Abstract
The four pillars of advanced healthcare practice (AHCP) are clinical practice, leadership and management, education, and research. It is unclear, however; how competencies of AHCP as defined by individual health professions relate to these pillars. Addressing this knowledge gap will help to facilitate the operationalization of AHCP as a concept and help inform educational curricula. To identify existing competencies across AHCP literature and examine how they relate to the four pillars of a multi-professional AHCP framework. An umbrella review was conducted in accordance with JBI methodology. The electronic search for published and grey literature was completed using CINAHL, Scopus, Medline (OVID), Embase (OVID), ERIC (OVID) and Google. Secondary reviews and research syntheses of master level AHCP programs published after 1990 in either English or French were considered for inclusion and results were analyzed using a directed content analysis. Seventeen publications detailing 620 individual competencies were included. AHCP competencies were described across four professions and 22 countries, with many publications related to nursing and AHCP in the United Kingdom, Canada, and Australia. Many retrieved competencies were found to map to the four pillars of AHCP, although clinical practice and leadership and management pillars were addressed more often. Competencies of AHCP are generally consistent with the four pillars. However, the distribution of competencies is unequal across pillars, professions, and geographical regions, which may provide direction for further research.
Doi: 10.17605/OSF.IO/KV2FD Published on March 07, 2023.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
The concept of advanced healthcare practice (AHCP) was first introduced in Western countries by the nursing profession in the 1960s (Hulse, 2022) to meet the needs of underserved rural populations better (Hibbert et al., 2017). Now firmly established as a key strategy in accommodating the increasing demands and complexity of patient populations (Lawler et al., 2020), AHCP has been linked to improved patient outcomes, facilitation of interprofessional practice and enhanced clinician work satisfaction (HEE, 2017; Hulse, 2022). These benefits have prompted healthcare professions outside of nursing to develop AHCP roles. Such roles have been labelled using various titles, including advanced practitioner, clinical specialist, advanced clinical practitioner, and clinicians with expanded scope, as well as by specific professional designations, such as Nurse Practitioner (Evans et al., 2020a, 2020b; Hulse, 2022; Leslie et al., 2021).
In 2017, Health Education England (HEE), a public body coordinating and supporting healthcare education and training, published a multi-professional framework for AHCP (HEE, 2017) that provided one of the first multi-profession definitions of AHCP. AHCP was defined as being:
… delivered by experienced, registered health and care practitioners. It is a level of practice characterized by a high degree of autonomy and complex decision-making. This is underpinned by a master level award or equivalent that encompasses the four pillars of clinical practice, leadership and management, education, and research, with demonstration of core capabilities and area of specific clinical competence.
(HEE, 2017, pg. 8).
Among healthcare providers, competency has been defined as “an observable ability of a health professional, integrating multiple components, such as knowledge, skills, values and attitude” (Frank et al., 2010, pg. 641). While the terms competency and capability have been used interchangeably in relevant literature, in this review the term competency will be used to encompass the concept of core capabilities and skills. Competency is an integral concept in understanding competency-based education, proposed as an alternative to process-based education in the 1970’s. Seeking to ensure that graduates are adequately prepared to meet the needs of a given population, competency-based education considers the desired outcomes of training with a focus on both the needs of the learner and patient (Frank et al., 2010; Schumacher et al., 2024). Therefore, just as AHCP roles have emerged to meet population and healthcare needs, so too, has competency-based education (Frank et al., 2010; HEE, 2017). Assessment within competency-based education is guided by the attainment, maintenance, and enhancement of competencies as a measurement unit (Schumacher et al., 2024). This lends itself to assessment of learners at various levels of practice. To develop and implement defined AHCP roles, there must first be an overarching understanding of the competency of practice.
The development of HEE’s multi-professional framework was a critical step in promoting competency-based education for the implementation of AHCP. This framework is specific to England, yet multi-professional AHCP has not been clearly defined internationally (Evans et al., 2020a, 2020b; Lawler et al., 2020; Leslie et al., 2021). Furthermore, a recent scoping review examined the implementation of AHCP in the United Kingdom (UK) following the publication of the HEE framework and found that ongoing ambiguity in competency and educational requirements of AHCP has hindered its successful implementation (Evans et al., 2020a, 2020b). Similarly, a recent case study comparing scope of practice policy and regulation in the UK, United States, Canada, and Australia found poor agreement on the education requirements, accreditation, and competency of those in relevant roles (Leslie et al., 2021). This lack of mutual understanding around AHCP competency has resulted in disagreements around roles, scope of practice, underutilization of skills sets and limited integration of AHCP roles in the workplace (Lawler et al., 2020; Leslie et al., 2021).
Although the concept of AHCP competency has been examined in both primary and secondary literature, current considerations are limited to single professions or specific roles, and little is known about competencies across AHCP and how these competencies relate to the four pillars outlined by the HEE framework (Leslie et al., 2021). Developing a broader understanding of existing competencies and whether they map to the four established pillars will continue to inform the development of competency-based educational curricula, enhance team-based care and contribute to health systems planning (Evans et al., 2020a, 2020b; Frank et al., 2010). Addressing this knowledge gap will help further support the operationalization of multi-profession AHCP and information to help inform AHCP educational curricula.
Objectives
-
1.
To determine which professions, have core competencies for graduates of AHCP degree-granting programs.
-
2.
To identify competencies across AHCP.
-
3.
To examine how identified competencies map to the four pillars of AHCP. (HEE, 2017).
Methods and methodology
An umbrella review was conducted to provide an overview of existing systematic and secondary reviews (Aromataris et al., 2014a, b). Umbrella reviews offer the ability to broadly examine a topic of interest and determine if there is general consensus within the literature examining similar review questions (Aromataris et al., 2014a, b). The methodology for this review was based on the Joanna Briggs Institute (JBI) Manual for Evidence Synthesis (Aromataris et al., 2024. A study protocol was developed a priori and made available on Open Science Framework (Kenyon et al., 2022). Following the development of the protocol, changes were made to the wording of the review objectives to improve their clarity. A second quality appraisal tool was also identified and used to assess the methodological quality of the included reviews.
Eligibility criteria
Inclusion and exclusion criteria were identified using the PEO Model (Aromataris & Munn, 2020) for clinical questions and can be found in Table 1.
Search strategy
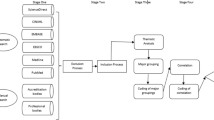
The search strategy was developed and executed in consultation with an Information and Research Librarian. This was conducted in three phases. In the first phase, initial key words were identified in a preliminary search using CINAHL and Google Scholar. Relevant keywords were then categorized for the Population, Exposure and Outcome model described by JBI (Aromataris & Munn, 2020). Search terms were entered into CINAHL, Scopus, Medline (OVID), Embase (OVID), and ERIC (OVID) using Boolean operators and truncation to ensure the search was adequately comprehensive. Any results not in English or French were excluded. A grey literature search was completed by entering the keywords identified in the preliminary search into an advanced Google search. The first two hundred returned results were screened for inclusion. Additionally, a hand search from personal files was conducted reviewing articles and their reference lists. The details of the final search are listed in Appendix A.
Study selection
All yielded studies were exported to Mendeley for citation management and to Covidence (https://www.covidence.org) for citation screening and the removal of duplicates. The screening was completed by E.K., S.D., R.E., D.L., and B.S. and occurred in two steps: title and abstract screening followed by full-text review. Two independent reviewers chosen by Covidence conducted all screening based on the identified inclusion and exclusion criteria, with disagreements resolved by a third independent reviewer. Reasons for exclusion at full text stage were recorded.
Data extraction
Data extraction from included studies was completed using a modified version of the JBI Extraction Form for Review for Systematic Reviews and Research Synthesis (Aromataris & Munn, 2020). As recommended, this tool was reviewed by the authors and amended by consensus before beginning data extraction (Aromataris & Munn, 2020). Amendments allowed for the addition of data extraction fields for target data as specified in the PEO Model. This included data fields to capture the profession a review pertained to, identified competencies and if reference was made to the HEE multi-professional framework. The amended version of this tool can be found in Appendix B. Consistent use of the tool was ensured by predetermining definitions for all data extraction fields and by piloting the tool using one randomly selected study from those included. Data extraction was completed in duplicate by two independent reviewers (S.D., R.E., E.K., D.L., B.S.) using Covidence. A third independent reviewer resolved conflicts.
Data analysis and synthesis
Data was analyzed using directed content analysis; a deductive qualitative approach described by Mayring (2000). Using previously established research and theories to define categories and subcategories, the authors organized extracted data for analysis according to the steps outlined by Mayring (2000). HEE’s four pillars of AHCP were used to define codes to which competencies retrieved from the literature were mapped. Findings were then summarized in a heat map indicating which HEE pillars and competencies were described within the retrieved reviews and their frequency. Abbreviated versions of the competencies listed in the HEE multi-professional framework have been used in the heat map. These abbreviations had been previously established in the work of Fennelly et al. (2020) (Appendix C).
Mapping was completed by two independent reviewers (S.D., R.E., D.L., S.B.) with conflicts resolved by a third independent reviewer. Reviewers were permitted to assign multiple codes to a single competency. Consistency in coding was achieved by reviewing the use of codes between raters at three points during analysis: after 50 competencies had been coded, on completion of coding by independent reviewers and on completion of consensus (Mayring, 2000).
Methodological quality appraisal
It was initially proposed that methodological quality of the included reviews would be appraised using the JBI (Joanna Briggs Institute) Critical Appraisal Checklist for Systematic Reviews and Research Syntheses (Aromataris et al., 2024). This tool consists of an 11-question checklist that prompts the user to select “yes,” “no,” “unclear,” or “not applicable,” as well as an overall appraisal rating of “include,” “exclude,” or “seek further info.” After study selection, most included reviews utilized qualitative study designs and presented their findings narratively rather than quantitatively. The Scale for the Assessment of Narrative Review Articles (SANRA) (Baethge et al., 2019) was identified to appraise narrative-type studies, defined as “any attempt to summarize the literature in a way which is not explicitly systematic, where the minimum requirement for the term systematic related to the method of the literature search” (Baethge et al., 2019). The SANRA is a 6-item scale that includes anchored definitions for each item. Each item is rated as a 0, 1 or a 2 with a total score < 4 indicating very poor quality (Baethge et al., 2019). Quality assessments using both the JBI checklist and SANRA were completed by two independent reviewers (S.D., R.E., D.L., S.B.), with conflicts being resolved by a third independent reviewer. Findings of the methodological quality appraisal were not used to determine inclusion, rather to provide comment on the overall quality of the included literature.
Results
Studies
The final search was completed between November 2022 and January 2023 with 3460 articles retrieved from databases. After removal of duplicates, 2102 articles underwent title and abstract screening and subsequently 97 underwent full-text screening. Following full text screening, 33 articles were excluded as they did not determine competencies, 21 articles were not secondary reviews or research syntheses, 19 did not examine master level or degree granting programs, 6 were published in languages other than English or French, 4 did not pertain to governed professions, and 1 full text was not available despite two attempts to contact the author. Three additional articles were identified from the grey literature. Seventeen reviews were included. A PRISMA diagram outlining study selection can be found in Fig. 1.
PRISMA Diagram of AHCP Competencies (Haddaway et al., 2022)
Characteristics of included reviews
Included reviews were published between 2004 and 2023 with countries of origin including the United States, the United Kingdom, Canada, Australia, the Netherlands, Switzerland, Germany, Spain, Singapore, Thailand, and China. One review was published in French. Nine reviews were literature reviews; four were scoping reviews, and two were integrative reviews in addition to both a single narrative review and a Ph.D. thesis. Of the included studies, 71% (n = 12/17) examined competencies of advanced practice nursing, while the remainder examined advanced practice physiotherapy (n = 3/17), midwifery (n = 1/17), and pharmacy (n = 1/17). Characteristics of all included reviews can be found in Table 2.
Methodological quality
When methodological quality was evaluated using the JBI checklist, six studies met at least eight of the 11 criteria, five met at least six criteria and six met five or fewer criteria. When evaluated using the SANRA, 12 reviews scored nine or more, four scored at least five and one scored less than four. Those studies that met a higher number of criteria or scored higher are suggested to be of higher methodological quality. Quality appraisal suggests that, although the quality of the data was rated more favorably when using the SANRA compared to the JBI checklist, the quality of the data is moderate to high. The JBI tool commonly identified studies failing to critically appraise data and determine risk for publication bias, whereas the SANRA tool commonly identified studies failing to state specific research questions or adequately describe the search strategy. These findings reflect the differences in content validity of the two tools (Aromataris & Munn, 2020; Baethge et al., 2019; Sadoyu et al., 2022). Scoring of methodological quality can be found in Table 2.
Identified competencies based on profession
The included reviews identified 620 individual competencies. Most of the retrieved competencies were from nursing (62%, n = 387/620) and physiotherapy studies (10%, n = 62/620). The competencies retrieved from the pharmacy (5%, n = 33/620) and midwifery (< 1%, n = 4/620) were limited in number, and each retrieved from a single review. Several of the reviews reported lists of competencies across multiple professions and geographical regions (Fennelly et al., 2020; Tawiah, 2022), but did not specify which professions or region each competency was sourced from. This accounted for 20% (n = 123/620) of the retrieved competencies. Within nursing literature, a unique pattern was identified. Six of the studies examining AHCP nursing competencies cited consensus statements and policy documents published by national governing bodies, professional associations, and regulators (Bender, 2014; Chan et al., 2020; Egerod et al., 2021; Elliott & Walden, 2015; Fennelly et al., 2020; Heinen et al., 2019). These citations were not identified in studies from other professions.
Data synthesis and analysis of the competencies
585 of the 620 retrieved competencies (94%) mapped to the four pillars. Thirty-five of the retrieved competencies were coded as other (6%), indicating that they did not map to the competencies.
A heat map of the retrieved competencies can be found in Fig. 2. Most retrieved competencies were found to map to the clinical practice pillar, accounting for 41% of all assigned codes. Leadership and management were the next most frequently represented pillar (27%),
Data analysis demonstrated that some competencies were described more frequently within the included reviews than others. The most mapped competencies were found within the Clinical Practice Pillar. The most frequently described competencies in order were “clinical reasoning and decision making,” "effective communication” and “assessment methods”. Within the Leadership & Management pillar the fourth overall highest competency was “negotiate scope of practice.” The fifth most common competency was “subject-specific competencies” which is also found within the clinical practice pillar. The competencies associated with the pillars of education (16%) and research (16%) were significantly less, with the combined number of competencies coded to both pillars being less than the number used for the clinical practice pillar alone.
Discussion
Professions that have defined core competencies of AHCP
This review determined that four professions have sought to determine competencies of degree granting AHCP programs. Many of the competencies retrieved by the search originated from nursing literature. This is not surprising as nursing was one of the first professions to establish an advanced practice role (Hulse, 2022). Within the included reviews, it became evident that the nursing profession has determined internationally accepted definitions of profession specific AHCP, and related competencies as well as expanded on their understanding of AHCP for specialized roles and practice settings, such as genetics (Lea et al., 2005), family practice (Schlunegger et al., 2023) and geriatric medicine (Goldberg et al., 2016). Given the successful establishment and implementation of AHCP nursing competencies, there may be key strategies for other professions that are working to establish and regulate advanced practice roles and educational programs.
Among reviews examining the nursing profession, there is evidence of cooperative and collaborative efforts among member organizations, professional associations, and regulatory groups to ensure consensus around capabilities, role definition, nomenclature and policy (Bender, 2014; Chan et al., 2020; Egerod et al., 2021; Elliott & Walden, 2015; Fennelly et al., 2020; Heinen et al., 2019). This comprehensive approach was not observed among reviews of other professions that have more recently begun to implement advanced practice roles, such as physiotherapy (Fennelly et al., 2020; Harding et al., 2015; Tawiah, 2022), pharmacy and midwifery (Goemaes et al., 2016; Harding et al., 2015; Meadows et al., 2004). Unclear definitions of role, role awareness and disagreements around scope have been identified in the literature as barriers to successfully determining competencies and implementing AHCP (Evans et al., 2020a, 2020b; Lawler et al., 2020). Therefore, it appears that collaborative efforts between these stakeholders may be essential in determining core competencies and establishing and regulating educational programs.
Competencies
The distribution of retrieved competencies under the pillars was not uniform,. The most frequent competency for AHCP was found under the “Clinical Practice” pillar. It has been suggested that teachings of competencies related to clinical practice likely underpin skills of the other pillars, such as education and research (Utley et al., 2017). It must be considered that the findings of this review may highlight potential overlap between teachings of clinical reasoning and technical skills, as evidenced by “subject-specific competencies” being found to be the fifth most common competency. Retrieved competencies found to map to this competency included nurse practitioners' assessment and management of geriatric populations (Fennelly et al., 2020). These represent competencies that are specific to professional roles and practice settings rather than those common to AHCP and were often discussed in the literature in a manner that did not make mention of competencies relating to the other pillars, such as education and research. This indicates that the current curriculum and evaluations of candidates in AHCP educational programs may focus on developing clinical skills to the exclusion of the competencies of the other three pillars. This is reflected in a cross-sectional survey of policymakers and clinicians at various levels of practice, which suggests that, although most clinicians consider the four pillars of AHCP important, knowledge of the HEE framework was minimal and competencies within the clinical practice pillar were consistently prioritized in their training (Fothergill et al., 2022).
To ensure that AHCP educational programs equip graduates to achieve the competency required to practice at the advanced level, curricula should consider mapping of program competencies across all four pillars. The development of such curricula, however, must also consider how to best ensure that candidates are proficient in the seamless application of multiple competencies in a holistic manner to manage complex and multi-faceted care environments. Therefore, although helpful in developing an overarching understanding of the current landscape of AHCP, consideration of competencies using only commonality may limit contextual understanding in an educational environment. This may be achieved in educational settings by considering the intention of the HEE multi-professional framework (2017) to be used alongside profession-specific national frameworks, such as that developed for AHCP nursing in England (HEE, 2020) to develop competency-based curricula. Using both frameworks allows for profession-specific competencies to be further defined while also ensuring that curricula map across pillars of AHCP, thus avoiding prioritization of only clinical skills.
Alignment with the four pillars of AHCP
This review found that, although only four of the included reviews mentioned HEE’s multi-professional framework (2017), there was a strong alignment between the competencies retrieved from the literature and the competencies of the four pillars of AHCP. Therefore, the findings of this review suggest that HEE’s multi-professional framework describes the competencies common to AHCP both internationally and across professions. This suggests the potential of this framework to be considered as a guiding document for mapping educational curricula internationally to ensure alignment with advanced-level training requirements. (Fothergill et al., 2022). A small number of retrieved competencies (6%) did not map to the four pillars. Two themes were evident within these unmapped competencies: cultural sensitivity and business management skills. The finding of competencies that do not map to the existing framework suggests that future research may be warranted to determine if such competencies are integral to AHCP and to determine if existing frameworks may need to be reviewed and updated to ensure that they are contemporary and continue to reflect the needs of the dynamic healthcare systems.
Strengths and limitations
This was the first large-scale international review of AHCP across professions and practice settings. This review utilized an umbrella review methodology, which permitted a systematic evaluation of the current body of literature and directions for future research. Screening and data analysis procedures were undertaken using two independent reviewers with a third to resolve conflicts, which along with the inclusion of a quality appraisal, strengthened the methodology of this review. This study has some potential limitations. The results of this review are limited to master and doctoral level educational programs and only captured data from professions which have examined AHCP with secondary research, therefore; results may not be inclusive of countries or professions with established or emerging advanced roles that are developed through experiential or diploma/certificate programs. Lastly, both the JBI checklist and SANRA lacked defined cut-off scores, limiting their ability to compare the methodological quality of the included studies (Sadoyu et al., 2022).
Future recommendations
Further research is needed to determine the essential competencies of AHCP of professions and countries with newly established or emerging AHCP roles. Research with a focus on the development and assessment of competencies of leadership and management, education, and research is also needed as the current body of research focuses heavily on competencies related to the pillar of clinical practice (Evans et al., 2020a, 2020b; Fothergill et al., 2022). This may be achieved through the development of profession-specific national frameworks to be used in conjunction with the HEE multi-professional framework (HEE, 2017).
Conclusions
The benefit of AHCP roles to patient outcomes and healthcare systems as a whole has been well substantiated in the literature (Evans et al., 2020a, 2020b; Evans et al., 2020a, 2020b; Fothergill et al., 2022; Hulse, 2022; Kleinpell et al., 2022), yet confusion remains regarding educational requirements, role delineation and the competency of those occupying AHCP roles (Evans et al., 2020a, 2020b; Lawler et al., 2020; Leslie et al., 2021). This review demonstrated that competencies of AHCP across different professions are consistent with the four pillars of HEE’s multi-professional framework (2017). The distribution of described competencies, however, is not equal across pillars, professions, or geographical regions, which may provide direction for further research. Therefore, the HEE multi-professional framework (HEE, 2017) may be useful as a guiding document in the design and evaluation of AHCP, although additional work is needed to establish profession-specific national frameworks and to ensure that competencies are developed across all four pillars.
References
Aromataris, E., Fernandez, R. S., Godfrey, C., Holly, C., & Khalil, H. (2014). Methodology for JBI umbrella reviews. https://ro.uow.edu.au/smhpapers/3344
Aromataris, E., Fernandez, R. S., Godfrey, C., Holly, C., Khalil, H., & Tungpunkom, P. (2014). Methodology for JBI umbrella reviews. Faculty of Science, Medicine and Health -Papers: Part A. 3344. https://ro.uow.edu.au/smhpapers/3344(20) (PDF) Chapter 10: Umbrella Reviews.: https://www.researchgate.net/publication/342598533_Chapter_10_Umbrella_Reviews
Aromataris, E., Lockwood, C., Porritt, K., Pilla, B., Jordan, Z., (eds.), (2024). JBI manual for evidence synthesis. JBI https://doi.org/10.46658/JBIMES-24-01
Aromataris, E., & Munn, Z. (2020). JBI Manual for Evidence Synthesis. JBI. https://doi.org/10.46658/JBIMES-20-01
Baethge, C., Goldbeck-Wood, S., & Mertens, S. (2019). SANRA—a scale for the quality assessment of narrative review articles. Research Integrity and Peer Review, 4(1), 5. https://doi.org/10.1186/s41073-019-0064-8
Bender, M. (2014). The current evidence base for the clinical nurse leader: A narrative review of the literature. Journal of Professional Nursing, 30(2), 110–123. https://doi.org/10.1016/j.profnurs.2013.08.006
Chan, T. E., Lockhart, J. S., Thomas, A., Kronk, R., & Schreiber, J. B. (2020). An integrative review of nurse practitioner practice and its relationship to the core competencies. Journal of Professional Nursing, 36(4), 189–199. https://doi.org/10.1016/j.profnurs.2019.11.003
Chua, C. M. S., Nantsupawat, A., Wichaikhum, O. A., & Shorey, S. (2023). Content and characteristics of evidence in the use of standardized patients for advanced practice nurses: A mixed-studies systematic review. Nurse Education Today, 120, 105621. https://doi.org/10.1016/j.nedt.2022.105621
Egerod, I., Kaldan, G., Nordentoft, S., Larsen, A., Herling, S. F., Thomsen, T., & Endacott, R. (2021). Skills, competencies, and policies for advanced practice critical care nursing in Europe: A scoping review. Nurse Education in Practice, 54, 103142. https://doi.org/10.1016/j.nepr.2021.103142
Elliott, E. C., & Walden, M. (2015). Development of the transformational advanced professional practice model. Journal of the American Association of Nurse Practitioners, 27(9), 479–487. https://doi.org/10.1002/2327-6924.12171
Evans, C., Pearce, R., Greaves, S., & Blake, H. (2020a). Advanced clinical practitioners in primary care in the UK: A qualitative study of workforce transformation. International Journal of Environmental Research and Public Health, 17(12), 4500. https://doi.org/10.3390/ijerph17124500
Evans, C., Poku, B., Pearce, R., Eldridge, J., Hendrick, P., Knaggs, R., McLuskey, J., Tomczak, P., Thow, R., Harris, P., Conway, J., & Collier, R. (2020b). Characterising the evidence base for advanced clinical practice in the UK: A scoping review protocol. British Medical Journal Open, 10(5), e036192. https://doi.org/10.1136/bmjopen-2019-036192
Fennelly, O., Desmeules, F., O’Sullivan, C., Heneghan, N. R., & Cunningham, C. (2020). Advanced musculoskeletal physiotherapy practice: Informing education curricula. Musculoskeletal Science and Practice, 48, 102174. https://doi.org/10.1016/j.msksp.2020.102174
Fothergill, L. J., Al-Oraibi, A., Houdmont, J., Conway, J., Evans, C., Timmons, S., Pearce, R., & Blake, H. (2022). Nationwide evaluation of the advanced clinical practitioner role in England: A cross-sectional survey. British Medical Journal Open, 12(1), e055475. https://doi.org/10.1136/bmjopen-2021-055475
Frank, J. R., Snell, L. S., Cate, O. T., Holmboe, E. S., Carraccio, C., Swing, S. R., Harris, P., Glasgow, N. J., Campbell, C., Dath, D., Harden, R. M., Iobst, W., Long, D. M., Mungroo, R., Richardson, D. L., Sherbino, J., Silver, I., Taber, S., Talbot, M., & Harris, K. A. (2010). Competency-based medical education: Theory to practice. Medical Teacher, 32(8), 638–645. https://doi.org/10.3109/0142159X.2010.501190
Gavarkovs, A., Kusurkar, R. A., Kulasegaram, K., Crukley, J., Miller, E., Anderson, M., & Brydges, R. (2022). Motivational design for web-based instruction in health professions education: Protocol for a systematic review and directed content analysis. JMIR Research Protocols, 11(11), e42681. https://doi.org/10.2196/42681
Goemaes, R., Beeckman, D., Goossens, J., Shawe, J., Verhaeghe, S., & Van Hecke, A. (2016). Advanced midwifery practice: An evolutionary concept analysis. Midwifery, 42, 29–37. https://doi.org/10.1016/j.midw.2016.09.004
Goldberg, S. E., Cooper, J., Blundell, A., Gordon, A. L., Masud, T., & Moorchilot, R. (2016). Development of a curriculum for advanced nurse practitioners working with older people with frailty in the acute hospital through a modified Delphi process. Age and Ageing, 45(1), 48–53. https://doi.org/10.1093/ageing/afv178
Haddaway, N. R., Page, M. J., Pritchard, C. C., & McGuinness, L. A. (2022). PRISMA2020: An R package and Shiny app for producing PRISMA 2020-compliant flow diagrams, with interactivity for optimised digital transparency and Open Synthesis. Campbell Systematic Reviews, 18, 1230. https://doi.org/10.1002/cl2.1230
Harding, P., Prescott, J., Sayer, J., & Pearce, A. (2015). Advanced musculoskeletal physiotherapy clinical education framework supporting an emerging new workforce. Australian Health Review, 39(3), 271. https://doi.org/10.1071/AH14208
Health Education England. (2017). Multi-professional framework for advanced clinical practice in England. http://www.aomrc.org.uk/wp-content/
Health Education England. (2020). Core Capabilities Framework for Advanced Clinical Practice (Nurses) Working in General Practice/Primary Care in England.
Heinen, M., Oostveen, C., Peters, J., Vermeulen, H., & Huis, A. (2019). An integrative review of leadership competencies and attributes in advanced nursing practice. Journal of Advanced Nursing, 75(11), 2378–2392. https://doi.org/10.1111/jan.14092
Hibbert, D., Aboshaiqah, A. E., Sienko, K. A., Forestell, D., Harb, A. W., Yousuf, S. A., Kelley, P. W., Brennan, P. F., Serrant, L., & Leary, A. (2017). Advancing nursing practice: The emergence of the role of advanced practice nurse in Saudi Arabia. Annals of Saudi Medicine, 37(1), 72–78. https://doi.org/10.5144/0256-4947.2017.72
Hulse, A. L. (2022). A multidisciplinary learning approach: A narrative review. British Journal of Nursing, 31(7), 364–370. https://doi.org/10.12968/bjon.2022.31.7.364
Kenyon, E., DeBoer, S., El-Khoury, R., La, D., Saville Brendan, Alcock, G., Gillis, H., Miller, E., & Sadi, J. (2022). Identifying Common Competencies for Advanced Healthcare Practice Programs: An Umbrella Review Protocol [Internet]. OSF; 2023. Available from: osf.io/kv2fd. Open Science Framework. https://doi.org/10.17605/OSF.IO/KV2FD
Kleinpell, R., Myers, C. R., Likes, W., & Schorn, M. N. (2022). Breaking down institutional barriers to advanced practice registered nurse practice. Nursing Administration Quarterly, 46(2), 137–143. https://doi.org/10.1097/NAQ.0000000000000518
Lawler, J., Maclaine, K., & Leary, A. (2020). Workforce experience of the implementation of an advanced clinical practice framework in England: A mixed methods evaluation. Human Resources for Health, 18(1), 96. https://doi.org/10.1186/s12960-020-00539-y
Lea, D. H., Cooksey, J. A., Flanagan, P. A., Williams, J. K., & Forte, G. (2005). Innovations in United States genetics nursing: Practice and research. Japan Journal of Nursing Science, 2(2), 71–83. https://doi.org/10.1111/j.1742-7924.2005.00043.x
Leslie, K., Moore, J., Robertson, C., Bilton, D., Hirschkorn, K., Langelier, M. H., & Bourgeault, I. L. (2021). Regulating health professional scopes of practice: Comparing institutional arrangements and approaches in the US, Canada, Australia and the UK. Human Resources for Health, 19(1), 15. https://doi.org/10.1186/s12960-020-00550-3
Mayring, P. (2000). Qualitative content analysis. http://www.zuma-mannheim.de/research/en/methods/textanalysis/
Meadows, N., Davies, G., Webb, D., Bates, I., McRobbie, D., & Sotiris, A. (2004). Developing a competency framework for advanced pharmacy practitioners. Pharmaceutical Journal, 273(7327), 789–792.
Poulin, V., Mailhot-Bisson, D., & Turcotte-Brousseau, A. A. (2021). Le déploiement du rôle d’une infirmière en pratique avancée en gériatrie à l’urgence: Une innovation en Estrie. Soins D’urgence, 2(2), 35–44. https://doi.org/10.7202/1101813ar
Sadoyu, S., Tanni, K. A., Punrum, N., Paengtrai, S., Kategaew, W., Promchit, N., Lai, N. M., Thakkinstian, A., Ngorsuraches, S., Bangpan, M., Veettil, S., & Chaiyakunapruk, N. (2022). Methodological approaches for assessing certainty of the evidence in umbrella reviews: A scoping review. In PLoS ONE (Vol. 17, Issue 6 June). Public Library of Science. https://doi.org/10.1371/journal.pone.0269009
Sastre-Fullana, P., De Pedro-Gómez, J. E., Bennasar-Veny, M., Serrano-Gallardo, P., & Morales-Asencio, J. M. (2014). APN competency frameworks review. International Nursing Review, 61, 534–542. https://doi.org/10.1111/inr.12132
Schlunegger, M. C., Aeschlimann, S., Palm, R., & Zumstein-Shaha, M. (2023). Competencies of nurse practitioners in family practices: A scoping review. Journal of Clinical Nursing, 32(11–12), 2521–2532. https://doi.org/10.1111/jocn.16382
Schumacher, D. J., Kinnear, B., Carraccio, C., Holmboe, E., Busari, J. O., van der Vleuten, C., & Lingard, L. (2024). Competency-based medical education: The spark to ignite healthcare’s escape fire. Medical Teacher, 46(1), 140–146. https://doi.org/10.1080/0142159X.2023.2232097
Tawiah, A. K. (2022). Developing a competency profile for international standardization of Advanced Practice Physiotherapy. PhD dissertation (2022 era.library.ualberta.ca) https://doi.org/10.7939/r3-0xnv-gz42
Utley, R., Henry, K., & Smith, L. (2017). Frameworks for advanced nursing practice and research: Philosophies, theories, models and taxonomies. Springer Publishing Company.
Xu, H., Dong, C., Yang, Y., & Sun, H. (2022). Developing a professional competence framework for the master of nursing specialist degree program in China: A modified Delphi study. Nurse Education Today, 118, 105524. https://doi.org/10.1016/j.nedt.2022.105524
Acknowledgements
The authors would like to acknowledge Meagan Stanley, Information and Research Librarian at Western University for her assistance in the development and execution of a search strategy.
Funding
The authors have no funding sources to declare.
Author information
Authors and Affiliations
Contributions
The authors confirm contribution to the paper as follows: study conception J.S., H.G., G.A.; study design J.S., E.M., E.K., S.D,, R.E,, D.L., B.S.; data collection, analysis and interpretations of results E.K., S.D., R.E., D.L., B.S.; draft manuscript preparation E.K., S.D., R.E., D.L., B.S., J.S., H.G., G.A., E.M. All authors reviewed the results and approved the final version of the manuscript.
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Appendices
Appendix A: Search strategy for electronic databases
Concept | Key words | |
|---|---|---|
Population | Level of profession | “Extend* Scope” OR “Extend* Practi*” Expert* OR “Advanc* Practi*” OR “Advanc* Clinic*” OR “Speciali*” OR “Expert* Clinic*” or “expanded scope*” OR “advance* role” |
Health care professions | "audiolog*" or "arts therap*" OR "chiropod*" OR "podiatr*" OR "chiropract*" OR "dental hygien*" OR "dental techn*" OR "Dental therap*" OR "Dentis*" OR "Denturis*" OR "dietet*" OR “Dietician*” or "hearing aid dispens*" OR "Homeopath*" OR "massage therap*" OR "medical laboratory technolog*" OR "Medical radiation techn*" OR "medicine" OR "midwif*" OR "Naturopath*" OR "osteopath*" OR "nurs*" OR "occupational therap*" OR "operating department practition*" OR "optician*" OR "optometr*" OR "Orthodontic therap*" OR "orthoptic*" OR "Paramedic*" OR "pharmac*" OR "pharmacy techn*" OR "physiotherap*" OR "psychotherap*" OR "prostheti*" OR "pedorthist*" OR "orthotis*" OR "respiratory therap*" OR "speech-language patholog*" OR "Traditional Chinese medic*" OR "acupunctur*" OR “medicin*” OR “Health*” OR “healthcare*” OR “Clinician*” OR “Practition*” OR “Physician* | |
Exposure | University level degree granting program | "Education" OR "Program" OR "Curricul*" OR "Degree" OR “Framework” OR “Model” OR “Theor*” OR “Master*” OR “Doctorate” |
Outcome | Core capabilities | "core competen*" OR "competen*" OR "competen* based" OR "Scope" OR “Capabilit*” OR “Capacit*” OR “expertise” OR “Proficienc*” Or “skill*” or “attribute*” or “proficien*” |
Study type | Research syntheses | "Systematic Review" OR "Literature Review” OR "Concept Analysis" OR "Scop* Review" OR “Narrative” OR "meta analysis" OR "secondary analysis" OR “integrative review” OR “qualitative review” OR “research synthes*” OR “umbrella review” OR (MH "Systematic Review") OR (MH "Literature Review") OR (MH "Concept Analysis") OR (MH "ScopingReview") |
Grey literature search terms
Advanced google search parameters | English | French |
|---|---|---|
All these words | Competency | Compétence |
This exact word or phrase | “systematic” OR “scoping” OR “Narrative” OR “meta-analysis” OR “integrative” OR “qualitative” | “Systématique” OR “Examen de la portée” OR “Étude de la portée” OR “Narrative” OR “Meta analyse” OR “Intégrative” |
Any of these words | “Healthcare” OR “advanced practice” OR “scope” | “professionnel de la santé” OR “pratique avancée” OR “champ d’exercice” OR “domaines d’exercice” |
Citations for sources identified for inclusion | Tawiah, A. K. (2022). Developing a competency profile for international standardization of Advanced Practice Physiotherapy (PhD dissertation- 2022 · era.library.ualberta.ca) Health Education England. (2017). Multi-professional framework for advanced clinical practice in England. London: Health Education England Evans, C., Poku, B., Pearce, R., Eldridge, J., Hendrick, P., Knaggs, R., McLuskey, J., Tomczak, P., Thow, R., Harris, P. and Conway, J., (2020). Characterizing the evidence base for advanced clinical practice in the UK: a scoping review protocol. BMJ open, 10(5) | |
Appendix B: Modified JBI data collection tool used for data extraction
Study details | Analysis | ||
|---|---|---|---|
Study title: | Method of analysis: | ||
Author/year: | Results | ||
Journal: | Were the HEE four pillars discussed? | Y/N Another category was used: | |
Study objective: | Competencies | Related HEE pillar (if referenced) | |
Year of data collection | 1990–2000 2001–2010 2011–2020 2021-present | ||
Level of education | Master PhD Other: | ||
Study type | Literature review Narrative review Integrative review Scoping review Systematic review Umbrella review Other: | Significance/importance Indicate which review questions were addressed by the findings of this study | |
Country: | Canada UK Australia Other: | For which professions have competencies for AHCP been determined? | |
Healthcare profession | Nurse Physiotherapist Midwife Dentist Radiologist Respiratory Therapist Other: | What are the core competencies of degree granting AHCP programs? | |
Healthcare setting | Outpatient Inpatient Other: | Do the identified competencies align with HEE’s four pillars of advanced clinical practice (i.e., clinical practice, leadership and management, education, and research)? | |
Search details | Authors recommendations Please indicate and conclusion, implications for practice or areas for further research that the authors' have proposed | ||
Sources searched: | Final recommendation | ||
Number of studies included: | Include | ||
Types of studies included: | Exclude | ||
Country of studies origin: | Additional comments | ||
Appendix C: Abbreviated competencies terms used to describe competencies of the four pillars of AHCP
Pillar of advance practice | Abbreviated Competencies as defined by Fennelly et al. (2020) | HEE Competency descriptions (Health Education England, 2017) |
|---|---|---|
Clinical practice | Professional conduct | 1.1 Practice in compliance with their respective code of professional conduct and within their scope of practice, being responsible and accountable for their decisions, actions, and omissions at this level of practice |
Scope of practice | 1.2 Demonstrate a critical understanding of their broadened level of responsibility and autonomy and the limits of own competence and professional scope of practice, including when working with complexity, risk, uncertainty and incomplete information | |
Professional judgement | 1.3 Act on professional judgement about when to seek help, demonstrating critical reflection on own practice, self-awareness, emotional intelligence, and openness to change | |
Assessment methods | 1.4 Work in partnership with individuals, families to provide assessments; requesting, undertaking and/or interpreting diagnostic tests; and conducting health needs assessments) | |
Effective communication | 1.5 Demonstrate effective communication skills, supporting people in making decisions, planning care or seeking to make positive changes, using Health Education England’s framework to promote person-centered approaches in health and care | |
Clinical reasoning and decision making | 1.6 Use expertise and decision-making skills to inform clinical reasoning approaches when dealing with differentiated and undifferentiated individual presentations and complex situations, synthesizing information from multiple sources to make appropriate, evidence-based judgements and/or diagnoses | |
Interventions | 1.7 Initiate, evaluate and modify a range of interventions which may include prescribing medicines, therapies, lifestyle advice and care | |
Managing risk | 1.8 Exercise professional judgement to manage risk appropriately, especially where there may be complex and unpredictable events and supporting teams to do likewise to ensure safety of individuals, families and carers | |
Working collaboratively | 1.9 Work collaboratively with an appropriate range of multi-agency and inter-professional resources, developing, maintaining and evaluating links to manage risk and issues across organizations and settings | |
Clinical role model | 1.10 Act as a clinical role model/advocate for developing and delivering care that is responsive to changing requirements, informed by an understanding of local population health needs, agencies and networks | |
Subject specific competencies | 1.11 Evidence the underpinning subject-specific competencies i.e. knowledge, skills and behaviors relevant to the role setting and scope, and demonstrate application of the capabilities to these, in an approach that is appropriate to the individual role, setting and scope | |
Leadership and management | Effective relationships | 2.1 Pro-actively initiate and develop effective relationships, fostering clarity of roles within teams, to encourage productive working |
Person-centered approach | 2.2 Role model the values of their organization/place of work, demonstrating a person-centered approach to service delivery and development | |
Self and team evaluation | 2.3 Evaluate own practice, and participate in multi-disciplinary service and team evaluation, demonstrating the impact of advanced clinical practice on service function and effectiveness, and quality (i.e. outcomes of care, experience and safety) | |
Peer review | 2.4 Actively engage in peer review to inform own and other’s practice, formulating and implementing strategies to act on learning and make improvements | |
Service development | 2.5 Lead new practice and service redesign solutions in response to feedback, evaluation and need, working across boundaries and broadening sphere of influence | |
Seek feedback and involvement | 2.6 Actively seek feedback and involvement from individuals, families, carers, communities and colleagues in the co-production of service improvements | |
Provide consultancy | 2.7 Critically apply advanced clinical expertise inappropriate faciliatory ways to provide consultancy across professional and service boundaries, influencing clinical practice to enhance quality, reduce unwarranted variation and promote the sharing and adoption of best practice | |
Leadership | 2.8 Demonstrate team leadership, resilience and determination, managing situations that are unfamiliar, complex or unpredictable and seeking to build confidence in others | |
Practice development | 2.9 Continually develop practice in response to changing population health need, engaging in horizon scanning for future developments (e.g. impacts of genomics, new treatments and changing social challenges) | |
Receptive to challenge | 2.10 Demonstrate receptiveness to challenge and preparedness to constructively challenge others, escalating concerns that affect individuals’, families’, carers’, communities’ and colleagues’ safety and well-being when necessary | |
Negotiate scope of practice | 2.11 Negotiate an individual scope of practice within legal, ethical, professional and organizational policies, governance and procedures, with a focus on managing risk and upholding safety | |
Education | Assess own learning needs | 3.1 Critically assess and address own learning needs, negotiating a personal development plan that reflects the breadth of ongoing professional development across the four pillars of advanced clinical practice |
Self-directed learning | 3.2 Engage in self-directed learning, critically reflecting to maximize clinical skills and knowledge, as well as own potential to lead and develop both care and services | |
Appraise others | 3.3 Engage with, appraise and respond to individuals’ motivation, development stage and capacity, working collaboratively to support health literacy and empower individuals to participate in decisions about their care and to maximize their health and well-being | |
Advocacy | 3.4 Advocate for and contribute to a culture of organizational learning to inspire future and existing staff | |
Facilitate collaboration | 3.5 Facilitate collaboration of the wider team and support peer review processes to identify individual and team learning | |
Support team development | 3.6 Identify further developmental needs for the individual and the wider team and supporting them to address these | |
Support interprofessional learning | 3.7 Supporting the wider team to build capacity and capability through work-based and interprofessional learning, and the application of learning to practice | |
Educator/mentor | 3.8 Act as a role model, educator, supervisor, coach and mentor, seeking to instill and develop the confidence of others | |
Research | Engage in research | 4.1 Critically engage in research activity, adhering to good research practice guidance, so that evidence-based strategies are developed and applied to enhance quality, safety, productivity and value for money |
Evaluation and audits | 4.2 Evaluate and audit own and others’ clinical practice, selecting and applying valid, reliable methods, then acting on the findings | |
Use results to underpin practice | 4.3 Critically appraise and synthesize the outcome of relevant research, evaluation and audit, using the results to underpin own practice and to inform that of others | |
Identify gaps in evidence | 4.4 Take a critical approach to identify gaps in the evidence base and its application to practice, alerting appropriate individuals and organizations these and how they might be addressed in a safe and pragmatic way | |
Identify needs to strengthen evidence | 4.5 Actively identify potential need for further research to strengthen evidence for best practice. This may involve acting as an educator, leader, innovator and contributor to research activity and/or seeking out and applying for research funding | |
Develop and implement governance | 4.6 Develop and implement robust governance systems and systematic documentation processes, keeping the need for modifications under critical review | |
Dissemination | 4.7 Disseminate best practice research findings and quality improvement projects through appropriate media and fora (e.g. presentations and peer review research publications) | |
Facilitate links between clinic and research | 4.8 Facilitate collaborative links between clinical practice and research through proactive engagement, networking with academic, clinical and other active researchers |
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Kenyon, E., DeBoer, S., El-Khoury, R. et al. Identifying competencies in advanced healthcare practice: an umbrella review. Adv in Health Sci Educ (2024). https://doi.org/10.1007/s10459-024-10349-9
Received:
Accepted:
Published:
DOI: https://doi.org/10.1007/s10459-024-10349-9