Abstract
Cardiovascular disease (CVD) is a major complication of systemic lupus erythematosus (SLE) and is now a leading cause of death for these patients. In this study, 23 SLE patients asymptomatic for CVD underwent a comprehensive echocardiographic examination to detect subclinical cardiac involvement. According to their SELENA-SLEDAI score, they were divided into two groups: SELENA-SLEDAI ≤ 12 (n = 13, 12 females) and SELENA-SLEDAI > 12 (n = 10, all females), indicative of mild-to-moderate and severe SLE, respectively. Patients in the latter group had significant increases in left ventricular (LV) mass, LV end-diastolic volume, left atrial volume and right heart parameters (pulmonary arterial pressure, tricuspid regurgitation velocity and diameter of the inferior cava) compared to the mild-to-moderate group. Alterations of the early to late diastolic trans-mitral flow velocity (E/A) were found in 39% of patients, equally distributed between the two groups. The Framingham score of all patients correlated directly with LV mass, interventricular septum thickness and posterior wall thickness, but did not significantly differ between patients with severe and mild-to-moderate SLE. These findings reveal the presence of early-stage, and thus clinically silent, diastolic dysfunction in patients with severe SLE. They demonstrate the poor predictive value of the Framingham score in CVD risk stratification of patients with SLE, thus highlighting the crucial role of echocardiography in the diagnostic workup of these patients.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Systemic lupus erythematosus (SLE) is a chronic and multifaceted autoimmune disease that mostly affects young women [1]. Although the survival of SLE patients has remarkably improved in the last years, cardiovascular disease (CVD) is being diagnosed with increasing frequency and is currently detected in up to 50% of SLE patients. All cardiac structures may be involved, including the pericardium, endocardium, myocardium, coronary arteries and conductive tissue [2]. Compared to the general population, SLE patients have a two- to ninefold higher risk of cardiovascular events, such as myocardial infarction, stroke and heart failure [3,4,5]. The mechanisms underlying CVD in SLE are multifactorial and still not well understood. Traditional risk factors, such as hypertension, smoking, sedentary lifestyle and elevated lipid levels, do not fully explain the higher risk of CVD in SLE, and SLE itself is an independent risk factor for CVD [6]. SLE-specific factors that play an additional role include disease activity, persistence of systemic and local inflammation, immune abnormalities, anti-phospholipid antibodies (anti-cardiolipin and anti-β2-glycoprotein-I) and potential adverse effects of therapies, especially glucocorticoids (GCs) and nonsteroidal anti-inflammatory drugs [7,8,9,10,11,12,13,14,15].
Given this complex interplay between traditional and SLE-specific risk factors, standard risk calculators such as the Framingham equations, the Atherosclerotic Cardiovascular Disease Risk Algorithm (ASCVD), and Systematic Coronary Risk evaluation (SCORE) underestimate the risk of CVD in the context of SLE [16, 17]. Cardiac abnormalities, especially left ventricular (LV) diastolic dysfunction, are common and persistent findings in SLE patients and may be the only manifestation of cardiac involvement preceding global systolic dysfunction [18].
In this study, we examined the echocardiographic parameters in SLE patients to assess the CVD risk. Our results point to an increased LV mass and left atrial (LA) volume as early markers of diastolic dysfunction in SLE patients.
Materials and methods
Patients
Twenty-three SLE patients attending our Internal Medicine unit from January to December 2017 were included in the study. All patients fulfilled the American College of Rheumatology’s diagnostic criteria for SLE [19]. Patients completed a questionnaire and underwent a comprehensive physical examination. Blood samples obtained from all patients were analyzed for the following: complete blood count, low-/high-density lipoproteins, triglycerides and anti-double-stranded DNA (anti-dsDNA) antibodies. Additional laboratory tests included erythrocyte sedimentation rate, C-reactive protein level, estimated glomerular filtration rate, as well as uric acid and complement (C3, C4) levels. The Safety of Estrogens in Lupus Erythematosus National Assessment (SELENA) version of the SLE Disease Activity Index (SLEDAI) score [20] was adopted to determine SLE disease activity. All patients were evaluated by standard trans-thoracic echocardiography. Demographic characteristics as well as clinical and laboratory findings were recorded. Patients with any congenital or acquired CVD event, any systemic disease (endocrine, metabolic or infectious), hypertension, diabetes mellitus, chronic kidney diseases or chest disease were excluded. All patients provided written informed consent. The study protocol was approved by the Ethics Committee of the University of Bari Medical School and conformed to the good clinical practice guidelines of the Italian Ministry of Health and the ethical guidelines of the Declaration of Helsinki, as revised and amended in 2004.
Echocardiography
All echocardiographic measurements were assessed using an Esaote ultrasound machine (MyLab™Seven) with a 2.5-MHz electronic transducer. The patients were examined in the left lateral decubitus position.
From the parasternal log-axis view, B-mode and M-mode echocardiography was used to obtain end-diastole measurements of interventricular septum thickness, LV posterior wall thickness, and interior LV diameter (Fig. 1a, b). LV mass was determined using the Devereux and Reichek “cube” formula [21]. Relative wall thickness was calculated using an internationally validated formula [22]. An apical four-chamber (A4C) view was used to evaluate the tricuspid annular plane systolic excursion, right atrial area, LV end-diastolic volume, LV ejection fraction, and LA volume (Fig. 1c–f). A subcostal view was used to measure the diameter of the inferior vena cava (IVC). Aortic root diameter (Ao) and Doppler measurements were obtained using B-mode echocardiography and a parasternal log-axis view. Ao, LA volume and LV mass were indexed to body surface area (LAVi and LVMi) or height2.7. (LAVh2.7 and LVMh2.7) End-diastolic (AoD) and end-systolic (AoS) aortic root diameters were also measured in the M-mode parasternal long axis view to determine the aortic stiffness index (ASI) according to the following equation: log (systolic blood pressure/diastolic blood pressure)/(AoS–AoD)/AoD [23]. Tricuspid regurgitation velocity (TRV) was estimated by measuring the maximum velocity of the regurgitation jet using continuous-wave Doppler and an A4C view (Fig. 2a). The peak value was then used to calculate the pressure difference between the right ventricle and right atrium according to the simplified Bernoulli equation (P = 4[TRVmax]2). The estimated TRV was then used to estimate pulmonary arterial pressure as a derivative sum with the right atrial filling pressure (estimated based on the size and respiratory collapsibility of the IVC during normal respiration) and the tricuspid regurgitation pressure. Pulsed-wave Doppler was used to detect the peak velocity during early (E) and late (A) diastole (Fig. 2b). The septal velocity (e′) was measured using tissue Doppler (Fig. 2c) or pulsed-wave Doppler (Fig. 2d) imaging. Diastolic dysfunction was diagnosed as an E/A ratio < 1 or > 2 and/or an E/e′ ratio > 15.
Echocardiographic morphological parameters. End-diastolic measurements of interventricular septum thickness (IVS), left ventricular posterior wall thickness (PWt) and interior left ventricular diameter (LVD) from the parasternal log-axis view in a B-mode and b M-mode echocardiography. The area and volume of the atria and ventricles were calculated from an apical four-chamber (A4C) view in two representative patients from the mild-to-moderate group (e, f) and two from the severe group (c, d)
Statistical analysis
All statistical analyses were carried out using the Prism program (GraphPad Software). The distribution of dichotomous values was analyzed using a Chi-square test. Non-normally distributed data were analyzed using nonparametric statistics. The Mann–Whitney test was used for comparisons of groups and the Spearman rank test for correlations. Normally distributed data were analyzed using parametric statistics; group comparisons were carried out using unpaired t tests. P values are shown only for comparisons in which the differences were statistically significant, defined as P values < 0.05.
Results
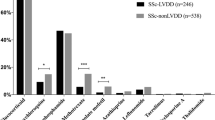
The demographic and clinical characteristics of the study patients are summarized in Table 1. The 22 female patients (96%) and 1 male patient (4%) had a mean age of 43.7 ± 11.9 years and a disease duration of 8.9 ± 10.4 years. At the time of analysis, 65.2% of the patients were being treated with GCs; the mean daily oral dose of prednisone or prednisone equivalent was 9.2 ± 4.2 mg/day. In addition, 39.1% of patients were being treated with disease-modifying antirheumatic drugs, including methotrexate, sulfasalazine and leflunomide; 21.7% with antimalarials; 13% with mycophenolate mofetil; and 17.4% with belimumab. An additional subgroup of 26.1% patients was not receiving treatment at the time of the study. All patients had a normal body mass index and body surface area. Systolic and diastolic blood pressures were also normal. All patients were negative for lupus anticoagulant or anti-phospholipid antibody syndrome, none were diabetic, and four were smokers.
Based on the SELENA-SLEDAI score, the patients were grouped into two groups, SELENA-SLEDAI ≤ 12 and SELENA-SLEDAI > 12, corresponding to mild-to-moderate and severe disease, respectively [24]. The 12 females and 1 male in the mild-to-moderate group had a mean age of 44.36 ± 14.40 years. All 10 patients in the severe group were female; their mean age was 41.75 ± 8.57 years (Table 2).
A comparison of the clinical and laboratory parameters of the two groups showed a significantly higher mean SELENA-SLEDAI score (5.5 ± 3.1 vs. 20.4 ± 8.8; P < 0.0001) and mean anti-dsDNA antibody titer (39.5 ± 21.1 vs. 838.0 ± 523.8; P = 0.03) in the severe than in the mild-to-moderate group. Patients with severe disease also had significantly lower mean serum C3 (0.99 ± 0.45 vs. 0.60 ± 0.35, P = 0.04) and C4 (0.21 ± 0.1 vs. 0.10 ± 0.07; P = 0.006) levels. The mean values of all other parameters did not significantly differ between the two groups (Table 2).
There were no significant differences between the two groups with respect to traditional CVD risk factors such as the Framingham score, including any of its components [age, sex, presence of hypertension, smoking habit, total cholesterol, low-density lipoproteins, systolic blood pressure]. The differences in the high-density lipoprotein level, uric acid level, and diastolic blood pressure were also not significant (Table 3). However, the mean triglyceride level (122.0 ± 33.2 vs. 198.4 ± 96.0; P = 0.025) was significantly higher in the severe group (Table 3).
Asymptomatic cardiac hypertrophy, defined according to recent ASE/EACVI guidelines [25], was detected in both groups although none of the patients had hypertension, as per the exclusion criteria. Echocardiography revealed a greater absolute (169.3 ± 34.6 g vs. 215.4 ± 61.5 g, P = 0.048) and indexed (LVMi: 101.8 ± 15.6 g/m2 vs. 133.3 ± 45.1 g/m2, P = 0.045; LVMh2.7: 45.3 ± 10.8 g/m2.7 vs. 58.8 ± 20.8 g/m 2.7, P = 0.036) LV mass in the severe group, suggesting a worsening of cardiac involvement in these patients (Table 4). Further support for this finding was obtained by analyzing the single parameters included in the Devereux formula for LV mass determination: LV diameter, interventricular septum thickness, and posterior wall thickness. LV diameter was higher, with a trend toward statistical significance, in the severe than in the mild-to-moderate group, whereas interventricular septum thickness and posterior wall thickness were similar.
Significant increases in LV end-diastolic volume (84.3 ± 15.3 ml vs. 105.9 ± 23.9 ml, P = 0.028), absolute LA volume (47.5 ± 14.9 ml vs. 65.4 ± 20.1 ml, P = 0.039) and indexed LA volume (LAVi: 28.5 ± 8.4 ml/m2 vs. 39.9 ± 15.5 ml/m2, P = 0.049; LAVh2.7: 12.9 ± 3.5 g/m2.7 vs. 16.6 ± 7.0 g/m2.7, P = 0.035) were also determined in the severe versus mild-to-moderate group. The mean LA volume of the severe group was larger than the upper value for normal adults reported in the international “Recommendations for cardiac chamber quantification” (< 58 ml for males and < 52 ml for females) [25]. In addition, diastolic dysfunction was detected in 9 of the 23 patients (7 with E/A < 1 and 2 with E/A > 2), with no significant differences between the severe and mild-to-moderate groups (38.5% vs. 50.0%, P = ns; Table 4). Arterial stiffness, evaluated by measuring ASI, was found to be higher in the severe compared to the mild-to-moderate group (17.0 ± 6.2 vs. 12.8 ± 3.0; P = 0.046; Table 4).
Right heart parameters, including pulmonary arterial pressure, TRV and IVC diameter, were significantly increased in the severe compared to the mild-to-moderate group. Right atrial area was larger than the upper value for normal adults [25] but not significantly different between the two groups. No significant differences were determined for any of the other parameters (Table 4).
Since the Framingham score was not significantly different between patients with severe versus mild-to-moderate SLE (Table 3), we examined the data of all 23 patients for a possible correlation between the Framingham score and echocardiographic measurements. We found that the Framingham score was directly related to LV mass, interventricular septum thickness and posterior wall thickness, as expected due to the correlation of these parameters with the blood pressure level even in normotensive patients (Fig. 3). No such relationship was found for LV diameter, LV end-diastolic volume and LA volume (data not shown). Finally, a direct correlation (r = 0.42; P = 0.049) between disease duration and echocardiographic LV end-diastolic volume values was identified (Fig. 4).
Correlation between the Framingham score and a left ventricular mass (LVM), b interventricular septum thickness (IVS), c left ventricular posterior wall thickness (PWt); Spearman rank test. d Differences in the Framingham score between patients without (plain histograms) and with (striped histograms) abnormal E/A and/or E/e′ ratio; t test
Discussion
Cardiovascular disease has emerged as one of the most important causes of death in SLE patients [26]. Consequently, the early identification of patients at increased risk is an essential step in the successful prevention of CVD in this population. During the active phase of SLE, patients may develop subclinical myocarditis associated with enlargement of the heart chambers [27]. Here, it is important to emphasize that in this study patients with hypertension or any congenital or acquired CVD event that could have influenced the echocardiographic measurements were excluded from participation.
In the 23 patients enrolled in the study, there was no correlation between disease activity and traditional risk factors such as smoking and hyperlipidemia. With the exception of triglyceride levels, the values of all laboratory parameters were similar in patients with mild-to-moderate and severe SLE, thus indicating that these values cannot be used to identify patients at higher risk of CVD. The Framingham score, commonly used in the CVD risk chart, was also ineffective in predicting which patients were at the highest risk of CVD; in fact, the mean values of the two study groups were not substantially different.
We therefore used echocardiographic measurements to examine the relationship between SLE and CVD. The results of those analyses showed that absolute and indexed LV mass and LA volume as well as LV end-diastolic volume were significantly higher in patients with severe than mild-to-moderate SLE. While the values in the former indicated LV diastolic dysfunction, neither the E/A ratio nor the E/e′ ratio differed significantly between the two groups. The lack of alterations in the early and late diastolic velocities can be explained by the fact that the SLE patients in our study were relatively young and had stable disease, such that the elasticity reserve of the left ventricle was still intact. However, the increased LV end-diastolic volume implied myocardial involvement.
Further evidence of LV diastolic dysfunction in severe SLE came from the significant increase in LA volume determined in this group of patients. This finding is consistent with the close link between LA dynamics and LV filling pressure. Indeed, in subjects without atrial arrhythmia, congenital heart disease, or mitral valve disease, increased LA volume typically reflects elevated LV filling pressure. During diastole, the LA is directly exposed to pressures in the LV. With increased stiffness or reduced compliance of the LV, the LA pressure rises to preserve adequate LV filling; therefore, the increased atrial wall tension leads to chamber dilatation and stretching of the atrial myocardium. [28]. Several studies have described LV diastolic dysfunction in SLE patients, including that it is more pronounced in patients with active disease [2, 29,30,31,32,33,34,35,36,37]. In our study, the Framingham score correlated directly with LV mass, LV posterior wall thickness, interventricular septum thickness and indirectly with the E/A ratio. These results provide evidence for subclinical myocardial involvement in patients with severe SLE.
Although the precise mechanisms responsible for these cardiac abnormalities in SLE patients are unknown, coronary artery disease, caused by premature atherosclerosis, endothelial damage, immune complex-mediated inflammation, renal failure, hypertension, dyslipidemia and toxicity from medications such as GCs, cyclophosphamide and chloroquine, is likely to be involved [2, 12, 34, 38]. Previous studies have reported evidence of a relationship between CVD and the exacerbation of atherogenesis by systemic inflammation [10, 39, 40]. In an animal model, the relationship between systemic immune activation, arterial inflammation and coronary lesions was shown to be significant. Activated immune cells infiltrate atherosclerotic plaques, where they release interleukins, tumor necrosis factor-α, platelet-derived growth factor and other cytokines that enhance the formation of atherosclerotic lesions. Atherogenesis is also supported by a cellular immune response specifically directed at oxidized low-density lipoprotein, heat-shock proteins, cardiolipin and β2-glycoprotein-I (reviewed in [41]). It should also be emphasized that the use of immunosuppressive therapy may not adequately target the chronic atherogenic inflammatory microenvironment [42].
An alternative explanation for the cardiac hypertrophy seen in our SLE patients is that enhanced inflammation results in salt retention, as chloride is necessary for immune cell function and sodium is a potent fluid modulator that contributes to fluid retention, thus aggravating diastolic dysfunction and myocardial hypertrophy [43,44,45]. This hypothesis is supported by the larger IVC diameter measured in patients with severe SLE. The higher TRV, pulmonary arterial pressure, and aortic stiffness in the severe group may reflect fluid overload or pulmonary capillaritis, both of which occur in patients with SLE of longer duration [46,47,48,49].
Our study also had several limitations. First, it lacked a control group. Second, the majority of the patients were young, which might have influenced the results. Third, the exams were conducted by a single observer. Finally, perhaps the most important limitation was the small number of patients. Our findings should therefore be interpreted with caution and evaluated in further studies of larger SLE populations.
Nevertheless, our results demonstrate the utility of echocardiography as a largely available noninvasive screening tool in SLE patients. Increases in LV mass and LA volume may allow the identification of SLE patients with early-stage myocardial damage. Since diastolic dysfunction typically develops at the initial phase of LV hypertrophy and can remain asymptomatic for several years, it would be important to determine whether these abnormalities are potentially reversible after clinical remission in patients with active disease.
References
Mok CC. Epidemiology and survival of systemic lupus erythematosus in Hong Kong Chinese. Lupus. 2011;20(7):767–71. https://doi.org/10.1177/0961203310388447.
Doria A, Iaccarino L, Sarzi-Puttini P, Atzeni F, Turriel M, Petri M. Cardiac involvement in systemic lupus erythematosus. Lupus. 2005;14(9):683–6. https://doi.org/10.1191/0961203305lu2200oa.
Bartels CM, Buhr KA, Goldberg JW, Bell CL, Visekruna M, Nekkanti S, et al. Mortality and cardiovascular burden of systemic lupus erythematosus in a US population-based cohort. J Rheumatol. 2014;41(4):680–7. https://doi.org/10.3899/jrheum.130874.
Bengtsson C, Ohman ML, Nived O, Rantapaa Dahlqvist S. Cardiovascular event in systemic lupus erythematosus in northern Sweden: incidence and predictors in a 7-year follow-up study. Lupus. 2012;21(4):452–9. https://doi.org/10.1177/0961203311425524.
Hesselvig JH, Ahlehoff O, Dreyer L, Gislason G, Kofoed K. Cutaneous lupus erythematosus and systemic lupus erythematosus are associated with clinically significant cardiovascular risk: a Danish nationwide cohort study. Lupus. 2017;26(1):48–53. https://doi.org/10.1177/0961203316651739.
Salmon JE, Roman MJ. Subclinical atherosclerosis in rheumatoid arthritis and systemic lupus erythematosus. Am J Med. 2008;121(10 Suppl 1):S3–8. https://doi.org/10.1016/j.amjmed.2008.06.010.
Favoino E, Favia EI, Digiglio L, Racanelli V, Shoenfeld Y, Perosa F. Effects of adjuvants for human use in systemic lupus erythematosus (SLE)-prone (New Zealand black/New Zealand white) F1 mice. Clin Exp Immunol. 2014;175(1):32–40. https://doi.org/10.1111/cei.12208.
Hong J, Maron DJ, Shirai T, Weyand CM. Accelerated atherosclerosis in patients with chronic inflammatory rheumatologic conditions. Int J Clin Rheumtol. 2015;10(5):365–81. https://doi.org/10.2217/ijr.15.33.
Negrini S, Pappalardo F, Murdaca G, Indiveri F, Puppo F. The antiphospholipid syndrome: from pathophysiology to treatment. Clin Exp Med. 2017;17(3):257–67. https://doi.org/10.1007/s10238-016-0430-5.
Roman MJ, Shanker BA, Davis A, Lockshin MD, Sammaritano L, Simantov R, et al. Prevalence and correlates of accelerated atherosclerosis in systemic lupus erythematosus. N Engl J Med. 2003;349(25):2399–406. https://doi.org/10.1056/NEJMoa035471.
Schoenfeld SR, Kasturi S, Costenbader KH. The epidemiology of atherosclerotic cardiovascular disease among patients with SLE: a systematic review. Semin Arthritis Rheum. 2013;43(1):77–95. https://doi.org/10.1016/j.semarthrit.2012.12.002.
Tincani A, Rebaioli CB, Taglietti M, Shoenfeld Y. Heart involvement in systemic lupus erythematosus, anti-phospholipid syndrome and neonatal lupus. Rheumatology. 2006;45(Suppl 4):iv8–13. https://doi.org/10.1093/rheumatology/kel308.
Tsao JT, Hsieh SC, Chiang BL, Yu CL, Lin SC. Altered IL-10 and TNF-alpha production in peripheral blood mononuclear cells of systemic lupus erythematosus patients after Toll-like receptor 2, 4, or 9 activation. Clin Exp Med. 2012;12(3):153–8. https://doi.org/10.1007/s10238-011-0161-6.
Westerweel PE, Luyten RK, Koomans HA, Derksen RH, Verhaar MC. Premature atherosclerotic cardiovascular disease in systemic lupus erythematosus. Arthritis Rheum. 2007;56(5):1384–96. https://doi.org/10.1002/art.22568.
Yang Z, Liang Y, Xi W, Li C, Zhong R. Association of increased serum IL-33 levels with clinical and laboratory characteristics of systemic lupus erythematosus in Chinese population. Clin Exp Med. 2011;11(2):75–80. https://doi.org/10.1007/s10238-010-0115-4.
Esdaile JM, Abrahamowicz M, Grodzicky T, Li Y, Panaritis C, du Berger R, et al. Traditional Framingham risk factors fail to fully account for accelerated atherosclerosis in systemic lupus erythematosus. Arthritis Rheum. 2001;44(10):2331–7.
Jafri K, Ogdie A, Qasim A, Patterson SL, Gianfrancesco M, Izadi Z, et al. Discordance of the Framingham cardiovascular risk score and the 2013 American College of Cardiology/American Heart Association risk score in systemic lupus erythematosus and rheumatoid arthritis. Clin Rheumatol. 2018;37(2):467–74. https://doi.org/10.1007/s10067-017-3860-x.
Shang Q, Yip GW, Tam LS, Zhang Q, Sanderson JE, Lam YY, et al. SLICC/ACR damage index independently associated with left ventricular diastolic dysfunction in patients with systemic lupus erythematosus. Lupus. 2012;21(10):1057–62. https://doi.org/10.1177/0961203312446628.
Hochberg MC. Updating the American College of Rheumatology revised criteria for the classification of systemic lupus erythematosus. Arthritis Rheum. 1997;40(9):1725. https://doi.org/10.1002/1529-0131(199709)40:9<1725::AID-ART29>3.0.CO;2-Y.
Petri M, Orbai AM, Alarcon GS, Gordon C, Merrill JT, Fortin PR, et al. Derivation and validation of the Systemic Lupus International Collaborating Clinics classification criteria for systemic lupus erythematosus. Arthritis Rheum. 2012;64(8):2677–86. https://doi.org/10.1002/art.34473.
Devereux RB. Left ventricular geometry, pathophysiology and prognosis. J Am Coll Cardiol. 1995;25(4):885–7. https://doi.org/10.1016/0735-1097(94)00547-4.
Lang RM, Bierig M, Devereux RB, Flachskampf FA, Foster E, Pellikka PA, et al. Recommendations for chamber quantification: a report from the American Society of Echocardiography’s Guidelines and Standards Committee and the Chamber Quantification Writing Group, developed in conjunction with the European Association of Echocardiography, a branch of the European Society of Cardiology. J Am Soc Echocardiogr. 2005;18(12):1440–63. https://doi.org/10.1016/j.echo.2005.10.005.
Pitsavos C, Toutouzas K, Dernellis J, Skoumas J, Skoumbourdis E, Stefanadis C, et al. Aortic stiffness in young patients with heterozygous familial hypercholesterolemia. Am Heart J. 1998;135(4):604–8. https://doi.org/10.1016/s0002-8703(98)70274-1.
Gordon C, Amissah-Arthur MB, Gayed M, Brown S, Bruce IN, D’Cruz D, et al. The British Society for Rheumatology guideline for the management of systemic lupus erythematosus in adults. Rheumatology. 2018;57(1):e1–45. https://doi.org/10.1093/rheumatology/kex286.
Lang RM, Badano LP, Mor-Avi V, Afilalo J, Armstrong A, Ernande L et al. Recommendations for cardiac chamber quantification by echocardiography in adults: an update from the American Society of Echocardiography and the European Association of Cardiovascular Imaging. J Am Soc Echocardiogr. 2015;28(1):1–39 e14. https://doi.org/10.1016/j.echo.2014.10.003.
Knight JS, Kaplan MJ. Cardiovascular disease in lupus: insights and updates. Curr Opin Rheumatol. 2013;25(5):597–605. https://doi.org/10.1097/BOR.0b013e328363eba3.
Mohammed AG, Alghamdi AA, ALjahlan MA, Al-Homood IA. Echocardiographic findings in asymptomatic systemic lupus erythematosus patients. Clin Rheumatol. 2017;36(3):563–8. https://doi.org/10.1007/s10067-016-3486-4.
Hsiao SH, Lin KL, Chiou KR. Comparison of left atrial volume parameters in detecting left ventricular diastolic dysfunction versus tissue Doppler recordings. Am J Cardiol. 2012;109(5):748–55. https://doi.org/10.1016/j.amjcard.2011.10.040.
Astorri E, Fiorina P, Ridolo E, Contini GA, Albertini D, Dall’Aglio P. Doppler echocardiographic study of left ventricular function in patients with systemic lupus erythematosus. Cardiologia. 1997;42(11):1179–83.
Chen J, Tang Y, Zhu M, Xu A. Heart involvement in systemic lupus erythematosus: a systemic review and meta-analysis. Clin Rheumatol. 2016;35(10):2437–48. https://doi.org/10.1007/s10067-016-3373-z.
Kalke S, Balakrishanan C, Mangat G, Mittal G, Kumar N, Joshi VR. Echocardiography in systemic lupus erythematosus. Lupus. 1998;7(8):540–4. https://doi.org/10.1191/096120398678920578.
Leung WH, Wong KL, Lau CP, Wong CK, Cheng CH. Cardiac abnormalities in systemic lupus erythematosus: a prospective M-mode, cross-sectional and Doppler echocardiographic study. Int J Cardiol. 1990;27(3):367–75.
Leung WH, Wong KL, Lau CP, Wong CK, Cheng CH, Tai YT. Doppler echocardiographic evaluation of left ventricular diastolic function in patients with systemic lupus erythematosus. Am Heart J. 1990;120(1):82–7.
Pieretti J, Roman MJ, Devereux RB, Lockshin MD, Crow MK, Paget SA, et al. Systemic lupus erythematosus predicts increased left ventricular mass. Circulation. 2007;116(4):419–26. https://doi.org/10.1161/CIRCULATIONAHA.106.673319.
Teixeira AC, Bonfa E, Herskowictz N, Barbato AJ, Borba EF. Early detection of global and regional left ventricular diastolic dysfunction in systemic lupus erythematosus: the role of the echocardiography. Rev Bras Reumatol. 2010;50(1):16–30.
Wislowska M, Deren D, Kochmanski M, Sypula S, Rozbicka J. Systolic and diastolic heart function in SLE patients. Rheumatol Int. 2009;29(12):1469–76. https://doi.org/10.1007/s00296-009-0889-4.
Yip GW, Shang Q, Tam LS, Zhang Q, Li EK, Fung JW, et al. Disease chronicity and activity predict subclinical left ventricular systolic dysfunction in patients with systemic lupus erythematosus. Heart. 2009;95(12):980–7. https://doi.org/10.1136/hrt.2008.153551.
Dammacco F, Della Casa Alberighi O, Ferraccioli G, Racanelli V, Casatta L, Bartoli E. Cyclosporine-A plus steroids versus steroids alone in the 12-month treatment of systemic lupus erythematosus. Int J Clin Lab Res. 2000;30(2):67–73. https://doi.org/10.1007/s005990070017.
Hansson GK. Inflammation, atherosclerosis, and coronary artery disease. N Engl J Med. 2005;352(16):1685–95. https://doi.org/10.1056/NEJMra043430.
Selzer F, Sutton-Tyrrell K, Fitzgerald SG, Pratt JE, Tracy RP, Kuller LH, et al. Comparison of risk factors for vascular disease in the carotid artery and aorta in women with systemic lupus erythematosus. Arthritis Rheum. 2004;50(1):151–9. https://doi.org/10.1002/art.11418.
Sanjadi M, Rezvanie Sichanie Z, Totonchi H, Karami J, Rezaei R, Aslani S. Atherosclerosis and autoimmunity: a growing relationship. Int J Rheum Dis. 2018;21(5):908–21. https://doi.org/10.1111/1756-185X.13309.
Doria A, Shoenfeld Y, Wu R, Gambari PF, Puato M, Ghirardello A, et al. Risk factors for subclinical atherosclerosis in a prospective cohort of patients with systemic lupus erythematosus. Ann Rheum Dis. 2003;62(11):1071–7.
Mak GS, Sawaya H, Khan AM, Arora P, Martinez A, Ryan A, et al. Effects of subacute dietary salt intake and acute volume expansion on diastolic function in young normotensive individuals. Eur Heart J Cardiovasc Imaging. 2013;14(11):1092–8. https://doi.org/10.1093/ehjci/jet036.
Matsui H, Ando K, Kawarazaki H, Nagae A, Fujita M, Shimosawa T, et al. Salt excess causes left ventricular diastolic dysfunction in rats with metabolic disorder. Hypertension. 2008;52(2):287–94. https://doi.org/10.1161/HYPERTENSIONAHA.108.111815.
Wang G, Nauseef WM. Salt, chloride, bleach, and innate host defense. J Leukoc Biol. 2015;98(2):163–72. https://doi.org/10.1189/jlb.4RU0315-109R.
Huang C, Li M, Liu Y, Wang Q, Guo X, Zhao J, et al. Baseline characteristics and risk factors of pulmonary arterial hypertension in systemic lupus erythematosus patients. Medicine. 2016;95(10):e2761. https://doi.org/10.1097/MD.0000000000002761.
Johnson SR, Granton JT. Pulmonary hypertension in systemic sclerosis and systemic lupus erythematosus. Eur Respir Rev. 2011;20(122):277–86. https://doi.org/10.1183/09059180.00003811.
Prete M, Fatone MC, Vacca A, Racanelli V, Perosa F. Severe pulmonary hypertension as the initial manifestation of systemic lupus erythematosus: a case report and review of the literature. Clin Exp Rheumatol. 2014;32(2):267–74.
Quadrelli SA, Alvarez C, Arce SC, Paz L, Sarano J, Sobrino EM, et al. Pulmonary involvement of systemic lupus erythematosus: analysis of 90 necropsies. Lupus. 2009;18(12):1053–60. https://doi.org/10.1177/0961203309106601.
Funding
This work was supported by the Italian Association for Cancer Research (AIRC) through an Investigator Grant (No. 20441) to VR.
Author information
Authors and Affiliations
Contributions
PL, SC and VR planned the study and prepared the draft of the manuscript. MP contributed to the study design. AGS, NS, LC, AB and PC cared for the patients, collected data and contributed to data analyses and interpretation. FD, AV and VR provided critical revisions of the manuscript related to its intellectual content. All authors reviewed and approved the manuscript and accept their accountability for all aspects of this study.
Corresponding author
Ethics declarations
Conflict of interest
The authors have no potential conflict of interest to declare with respect to the research, authorship and/or publication of this article.
Ethical approval
The study protocol was approved by the Ethics Committee of the University of Bari Medical School and conformed to the good clinical practice guidelines of the Italian Ministry of Health and the ethical guidelines of the Declaration of Helsinki, as revised and amended in 2004.
Informed consent
All study patients provided written informed consent.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Leone, P., Cicco, S., Prete, M. et al. Early echocardiographic detection of left ventricular diastolic dysfunction in patients with systemic lupus erythematosus asymptomatic for cardiovascular disease. Clin Exp Med 20, 11–19 (2020). https://doi.org/10.1007/s10238-019-00600-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10238-019-00600-8