Abstract
Introduction
Point-of-care ultrasound (POCUS) education is a requirement of graduate medical education in EM. Milestones have been established to assess resident US competency. However, the delivery of POCUS education has not been standardized. This study aims to evaluate the impact of implementing a longitudinal, structured POCUS curriculum during EM residency on trainee competency and confidence.
Methods
A prospective study of PGY-3 trainees before and after implementation of a novel POCUS curriculum was performed over an 18-month period at an EM residency training program. Curriculum design included longitudinal POCUS application–based monthly electronic content, bi-monthly residency conference sessions, and hands-on rotations. PGY-3 resident’s POCUS knowledge was assessed with a 38-question multiple-choice and image-based exam. Further, PGY-3 residents were surveyed regarding POCUS confidence. Survey results evaluated provider confidence, satisfaction with the novel curriculum, and overall perception of POCUS utility scored on a 1 (low) to 5 (high) scale. Results were evaluated using an unpaired t test for data analysis.
Results
Mean quiz scores of 8 pre-curriculum PGY-3 residents (84%; 95%CI 78.46–89.54) were not significantly different when compared with 13 post-curriculum PGY-3 residents (82%; 95%CI 77.11–86.89) (p = 0.6126). Survey results for pre-curriculum trainees across each section were 4.13 (95%CI 3.91–4.35), 3.68 (95%CI 3.32–4.04), and 4.33 (95%CI 4.06–4.6). Results for post-curriculum trainees trended higher for each section at 4.22 (95%CI 4.04–4.40) (p = 0.4738), 3.84 (95%CI 3.52–4.16) (p = 0.5279), and 4.49 (95%CI 4.21–4.77) (p = 0.4534).
Conclusions
Implementation of a structured, longitudinal POCUS curriculum resulted in a trend towards improved trainee confidence, satisfaction, and perception of POCUS. Future studies are needed to identify the optimal structure for POCUS educational content delivery and competency assessment for EM resident providers.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Introduction
The American College of Emergency Medicine (ACEP) defines point-of-care ultrasound (POCUS) competency as the ability to recognize the indications and contraindications when performing an ultrasound exam, the skill to acquire POCUS images and distinguish normal anatomy from pathology, and finally, the knowledge to incorporate POCUS findings into patient care [1]. ACEP further described POCUS as “a skill integral to the practice of emergency medicine (EM),” resulting in the Accreditation Council for Graduate Medical Education (ACGME) and the American Board of Emergency Medicine (ABEM) designating POCUS as one of twenty-three (23) EM residency competency milestones [2,3,4,5,6]. In order to meet POCUS training requirements, the model curriculum, including minimum education standards and approaches to competency assessment, has been published [6, 7]. Despite this, recent studies demonstrate significant variation in the method of POCUS education delivery and assessment, as well as recommend the need to standardize ultrasound training for all EM residency programs [8,9,10]. Our study sought to assess the impact of a novel POCUS curriculum, patterned after established POCUS education guidelines, on resident POCUS confidence and competency.
Methods
This study was conducted as a prospective observational study of post-graduate year (PGY) three residents in a PGY 1–3 EM residency program before and after the implementation of a longitudinal novel POCUS curriculum. The study was approved by the institutional review board.
Prior to the implementation of the novel POCUS curriculum, EM resident POCUS training included bi-annual resident conference training sessions, a required four-week PGY-1 POCUS rotation, and an elective PGY-2 or 3 POCUS rotation. The novel longitudinal POCUS curriculum was implemented over an 18-month period and involved the bi-monthly delivery of POCUS application–based content during 2-h residency conference didactic sessions, structured four-week required PGY-1 and elective PGY-3 POCUS rotations, a twenty-four (24)-month POCUS pre-fellowship track, asynchronous online content including instructional videos, research articles, content summaries and quizzes, rigorous POCUS image review with provider feedback, cumulative Standardized Direct Observation Tool (SDOT) evaluation, and core faculty training and POCUS credentialing.
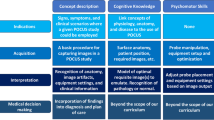
Residency conference didactic sessions consisted of an introductory presentation of the POCUS topic, demonstration of scanning techniques, and the opportunity for individual-proctored hands-on training with each resident provider (Fig. 1). The structure and content of the curriculum followed the ACEP POCUS residency training pathway guideline, POCUS milestone, and model curriculum recommendations, including both basic and advanced topics (Table 1) [3,4,5,6,7].
The impact of the novel POCUS curriculum on resident competency was assessed through an image-based thirty-eight (38) multiple-choice question quiz administered to PGY-3 residents before and after curriculum implementation. Additionally, a survey was also administered pre- and post-curriculum to assess provider confidence. Survey results were condensed into 3 sections that evaluated provider confidence, satisfaction with the novel curriculum, and overall perception of POCUS utility scored on a 1 (low) to 5 (high) scale. Results were evaluated using an unpaired t test for data analysis.
Results
Mean pre-curriculum quiz scores obtained from 8 of 14 (57.1%) PGY-3 residents (84%; 95%CI 78.46–89.54) who completed the quiz were not significantly different when compared with 13 of 14 (92.9%) post-curriculum PGY-3 residents (82%; 95%CI 77.11–86.89) (p = 0.6126). Survey results for the same pre-curriculum trainees across each section were 4.13 (95%CI 3.91–4.35), 3.68 (95%CI 3.32–4.04), and 4.33 (95%CI 4.06–4.6). Results for post-curriculum trainees, while not statistically significant, trended higher for each section at 4.22 (95%CI 4.04–4.40) (p = 0.4738), 3.84 (95%CI 3.52–4.16) (p = 0.5279), and 4.49 (95%CI 4.21–4.77) (p = 0.4534).
Discussion
Due to continuously evolving EM resident training standards, educators must identify and implement novel POCUS curricula resulting in consistent competency outcomes [1]. While multiple specialties have demonstrated the benefits of standardized POCUS curricula on trainee education and confidence, few EM-based studies exist [11,12,13]. Our study sought to describe a novel, structured POCUS curriculum and assess its impact on EM resident education and competency.
There exists a variety of approaches to the delivery of POCUS educational content and competency assessment. Recommended approaches for content delivery include didactic classroom or conference sessions, asynchronous web-based and textbook reading assignments, question banks, and proctored hands-on training spread longitudinally over the entirety of residency training. Competency assessment may occur through review of the resident’s POCUS images during scheduled quality assurance (QA) teaching sessions or at the bedside, and through standardized knowledge assessments, including Observed Structured Clinical Examinations (OSCEs) and standardized direct observation tools (SDOTs) [1, 6]. Given the significant breadth of approaches to POCUS education and competency assessment, it may be difficult for educators to identify methods which will have the greatest impact on their resident learners.
The longitudinal curriculum successfully maintained a high level of POCUS competency (> 80%), while developing a trend towards increased POCUS confidence, satisfaction, and perception. Further, it demonstrated that an established POCUS curriculum could be successfully expanded to meet published guidelines without negatively impacting resident education, which may be beneficial to EM POCUS educators looking to update their curricula. During curriculum development and implementation, potential future approaches to improving EM POCUS education and competency assessment were identified. Conversion of the large, residency conference-based sessions into smaller, hands-on sessions focused by PGY group, which integrate POCUS training with clinical scenarios and simulation cases, might allow for improved content retention. Further, exchanging electronic mail content delivery with a cloud, podcast, or website-based approach, might more closely match today’s learners approach to content consumption and improve retention. Additionally, annual OSCE and SDOT-based competency assessments, as opposed to a single session prior to graduation, may allow educators to tailor content to the individual learner and provide timely remediation. Future studies are needed to evaluate these approaches to POCUS educational content delivery and competency assessment.
Conclusion
Implementation of a structured, longitudinal POCUS curriculum resulted in a trend towards improved trainee confidence, satisfaction, and perception of POCUS. Future studies are needed to identify the optimal structure for POCUS educational content delivery and competency assessment for EM resident providers.
References
Ultrasound Guidelines (2017) Emergency, point-of-care and clinical ultrasound guidelines in medicine. Ann Emerg Med 69:27–54
Hockberger RS, Binder LS, Graber MA et al (2001) The model of the clinical practice of emergency medicine. Ann Emerg Med 37:745–770
Beeson MS, Carter WA, Christopher TA, Heidt JW, Jones JH, Meyer LE, Promes SB, Rodgers KG, Shayne PH, Wagner MJ, Swing SR (2013) Emergency medicine milestones. J Grad Med Educ 5:5–13
Lewiss RE, Pearl M, Nomura JT, Baty G, Bengiamin R, Duprey K, Stone M, Theodoro D, Akhtar S (2013) CORD-AEUS: consensus document for the emergency ultrasound milestone project. Burton J, ed. Acad Emerg Med 20:740–745
Nelson M, Abdi A, Adhikari S, Boniface M, Bramante RM, Egan DJ, Matthew Fields J, Leo MM, Liteplo AS, Liu R, Nomura JT, Pigott DC, Raio CC, Ruskis J, Strony R, Thom C, Lewiss RE (2016) Goal-directed focused ultrasound milestones revised: a multiorganizational consensus. DeIorio NM, ed. Acad Emerg Med 23:1274–1279
Akhtar S, Theodoro D, Gaspari R et al (2009) Resident training in emergency ultrasound: consensus recommendations from the 2008 council of emergency medicine residency directors conference. Acad Emerg Med 16:32–36
Mateer J, Plummer D, Heller M, Olson D, Jehle D, Overton D, Gussow L (1994) Model curriculum for physician training in emergency ultrasonography. Ann Emerg Med 23:95–102
Ahern M, Mallin MP, Weitzel S et al (2010) Variability in ultrasound education among emergency medicine residencies. West J Emerg Med 11:314–318
Amini R, Adhikari S, Fiorello A (2014) Ultrasound competency assessment in emergency medicine residency programs. Yarris LM, ed. Acad Emerg Med 21:799–801
Smalley CM, Dorey A, Thiessen M, Kendall JL (2016) A survey of ultrasound milestone incorporation into emergency medicine training programs. J Ultrasound Med 35:1517–1521
Turner EE, Fox JC, Rosen M, Allen A, Rosen S, Anderson C (2015) Implementation and assessment of a curriculum for bedside ultrasound training. J Ultrasound Med 34:823–828
Nassour I, Spalding MC, Hynan LS, Gardner AK, Williams BH (2017) The surgeon-performed ultrasound: a curriculum to improve residents’ basic ultrasound knowledge. J Surg Res 213:51–59
Anstey JE, Jensen TP, Afshar N (2018) Point-of-care ultrasound needs assessment, curriculum design, and curriculum assessment in a large academic internal medicine residency program. South Med J 111:444–448
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Conflict of interest
The authors declare that they have no conflict of interest.
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
About this article
Cite this article
Filler, L., Orosco, D., Rigdon, D. et al. Evaluation of a novel curriculum on point-of-care ultrasound competency and confidence. Emerg Radiol 27, 37–40 (2020). https://doi.org/10.1007/s10140-019-01726-8
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10140-019-01726-8