Abstract
It is important for the elderly to maintain their skeletal muscle mass, which in turn helps to maintain physical functions. This study aimed to clarify factors related to skeletal muscle mass maintenance. Home-bound elderly (94 men and 216 women), at least 75 years of age, attending a day-care center in Tokyo, were enrolled in this study. Dentists specializing in dysphagia rehabilitation evaluated skeletal muscle mass, occlusal status and swallowing function. Physical function, cognitive function and nutritional status were also evaluated by interviewing caregivers. Correlations of skeletal muscle mass with various factors were determined in each gender group. Multiple regression analysis revealed that skeletal muscle mass was significantly related to nutritional status in both men and women. In men, there was a significant difference in skeletal muscle mass between those with and without occlusion of the natural teeth. Our results suggest that dental treatments and dentures would be useful for maintaining skeletal muscle mass, especially in men.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Decreased skeletal muscle mass with aging may reduce quality of life for the elderly. It is important for the elderly to maintain skeletal muscle mass, which in turn helps to maintain physical functions [1]. “Frailty”, a concept which describes physical disabilities in the elderly, is defined as “a state of increased vulnerability to various health impairments based on various decreased physical functions associated with aging”. When elderly people become frail, their activities of daily living (ADL) may be impaired, making them more likely to require nursing care. Sarcopenia, defined as a loss of whole-body muscle mass associated with aging, is one of the factors contributing to acceleration of frailty, and is reportedly associated with conditions such as malnutrition and disuse syndrome [2]. Declines in muscle mass and strength are expected features of aging, but there is significant variability among individuals in the rates of loss. Although some of these differences can be explained by fixed factors, such as gender, much of the remaining variation remains unexplained.
Oropharyngeal function is extremely important for the adequate nutritional intake needed to prevent frailty and sarcopenia. Many studies have demonstrated the relationship between nutritional status and oral functions, such as the number of remaining teeth, occlusal support and denture use [3–5]. We previously reported that elderly people receiving home care without occlusal support in the molar region were found to have decreased swallowing function and poor nutritional status [6, 7]. However, whether reduced oral function is a cause of malnutrition, resulting in sarcopenia, is still a subject of debate.
To elucidate the relationship between oral status and skeletal muscle mass, not only nutritional status, but also other factors, such as age, general condition and the capability of subjects to perform ADL, must be taken into consideration. This study was designed to examine oral status, eating and swallowing functions and feeding status, as well as to clarify the factors associated with skeletal muscle mass maintenance in the frail elderly.
Methods
Subjects
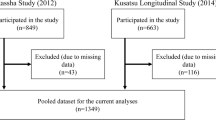
The subjects were enrolled at an outpatient long-term day care center in the Tokyo metropolitan which provides bathing, bodily waste elimination, meals and other forms of daily activity care during daytime hours on weekdays. Three hundred and twelve subjects, at least 75 years of age, agreed to participate and written informed consent was obtained from these subjects or family members. This study was approved by the Ethics Committee of The Nippon Dental University. (NDU-T2012-14).
Measurements
Five dentists specializing in dysphasia rehabilitation visited the subjects attending the long-term day care center and evaluated skeletal muscle mass, occlusal status and swallowing function. The following factors associated with skeletal muscle mass were evaluated by interviewing caregivers: physical function as represented by the Barthel Index (BI), cognitive function as represented by the cognitive dementia rating (CDR), nutritional status as represented by the body mass index (BMI) and the Mini Nutritional Assessment-Short Form (MNA-SF).
Skeletal muscle mass
InBody S10 (Biospace Co. Ltd., Tokyo) was used for all measurements. This instrument is equipped for performance of the bioelectrical impedance analysis (BIA) method with eight-point electrodes [8]. In our study, skeletal muscle mass was calculated employing the equation originally used by Janssen et al. [1]. This equation is designed to calculate skeletal muscle mass using the resistance value (R) at 50 kHz measured by InBody S10.
where “Ht” is height; for “sex”, men = 1 and women = 0).
Oral status
Oral status was evaluated by determining whether occlusion of the molar region was maintained with natural teeth. When the molar occlusion on either side was maintained with natural teeth, the subjects were classified into the natural teeth occlusion group and all others were classified into the no natural teeth occlusion group.
Swallowing function
Cervical auscultation was used to evaluate swallowing function [9]. Cervical auscultation is a method employed for dysphagia screening. The individual performing the evaluations in the present study had more than 3 years of experience with this method and calibration was carried out prior to the measurements. The subjects were asked to drink 3 ml of water, and respiratory sounds after swallowing were examined. Any subjects with choking, labored breathing and/or wheezing after swallowing were regarded as having possible dysphagia [10].
Physical function
The BI was used to evaluate physical function [11]. This index is frequently used to evaluate ADL. People with a BI score of 60 and greater are considered to be able to perform basic daily activities independently] [12]. In this study, the subjects were divided into the maintained ADL group with BI scores of 60 and greater and the low ADL group with BI scores of less than 60.
Cognitive function
The CDR was used to evaluate cognitive function [13]. The CDR is a five-stage rating scale which is widely used for the diagnosis of dementia. The subjects with scores of 0 (no cognitive impairment) and 0.5 (very mild cognitive impairment) were classified as the maintained cognitive function group and those with scores of 1 (mild cognitive impairment), 2 (moderate cognitive impairment) and 3 (severe cognitive impairment) as the cognitive impairment group.
Nutritional status
The MNA-SF was used to assess nutritional status [14]. The MNA-SF is a tool for evaluating the nutritional status of those 65 years of age and older. It provides a guide, allowing caregivers to check or record relevant information in the medical record. The subjects were divided into the good nutritional status group with MNA-SF scores of 12–14, and the poor nutritional status group with scores of less than 12.
Though BMI is one of the items included in the MNA-SF, this parameter was also used independently to evaluate the nutritional status of our subjects. The subjects were divided into the maintained and decreased body weight groups with BMI of at least 18.5 and of less than 18.5, respectively.
Statistical analysis
Skeletal muscle mass as well as related items were compared between the sexes with the Chi-squared test and the Wilcoxon signed rank test. Multiple regression analysis was used to identify the factors closely related to skeletal muscle mass for each male and female subject. PASW statistics 22 software (IBM, Tokyo) was used for all statistical analyses and the level of statistical significance was set at p < 0.05.
Results
The subjects consisted of 94 men (mean age: 83.3 ± 5.4 years) and 216 women (mean age 86.4 ± 5.0 years). Significant differences in skeletal muscle mass were observed between male and female subjects (men: 13.1 ± 1.9, women: 6.4 ± 1.4, p < 0.001) (Table 1). Therefore, the following analyses involving the comparisons of skeletal muscle mass and other items were conducted separately for men and women, considering the age effect.
In men, there was a significant difference in skeletal muscle mass between those with and without natural teeth occlusion (p = 0.024), between the MNA-SF groups (p = 0.031) and between those with and without dysphagia (p = 0.024) (Table 2).
In women, there was a significant difference in skeletal muscle mass between the MNA-SF groups (p = 0.001), the BI groups (p = 0.023) and the BMI groups (p = 0.002) (Table 3).
Multiple regression analysis revealed that skeletal muscle mass was significantly related to the presence versus absence of natural teeth occlusion and with high MNA-SF in men, as well as in women (Tables 4, 5).
Discussion
The results of this study suggest that different approaches are needed for men and women to achieve the goal of maintaining skeletal muscle mass.
In this study, we used the BIA method to measure skeletal muscle mass and calculated this value with Janssen’s equation which is widely used for determining skeletal muscle mass. Dual energy X-ray absorptiometry (DXA) has long been recommended worldwide for the measurement of skeletal muscle mass. However, since DXA is sensitive to water and, strictly speaking, estimates the fat-free mass, some investigators have pointed out that it may not be an appropriate method of evaluating skeletal muscle mass in the elderly [15–17]. In addition, the DXA scan is a rather large instrument, and only those who are able to come to a DXA facility can undergo measurement. In contrast, the BIA instrument is portable and can be taken to subjects’ homes and nursing homes. Therefore, even the elderly with reduced ADL can undergo BIA measurements. However, BIA has one disadvantage. The equation used for skeletal muscle mass calculation is in a black box and differs depending on the instrument model. Therefore, caution is essential when we directly use the skeletal muscle mass values measured employing different types of instruments. Considering this potential shortcoming, we decided to calculate the skeletal muscle mass ourselves using Janssen’s equation obtained from impedance values at 50 kHz. Although there is a report indicating that this method of calculation may lack accuracy in Asian populations [18], we used it because we believe it to be the best among the existing methods of calculating skeletal muscle mass.
It is not surprising that in both men and women, skeletal muscle mass differed significantly between the two MNA-SF groups. Many previous studies have demonstrated nutritional status to be related to skeletal muscle mass [19, 20]. However, in the present study, we found that natural teeth occlusion affected skeletal muscle mass only in men. Tominaga et al. investigated the relationship between the ability of the elderly living in the community to prepare meals independently and masticatory function or nutritional status [21]. They reported that the elderly who answered that they cooked regularly showed no significant relationship between MNA-SF and masticatory function. On the other hand, those who responded that they did not cook on a daily basis showed a significant relationship between MNA-SF and masticatory function. This observation may indicate that those who could cook their own meals were able to prepare foods with easy-to-eat textures. Usually, men do not usually prepare meals on their own. In our study, 93.2 % of male subjects ate meals provided by their families or a meal delivery service. This is a possible reason for only the men in our study being at risk of skeletal muscle loss in association with loss of dental occlusion.
Our results raise the possibility that if the necessary nutrition is served in the form of foods with an easy-to-eat texture, malnutrition can be prevented even when oral function has deteriorated. Furthermore, dental treatments and dentures would be useful for maintaining skeletal muscle mass, especially in men. However, since this was a cross-sectional study, it is difficult to identify any possible causal relationships. Further well-designed intervention studies, involving both men and women, will be needed to confirm the utility of this approach for preventing sarcopenia and frailty.
References
Janssen I. Influence of sarcopenia on the development of physical disability: the cardiovascular health study. J Am Geriatr Soc. 2006;54:56–62.
Cruz-Jentoft AJ, Baeyens JP, Bauer JM, Boirie Y, Cederholm T, Landi F, Martin FC, Michel JP, Rolland Y, Schneider SM, Topinková E, Vandewoude M, Zamboni M. European Working Group on Sarcopenia in Older People. Sarcopenia: European consensus on definition and diagnosis: Report of the European Working Group on Sarcopenia in Older People. Age Ageing. 2010;39:412–23.
Nowjack-Raymer RE, Sheiham A. Association of edentulism and diet and nutrition in US adults. J Dent Res. 2003;82:123–6.
Yoshida M, Suzuki R, Kikutani T. Nutrition and oral status in elderly people. Jpn Dent Sci Rev. 2014;50:9–14.
Sahyoun NR, Lin CL, Krall E. Nutritional status of the older adult is associated with dentition status. J Am Diet Assoc. 2003;103:61–6.
Yoshida M, Kikutani T, Yoshikawa M, Tsuga K, Kimura M, Akagawa Y. Correlation between dental and nutritional status in community-dwelling elderly Japanese. Geriatr Gerontol Int. 2011;11:315–9.
Kikutani T, Yoshida M, Enoki H, Yamashita Y, Akifusa S, Shimazaki Y, Hirano H, Tamura F. Relationship between nutrition status and dental occlusion in community-dwelling frail elderly people. Geriatr Gerontol Int. 2013;13:50–4.
Ishii S, Tanaka T, Shibasaki K, Ouchi Y, Kikutani T, Higashiguchi T, Obuchi SP, Ishikawa-Takata K, Hirano H, Kawai H, Tsuji T, Iijima K. Development of a simple screening test for sarcopenia in older adults. Geriatr Gerontol Int. 2014;14:93–101.
Zenner PM, Losinski DS, Mills RH. Using cervical auscultation in the clinical dysphagia examination in long-term care. Dysphagia. 1995;10:27–31.
Sudo E, Tanuma S, Sudo E, Takahashi Y, Yoshida A, Kobayashi C, Ohama Y. The usefulness of the water swallowing test and videofluorography in swallowing rehabilitation in patients with cerebrovascular disease. Nihon Ronen Igakkai Zasshi. 2002;39:427–32 (in Japanese).
Collin C, Wade DT, Davies S, Horne V. The Barthel ADL Index: a reliability study. Int Disabil Stud. 1988;10: 61–3.
Granger CV, Albrecht GL, Hamilton BB. Outcome of comprehensive medical rehabilitation: measurement by PULSES profile and the Barthel Index. Arch Phys Med Rehabil. 1979;60:145–54.
Burke WJ, Miller JP, Rubin EH, Morris JC, Coben LA, Duchek J, Wittels IG, Berg L. Reliability of the Washington University Clinical Dementia Rating. Arch Neurol. 1988;45:31–2.
Rubenstein LZ, Harker JO, Salvà A, Guigoz Y, Vellas B. Screening for undernutrition in geriatric practice: developing the short-form mini-nutritional assessment (MNA-SF). J Gerontol A Biol Sci Med Sci. 2001;56:M366–72.
Proctor DN, O’Brien PC, Atkinson EJ Nair KS. Comparison of techniques to estimate total body skeletal muscle mass in people of different age groups. Am J Physiol. 1999; 277:E489–95.
Yamada Y, Masuo Y, Yokoyama K, Hashii Y, Ando S, Okayama Y, Morimoto T, Kimura M, Oda S. Proximal electrode placement improves the estimation of body composition in obese and lean elderly during segmental bioelectrical impedance analysis. Eur J Appl Physiol. 2009;107:135–44.
Yamada Y, Matsuda K, Björkman MP, Kimura M. Application of segmental bioelectrical impedance spectroscopy to the assessment of skeletal muscle cell mass in elderly men. Geriatr Gerontol Int. 2014;14:129–34.
Janssen I, Heymsfield SB, Baumgartner RN, Ross R. Estimation of skeletal muscle mass by bioelectrical impedance analysis. J Appl Physiol. 2000;89:465–71.
Houston DK, Nicklas BJ, Ding J, Harris TB, Tylavsky FA, Newman AB, Lee JS, Sahyoun NR, Visser M, Kritchevsky SB. Dietary protein intake is associated with lean mass change in older, community-dwelling adults: the Health, Aging, and Body Composition (Health ABC) Study. Am J Clin Nutr. 2008;87:150–5.
Bahat G, Saka B, Tufan F, Akin S, Sivrikaya S, Yucel N, Erten N, Karan MA. Prevalence of sarcopenia and its association with functional and nutritional status among male residents in a nursing home in Turkey. Aging Male. 2010;13:211–4.
Tominaga K, Ando Y. The relationship between nutritional intake and mastication based on elderly people’s practice of preparing meals. J Dent Hlth. 2013;63:328–36 (in Japanese with English abstract).
Acknowledgments
This study was supported by a Grant-in-Aid for Scientific Research for Comprehensive Research on Aging and Health (Research on Dysphagia and Nutritional Disorders of the Elderly Living in the Community or at Home) from the Ministry of Health, Labor and Welfare.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of Interest
The authors declare that they have no conflict of interest.
Rights and permissions
About this article
Cite this article
Sagawa, K., Kikutani, T., Tamura, F. et al. Factors related to skeletal muscle mass in the frail elderly. Odontology 105, 91–95 (2017). https://doi.org/10.1007/s10266-015-0231-4
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10266-015-0231-4