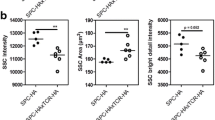
A comprehensive morphofunctional study of the lungs and alveolar macrophages was carried out in Sprague-Dawley rats with acute respiratory distress syndrome (n=10) induced by intratracheal administration of E. coli LPS 0111:B4 in a dose of 15 mg/kg. On the first day after LPS administration, bronchopneumonia was observed in the lungs, the number of macrophages of the bone marrow origin and the number of M1 macrophages with the proinflammatory phenotype in the bronchoalveolar lavage increased, the expression of proinflammatory cytokines increased and the expression of anti-inflammatory cytokines decreased, which was accompanied by an increase in LPS and C-reactive protein in the blood serum. The revealed changes correspond to the development of acute respiratory distress syndrome in humans, and the decrease in the number of macrophages in the lungs and their predominant polarization to the M1-proinflammatory phenotype substantiate the use of cell therapy with reprogrammed M2 macrophages.
Article PDF
Similar content being viewed by others
Avoid common mistakes on your manuscript.
References
Prompetchara E, Ketloy C, Palaga T. Immune responses in COVID-19 and potential vaccines: Lessons learned from SARS and MERS epidemic. Asian Pac. J. Allergy Immunol. 2020;38(1):1-9. doi: https://doi.org/10.12932/AP-200220-0772
Wu C, Chen X, Cai Y, Xia J, Zhou X, Xu S, Huang H, Zhang L, Zhou X, Du C, Zhang Y, Song J, Wang S, Chao Y, Yang Z, Xu J, Zhou X, Chen D, Xiong W, Xu L, Zhou F, Jiang J, Bai C, Zheng J, Song Y. Risk Factors Associated With Acute Respiratory Distress Syndrome and Death in Patients With Coronavirus Disease 2019 Pneumonia in Wuhan, China. JAMA Intern. Med. 2020;180(7):934-943. doi: https://doi.org/10.1001/jamainternmed.2020.0994
Banavasi H, Nguyen P, Osman H, Soubani AO. Management of ARDS - What Works and What Does Not. Am. J. Med. Sci. 2021;362(1):13-23. doi: https://doi.org/10.1016/j.amjms.2020.12.019
Wendisch D, Dietrich O, Mari T, von Stillfried S, Ibarra IL, Mittermaier M, Mache C, Chua RL, Knoll R, Timm S, Brumhard S, Krammer T, Zauber H, Hiller AL, Pascual-Reguant A, Mothes R, Bülow RD, Schulze J, Leipold AM, Djudjaj S, Erhard F, Geffers R, Pott F, Kazmierski J, Radke J, Pergantis P, Baßler K, Conrad C, Aschenbrenner AC, Sawitzki B, Landthaler M, Wyler E, Horst D; Deutsche COVID-19 OMICS Initiative (DeCOI); Hippenstiel S, Hocke A, Heppner FL, Uhrig A, Garcia C, Machleidt F, Herold S, Elezkurtaj S, Thibeault C, Witzenrath M, Cochain C, Suttorp N, Drosten C, Goffinet C, Kurth F, Schultze JL, Radbruch H, Ochs M, Eils R, Müller-Redetzky H, Hauser AE, Luecken MD, Theis FJ, Conrad C, Wolff T, Boor P, Selbach M, Saliba AE, Sander LE. SARS-CoV-2 infection triggers profibrotic macrophage responses and lung fibrosis. Cell. 2021;184(26):6243-6261.e27. doi: https://doi.org/10.1016/j.cell.2021.11.033
Lee YJ, Moon C, Lee SH, Park HJ, Seoh JY, Cho MS, Kang JL. Apoptotic cell instillation after bleomycin attenuates lung injury through hepatocyte growth factor induction. Eur. Respir. J. 2012;40(2):424-435. doi: https://doi.org/10.1183/09031936.00096711
Herold S, Gabrielli NM, Vadász I. Novel concepts of acute lung injury and alveolar-capillary barrier dysfunction. Am. J. Physiol. Lung Cell. Mol. Physiol. 2013;305(10):L665-L681. doi: https://doi.org/10.1152/ajplung.00232.2013
Matute-Bello G, Frevert CW, Martin TR. Animal models of acute lung injury. Am. J. Physiol. Lung. Cell. Mol. Physiol. 2008;295(3):L379-L399. doi: https://doi.org/10.1152/ajplung.00010.2008
Arber Raviv S, Alyan M, Egorov E, Zano A, Harush MY, Pieters C, Korach-Rechtman H, Saadya A, Kaneti G, Nudelman I, Farkash S, Flikshtain OD, Mekies LN, Koren L, Gal Y, Dor E, Shainsky J, Shklover J, Adir Y, Schroeder A. Lung targeted liposomes for treating ARDS. J. Control Release. 2022;346:421-433. doi: https://doi.org/10.1016/j.jconrel.2022.03.028
Zhou S, Wang G, Zhang W. Effect of TLR4/MyD88 signaling pathway on sepsis-associated acute respiratory distress syndrome in rats, via regulation of macrophage activation and inflammatory response. Exp. Ther. Med. 2018;15(4):3376-3384. doi: https://doi.org/10.3892/etm.2018.5815
Li W, Yang GL, Zhu Q, Zhong XH, Nie YC, Li XH, Wang Y. TLR4 promotes liver inflammation by activating the JNK pathway. Eur. Rev. Med. Pharmacol. Sci. 2019;23(17):7655-7662. doi: https://doi.org/10.26355/eurrev_201909_18889
Chen X, Tang J, Shuai W, Meng J, Feng J, Han Z. Macrophage polarization and its role in the pathogenesis of acute lung injury/acute respiratory distress syndrome. Inflamm. Res. 2020;69(9):883-895. doi: https://doi.org/10.1007/s00011-020-01378-2
Knoll R, Schultze JL, Schulte-Schrepping J. Monocytes and Macrophages in COVID-19. Front. Immunol. 2021;12:720109. doi: https://doi.org/10.3389/fimmu.2021.720109
Zhang D, Guo R, Lei L, Liu H, Wang Y, Wang Y, Qian H, Dai T, Zhang T, Lai Y, Wang J, Liu Z, Chen T, He A, O’Dwyer M, Hu J. Frontline Science: COVID-19 infection induces readily detectable morphologic and inflammation-related phenotypic changes in peripheral blood monocytes. J. Leukoc. Biol. 2021;109(1):13-22. doi: https://doi.org/10.1002/JLB.4HI0720-470R
Xie X, Sun S, Zhong W, Soromou LW, Zhou X, Wei M, Ren Y, Ding Y. Zingerone attenuates lipopolysaccharide-induced acute lung injury in mice. Int. Immunopharmacol. 2014;19(1):103-109. doi: https://doi.org/10.1016/j.intimp.2013.12.028
Monticelli LA, Buck MD, Flamar AL, Saenz SA, Tait Wojno ED, Yudanin NA, Osborne LC, Hepworth MR, Tran SV, Rodewald HR, Shah H, Cross JR, Diamond JM, Cantu E, Christie JD, Pearce EL, Artis D. Arginase 1 is an innate lymphoid-cell-intrinsic metabolic checkpoint controlling type 2 inflammation. Nat. Immunol. 2016;17(6):656-665. doi: https://doi.org/10.1038/ni.3421
Shapouri-Moghaddam A, Mohammadian S, Vazini H, Taghadosi M, Esmaeili SA, Mardani F, Seifi B, Mohammadi A, Afshari JT, Sahebkar A. Macrophage plasticity, polarization, and function in health and disease. J. Cell. Physiol. 2018;233(9):6425-6440. doi: https://doi.org/10.1002/jcp.26429
Author information
Authors and Affiliations
Corresponding author
Additional information
Translated from Byulleten’ Eksperimental’noi Biologii i Meditsiny, Vol. 175, No. 6, pp. 786-792, June, 2023
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kosyreva, A.M., Miroshnichenko, E.A., Tsvetkov, I.S. et al. Morphofunctional Characteristics of Lung Macrophages in Rats with Acute Respiratory Distress Syndrome. Bull Exp Biol Med 175, 822–827 (2023). https://doi.org/10.1007/s10517-023-05954-4
Received:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10517-023-05954-4