Abstract
Purpose
The emergence of carbapenem-resistant P. aeruginosa (CRPA) harbouring acquired carbapenemase genes (blaVIM, blaIMP and blaNDM) has become a global public health threat. Three CRPA isolates included in the study had an extensively drug-resistant phenotype with susceptibility to colistin only and were positive for the blaNDM-1 gene. The current study aimed to investigate the genomic epidemiology and molecular characteristics of the blaNDM-1-positive CRPA isolates collected from the Gauteng region, South Africa.
Methods
Short read whole genome sequencing (WGS) was performed to determine sequence types (STs), genetic relatedness, resistome, virulome and the genetic environment of the blaNDM-1 gene.
Results
The WGS and phylogenetic analyses revealed that the study isolates belonged to an international high-risk clone ST773 and belonged to the same clade with eight blaNDM-1-positive ST773 isolates from Hungary, India, Nigeria, South Korea and USA. The study isolates harboured a wide repertoire of intrinsic and acquired antibiotic resistance genes (ARGs) related with mobile genetic elements, porins and efflux pumps, as well as virulence factor genes. The clade-specific ARGs (blaNDM-1, floR2/cmlA9, rmtB4, tetG) were found in a putative integrative and conjugative element (ICE) region similar to ICE6660-like.
Conclusion
As ICE carrying the blaNDM-1 gene can easily spread to other P. aeruginosa isolates and other Gram-negative bacteria, the findings in this study highlight the need for appropriate management strategies and active surveillance of CRPA isolates in the Gauteng region, South Africa.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Pseudomonas aeruginosa is an important opportunistic pathogen causing a wide range of healthcare-associated infections, including ventilator-associated pneumonia, catheter-associated urinary tract, surgical site, burn wound and bloodstream infections (BSIs) [1,2,3]. In recent years, the emergence of carbapenem-resistant P. aeruginosa (CRPA), along with international/global “high-risk clones” (specific epidemic P. aeruginosa clones that exhibit multidrug-resistant (MDR) or extensively drug-resistant (XDR) phenotypes and are characterised by worldwide dissemination in the hospital environments; e.g. sequence type (ST) 235, ST111, ST233, ST308, ST654 and ST773), has become a major national and international public health concern due to its intrinsic and acquired ability to rapidly become resistant against multiple antibiotics including carbapenems [4,5,6].
Carbapenem resistance in P. aeruginosa can be achieved by one or a combination of resistance mechanisms, which can include (i) chromosomal mutations that alter the OprD porin activity (reduced permeability) and promote down-regulation (e.g. mutation in mexT) or loss of the OprD porin; (ii) overexpression of the efflux pump systems and chromosomal cephalosporinases (AmpC); and (iii) enzymatic inactivation of carbapenems by carbapenemases that are acquired through horizontal transfer (HGT) of mobile genetic elements (MGEs) [6,7,8,9]. The most common carbapenemases found in P. aeruginosa are metallo-β-lactamases (MBLs), such as the Verona integron–encoded MBL (VIM) and imipenem-hydrolysing MBL (IMP) [10,11,12]. In contrast, another type of MBL called the New Delhi MBL (NDM) is rare in P. aeruginosa (ranging from 0.04% (3/8010) to 0.88% (26/2953)) [10, 12]. Amongst the NDM variants, NDM-1 is the most widely spread and the most prevalent variant that can be found across the Enterobacterales order (K. pneumoniae, E. coli, the Enterobacter cloacae complex and others) and 10 bacterial families of Gammaproteobacteria, including the Moraxellaceae family (Acinetobacter spp.) and the Pseudomonadaceae family (Pseudomonas spp.) in over 80 countries on all continents except Antarctica [10, 13, 14].
In South Africa, the first laboratory-confirmed case of NDM-1 was reported in 2011 in a carbapenem-resistant E. cloacae isolate, which was recovered from a patient admitted to an academic hospital in Johannesburg [15]. Four years later, the blaNDM-1 gene was reported in P. aeruginosa isolates from cystic fibrosis patients in Durban [16]. However, the molecular epidemiological characteristics of these isolates or the genetic context of the blaNDM-1 gene in these isolates was not further explored. Here, the presence of the blaNDM-1 gene was revealed by short read whole genome sequencing (WGS) in three CRPA isolates belonging to ST773 in the Gauteng region, South Africa. This study further aimed to elucidate the genomic epidemiology and molecular characteristics of the blaNDM-1-positive ST773 CRPA isolates and the genetic environment of the blaNDM-1 gene.
Materials and methods
Bacterial isolates, species identification and antimicrobial susceptibility testing
Three blaNDM-1-positive P. aeruginosa isolates from a biobank collection of 82 clinical CRPA isolates at Department of Medical Microbiology, University of Pretoria, were investigated in this study (referred as “the study isolates” below). The biobank collection consisted of any consecutive P. aeruginosa isolates showing resistance to imipenem (IPM) or meropenem (MEM) during routine microbiological analysis and antimicrobial susceptibility testing (AST) by public and private diagnostic laboratories in Pretoria, South Africa, from May 2016 to September 2019. Corresponding isolate data (collection date, specimen type, hospital ward, city) of the study isolates were obtained from the diagnostic laboratories. One of the study isolates (PA-P104) was originated from a sputum specimen collected during December 2017 from a patient admitted to the general ward of a private hospital in Johannesburg, South Africa. The other two study isolates (PA-D5 and PA-A18) were originated from pus and endotracheal aspirate specimens collected during March and June 2019 from patients admitted to the intensive care unit (PA-D5) and the high care ward (PA-A18) of private hospitals in Benoni and Boksburg (situated approximately 27 km and 37 km from Johannesburg), respectively.
The routine species identification and AST were performed using the VITEK® 2 system (bioMérieux SA, Marcy l’Etoile, France) with the VITEK® GN cards (bioMérieux SA, Marcy l’Etoile, France). The tested antibiotics were piperacillin-tazobactam (TZP), ceftazidime (CAZ), cefepime (FEP), imipenem (IPM), meropenem (MEM), amikacin (AMK), gentamicin (GEN) and ciprofloxacin (CIP). An additional disc diffusion assay was performed to confirm IPM resistance for isolate PA-D5, as the VITEK minimum inhibitory concentration (MIC) was not available. Colistin (CST) MIC was determined using the broth microdilution (BMD) method. The MICs and zone diameter interpretations were as per the European Committee on Antimicrobial Susceptibility Testing (EUCAST) Clinical Breakpoints Table version 9.0 [17]. The P. aeruginosa isolates were defined as MDR if isolates were resistant to three or more tested antibiotic classes, or as XDR if isolates were resistant to all but two or less antibiotic classes, as defined by Magiorakos et al. [18]. The study was approved by the Faculty of Health Sciences Research Ethics Committee, University of Pretoria (ethics reference no. 671/2018).
Whole genome sequencing and bioinformatics analyses
Genomic DNA was extracted using the MasterPure™ Complete DNA and RNA Purification Kit (Lucigen Corporation, Middleton, WI, USA) as per manufacturer’s instructions. Libraries were prepared by using the Riptide™ High-Throughput Rapid Library Prep (HT-RLP) kit (iGenomeX, San Diego, CA, USA). Whole genome sequencing was performed on the NovaSeq™ 6000 Sequencing System (Illumina Inc., San Diego, CA, USA) with the NovaSeq™ S Prime (SP) flow cell (Illumina Inc., San Diego, CA, USA) generating 2 × 150 bp paired-end reads (at an average of 190 × sequencing depth). Raw reads were trimmed using cutadapt (–nextseq-trim = 20) [19], Trimmomatic (leading 20, trailing 20, minimum length 25) [20] and ERNE-FILTER (–min-mean-phred-quality 30 –min-phred-value-mott 30 –sensitive) [21]. De novo assembly was performed using SPAdes 3.13.0 (–phred-offset 33 -k 35,55,75,95,115,127) [22] and assembly improvement was performed using Pilon 1.22 [23]. The assembled draft genomes/contigs were annotated using Prokka 1.14.6 [24] with default databases, as well as additionally installed TIGRFAMs (database version 2021–08-02) [25] and the Pfam hidden Markov model (HMM) databases (database version 2021–03-19) [26]. Multilocus sequence typing (MLST) was performed in silico using the mlst software (https://github.com/tseemann/mlst) based on the P. aeruginosa PubMLST database (https://pubmlst.org/organisms/pseudomonas-aeruginosa) [27]. The draft genomes were screened for antibiotic resistance genes (ARGs) and virulence factor genes (VFGs) in the Comprehensive Antibiotic Resistance Database (CARD) [28] and the VFDB [29] using ABRicate 1.0.1 (https://github.com/tseemann/abricate; database version 2021–09-22). Point mutations associated with fluoroquinolone resistance in the gyrA, parC and parE genes were detected by AMRFinder [30].
For determination of the genetic environment surrounding the blaNDM-1 gene, the annotated draft genomes were further investigated for the presence of flanking transfer RNA (tRNA) genes, mobility genes (transposases and integrases), insertion sequence (IS) elements and virulence genes with the following bioinformatics tools: Artemis [31], Artemis Comparison Tool (ACT) [32], BLASTN and BLASTP searches against the NCBI nucleotide (nt) and nr databases and the UniProt Knowledgebase [33], ICEfinder [34], ISfinder [35], IslandViewer 4 webserver (http://www.pathogenomics.sfu.ca/islandviewer/) [36] (ordered against P. aeruginosa isolate ST773, accession number NZ_CP041945.1; most closely related genome according to the PathoSystems Resource Integration Center (PATRIC) Similar Genome Finder [37]) and Mauve Contig Mover [38]. Easyfig version 2.2.2 [39] was used to visualise the linear comparison between (i) the putative ICE regions, ICE6660-like and ICE6660; and (ii) the blaNDM-1-surrounding regions in the study isolates and the corresponding regions in ICE6660-like and ICE6660.
Phylogenetic analysis and calculation of the single nucleotide polymorphism difference matrix
For phylogenetic analysis, 19 complete and draft genome sequences of ST773 P. aeruginosa isolates (all available isolates that belonged to ST773 according the PATRIC website [37] as of 15 June 2021; 11 isolates were blaNDM-1-negative and eight were blaNDM-1-positive) were downloaded from the NCBI website (https://www.ncbi.nlm.nih.gov/genome/browse/#!/prokaryotes/187) (Table 1). Parsnp 1.5.6 from the Harvest Suite package [40] (with the “-x” option for filtering recombination sites based on PhiPack [41]) was used to obtain a recombination-free core genome by aligning draft genome sequences of the study isolates and the downloaded genome sequences (Table 1) against the reference genome (NZ_CP041945.1), of which prophage regions identified by PHASTER [42] were masked using the maskseq tool [43]. A recombination-free, core SNP-based maximum likelihood tree was constructed using RAxML 8.2.12 [44] with the rapid bootstrapping mode (“-f a”) and the GTRGAMMA model of nucleotide substitution, which was visualised using FigTree 1.4.4 (http://tree.bio.ed.ac.uk/software/figtree/). Branch support was estimated by 100 bootstrap replicates. The SNP difference matrix was calculated from the core genome alignment using the snp-dists 0.7.0 (https://github.com/tseemann/snp-dists). A previously suggested threshold of ≤ 37 SNP differences was used to define relatedness [45]. Hierarchical Bayesian clustering analysis was performed using fastbaps 1.0.6 [46] on the core SNP-only alignment in R 4.1.1 [47] (with the “optimise_baps” prior parameters and the “multi_res_baps” function for multi-level clustering). Clades were defined by using the first level of clustering and subclades by using the second level of clustering.
Results
General features of the study isolates collected in the Gauteng region, South Africa
Three CRPA isolates that contained the blaNDM-1 gene were investigated in this study, of which the AST results are summarised in Table 2. All three isolates were resistant to all tested antibiotics, except for colistin (an XDR phenotype), and belonged to ST773 according to MLST. The genome size of the blaNDM-1-positive ST773 isolates varied between 7 and 7.1 Mbp and had similar guanine-cytosine (GC) content (65.61% to 65.78%) (Table 2).
Genetic relatedness, resistome and virulome of the study isolates in comparison with ST773 P. aeruginosa isolates from different countries
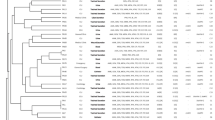
Genetic relatedness of the study isolates in comparison with the 19 downloaded ST773 P. aeruginosa isolates from the NCBI website (referred as “ST773 isolates” below) is shown in Fig. 1. The pairwise core SNP differences between the study isolates and the 19 ST773 isolates within clades and subclades are listed in Table 3. The study isolates and the ST773 isolates had 192 median SNP differences (interquartile range (IQR), 93.5–231.5), which ranged from 13 to 393 SNP differences (Table 3). The hierarchical Bayesian clustering (fastbaps) analysis identified three clades (1st level of clustering), of which the study isolates and all eight blaNDM-1-positive ST773 isolates were grouped into the same clade (clade 1; 39 median SNP differences; IQR, 30.5–152) (Fig. 1; Table 3). Eleven blaNDM-1-negative ST773 isolates were grouped into clade 2 (38 median SNP differences; IQR, 30–40) and clade 3 (119 median SNP differences; IQR, 88–126.25), consisting of three and eight isolates, respectively (Fig. 1; Table 3). The 2nd level of clustering further grouped clade 1 into four subclades (subclades 1 to 4), clade 2 into subclade 5 and clade 3 into three subclades (subclades 6 to 8) (Fig. 1; Table 3). Although subclade 1 (the study isolates) and subclade 3 (five blaNDM-1-positive ST773 isolates (PA790, ST773, PS1, PA-50010278, 15965) from India, USA, Hungary and Nigeria) were separately grouped by fastbaps, these two subclades were closely related (34 median SNP differences; 39.4 average SNP differences; SNP difference range, 13–78; IQR, 28.5–39; Fig. 1). Amongst the study isolates, isolates PA-A18 and PA-D5 were highly related (13 SNP differences), whilst isolate PA-P104 was less related to the prior two isolates (59 and 58 SNP differences with isolates PA-A18 and PA-D5) (Fig. 1).
A recombination-free maximum likelihood tree based on the core SNP alignment against the reference genome (P. aeruginosa isolate ST773, CP041945.1). Three clades and eight subclades were identified by fastbaps 1.0.6 [46]. The bold number in red indicates the within-clade median SNP differences. Each colour represents subclades with bold number showing the within-subclade median SNP differences. The study isolates are indicated in blue box. Branches with bootstrap support ≥ 87% are coloured in red. Scale bar represents number of SNPs per variable site
The study isolates harboured a wide variety of intrinsic and acquired ARGs that confer resistance to multiple antibiotics including aminoglycosides, β-lactam antibiotics (carbapenems, cephamycin, cephalosporins, monobactams), chloramphenicol, fluoroquinolones, fosfomycin, macrolides, sulfonamide, tetracycline and triclosan (Table 4). The intrinsic ARGs unique to all study isolates included blaOXA-906 (encodes an OXA-50 family β-lactamase; 99.37% (784/789 nucleotides) similar to blaOXA-395 found in the rest of ST773 isolates) and blaPDC-19b (99.66% (1190/1194 nucleotides) similar to blaPDC-385 found in the rest of ST773 isolates). In addition, isolate PA-A18 contained the dfrB5 gene conferring trimethoprim resistance, which was absent in the other two isolates. The study isolates also contained acquired ARGs specific to clade 1, which included genes encoding the aminoglycoside-modifying enzymes (aadA11), carbapenemase (blaNDM-1), quinolone resistance pentapeptide repeat protein (qnrVC1) and the major facilitator superfamily (MFS)-type efflux pumps (floR2/cmlA9).
The search against the virulence factor database (VFDB) revealed that the study isolates harbour 12 different types of VFGs, which included genes responsible for alginate production, the las and rhl quorum sensing systems, and pyochelin and pyoverdine production (iron uptake), as well as genes encoding type IV pili, flagella, lipopolysaccharide (LPS) and protein secretion systems (type II, III, IV and VI) (Table 5). The VFGs unique to the study isolates were genes encoding the VI secretion systems (hsiB1/vipA, hsiC1/vipB, hsiF1, hsiG1, hsiH1).
Genetic context of the bla NDM-1 gene
The characteristics of the putative blaNDM-1-carrying ICEs found in isolates PA-D5, PA-A18 and PA-P104 and seven blaNDM-1-positive ST773 isolates in comparison with the ICE6660 (MK497171.1) from isolate “1334/14” (CP035739.1) and the ICE6660-like from isolate PSE6684 (CP053917.1) are summarised in Table 6. The blaNDM-1 gene was found in the putative integrative and conjugative element (ICE) regions varying in sizes from ~117 to ~204 kilobase pairs (kbp), which had the same 23-bp direct repeat sequence (5ʹ-GTCTCGTTTCCCGCTCCAAACAT-3ʹ) at both terminal ends and were integrated within the tRNAGly gene (Table 6). The “variable blaNDM-1 region” (size 113,940 bp (PA-D5); 28,224 bp (PA-A18); 27,773 bp (PA-P104)), with almost identical orientation and structure except for isolates PA-D5 and PS1, was always found inserted within the DNA methyltransferase gene in all study isolates and eight ST773 isolates, as well as in ICE6660-like (29,492 bp) and ICE6660 (30,933 bp) (Fig. 2). Most notably, a unique “subregion” (85,907 bp) was found within the “variable blaNDM-1 region” in isolate PA-D5, which was absent in the other two study isolates (PA-A18 and PA-P104), eight ST773 isolates, ICE6660 and ICE6660-like. This “subregion” was completely identical (100% coverage; 100% identity) to a genomic region in the P. aeruginosa PSE6684 genome (position 2,815,086 to 2,900,992), which included a putative class 1 integron (containing the plasmid-mediated “quinolone resistance determinant” VC1 (qnrVC1) and an aminoglycoside-modifying enzyme (aadA11) gene), a Tn7 transposon and the ISPa32 (IS3 family) element.
Graphical representation of putative integrative and conjugative elements (ICEs) found in study isolates and seven blaNDM-1-positive ST773 isolates, in comparison with ICE6660-like (part of CP053917.1) and ICE6660 (MK497171.1). The image was generated by Easyfig version 2.2.2 [39]. The ICE6660-like and the ICE6660 were reversed for better comparison. Arrows indicate all genes/coding sequences (CDSs) proportional to its size and orientation. Each colour of the arrow represents type of genes as indicated in the legend. Δ indicates a truncated/incomplete gene. Grey shades show homologous regions by nucleotide BLAST comparison and the sequence identity level
Likewise, the genetic environment in the “variable blaNDM-1 region” was almost similar for two study isolates (PA-D5 and PA-A18), six ST773 isolates (15,965, PA790, PA-50010278, ST773, U1849 and U3484) and ICE6660-like (Fig. 3). The IS91 family transposase gene was almost always found downstream of the ΔISAba125-blaNDM-1-ΔbleMBL gene set, with only exception that the aminoglycoside-(3)-N-acetyltransferase III gene (aacC3) was located downstream of the ΔISAba125-blaNDM-1-ΔbleMBL gene set in isolate PA-P104 and that it was absent in isolate PS1 (Fig. 3). The ARGs specific to clade 1 (floR2/cmlA9, rmtB4, tetG) other than the blaNDM-1 and ΔbleMBL genes were always found within the “variable blaNDM-1 region” except for isolate PS1.
Comparison of the “variable blaNDM-1 region” of study isolates, seven blaNDM-1-positive ST773 isolates, ICE6660-like (part of CP053917.1) and ICE6660 (MK497171.1). The ICE6660-like and the ICE6660 blaNDM-1 regions were reversed and the isolate PA-D5 subregion was omitted for better comparison. Image was generated using Easyfig 2.2.2 [39]. Arrows indicate all genes/coding sequences (CDSs) with each colour representing each type of genes and yellow frames indicate assembly gaps. Grey shades indicate homologous regions by nucleotide BLAST comparison and the sequence identity levels. Δ indicates a truncated gene
Discussion
The emergence and worldwide dissemination of CRPA and international high-risk clones have become a major public health threat due to its ability to acquire genes producing carbapenemases, aminoglycoside-modifying enzymes and quinolone resistance determinants through HGT of MGEs such as integrons and ICEs [5, 6]. The present study describes the genomic and molecular epidemiological characteristics of three blaNDM-1-positive CRPA isolates detected in the Gauteng region, South Africa. The key findings of the study were as follows: (i) the study isolates belonged to the same clade with the blaNDM-1-positive global ST773 isolates, which shared a few clade-specific ARGs/molecular markers; (ii) the study isolates showed an XDR phenotype and had a wide range of intrinsic and acquired ARGs (including ARGs related with MGEs, porins and efflux pumps) and VFGs; and (iii) the clade-specific ARGs (blaNDM-1, floR2/cmlA9, rmtB4, tetG) were found in the similar genetic environment as in the ICE6660-like.
ST773 is an international high-risk clone associated with MDR and XDR phenotypes that produce MBLs (VIMs, IMPs, NDMs), which is widely distributed in countries like Hungary [50], India [51], Nepal [52], Nigeria [53], Saudi Arabia [54], South Korea [55], the UK [56] and the USA [57]. The core SNP-based phylogenetic analysis of the study isolates with 19 global ST773 isolates revealed that the study isolates and the eight blaNDM-1-positive ST773 isolates belonged to the same clade. Especially, the CRPA isolates were closely related (median SNP differences, 34; IQR 28.5–39; Fig. 1) to five blaNDM-1-positive ST773 isolates (PA790, ST773, PS1, PA-50010278, 15,965) from India, the USA, Hungary and Nigeria, which may indicate a recently shared origin of the study isolates with isolates from these countries. Previous hospitalisation or international travel in endemic countries such as India is an important risk factor for colonisation or infection of carbapenemase-producing, MDR or XDR Gram-negative bacteria (including NDM-producing P. aeruginosa and Enterobacterales) in returning countries (39–42). However, further investigation is required to confirm this finding as no travel history of patients was available in this study.
In the study isolates and seven blaNDM-1-positive ST773 isolates (clade 1), the blaNDM-1 gene was found within the ~117- to ~204-kbp putative ICE regions similar to the ICE6660-like. Interestingly, the majority of the clade-specific ARGs (floR2/cmlA9, rmtB4, tetG) were found in proximity with blaNDM-1 (except for isolate PS1), whilst the class 1 integrons containing aadA11 and qnrVC1 were also found within the “variable blaNDM-1 region” in isolate PA-D5. These findings may suggest that this particular blaNDM-1-positive ST773 clade may have emerged by acquiring ICEs and integrons carrying ARGs that confer resistance to aminoglycosides, carbapenems, chloramphenicol, fluoroquinolones and tetracyclines. This is consistent with previous studies that suggest the blaNDM-1 and qnrVC1 genes as molecular markers of ST773 and that there is some phylogenomic preference in the blaNDM-1 gene acquisition in P. aeruginosa [50, 55, 58]. The ICE specifically carrying the aacC3, blaNDM-1 and rmtB4 genes was first reported in the P. aeruginosa isolate “ST773” in the USA in 2019, which was obtained from a returning traveller that underwent surgery in India [59]. The ICE with the same genetic structure, composition and direct repeat sequences, designated as ICE6660-like, was also recently found in South Korea [55], Nepal [52], Saudi Arabia [54] and Nigeria [53]. The international distribution of the blaNDM-1-positive ST773 clade carrying ARGs on the genetic platforms such as ICEs warrants special attention since ICEs are self-transmissible and can facilitate intra- and intercellular mobility of ARGs [60, 61] to other carbapenem-susceptible P. aeruginosa isolates and other Gram-negative bacteria (Enterobacterales) in the same region and other countries by travelling, which may further increase the health burden caused by MDR and XDR P. aeruginosa infections.
Other than ARGs, the WGS analysis of the ST773 CRPA isolates in this study revealed a wide repertoire of cell-associated (flagella, type IV pili, alginate, LPS, type II, III, IV and VI protein secretion systems) and extracellular VFGs (proteases, phospholipase C, pyoverdine, pyochelin, pyocyanin, exotoxin A). These findings are not surprising as ST773 has often been associated with many VFGs such as aprA, algD, exoT, exoU, exoY, lasA, lasB, phzM, phzS and toxA [62, 63]. Although it is known that virulence of P. aeruginosa may be suppressed whilst being MDR or XDR as a result of the fitness cost, the exoU+-genotype STs such as ST235 have been found to be highly virulent and were associated with early mortality in patients with BSIs [64,65,66]. The presence of the exoU gene and a wide variety of VFGs in the study isolates may show the virulence potential of the blaNDM-1-positive ST773 clade, which may further pose a challenge for the recovery of critically ill patients in the hospitals.
To the authors’ knowledge, this is the first study to report genomic characteristics of blaNDM-1-positive ST773 CRPA isolates in South Africa and the genetic environment of the blaNDM-1 gene in these CRPA isolates. However, the authors acknowledge some limitations. First, BMD was performed to CST only and novel β-lactam combinations such as ceftolozane/tazobactam, ceftazidime/avibactam and cefiderocol were not tested. In South Africa, these antibiotics are not available in public sectors and are often not available due to stock issues [67]. Second, no epidemiological information (e.g. travel history) was available in this study to confirm any direct epidemiological link of the ST773 isolates. Third, draft genomes and putative ICE predictions in this study were obtained by short read sequencing only, which resulted in fragmented contigs with some assembly gaps. In future, a hybrid assembly approach using both short- and a long-read sequencing technologies such as Oxford Nanopore DNA sequencing (Oxford Nanopore Technologies, Oxford, UK) or PacBio single molecule real-time (SMRT) sequencing (PacBio®, Menlo Park, CA, USA) could be useful in obtaining complete genome sequences and sequences of longer MGEs such as ICEs and plasmids.
In conclusion, this study reports the presence of the blaNDM-1-positive ST773 clone in the Gauteng region, South Africa, and the carriage of the blaNDM-1 gene and ARGs on a putative ICE similar to ICE6660-like. Continuous and active molecular/genomic surveillance of CRPA in the Gauteng region, South Africa, is needed to monitor the emergence and spread of clones harbouring the carbapenemase gene and VFGs to prevent its establishment and transmission in healthcare settings.
Data availability
The draft genome sequences of the isolates PA-A18, PA-D5 and PA-P104 have been deposited to the public database (NCBI GenBank database) with the following accession numbers: JAVKRX000000000, JAVKRY000000000, JAVKRZ000000000, under the BioProject no. PRJNA1010667. Supporting data and protocols have been provided within the article.
Code availability
Not applicable.
References
European Centre for Disease Prevention and Control (2023) Point prevalence survey of healthcare-associated infections and antimicrobial use in European acute care hospitals, 2016–2017. European Centre for Disease Prevention and Control, Stockholm. https://www.ecdc.europa.eu/sites/default/files/documents/healthcare-associated--infections-antimicrobial-use-point-prevalence-survey-2016-2017.pdf. Accessed 12 Jul 2023
Weiner-Lastinger LM, Abner S, Edwards JR, Kallen AJ, Karlsson M, Magill SS, Pollock D, See I, Soe MM, Walters MS, Dudeck MA (2020) Antimicrobial-resistant pathogens associated with adult healthcare-associated infections: summary of data reported to the National Healthcare Safety Network, 2015–2017. Infect Control Hosp Epidemiol 41(1):1–18
Shortridge D, Gales AC, Streit JM, Huband MD, Tsakris A, Jones RN (2019) Geographic and temporal patterns of antimicrobial resistance in Pseudomonas aeruginosa over 20 years from the SENTRY Antimicrobial Surveillance Program, 1997–2016. Open Forum Infect Dis 6(Suppl 1):S63–S68
del Barrio-Tofiño E, López-Causapé C, Oliver A (2020) Pseudomonas aeruginosa epidemic high-risk clones and their association with horizontally-acquired beta-lactamases: 2020 update. Int J Antimicrob Agents 56(6):106196
Kocsis B, Gulyás D, Szabó D (2021) Diversity and distribution of resistance markers in Pseudomonas aeruginosa international high-risk clones. Microorganisms 9(2):359
van der Zee A, Kraak WB, Burggraaf A, Goessens WHF, Pirovano W, Ossewaarde JM, Tommassen J (2018) Spread of carbapenem resistance by transposition and conjugation among Pseudomonas aeruginosa. Front Microbiol 9:2057
Fusté E, López-Jiménez L, Segura C, Gainza E, Vinuesa T, Viñas M (2013) Carbapenem-resistance mechanisms of multidrug-resistant Pseudomonas aeruginosa. J Med Microbiol 62(Pt 9):1317–1325
Xu C, Wang D, Zhang X, Liu H, Zhu G, Wang T, Cheng Z, Wu W, Bai F, Jin Y (2020) Mechanisms for rapid evolution of carbapenem resistance in a clinical isolate of Pseudomonas aeruginosa. Front Microbiol 11:1390
Watanabe M, Iyobe S, Inoue M, Mitsuhashi S (1991) Transferable imipenem resistance in Pseudomonas aeruginosa. Antimicrob Agents Chemother 35(1):147–151
Kazmierczak KM, Rabine S, Hackel M, McLaughlin RE, Biedenbach DJ, Bouchillon SK, Sahm DF, Bradford PA (2016) Multiyear, multinational survey of the incidence and global distribution of metallo-β-lactamase-producing Enterobacteriaceae and Pseudomonas aeruginosa. Antimicrob Agents Chemother 60(2):1067–1078
Kindu M, Derseh L, Gelaw B, Moges F (2020) Carbapenemase-producing non-glucose-fermenting Gram-negative bacilli in Africa, Pseudomonas aeruginosa and Acinetobacter baumannii: a systematic review and meta-analysis. Int J Microbiol 2020:9461901
Wang M-G, Liu ZY, Liao XP, Sun RY, Li RB, Liu Y, Fang LX, Sun J, Liu YH, Zhang RM (2021) Retrospective data insight into the global distribution of carbapenemase-producing Pseudomonas aeruginosa. Antibiotics (Basel) 10(5):548
Wu W, Feng Y, Tang G, Qiao F, McNally A, Zong Z (2019) NDM metallo-β-lactamases and their bacterial producers in health care settings. Clin Microbiol Rev 32(2):e00115-00118
Karlowsky JA, Lob SH, Kazmierczak KM, Badal RE, Young K, Motyl MR, Sahm DF (2017) In vitro activity of imipenem against carbapenemase-positive Enterobacteriaceae isolates collected by the SMART Global Surveillance Program from 2008 to 2014. J Clin Microbiol 55(6):1638–1649
Lowman W, Sriruttan C, Nana T, Bosman N, Duse A, Venturas J, Clay C, Coetzee J (2011) NDM-1 has arrived: first report of a carbapenem resistance mechanism in South Africa. S Afr Med J 101(12):873–875
Mhlongo N, Essack S, Govinden U (2015) NDM-1, novel TEM-205, novel TEM-213 and other extended-spectrum β-lactamases co-expressed in isolates from cystic fibrosis patients from South Africa. S Afr J Infect Dis 30(3):103–107
European Committee on Antimicrobial Susceptibility Testing (2019) Breakpoint tables for interpretation of MICs and zone diameters. EUCAST, Växjö
Magiorakos A-P, Srinivasan A, Carey RB, Carmeli Y, Falagas ME, Giske CG, Harbarth S, Hindler JF, Kahlmeter G, Olsson-Liljequist B, Paterson DL, Rice LB, Stelling J, Struelens MJ, Vatopoulos A, Weber JT, Monnet DL (2012) Multidrug-resistant, extensively drug-resistant and pandrug-resistant bacteria: an international expert proposal for interim standard definitions for acquired resistance. Clin Microbiol Infect 18(3):268–281
Martin M (2011) Cutadapt removes adapter sequences from high-throughput sequencing reads. EMBnetjournal 17(1):10–12
Bolger AM, Lohse M, Usadel B (2014) Trimmomatic: a flexible trimmer for Illumina sequence data. Bioinformatics 30(15):2114–2120
Prezza N, Del Fabbro C, Vezzi F, De Paoli E, Policriti A (2012) ERNE-BS5: aligning BS-treated sequences by multiple hits on a 5-letters alphabet. BCB '12: ACM Conference on Bioinformatics, Computational Biology and Biomedicine. Association for Computing Machinery, Orlando, Florida, pp 12–19
Bankevich A, Nurk S, Antipov D, Gurevich AA, Dvorkin M, Kulikov AS, Lesin VM, Nikolenko SI, Pham S, Prjibelski AD, Pyshkin AV, Sirotkin AV, Vyahhi N, Tesler G, Alekseyev MA, Pevzner PA (2012) SPAdes: a new genome assembly algorithm and its applications to single-cell sequencing. J Comput Biol 19(5):455–477
Walker BJ, Abeel T, Shea T, Priest M, Abouelliel A, Sakthikumar S, Cuomo CA, Zeng Q, Wortman J, Young SK, Earl AM (2014) Pilon: an integrated tool for comprehensive microbial variant detection and genome assembly improvement. PLoS ONE 9(11):e112963
Seemann T (2014) Prokka: rapid prokaryotic genome annotation. Bioinformatics 30(14):2068–2069
Li W, O’Neill KR, Haft DH, DiCuccio M, Chetvernin V, Badretdin A, Coulouris G, Chitsaz F, Derbyshire MK, Durkin AS, Gonzales NR, Gwadz M, Lanczycki CJ, Song JS, Thanki N, Wang J, Yamashita RA, Yang M, Zheng C, Marchler-Bauer A, Thibaud-Nissen F (2021) RefSeq: expanding the Prokaryotic Genome Annotation Pipeline reach with protein family model curation. Nucleic Acids Res 49(D1):D1020–D1028
Mistry J, Chuguransky S, Williams L, Qureshi M, Salazar GA, Sonnhammer ELL, Tosatto SCE, Paladin L, Raj S, Richardson LJ, Finn RD, Bateman A (2021) Pfam: the protein families database in 2021. Nucleic Acids Res 49(D1):D412–D419
Jolley KA, Bray JE, Maiden MCJ (2018) Open-access bacterial population genomics: BIGSdb software, the PubMLST.org website and their applications. Wellcome Open Res 3:124
Alcock BP, Raphenya AR, Lau TTY, Tsang KK, Bouchard M, Edalatmand A, Huynh W, Nguyen AV, Cheng AA, Liu S, Min SY, Miroshnichenko A, Tran HK, Werfalli RE, Nasir JA, Oloni M, Speicher DJ, Florescu A, Singh B, Faltyn M, Hernandez-Koutoucheva A, Sharma AN, Bordeleau E, Pawlowski AC, Zubyk HL, Dooley D, Griffiths E, Maguire F, Winsor GL, Beiko RG, Brinkman FSL, Hsiao WWL, Domselaar GV, McArthur AG (2020) CARD 2020: antibiotic resistome surveillance with the comprehensive antibiotic resistance database. Nucleic Acids Res 48(D1):D517–D525
Liu B, Zheng D, Jin Q, Chen L, Yang J (2019) VFDB 2019: a comparative pathogenomic platform with an interactive web interface. Nucleic Acids Res 47(D1):D687–D692
Feldgarden M, Brover V, Haft DH, Prasad AB, Slotta DJ, Tolstoy I, Tyson GH, Zhao S, Hsu CH, McDermott PF, Tadesse DA, Morales C, Simmons M, Tillman G, Wasilenko J, Folster JP, Klimke W (2019) Validating the AMRFinder tool and resistance gene database by using antimicrobial resistance genotype-phenotype correlations in a collection of isolates. Antimicrob Agents Chemother 63(11):e00483-e419
Carver T, Harris SR, Berriman M, Parkhill J, McQuillan JA (2012) Artemis: an integrated platform for visualization and analysis of high-throughput sequence-based experimental data. Bioinformatics 28(4):464–469
Carver TJ, Rutherford KM, Berriman M, Rajandream MA, Barrell BG, Parkhill J (2005) ACT: the Artemis Comparison Tool. Bioinformatics 21(16):3422–3423
The UniProt Consortium (2021) UniProt: the universal protein knowledgebase in 2021. Nucleic Acids Res 49(D1):D480–D489
Liu M, Li X, Xie Y, Bi D, Sun J, Li J, Tai C, Deng Z, Ou HY (2019) ICEberg 2.0: an updated database of bacterial integrative and conjugative elements. Nucleic Acids Res 47(D1):D660–D665
Siguier P, Perochon J, Lestrade L, Mahillon J, Chandler M (2006) ISfinder: the reference centre for bacterial insertion sequences. Nucleic Acids Res 34(Database issue):D32–D36
Bertelli C, Laird MR, Williams KP, Simon Fraser University Research Computing Group, Lau BY, Hoad G, Winsor GL, Brinkman FSL (2017) IslandViewer 4: expanded prediction of genomic islands for larger-scale datasets. Nucleic Acids Res 45(W1):W30–W35
Davis JJ, Wattam AR, Aziz RK, Brettin T, Butler R, Butler RM, Chlenski P, Conrad N, Dickerman A, Dietrich EM, Gabbard JL, Gerdes S, Guard A, Kenyon RW, Machi D, Mao C, Murphy-Olson D, Nguyen M, Nordberg EK, Olsen GJ, Olson RD, Overbeek JC, Overbeek R, Parrello B, Pusch GD, Shukla M, Thomas C, VanOeffelen M, Vonstein V, Warren AS, Xia F, Xie D, Yoo H, Stevens R (2020) The PATRIC Bioinformatics Resource Center: expanding data and analysis capabilities. Nucleic Acids Res 48(D1):D606–D612
Rissman AI, Mau B, Biehl BS, Darling AE, Glasner JD, Perna NT (2009) Reordering contigs of draft genomes using the Mauve aligner. Bioinformatics 25(16):2071–2073
Sullivan MJ, Petty NK, Beatson SA (2011) Easyfig: a genome comparison visualizer. Bioinformatics 27(7):1009–1010
Treangen TJ, Ondov BD, Koren S, Phillippy AM (2014) The Harvest suite for rapid core-genome alignment and visualization of thousands of intraspecific microbial genomes. Genome Biol 15(11):524
Bruen TC, Philippe H, Bryant D (2006) A simple and robust statistical test for detecting the presence of recombination. Genetics 172(4):2665–2681
Arndt D, Grant JR, Marcu A, Sajed T, Pon A, Liang Y, Wishart DS (2016) PHASTER: a better, faster version of the PHAST phage search tool. Nucleic Acids Res 44(W1):W16–W21
Rice P, Longden I, Bleasby A (2000) EMBOSS: the European Molecular Biology Open Software Suite. Trends Genet 16(6):276–277
Stamatakis A (2014) RAxML version 8: a tool for phylogenetic analysis and post-analysis of large phylogenies. Bioinformatics 30(9):1312–1313
Schürch AC, Arredondo-Alonso S, Willems RJL, Goering RV (2018) Whole genome sequencing options for bacterial strain typing and epidemiologic analysis based on single nucleotide polymorphism versus gene-by-gene-based approaches. Clin Microbiol Infect 24(4):350–354
Tonkin-Hill G, Lees JA, Bentley SD, Frost SDW, Corander J (2019) Fast hierarchical Bayesian analysis of population structure. Nucleic Acids Res 47(11):5539–5549
R Core Team (2021) R: a language and environment for statistical computing. R Foundation for Statistical Computing, Vienna, Austria
Winsor GL, Griffiths EJ, Lo R, Dhillon BK, Shay JA, Brinkman FS (2016) Enhanced annotations and features for comparing thousands of Pseudomonas genomes in the Pseudomonas genome database. Nucleic Acids Res 44(D1):D646–D653
Camacho C, Coulouris G, Avagyan V, Ma N, Papadopoulos J, Bealer K, Madden TL (2009) BLAST+: architecture and applications. BMC Bioinformatics 10:421
Kocsis B, Toth A, Gulyas D, Ligeti B, Katona K, Rokusz L, Szabo D (2019) Acquired qnrVC1 and blaNDM-1 resistance markers in an international high-risk Pseudomonas aeruginosa ST773 clone. J Med Microbiol 68(3):336–338
Singh S, Pulusu CP, Pathak A, Pradeep BE, Prasad KN (2021) Complete genome sequence of an extensively drug-resistant Pseudomonas aeruginosa ST773 clinical isolate from North India. J Glob Antimicrob Resist 27:244–246
Takahashi T, Tada T, Shrestha S, Hishinuma T, Sherchan JB, Tohya M, Kirikae T, Sherchand JB (2021) Molecular characterisation of carbapenem-resistant Pseudomonas aeruginosa clinical isolates in Nepal. J Glob Antimicrob Resist 26:279–284
Olalekan A, Bader BK, Iwalokun B, Wolf S, Lalremruata A, Dike A, Mannie-Udoh M, Lo Presti L, Liese J, Guther J, D’Alvise P, Peter S (2023) High incidence of carbapenemase-producing Pseudomonas aeruginosa clinical isolates from Lagos, Nigeria. JAC Antimicrob Resist 5(2):dlad038
Doumith M, Alhassinah S, Alswaji A, Alzayer M, Alrashidi E, Okdah L, Aljohani S, Group NAS, Balkhy HH, Alghoribi MF (2021) Genomic characterization of carbapenem-non-susceptible Pseudomonas aeruginosa clinical isolates from Saudi Arabia revealed a global dissemination of GES-5-producing ST235 and VIM-2-producing ST233 sub-lineages. Front Microbiol 12:765113
Hong JS, Song W, Park MJ, Jeong S, Lee N, Jeong SH (2021) Molecular characterization of the first emerged NDM-1-producing Pseudomonas aeruginosa isolates in South Korea. Microb Drug Resist 27(8):1063–1070
Taylor E, Jauneikaite E, Sriskandan S, Woodford N, Hopkins KL (2022) Detection and characterisation of 16S rRNA methyltransferase-producing Pseudomonas aeruginosa from the UK and Republic of Ireland from 2003–2015. Int J Antimicrob Agents 59(3):106550
Alamarat ZI, Babic J, Tran TT, Wootton SH, Dinh AQ, Miller WR, Hanson B, Wanger A, Gary JL, Arias CA, Pérez N (2020) Long-term compassionate use of cefiderocol to treat chronic osteomyelitis caused by extensively drug-resistant Pseudomonas aeruginosa and extended-spectrum-β-lactamase-producing Klebsiella pneumoniae in a pediatric patient. Antimicrob Agents Chemother 64(4):e01872-e1819
Fortunato G, Vaz-Moreira I, Gajic I, Manaia CM (2023) Insight into phylogenomic bias of blaVIM-2 or blaNDM-1 dissemination amongst carbapenem-resistant Pseudomonas aeruginosa. Int J Antimicrob Agents 61(5):106788
Khan A, Shropshire WC, Hanson B, Dinh AQ, Wanger A, Ostrosky-Zeichner L, Arias CA, Miller WR (2020) Simultaneous infection with Enterobacteriaceae and Pseudomonas aeruginosa harboring multiple carbapenemases in a returning traveler colonized with Candida auris. Antimicrob Agents Chemother 64(2):e01466-e1419
Botelho J, Mourao J, Roberts AP, Peixe L (2020) Comprehensive genome data analysis establishes a triple whammy of carbapenemases, ICEs and multiple clinically relevant bacteria. Microb Genom 6(10):mgen000424
Botelho J, Schulenburg H (2021) The role of integrative and conjugative elements in antibiotic resistance evolution. Trends Microbiol 29(1):8–18
Gómez-Martínez J, Rocha-Gracia RDC, Bello-López E, Cevallos MA, Castañeda-Lucio M, Sáenz Y, Jiménez-Flores G, Cortés-Cortés G, López-García A, Lozano-Zarain P (2023) Comparative genomics of Pseudomonas aeruginosa strains isolated from different ecological niches. Antibiotics (Basel) 12(5):866
Park Y, Koo SH (2022) Epidemiology, molecular characteristics, and virulence factors of carbapenem-resistant Pseudomonas aeruginosa isolated from patients with urinary tract infections. Infect Drug Resist 15:141–151
Sánchez-Diener I, Zamorano L, López-Causapé C, Cabot G, Mulet X, Peña C, Del Campo R, Cantón R, Doménech-Sánchez A, Martínez-Martínez L, Arcos SC, Navas A, Oliver A (2017) Interplay among resistance profiles, high-risk clones, and virulence in the Caenorhabditis elegans Pseudomonas aeruginosa infection model. Antimicrob Agents Chemother 61(12):e01586-e1517
Gómez-Zorrilla S, Juan C, Cabot G, Camoez M, Tubau F, Oliver A, Dominguez MA, Ariza J, Peña C (2016) Impact of multidrug resistance on the pathogenicity of Pseudomonas aeruginosa: in vitro and in vivo studies. Int J Antimicrob Agents 47(5):368–374
Recio R, Mancheno M, Viedma E, Villa J, Orellana MA, Lora-Tamayo J, Chaves F (2020) Predictors of mortality in bloodstream infections caused by Pseudomonas aeruginosa and impact of antimicrobial resistance and bacterial virulence. Antimicrob Agents Chemother 64(2):e01759-e1719
Brink AJ, Coetzee J, Richards GA, Feldman C, Lowman W, Tootla HD, Miller MGA, Niehaus AJ, Wasserman S, Perovic O, Govind CN, Schellack N, Mendelson M (2022) Best practices: appropriate use of the new beta-lactam/beta-lactamase inhibitor combinations, ceftazidime-avibactam and ceftolozane-tazobactam in South Africa. S Afr J Infect Dis 37(1):453
Acknowledgements
The authors would like to thank Dr. Gisele Peirano from Alberta Precision Laboratories, Prof. Rebekah DeVinney and Dr. Thomas Finn from University of Calgary for assistance with the DNA extraction and for arranging the WGS service.
Funding
Open access funding provided by University of Pretoria. This study was supported by the National Health Laboratory Service Research trust (South Africa) and research grants from the JPIAMR/Canadian Institute Health Research program (no. 10016015) and National Institute of Health (no. 10028552). The funders had no role in study design, data collection and interpretation, or the decision to submit the work for publication.
Author information
Authors and Affiliations
Contributions
HJ was involved in the concept design, experimental work, data analysis and interpretation as well as the writing of the original draft and editing of the manuscript. YM was involved in data acquisition (genome assembly). JDDP is the budget owner of research grants from JPIAMR/Canadian Institute Health Research program and National Institute of Health and was involved in the concept design. K-AS and CK provided a set of carbapenem-resistant P. aeruginosa isolates for the study. MME was involved in the critical review of the manuscript. MMK is the principal investigator and the budget owner of a research grant provided by the National Health Laboratory Service Research trust, who was involved in the concept design of the study. All the authors have agreed to the submission of this draft and have critically reviewed the manuscript.
Corresponding author
Ethics declarations
Ethics approval
The study was approved by the Faculty of Health Sciences Research Ethics Committee, University of Pretoria (ethics reference no., 671/2018).
Consent to participate
Not applicable.
Consent for publication
Not applicable.
Competing interests
The authors declare no competing interests.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Rights and permissions
Open Access This article is licensed under a Creative Commons Attribution 4.0 International License, which permits use, sharing, adaptation, distribution and reproduction in any medium or format, as long as you give appropriate credit to the original author(s) and the source, provide a link to the Creative Commons licence, and indicate if changes were made. The images or other third party material in this article are included in the article's Creative Commons licence, unless indicated otherwise in a credit line to the material. If material is not included in the article's Creative Commons licence and your intended use is not permitted by statutory regulation or exceeds the permitted use, you will need to obtain permission directly from the copyright holder. To view a copy of this licence, visit http://creativecommons.org/licenses/by/4.0/.
About this article
Cite this article
Jung, H., Pitout, J.D.D., Matsumura, Y. et al. Genomic epidemiology and molecular characteristics of blaNDM-1-positive carbapenem-resistant Pseudomonas aeruginosa belonging to international high-risk clone ST773 in the Gauteng region, South Africa. Eur J Clin Microbiol Infect Dis 43, 627–640 (2024). https://doi.org/10.1007/s10096-024-04763-5
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-024-04763-5