Abstract
Conventional nanoporous hydrogels often lead to slow cartilage deposition by MSCs in 3D due to physical constraints and requirement for degradation. Our group has recently reported macroporous gelatin microribbon (μRB) hydrogels, which substantially accelerate MSC-based cartilage formation in vitro compared to conventional gelatin hydrogels. To facilitate translating the use of μRB-based scaffolds for supporting stem cell-based cartilage regeneration in vivo, there remains a need to develop a customize-designed drug delivery system that can be incorporated into μRB-based scaffolds. Towards this goal, here we report polydopamine-coated mesoporous silica nanoparticles (MSNs) that can be stably incorporated within the macroporous μRB scaffolds, and allow tunable release of transforming growth factor (TGF)-β3. We hypothesize that increasing concentration of polydopamine coating on MSNs will slow down TGF- β3 release, and TGF-β3 release from polydopamine-coated MSNs can enhance MSC-based cartilage formation in vitro and in vivo. We demonstrate that TGF-β3 released from MSNs enhance MSC-based cartilage regeneration in vitro to levels comparable to freshly added TGF-β3 in the medium, as shown by biochemical assays, mechanical testing, and histology. Furthermore, when implanted in vivo in a mouse subcutaneous model, only the group containing MSN-mediated TGF-β3 release supported continuous cartilage formation, whereas control group without MSN showed loss of cartilage matrix and undesirable endochondral ossification. The modular design of MSN-mediated drug delivery can be customized for delivering multiple drugs with individually optimized release kinetics, and may be applicable to enhance regeneration of other tissue types.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Hydrogels are attractive scaffolds for cartilage regeneration given their injectability, ease for homogeneous cell encapsulation and tunable chemical and physical properties.21,40 Conventional hydrogels are nanoporous and have been used as 3D matrices for mesenchymal stem cells (MSCs) or chondrocytes to support new cartilage formation.19,20 Given one important function of articular cartilage is shock-absorbing and weight bearing, it is critical to accelerate cartilage formation and restore mechanical properties of lost cartilage. However, physical restriction of nanoporous hydrogels often delay the speed of new matrix deposition, and it takes time for degradation before encapsulated cells can deposit new matrix. While a few studies have demonstrated obtaining cartilage with biomimetic strength, they require extremely high initial cell seeding density (i.e. 60 million/mL), dynamic mechanical loading, and prolonged in vitro culture with supplemented chondrogenic factors.9,10,13 To accelerate the speed of cartilage deposition in hydrogels, our group recently reported a gelatin (GEL)-based microribbon (μRB) scaffold as 3D niche for stem cell-based tissue regeneration.8 Unlike conventional hydrogels, the μRB scaffold is inherent macroporous, exhibit shock-absorbing capacity when subject to cyclic compression,17 and significantly accelerate MSC-based cartilage deposition in vitro.8 Using lower density of MSCs (10 M/mL) for encapsulation, gelatin (μRB)-based scaffold led to over 20-fold increase in compressive moduli to 225 kPa after only 3 weeks of culture in vitro.8 In contrast, conventional gelatin hydrogels only showed a slight increase in compressive modulus to ~ 65 kPa. While our study clearly demonstrated the advantage of macroporous μRB-based scaffold over conventional hydrogels as 3D matrix for accelerating MSC-based cartilage regeneration, it was limited to in vitro studies only and require supplement of full chondrogenic medium throughout the culture containing transforming growth factor-β3 (TGF-β3). TGF-β has been shown to play a key role in regulating cartilage development and homeostasis by impacting proliferation and phenotype of chondrocytes, the main resident cell type in cartilage.15,45 When adding into cell culture medium, TGF-β has also been shown to promote MSC chondrogenesis in vitro.1,16 However, TGF-β exhibits short half-life, and requires continuous supplementation. To facilitate translating the use of μRB-based scaffolds for supporting stem cell-based cartilage regeneration in vivo, there remains a need to develop a customize-designed drug delivery system with local and sustained release of TGF-β that can be incorporated into μRB-based scaffolds.
Several strategies have been developed to achieve sustained release of TGF-β to enhance chondrogenesis and cartilage regeneration in vitro and in vivo.11,27,37,43 Injection of magnetic liposome-containing TGF-β1 into cartilage defects in a rabbit model was reported to significantly improve cartilage regeneration after 12 weeks.43 In another study, TGF-β was bound to heparin and co-delivered with dexamethasone from PLGA microspheres to enhance chondrogenesis in vitro and in vivo.33 However, these systems are usually associated with poor protein loading efficiency due to the hydrophobic nature of particles, and the usage of organic solvents in fabricating PLGA microparticles can reduce bioactivity of encapsulated growth factors. Additionally, the particles used in these studies are physically entrapped within conventional nanoporous hydrogels, which will not be retained in the μRB scaffolds due to the macroporosity.
The main goal of the present study is to design drug delivery components specifically for μRB scaffolds that can be entrapped within μRB scaffold, supporting tunable release kinetics, and retain bioactivity in vitro and in vivo to accelerate MSC-based cartilage regeneration. TGF-β3 was used as a model protein given its demonstrated efficacy in enhancing MSC chondrogenesis.22,30 We chose mesoporous silica nanoparticles (MSNs) as the drug delivery vehicles due to their high surface area, high drug loading capacity, commercial availability and demonstrated biocompatibility in vivo.39,48 To allow stable incorporation of MSNs in macroporous μRB scaffold and achieve tunable release kinetics, we chose to coat MSNs with polydopamine, which have been widely used as an adhesive coating 4,23 and for tuning drug release.2,26 MSNs have been previously used to deliver chemotherapeutic agents, proteins, and therapeutic genetic materials.48 The drug payloads can be either diffused into the pores and then coated using a polymeric network to prevent the burst release, or chemically conjugated to the particle surface through a chemical reaction.39 We selected the diffusion loading due to its ease and minimal perturbation to the bioactivity of growth factors.
In this study, we hypothesized that by increasing the concentration of dopamine in the precursor solution, the rate of dopamine polymerization and consequently, the amount of polydopamine coating on the surface of MSNs would increase which can further slow down the diffusion of TGF-β3 through MSNs.6,49 In addition, we hypothesized that incorporating MSN-mediated TGF-β3 release in μRB scaffold could enhance MSC-based cartilage regeneration in vivo. We first characterize the scaffold morphology and release kinetics using MSN coated with varying concentration of dopamine. The bioactivity of released TGF-β3 was first evaluated in vitro, and subsequently in vivo using a mouse subcutaneous model. Outcomes were evaluated using ELISA, scanning electron microscopy, biochemical assays, mechanical testing, histology, and immunofluorescent staining.
Materials and Methods
Fabrication of TGF-β:MSNs
Hydrophilic mesoporous silica nanoparticles (MSNs) were purchased from Degussa AG (Hanau, Germany). For protein loading, MSNs (40 µg/mL) were soaked in TGF-β3 (Peprotech, Rocky Hill, NJ) solution (1 µg/mL) and incubated while mixing (400 rpm, 25 °C) for 30 min to allow the protein molecules diffuse into the mesoporous pores within MSNs. To prepare polydopamine-coated MSNs, 10 mg protein-loaded MSN was dispersed in 1 mL Tris-HCl buffer (pH 8.5) containing dopamine at various concentrations (0.5, 1.0 and 2.0 mg/mL) for 3 hr to allow dopamine polymerization on the surface of MSNs. Polydopamine-coated MSNs were then washed in PBS and centrifuged to remove the unloaded protein, and this process was repeated three times. The amount of unloaded TGF-β3 (in supernatants after each washing step) was quantified using ELISA. By subtracting unloaded protein from total initial protein, the loading efficiency is defined as as (total protein-unloaded protein)/total protein. The loading efficiency of TGF-β3 in MSNs was calculated to be 43 ± 6%.
μRB Fabrication
Gelatin (GEL) μRBs were fabricated as previously reported.13,24 To fabricate chondroitin sulfate (CS) μRBs, chondroitin sulfate sodium salt (from bovine cartilage, Sigma-Aldrich) was functionalized with acrylamide and 2.5 mM CRGDS. CS solution (7.5% (w/v)) was spun into a stirring bath of 2-propanol and internally crosslinked with dithiolretinol to fix the μRB shape.
Scanning Electron Microscopy
To verify if polydopamine coating can enable stable incorporation of MSNs onto the surface of gelatin-CS μRB scaffolds, scaffolds before and after MSN incorporation was assessed using a Hitachi S‐3400N variable pressure scanning electron microscope (VP‐SEM) as previously described.13
Cell Encapsulation in 3D μRB Scaffolds
GEL and CS μRBs were mixed in a 1:1 ratio and hydrated in PBS containing 0.1% (w/v) of photoinitiator lithium phenyl-2,4,6-trimethylbenzoylphosphinate (LAP), reaching a final total μRB density of 7.5% (w/v). For groups with MSNs, the TGF-β:MSNs were added to the LAP solution before hydrating the μRBs. In the in vitro study, the culture medium of each sample were replaced by 1.5 mL of fresh cohndrogenic medium (containing 10 ng/mL TGF-β3)52 every other day (15 ng fresh TGF-β3 every other day). Therefore, the amount of TGF-β3 loaded in “MSN+DPA 1” was adjusted in a way that the average amount of released TGF-β3 would be ~ 7.5 ng/day to be able to compare the results with the group with freshly added TGF-β3 to the medium. For the control group containing directly encapsulated TGF-β3, 150 ng of TGF-β3 was added to PBS used to hydrate μRBs. Human MSCs (Lonza, passage 6) were mixed with the hydrated µRB to reach a density of 10 M mL−1, and incubated for 15 mins at 37 °C to ensure full hydration. After incubation, the cell/μRB mixture was loaded into cylindrical molds (4 mm in diameter and 2 mm in height), photocrosslinked by exposing to UV light (365 nm, 4 mW cm−2, 5 min). Crosslinked µRB scaffolds containing MSCs were transferred to 24-well plates for culture.
Quantifying TGF-β3 Release Using ELISA
TGF-β:MSNs were encapsulated within GEL:CS μRB scaffolds as described above and incubated at 37 °C in DMEM with 10% FBS. To determine the protein release kinetics, the supernatant was collected at every time point and replaced completely with fresh medium. TGF-β3 release was determined using an ELISA assay with purified human TGF-β3 as the standard, following the manufacturer’s protocol (BioGems).
Cell Culture and Quantification of Cartilage Formation In Vitro
Cell-laden μRB scaffolds were first cultured in growth medium for 24 h and then switched to chondrogenic medium for 21 days before final harvest. Four groups were examined including no TGF-β (−T), TGF-β directly encapsulated in μRB scaffolds (+T-encap), freshly added TGF-β in medium (+T-media), and TGF-β released from MSN encapsulated in scaffolds (+T:MSN). A separate in vitro study was performed to determine what components from chondrogenic medium are essential for inducing MSC chondrogenesis. Samples were cultured in DMEM supplemented with single or combination of various components from chondrogenic medium. All in vitro groups were cultured for 21 days before analysis. After 21 days of culture in chondrogenic medium, scaffolds were harvested and digested in papainase solution. DNA, sGAG, and collagen were quantified as previously reported.47 To measure mechanical properties of MSC-produced cartilage after 21 days of in vitro culture, unconfined compression tests were conducted using an Instron 5944 materials testing system (Instron Corporation) with a 10 N load cell (Interface, Inc.).13 Compressive moduli of all samples were determined from the 10–20% region of linear fit curve from the stress versus strain plot. Additionally, histology analyses was performed for cartilage and bone markers including Collagen II, and Collagen X, Collagen I, Safronin O, Masson’s trichrome and alizarin red S staining (ARS).
For in vitro study, each sample was cultured in 1.5 mL of chondrogenic medium (containing 10 ng/mL TGF-β3),47 which is refreshed every other day (i.e. consuming 15 ng TGF-β3 every other day). This is equivalent to consuming 7.5 ng TGF-β3 per day per sample. To match the total amount of TGF-β3 loaded in scaffolds (+T-encap) with the total amount of free TGF-β3 used over 20 days of culture, 150 ng of TGF-β3 was added to PBS used to hydrate μRBs. For T:MSN group, we calculated the amount of MSN with a total accumulated release of 150 ng TGF-β3 after 21 days. Based on our calculated loading efficiency (43%) and 35% accumulated release in vitro after 21 days, MSNs were incubated in solution containing 1000 ng TGF-β3, which led to 1000 ng × 43% × 35% = 150 ng.
Evaluating the Efficacy of TGF-β
MSN in Supporting MSC-Based Cartilage Formation In Vivo Using a Mouse Subcutaneous Model
Animal studies were performed in accordance with the guidelines for the care and use of laboratory animals. All protocols were approved by the Stanford Institutional Animal Care and Use committee. For in vivo subcutaneous study, all groups were first primed in chondrogenic medium for 14 days in vitro to induce chondrogenesis before implantation. Two groups were compared including samples exposed to freshly added TGF-β in vitro before implantation, or samples containing TGF-β:MSN for controlled release over time. Scaffolds were prepared as explained above and implanted subcutaneously into nude female mice (NCr nude, 6 weeks old, Taconic). Mice were sacrificed to obtain constructs after 21 days in vivo. Four samples per group were evaluated for histology analyses for cartilage and bone markers including Collagen II, and Collagen X, Collagen I, Safronin O, Masson’s trichrome and alizarin red S staining (ARS).
Histology and Immunostaining
At each harvesting time point for histology, samples were fixed first in 4% paraformaldehyde for 2 h, before being embedded in optimal cutting temperature compound for cryo-sectioning. For in vivo samples, they were also transferred to 16% ethylenediaminetetraacetic acid for two weeks for decalcification before being embedded. For histological staining, sectioned tissue slices were stained with Safronin O (for sulfated glycosaminoglycans), Masson’s trichrome (for total collagen), and alizarin red S staining (for mineralization). Staining reagents were obtained from Thermo Scientific (Waltham, MA). For immunostaining, sectioned slices were first treated with blocking buffer consisting of 2% goat serum and 3% bovine serum albumin in 1X PBS, then incubated overnight at 48 °C in primary antibody solution containing rabbit polyclonal antibody against Collagen II (1:100 dilution), Collagen I (1:100 dilution), or Collagen X (1:100 dilution). All primary antibodies were purchased from Abcam (Cambridge, MA). After washing, sectioned tissue slices were subsequently incubated with secondary antibody solution for 1 h at room temperature. The following secondary antibody was used including goat anti-rabbit Alexa 488 (1:200 dilution) (Invitrogen, Carlsbad, CA). Nuclei were counterstained with Hoechst 33342 stain (Thermo Scientific, Waltham, MA) and images were taken using a Zeiss fluorescence microscope as previously described.8 Sections were stained with all reagents without primary antibody for negative controls.
Statistical Analysis
All experiments were conducted with a minimum of three distinct samples to verify the trend of results. All data are presented as mean ± standard deviation (n ≥ 3/group). GraphPad Prism (GraphPad Software) was used to perform a one- or two-way analysis of variance followed by Tukey’s multiple comparisons test.
Results
Varying Polydopamine Coating Modulates TGF-β3 Release from MSN
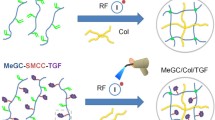
To determine the release kinetics of TGF-β3 from MSNs, TGF-β3 was loaded into MSNs which were then coated with three different concentrations of dopamine (Fig. 1a). The lowest concentration of dopamine (0.5 mg/mL) resulted in burst release of TGF-β3, with all growth factor released by day 7. The highest concentration of dopamine (2 mg/mL) resulted in the slowest release, with only about 20% of the loaded TGF-β3 released after 14 days (Fig. 1b). MSNs coated with intermediate concentration (1 mg/mL) dopamine showed the most desirable release kinetics, with accumulated release up to 30% of the loaded TGF-β3 after 14 days of incubation in vitro (Fig. 1b). Based on an initial loading efficiency of 43%, this is equivalent to ~ 7 ng/day release on average, which is comparable to the dosage used in the free TGF-β3 control group. As such, we chose MSNs coated with 1.0 mg/mL dopamine for all further in vitro and in vivo studies. SEM imaging showed that polydopamine-coated MSNs attached homogenously to the μRB scaffolds (Fig. 1c). In contrast, uncoated MSN failed to be encapsulated inside the μRB scaffolds, and minimal MSN can be observed by SEM (Supplementary Fig. S1). This result is expected as the macroporosity in μRB scaffolds is much larger than the diameter of nanosize MSN, highlighting the importance of using adhesion coating to support stable MSN incorporation.
Fabrication and characterization of release kinetics of TGF-β MSNs coated with varying concentration of dopamine. (a) Schematic of preparing TGF-β:MSN with varying concentrations of dopamine coating; (b) Accumulated percentage of TGF-β released from MSNs with varying dopamine coating; Data are presented as means ± s.d. (n = 3/group). (c) Scanning electron microscopy images of 3D gelatin/CS µRB scaffolds without (left) and with (right) MSNs coated with DPA1. Scale bar: 1 µm.
MSN-Released TGF-β Enhances Cartilage Formation by MSCs In Vitro
To test the efficacy of TGF-β:MSNs in stimulating MSC chondrogenesis in vitro, we evaluated four groups with MSC encapsulated in gelatin-CS μRB scaffolds: without TGF-β3 (− T), TGF-β3 directly encapsulated in the μRB scaffold (+ T encap), TGF-β3 supplemented to the media freshly every other day (+ T media), and TGF-β3 loaded into MSNs (+ T:MSN). All groups showed high cell viability (Fig. 2a), similar cell number and scaffold background on Day 1 (Supplementary Fig. S2), indicating MSNs are cytocompatible and do not interfere with cell adhesion. After 21 days of culture, scaffolds without TGF-β3 or with directly encapsulated TGF-β3 within the scaffold show very little proliferation or cartilage deposition, as shown both by biochemical assays (Figs. 2b and 2c), mechanical testing (Fig. 2d), and histology (Fig. 3). To characterize the phenotype of newly deposition matrix, we performed staining of Safranin-O (sGAG), Masson’s Trichrome (total collagen), Collagen II (articular cartilage marker), Collagen I (fibrocartilage marker) and Collagen X (hypertrophic marker) (Fig. 3). In contrast, TGF-β:MSN group supported robust cartilage deposition to a level comparable to the freshly added TGF-β (positive control) (Figs. 2 and 3). The groups without TGF-β3 or with encapsulated TGF-β3 exhibited very low compressive moduli at the end of culture (~ 5 kPa) (Fig. 2e), which is similar to Day 1 (Supplementary Fig. S2F). In contrast, TGF-β:MSN group and free TGF-β group exhibited over 50-fold increase in compressive moduli up to ~ 400 to 500 kPa (Fig. 2e). Together, these findings validate that MSN-mediated TGF-β release can support MSC chondrogenesis and robust cartilage deposition in vitro.
TGFβ released from MSNs, but not direct TGFβ encapsulation, support robust cartilage deposition by MSCs in vitro to a level comparable to freshly supplemented TGFβ in medium (positive control). A total of four groups were evaluated: – T: no TGFβ in medium, + T encap: TGFβ directly encapsulated in µRB scaffolds, + T media: freshly supplemented TGFβ in medium, + T:MSN: TGFβ-releasing MSNs in µRB scaffolds. (a) Cell viability and morphology at day 1 as shown by live/dead staining, scale bar: 200 µm. (b) fold of cell proliferation at day 21; (c, d) normalized total sGAG and collagen per dry weight at day 21; (e) Compressive moduli of cell-laden µRB scaffolds at day 21. Data is reported as mean ± SD (n = 3/group). *p < 0.05, **p < 0.001. Data are presented as means ± s.d. (n = 3/group).
Histological staining of MSC-laden µRB scaffolds after 21 days of culture in chondrogenic medium. A total of four groups were evaluated: – T: no TGFβ in medium, + T encap: free TGFβ directly encapsulated in µRB scaffolds, + T media: freshly supplemented TGFβ in medium, + T:MSN: TGFβ-releasing MSNs in µRB scaffolds (n = 3/group). (a) Safranin-O to visualize glycosaminoglycans, (b) Masson’s Trichrome to visualize collagen, (c) Collagen II (articular) staining, (d) Collagen I (fibrocartilage) staining, and (e) Collagen X (hypertrophic) staining. Scale bars: 250 µm.
MSN-Mediated TGF-β3 Release Supports Continuous Cartilage Formation In Vivo
When cultured in PBS in vitro, polydopamine-coated MSNs support continuous release of TGF-β3 over long periods for up to 75 days (Fig. 4a). We next evaluated whether TGF-β:MSN can support MSC-based cartilage formation in vivo. Two groups were evaluated including gelatin/CS scaffolds with (+T:MSN) or without (−T:MSN) MSN containing TGF-β. All samples were primed in vitro in chondrogenic medium for 14 days prior to subcutaneous implantation, then harvested at day 35 (21 days of in vivo) (Fig. 4b). − T:MSN group also received exogenous TGF-β (10 ng/mL) during in vitro priming. After 14 days of in vitro culture, both groups showed interconnected sGAG and collagen deposition, high collagen II expression, and minimal hypertrophy (collagen X) or mineralization (ARS) (Fig. 4c). Upon in vivo harvest at day 35, -T:MSN groups showed substantial loss of sGAG and robust mineralization, which was accompanied by decreased collagen II and increased collagen I and collagen X staining (Fig. 4d). In contrast, the + T:MSN group showed increased sGAG and collagen production, robust collagen II staining, and low level of mineralization. Together, these results showed in situ continued release of TGF-β is necessary for supporting continuous cartilage deposition in vivo, and MSN-mediated release was sufficient to support cartilage deposition while reducing undesirable endochondral ossification in a subcutaneous model.
µRB scaffolds containing TGF-β releasing MSNs support continuous cartilage formation by MSCs and minimizes endochondral ossification in a mouse subcutaneous model. Data are presented as means ± s.d. (n = 3/group). (a) TGF-β release from MSNs can be detected for up to 75 days in vitro. (b) Schematic of in vivo experimental design. All samples were primed in chondrogenic medium for 14 days prior to implantation. – T:MSN group also received exogenous TGF-β (10 ng/mL) during in vitro priming. Histology and immunofluorescence staining of cartilage and bone markers of MSC-laden sample at (c) day 14 (the end of in vitro priming) and (d) day 35 (the end of in vivo implantation). Safranin-O (glycosaminoglycan), Trichrome: total collagen, ARS: alizarin red S staining for mineralization. Collagen II (articular cartilage marker), Collagen I (fibrocartilage marker), and Collagen X (hypertrophic marker). Scale bars: 250 µm.
Discussion
Our previous work has shown macroporous gelatin μRB scaffolds are more efficient in accelerating MSC-based cartilage regeneration in vitro than conventional gelatin hydrogels.8 To realize the potential of gelatin μRB scaffolds for supporting MSC-based cartilage regeneration in vivo, it is important to develop an in situ drug delivery system that is compatible with the macroporous μRB scaffolds. Here we report a drug delivery platform specifically designed for the macroporous μRB scaffold using polydopamine-coated mesoporous silica nanoparticles (MSNs). The polydopamine coating of MSN allows easy and stable incorporation of MSNs into macroporous µRB scaffolds (Fig. 1) and enables tunable release kinetics with retained bioactivity (Figs. 1 and 2). The way polydopamine coating enable tunable TGF-β3 release can be mediated through a combination of several possible mechanisms. First, the adhesive polydopamine coating on the surface of MSNs sets up a physical barrier against the protein diffusion out of the mesopores of MSN. As such, increasing polydopamine concentration is expected to increase the diffusion barrier, thereby slowing down the release, as validated by our in vitro release data (Fig. 1b). Second, polydopamine is formed at pH ~ 8.5, but degrades in lower pH than 8.5.42 Therefore, when cultured in physiological pH (7.4) in vitro or in vivo, polydopamine coating will slowly degrade over time, allowing protein release. It should be noted that some of the TGF-β3 may interact with dopamine or denature during the coating step, therefore not detectable by ELISA. In this case, these growth factors will probably also not be bioactive for the cells. As such, it is still reasonable to use the trend of release kinetics from ELISA to choose the optimal concentration of dopamine coating (1 mg/mL) that avoids burst release but still allows more sustained protein release over time.
MSNs have been widely used for various drug delivery applications in vivo due to their mesoporous structures and high surface areas for loading anticancer drugs or biologically active molecules (e.g., proteins and nucleotides).5,42 In general, the cytotoxicity and biocompatibility of nanomaterials depend on the size, shape, surface chemistry, and charge of particles. Several studies show that when MSNs were used at concentrations lower than 100 µg/mL, minimum cytotoxicity was observed.18,44 In the current study, we used 25 µg/mL of MSNs in the scaffold, and did not observe any fibrosis or cytotoxicity both in vitro and in vivo. In addition, it has been shown that in low concentrations (< 100 µg/mL), MSNs could be cleared from the body through excretion with urine.44
Our results demonstrate that TGF-β3 released from polydopamine-coated MSNs enhance cartilage deposition by MSCs to levels comparable to the control treated with fresh TGF-β3 control in vitro (Figs. 2 and 3). Furthermore, only μRB scaffolds containing T:MSN support continuous cartilage deposition in vivo (Fig. 4). These results confirm that sufficient amount of TGF-β3 released from MSNs retain bioactivity to achieve the desirable biological outcomes. It is possible that some of the loaded TGF-β3 remain bound to MSNs. Previous studies have shown that even the immobilized TGF-β3 can induce chondrogenic differentiation of MSCs.28,31 As such, both freely released TGF-β3 and MSN-bound TGF-β3 could contribute to the enhanced cartilage deposition observed in our study.
An important finding of the current study is that the continued release of TGF-β3 after subcutaneous implantation is essential for maintaining cartilage phenotype and reducing undesirable endochondral ossification (Figs. 4c and 4d). MSC-formed cartilage tissues often shows hypertrophy marker and early bone markers including type X collagen, alkaline phosphatase (ALP) and matrix metallopeptidase 13 (MMP-13),30,50 which is similar to the phenotype of chondrocytes in growth plates during endochondral ossification. Additionally, some in vivo studies have observed the invasion of blood vessels and matrix calcification after human chondrogenic MSCs pellet transplantation into mice.35,36 This natural behavior is one of the main concerns with applications of MSCs for articular cartilage regeneration. Further, it has been demonstrated that TGF-β signaling can reduce undesirable calcification and catabolic gene expression, such as collagen X and MMP13; while increase collagen II and aggrecan expressions.15,29,38,45 Interestingly, this is consistent with our observations that TGF-β:MSNs group reduced endochondral ossification that was observed in control group without MSNs, possibly due to the sustained release of TGF-β.
It is also worth pointing out that mouse subcutaneous model does not mimic the soluble factors or weight-bearing stimuli in the joint, which may explain the observed endochondral ossification.12,32 Previous studies have shown endochondral ossification is commonly observed in the subcutaneous model, but much less so in the cartilage defect model.41,46 We chose the mouse subcutaneous model in the present study as this is the first proof-of-concept in vivo study for MSN-mediated drug delivery in macroporous µRB scaffolds. Compared to other more complicated animal models, the subcutaneous model allows testing a larger sample size using less animals, and is commonly used as the first animal model for initial assessment of new biomaterials for supporting cartilage regeneration in vivo. Now that we have established MSN-containing μRB scaffolds can enhance MSC-based cartilage regeneration in a mouse subcutaneous model, future studies can validate its efficacy using more disease relevant models such as rat cartilage defect model and other larger animal cartilage defect models.7
Another limitation of the current study is the need to prime MSC-seeded μRB scaffolds in vitro for 2 weeks prior to in vivo implantation. This is because the current study focuses on single factor delivery, yet we found from our in vitro screening study that multiple factors in chondrogenic medium are necessary to initiate robust MSC chondrogenesis (Supplementary Fig. S4). To reduce or eliminate the need for in vitro priming, future studies are necessary to determine the optimal MSN formulation for co-delivery multiple factors from μRB scaffolds. Given the modular design of polydopamine-coated MSNs (Fig. 1b), different MSNs formulated for delivering various factors can be optimized independently, and mixed and co-encapsulated together in the μRB scaffolds to achieve the sustained release of multiple factors.
While the present paper focuses on cartilage regeneration application, the concept of μRB scaffolds capable of achieving in situ drug delivery can be broadly applicable to enhance regeneration of other tissue types. For example, controlled release of bone morphogenetic protein-2 (BMP-2) may be used to accelerate stem cell-based bone formation in vivo.3,25 Moreover, the facile and tunable polydopamine coatings allows customized design of MSNs to achieve temporal release of different growth factors. For example, synovial-derived MSC pellets treated with FGF-2 followed by exposure to a combination of TGF-β1 and IGF-1 showed significantly more cartilage formation compared to other temporal growth factor regimes.34 Sequential treatment with TGF-β1 followed by IGF-1 has been shown to enhance MSC chondrogenesis compared to control without sequential exposure51 or TGF-β3 exposure alone.14
In summary, here we developed MSN-containing macroporous μRB scaffolds capable of prolonged release of TGF-β3 release to enhance MSC-based cartilage regeneration in vitro and in vivo. By tuning polydopamine coating, we can achieve tunable release kinetics. TGF-β3 released from MSNs retained its bioactivity comparable to freshly added TGF-β3 control, and led to robust cartilage formation in vitro. When implanted in vivo in a mouse subcutaneous model, MSN-mediated TGF-β3 release was essential to support continuous cartilage formation while reducing undesirable endochondral ossification. The modular design of MSN-mediated drug delivery allows expanding the platform for delivering multiple soluble factors with individually optimized release kinetics, and can be applicable to enhance regeneration of other tissue types.
References
Andrades, J. A., S. C. Motaung, P. Jiménez-Palomo, S. Claros, J. M. López-Puerta, J. Becerra, et al. Induction of superficial zone protein (SZP)/lubricin/PRG 4 in muscle-derived mesenchymal stem/progenitor cells by transforming growth factor-β1 and bone morphogenetic protein-7. Arthritis Res Therapy 14:R72, 2012.
Bai, Y.-X., Y.-F. Li, Y. Yang, and L.-X. Yi. Covalent immobilization of triacylglycerol lipase onto functionalized nanoscale SiO2 spheres. Process. Biochem. 41:770–777, 2006.
Barati, D., S. R. P. Shariati, S. Moeinzadeh, J. M. Melero-Martin, A. Khademhosseini, and E. Jabbari. Spatiotemporal release of BMP-2 and VEGF enhances osteogenic and vasculogenic differentiation of human mesenchymal stem cells and endothelial colony-forming cells co-encapsulated in a patterned hydrogel. J. Control. Release 223:126–136, 2016.
Bernsmann, F., V. Ball, F. Addiego, A. Ponche, M. Michel, J. J. D. A. Gracio, et al. Dopamine–melanin film deposition depends on the used oxidant and buffer solution. Langmuir 27:2819–2825, 2011.
Bharti, C., U. Nagaich, A. K. Pal, and N. Gulati. Mesoporous silica nanoparticles in target drug delivery system: a review. Int. J. Pharm. Investig. 5:124, 2015.
Cheng, W., J. Nie, L. Xu, C. Liang, Y. Peng, G. Liu, et al. pH-sensitive delivery vehicle based on folic acid-conjugated polydopamine-modified mesoporous silica nanoparticles for targeted cancer therapy. ACS Appl. Mater. Interfaces 9:18462–18473, 2017.
Chu, C. R., M. Szczodry, and S. Bruno. Animal models for cartilage regeneration and repair. Tissue Eng. B 16:105–115, 2010.
Conrad, B., L. H. Han, and F. Yang. Gelatin-based microribbon hydrogels accelerate cartilage formation by mesenchymal stem cells in 3D. Tissue Eng. A 24:1630–1641, 2018.
Erickson, I. Optimization and Translation of MSC-Based Hyaluronic Acid Hydrogels for Cartilage Repair. Pennsylvania: University of Pennsylvania, 2011.
Erickson, I. E., S. R. Kestle, K. H. Zellars, M. J. Farrell, M. Kim, J. A. Burdick, et al. High mesenchymal stem cell seeding densities in hyaluronic acid hydrogels produce engineered cartilage with native tissue properties. Acta Biomater. 8:3027–3034, 2012.
Ertan, A. B., P. Yılgor, B. Bayyurt, A. C. Çalıkoğlu, Ç. Kaspar, F. N. Kök, et al. Effect of double growth factor release on cartilage tissue engineering. J. Tissue Eng. Regener. Med. 7:149–160, 2013.
Fahy, N., M. Alini, and M. J. Stoddart. Mechanical stimulation of mesenchymal stem cells: implications for cartilage tissue engineering. J. Orthop. Res. 36:52–63, 2018.
Farrell, M. J., M. B. Fisher, A. H. Huang, J. I. Shin, K. M. Farrell, and R. L. Mauck. Functional properties of bone marrow-derived MSC-based engineered cartilage are unstable with very long-term in vitro culture. J Biomech. 47:2173–2182, 2014.
Fong, C.-Y., A. Subramanian, K. Gauthaman, J. Venugopal, A. Biswas, S. Ramakrishna, et al. Human umbilical cord Wharton’s jelly stem cells undergo enhanced chondrogenic differentiation when grown on nanofibrous scaffolds and in a sequential two-stage culture medium environment. Stem Cell Rev. Rep. 8:195–209, 2012.
Freyria, A.-M., and F. Mallein-Gerin. Chondrocytes or adult stem cells for cartilage repair: the indisputable role of growth factors. Injury 43:259–265, 2012.
Gegg, C., and F. Yang. Spatially patterned microribbon-based hydrogels induce zonally-organized cartilage regeneration by stem cells in 3D. Acta Biomater. 101:196–205, 2019.
Han, L.-H., B. Conrad, M. T. Chung, L. Deveza, X. Jiang, A. Wang, et al. Microribbon-based hydrogels accelerate stem cell-based bone regeneration in a mouse critical-size cranial defect model. J. Biomed. Mater. Res. A 104:1321, 2016.
He, Q., and J. Shi. Mesoporous silica nanoparticle based nano drug delivery systems: synthesis, controlled drug release and delivery, pharmacokinetics and biocompatibility. J. Mater. Chem. 21:5845–5855, 2011.
Karimi, T., D. Barati, O. Karaman, S. Moeinzadeh, and E. Jabbari. A developmentally inspired combined mechanical and biochemical signaling approach on zonal lineage commitment of mesenchymal stem cells in articular cartilage regeneration. Integr. Biol. 7:112–127, 2014.
Kim, T.-K., B. Sharma, C. Williams, M. Ruffner, A. Malik, E. G. McFarland, et al. Experimental model for cartilage tissue engineering to regenerate the zonal organization of articular cartilage. Osteoarthritis Cartil. 11:653–664, 2003.
Kisiday, J., M. Jin, B. Kurz, H. Hung, C. Semino, S. Zhang, et al. Self-assembling peptide hydrogel fosters chondrocyte extracellular matrix production and cell division: implications for cartilage tissue repair. Proc. Natl. Acad. Sci. USA 99:9996–10001, 2002.
Kondo, M., K. Yamaoka, K. Sonomoto, S. Fukuyo, K. Oshita, Y. Okada, et al. IL-17 inhibits chondrogenic differentiation of human mesenchymal stem cells. PLoS ONE 8:e79463, 2013.
Lee, H., S. M. Dellatore, W. M. Miller, and P. B. Messersmith. Mussel-inspired surface chemistry for multifunctional coatings. Science 318:426–430, 2007.
Lee, S., X. Tong, L.-H. Han, A. Behn, and F. Yang. Aligned microribbon-like hydrogels for guiding three-dimensional smooth muscle tissue regeneration. J. Biomed. Mater. Res. A 104:1064–1071, 2016.
Lissenberg-Thunnissen, S. N., D. J. de Gorter, C. F. Sier, and I. B. Schipper. Use and efficacy of bone morphogenetic proteins in fracture healing. Int. Orthop. 35:1271, 2011.
Liu, C.-Y., and C.-J. Huang. Functionalization of polydopamine via the aza-michael reaction for antimicrobial interfaces. Langmuir 32:5019–5028, 2016.
Madry, H., A. Rey-Rico, J. K. Venkatesan, B. Johnstone, and M. Cucchiarini. Transforming growth factor beta-releasing scaffolds for cartilage tissue engineering. Tissue Eng. B 20:106–125, 2013.
Motoyama, M., M. Deie, A. Kanaya, M. Nishimori, A. Miyamoto, S. Yanada, et al. In vitro cartilage formation using TGF-β-immobilized magnetic beads and mesenchymal stem cell-magnetic bead complexes under magnetic field conditions. J. Biomed. Mater. Res. A 92:196–204, 2010.
Mueller, M. B., M. Fischer, J. Zellner, A. Berner, T. Dienstknecht, L. Prantl, et al. Hypertrophy in mesenchymal stem cell chondrogenesis: effect of TGF-β isoforms and chondrogenic conditioning. Cells Tissues Organs 192:158–166, 2010.
Mueller, M. B., and R. S. Tuan. Functional characterization of hypertrophy in chondrogenesis of human mesenchymal stem cells. Arthritis Rheum. 58:1377–1388, 2008.
Niger, C., K. E. Beazley, and M. Nurminskaya. Induction of chondrogenic differentiation in mesenchymal stem cells by TGF-beta cross-linked to collagen-PLLA [poly (L-lactic acid)] scaffold by transglutaminase 2. Biotechnol. Lett. 35:2193–2199, 2013.
O’Conor, C. J., N. Case, and F. Guilak. Mechanical regulation of chondrogenesis. Stem Cell Res. Therapy 4:61, 2013.
Park, J. S., K. Na, D. G. Woo, H. N. Yang, and K.-H. Park. Determination of dual delivery for stem cell differentiation using dexamethasone and TGF-β3 in/on polymeric microspheres. Biomaterials 30:4796–4805, 2009.
Pei, M., F. He, and G. Vunjak-Novakovic. Synovium-derived stem cell-based chondrogenesis. Differentiation 76:1044–1056, 2008.
Pelttari, K., A. Winter, E. Steck, K. Goetzke, T. Hennig, B. G. Ochs, et al. Premature induction of hypertrophy during in vitro chondrogenesis of human mesenchymal stem cells correlates with calcification and vascular invasion after ectopic transplantation in SCID mice. Arthritis Rheum. 54:3254–3266, 2006.
Scotti, C., B. Tonnarelli, A. Papadimitropoulos, A. Scherberich, S. Schaeren, A. Schauerte, et al. Recapitulation of endochondral bone formation using human adult mesenchymal stem cells as a paradigm for developmental engineering. Proc. Natl Acad. Sci. 107:7251–7256, 2010.
Sellers, R. S., D. Peluso, and E. A. Morris. The effect of recombinant human bone morphogenetic protein-2 (rhBMP-2) on the healing of full-thickness defects of articular cartilage. JBJS 79:1452–1463, 1997.
Shintani, N., K. A. Siebenrock, and E. B. Hunziker. TGF-ss1 enhances the BMP-2-induced chondrogenesis of bovine synovial explants and arrests downstream differentiation at an early stage of hypertrophy. PLoS ONE 8:e53086, 2013.
Slowing, I. I., J. L. Vivero-Escoto, C. W. Wu, and V. S. Lin. Mesoporous silica nanoparticles as controlled release drug delivery and gene transfection carriers. Adv. Drug Deliv. Rev. 60:1278–1288, 2008.
Spiller, K. L., S. A. Maher, and A. M. Lowman. Hydrogels for the repair of articular cartilage defects. Tissue Eng. B 17:281–299, 2011.
Steck, E., J. Fischer, H. Lorenz, T. Gotterbarm, M. Jung, and W. Richter. Mesenchymal stem cell differentiation in an experimental cartilage defect: restriction of hypertrophy to bone-close neocartilage. Stem Cells Dev. 18:969–978, 2009.
Tamanna, T., J. B. Bulitta, C. B. Landersdorfer, V. Cashin, and A. Yu. Stability and controlled antibiotic release from thin films embedded with antibiotic loaded mesoporous silica nanoparticles. RSC Adv. 5:107839–107846, 2015.
Tanaka, H., T. Sugita, Y. Yasunaga, S. Shimose, M. Deie, T. Kubo, et al. Efficiency of magnetic liposomal transforming growth factor-beta 1 in the repair of articular cartilage defects in a rabbit model. J. Biomed. Mater. Res. A 73:255–263, 2005.
Tang, F., L. Li, and D. Chen. Mesoporous silica nanoparticles: synthesis, biocompatibility and drug delivery. Adv. Mater. 24:1504–1534, 2012.
Trippel, S. B. Growth factor actions on articular cartilage. J. Rheumatol. Suppl. 43:129–132, 1995.
Vinardell, T., E. J. Sheehy, C. T. Buckley, and D. J. Kelly. A comparison of the functionality and in vivo phenotypic stability of cartilaginous tissues engineered from different stem cell sources. Tissue Engineering. A 18:1161–1170, 2012.
Wang, T., J. H. Lai, and F. Yang. Effects of hydrogel stiffness and extracellular compositions on modulating cartilage regeneration by mixed populations of stem cells and chondrocytes in vivo. Tissue Eng. A 22:1348–1356, 2016.
Wang, Y., Q. Zhao, N. Han, L. Bai, J. Li, J. Liu, et al. Mesoporous silica nanoparticles in drug delivery and biomedical applications. Nanomedicine 11:313–327, 2015.
Wei, Y., L. Gao, L. Wang, L. Shi, E. Wei, B. Zhou, et al. Polydopamine and peptide decorated doxorubicin-loaded mesoporous silica nanoparticles as a targeted drug delivery system for bladder cancer therapy. Drug Deliv. 24:681–691, 2017.
Winter, A., S. Breit, D. Parsch, K. Benz, E. Steck, H. Hauner, et al. Cartilage-like gene expression in differentiated human stem cell spheroids: a comparison of bone marrow-derived and adipose tissue-derived stromal cells. Arthritis Rheum. 48:418–429, 2003.
Worster, A. A., B. D. Brower-Toland, L. A. Fortier, S. J. Bent, J. Williams, and A. J. Nixon. Chondrocytic differentiation of mesenchymal stem cells sequentially exposed to transforming growth factor-beta1 in monolayer and insulin-like growth factor-I in a three-dimensional matrix. J. Orthop. Res. 19:738–749, 2001.
Xia, P., X. Wang, Y. Qu, Q. Lin, K. Cheng, M. Gao, et al. TGF-β1-induced chondrogenesis of bone marrow mesenchymal stem cells is promoted by low-intensity pulsed ultrasound through the integrin-mTOR signaling pathway. Stem Cell Res. Therapy 8:281, 2017.
Acknowledgments
The authors would like to thank NIH R01DE024772, NIH R01AR074502, Stanford Coulter translational seed grant, and Stanford SPARK program for funding. C.G. would like to thank the Stanford Bio-X graduate fellowship for support. The authors would also like to thank Anthony Behn for technical assistance with mechanical testing.
Conflict of interest
No potential conflicts of interest exist.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Debra T. Auguste oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Barati, D., Gegg, C. & Yang, F. Nanoparticle-Mediated TGF-β Release from Microribbon-Based Hydrogels Accelerates Stem Cell-Based Cartilage Formation In Vivo. Ann Biomed Eng 48, 1971–1981 (2020). https://doi.org/10.1007/s10439-020-02522-z
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-020-02522-z