Abstract
Articular cartilage has limited healing and self-repair capability. Damage to articular cartilage becomes irreversible leading to osteoarthritis, which can impact a person’s quality of life. Approximately, 5–10% of cartilage tissue is made up of sulfated glycosaminoglycans (GAGs), which sequester growth factors as well as provide structural integrity to the native cartilage tissue. This study evaluated the chondrogenic differentiation of human mesenchymal stem cells (MSCs) on gelatin-based scaffolds containing partially sulfated cellulose (pSC), a GAG mimetic derived from cellulose, in comparison to native GAGs, chondroitin sulfate-A (CS-A) and chondroitin sulfate-C (CS-C), where pSC has similarity to CS-C in terms of degree and pattern of sulfation. Scaffolds were prepared by electrospinning gelatin with pSC or the native GAGs. All scaffolds consist of fibers having average diameters of approximately 3 μm and inter-fiber spacing of approximately 30 μm and were hydrolytically stable throughout the culture. MSCs cultured on pSC containing scaffolds showed early production of sulfated GAGs and higher collagen type II to type I ratio than native GAGs. Among the native GAGs, chondrogenesis was promoted to a greater extent for CS-C in comparison to CS-A containing scaffolds, which suggests the pattern of sulfation impacts chondrogenesis. Partially sulfated cellulose could be used as a potential GAG mimic for cartilage tissue engineering applications.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Adult cartilage tissue has been shown to have limitations in intrinsic healing or self-repair.4,39 Various surgical techniques have been implemented in treatment and restoration of injured articular cartilage tissue, including abrasion arthroplasty, microfracture, drilling, osteochondral autograft or allograft transplantation and autologous chondrocyte implantation.11 These methods have not proven to be completely effective since they have resulted in formation of mechanically inferior fibrocartilage.32 The extracellular matrix of cartilage is made up of collagen type II and proteoglycans. Proteoglycans make up 10–15% of cartilage tissue and are composed of 5% protein and 95% glycosaminoglycans (GAGs).39,41 The major GAGs found in articular cartilage are hyaluronic acid, chondroitin sulfate, keratan sulfate, dermatan sulfate and heparan sulfate.6,45 GAGs play an important role in cell signaling, proliferation and differentiation. Sulfated GAGs, chondroitin sulfates (CS-A, CS-C, CS-E), heparin, heparan sulfate and dermatan sulfate, have been used for studies in promoting chondrogenesis5,8,9,10,23,43,46 and may have potential for use for cartilage tissue engineering strategies. However, native GAGs have limited availability and lack homogeneity when isolated from native tissues.
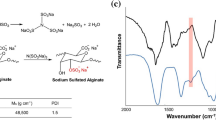
Cellulose is a linear polysaccharide abundantly found in nature and could be modified via sulfation to form cellulose sulfate. Cellulose sulfate has been used for a variety of biomedical applications such as an anticoagulant, antiviral agent, microbicide, contraceptive agent1,14,24,40 and for encapsulating cells.36 Since the chemical structure of cellulose sulfate is known to mimic that of natural sulfated GAGs such as CS-C (Fig. 1), it has been used as GAG mimetic for cartilage tissue engineering approaches and supports chondrogenic differentiation of mesenchymal stem cells.16,17
In this study, partially sulfated cellulose (sulfated predominantly at 6-carbon position on the glucose monomer unit, pSC) incorporated in fibrous gelatin scaffolds was investigated for its effect on the chondrogenic differentiation of human mesenchymal stem cells (MSCs). This was compared to gelatin fibers containing commercially available chondroitin sulfates (CS-A, which is sulfated mainly at the 4-carbon position of the monosaccharide unit and CS-C sulfated mainly at 6-carbon position of the monosaccharide unit). Gelatin was chosen since it provides sites for cellular attachment. This study is the first study to compare the chondro-inductive nature of cellulose sulfate in comparison to native GAGs as a potential GAG mimetic for cartilage tissue engineering applications.
Materials and Methods
Materials
Gelatin type B, from bovine skin (Sigma, St Louis, MO, USA); chondroitin sulfate A sodium salt from bovine trachea (CS-A, Sigma), chondroitin sulfate sodium salt from shark cartilage (CS-C, Sigma), sodium cellulose (pSC, prepared as published16). Ethanol (200 proof, Sigma), N-(3-Dimethylaminopropyl)-N’-ethyl carbodiimide (EDC) (Sigma), N-hydroxysulfosuccinimide (NHS) (Sigma); Human bone marrow (Lonza, Walkersville, MD, USA); tissue culture polystyrene flasks (NunC, (Fisher Scientific, Waltham, MA, USA); Dubelcco’s Modified Eagle’s Medium (DMEM, Fisher Scientific), fetal bovine serum (Hyclone, Fisher Scientific) and antibiotic–antimycotic (Fisher Scientific); trypsin (Fisher Scientific); polypropylene 96-well plates (Fisher Scientific); DMEM high glucose containing 4 mM l-glutamine (Fisher Scientific), Dexamethasone (Sigma), Ascorbic acid-2-phosphate (Wako Chemicals, Richmond, VA, USA), ITS + Premix Culture Supplement (Corning, Teterboro, NJ, USA), Sodium Pyruvate (Sigma), Proline (Sigma), Transforming Growth Factor-Beta 3 (TGF-β3, ProSpec, Israel); Quant-iT dsDNA Picogreen Assay Kit (Fisher Scientific); Papain (Sigma); Triton X-100 (Sigma); TE buffer (Invitrogen); paraformaldehyde (Sigma); donkey serum (Sigma); monoclonal rabbit anti-human collagen type II antibody (EMD Millipore, Burlington, MA, USA), polyclonal rabbit anti-human aggrecan (Abcam, Cambridge, MA, USA), donkey anti-rabbit Immunoglobin G conjugated to Alexa Fluor 488 (EMD Millipore); rhodamine phalloidin (Fisher Scientific); 4′,6-diamidino-2-phenylindole (DAPI, Fisher Scientific); 1,9-dimethylmethylene blue dye (DMMB, Sigma); QuantiTect SYBR Green RT-PCR Kit (Qiagen, Hilden, Germany); RNeasy Micro Kit (Qiagen); Collagen type II ELISA kit (Chondrex, Redmond, WA, USA); Collagen type I ELISA kit (Chondrex).
pSC was characterized for molecular weight, degree of sulfation and sulfate position, as previously described.25 pSC had a molecular weight of 365 kDa, degree of sulfation per monosaccharide unit of 0.5 and sulfate position predominantly at the 6-carbon position of the glucose monomer unit. CS-A and CS-C had a molecular weight of 34 kDa and 50 kDa, respectively, and degree of sulfation of 0.32 and 0.54, respectively. For the sulfate positions, CS-C, derived from shark cartilage, is a mixture of CS-4 (CS-A), CS-6 (CS-C), and CS-2,6 (CS-D) in a 1:1:1 ratio where the sulfate positions are at the 4-, 6- and 2- and 6-carbon positions of the disaccharide unit, respectively. CS-A from bovine trachea is a mixture of CS-A and CS-C in a 2:1 ratio where the sulfate positions occur at the 4- and 6-carbon positions of the disaccharide unit, respectively, as previously described.25
Fabrication of Scaffolds
Gelatin scaffolds containing 5 w/w% native GAGs (CS-A, CS-C) and pSC were fabricated using previously published protocols.16,17 Briefly, solutions containing 24 w/w% gelatin and the different GAGs in deionized water (DI water) were prepared by mixing in 60 °C water bath. Gelatin only solutions were also prepared similarly. For electrospinning, the syringe containing the gelatin-GAG solution was maintained at 60 °C using a heating chamber. The solution was charged by applying a voltage of 40 kV to a 14-gauge needle attached to the syringe containing the solution as the solution is being ejected at flow rate of 6.5 ml/hour. A negative voltage charge of 20 kV was applied to a flat collector plate to allow the electrospinning of the gelatin solution onto the collector. Approximately, 30 cm distance was maintained between the needle and the collector. Optimum humidity of 25–30% and temperature of 24 °C was maintained in the electrospinning chamber throughout the process. Scaffolds were crosslinked using N-(3-dimethyl aminopropyl)-N’-ethyl carbodiimide (EDC) with N-hydroxysucciamide (NHS) for 96 h, followed by immersion in 0.1 M sodium phosphate dibasic (Fisher Scientific) containing solution for two hours to remove byproducts of the crosslinker and then, washed with DI water thrice. All steps were performed at room temperature. The scaffolds were allowed to air dry until use. The scaffold thickness of hydrated scaffolds for all further analyses was approximately 0.2 ± 0.05 mm, as measured using a caliper (VWR Traceable digital caliper).
Scaffold Morphology
The dried scaffolds were hydrated in 1 × Dulbecco Phosphate Buffer Saline (PBS, Invitrogen) for one hour and then lyophilized until completely dried. They were further sputter coated with gold palladium (EMS 150 TES, PA, USA) and viewed using a Scanning Electron Microscope (SEM, LEO 1530 Gemini, Germany) with accelerating voltage of 2-3 kV and working distance of 4 to 9 mm. The average fiber diameter was determined by measuring diameters of 80 fibers (16 fibers of n = 5 per scaffold) of each scaffold type from the images obtained from SEM using ImageJ software (National Institute of Health, MD, USA). The inter-fiber spacing was measured by measuring the voids created by three intersecting fibers. Eighty inter-fiber spaces (16 for n = 5 per scaffold) for each scaffold were measured and their average was determined as the inter-fiber spacing. The porosity of the scaffold was measured as follows.

where  is the density of the scaffold (mass of scaffold divided by total volume) and raw is relative density of the gelatin which is approximately 1.4 g/cm3.
is the density of the scaffold (mass of scaffold divided by total volume) and raw is relative density of the gelatin which is approximately 1.4 g/cm3.
Scaffold Mechanical Properties
Tensile and compression testing was used to evaluate mechanical properties of the scaffolds. Tensile testing of the scaffolds was performed as described previously16,17,18,19 to determine ultimate tensile stress and elastic modulus. Briefly, all samples were hydrated in PBS for 1 h prior to testing. The hydrated samples were cut into rectangular strips of 5 mm width and 15 mm length. The samples were then mounted onto a customized holder having a 5 mm*5 mm cutout of the testing area to avoid slippage or damage from the grips where the gauge length was 5 mm. The tensile testing was conducted using a crosshead speed of 5 mm/min at room temperature using an Instron Model 3342 (Instron, MA). The compressive elastic modulus and stress at 10% strain of the samples were determined using TA Electroforce® 3100 (TA Instruments, TA Electroforce Group, Eden Priarie, MN, USA). The scaffolds were hydrated in PBS for an hour and cut in 6 mm discs using biopsy punches. They were stacked to 0.4 mm thickness for evaluation. Compression testing was performed at 10% strain at equilibrium. A sample size of 10 per group was tested for both tensile and compression testing.
Characterizing the Presence of the Sulfated GAGs in the Fibers
The presence of the sulfated GAG in the fibers was detected using Fourier transform infrared-attenuated total reflectance analysis (FTIR-ATR, Perkin-Elmer, Shelton, CT, USA) and energy-dispersive X-ray (EDX) spectroscopy (SEM–EDX; Inca analyzer, Oxford Instruments). The gold–palladium sputter coated samples were analyzed using a high voltage of 5 kV in vacuum to detect the presence of sulfur on the scaffold fibers.
Hydrolytic Stability of the Scaffolds
The stability of the scaffolds in aqueous conditions was determined since they are used in cell culture conditions for up to 28 days. The scaffolds were initially hydrated in PBS and cut to 6 mm in diameter. They were then dried and their dimensions (diameter and thickness) and weight were measured. The scaffolds (n = 4) were then incubated in 100 ul PBS at 37 °C. PBS was changed at 10 min, 6 h, and 1, 2, 4, 7, 10, 14, 21 and 28 days. The weights and dimensions were measured at all time points. Change in swelling was measured as,
where Whydrated is the weight of the hydrated scaffold at each time point. Winitial is the initial dry weight of each scaffold. Change in dimension was measured as change in the cross-sectional area of hydrated scaffolds as compared to the initial dry scaffolds. The change in weight and dimension over time was reported as fold change in comparison to 10 min of PBS incubation.
The dissolution of GAGs from the scaffold was tested using the DMMB assay.12 The scaffolds (n = 5) were incubated in PBS for 28 days. The PBS was collected after days 1, 2, 4, 7, 10, 14, 21 and 28 and was measured with respect to the standard curve obtained for corresponding sulfated GAGs.
Evaluation of In Vitro Chondrogenesis on Scaffolds
Human MSCs were obtained from human bone marrow aspirates (Lonza) from three male and female donors, ages 18–30 years old, according to previous published protocols and cryopreserved before use.20 Cryopreserved MSCs were thawed and expanded on tissue culture polystyrene flasks (NunC, Rochester, NY, USA) in general media (GM) comprised of Dubelcco’s Modified Eagle’s Medium (DMEM, Gibco, Carlsbad, CA, USA), 10% fetal bovine serum (FBS, Hyclone, Logan, UT, USA) and 1% 1 × Antibiotic–Antimycotic (Gibco, Carlsbad, CA, USA) until 70–80% confluent. MSCs, at passage 3, were seeded on scaffolds, gelatin alone, and gelatin containing pSC (Gel-pSC) CS-C, (Gel-CS-C), or CS-A (Gel-CS-A). All scaffolds were sterilized by immersing in 100% ethanol (Fisher Scientific, USA) for 20 min, allowed to air dry overnight and washed three times with PBS before cell seeding. Scaffolds were inserted into low attachment polypropylene plates (96 well-plates, Non-treated, Corning, UT, USA) for 6 mm disks or ultra-low attachment 24 well-plates (Corning, UT, USA) for 12 mm disks. MSCs were seeded on scaffolds at 500,000 cells/mL in chondrogenesis induction medium (CCM+) consisting of high-glucose DMEM supplemented with 1 mM sodium pyruvate, 0.35 mM l-proline, 4 mM l-glutamine, 1% antibiotic–antimycotic, 1% ITS-Premix consisting of insulin, human transferrin and selenous acid and 10 ng/ml of TGF-β3. Cultures were maintained for 28 days. CCM + media was used throughout the culture period and was replaced every 3–4 days. The samples were collected at days 1, 4, 7, 14 and 28 for assays. The following experiments were performed thrice using three different donors.
Cell Growth on Scaffolds
Cells were evaluated for cell growth on scaffolds at days 14 and 28 using the Quant-iT dsDNA Picogreen Assay Kit (Invitrogen). Four samples of each scaffold were collected at each time point. Standards using MSCs were prepared to quantify the cell number. The samples and standards were incubated in Papain (Sigma Aldrich) extraction solution overnight at 65 °C. The picogreen reagent was diluted in 1× TE buffer (1:200, Fisher Scientific, USA) and then further mixed in equal amounts of lysate. The fluorescence intensity of the samples was measured using fluorescence microplate reader (FLX800, Biotek instruments, VT, USA) at 480 nm excitations and 520 nm emissions. The number of cells was obtained by using a standard curve relating fluorescent intensity with a known number of MSCs.
GAG Production
The presence of GAGs was measured using 1,9-dimethyl methylene blue (DMMB) assay at days 14 and 28. This assay is used to measure the amount of sulfated GAG as reported by Enobakhare et al.12 The papain digested samples used for the pico green assay also was used to detect the sulfated GAG in each sample using the DMMB assay. The values of the sulfated GAGs obtained in media and cells cultured on the scaffolds were added and then subtracted from the GAGs initially present in the scaffold before cell culture. Absorbances were measured at 595 nm using spectrophotometer (Emax, Molecular Devices, San Jose, CA). CS-A was used as a standard. N of 4 per group was used.
Collagens Type I and II Production
Samples were evaluated for the production of collagen types I and II using the ELISA method for human collagens type I and II at day 28 according to the manufacturer’s protocol (Chondrex). Collagen production was measured in the media and on the scaffolds. Briefly, collagen was solubilized from the scaffolds using pepsin digestion. This was followed by incubating the sample in an elastase solution until the sample was solubilized. The sample lysate was stored at − 20 °C until tested for ELISA. The ELISA plates were read using a spectrophotometer (Emax, Molecular Devices, San Jose, CA) at 490 nm. Each sample was run in triplicate. The ratio of Collagen type II to Collagen type I was also determined.
Gene Expression
Gene expression was determined using quantitative reverse transcriptase polymerase chain reaction (qRT-PCR), as previously described.16 The samples (n = 5 per group) were collected at days 4, 7, 14 and 28. Briefly, samples were lysed in RNeasy lysis (RLT) buffer (Qiagen, USA) using a soft tissue homogenizer (Cole Parmer, IL, USA). RNA was extracted from the tissue lysate using RNAeasy microkit (Qiagen, USA). The reaction was performed using One Step QuantiTect SYBR Green RT-PCR kit (Qiagen, USA) and gene specific Quantitech Assay primers (Qiagen, USA). The amount of RNA quantified per sample was 10 ng per reaction and each sample was assayed in triplicate. Real-Time instrument (Stratagene-Mx 3000P) was used to process and quantify the reaction. The values obtained were normalized to the housekeeping gene ribosomal protein, large, PO (RPLPO) in the same samples. The genes measured were matrix metalloproteinases (MMP2), sex-determining region Y- box9 (Sox9), Collagen type I (Col I), collagen type II (Col II), Aggrecan (Agg), Chondroadherin (CHAD), Collagen type X (Col X), vascular endothelial growth factor (VEGF). MMP2 was measured at days 4, 7 and 14 since it is expressed early and decreases as MSCs undergo chondrogenesis and is associated with matrix remodeling.3,7 The remaining genes were measured at days 7, 14, and 28. CHAD, VEGF and Col X are expressed at late stages of differentiation and were measured at days 14 and 28. VEGF and Col X are associated with hypertrophy.28,30,31
Confocal Microscopy for Cell Morphology and Immunostaining for Matrix Proteins
Samples were harvested at days 14 and 28 (n = 4 per group) and evaluated for cell morphology, distribution and the production of collagen II and aggrecan using immunofluorescence staining. The samples were fixed using 4% paraformaldehyde (PFA) for 20 min. This was followed by rinsing with PBS and incubating the samples with 0.1% Triton-X 100 for 15 min to permeabilize the cell membrane. The cultures were blocked using 5% donkey serum (host of the secondary antibody) for one hour. After blocking the samples, they were incubated with primary antibodies, monoclonal rabbit anti-human collagen type 2 and polyclonal rabbit anti-human aggrecan (1:500 dilution in 1% BSA) overnight at 4 °C. The samples were rinsed with PBS and then incubated with Alexa Fluor 488 conjugated donkey anti-rabbit immunoglobulin G (1:1000 dilution in 1% BSA) for an hour. The cytoskeleton was stained by incubating the samples with 1:250 dilution of rhodamine-conjugated phalloidin which binds to F-actin filament of the cytoskeleton. The nucleus was stained by 4′-6-diamidino-2-phenylindole (DAPI, Invitrogen, USA) prior to imaging. These samples were viewed using fluorescence confocal microscope (Nikon C1, USA) at × 20 magnification and images were rendered using the NIS Elements software (Nikon).
Statistical Analysis
Statistical analysis was performed using multi-factorial two-way analysis of variance (ANOVA) to determine significant differences between groups and time (p < 0.05). Shapiro Wilk test and Levene’s equal variance test was used to determine the normality. The multiple comparisons within groups were made using Tukey’s posthoc test (p < 0.05). All the statistical analysis was performed using GraphPad Prism (La Jolla, CA, USA) software. Graphs were plotted using either Microsoft excel, Origin or GraphPad Prism software. All values are reported as mean ± standard deviation.
Results
Scaffold Morphology
Scaffolds were characterized for their fiber morphology and inter-fiber spacing post cross-linking using SEM images (Fig. 2). The scaffolds retained their fibrous morphology post cross-linking. Table 1 summarizes the fiber diameter, inter-fiber spacing and porosity measurements for Gelatin as well as Gelatin and GAG containing scaffolds. The average fiber diameter for all the scaffolds was approximately 3 µm. There was no significant difference in fiber diameter between groups. The average inter-fiber spacing in all the groups was approximately 30 µm without any significant difference in between the groups. The average porosity of the scaffold was approximately 80%.
Scaffold Mechanical Properties
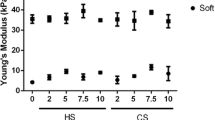
Mechanical properties of cross-linked Gelatin and Gelatin with GAGs are shown in Table 2. Gelatin showed the lowest tensile properties in comparison to the other scaffolds. No significant difference in elastic modulus was detected among the GAG containing gelatin scaffolds. No significant difference detected in compressive mechanical properties for all the scaffolds tested at 10% strain.
Determining the Presence and Distribution of Sulfated GAGs
FTIR was used to determine the presence of sulfated GAGs on the surface of the scaffolds. All electrospun and crosslinked gelatin scaffolds showed distinct amide I, II and III peaks at 1634 cm−1, 1528 cm−1 and 1238 cm−1 (Fig. S.1).44 Also, all gelatin scaffolds showed a distinct peak at 1449 cm−1 which is attributed to the presence of triple helical structure native to collagen.44 Gelatin scaffolds containing sulfated GAGs showed loss of minimum around 1222 cm−1- 1230 cm−1 suggesting the emergence of a sulfated peak. The presence of sulfated GAGs on the surface of the gelatin fiber was also detected using SEM–EDX elemental analysis. The scaffolds containing sulfated GAG and pSC showed the presence of a sulfur peak which was not visible on the gelatin scaffold (Fig. S.2).
Hydrolytic Stability
The initial swelling and change in dimension of electrospun gelatin scaffolds and gelatin scaffolds containing GAGs and pSC was evaluated by incubating scaffolds for 10 min at 37 °C in PBS. The change in swelling and dimension is reported in Fig. 3. A large change in dimension and swelling occurred for the scaffolds after immersion in PBS in comparison to the dry scaffolds. The Gelatin showed less swelling in comparison to Gel-CS-A, Gel-CS-C and Gel-pSC scaffolds. Among GAG containing scaffolds, Gel-CS-A had the lowest % swelling. No statistical differences in the change of dimension were detected for all scaffolds after 10 min in PBS.
(a) Percent swelling and (b) dimensional changes in gelatin scaffold (gelatin) and gelatin scaffolds containing CS-A (Gel-CS-A), CS-C (Gel-CS-C), pSC (Gel-pSC) from initial dry state incubated in PBS for 10 min at 37 °C. (Values are mean ± standard deviation, *Significant difference from CS-C and pSC (p < 0.05), **Significant difference from CS-A (p < 0.05)).
The change in swelling and dimension until day 28 was reported as fold change with respect to values obtained at 10 min of incubation in PBS (Fig. S.3). Significant differences were detected for swelling for Gelatin at day 28 in comparison to 6 h (Fig. S.3A). No differences in swelling were detected between GAGs and pSC containing groups for all time points. No differences were detected over 28 days for change in dimension for all scaffolds (Fig. S.3B). The release of the sulfated native GAGs and pSC from the gelatin scaffolds over 28 days was analyzed using DMMB assay. Approximately 20% of the total GAG was released from all three scaffolds by day 14 and remained unchanged by day 28.
Cell Growth
A significant increase in cell number was observed on gelatin and Gel-CS-A scaffolds from days 14 to 28 (Fig. 4a). No statistical differences were detected in cell number between all scaffold groups by day 28.
(a) Cell number on gelatin scaffolds and gelatin scaffolds containing native GAGs and pSC. (# significantly different from day 14 (p < 0.05)), (b) sulfated glycosaminoglycans produced per cell on gelatin scaffold and gelatin scaffold containing native GAGs and pSC. *Significantly greater than gelatin, gel-CS-A and gel-CS-C at day 14 (p < 0.05). **Significantly greater than gelatin (p < 0.05). #Significantly greater than gel-CS-A (p < 0.05).) (Values represent mean ± standard deviation).
Sulfated GAG Production
Cells on all scaffolds containing native GAGs had similar production of sulfated GAGs per cell (Fig. 4b). Highest production of sulfated GAG was observed for cells on Gel-pSC group at day 14 in comparison to cells on all other scaffolds. Also, cells on Gel-CS-C and Gel-pSC scaffolds had similar production of sulfated GAG which was higher than gelatin scaffolds at day 28. Cells on Gel-pSC scaffold produced higher sulfated GAG in comparison to Gel-CS-A scaffold at day 28.
Gene Expression
Expression of MMP2 was evaluated on days 4, 7 and 14. Expression of MMP2 was significantly higher on day 4 in comparison to day 14 for all scaffold groups (Fig. 5a). Cells on gelatin and pSC containing gelatin scaffolds showed higher expression of MMP2 at day 4 in comparison to CS-A and CS-C containing scaffold groups. Expression of Col I was evaluated on days 7, 14 and 28 (Fig. 5b). Highest expression of Col I was observed at day 28 for cells on Gel-CS-C scaffolds in comparison to Gel-CS-A scaffolds. Col I decreased by day 28 for cells on gelatin scaffolds containing CS-A. Whereas for cells on scaffolds containing CS-C, Col I significantly increased in comparison to days 7 and 14. Col I expression also significantly increased for cells on pSC containing scaffolds at day 28 with respect to day 7.
Gene expression for (a) MMP2 (**significantly different than CS-A and CS-C containing gelatin scaffold at time point (p < 0.05). aSignificantly different than day 4 (p < 0.05). bSignificantly different than day 7 (p < 0.05)), (b) collagen type I (Col I) (*significantly different from gelatin scaffolds containing CS-C, aSignificantly different than day 7, bSignificantly different than day 14 (p < 0.05)), (c) Sox9, (d) collagen type II (Col II), (e) Aggrecan (Agg), (f) chondroadherin (CHAD) (c–f) *Significantly higher than all the groups at time point (p < 0.05). #Significantly higher than gelatin and Gel-CS-A group at a time point (p < 0.05). a,b,cSignificantly different from day 7, 14 and 28, respectively (p < 0.05)), (g) collagen type X (Col X) (#Significantly higher than gelatin and gelatin scaffolds containing CS-C (p < 0.05)). (h) Vascular endothelial growth factor (VEGF) (#Significantly higher than gelatin and CS-A containing scaffolds (p < 0.05)) (g, h) *Significantly higher than all scaffolds, aSignificantly different than day 14 (p < 0.05)) (all values are normalized to RPLPO and represented as mean ± SD).
Expression of sox9 was evaluated at days 7, 14 and 28 (Fig. 5c). The expression of sox9 increased with time. The highest expression of sox9 was observed at day 28. Cells on pSC containing gelatin scaffolds had the highest expression of sox9 in comparison to all other scaffold groups. Cells on gelatin only scaffolds had the lowest expression of sox9 in comparison to all other scaffolds at day 28.
Expression of Col II and Agg was evaluated on days 7, 14 and 28. An increase in Col II gene expression was detected from days 7 to 28 for cells on gelatin scaffolds containing pSC (Fig. 5d). A decrease in Col II gene expression was detected at day 28 for cells on gelatin and gelatin scaffolds containing CS-A. Cells on gelatin scaffolds containing CS-C showed the highest expression of Col II gene at day 28 among the CS containing scaffold groups. The highest expression of Col II was observed at day 28 for cells on pSC containing gelatin scaffolds. Expression of Agg showed a similar trend as Col II (Fig. 5e). The highest expression was observed on pSC containing gelatin groups in comparison to all other scaffold groups at day 28. Expression of CHAD was evaluated on days 14 and 28 (Fig. 5f) The highest expression was seen for cells on pSC containing gelatin scaffolds for both days in comparison to cells cultured on gelatin and gelatin containing CS scaffolds.
Expression of hypertrophic markers Col X and VEGF were evaluated at days 14 and 28 (Figs. 5g and 5 h). Col X expression was highest for the pSC containing gelatin group at day 28. VEGF expression was also the highest for cells on pSC containing scaffolds at day 28. Among the native GAGs, CS-C containing group showed a high expression of VEGF as compared to gelatin and CS-A groups.
Cell Morphology and Extracellular Matrix Production
Intense actin staining was detected for cells on all scaffolds at day 14 and to a less extent by day 28. Collagen type II (Col II) and aggrecan (Agg) were examined by immunofluorescent staining at days 14 and 28 (Figs. 6 and 7). Cells on gelatin scaffolds containing CS-A, CS-C, and pSC had Col II and Agg present as early as day 14. A more intense staining of the cartilage matrix proteins was present for cells on CS-C and pSC containing groups at day 28. Cells on gelatin and the CS-A containing group appeared to have less staining for both proteins.
Collagens Type I and II Production
Production of collagens type I and II was quantified for cells on gelatin and gelatin scaffolds containing native GAGs and pSC at day 28 (Fig. 8). Highest production of collagen type II was detected for cells on gelatin scaffolds containing CS-C and pSC. Lowest collagen type II production was detected for cells on scaffolds containing gelatin and CS-A. For production of collagen type I, the highest was for cells on gelatin scaffolds and all CS containing gelatin scaffolds. Cells on gelatin scaffolds containing pSC showed the least production of collagen type I.
(a) Production of collagen types I and II for cells on gelatin and gelatin scaffolds containing chondroitin sulfates and pSC after 28 days culture in CCM+. (#Significantly higher Collagen I production than Gel-pSC, **Significantly higher collagen I than all the groups, *Significantly high collagen II than all the groups, aSignificantly different than collagen type I production (p < 0.05)), (b) ratio of collagen type II production to type I. (#Significantly higher than gelatin and Gel-CS-A, *significantly higher than all the groups (p < 0.05)) (values are mean ± SD).
Discussion
This study investigated MSC chondrogenesis on the scaffolds containing the GAG-mimetic pSC for its potential use in cartilage tissue regeneration by comparing its performance to commercially available native chondroitin sulfates, CS-A, and CS-C. pSC mimicked CS-C in terms of position and degree of sulfation where the sulfate group is predominantly on the 6-carbon position of the glucose moiety and CS-A has sulfate groups on the 4-carbon position of the monosaccharide unit.25 Both CS-C and CS-A are routinely investigated native GAGs for promoting chondrogenesis. This study demonstrated that the MSCs undergoing chondrogenesis had higher expression of chondrogenic gene expression and a more homogenous cartilage-like matrix with the highest ratio of collagens type II to I on gelatin scaffolds containing pSC in comparison to native GAGs.
All fibrous scaffolds had similar material behavior except for subtle changes in mechanical properties and swelling with the addition of the native GAGs or pSC. All gelatin containing scaffolds post crosslinking and hydration retained their fibrous morphology and showed micron-sized fiber diameters and interfiber spacing. The scaffolds also had a high porosity, which may be beneficial for chondrogenesis.37 The tensile mechanical properties of the scaffolds increased with the addition of both native CSs and pSCs in the gelatin scaffolds. This result is consistent with earlier reports showing the addition of chondroitin sulfate increases the mechanical properties of electrospun gelatin scaffolds.35,44 Yet, the compressive mechanical properties were similar amongst groups despite the presence of sulfated GAGs. FTIR characterization and SEM–EDX of the electrospun crosslinked gelatin scaffolds containing native GAGs and pSC confirmed the presence of sulfated groups which were absent in gelatin only scaffolds. The stability and swelling of the scaffold over 28 days was similar to that reported in previous studies.17 The CS and pSC containing gelatin scaffolds showed an increase in swelling in comparison to gelatin only scaffolds initially (within 10 min after immersion in PBS), but then stabilized long-term. All GAGs showed a gradual release of up to 20% from the scaffolds, which may be due to the extent of crosslinking, differences in molecular weight of the GAGs, and/or entrapment of the GAG. The release of GAGs from all the scaffolds was stabilized by day 14. Gelatin was used instead of collagen, to create electrospun fibrous scaffolds since it could be processed using non-harsh solvents such as water and ethanol. Electrospinning of collagen generally requires the use of harsh solvents, such as 2,2,2-trifluoroethanol (TFE), 1,1,1,3,3,3 hexafluoro-2-propanol (HFP) and trifluoracetic acid (TFA), which results in the denaturing of collagen and a decrease in water stability.38,42,47 EDC-NHS crosslinker has been commonly used for crosslinking proteins such as collagen, gelatin and improves mechanical properties as well as stability of the scaffold in aqueous conditions.16,18 This crosslinker is also non-cytotoxic allowing for cell attachment and proliferation.18
Chondrogenesis was promoted on pSC containing scaffolds with an early production of GAG and collagen type II with low amounts of collagen I, which indicates a more uniform cartilage-like matrix. Although pSC has a similar structure to CS-C, chondrogenesis was more favorable on the cellulose-derived GAG mimetic. GAGs are known to interact with bioactive molecules such as growth factors and cytokines. In this study, TGF-β3 was provided in the media to induce chondrogenic differentiation of MSCs. pSC is known to interact and bind TGF-β3 to a higher extent than gelatin only scaffolds.16 Also, degree of sulfation and sulfation pattern plays an important role in interaction of growth factors with GAGs resulting in the spatial availability of these growth factor for interaction with cell receptors. This results in a difference in cellular response.13,34 Our findings help support the important role of the sulfation pattern of GAGs in promoting chondrogenesis, where CS-A had less of an effect on chondrogenesis as compared to CS-C and pSC. This finding was comparable to earlier published results suggesting that the sulfation patterns of the GAGs play an important role in chondrogenesis.2,16,17,21
Gene expression for markers associated with chondrogenic differentiation also increased for cells on pSC containing scaffolds. MMP2, which is known to degrade gelatin and collagen type I33and is expressed during chondrogenic differentiation of mesenchymal stem cells,3 was expressed by cells on all scaffolds suggesting cells are promoting matrix remodeling and creating zones around the cells for accumulation of growth factors and deposition of synthesized matrix.7 Gelatin scaffolds containing pSC showed a reduction in MMP2 gene expression as the culture duration progressed. The expression of chondrogenic markers such as Sox9, Col II, Agg, were highest for cells on pSC containing gelatin scaffolds followed by cells on CS-C containing gelatin scaffolds at day 28. CS-A did not show enhanced expression of chondrogenic genes in comparison to CS-C and pSC containing scaffolds. Bovine derived CS-A is mostly CS-A but also contains CS-C.24,26 CS-C obtained from shark cartilage has CS-C, CS-A and CS-D in equivalent ratios.24,26 This heterogeneity in commercially available chondroitin sulfates may play a role in chondroinduction. In addition, the sulfate position in the native GAGs and pSC may affect chondrogenesis where the sulfate position for pSC is predominantly on the 6-carbon position, which is similar to CS-C. Whereas CS-A has a sulfate predominately on the 4-carbon position. The expression of hypertrophic factors Col X and VEGF was higher for cells cultured on the scaffolds containing pSC, which could be due to the presence of 10 ng/mL TGF-β3 in the media.27,29 Strategies utilizing growth factor dosing and/or combinations of growth factors may have to be implemented in order to reduce the expression of these markers leading to terminal differentiation.15,22,27,29
Conclusion
The gelatin scaffolds containing the cellulose derived GAG-mimetic promoted MSC chondrogenesis in culture conditions containing TGF-β. Commercially available chondroitin sulfates had less of an effect, which supports the need for GAG mimetics that can be synthesized and potentially tailored to improve biological function. Commercially available native GAGs are heterogeneous, which can have an effect on biological response. Constructs containing partially sulfated cellulose sulfate may be a viable approach for supporting chondrogenesis in the presence of growth factors and potentially for use in cartilage repair.
References
Anderson, R. A., K. Feathergill, X.-H. Diao, C. Chany, W. F. Rencher, L. J. D. Zaneveld, and D. P. Waller. Contraception by Ushercell™ (cellulose sulfate) in formulation: duration of effect and dose effectiveness. Contraception 70:415–422, 2004.
Antonio, J. D. S., B. M. Winston, and R. S. Tuan. Regulation of chondrogenesis by heparan sulfate and structurally related glycosaminoglycans. Dev. Biol. 123:17–24, 1987.
Arai, Y., S. Park, B. Choi, K.-W. Ko, W. Choi, J.-M. Lee, D.-W. Han, H.-K. Park, I. Han, J. Lee, and S.-H. Lee. Enhancement of matrix metalloproteinase-2 (MMP-2) as a potential chondrogenic marker during chondrogenic differentiation of human adipose-derived stem cells. International Journal of Molecular Sciences 17:963, 2016.
Bhosale, A. M., and J. B. Richardson. Articular cartilage: structure, injuries and review of management. British Medical Bulletin 87:77–95, 2008.
Brown, G. C., K. S. Lim, B. L. Farrugia, G. J. Hooper, and T. B. Woodfield. Fabrication of gelatin-heparin hydrogels with enhanced chondrogenic differentiation and tunable degradation. Front. Bioeng. Biotechnol., 2016. https://doi.org/10.3389/conf.fbioe.2016.01.00613.
Buckwalter, J. A., and H. J. Mankin. Articular cartilage: tissue design and chondrocyte-matrix interactions. Instructional Course Lectures 47:477–486, 1998.
Chameettachal, S., S. Midha, and S. Ghosh. Regulation of chondrogenesis and hypertrophy in silk fibroin-gelatin-based 3D bioprinted constructs. ACS Biomater. Sci. Eng. 2:1450–1463, 2016.
Chang, K.-Y., L.-W. Cheng, G.-H. Ho, Y.-P. Huang, and Y.-D. Lee. Fabrication and characterization of poly(γ-glutamic acid)-graft-chondroitin sulfate/polycaprolactone porous scaffolds for cartilage tissue engineering. Acta Biomater. 5:1937–1947, 2009.
Chen, J., Y. Wang, C. Chen, C. Lian, T. Zhou, B. Gao, Z. Wu, and C. Xu. Exogenous heparan sulfate enhances the TGF-β3-induced chondrogenesis in human mesenchymal stem cells by activating TGF-β/Smad signaling. Stem Cells Int. 2016:10, 2016.
Chen, F., S. Yu, B. Liu, Y. Ni, C. Yu, Y. Su, X. Zhu, X. Yu, Y. Zhou, and D. Yan. An injectable enzymatically crosslinked carboxymethylated pullulan/chondroitin sulfate hydrogel for cartilage tissue engineering. Sci. Rep. 6:20014, 2016.
Detterline, A. J., S. Goldberg, B. R. J. Bach, and B. J. Cole. Treatment options for articular cartilage defects of the knee. Orthop. Nurs. 24:361–366, 2005.
Enobakhare, B. O., D. L. Bader, and D. A. Lee. Quantification of sulfated glycosaminoglycans in chondrocyte/alginate cultures, by use of 1,9-dimethylmethylene blue. Anal. Biochem. 243:189–191, 1996.
Gama, C. I., S. E. Tully, N. Sotogaku, P. M. Clark, M. Rawat, N. Vaidehi, W. A. Goddard, A. Nishi, and L. C. Hsieh-Wilson. Sulfation patterns of glycosaminoglycans encode molecular recognition and activity. Nature Chemical Biology 2:467, 2006.
Groth, T., and W. Wagenknecht. Anticoagulant potential of regioselective derivatized cellulose. Biomaterials 22:2719–2729, 2001.
Hempel, U., V. Hintze, S. Möller, M. Schnabelrauch, D. Scharnweber, and P. Dieter. Artificial extracellular matrices composed of collagen I and sulfated hyaluronan with adsorbed transforming growth factor β1 promote collagen synthesis of human mesenchymal stromal cells. Acta Biomater. 8:659–666, 2012.
Huang, G. P., R. Menezes, R. Vincent, W. Hammond, L. Rizio, G. Collins, and T. L. Arinzeh. Gelatin scaffolds containing partially sulfated cellulose promote mesenchymal stem cell chondrogenesis. Tissue Eng. A 23:1011–1021, 2017.
Huang, G. P., A. Molina, N. Tran, G. Collins, and T. L. Arinzeh. Investigating cellulose derived glycosaminoglycan mimetic scaffolds for cartilage tissue engineering applications. J. Tissue Eng. Regen. Med. 12:e592–e603, 2018.
Huang, G. P., S. Shanmugasundaram, P. Masih, D. Pandya, S. Amara, G. Collins, and T. L. Arinzeh. An investigation of common crosslinking agents on the stability of electrospun collagen scaffolds. J. Biomed. Mater. Res. A 103:762–771, 2015.
Huang, Z.-M., Y. Z. Zhang, S. Ramakrishna, and C. T. Lim. Electrospinning and mechanical characterization of gelatin nanofibers. Polymer 45:5361–5368, 2004.
Jaiswal, N., S. E. Haynesworth, A. I. Caplan, and S. P. Bruder. Osteogenic differentiation of purified culture-expanded human mesenchymal stem cells in vitro. J. Cell. Biochem. 64:295–312, 1997.
Kawamura, D., T. Funakoshi, S. Mizumoto, K. Sugahara, and N. Iwasaki. Sulfation patterns of exogenous chondroitin sulfate affect chondrogenic differentiation of ATDC5 cells. J. Orthop. Sci. 19:1028–1035, 2014.
Kim, M., I. E. Erickson, M. Choudhury, N. Pleshko, and R. L. Mauck. Transient exposure to TGF-β3 improves the functional chondrogenesis of msc-laden hyaluronic acid hydrogels. J. Mech. Behav. Biomed. Mater. 11:92–101, 2012.
Levett, P. A., F. P. W. Melchels, K. Schrobback, D. W. Hutmacher, J. Malda, and T. J. Klein. A biomimetic extracellular matrix for cartilage tissue engineering centered on photocurable gelatin, hyaluronic acid and chondroitin sulfate. Acta Biomater. 10:214–223, 2014.
McCarthy, B. Antivirals—an increasingly healthy investment. Nat. Biotechnol. 25:1390, 2007.
Menezes, R., S. Hashemi, R. Vincent, G. Collins, J. Meyer, M. Foston, and T. L. Arinzeh. Investigation of glycosaminoglycan mimetic scaffolds for neurite growth. Acta Biomater. 90:169–178, 2019.
Mucci, A., L. Schenetti, and N. Volpi. 1H and 13C nuclear magnetic resonance identification and characterization of components of chondroitin sulfates of various origin. Carbohydr. Polym. 41:37–45, 2000.
Mueller, M. B., M. Fischer, J. Zellner, A. Berner, T. Dienstknecht, L. Prantl, R. Kujat, M. Nerlich, R. S. Tuan, and P. Angele. Hypertrophy in mesenchymal stem cell chondrogenesis: effect of TGF-β isoforms and chondrogenic conditioning. Cells Tissues Organs 192:158–166, 2010.
Mueller, M. B., and R. S. Tuan. Functional characterization of hypertrophy in chondrogenesis of human mesenchymal stem cells. Arthritis Rheum. 58:1377–1388, 2008.
Nazempour, A., and B. J. Van Wie. Chondrocytes, mesenchymal stem cells, and their combination in articular cartilage regenerative medicine. Ann. Biomed. Eng. 44:1325–1354, 2016.
Petersen, W., M. Tsokos, and T. Pufe. Expression of VEGF121 and VEGF165 in hypertrophic chondrocytes of the human growth plate and epiphyseal cartilage. J. Anat. 201:153–157, 2002.
Pfander, D., D. Kortje, R. Zimmermann, G. Weseloh, T. Kirsch, M. Gesslein, T. Cramer, and B. Swoboda. Vascular endothelial growth factor in articular cartilage of healthy and osteoarthritic human knee joints. Ann. Rheum. Dis. 60:1070–1073, 2001.
Portocarrero, G., G. Collins, and T. Livingston Arinzeh. Challenges in cartilage tissue engineering. J. Tissue Sci. Eng. 4:120, 2013.
Rastogi, A., H. Kim, J. D. Twomey, and A. H. Hsieh. MMP-2 mediates local degradation and remodeling of collagen by annulus fibrosus cells of the intervertebral disc. Arthritis Res. Therapy 15:R57–R57, 2013.
Robinson, D. E., D. J. Buttle, R. D. Short, S. L. McArthur, D. A. Steele, and J. D. Whittle. Glycosaminoglycan (GAG) binding surfaces for characterizing GAG-protein interactions. Biomaterials 33:1007–1016, 2012.
Saporito, F., G. Sandri, M. C. Bonferoni, S. Rossi, L. Malavasi, C. D. Fante, B. Vigani, L. Black, and F. Ferrari. Electrospun gelatin-chondroitin sulfate scaffolds loaded with platelet lysate promote immature cardiomyocyte proliferation. Polymers 10:208, 2018.
Schaffellner, S., V. Stadlbauer, P. Stiegler, O. Hauser, G. Halwachs, C. Lackner, F. Iberer, and K. H. Tscheliessnigg. Porcine islet cells microencapsulated in sodium cellulose sulfate. Transplant. Proc. 37:248–252, 2005.
Shanmugasundaram, S., H. Chaudhry, and T. L. Arinzeh. Microscale versus nanoscale scaffold architecture for mesenchymal stem cell chondrogenesis. Tissue Eng. A 17:831–840, 2010.
Skotak, M., S. Noriega, G. Larsen, and A. Subramanian. Electrospun cross-linked gelatin fibers with controlled diameter: the effect of matrix stiffness on proliferative and biosynthetic activity of chondrocytes cultured in vitro. J. Biomed. Mater. Res. A 95A:828–836, 2010.
Sophia-Fox, A. J., A. Bedi, and S. A. Rodeo. The basic science of articular cartilage: structure, composition, and function. Sports Health 1:461–468, 2009.
Stone, A. Microbicides: a new approach to preventing HIV and other sexually transmitted infections. Nat. Rev. Drug Discov. 1:977, 2002.
Temenoff, J. S., and A. G. Mikos. Review: tissue engineering for regeneration of articular cartilage. Biomaterials 21:431–440, 2000.
Ting, L., T. W. Keng, B. P. Chew, and C. S. Yian. Photochemical crosslinked electrospun collagen nanofibers: synthesis, characterization and neural stem cell interactions. J. Biomed. Mater. Res. A 95A:276–282, 2010.
Varghese, S., N. S. Hwang, A. C. Canver, P. Theprungsirikul, D. W. Lin, and J. Elisseeff. Chondroitin sulfate based niches for chondrogenic differentiation of mesenchymal stem cells. Matrix Biology 27:12–21, 2008.
Wang, H., Y. Feng, Z. Fang, R. Xiao, W. Yuan, and M. Khan. Fabrication and characterization of electrospun gelatin-heparin nanofibers as vascular tissue engineering. Macromolecular Research 21:860–869, 2013.
Wirth, C. J., and M. Rudert. Techniques of cartilage growth enhancement: a review of the literature. Arthroscopy 12:300–308, 1996.
Yoo, H. S., E. A. Lee, J. J. Yoon, and T. G. Park. Hyaluronic acid modified biodegradable scaffolds for cartilage tissue engineering. Biomaterials 26:1925–1933, 2005.
Zheng, W., W. Zhang, and X. Jiang. Biomimetic collagen nanofibrous materials for bone tissue engineering. Advanced Engineering Materials 12:B451–B466, 2010.
Acknowledgments
We would like to thank support from Musculoskeletal Transplant Foundation and the National Science Foundation #1207173.
Author information
Authors and Affiliations
Corresponding author
Additional information
Associate Editor Jennifer West oversaw the review of this article.
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Electronic supplementary material
Below is the link to the electronic supplementary material.
Rights and permissions
About this article
Cite this article
Menezes, R., Arinzeh, T.L. Comparative Study of Electrospun Scaffolds Containing Native GAGs and a GAG Mimetic for Human Mesenchymal Stem Cell Chondrogenesis. Ann Biomed Eng 48, 2040–2052 (2020). https://doi.org/10.1007/s10439-020-02499-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10439-020-02499-9