Abstract
The transurethral resection of bladder tumor (TURBT) remains the most widely used method in the surgical treatment of the non-muscle invasive bladder tumor (NMIBT). Despite its popularity, the laser technique has been widely used in urology as an alternative, via the application of transurethral laser enucleation of bladder tumor. The aim of the present study was to compare the efficacy and feasibility between transurethral laser enucleation and transurethral resection of bladder tumor. A systematic search of the following databases was conducted: PubMed, Wed of Science, Cochrane Library, EMBASE, Google scholar, and Medline. The search included studies up to the 1st of January 2017. The outcomes of interest that were used in order to assess the two techniques included operation time, catheterization time, hospitalization time, obturator nerve reflex, bladder perforation, bladder irritation, 24-month-recurrence rate, and the postoperative adjuvant intravesical chemotherapy. A total of 13 trials with 2012 participants were included, of which 975 and 1037 underwent transurethral laser enucleation and transurethral resection of bladder tumor, respectively. No significant difference was noted in the operation time between the two groups, although significant differences were reported for the variables catheterization time, hospitalization time, obturator nerve reflex, bladder perforation, bladder irritation, and 24-month-recurrence rate. In the mitomycin and epirubicin subgroups, no significant differences were observed in the laser enucleation and TURBT methods with regard to the 24-month-recurrence rate. The laser enucleation was superior to TURBT with regard to the parameters obturator nerve reflex, bladder perforation, catheterization time, hospitalization time, and 24-month-recurrence rate. Moreover, laser enucleation can offer a more accurate result of the tumor’s pathological stage and grade.
Similar content being viewed by others
Explore related subjects
Discover the latest articles, news and stories from top researchers in related subjects.Avoid common mistakes on your manuscript.
Urinary carcinoma of the bladder (UCB) is the second most common urological malignancy worldwide. The increasing trends of bladder tumor and related cancers have been reported due to the prevalent smoking habits of large populations worldwide. UCB ranks ninth in the worldwide cancer incidence. It is the seventh most common malignancy in men and the seventeenth in women [1, 2]. Bladder cancer exhibits three biological characteristics: local infiltration, recurrence, and distant metastasis. Transurethral resection of bladder tumor (TURBT) is the gold standard to treat the non-muscle invasive bladder tumor (NMIBT). However, TURBT is a procedure that is potentially associated with morbidity, and complications such as bleeding, obturator nerve reflex, and bladder perforation are frequently reported. In order to improve the safety and efficacy of TURBT, alternative procedures have been developed [3, 4]. The application of laser has been widely used in surgery notably in urology, due to certain advantages in lithotripsy cutting, vaporization, and hemostasis function. The latter methodological procedures have been employed in place of the traditional conventional operation [5]. The present study aimed to compare the efficacy and feasibility of transurethral laser enucleation versus transurethral resection of bladder tumor for the treatment of NMIBC.
Materials and methods
Literature search
A systematic search of the following databases was conducted: PubMed, Wed of Science, Cochrane Library, EMBASE, Google scholar, and Medline. The search included all published trials up to the 1st of January 2017, which comparing transurethral laser enucleation and TURBT with following MESH search heading:“en bloc resection” “transurethral resection” “bladder tumor” “bladder cancer” “bladder carcinoma” “TURBT” “holmium laser resection of the bladder tumor” “HoLRBT”. Meanwhile, a full manual search from the reference list of each relevant article was carried out. All article of language was constricted to English and all relevant studies were included for further screening.
Inclusion criteria and exclusion criteria
Trials were included according to the following criteria: (1) randomized controlled trials (RCTs) and/or non-RCTs, (2) studies that involved the comparison of laser enucleation and TURBT, (3) studies that included patients with primary bladder cancer grade of G1 to G3, as demonstrated by biopsy and non-muscle invasion (Ta, Tis, and T1) as demonstrated by computerized tomography and/or cystoscopy, (4) studies that included patients who underwent no prior transurethral resection procedure such as TURBT or TURP, (5) and studies that included at least one outcome of interest as described in the following section.
The exclusion criteria were the following: (1) studies that included patients with other diseases, such as prostate cancer, BPH and/or other urological neoplasms, (2) studies that included no outcomes of interest and/or lack of data calculation and/or extrapolation from the published results regarding either laser enucleation or TURBT.
Data extraction and outcome of interest
A total of two reviewers independently extracted the following data: first author, year of publication, country, study interval, study design, number of patients who underwent laser enucleation and/or TURBT, and outcomes of interest. The extracted outcomes included the baseline characteristics of the patients, such as age, surgical method, operation time, catheterization time, hospitalization time, obturator nerve reflex, bladder perforation, bladder irritation, 24-month-recurrence rate, and the postoperative adjuvant intravesical chemotherapy.
Study quality and level of evidence
The level of evidence of the included studies was rated according to the criteria by the Centre for Evidence-Based Medicine in Oxford, United Kingdom [6]. A total of two reviewers independently assessed the quality of the studies and any disagreement was resolved by consensus.
Statistical analyses
The present meta-analysis was conducted according to the recommendations of the Cochrane Collaboration and the Quality of Reporting of Meta-analyses guidelines [7]. All the statistical analyses were carried out using RevMan 5.3 (Cochrane Library Software, Oxford, United Kingdom). For continuous variables, weighted mean difference (WMD) was used, whereas for dichotomous parameters, odds ratio (OR) was used. The confidence interval (CI) was set at 95%. All the pooled effects were determined by the Z test, and a probability value of less than 0.05 (P < 0.05) was considered statistically significant. The quantity of heterogeneity among included studies was assessed by the chi-square-based Q test and the I 2 test when I 2 < 50% and P > 0.05. The fixed-effects model was used, when no heterogeneity was noted. In the presence of heterogeneity, the random-effects model was used. Sensitivity analysis outcomes were reported by three and/or more studies in the overall meta-analysis.
Result
Workflow of literature research
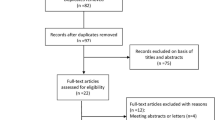
There were 437 potential studies in the primary literature research, in which 41 duplicated studies existed. The remaining 396 studies were further screened by reading the title and abstract. Thirty-two studies with full-text articles were screened and 13 studies were included in the meta-analysis which contain 4 RCTs and 9 retrospective trials. We described the study procedure’s details in Fig. 1.
Study characteristics
A total of 13 trials with 2012 participants were included, of which 975 and 1037 underwent transurethral laser enucleation and transurethral resection of bladder tumor, respectively. The demographics of enrolled individuals and tumor characteristics are presented in Table 1.
The data of outcome of interest
The main results of complications and periopretive data were enumerated in Table 2. No significant difference was noted in the operation time between the two groups (Fig. 2: mean difference [WMD] − 0.6, 95% confidence interval [CI] − 1.35 to 0.16, P = 0.12). In contrast to the operation time, significant differences were noted for the parameters catheterization time (Fig. 3: [WMD] − 0.95, [CI] − 1.03 to −0.87, P < 0.00001), hospitalization time (Fig. 4: [WMD] − 1.34, [CI] − 1.43 to − 1.25, P < 0.00001), obturator nerve reflex (Fig. 5: OR = 0.04, [CI] 0.02 to 0.11, P < 0.00001), bladder perforation (Fig. 6: OR = 0.14, [CI]0.05 to 0.39, P = 0.00001), bladder irritation (Fig. 7: OR = 0.32, [CI] 0.23 to 0.45, P < 0.00001), and 24-month-recurrence rate (Fig. 8: OR = 0.72,[CI]0.53 to 0.96, P = 0.03). In the mitomycin and the epirubicin subgroups, no significant differences were noted in the laser enucleation and TURBT in the 24-month-recurrence rate (Fig. 9: OR = 0.73, [CI] 0.49 to 1.09, P = 0.12; OR = 0.70,[CI] 0.45 to 1.09, P = 0.12).
Discussion
In 2012, 429,793 cases of bladder cancer were diagnosed and 165,084 deaths were attributable to bladder cancer. Approximately 75% of newly diagnosed patients were non-muscle-invasive bladder cancer cases (NMIBC), whereas the remaining 25% were muscle invasive bladder cancer (MIBC) and/or metastatic disease cases [21]. TURBT is a sufficient and potentially curative therapy and is considered the gold standard treatment to the NMIBC [22]. Laser application is a new, streamlined, safe, and effective technology that can meet the growing demands of the surgery and fulfill the requirement for clinical performance, notably in urology [5]. The laser enucleation of bladder tumor has been widely adopted in clinical practice, notably in surgery, due to its advantages. The following advantages were summarized from literature search regarding laser enucleation of bladder tumor: Firstly, the absence of the electric field effect is considered a significant advantage since the laser can reduce the obturator nerve stimulation and avoid its reflection. Consequently, the incidence of serious complications, such as bladder perforation, decreases, and the technique is considered safe for the patients with cardiac pacemaker [23]. Secondly, the tumor stage and grade can be diagnosed more effectively using sufficient tissue for pathological examination by adequate resection depth of the basal parts of the tumors. This contributes in the formulation of an appropriate follow-up treatment and the prediction of the recurrence rate [24]. Lastly, the perfusion fluid used is physiological saline that reduces the occurrence of the TUR syndrome [25].
In the present meta-analysis, no significant difference in the operation time was noted. However, the parameters obturator nerve reflex, bladder perforation, bladder irritation, catheterization time, hospitalization time, and 24-month-recurrence rate were significantly different between the laser enucleation and TURBT methods. The data conform to our experience. In addition, the postoperative adjuvant intravesical chemotherapy was carried out in the subgroup (mitomycin and epirubicin groups), and there was no significant difference between laser enucleation and TURBT in the 24-month-recurrence rate, although a significant difference was noted between the aforementioned methodological techniques in the 24-month-recurrence rate in total. This result demonstrated that the postoperative adjuvant intravesical chemotherapy is an important factor which affected the 24-month-recurrence rate between the groups of laser enucleation and transurethral resection of bladder tumor. In the present study, we can conclude that the postoperative complication of laser enucleation is lower in the bladder perforation and the bladder irritation. Furthermore, the group of laser enucleation exhibited optimal recovery with shorter catheterization and hospitalization time periods. An apparent superiority was noted for the laser enucleation versus TURBT. According to the biological characteristics of bladder tumors, the postoperative adjuvant intravesical chemotherapy is an important factor that affects the recurrence of the bladder tumor. Despite these findings, the current study suffers from several limitations. Firstly, we only included studies published in English, and certain related studies published in other languages might have been missed. Secondly, a study heterogeneity was evident notably regarding the parameters for bladder perforation, 24-month-recurrence rate, and postoperative adjuvant intravesical chemotherapy (Table 2). These may be caused by the heterogeneities of the patients’ conditions, operators’ surgical technique, laser’s type, and/or the limited sample size of certain data. Thirdly, although the funnel plots indicated no visible publication bias, the influence of bias cannot be completely excluded. Lastly, the included studies lacked selection criteria regarding the follow-up, and the follow-up was not long enough in order to provide long-term recurrence data.
Conclusion
The laser enucleation was superior to TURBT with regard to the parameters obturator nerve reflex, bladder perforation, catheterization time, hospitalization time, and 24-month-recurrence rate. Moreover, laser enucleation can offer a more accurate result of the tumor’s pathological stage and grade by providing a better specimen.
References
Ferlay J, Soerjomataram I, Dikshit R et al (2015) Cancer incidence and mortality worldwide: sources, methods and major patterns in GLOBOCAN 2012. Int J Cancer 136(5):E359–E386
Siegel RL, Miller KD, Jemal A (2016) Cancer statistics, 2016. Ca A Cancer J Clin 66(1):7–30
Sanli O, Dobruch J, Knowles MA et al (2017) Bladder cancer, 2017. Nat Rev Dis Primers 3:1–19
Kaufman DS, Shipley WU, Feldman AS (2009) Bladder cancer. Lancet 374(9685):239
Zarrabi A, Gross AJ (2011) The evolution of lasers in urology. Ther Adv Urol 3(2):81–89
Phillips B (2004) GRADE: levels of evidence and grades of recommendation. Arch Dis Child 89:489
Clarke MRH (2001) Bringing it all together: Lancet-Cochrane collaborate on systematic reviews. Lancet 357:1728
D'Souza N, Verma A (2016) Holmium laser transurethral resection of bladder tumor: our experience. Urol Ann 8(4):439
Tao W, Yang D, Shan Y et al (2013) Safety and efficacy of 120W high performance system greenlight laser vaporization for non-muscle-invasive bladder cancer. J X-ray sci and technol 21(2):309–316
Zhang XR, Feng C, Zhu WD et al (2015) Two micrometer continuous-wave thulium laser treating primary non-muscle-invasive bladder cancer: is it feasible? A randomized prospective study. Photomed Laser Surg 33(10):517–523
Migliari R, Buffardi A, Ghabin H (2015) Thulium laser endoscopic en bloc enucleation of nonmuscle-invasive bladder cancer. J Endourol 29(11):1258
Huang J-H, Hu Y-Y, Liu M et al (2016) Comparative study of 2 um laser versus Holmium laser for the resection of non-muscle invasive bladder cancer. Int J Clin Exp Med 9(12):23618–23623
Kramer MW, Rassweiler JJ, Klein J et al (2015) En bloc resection of urothelium carcinoma of the bladder (EBRUC): a European multicenter study to compare safety, efficacy, and outcome of laser and electrical en bloc transurethral resection of bladder tumor. World J Urol 33(12):1937–1943
Yang D, Xue B, Zang Y, et al (2014) Efficacy and safety of potassium-titanyl-phosphate laser vaporization for clinically non-muscle invasive bladder cancer. Urol J 11(1):1258–1263
Chen Z, Guo SW, Tang YQ et al (2010) Clinical obervation on 2 micron laser for non-muscle -invasive bladder tumor treatment: single-center experience. World J Urol 28:157–161
Xishuang S, Deyong Y, Xiangyu C et al (2010) Comparing the safety and efficiency of conventional monopolar, plasmakinetic, and holmium laser transurethral resection of primary non-muscle invasive bladder cancer. J Endourol 24(1):69–73
Zhu Y, Jiang X, Zhang J et al (2008) Safety and efficacy of holmium laser resection for primary nonmuscle-invasive bladder cancer versus transurethral electroresection: single-center experience. Urology 72(3):608–612
Liu H, Wu J, Xue S et al (2013) Comparison of the safety and efficacy of conventional monopolar and 2-micron laser transurethral resection in the management of multiple nonmuscle-invasive bladder cancer. J Int Med Res 41(4):984
Chen X, Liao J, Chen L et al (2015) En bloc transurethral resection with 2-micron continuous-wave laser for primary non-muscle-invasive bladder cancer: a randomized controlled trial.World. J Urol 33(7):989–995
Chen J, Zhao Y, Wang S et al (2016) Green-light laser en bloc resection for primary non-muscle-invasive bladder tumor versus transurethral electroresection: a prospective, nonrandomized two-center trial with 36-month follow-up. Laser Surg Med 48(9):859–865
Smith AB, Deal AM, Woods ME et al (2014) Muscle-invasive bladder cancer: evaluating treatment and survival in the National Cancer Data Base. BJU Int 114(5):719–726
Burger M, Catto JW, Dalbagni G et al (2013) Epidemiology and risk factors of urothelial bladder cancer. Eur Urol 63(2):234–241
Kramer MW, Rassweiler JJ, Klein J et al (2015) En bloc resection of urothelium carcinoma of the bladder (EBRUC): a European multicenter study to compare safety, efficacy, and outcome of laser and electrical en bloc transurethral resection of bladder tumor. World J Urol 14(12):1937–1943
Wolters M, Kramer MW, Becker JU et al (2011) Tm:YAG laser en bloc mucosectomy for accurate staging of primary bladder cancer: early experience. World J Urol 29(4):429–432
Kramer MW, Abdelkawi IF, Wolters M et al (2014) Current evidence for transurethral en bloc resection of non-muscle-invasive bladder cancer. Minim Invasive Ther Allied Technol 23(4):206
The role of funding source
The work was supported by Independent innovation research fund of Huazhong University of Science and Technology, China; Award Number: 1802030.
Author information
Authors and Affiliations
Corresponding author
Ethics declarations
Ethnical approval
All analyses were based on previous published studies, thus no ethical approval and patient consent are required.
Conflict of interest
The authors declare that they have no competing interest.
Rights and permissions
About this article
Cite this article
Yang, H., Wang, N., Han, S. et al. Comparison of the efficacy and feasibility of laser enucleation of bladder tumor versus transurethral resection of bladder tumor: a meta-analysis. Lasers Med Sci 32, 2005–2012 (2017). https://doi.org/10.1007/s10103-017-2308-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10103-017-2308-5