Abstract
Remifentanil postconditioning (RPC) elicits cardioprotection against ischemia/reperfusion injury (IRI) by attenuating apoptosis associated with endoplasmic reticulum stress (ERS). Histone H3, acetylation modifications of histone H3, and histone deacetylases (HDAC) also have key roles in the mediation of the survival and apoptosis of cardiomyocytes. In this study, an in vitro IRI model was established with H9c2 cardiomyoblasts to investigate the role of histone H3 acetylation and HDAC3 in RPC-induced attenuation of ERS-associated apoptosis. Briefly, H9c2 cardiomyoblasts were randomly subjected to hypoxia/reoxygenation with and without remifentanil administered at the onset of reoxygenation. Results showed that RPC increased cell viability and prevented cell apoptosis (evidenced by CCK-8 cell viability assays and flow cytometry), and these effects were accompanied by lower levels of expression of GRP78, CHOP, cleaved caspase-12, and cleaved caspase-3. RPC also mimicked the effects of SAHA by increasing the amount of histone H3 deacetylation and decreasing up-regulation of HDAC at both the mRNA and protein levels in response to HR. Finally, RPC-induced protective effects against HR, including attenuation of ERS-associated protein markers, deacetylation of histone H3, and down-regulation of HDAC3 were completely abolished by pretreatment with thapsigargin (TG, a specific ERS activator). In contrast, these effects were not found to be enhanced after pretreatment with 4-phenyl butyric acid (4-PBA, a widely used ERS inhibitor). The present results demonstrate that RPC protects H9c2 cardiomyoblasts from HR injury, and this protection involves an attenuation of ERS-associated apoptosis, which mediates a reduction in HDAC3 expression and an increase in histone H3 deacetylation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Myocardium ischemia/reperfusion injury (IRI) contributes to high rates of morbidity and mortality in patients with coronary artery disease, myocardial ischemia, or both during the perioperative period [1]. The administration of opioid analgesics at the onset of reperfusion is referred to as opioid postconditioning (OPC), and this treatment has been widely proven to limit ischemic damage to myocardium tissue [2, 3]. In particular, remifentanil is an ultra-short-acting opioid analgesic agent that is widely used for clinical anesthesia. Remifentanil is rapidly metabolized and has little influence on blood flow [4, 5]. We previously demonstrated that remifentanil postconditioning (RPC) conferred robust cardioprotection against IRI both in preclinical [6] and clinical settings [7]. However, in order to effectively translate laboratory evidence of OPC-induced cardioprotection into daily clinical practice, the underlying mechanisms need to be elucidated.
The endoplasmic reticulum has attracted a great deal of attention because of its role as an effector for a diverse set of cardioprotective strategies, while also being a target of myocardium IRI [8–10]. In ischemic myocardial tissue, the supply of oxygen and nutrients is disrupted, and this adversely affects the homeostasis of the endoplasmic reticulum and induces endoplasmic reticulum stress (ERS) [8, 9]. Subsequently, the unfolded protein response is triggered, which involves PKR-like ER kinase (PERK), transcription factor 6 (ATF6), and inositol-requiring enzyme-1α (IRE1) pro-survival signaling [8]. Prolonged, intense pathological stress triggers excessive ERS and cell apoptosis via activation of the pro-apoptotic transcription factor, c-Jun N-terminal kinase (JNK), and caspase-12 and C/EBP homologous protein (CHOP). It has previously been demonstrated that attenuation of ERS-associated apoptosis is involved in RPC-induced cardioprotection [6]. While systemic and cellular responses to ERS-associated apoptosis have been characterized, the effect of ERS-associated apoptosis on nuclear DNA fragmentation that is triggered by ERS in ischemic cardiomyocytes remains unclear.
Histones are the basic structural components of nucleosomes and they organize chromatin in eukaryotic cells. Of the five types of histones present in the nucleus, histone H3 and its associated acetylation are reported to play key roles in regulating chromatin remodeling and gene transcription in mammalian cells [11]. It is here hypothesized that apoptotic signals may trigger the release of H3 and other core histones from genomic DNA and induce their translocation into the extracellular space [12]. Hyperacetylation of H3 has been shown to contribute to the accumulation of histone H3 in the extracellular space and to correspond with cell apoptosis [13]. The important roles that histones and their acetylation modifications have in IRI and tissue injury have also been demonstrated in the kidney [14], liver [15], and lung [16]. In mice, chronic exposure to opioids has been found to be associated with acetylation of histone H3 at the K9 site in spinal cord tissue [17]. However, the roles of histone H3 and acetylation of histone H3 in myocardium IRI, as well as in RPC-induced attenuation of ERS-associated apoptosis, remain unknown.
Histone modifications are regulated by histone acetyltransferases (HATs) and histone deacetylases (HDACs). Inhibitors of HDACs can block the catalytic activity of both class I and class II HDACs and have been reported to confer robust protection against IRI in myocardium tissue [18]. HDAC3 is a member of the class I HDAC family and has been proposed to regulate cardiac growth, proliferation, differentiation, and hypertrophy [19]. However, HDAC3 has not previously been linked to cardiovascular disease or myocardial IRI. For this reason, the aims of this study were to identify the roles of modified histone H3 acetylation and HDAC3 in RPC-induced cardioprotection and to elucidate their possible relationship in regard to attenuation of ERS-associated apoptosis in H9c2 cardiomyoblasts.
Methods
Cell culture
H9c2 cardiomyocytes were obtained from the American Type Culture Collection (ATCC, U.S.) and were cultured in DMEM/F12 medium (Hyclone, U.S.) supplemented with 10% (v/v) fetal bovine serum (Wisent, Australia) and 1% (v/v) penicillin–streptomycin solution. Cells were maintained at 37 °C in 95% O2/5% CO2. Upon reaching 90% confluency, the cells were passaged with 0.25 mM trypsin/0.03% EDTA (Wisent, Australia). The 3rd through 10th cell passages were used for the experiments.
Experimental hypoxia and preconditioning
H9c2 cardiomyoblasts were seeded in 6-well or 96-well plates at 1 × 104 cells/cm2 and fresh medium was provided prior to each experiment. Briefly, H9c2 cells were pretreated with 1 mM 4-PBA (a widely used ERS inhibitor) for 2 h, or with a specific ERS activator, TG (0.1 mM) for 12 h. Both sets of cells were then subjected to HR with or without exposure to RPC or SAHA (a widely-used HDACs inhibitor; Sigma, U.S.) for post-conditioning. An HR model was established as previously described [20]. Briefly, cells were incubated in a hypoxic chamber (Adelbio, Clermont-Ferrand, France) at 37 °C with 95% N2/5% CO2 and in culture medium containing a tyrode solution (130 mM NaCl, 5 mM KCl, 10 mM HEPES, 1 mM MgCl2, 1.8 mM CaCl2 at pH 7.4) to simulate ischemia. After 5 h, the cells were moved to an incubator with 95% O2/5% CO2 and the medium was replaced with standard DMEM/F12 medium for 1 h of reoxygenation to simulate reperfusion. The latter reoxygenation step also included postconditioning with varying concentrations of remifentanil (0.1, 1, or 10 μM) or SAHA (2 μM) as indicated.
Cell viability assay
Cell viability was measured by using the CCK-8 Counting Kit (Vazyme, U.S.). Briefly, cells were seeded in 96-well plates at 1 × 104 cells/well. After reoxygenation, the cells were incubated with CCK8 at a final concentration of 0.5 mg/mL. After 4 h, absorbance measurements at 570 nm were recorded by a microplate reader (Tecan Infinite M1000, Austria).
Cell apoptosis assay
Cell apoptosis was detected with an Annexin V-FITC/propidium iodide (PI) kit (Bestbio, China) and measured with flow cytometry. Briefly, cells were trypsinized and then washed twice with cold phosphate-buffered saline (PBS). After the cells were resuspended in binding buffer, they were incubated with 10 μL Annexin V-FITC for 15 min and then incubated with 5 μL PI for 5 min in the dark at 4 °C. The samples were analyzed using a FACScan Flow Cytometer (BD Biosciences, U.S.) and associated software.
Quantitative real-time PCR
Total RNA was extracted from treated and control H9c2 cells using TRIzol reagent (Thermo Fisher Scientific, U.S.). The RNA samples were then reverse-transcribed with a HiScript II 1st Strand cDNA Synthesis Kit (Vazyme, U.S.). The resulting cDNAs were combined with SYBR Green qPCR Master Mix (TaKaRa, Japan) and triplicate samples were added to optically clear 96-well plates (Corning, U.S.). The cycling parameters used for an ABI Prism 7500 sequence detector (Biosystems, U.S.) were: 95 °C for 10 min, followed by 40 cycles of 95 °C for 15 s, 60 °C for 1 min, and 72 °C for 30 s. HDAC3 forward (5′-GCCTCTGGCTTCTGCTATGT-3′) and reverse (5′-GCTGATGACTGGCTGGAAA-3′) primers were included in the reactions. Amplification of GAPDH was performed as a control. The relative levels of target mRNA expression were calculated using the 2−ΔΔCt method.
Western blotting
H9c2 cells were collected and lysed in a RIPA buffer (Vazyme, U.S.) containing phenylmethanesulfonyl fluoride (PMSF; Amresco, U.S.) at 4 °C. A BCA protein assay kit (Beyotime Institute of Biotechnology, China) was used to measure total protein concentration according to the manufacturer’s protocol. Protein samples were separated on 12% SDS-PAGE gels and transferred to PVDF membranes (Bio-Rad, U.S.). The membranes were blocked in 5% nonfat milk for 2 h and then incubated with primary antibodies raised against GRP78 (1:1000, Abcam, U.K.), CHOP (1:100, Santa Cruz, U.S.), caspase-12 (1:1000, Cell Signaling, U.S.), cleaved caspase-3 (1:1000, Cell Signaling, U.S.), Acetyl-Histone H3 (Lys9) (1:1000, Cell Signaling, U.S.), Histone H3 (1:1000, Cell Signaling, U.S.), HDAC3 (1:1000, Cell Signaling, U.S.), and GAPDH (1:1000, Abcam, U.S.) overnight at 4 °C. The membranes were washed three times (10 min each) with PBS-T and then incubated with the corresponding horseradish peroxidase (HRP)-conjugated secondary antibodies (1:8000, Abcam, U.S.) for 1 h at room temperature. After the membranes were washed again with PBS-T 3×, bound antibodies were visualized with enhanced ECL reagent (Thermo Scientific, U.S.) and analyzed using Quantity One software (Bio-Rad Laboratories, U.S.). Detection of GAPDH was used as a control.
Statistical analysis
Data are presented as the mean ± standard deviation (SD). One-way analysis of variance (ANOVA) with the Student–Newman–Keuls post-test was used for comparisons of data between groups. P-values below 0.05 were considered indicative of statistical significance.
Results
RPC protects H9c2 cardiomyoblasts against HR injury
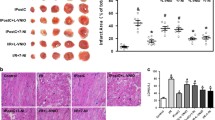
An HR model with H9c2 cardiomyoblasts was established as described in a previous work [16]. To evaluate the potential cardioprotective capacity of RPC for H9c2 cardiomyoblasts subjected to HR, CCK-8 assays and Annexin V-FITC/PI flow cytometry assays were performed. After HR, a significant reduction in cell viability (from 0.89 ± 0.05 to 0.38 ± 0.12, P < 0.05) (Fig. 1A) and an increase in cell apoptosis (from 5.8 ± 2.2 to 31.5 ± 5.1, P < 0.05) (Fig. 1B, C) relative to controls were observed in these assays. However, there was no significant difference between cell viability or the rate of apoptosis for the H9c2 cells that were pretreated with 0.1 μM remifentanil (0.38 ± 0.03 and 29.1 ± 4.8, respectively) and the HR group (P > 0.05). In contrast, remifentanil at concentrations of 1 or 10 μM increased cell viability (from 0.38 ± 0.12 to 0.81 ± 0.02, 0.82 ± 0.03, vs HR, P < 0.05) and decreased the rate of cell apoptosis (from 31.5 ± 5.1 to 15.4 ± 3.8, 15.3 ± 3.7, vs. HR, P < 0.05) (Fig. 1A–C). These data indicate that concentrations of RPC between 1 and 10 μM protect H9c2 cardiomyoblasts from HR injury by increasing cell viability and attenuating cell apoptosis.
RPC protects H9c2 cardiomyoblasts from HR injury. H9c2 cardiomyoblasts were exposed to 5 h of hypoxia and then 1 h of reoxygenation with or without remifentanil (0.1, 1, or 10 μM), which was administered at the onset of reoxygenation (RPC). A Cell viability was detected with CCK-8 assays. B Cell apoptosis was detected with Annexin V-fluorescein isothiocyanate (FITC)/propidium iodide (PI) staining and flow cytometry. Apoptosis rates are expressed as the relative number of apoptotic cells versus total cells. C Representative scatter plots of the flow cytometry data for each group. CON control, HR hypoxia reoxygenation, RPC remifentanil postconditioning. *P < 0.05 versus CON; # P < 0.05 versus HR
RPC suppresses HR-induced ERS to alleviate ERS-associated apoptosis and provide cardioprotection in H9c2 cardiomyoblasts
To confirm the involvement of ERS in HR-induced apoptosis, and the role of RPC-induced cardioprotection, the expression levels of the ERS biomarker, GRP78, and the ERS-associated apoptotic markers, CHOP, cleaved caspase-12, and cleaved caspase-3 were analyzed in H9c2 cardiomyoblasts subjected to HR. Significantly more expression was observed for all four proteins than in the control group (P < 0.05) (Fig. 2). When the H9c2 cells were pretreated with remifentanil at concentrations of 1 or 10 μM prior to HR, reduced up-regulation of the four proteins was observed in response to HR (P < 0.05). In addition, pretreatment with 0.1 μM remifentanil had no effect (P > 0.05) (Fig. 2). These results suggest that concentrations of RPC between 1 and 10 μM are capable of preventing HR-induced ERS and ERS-associated apoptosis. For this reason, 1 μM remifentanil was selected as the minimal effective concentration for subsequent experiments.
Effects of RPC (0.1, 1, 10 μM) on levels of expression of the ERS biomarker GRP78 and the ERS-associated apoptotic markers CHOP, cleaved caspase-12, and cleaved caspase-3, in H9c2 cardiomyoblasts. A Western blot analysis of GRP78, CHOP, cleaved caspase-12, and cleaved caspase-3 levels in H9c2 cells exposed to HR injury with or without RPC. Detection of GAPDH was used as a loading control. B Western blot data were analyzed by Quantity One and protein levels of ERS-associated biomarkers were normalized to GAPDH. CON control, HR hypoxia reoxygenation, RPC remifentanil postconditioning. *P < 0.05 versus CON; # P < 0.05 versus HR
RPC increases HR-induced deacetylation of histone H3 and attenuates up-regulation of HDAC3 mRNA and protein in H9c2 cardiomyoblasts
To investigate the expression levels of acetylated histone H3 and HDAC3, Western blotting was performed. The HDAC inhibitor, SAHA, was included as a positive control. After HR treatment, acetylation of histone H3 decreased (P < 0.05) (Fig. 3A, B), while expression of HDAC3 was higher than in control cells (P < 0.05) (Fig. 3C, D). Following SAHA and remifentanil (1 μM) post-conditioning, a significant increase in histone H3 deacetylation (P < 0.05) (Fig. 3A, B) and a reduction in HDAC up-regulation (P < 0.05) (Fig. 3C, D) were detected.
Effects of RPC and SAHA on histone H3 acetylation and mRNA and protein levels of HDAC3 in H9c2 cardiomyoblasts exposed to HR injury. Western blot analysis of A acetylated histone H3 normalized to total histone H3 and C HDAC3 normalized to GAPDH. Relative protein levels of B acetylated histone H3 and D HDAC3 as quantified by Quantity One. E Relative mRNA levels of HDAC3 detected by quantitative real-time PCR. CON: control group not exposed to HR injury. CON control, HR hypoxia reoxygenation, RPC remifentanil postconditioning, Ac H3 acetylation of histone H3. *P < 0.05 versus CON; # P < 0.05 versus HR
We next investigated whether HDAC3 is down-regulated at the transcriptional level during RPC. After HR, significantly more HDAC3 mRNA was observed than in the control group (1.8 ± 0.02, P < 0.05) (Fig. 3E). However, SAHA and remifentanil (1 μM) post-conditioning resulted in a decrease in the up-regulation of HDAC3 mRNA in response to HR (from 1.8 ± 0.02 to 0.64 ± 0.03, 0.68 ± 0.04, vs. HR, P < 0.05) (Fig. 3E). These data indicate that down-regulation of HDAC3, accompanied by hyperacetylation of histone H3, mediates the protective effect of RPC against HR injury.
Attenuation of ERS-associated apoptosis is essential in RPC-induced cardioprotection in H9c2 cardiomyoblasts
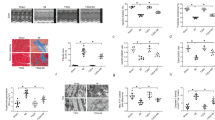
To determine whether attenuation of ERS-associated apoptosis is a consequence of RPC, the H9c2 cells were pretreated with 4-PBA as a positive control and with TG as a negative control. As shown in Fig. 4A, B, RPC significantly reduced the increase in expression of GRP78, CHOP, and cleaved caspase-12 that had been induced by HR (P < 0.05) (Fig. 4A, B). Similarly, RPC and 4-PBA increased cell viability (from 0.43 ± 0.09 to 0.86 ± 0.09, 0.70 ± 0.09 vs. HR, P < 0.05), reduced cell apoptosis relative to the HR group (from 23.1 ± 21.1 to 7.2 ± 6.3, 11.9 ± 11.0 vs. HR, P < 0.05) (Fig. 4C, D). These protective effects of RPC did not further increase in the presence of 4-PBA (0.79 ± 0.07, 9.0 ± 8.2 in 4-PBA-RPC group), yet were blunted by TG (0.38 ± 0.07, 21.4 ± 19.6 in TG group, 0.45 ± 0.03, 20.5 ± 18.7 in TG-RPC group, respectively, P > 0.05). Similarly, 4-PBA treatment did not further increase cell viability or reduce cell apoptosis compared to HR and RPC (P > 0.05). However, pretreatment with TG completely abolished the increase in cell viability and the decrease in cell apoptosis mediated by RPC (0.38 ± 0.07, 21.4 ± 19.6 in TG group, 0.45 ± 0.03, 20.5 ± 18.7 in TG-RPC group, respectively, P < 0.05). Taken together, these data demonstrate that attenuation of ERS-associated apoptosis plays a major role in RPC-induced protection against HR injury.
Attenuation of ERS-associated apoptosis is responsible for RPC-induced cardioprotection in H9c2 cardiomyoblasts. H9c2 cells were pretreated with 1 mM 4-PBA or 0.1 mM TG for 2 or 12 h, respectively, before HR. The two sets of cells were also subjected to HR with or without exposure to RPC (1 μM). A Western blot analysis of GRP78, CHOP, cleaved caspase-12, and cleaved caspase-3 levels in H9c2 cells exposed to HR injury with and without RPC. Detection of GAPDH was used as a loading control. B Protein levels of ERS-associated biomarkers were normalized to GAPDH and quantified by Quantity One. C Cell viability was detected in CCK-8 assays. D Cell apoptosis was stained with annexin V-fluorescein isothiocyanate (FITC)/propidium iodide (PI) and analyzed by flow cytometry. Apoptosis rates are expressed as the percentage of apoptotic cells versus total cells. E Representative scatter plots of the annexin V-FITC/PI flow cytometry data for each group. CON control, HR hypoxia reoxygenation, RPC remifentanil postconditioning. *P < 0.05 versus CON; # P < 0.05 versus HR
Attenuation of ERS-associated apoptosis is induced by RPC and it mediates hyperacetylation of histone H3 and down-regulation of HDAC3 in H9c2 cardiomyoblasts
As shown in Fig. 5, H9c2 cells that were pretreated with 4-PBA prior to HR and RPC did not exhibit any further increase in histone H3 hyperacetylation or up-regulation of HDAC3 compared to cells subjected to HR and RPC (P > 0.05) (Fig. 5). In contrast, pretreatment with TG dramatically abolished RPC-induced protective effects against HR, attenuation of ERS-associated protein markers, deacetylation of histone H3, and down-regulation the protein expression of HDAC3 and the mRNA expression (1.4 ± 0.54 in HR, 0.73 ± 0.08 in RPC, 0.70 ± 0.01 in 4-PBA, 0.62 ± 0.09 in 4-PBA-RPC, 1.8 ± 0.14 in TG, 1.8 ± 0.06) (Fig. 5), (P > 0.05). These results indicate that attenuation of ERS-associated apoptosis in response to RPC involves acetylation of histone H3 and suppression of HDAC3.
RPC attenuates ERS-associated apoptosis, which itself induces hyperacetylation of histone H3 and down-regulation of HDAC3 in H9c2 cardiomyoblasts. Western blot analysis of A acetylated histone H3 normalized to total histone H3 and C HDAC3 normalized to GAPDH. Relative protein levels of B acetylated histone H3 and D HDAC3 as quantified by Quantity One. E Relative mRNA levels of HDAC3 detected by quantitative real-time PCR. CON: control group not exposed to HR injury. CON control, HR hypoxia reoxygenation, RPC remifentanil postconditioning, Ac H3 acetylation of histone H3. *P < 0.05 versus CON; # P < 0.05 versus HR
Discussion
Myocardium IRI induces apoptosis in significant numbers of cardiomyocytes and is also considered the basic mechanism that underlies many forms of cardiovascular disease. Acetylation of histone H3 has been identified as a key regulator of chromatin remodeling and gene transcription and has also been implicated in the process of IRI and tissue injury [11]. For this reason, it has been hypothesized that acetylation of histone H3 may serve as a biomarker or novel therapeutic target in efforts to prevent or minimize IRI in the myocardium. The present study provides in vitro evidence that RPC can protect H9c2 cardiomyoblasts from HR injury by attenuating ERS-associated apoptosis and HDAC3 expression, while increasing acetylation of histone H3. Moreover, the present results indicate that RPC induces attenuation of ERS-associated apoptosis which subsequently mediates hyperacetylation of histone H3 and suppression of HDAC3 to provide a protective effect against HR injury.
In both preclinical and clinical studies, substantial evidence has indicated that remifentanil is able to confer robust cardioprotection against IRI [2, 7]. In the present study, a decrease in cell viability and an increase in cell apoptosis in response to HR were ameliorated by postconditioning treatment with 1 or 10 μM remifentanil that was administered at the onset of the reoxygenation step. In this way, RPC appears to confer a cardioprotective effect at the cardiomyocyte level in a dose-dependent manner. In other studies, remifentanil triggered intracellular anti-apoptotic signaling and alleviated cell apoptosis in ischemic myocardium through the activation of opioid receptors [2]. Remifentanil has been shown to have a high affinity for μ-receptors and a lower affinity for δ- and κ-receptors [21]. After IR, reduction of myocardial infarct size by remifentanil has been found to involve cardiac δ- and κ-receptors, and not μ-receptors [21]. Activation of opioid receptor signaling has also been found to play an important role in histone acetylation, especially acetylation of histone H3 at the K9 site in spinal tissue [22]. However, the role of histone H3 acetylation in RPC-induced cardioprotection against IRI has not previously been reported.
Histone H3 is a core histone that binds DNA to form nucleosomes [23]. Histones can undergo post-translational modifications, and modified acetylation at the K9 site of H3 has been shown to affect gene transcription [11]. Stimuli from IR and tissue injury have been shown to disturb acetylation modifications of histone H3 to regulate gene transcription and cause cell injury [14, 24, 25]. Hyperacetylation of histone H3 also mediates a protective effect against IRI injury and other tissue injuries by regulating related gene transcription [14]. As a class I HDAC, HDAC3 contributes to the regulation of histone acetylation. HDAC inhibitors that suppress the activation of class I HDACs have been found to be associated with robust cardioprotection [18, 26]. In the present study, HR attenuated histone H3 acetylation and increased HDAC3 expression in H9c2 cells, and these results are consistent with those of previous studies of IR in kidney [14]. RPC also mimics the effects of SAHA by significantly down-regulating expression of HDAC3 and enhancing acetylation of histone H3 in the H9c2 cardiomyocytes. However, the regulatory role of gene transcription in the experiments performed was not assayed in the present study.
Accumulating evidence indicates a role for ERS in the pathology of myocardium IRI [19]. In previous studies, prolonged ERS resulted in cell apoptosis that included activation of CHOP and caspase-12 pro-apoptotic signaling. CHOP regulates transcription and promotes apoptosis [27, 28], while localization of caspase-12 to the endoplasmic reticulum initiates caspase signaling cascades to up-regulate caspase-3 in response to sustained stimuli [29]. Inhibition of ERS-associated apoptosis has been reported to play a role in the protective effect against IRI that is mediated by HDAC inhibitors and other protective strategies [19, 30]. In the present study, RPC led to reduced upregulation of CHOP, cleaved caspase-12, and cleaved caspase-3 in response to HR and increased cell viability and reduced cell apoptosis. However, all these effects of RPC were abolished by the specific ERS activator, TG, and were not further promoted by the ERS inhibitor, 4-PBA. Taken together, these results indicate that attenuation of ERS-associated apoptosis is responsible for the protective effects induced by RPC against HR injury in H9c2 cardiomyoblasts.
It was here observed that 4-PBA down-regulated HDAC3 and increased acetylation of histone H3 similar to SAHA and RPC. TG, which inhibited the attenuation of ERS-associated apoptosis, also down-regulated expression of HDAC3, yet abolished RPC-induced hyperacetylation of H3. These results indicate the essential role of attenuated ERS-associated apoptosis in the hyperacetylation of H3 and suppression of HDAC3, and these results are consistent with the results of previous studies. For example, Zhang et al. found that Valproate, which inhibits the activity of HDACs and facilitates the hyperacetylation of H3, induced protective effects in a retinal IRI model by alleviating ERS-associated apoptosis [31]. In addition, SIRT1, a class III HDAC, was found to trigger ERS via the PI3K-Akt-GSK3β signaling pathway [32].
The current study has some limitations. First, the experimental model employed used a cultured cell line and did not fully mimic clinical conditions. Second, the possibility that gene transcription may be regulated by RPC-induced hyperacetylation of H3 was not investigated. Finally, the relationship between HDAC3 and hyperacetylation of H3 could not be elucidated based on the experiments that were performed.
High concentrations of serum nucleosomes have been detected in patients affected by cerebral stroke, especially patients with large infarction volumes [33]. Elevated serum levels of histones and nucleosomes have also been implicated in multiple pathophysiological processes and the progression of various diseases [11]. To date, histones, histone acetylation modifications, and HDACs, appear to represent targets in IRI and related cardioprotective strategies. In the present study, HDAC3 and acetylation of histone H3 represented downstream targets of RPC-induced attenuation of ERS in an experimental IRI model of H9c2 cardiomyoblasts. It is anticipated that the present results can be translated into a clinical strategy to provide cardioprotection via RPC upon further study.
References
Xia Z, Li H, Irwin MG (2016) Myocardial ischaemia reperfusion injury: the challenge of translating ischaemic and anaesthetic protection from animal models to humans. Br J Anaesth 117(suppl 2):ii44–ii62. doi:10.1093/bja/aew267
Tanaka K, Kersten JR, Riess ML (2014) Opioid-induced cardioprotection. Curr Pharm Des 20(36):5696–5705
Irwin MG, Wong GT (2015) Remifentanil and opioid-induced cardioprotection. J Cardiothorac Vasc Anesth 29(Suppl 1):S23–S26. doi:10.1053/j.jvca.2015.01.021
Cimen NK, Kosem B, Cimen T, Kartal S, Muslu B, Karabayirli S, Gozdemir M, Kilinc H (2016) Effects of remifentanil, nitroglycerin, and sevoflurane on the corrected QT and Tp-e intervals during controlled hypotensive anesthesia. J Clin Anesth 33:365–372. doi:10.1016/j.jclinane.2016.04.048
Rasmussen LA, Ryhammer PK, Greisen J, Bhavsar RR, Lorentzen AG, Jakobsen CJ (2016) Ultrashort acting remifentanil is not superior to long-acting sufentanil in preserving cognitive function-a randomized study. J Clin Anesth 33:127–134. doi:10.1016/j.jclinane.2016.03.023
Chen L, Chen M, Du J, Wan L, Zhang L, Gu E (2016) Hyperglycemia attenuates remifentanil postconditioning-induced cardioprotection against hypoxia/reoxygenation injury in H9c2 cardiomyoblasts. J Surg Res 203(2):483–490. doi:10.1016/j.jss.2016.03.052
Zuo Y, Cheng X, Gu E, Liu X, Zhang L, Cao Y (2014) Effect of aortic root infusion of sufentanil on ischemia-reperfusion injury in patients undergoing mitral valve replacement. J Cardiothorac Vasc Anesth 28(6):1474–1478. doi:10.1053/j.jvca.2014.04.023
Cominacini L, Mozzini C, Garbin U, Pasini A, Stranieri C, Solani E, Vallerio P, Tinelli IA, Fratta Pasini A (2015) Endoplasmic reticulum stress and Nrf2 signaling in cardiovascular diseases. Free Radic Biol Med 88(Pt B):233–242. doi:10.1016/j.freeradbiomed.2015.05.027
Yu Y, Sun G, Luo Y, Wang M, Chen R, Zhang J, Ai Q, Xing N, Sun X (2016) Cardioprotective effects of Notoginsenoside R1 against ischemia/reperfusion injuries by regulating oxidative stress- and endoplasmic reticulum stress- related signaling pathways. Sci Rep 6:21730. doi:10.1038/srep21730
Liao F, Zheng Y, Cai J, Fan J, Wang J, Yang J, Cui Q, Xu G, Tang C, Geng B (2015) Catestatin attenuates endoplasmic reticulum induced cell apoptosis by activation type 2 muscarinic acetylcholine receptor in cardiac ischemia/reperfusion. Sci Rep 5:16590. doi:10.1038/srep16590
Chen R, Kang R, Fan XG, Tang D (2014) Release and activity of histone in diseases. Cell Death Dis 5:e1370. doi:10.1038/cddis.2014.337
Wu D, Ingram A, Lahti JH, Mazza B, Grenet J, Kapoor A, Liu L, Kidd VJ, Tang D (2002) Apoptotic release of histones from nucleosomes. J Biol Chem 277(14):12001–12008. doi:10.1074/jbc.M109219200
Barrero CA, Perez-Leal O, Aksoy M, Moncada C, Ji R, Lopez Y, Mallilankaraman K, Madesh M, Criner GJ, Kelsen SG, Merali S (2013) Histone 3.3 participates in a self-sustaining cascade of apoptosis that contributes to the progression of chronic obstructive pulmonary disease. Am J Respir Crit Care Med 188(6):673–683. doi:10.1164/rccm.201302-0342OC
Zhang Z, Qin X, Tong N, Zhao X, Gong Y, Shi Y, Wu X (2012) Valproic acid-mediated neuroprotection in retinal ischemia injury via histone deacetylase inhibition and transcriptional activation. Exp Eye Res 94(1):98–108. doi:10.1016/j.exer.2011.11.013
Huang H, Chen HW, Evankovich J, Yan W, Rosborough BR, Nace GW, Ding Q, Loughran P, Beer-Stolz D, Billiar TR, Esmon CT, Tsung A (2013) Histones activate the NLRP3 inflammasome in Kupffer cells during sterile inflammatory liver injury. J Immunol 191(5):2665–2679. doi:10.4049/jimmunol.1202733
Bosmann M, Grailer JJ, Ruemmler R, Russkamp NF, Zetoune FS, Sarma JV, Standiford TJ, Ward PA (2013) Extracellular histones are essential effectors of C5aR- and C5L2-mediated tissue damage and inflammation in acute lung injury. FASEB J 27(12):5010–5021. doi:10.1096/fj.13-236380
Liang DY, Li X, Clark JD (2013) Epigenetic regulation of opioid-induced hyperalgesia, dependence, and tolerance in mice. J Pain 14(1):36–47. doi:10.1016/j.jpain.2012.10.005
Xie M, Kong Y, Tan W, May H, Battiprolu PK, Pedrozo Z, Wang ZV, Morales C, Luo X, Cho G, Jiang N, Jessen ME, Warner JJ, Lavandero S, Gillette TG, Turer AT, Hill JA (2014) Histone deacetylase inhibition blunts ischemia/reperfusion injury by inducing cardiomyocyte autophagy. Circulation 129(10):1139–1151. doi:10.1161/CIRCULATIONAHA.113.002416
Kee HJ, Kook H (2011) Roles and targets of class I and IIa histone deacetylases in cardiac hypertrophy. J Biomed Biotechnol 2011:928326. doi:10.1155/2011/928326
Paillard M, Tubbs E, Thiebaut PA, Gomez L, Fauconnier J, Da Silva CC, Teixeira G, Mewton N, Belaidi E, Durand A, Abrial M, Lacampagne A, Rieusset J, Ovize M (2013) Depressing mitochondria-reticulum interactions protects cardiomyocytes from lethal hypoxia-reoxygenation injury. Circulation 128(14):1555–1565. doi:10.1161/CIRCULATIONAHA.113.001225
Headrick JP, See Hoe LE, Du Toit EF, Peart JN (2015) Opioid receptors and cardioprotection—‘opioidergic conditioning’ of the heart. Br J Pharmacol 172(8):2026–2050. doi:10.1111/bph.13042
Sahbaie P, Liang DY, Shi XY, Sun Y, Clark JD (2016) Epigenetic regulation of spinal cord gene expression contributes to enhanced postoperative pain and analgesic tolerance subsequent to continuous opioid exposure. Mol Pain. doi:10.1177/1744806916641950
Campos EI, Reinberg D (2009) Histones: annotating chromatin. Annu Rev Genet 43:559–599. doi:10.1146/annurev.genet.032608.103928
Marinova Z, Ren M, Wendland JR, Leng Y, Liang MH, Yasuda S, Leeds P, Chuang DM (2009) Valproic acid induces functional heat-shock protein 70 via Class I histone deacetylase inhibition in cortical neurons: a potential role of Sp1 acetylation. J Neurochem 111(4):976–987. doi:10.1111/j.1471-4159.2009.06385.x
Ren M, Leng Y, Jeong M, Leeds PR, Chuang DM (2004) Valproic acid reduces brain damage induced by transient focal cerebral ischemia in rats: potential roles of histone deacetylase inhibition and heat shock protein induction. J Neurochem 89(6):1358–1367. doi:10.1111/j.1471-4159.2004.02406.x
Zhao TC, Cheng G, Zhang LX, Tseng YT, Padbury JF (2007) Inhibition of histone deacetylases triggers pharmacologic preconditioning effects against myocardial ischemic injury. Cardiovasc Res 76(3):473–481. doi:10.1016/j.cardiores.2007.08.010
Marciniak SJ, Yun CY, Oyadomari S, Novoa I, Zhang Y, Jungreis R, Nagata K, Harding HP, Ron D (2004) CHOP induces death by promoting protein synthesis and oxidation in the stressed endoplasmic reticulum. Genes Dev 18(24):3066–3077. doi:10.1101/gad.1250704
Miyazaki Y, Kaikita K, Endo M, Horio E, Miura M, Tsujita K, Hokimoto S, Yamamuro M, Iwawaki T, Gotoh T, Ogawa H, Oike Y (2011) C/EBP homologous protein deficiency attenuates myocardial reperfusion injury by inhibiting myocardial apoptosis and inflammation. Arterioscler Thromb Vasc Biol 31(5):1124–1132. doi:10.1161/ATVBAHA.111.224519
Nakagawa T, Zhu H, Morishima N, Li E, Xu J, Yankner BA, Yuan J (2000) Caspase-12 mediates endoplasmic-reticulum-specific apoptosis and cytotoxicity by amyloid-beta. Nature 403(6765):98–103. doi:10.1038/47513
Lu H, Lu L, Xu ZC, Lu YJ, Zhao B, Zhuang L, Hao BB, Zhang F (2014) Tauroursodeoxycholic acid and 4-phenyl butyric acid alleviate endoplasmic reticulum stress and improve prognosis of donation after cardiac death liver transplantation in rats. Hepatobiliary Pancreat Dis Int 13(6):586–593
Zhang Z, Tong N, Gong Y, Qiu Q, Yin L, Lv X, Wu X (2011) Valproate protects the retina from endoplasmic reticulum stress-induced apoptosis after ischemia-reperfusion injury. Neurosci Lett 504(2):88–92. doi:10.1016/j.neulet.2011.09.003
Koga T, Suico MA, Shimasaki S, Watanabe E, Kai Y, Koyama K, Omachi K, Morino-Koga S, Sato T, Shuto T, Mori K, Hino S, Nakao M, Kai H (2015) Endoplasmic reticulum (ER) stress induces sirtuin 1 (SIRT1) expression via the PI3K-Akt-GSK3beta signaling pathway and promotes hepatocellular injury. J Biol Chem 290(51):30366–30374. doi:10.1074/jbc.M115.664169
Geiger S, Holdenrieder S, Stieber P, Hamann GF, Bruening R, Ma J, Nagel D, Seidel D (2006) Nucleosomes in serum of patients with early cerebral stroke. Cerebrovasc Dis 21(1–2):32–37. doi:10.1159/000089591
Acknowledgements
We thank LetPub (http://www.letpub.com) for its linguistic assistance during the preparation of this manuscript.
Authors contributions
EG and MC designed experiments; MC and QL carried out experiments; LC analyzed experimental results. LZ analyzed sequencing data and developed analysis tools. MC wrote the manuscript and EG approved the final manuscript.
Funding
The funding was provided by the Key Research Project of education department of Anhui Province (No. KJ2013A161) and the Natural Science Foundation of China (No. 81341014).
Author information
Authors and Affiliations
Corresponding author
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Chen, M., Liu, Q., Chen, L. et al. Remifentanil postconditioning ameliorates histone H3 acetylation modification in H9c2 cardiomyoblasts after hypoxia/reoxygenation via attenuating endoplasmic reticulum stress. Apoptosis 22, 662–671 (2017). https://doi.org/10.1007/s10495-017-1347-5
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10495-017-1347-5