the spleen of AHC-treated mice at week 0 (2.57 ± 0.18 vs. 6.36 ± 0.03, p = 0.02), week 6 (4.52 ± 0.2 vs. 8.87 ± 0.32, p = 0.02), and week 12 (8.74 ± 0.37 vs. 15.4 ± 0.27, p = 0.02), but from 18 weeks onwards the Tregs were comparable between control and treated animals (Fig. 4d). Monocytes associated with regulatory function such as CD11b+CD11c+ and CD11c+CD103+ cells were higher in AHC-treated mice only at earlier time points (0 week (3.14 ± 0.29 vs. 5.81 ± 0.33, p = 0.02), 6 week (2.70 ± 0.61 vs. 7.28 ± 0.96, p = 0.028), and 12 week (8.23 ± 0.3 vs. 22.52 ± 1.16, p = 0.04), and 0 week (2.49 ± 0.05 vs. 3.92 ± 0.31, p = 0.02) and 6 week (3.68 ± 0.75 vs. 8.05 ± 0.95, p = 0.02)) respectively (Fig. 4e, f). The inflammatory monocyte cell population of CD11b+LY6c+ was lower in AHC-treated group but was significant only at 6 weeks (16.7 ± 0.83 vs. 13.25 ± 1.39, p = 0.02) and 12 weeks (28.08 ± 1.01 vs. 8.31 ± 1.77, p = 0.005) (Fig. 4g).
Effect of oral administration of AHC in immune cells in the spleen. Flow cytometer analysis of splenocytes from AHC-treated and control mice at the end of the experiment. a The graph represents the percentage of CD4 positive cells within the CD4 population. b Percentage of Th1 as seen by CD4 positive IFN-γ cells within the CD4 population. c Percentage of Th17 as seen by CD4 positive IL-17 cells within the CD4 population. d Percentage of Treg cells as seen by CD425positive FOX-P3 within the CD4 population. e Percentage of CD11C positive cells within the CD11b population. f Percentage of CD103 positive cells within the CD11c population. g Percentage ofLy6c positive cells within the CD11b population
Immune Response to Auto-antigens LDL and OX-LDL
Immune response to auto-antigens like native LDL and Ox-LDL was measured in the serum of both treated and control animal groups. Hyperlipidemia-induced IgM response to LDL (0 week (0.022 ± 0.03 vs. 0.028 ± 0.06), 6 weeks (0.14 ± 0.02 vs. 0.08 ± 0.05, p = 0.007), 12 weeks (0.215 ± 0.008 vs. 0.146 ± 0.006, p = 0.02), 18 weeks (0.273 ± 0.03 vs. 0.224 ± 0.009, p = 0.03), 24 week (0.357 ± 0.03 vs. 0.336 ± 0.02), and 30 weeks (0.383 ± 0.07 vs. 0.346 ± 0.09)) (Fig. 5a) was significantly lower in early to mid-weeks of disease progression, whereas response to Ox-LDL IgM antibody was significantly lower in the advanced disease stage in the treated group in comparison with control (0 week (0.059 ± 0.06 vs.0.056 ± 0.01), 6 week (0.073 ± 0.017 vs. 0.059 ± 0.01), 12 week (0.152 ± 0.02 vs. 0.106 ± 0.02), 18 week (0.184 ± 0.006 vs. 0.141 ± 0.03, p = 0.03), 24 weeks (0.219 ± 0.04 vs. 0.179 ± 0.05), and 30 weeks (0.274 ± 0.06 vs. 0.216 ± 0.08, p = 0.01)) (Fig. 5c). The levels of IgG antibody response to ox-LDL were significantly higher in the AHC group throughout the disease progression and peaked at 18 weeks and lowered moderately at later stages (Fig. 5d). The IgG antibody levels to native LDL were comparable but significantly higher at 24 weeks (0.335 ± 0.02 vs. 0.489 ± 0.03, p = 0.05) and 30 weeks (0.349 ± 0.03 vs. 0.562 ± 0.02, p = 0.02) (Fig. 5b).
Safety Profile of AHC Molecule
The animals were found to be healthy and normal for clinical observation for 14 days following a single dose of AHC at 200 times the efficacy dose in acute toxicity study. No treatment-related clinical signs of toxicity and mortalities or gross pathological changes were observed in the animals. In the animals subjected to repeated doses of AHC for 15 and 30 days at 10 times the efficacy dose, hematological biochemical and clinical parameters were found to be normal in both control and treated groups (Tables 2, 3, and 4). The external and internal gross pathological examinations of control and AHC-treated groups did not show any significant changes. Treatment-related gross or microscopic changes were not noticed, and all the microscopic changes noticed were considered to be incidental and spontaneous in nature (Fig. 6).
Discussion
In the present study, we show that oral administration of AHC molecule induces an antigen-specific immune tolerance and impedes the development of atherosclerosis, although the effect slows down with time. As the diseases advances, the tolerance mechanism is besieged by inflammation and the level of protection drops from 60 to 20%. Interestingly, antibodies to native and modified LDL were found to increase in the later weeks. At this stage, we did not observe any difference in the Treg cells between control and treated animals, leading to speculation that these antibodies may play a role in protection, once the tolerance mechanism weans off. In our earlier studies, we have shown that oral administration of AHC molecule induces antigen-specific tolerogenic dendritic cells and regulatory T cells, which control plaque development in mice and rabbit models at a single time point of 12 weeks [24]. The concept of inducing immune tolerance to atherogenic proteins has been described by several groups for short duration, but this is the first study which has monitored the effect in a progressive manner from 6 to 30 weeks of age. Further, we have shown that the AHC molecule in both acute and repeated doses for 28 continuous days at 10 times the therapeutic dose does not show any adverse reactions in mice.
During the early phase of development of the atherosclerotic plaque, oral treatment with the AHC molecule showed remarkable protection of 60% and 45% at 6 and 12 weeks respectively. In control animals, 31% of the sinus was covered with the plaque at 12 weeks, but it took 18 weeks for the plaque to grow to 33% in the treated animal, suggesting that the tolerance mechanism effectively impedes plaque growth. Oral therapy was effective in controlling the plaque stability in the later stages of the disease by delaying the appearance of necrosis.
As observed in our earlier studies, induction of tolerance was associated with lower inflammation, an increase in regulatory T cells, and reduction in pro-inflammatory cell types in the plaque. Tolerance-induced regulatory T cells were observed to significantly increase in the spleen until 12 weeks. From 18 weeks onwards, the numbers were comparable between treated and control. In corroboration, the expression of FoxP3 and CTLA4 (markers related to Treg cells) and TGF-β (an anti-inflammatory cytokine) and tolerogenic dendritic cells (CD11b+11c+ and CD11c+103+) were significantly higher in 6 and 12 weeks in the plaque of treated animals, and progressively decreased, starting from 18 to 30 weeks. In contrast, the inflammatory monocytes (CD11b+Ly6c+) and the Th1 cells (CD4+ IFNγ+), which were lower in the treated animals until 12 weeks, showed an increase and were comparable with untreated controls at later time points. The gene expression ratio of arginase 1to arginase 2 was higher in the aorta up to 24 weeks but by 30 weeks arginase 2 expression was higher, suggesting the presence of M2 macrophage in the treated aorta which is replaced by M1 macrophages with time. These results reiterate our earlier findings that oral administration of the AHC molecule induces a regulatory response which is mediated by Tregs, tolerogenic dendritic cells, and alternatively activated macrophages (M2) which accumulate in the aortic sinus to cumulatively reduce aortic inflammation. Significantly, higher expression of CTLA4 in the sinus at early stages suggests that the Tregs may act by inhibiting the co-stimulatory molecules CD80 and CD86 in antigen presenting cells, thereby reducing the T cell activation [28, 29], which was seen by the reduction in Th1 cells in the treated animals.
The adaptive immune response is well recognized as a major mediator of inflammation in atherosclerosis [30, 31]. The role of antibodies in protection against atherosclerosis is still under debate [32]. Natural cross-reactive antibodies of the IGM class were reported to have a protective effect in animal studies [33,34,35]. Natural and protective antibodies have been described by several groups. These antibodies are secreted by a distinct set of B1 lymphocytes, which interact with self determinants and are reported to play a major role in immune homeostasis. The germline encoded B-1 cell natural antibody, T15, has been reported to interact with oxidation-derived epitopes on apoptotic cells and oxidized low-density lipoproteins and are protective in nature [36,37,38,39]. In a recent publication, Que. et al. [40] have elegantly shown that secretion of the single-chain variable fragment of the natural antibody by transgenic LDLr−/− mice reduced foam cell formation and inflammation.
Immunization with ox-LDL was found to elevate the levels of IgG antibodies reactive to MDA-LDL and oxidized phospholipids, which could be correlated with the reduction in the lesion in mice [41]. Immunization with p210 an ApoB100-derived peptide was not found to alter the p210-specific antibody levels Apo E−/− mice. However, the study found that mice receiving adjuvant only or p210 vaccine developed high p210 IgG titer at 25 weeks [18]. Another recent study using the peptide derived from apoB100-specific T cell hybridoma observed that peptide immunization induced antibodies which were responsible for the reduction in atherosclerosis. This study clearly demonstrated that antigen-specific humoral immunity could block a pro-atherogenic cellular immune response and have a protective role in atherosclerosis [41]. IgG antibodies to the Ox-LDL epitope were also found to be protective in other studies [42, 43]. Interestingly, we observed that IgM antibodies to LDL and OX-LDL were higher in untreated animals, but IgG antibodies to these two antigens increased in treated animals compared with control especially in the later weeks, when the regulatory immune response to the AHC molecule was much lower. Presence of antibodies to LDL raises a question of whether they can contribute to atheroprotection.
The results of this long-term study suggest that markers of immune tolerance decline by week 18, but still the protection is maintained at 20% until the 30 weeks. Low level of protection could be due to the background effect of immune tolerance, which slowed down the disease progression. Another possibility is the increase in protective antibody levels induced by tolerance which may have a role in controlling the lesion especially in the later stages of the disease.
Preclinical safety is an important aspect of any interventional therapy. In the preliminary toxicity studies, we observed that the AHC molecule was well tolerated in a different species of mice at a concentration as high as 10 times the therapeutic dose for 30 days repeated dosing. Thus the molecule is likely to have a safe therapeutic window, which can be ascertained by chronic toxicity studies.
The study has also opened a plethora of unanswered questions. Oral tolerance was induced at the age of 5–6 weeks in animals. Our results suggest that during the period between 12 to 18 weeks, the autoimmune mechanism seems to overpower the immune tolerance. Interestingly, the protection was maintained, albeit at a low level up to 30 weeks. Another dose of AHC during this period may activate the tolerance and prolong the protective effect, which needs to be explored in future studies. The molecular changes occurring during this stage may help us to understand the process of disease development and immune regulation and help us modify our approach of immune therapy for greater benefits. We are trying to understand the mechanisms by monitoring the gene expression changes during the disease progression.
Conclusion
In summary, we have shown that inducing immune tolerance to the AHC protein by oral administration is able to control the progression of atherosclerosis up to 30 weeks in Apobtm2sgy/LDLrtm1Her/J mice. The therapeutic molecule was also found to be safe for oral administration. Further studies on the mechanism of control of immune response and autoimmunity during atherosclerosis will be very helpful in fine-tuning the therapeutic modalities of immune modulation.
References
Fredrikson GN, Soderberg I, Lindholm M, Dimayuga P, Chyu KY, Shah PK, et al. Inhibition of atherosclerosis in apoE-null mice by immunization with apoB-100 peptide sequences. Arterioscler Thromb Vasc Biol. 2003;23(5):879–84.
Binder CJ, Horkko S, Dewan A, Chang MK, Kieu EP, Goodyear CS, et al. Pneumococcal vaccination decreases atherosclerotic lesion formation: molecular mimicry between Streptococcus pneumoniae and oxidized LDL. Nat Med. 2003;9(6):736–43.
Jun L, Jie L, Dongping Y, Xin Y, Taiming L, Rongyue C, et al. Effects of nasal immunization of multi-target preventive vaccines on atherosclerosis. Vaccine. 2012;30(6):1029–37.
Wick G, Knoflach M, Xu Q. Autoimmune and inflammatory mechanisms in atherosclerosis. Annu Rev Immunol. 2004;22:361–403.
Nilsson J, Hansson GK. Autoimmunity in atherosclerosis: a protective response losing control? J Intern Med. 2008;263(5):464–78.
Binder CJ, Papac-Milicevic N, Witztum JL. Innate sensing of oxidation-specific epitopes in health and disease. Nat Rev Immunol. 2016;16(8):485–97.
Miller YI, Choi SH, Wiesner P, Fang L, Harkewicz R, Hartvigsen K, et al. Oxidation-specific epitopes are danger-associated molecular patterns recognized by pattern recognition receptors of innate immunity. Circ Res. 2011;108(2):235–48.
Fontenot JD, Gavin MA, Rudensky AY. Foxp3 programs the development and function of CD4+CD25+ regulatory T cells. Nat Immunol. 2003;4(4):330–6.
Libby P, Lichtman AH, Hansson GK. Immune effector mechanisms implicated in atherosclerosis: from mice to humans. Immunity. 2013;38(6):1092–104.
Nilsson J, Fredrikson GN, Bjorkbacka H, Chyu KY, Shah PK. Vaccines modulating lipoprotein autoimmunity as a possible future therapy for cardiovascular disease. J Intern Med. 2009;266(3):221–31.
Binder CJ, Hartvigsen K, Witztum JL. Promise of immune modulation to inhibit atherogenesis. J Am Coll Cardiol. 2007;50(6):547–50.
Mor A, Planer D, Luboshits G, Afek A, Metzger S, Chajek-Shaul T, et al. Role of naturally occurring CD4+ CD25+ regulatory T cells in experimental atherosclerosis. Arterioscler Thromb Vasc Biol. 2007;27(4):893–900.
Mallat Z, Gojova A, Brun V, Esposito B, Fournier N, Cottrez F, et al. Induction of a regulatory T cell type 1 response reduces the development of atherosclerosis in apolipoprotein E-knockout mice. Circulation. 2003;108(10):1232–7.
Herbin O, Ait-Oufella H, Yu W, Fredrikson GN, Aubier B, Perez N, et al. Regulatory T-cell response to apolipoprotein B100-derived peptides reduces the development and progression of atherosclerosis in mice. Arterioscler Thromb Vasc Biol. 2012;32(3):605–12.
Wigren M, Kolbus D, Duner P, Ljungcrantz I, Soderberg I, Bjorkbacka H, et al. Evidence for a role of regulatory T cells in mediating the atheroprotective effect of apolipoprotein B peptide vaccine. J Intern Med. 2011;269(5):546–56.
Klingenberg R, Ketelhuth DF, Strodthoff D, Gregori S, Hansson GK. Subcutaneous immunization with heat shock protein-65 reduces atherosclerosis in Apoe(−)/(−) mice. Immunobiology. 2012;217(5):540–7.
Lu X, Xia M, Endresz V, Faludi I, Szabo A, Gonczol E, et al. Impact of multiple antigenic epitopes from ApoB100, hHSP60 and Chlamydophila pneumoniae on atherosclerotic lesion development in Apob(tm2Sgy)Ldlr(tm1Her) J mice. Atherosclerosis. 2012;225(1):56–68.
Chyu KY, Zhao X, Dimayuga PC, Zhou J, Li X, Yano J, et al. CD8+ T cells mediate the athero-protective effect of immunization with an ApoB-100 peptide. PLoS One. 2012;7(2):e30780.
Tse K, Gonen A, Sidney J, Ouyang H, Witztum JL, Sette A, et al. Atheroprotective vaccination with MHC-II restricted peptides from ApoB-100. Front Immunol. 2013;4:493.
Hermansson A, Ketelhuth DF, Strodthoff D, Wurm M, Hansson EM, Nicoletti A, et al. Inhibition of T cell response to native low-density lipoprotein reduces atherosclerosis. J Exp Med. 2010;207(5):1081–93.
Zhong Y, Tang H, Wang X, Zeng Q, Liu Y, Zhao XI, et al. Intranasal immunization with heat shock protein 60 induces CD4(+) CD25(+) GARP(+) and type 1 regulatory T cells and inhibits early atherosclerosis. Clin Exp Immunol. 2016;183(3):452–68.
Long J, Lin J, Yang X, Yuan D, Wu J, Li T, et al. Nasal immunization with different forms of heat shock protein-65 reduced high-cholesterol-diet-driven rabbit atherosclerosis. Int Immunopharmacol. 2012;13(1):82–7.
Mundkur L, Mukhopadhyay R, Samson S, Varma M, Kale D, Chen D, et al. Mucosal tolerance to a combination of ApoB and HSP60 peptides controls plaque progression and stabilizes vulnerable plaque in Apob(tm2Sgy)Ldlr(tm1Her)/J mice. PLoS One. 2013;8(3):e58364.
Mundkur L, Ponnusamy T, Philip S, Rao LN, Biradar S, Deshpande V, et al. Oral dosing with multi-antigenic construct induces atheroprotective immune tolerance to individual peptides in mice. Int J Cardiol. 2014;175(2):340–51.
Thota LN, Ponnusamy T, Philip S, Lu X, Mundkur L. Immune regulation by oral tolerance induces alternate activation of macrophages and reduces markers of plaque destabilization in Apobtm2Sgy/Ldlrtm1Her/J mice. Sci Rep. 2017;7(1):3997.
Sutcliffe MJ, Jaseja M, Hyde EI, Lu X, Williams JA. Three-dimensional structure of the RGD-containing neurotoxin homologue dendroaspin. Nat Struct Mol Biol. 1994;1(11):802–7.
Kumar PU, Kumar BD, Annapurna VV, Krishna TP, Kalyanasundaram S, Suresh P, et al. Nonclinical toxicology study of recombinant-plasmid DNA anti-rabies vaccines. Vaccine. 2006;24(15):2790–8.
Misra N, Bayry J, Lacroix-Desmazes S, Kazatchkine MD, Kaveri SV. Cutting edge: human CD4+CD25+ T cells restrain the maturation and antigen-presenting function of dendritic cells. J Immunol. 2004;172(8):4676–80.
Qureshi OS, Zheng Y, Nakamura K, Attridge K, Manzotti C, Schmidt EM, et al. Trans-endocytosis of CD80 and CD86: a molecular basis for the cell-extrinsic function of CTLA-4. Science. 2011;332(6029):600–3.
Libby P, Ridker PM, Hansson GK, Leducq Transatlantic Network on A. Inflammation in atherosclerosis: from pathophysiology to practice. J Am Coll Cardiol. 2009;54(23):2129–38.
Greaves DR, Channon KM. Inflammation and immune responses in atherosclerosis. Trends Immunol. 2002;23(11):535–41.
Nilsson J. Can antibodies protect us against cardiovascular disease? EBioMedicine. 2016;9:29–30.
Rothstein TL. Natural antibodies as rheostats for susceptibility to chronic diseases in the aged. Front Immunol. 2016;7:127.
Faria-Neto JR, Chyu KY, Li X, Dimayuga PC, Ferreira C, Yano J, et al. Passive immunization with monoclonal IgM antibodies against phosphorylcholine reduces accelerated vein graft atherosclerosis in apolipoprotein E-null mice. Atherosclerosis. 2006;189(1):83–90.
Binder CJ, Shaw PX, Chang MK, Boullier A, Hartvigsen K, Horkko S, et al. The role of natural antibodies in atherogenesis. J Lipid Res. 2005;46(7):1353–63.
Binder CJ, Silverman GJ. Natural antibodies and the autoimmunity of atherosclerosis. Springer Semin Immunopathol. 2005;26(4):385–404.
Shaw PX, Horkko S, Chang MK, Curtiss LK, Palinski W, Silverman GJ, et al. Natural antibodies with the T15 idiotype may act in atherosclerosis, apoptotic clearance, and protective immunity. J Clin Invest. 2000;105(12):1731–40.
George J, Afek A, Gilburd B, Levkovitz H, Shaish A, Goldberg I, et al. Hyperimmunization of apo-E-deficient mice with homologous malondialdehyde low-density lipoprotein suppresses early atherogenesis. Atherosclerosis. 1998;138(1):147–52.
Chang MK, Binder CJ, Miller YI, Subbanagounder G, Silverman GJ, Berliner JA, et al. Apoptotic cells with oxidation-specific epitopes are immunogenic and proinflammatory. J Exp Med. 2004;200(11):1359–70.
Que X, Hung MY, Yeang C, Gonen A, Prohaska TA, Sun X, et al. Oxidized phospholipids are proinflammatory and proatherogenic in hypercholesterolaemic mice. Nature. 2018;558(7709):301–6.
Murdaca G, Spano F, Cagnati P, Puppo F. Free radicals and endothelial dysfunction: potential positive effects of TNF-alpha inhibitors. Redox Rep. 2013;18(3):95–9.
Lehrer-Graiwer J, Singh P, Abdelbaky A, Vucic E, Korsgren M, Baruch A, et al. FDG-PET imaging for oxidized LDL in stable atherosclerotic disease: a phase II study of safety, tolerability, and anti-inflammatory activity. J Am Coll Cardiol Img. 2015;8(4):493–4.
Schiopu A, Frendeus B, Jansson B, Soderberg I, Ljungcrantz I, Araya Z, et al. Recombinant antibodies to an oxidized low-density lipoprotein epitope induce rapid regression of atherosclerosis in apobec-1(−/−)/low-density lipoprotein receptor(−/−) mice. J Am Coll Cardiol. 2007;50(24):2313–8.
Acknowledgments
We are extremely grateful to late Professor Vijay V Kakkar, Scientific Chairman, Thrombosis Research Institute, Bangalore for his constant encouragement and support. The support from Bharathi foundation for PhD students is gratefully acknowledged.
Funding
This work was supported by Thrombosis Research Institute, London and Bangalore, and Department of Biotechnology, Ministry of Science and Technology, Government of India (BT/01/CDE/08/07), and Bharathi Mittal foundation.
Author information
Authors and Affiliations
Contributions
The study was planned by LM and LNT. Experiments were carried out by LNT. The first draft of the manuscript was written by LNT. The manuscript was improvised by LM and LNT.
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Ethical Approval
Animal studies were performed and followed according to the CPCSEA guidelines and institute animal ethics committee.
Additional information
Publisher’s Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
ESM 1
(DOCX 451 kb)
Rights and permissions
About this article
Cite this article
Thota, L.N., Ponnusamy, T., Lu, X. et al. Long-Term Efficacy and Safety of Immunomodulatory Therapy for Atherosclerosis. Cardiovasc Drugs Ther 33, 385–398 (2019). https://doi.org/10.1007/s10557-019-06890-0
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10557-019-06890-0