Abstract
People who identify as non-monosexual and transgender experience disparities in engagement with healthcare services relative to monosexual and cisgender persons, respectively. However, little is known about the healthcare utilization of those with intersecting sexual and gender minority identities. We explored the knowledge, attitudes, and health motivation of non-monosexually identified transgender participants regarding preventive care and access to sexual healthcare services. We surveyed 87 ciswomen, 34 transwomen, and 27 transmen, all of whom identified as bisexual, pansexual, or queer (bi+). We assessed their access to health care, health outcome experiences, confidence with talking about anogenital topics, proactivity toward their health, comfort with healthcare providers, and knowledge about HPV and examined differences across groups. The data indicated that bi+ transmen and transwomen were more likely to be uninsured or on a government-sponsored insurance plan relative to bi+ ciswomen. Only a minority of transmen and transwomen had seen an obstetrician/gynecologist compared with ciswomen. Transmen were less likely to have received a pelvic examination or cervical Pap smear in their lifetime. Transgender participants had significantly less correct knowledge about HPV relative to ciswomen. Finally, relative to ciswomen, transgender participants reported lower comfort talking with health providers. Our findings suggest that bi+ transmen and transwomen access care less than bi+ ciswomen and have less health knowledge and comfort with their providers. Implications for intervention include encouraging transgender individuals to seek routine screenings, reducing structural barriers to care based on medical coverage, and improving patient–provider competencies around bi+ and transgender health needs.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Bisexual people experience greater health disparities across multiple health risk factors and outcomes relative to heterosexual (Conron, Mimiaga, & Landers, 2010) and homosexual groups (Fredriksen-Goldsen et al., 2010). This is in part due to biphobia, which acts as a unique stressor that can lead to loneliness, psychological distress, and suicidality (Mereish, Katz-Wise, & Woulfe, 2017). Bisexual men have disproportionately higher rates of HIV and other sexually transmitted infections and are also at higher risk of HPV-related cancers (e.g., anal cancer) than heterosexual men (Friedman et al., 2014). Compared to other sexual minority women, bisexual women report lower rates of cervical Pap smears and mammograms, higher rates of unprotected sex, frequent use of emergency contraception and abortion, sex work, multiple sexual partners, and drug abuse (Chandra, Copen, & Stephen, 2013; Dilley, Simmons, Boysun, Pizacani, & Stakr, 2010; Friedman et al., 2014). Bisexual women are also more likely to be uninsured and have poorer socioeconomic status and, as a result, can have difficulty finding medical care (Diamant, Wold, Spritzer, & Gelberg, 2000; Solazzo, Gorman, & Denney, 2017).
People who are transgender also experience disparities in health and access to care (Bockting, Miner, Swinburne, Hamilton, & Coleman, 2013; Reisner et al., 2016). For example, transgender women (assigned male at birth, “transwomen”) have the highest rate of HIV in the U.S. (Baral et al., 2013). According to the Behavioral Risk Factor Surveillance System (BRFSS) Survey, transgender people were more likely to have a history of heart attacks than cisgender people, but did not differ on chronic illnesses such as diabetes, kidney disease, asthma, and cancers (Meyer, Brown, Herman, Reisner, & Bockting, 2017). They are also more likely to be uninsured, a major barrier to general and gender-affirming care (Khan, 2011; Meyer et al., 2017). Those who cannot afford gender-affirming care may resort to sharing needles for hormone or silicone injections, putting them at increased risk of contracting HIV or hepatitis C infection (Sanchez, Sanchez, & Danoff, 2009). Although not often included as a priority population for HIV/STIs, transgender men (assigned female at birth, “transmen”) are not impervious to those risks. Transmen who have sex with men have reported inconsistent condom use with partners (Sevelius, 2009). Transmen who use hormones may incorrectly believe they are not at risk of pregnancy due to their using testosterone and thus do not seek out proper sexual health care (Meriggiola & Gava, 2015). Transmen may feel uncomfortable asking for, or receiving, a cervical Pap smear or pelvic examination because of previous negative experiences (Semlyen & Kunasegaran, 2016). Overall, healthcare engagement can be difficult for transgender individuals, as they may experience misgendering, accidental or intended offensive language, or refusal to provide care (Johnson & Nemeth, 2014). From the provider perspective, education on the sexual health needs of transgender and other gender non-conforming people is lacking, so healthcare professionals may feel ill-prepared or uncomfortable treating them (Wylie et al., 2016). As such, trauma and stigma become unfortunate corollaries of transphobic attitudes, leading patients to eschew medical care or receive inadequate care.
Few studies have touched upon the sexuality of transgender people. Recent work suggests that bisexual-specific minority stress may impact bisexual transgender individuals more than cisgender individuals (Katz-Wise, Mereish, & Woulfe, 2017). Given that 9% of transgender people self-identify as bisexual compared to 3.95% as lesbian/gay and 1.92% as other (Meyer et al., 2017), more research specific to this group is needed. In response, we looked at the intersection of being both bisexual and transgender in terms of utilization of health services.
Method
Participant and Procedure
This study reflects the findings of a larger study conducted to assess health motivation, screening utilization, and knowledge of HPV and cancer. A cross-sectional survey was hosted online from July to October 2016 and targeted sexually active, English-speaking participants that did not identify as cisgender men. Participants accessed the survey through a link embedded in advertisement(s) for the study that were disseminated through LISTSERVs (e.g., American Public Health Association) and posted on various social media outlets/forums (e.g., Reddit, Twitter). Participants had to be 18 years old or older, sexually active, self-identified cisgender women, transgender men, or transgender women, and fluent in English. Upon completion of the 20-minute survey, participants could choose to be entered into a raffle for one of five prizes worth 20USD. We recruited 435 participants, 148 of whom qualified for the current analysis because they identified as either bisexual, pansexual, or queer (collectively, bi+). The analytic sample included cisgender women (n = 87), transgender women (n = 34), and transgender men (n = 27).
Measures
Demographics
We assessed sex/gender (i.e., male, female, transgender male, and transgender female), age, race/ethnicity, education, city size, and sexual orientation (i.e., straight, lesbian, bisexual, or other). Participants responding as “other” for sexual orientation could write in their own identification (e.g., queer, pansexual).
Access to Care and Medical Testing
We asked categorically for the type of insurance participants had and whether they had previously or ever seen, separately, a primary care provider, obstetrician/gynecologist (OB/GYN), and/or a nurse practitioner. Following that, participants reported if they had ever received a pelvic examination, cervical Pap smear, and/or anal Pap smear and whether any test was reported as abnormal. We also assessed whether participants were diagnosed with any STD(s) (chlamydia, gonorrhea, HIV, crabs, scabies or pubic lice, genital herpes, genital warts or asymptomatic HPV, hepatitis [any strain], syphilis, trichomoniasis) in the past year. HPV vaccination was also measured (yes, no, or not sure).
HPV Knowledge Scale
Knowledge of HPV was measured using 22 items (e.g., HPV is the virus that causes herpes; only gay men get HPV) on five-point scales ranging from 1 (100% false) to 5 (100% true) (Guvenc, Akyuz, & Açikel, 2011; Pitts, Fox, Willis, & Anderson, 2007). Items were averaged (i.e., divided by 22) and then multiplied by 20 to create a score out of 100 points, to mimic academic knowledge tests.
Confidence with Discussing Anogenital Sexual and Medical Aspects
Embedded in a section of the survey concerning HPV and anal cancer education, we ask participants how confident they were in discussing topics related to the anogenital region. These were split into two conceptual measures—sexual aspects and medical aspects. The topics that fell under sexual aspects were anal sex, rimming/anilingus, and pegging. Participants indicated confidence about discussing these aspects using a 5-point scale; scores were averaged and had good reliability (α = .84). The topics that fell under medical aspects were anal Pap smears, anal fissures, anal pain, anal warts, anal bleeding, hemorrhoids, and anal cancer. Again, participants indicated confidence about discussing these aspects using a 5-point scale. Scores were averaged and had excellent reliability (α = .95).
Proactivity Toward Health
Health proactivity was assessed through four items (e.g., “I look for new information to improve my health”; “I feel it is important to carry out activities which will improve my health.”). Participants agreed/disagreed using a five-point scale, which was averaged, with good reliability (α = .78). Higher scores reflected increased proactivity.
Comfort with Provider
Provider comfort was assessed through four items (e.g., “I don’t trust my doctor in general”; “I feel uncomfortable undressing for my doctor.”). Participants agreed/disagreed using a five-point scale, which was averaged, with good reliability (α = .77). Higher scores reflected more comfort.
Statistical Analysis
Chi-square analyses and ANOVA were performed using SPSS, version 20.0. Variations in sample size are noted in the results where they occurred. Missing data were minimal across the scales and were imputed using item-means.
Results
The Sample
As described in Table 1, the bi+ participants were mostly white and between the ages of 20 and 34. A majority had completed at least some college. In terms of population density, more than half of the bi+ transmen (51%) and bi+ transwomen (53%) lived in suburban or rural locations (populations under 100,000 people). The majority of bi+ cisgender women (54%), in contrast, lived in medium and large cities (above 100,000 people).
Access to Care
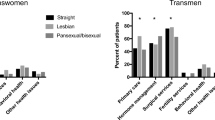
Table 2 describes the key sexual health outcomes measured across the bi+ participants. Transmen and transwomen were more likely to be uninsured or on a government-sponsored insurance plan relative to ciswomen, χ2(6) = 14.48, R2 = .05, p = .02. No differences were found across groups with respect to having seen a primary care physician or nurse practitioner; however, only a minority of transmen (48%) and transwomen (21%) had seen an OB/GYN compared to ciswomen (81%). Given the distributions, we calculated the number of bi+ participants that had seen no provider, one provider, or more than one provider in the past year. Only among transwomen did some individuals report never having seen a provider. Next, 22.2% of transmen and 34.48% of transwomen reported having seen one sort of provider. In contrast, 90.9% of ciswomen reported at least two or more provider visits, χ2(4) = 17.74, R2 = .12, p = .001.
Preventive Care
Only 9% of transwomen had received the HPV vaccine relative to majorities of ciswomen and transmen (both around 63%), χ2(4) = 38.41, R2 = .15, p < .001. One-third (37%) of transmen never received a pelvic examination or cervical Pap smear in their lifetime [pelvic examination: χ2(2) = 85.87, R2 = .48, p < .001; cervical Pap: χ2(2) = 87.99, R2 = .46, p < .001]. In comparison, 5% of ciswomen reported never being examined and roughly 10% reported never having had a cervical Pap. Notably, 18% of transwomen reported having had a pelvic examination. Regarding Pap smear results, 20% of ciswomen and 15% of transmen had received abnormal cervical results. Twenty-four percent of the sample reported having contracted some STIs within the past year, with herpes differentially impacting ciswomen (12.5%) compared to no reported cases among transmen and transwomen, χ2(2) = 12.19, R2 = .16, p = .002.
Sexual Health Knowledge and Attitudes
Transmen and transwomen had significantly less correct knowledge about HPV relative to ciswomen, F(2, 146) = 11.24, p < .001, R2 = .13, by − 4.82 and − 5.84 percentage points, respectively. All groups of participants reported similarly low levels of medical anogenital attitudinal confidence and similarly high levels of sexual anogenital attitudinal confidence. There were no differences regarding proactivity toward their health care. The final difference found among the groups was in their comfort with their providers, F(2, 146) = 5.22, p = .006, R2 = .07. Relative to ciswomen, transmen and transwomen reported lower comfort by − .50 and − .43 scale points, respectively (on a five-point scale).
Discussion
This is the first study to measure bi+ transgender people’s access to healthcare services. Consistent with previous findings (Katz-Wise et al., 2017), we identified disparities between bi+ cisgender and transgender individuals. For example, transgender participants reported lower access and utilization of health care (e.g., seeing an OB/GYN), with transwomen least likely to have seen a provider, received the HPV vaccine, or received a pelvic examination. Compared to ciswomen, transmen reported with greater frequency never receiving pelvic examinations or cervical Pap smears, despite a non-insubstantial frequency of abnormal results among transmen who had received the medical test. Potentially contributing to these gaps in healthcare utilization, transmen and transwomen were less comfortable with providers than were bi+ ciswomen. Lower health insurance coverage also indicates possible systemic barriers, limiting transgender patients from accessing preventive care. These findings indicate a lack of enabling factors that facilitate healthcare utilization among these populations (Gelberg, Andersen, & Leake, 2000). Individual differences in predisposing factors or perceived need (e.g., low awareness to see specific providers) may also impact transgender populations more acutely. Future work should continue to identify domains, especially those salient to vulnerable populations that perpetuate disparities (Gelberg et al., 2000).
Our results also suggest the need for interventions at multiple levels, including reducing structural barriers to care based on medical coverage, improving patient–provider competencies related to bisexual and transgender health needs, and creating targeted strategies to encourage transgender patients to seek routine screenings. Addressing these concerns will be no small feat. Biphobia and transphobia at the provider level are widespread and act as systemic disincentives to seek primary and secondary care (Johnson & Nemeth, 2014). At the patient level, transmen have been found to need motivation by their social and peer support to encourage genital screening (Semlyen & Kunasegaran, 2016), and transmen (and transwomen) may not have any awareness at all about seeing specialists (e.g., urologists or gynecologists) (Stephenson et al., 2017). Bisexuality adds an additional layer of identity for transmen and women, which may impact how they engage with healthcare providers and influence their experiences.
Limitations and Future Directions
The study was not without limitations. Our survey was cross-sectional and relied on participants to recall experiences, which may be influenced by recall bias. Participants were recruited through convenience sampling online, excluding anyone without Internet access, and the sample size was small, limiting generalizability. We also assessed sex assigned at birth and gender identity with only one item; thus, we may have underestimated the number of transgender people because some may have self-identified as “male” or “female” instead of “transgender male” or “transgender female.” Furthermore, many of our scales were created for this study and have not been previously validated; however, we reported acceptable reliability and believe face validity to be adequate. Validation of measures for this population should be an important focus of future work. Lastly, our study recruited mostly white participants, limiting the diversity of responses from other racial/ethnic groups. Recent data from the BRFSS Survey showed that transgender people are more likely to identify as racial/ethnic minorities (Meyer et al., 2017). These are all limitations that future research into transgender bisexuals should endeavor to correct. It is unclear how healthcare providers are trained on sexual history-taking for bisexual and transgender patients; it is similarly unclear whether clinical assessments of the intersection of sexuality and gender orientations are applied toward individuals’ health. Alternatively, as there are few other studies of bisexual transmen and transwomen in the literature, more targeted research with this group is necessary. Bi+ people experience more perceived stigma than other sexual orientation groups, which likely contributes to negative sexual health outcomes. The intersection with a transgender identity seems to exacerbate these outcomes.
References
Baral, S. D., Poteat, T., Strömdahl, S., Wirtz, A. L., Guadamuz, T. E., & Beyrer, C. (2013). Worldwide burden of HIV in transgender women: A systematic review and meta-analysis. Lancet, 13(3), 214–222.
Bockting, W. O., Miner, M. H., Swinburne Romine, R. E., Hamilton, A., & Coleman, E. (2013). Stigma, mental health, and resilience in an online sample of the US transgender population. American Journal of Public Health, 103(5), 943–951. https://doi.org/10.2105/AJPH.2013.301241.
Chandra, A., Copen, C. E., & Stephen, E. H. (2013). Infertility and impaired fecundity in the United States, 1982-2010: data from the National Survey of Family Growth (No. 2013). US Department of Health and Human Services, Centers for Disease Control and Prevention, National Center for Health Statistics.
Conron, K. J., Mimiaga, M. J., & Landers, S. J. (2010). A population-based study of sexual orientation identity and gender differences in adult health. American Journal of Public Health, 100(10), 1953–1960.
Diamant, A. L., Wold, C., Spritzer, K., & Gelberg, L. (2000). Health behaviors, health status, and access to and use of health care: A population-based study of lesbian, bisexual, and heterosexual women. Archives of Family Medicine, 9(10), 1043–1051.
Dilley, J. A., Simmons, K. W., Boysun, M. J., Pizacani, B. A., & Stark, M. J. (2010). Demonstrating the importance and feasibility of including sexual orientation in public health surveys: Health disparities in the Pacific Northwest. American Journal of Public Health, 100(3), 460–467.
Fredriksen-Goldsen, K. I., Kim, H. J., Barkan, S. E., Balsam, K. F., & Mincer, S. L. (2010). Disparities in health-related quality of life: A comparison of lesbians and bisexual women. American Journal of Public Health, 100(11), 2255–2261.
Friedman, M. R., Wei, C., Klem, M. L., Silvestre, A. J., Markovic, N., & Stall, R. (2014). HIV infections and sexual risk among men who have sex with men and women (MSMW): A systematic review and meta-analysis. PLoS ONE. https://doi.org/10.1371/journal.pone.0087139.
Gelberg, L., Andersen, R. M., & Leake, B. D. (2000). The behavioral model for vulnerable populations: Application to medical care use and outcomes for homeless people. Health Services Research, 34(6), 1273–1302.
Guvenc, G., Akyuz, A., & Açikel, C. H. (2011). Health belief model scale for cervical cancer and Pap smear test: psychometric testing. Journal of Advanced Nursing, 67(2), 428–437.
Johnson, M. J., & Nemeth, L. S. (2014). Addressing health disparities of lesbian and bisexual women: a grounded theory study. Women’s Health Issues, 24(6), 635–640.
Katz-Wise, S. L., Mereish, E. H., & Woulfe, J. (2017). Associations of bisexual-specific minority stress and health among cisgender and transgender adults with bisexual orientation. Journal of Sex Research, 54(7), 899–910.
Khan, L. (2011). Transgender health at the crossroads: Legal norms, insurance markets, and the threat of healthcare reform. Yale Journal of Health Policy, Law, and Ethics, 11, 375.
Mereish, E. H., Katz-Wise, S. L., & Woulfe, J. (2017). Bisexual-specific minority stressors, psychological distress, and suicidality in bisexual individuals: The mediating role of loneliness. Prevention Science, 18(6), 716–725. https://doi.org/10.1007/s11121-017-0804-2.
Meriggiola, M. C., & Gava, G. (2015). Endocrine care of transpeople part I. A review of cross-sex hormonal treatments, outcomes and adverse effects in transmen. Clinical Endocrinology, 83(5), 597–606.
Meyer, I. H., Brown, T. N., Herman, J. L., Reisner, S. L., & Bockting, W. O. (2017). Demographic characteristics and health status of transgender adults in select US regions: Behavioral Risk Factor Surveillance System, 2014. American Journal of Public Health, 107(4), 582–589. https://doi.org/10.2105/AJPH.2016.303648.
Pitts, M. K., Fox, C., Willis, J., & Anderson, J. (2007). What do gay men know about human papillomavirus? Australian gay men’s knowledge and experience of anal cancer screening and human papillomavirus. Sexually Transmitted Diseases, 34(3), 170–173.
Reisner, S. L., Poteat, T., Keatley, J., Cabral, M., Mothopeng, T., Dunham, E., … Baral, S. D. (2016). Global health burden and needs of transgender populations: A review. Lancet, 388, 401–411.
Sanchez, N. F., Sanchez, J. P., & Danoff, A. (2009). Health care utilization, barriers to care, and hormone usage among male-to-female transgender persons in New York City. American Journal of Public Health, 99(4), 713–719.
Semlyen, J., & Kunasegaran, K. (2016). Understanding barriers to cervical screening uptake in trans men: An exploratory qualitative analysis. Lancet, 388, S104. https://doi.org/10.1016/S0140-6736(16)32340-6.
Sevelius, J. (2009). “There’s no pamphlet for the kind of sex I have”: HIV-related risk factors and protective behaviors among transgender men who have sex with nontransgender men. Journal of the Association of Nurses in AIDS Care, 20(5), 398–410.
Solazzo, A. L., Gorman, B. K., & Denney, J. T. (2017). Cancer screening utilization among U.S. women: How mammogram and pap test use varies among heterosexual, lesbian, and bisexual women. Population Research and Policy Review, 36(3), 357–377.
Stephenson, R., Riley, E., Rogers, E., Suarez, N., Metheny, N., Senda, J., … Bauermeister, J. A. (2017). The sexual health of transgender men: A scoping review. Journal of Sex Research, 54(4–5), 424–445.
Wylie, K., Knudson, G., Khan, S. I., Bonierbale, M., Watanyusakul, S., & Baral, S. (2016). Serving transgender people: Clinical care considerations and service delivery models in transgender health. Lancet, 388, 401–411.
Acknowledgements
We would like to acknowledge the Division of Health Behavior and Community Health at the School of Health Sciences & Practice, New York Medical College, for its funding. We would also like to thank Dr. Greenberg, Dr. Liberatos, Dr. Watson, Atticus Ranck, Dr. Jason Ong, Dr. Brian Mustanski, and Dr. Brian Feinstein for their guidance, support, and advice.
Funding
This study was funded by the School of Health Sciences & Practice, New York Medical College.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Ethical Approval
All procedures performed in studies involving human participants were in accordance with the ethical standards of the institutional and/or national research committee and with the 1964 Declaration of Helsinki and its later amendments or comparable ethical standards.
Informed Consent
A waiver of informed consent was granted by the Institutional Review Board at New York Medical College.
Rights and permissions
About this article
Cite this article
Rahman, M., Li, D.H. & Moskowitz, D.A. Comparing the Healthcare Utilization and Engagement in a Sample of Transgender and Cisgender Bisexual+ Persons. Arch Sex Behav 48, 255–260 (2019). https://doi.org/10.1007/s10508-018-1164-0
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10508-018-1164-0