Abstract
The induction of host defense against Candida species is initiated by recognition of the fungi by pattern recognition receptors and activation of downstream pathways that produce inflammatory mediators essential for infection clearance. In this study, we present complementary evidence based on transcriptome analysis, genetics, and immunological studies in knockout mice and humans that the cytosolic RIG-I-like receptor MDA5 (IFIH1) has an important role in the host defense against C. albicans. Firstly, IFIH1 expression in macrophages is specifically induced by invasive C. albicans hyphae, and patients suffering from chronic mucocutaneous candidiasis (CMC) express lower levels of MDA5 than healthy controls. Secondly, there is a strong association between missense variants in the IFIH1 gene (rs1990760 and rs3747517) and susceptibility to systemic Candida infections. Thirdly, cells from Mda5 knockout mice and human peripheral blood mononuclear cells (PBMCs) with different IFIH1 genotypes display an altered cytokine response to C. albicans. These data strongly suggest that MDA5 is involved in immune responses to Candida infection. As a receptor for viral RNA, MDA5 until now has been linked to antiviral host defense, but these novel studies show unexpected effects in antifungal immunity as well. Future studies are warranted to explore the potential of MDA5 as a novel target for immunotherapeutic strategies.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Candida species are one of the most common human fungal pathogens. Oropharyngeal and vaginal Candida infections are often diagnosed in the population, while systemic candidiasis is the fourth most common form of bloodstream infections in the USA, with mortality rates reaching up to 40 % [1–4]. In addition to the known risk factors (immunosuppressive medication, parenteral nutrition, prolonged intensive care hospitalization, etc.), recent studies have described several genetic risk factors that contribute to the cause and severity of systemic candidiasis [5, 6]. Several monogenic disorders that result in primary immunodeficiencies increase the susceptibility to Candida infection, as demonstrated for mutations in CARD9 and STAT1 [7–9]. Common genetic variants, for example in pattern recognition receptors (e.g., Dectin-1 and TLR1) and interleukins (e.g., IL-4, IL-10, and IL-12B), also increase the risk of infection by affecting Candida recognition and cytokine signaling [6, 10].
However, more insight is needed to identify host defense pathways that are suitable targets for novel immunotherapeutic approaches. Recently, we described that the type I interferon (IFN) pathway plays a central role in host defense against C. albicans [11]. In the present work, we demonstrate that MDA5 (IFIHI), a RIG-I-like receptor, until now described as a receptor of viral RNA that induces a signaling pathway leading to the production of type I IFNs, is directly involved in the inflammatory response against Candida infections in humans. To this end, we present complementary evidence based on transcriptome analysis, genetics, and functional immunological studies in knockout mice and in healthy humans, as well as in patients suffering from systemic candidiasis or chronic mucocutaneous candidiasis (CMC). This is the first time that a receptor of the RIG-I-like helicase family has been shown to be involved in the antifungal immune response.
Materials and methods
Transcriptome analysis of Candida-stimulated macrophages
CD14+ monocytes derived from healthy volunteers were differentiated into macrophages using macrophage colony-stimulating factor (M-CSF) for 7 days. Macrophages (2 × 105/well) were stimulated for 4 or 24 h with either culture medium, a wild-type C. albicans strain (UC820), or an HGC1 null mutant strain. This mutant is unable to form hyphae and is, therefore, locked in a yeast form, although this form does not correspond to wild-type yeast cells, as the mutant expresses several filament-specific genes [12]. As yeast–hyphal transition is considered an invasive trait of C. albicans, gene expression induced by either the wild-type (hyphae) or HGC1 null (yeast) strains was profiled and compared to unstimulated macrophages, as described previously [11]. We identified genes that showed significant differential expression in at least one of the conditions after Benjamini–Hochberg correction (p < 0.05 and >2-fold change in expression). From this set, we selected the 62 genes that are exclusively induced after stimulation with wild-type C. albicans for 24 h.
Candidemia and control cohorts
In this study, we included 227 unrelated adult Caucasian candidemia patients (described in detail in [6]). Patient enrollment took place after confirmation of at least one positive blood culture for a Candida species. The control cohort of 176 Caucasians consists of non-infected (candidiasis-free) matched patients from the same medical centers as the patient cohort. Controls were recruited consecutively from the same hospital wards as infected patients during the study period, with a similar balance of medical, surgical, and oncology patients in the case and control groups. Review boards of the involved medical centers approved the study and patients were enrolled after giving written informed consent (see Supplementary Methods).
Genotyping and genetic analyses
Cases and controls in the candidemia cohort were genotyped on the Illumina Immunochip single nucleotide polymorphism (SNP) array platform, which contains ~200,000 SNPs focused on genomic regions known to be involved in immune-mediated diseases [13]. After the application of quality control filters, we tested 843 SNPs in the FAP-IFIH1-GCA-KCNH7 linkage disequilibrium (LD) region for candidemia case–control association. This 405-kb LD region (hg18 coordinates: chr2 162,720–163,125 kb) was defined based on the LD patterns in the larger genomic region (Figure S1). See Supplementary Methods for detailed information.
Expression analysis of PBMCs
To assess the expression levels of genes in the FAP-IFIH1-GCA-KCNH7 LD region, blood was collected from healthy volunteers. Peripheral blood mononuclear cells (PBMCs, 5 × 105/well) were stimulated with either culture medium, 1 × 106/ml heat-killed Borrelia burgdorferi [14], 1 × 106/ml heat-killed Candida albicans (UC820) [15], 10 ng/ml Escherichia coli-derived lipopolysaccharide (LPS), or 1 × 107/ml sonicated Mycobacterium tuberculosis (MTB) (Hv37Rv) for either 4 or 24 h. Gene expression was profiled using the Illumina HumanHT-12 Expression BeadChip kit [11]. Additionally, gene expression was assessed in PBMCs from two patients suffering from CMC due to STAT1 mutations (Arg274Trp) [8]. Cells were stimulated with C. albicans for 4 h and gene expression was measured by RNA sequencing as described elsewhere [11].
PBMC stimulations experiments
5 × 105 isolated PBMCs per well were stimulated with either heat-killed C. albicans yeast or hyphae (UC820, 1 × 106/ml) for 24 h (IL-10) or 7 days (IL-17 and IFN-γ). Additionally, PBMCs were stimulated with MTB (1 μg/μl) for 24 h. Supernatants were collected and measured for IL-10 and IFN-γ (Sanquin, Amsterdam, The Netherlands) and IL-17 cytokines (R&D Systems, Abingdon, UK). We excluded samples that showed a positive RPMI (control condition with contamination) or errors in the experimental readout.
Mda5 knockout mice studies
Mda5 −/− mice on C57BL/6 J background have been backcrossed at least ten times and were kindly provided by Dr. M. Colonna. Splenocytes were isolated from wild-type and Mda5 −/− mice and stimulated with RPMI, Poly I:C, and heat-killed C. albicans yeasts or hyphae for 24 h. Cytokines were measured in supernatants by enzyme-linked immunosorbent assay (ELISA). For quantitative real-time polymerase chain reaction (qPCR) experiments, splenocytes from both Mda5 knockout mice and B6 control mice were stimulated for 24 h with heat-killed C. albicans hyphae. RNA was isolated according to the TRIzol® isolation protocol (Life Technologies).
Results
Candida germination induces expression of RLR pathway components in macrophages
C. albicans is a dimorphic fungus that exists either in a colonizing yeast form or as an invasive filamentous form (hyphae). To identify the specific transcription profile induced by fungal germination into hyphae, we profiled the transcriptome of macrophages stimulated with either wild-type (which develop hyphae) and HGC1 null strains of C. albicans (which have a yeast-locked phenotype, though are different from wild-type) [12]. Sixty-two genes exhibited significant differential expression specifically in macrophages stimulated with Candida hyphae for 24 h (required for hyphal formation), but not for 4 h (Benjamini–Hochberg-corrected p < 0.05 and >2-fold change in expression compared to unstimulated macrophages, Fig. 1a). Many of these genes are involved in IFN signaling, consistent with a previous study [11]. Interestingly, four of the genes induced by Candida hyphae stimulation (IFIH1, ISG15, IL8, and TRIM25) are components of the RIG-I-like receptor (RLR) signaling pathway, significantly more than expected for a random set of genes (p = 4.3 × 10−3, 11.5-fold enrichment, Table 1).
Transcriptional changes in macrophages stimulated with Candida albicans. a The heat map shows differential gene expression after 4 or 24 h of stimulation of human macrophages with yeast-locked HGC1 null C. albicans (which are unable to form hyphae, but are known to express several hyphal proteins) or wild-type invasive C. albicans (that can form hyphae) compared to expression levels in unstimulated macrophages (control). Sixty-two genes exhibited a significant change in expression level (Benjamini–Hochberg-corrected p < 0.05 and > 2fold change in expression) specifically after 24 h of stimulation with wild-type Candida, during which germination into hyphae takes place. The signal-to-noise ratio scaled to the maximum absolute deviation is shown for each probe corresponding to the 62 differentially expressed genes. b C. albicans hyphae-induced genes, IFIH1, TRIM25, ISG15, and IL8 (indicated in red), are components of the RIG-I-like receptor (RLR) signaling pathway. These genes represent both the MDA5 (IFIH1) and RIG-I (ISG15 and TRIM25) branches, as well as inflammatory cytokines that are produced by activation of the pathway (IL8). Figure based on the Kyoto Encyclopedia of Genes and Genomes (KEGG) map of the RLR pathway [16]
RIG-I-like receptors are well-known intracellular receptors of viral RNA, leading to the production of type I IFNs and proinflammatory cytokines [18]. IFIH1, with its protein product known as MDA5, is the receptor of one branch of the RLR pathway (Fig. 1b). ISG15 and TRIM25 are involved in the RIG-I branch. Thus, the invasive form of Candida induces the expression of components of two branches of the virus-recognition RLR pathway in macrophages.
Genetic variation linked to IFIH1 modulates susceptibility to candidemia
To validate a role for components of the RLR pathway in invasive Candida infection, we investigated whether genetic variation linked to IFIH1, ISG15, IL8, or TRIM25 correlates with susceptibility to candidemia in patients. Analysis of 64 SNPs associated with IFIH1 revealed strong associations (Fig. 2a and Table 2). The IFIH1 locus is present in a 405-kb region on chromosome 2 with low recombination rates (Fig. 2a) and accompanying strong linkage disequilibrium (LD) in both the candidemia cohort and the HapMap CEU population (Figs. 2b and S1) [21–23]. Besides IFIH1, the LD region contains the genes FAP, GCA, and part of KCNH7. Fifteen of the 64 SNPs in the FAP-IFIH1-GCA-KCNH7 LD region differ significantly between cases and controls (Benjamini–Hochberg-corrected genotypic p < 0.05, Table S1). The significant SNPs are distributed mainly across the central part of the LD region (Fig. 2a) and the association does not extend beyond the LD region (Figure S2).
a Regional association plot and b linkage disequilibrium (LD) map for the FAP-IFIH1-GCA-KCNH7 LD region on chromosome 2. a Sixty-four single nucleotide polymorphisms (SNPs) with minor allele frequency (MAF) > 5 % in 403 Caucasian individuals of the candidemia cohort (cases and controls together) were assessed for genotypic association with candidemia. The resulting −log10(genotypic p values) (left y-axis) are plotted as a function of genomic coordinates (hg18, x-axis). The blue diamond highlights the most significant SNP, along with its p-value (rs984971). rs1990760 and rs3747517 are the only two significant missense SNPs; both are in the coding region of IFIH1. Recombination rates, estimated from the CEU, YRI, and JPT + CHB HapMap populations (HapMap 2, Release 22) [19], are plotted to reflect the local LD structure (right y-axis, cyan line). SNPs are colored according to the degree of LD with the most significant SNP, rs984971 (R-squared, calculated across the controls in the candidemia cohort; from strong to weak LD: red: r2 ≥ 0.8; orange: 0.5 ≤ r2 < 0.8; yellow: 0.2 ≤ r2 < 0.5; white: r2 < 0.2). Genes with their direction of transcription are shown at the bottom; KCNH7 is only partly in this region. b LD patterns across the 405-kb FAP-IFIH1-GCA-KCNH7 LD region are calculated based on genotypes of control individuals in the candidemia cohort, measured using the Immunochip SNP array. The intersections of the diagonals between pairs of SNPs are colored according to the degree of LD, which is calculated as D’ and LOD: SNPs with D’ values between 0 and 1 and with LOD ≥2 are colored from white to red. Haplotype blocks (triangles with bold black borders) are regions where at least 95 % of SNPs are in strong LD, defined by high D’ values [20]. Chromosome 2 coordinates (hg18) and Entrez genes are shown at the top. The orange boxes around SNP identifiers indicate the top SNP and two IFIH1 missense SNPs significantly associated with susceptibility to candidemia (see Table 2). The corresponding R-squared LD map for the candidemia cohort is depicted in Figure S1d. See Figures S1a–c for R-squared and D’/LOD LD maps calculated based on the HapMap CEU population
An intergenic SNP between GCA and KCNH7 shows the strongest association with candidemia (rs984971, genotypic p = 2.2 × 10−5, allelic p = 2.2 × 10−4, odds of disease 0.43–0.77, Table 2). Although the Immunochip covers missense coding variants in all four genes, only IFIH1 harbors significant missense SNPs (rs1990760–Ala946Thr and rs3747517–His843Arg, which are also in strong LD with each other; HapMap CEU: D’ = 1, r2 = 0.42; candidemia cohort: D’ = 1, r2 = 0.55). Furthermore, rs1990760 and rs3747517 are quantitative trait loci (QTLs) to IFIH1 expression, with the candidemia risk alleles correlating with higher IFIH1 expression in PBMCs [22, 24]. These results suggest that IFIH1 is involved in candidemia.
IFIH1 is strongly upregulated upon Candida stimulation of PBMCs, while FAP, GCA, and KCNH7 are not
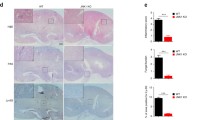
To provide additional evidence regarding which genes in the FAP-IFIH1-GCA-KCNH7 LD region are important for the host response to Candida, we assessed gene expression in PBMCs from healthy volunteers after stimulation with various microbes. Stimulation with C. albicans resulted in a strong increase of IFIH1 expression (p = 1.5 × 10−15 at 4 h and p = 1.9 × 10−12 at 24 h, Welch-corrected t-tests, Fig. 3a). Of the other LD region genes, only GCA was also weakly induced by C. albicans. In addition, we compared the expression patterns of IFIH1 in healthy individuals with two patients suffering from CMC due to a deleterious STAT1 mutation [8]. CMC patient cells expressed significantly lower levels of IFIH1 after stimulation with C. albicans than cells from healthy individuals (p = 0.04, Welch-corrected t-test, Fig. 3b), while of the other genes, only GCA also displayed minor differences (p = 0.05). Together, the observations in healthy individuals and CMC patients indicate that expression of IFIH1, and not expression of the other genes in the LD region, is specifically induced by stimulation with C. albicans.
Transcriptional response of genes in the FAP-IFIH1-GCA-KCNH7 LD region to various microbial stimuli. a Peripheral blood mononuclear cells (PBMCs) from healthy volunteers (minimum n = 23) were stimulated for either 4 or 24 h with Borrelia burgdorferi, Candida albicans, Escherichia coli-derived lipopolysaccharide (LPS), or Mycobacterium tuberculosis (MTB). Gene expression [mean ± standard deviation (SD)] was measured using microarrays and normalized to the control RPMI condition (untreated). p-Values (Welch-corrected t-test) compared expression distributions of individual stimuli to their respective untreated controls and were Bonferroni-corrected for testing 32 hypotheses (four stimuli across four genes at two time points). The asterisks represent all significant comparisons at α < 0.05. b Gene expression (mean ± SD) in PBMCs of healthy controls (n = 3) and patients suffering from chronic mucocutaneous candidiasis (CMC) (n = 2) were stimulated with C. albicans for 4 h. p-Values were calculated using the Welch-corrected t-test
Genetic variants in IFIH1 are associated with an altered cytokine profile in response to Candida
To investigate the functional consequences of genetic variants associated with IFIH1 that predispose individuals to candidemia (Table 2), we correlated the genotypes of the SNPs with in vitro cytokines levels upon Candida stimulation. A trend was observed towards an increased capacity to release the proinflammatory cytokines IFN-γ and IL-17 in cells isolated from individuals homozygous for the risk allele for both IFIH1 missense polymorphisms (TT for rs1990760; CC for rs3747517) (Fig. 4). In contrast, levels of the anti-inflammatory IL-10 tended to be lower in individuals carrying the risk allele. The top intergenic SNP associated with candidemia (rs984971) did not reveal the same trends (Figure S3). Furthermore, stimulation with other microbial stimuli did not reveal clear correlations between cytokine levels and IFIH1 missense SNP genotypes (Figure S4), suggesting specificity for Candida. Thus, genetic variation in IFIH1 may influence anti-Candida cytokine profiles in vitro.
IFIH1 missense SNP genotypes correlate with Candida-induced cytokine levels. PBMCs from healthy volunteers with different genotypes for a rs1990760 (candidemia risk allele T) and b rs3747517 (candidemia risk allele C) were stimulated in vitro with either C. albicans yeast or hyphae. Cytokine levels (scatterplots with mean indicated) were measured after 24 h (IL-10) or 7 days (IL-17 and IFN-γ) by enzyme-linked immunosorbent assay (ELISA). p-Values were calculated using the Mann–Whitney U-test comparing cytokine levels of the two homozygous genotypes
Missense SNPs could affect MDA5 protein function
We next sought to gain insight into the possible consequences of having alternative alleles at the IFIH1 missense SNPs on MDA5 protein function. In silico analysis shows that residue 946 (rs1990760, Ala946Thr) is part of an intrinsically disordered loop [25]. The equivalent loop is rigid in RIG-I, and this differential flexibility contributes to the different RNA binding preferences between MDA5 and RIG-I [26]. The human MDA5 crystal structure has an arginine at position 843 (rs3747517, His843Arg), which interacts with the negatively charged RNA backbone (Figure S5). Histidine would weaken this electrostatic interaction because it is less often positively charged at physiological pH than arginine. Furthermore, position 843 is close to the interface likely involved in interactions between MDA5 monomers (Figure S5) [26]. The formation of MDA5 filaments along the RNA is critical for downstream activation of MAVS [27] and mutation of nearby residues 841 and 842 disrupts signaling [26]. Thus, the Ala946Thr and His843Arg substitutions could alter dsRNA binding selectivity and affinity, and the latter might also affect signaling activity.
Mda5 knockout mice have reduced cytokine production in response to C. albicans
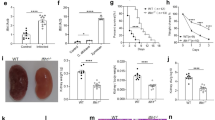
To provide an additional argument for the role of MDA5 in the anti-Candida response, we stimulated splenocytes from Mda5 knockout and B6 control mice with C. albicans yeasts or hyphae. Mda5-deficient cells showed a defective production of IFN-β induced by Candida (Fig. 5). Similarly, the IL-6 and IL-10 cytokine responses were lower in cells from Mda5 knockout mice. These differences were more pronounced in stimulations with hyphae compared to the yeast form (Figure S6).
Relative gene expression [mean ± standard error of the mean (SEM)] of mouse interferon β (mIFN-β) in splenocytes isolated from B6 control mice (C57BL/6J) and Mda5 knockout mice, upon stimulation with C. albicans hyphae (106/ml) (n = 5/group). The p-value was not significant at α < 0.05 (calculated using the Welch-corrected t-test)
Discussion
In the present study, we propose that the pattern recognition receptor MDA5, which belongs to the RLR family and plays an important role in antiviral immunity by recognizing viral RNA [18], is also involved in antifungal host defense. MDA5 modulates cytokine production induced in human leukocytes by C. albicans, while genetic variants in the IFIH1 gene that encodes MDA5 influence susceptibility to disseminated candidiasis. Based on these data and the known role of MDA5 in IFN production, it is most likely that this effect is mediated through the induction of type I IFNs.
C. albicans is a dimorphic fungus, and germination from yeasts to hyphae is a central process for the invasion of tissues. Surprisingly, transcriptome analysis aiming to identify the immunological programs induced in human macrophages specifically by Candida germination into hyphae identified the MDA5/RIG-I signaling pathway as one of the top targets. The hypothesis that MDA5 is important for host defense against Candida was strengthened by the observation that MDA5 induction is defective in cells isolated from patients suffering from CMC. Furthermore, assessment of genetic variation predisposing to candidemia in a patient cohort revealed a strong association between the disease and the genomic region that contains IFIH1. While genetic variation in IFIH1 has previously been shown to influence susceptibility to several autoimmune diseases such as type I diabetes, Graves’ disease, and multiple sclerosis [22–24, 28–33], this is the first report of polymorphisms in IFIH1 linked to a fungal infection. These data are in line with recent studies showing that polymorphisms in other pattern recognition receptors, such as TLRs [6, 34–36], or components of the IFN pathway, such as STAT1 or IRF1 [11], also influence susceptibility to systemic fungal infections.
It is important to point out that the candidemia-associated LD region contains several genes: FAP (fibroblast activation protein), IFIH1 (interferon induced with helicase C domain 1), GCA (grancalcin), and KCNH7 (potassium voltage-gated channel subfamily H member 7). IFIH1 and grancalcin were the strongest candidates for causing the susceptibility to candidemia, as these genes have known functions in immunity. Grancalcin is abundant in macrophages and neutrophils [37], and is thought to mediate leukocyte adhesion and migration [38]. Gene expression analysis confirmed that IFIH1 was strongly induced in PBMCs stimulated with Candida and GCA to lesser extent, while the other genes did not show any expression changes. IFIH1 and GCA are divergently transcribed neighboring genes with ~25 kb separating their transcription start sites. As such neighboring genes tend to be co-expressed [39, 40], the moderate upregulation of GCA in response to Candida stimulation could be a by-effect of the strong induction of IFIH1, although the genes are still relatively far apart. Importantly, grancalcin-deficient (Gca−/−) mice are not more susceptible to candidiasis than wild-type mice [41], which strongly argues against an important role for GCA in the immune response against C. albicans. Therefore, we concluded that genetic variants influencing IFIH1 are the most likely cause of the association of the FAP-IFIH1-GCA-KCNH7 LD region with candidemia.
The candidemia risk alleles of the IFIH1-linked SNPs identified in our study have previously been shown to lead to higher expression of IFIH1 in PBMCs [22, 24]. Furthermore, our protein structure analysis indicates a possibly stronger RNA binding by MDA5 through Arg843, which is encoded by the risk allele C of rs3747517. To gain insight into the downstream immunological effects of IFIH1 variants, we measured cytokine levels produced by PBMCs with different genotypes for the two IFIH1 missense SNPs (rs1990760 and rs3747517). These data indicate that cells from individuals bearing the candidemia risk alleles produce more proinflammatory cytokines (IFN-γ and IL-17) and less anti-inflammatory IL-10 in response to C. albicans yeast and hyphal forms than cells bearing the protective alleles.
These observations bring into discussion the nature of the involvement of MDA5 in the host defense against Candida. MDA5 activates the RLR pathway, leading to the production of type I IFNs during viral infections [42]. A similar biological activity during Candida stimulation was shown by our data from Mda5 knockout mouse splenocytes, which displayed a decreased capacity to induce IFN-β. A role for type I IFNs in antifungal immunity has been recently proposed [11], and MDA5 is likely the receptor that is at least partially responsible for the type I IFN induction during C. albicans infection.
Mutations leading to inherently increased expression or activity of MDA5 are likely to increase IFN production [43]. Aberrant production of type I IFNs, in turn, can cause imbalances in the immune response that are reflected in our observed alterations in the levels of other cytokines. The apparent deleterious effect of MDA5 hyperactivity on the anti-Candida host defense is consistent with observations that type I IFNs could be harmful for this response: mice defective in type I IFN receptors (Ifnar1−/− mice) are actually more resistant to systemic Candida infections [44]. This is also in line with our findings that PBMCs with the candidemia risk genotype in IFIH1 tend to release more inflammatory cytokines. The hypothesis that MDA5 has a negative effect on the anti-Candida immune response has been proven by a very recent elegant study demonstrating that Mda5 −/− mice are more resistant to disseminated candidiasis (Malireddi and Kanneganti, personal communication).
It is currently unclear which ligands cause activation of MDA5 in Candida infection. Candida is mainly recognized by cell surface pattern recognition receptors such as TLRs and C-type lectin receptors (CLRs), after which the fungus is internalized and subsequently digested in the phagolysosome [45, 46]. It is conceivable that, during this process, Candida-derived structures may leak from these organelles and enter the cytoplasm, a process described earlier for the recognition of mycobacterial peptidoglycans by the cytoplasmic receptor NOD2 [47–49]. Interestingly, a recent study has suggested that NOD2 is also important for the recognition of Candida chitin [50]. Nevertheless, there is currently no experimental evidence to support that either the wild-type form or a variant form of MDA5 has ligands other than the described RNAs.
In conclusion, this study demonstrates that the viral receptor MDA5 has an important role in modulating innate immune responses against the fungal pathogen C. albicans. Future research should shed light on the exact mechanisms through which MDA5 participates in the defense against the fungus. Nevertheless, the possible deleterious effects of MDA5-dependent stimulation during systemic candidiasis shown by our data suggest its potential usefulness as a novel therapeutic target.
References
Gudlaugsson O, Gillespie S, Lee K et al (2003) Attributable mortality of nosocomial candidemia, revisited. Clin Infect Dis 37(9):1172–1177
Wisplinghoff H, Bischoff T, Tallent SM, Seifert H, Wenzel RP, Edmond MB (2004) Nosocomial bloodstream infections in US hospitals: analysis of 24,179 cases from a prospective nationwide surveillance study. Clin Infect Dis 39(3):309–317
Miller LG, Hajjeh RA, Edwards JE Jr (2001) Estimating the cost of nosocomial candidemia in the united states. Clin Infect Dis 32(7):1110
Zaoutis TE, Argon J, Chu J, Berlin JA, Walsh TJ, Feudtner C (2005) The epidemiology and attributable outcomes of candidemia in adults and children hospitalized in the United States: a propensity analysis. Clin Infect Dis 41(9):1232–1239
Smeekens SP, van de Veerdonk FL, Kullberg BJ, Netea MG (2013) Genetic susceptibility to Candida infections. EMBO Mol Med 5(6):805–813
Plantinga TS, Johnson MD, Scott WK et al (2012) Toll-like receptor 1 polymorphisms increase susceptibility to candidemia. J Infect Dis 205(6):934–943
Glocker EO, Hennigs A, Nabavi M et al (2009) A homozygous CARD9 mutation in a family with susceptibility to fungal infections. N Engl J Med 361(18):1727–1735
van de Veerdonk FL, Plantinga TS, Hoischen A et al (2011) STAT1 mutations in autosomal dominant chronic mucocutaneous candidiasis. N Engl J Med 365(1):54–61
Liu L, Okada S, Kong XF et al (2011) Gain-of-function human STAT1 mutations impair IL-17 immunity and underlie chronic mucocutaneous candidiasis. J Exp Med 208(8):1635–1648
Babula O, Lazdāne G, Kroica J, Linhares IM, Ledger WJ, Witkin SS (2005) Frequency of interleukin-4 (IL-4) -589 gene polymorphism and vaginal concentrations of IL-4, nitric oxide, and mannose-binding lectin in women with recurrent vulvovaginal candidiasis. Clin Infect Dis 40(9):1258–1262
Smeekens SP, Ng A, Kumar V et al (2013) Functional genomics identifies type I interferon pathway as central for host defense against Candida albicans. Nat Commun 4:1342
Zheng X, Wang Y, Wang Y (2004) Hgc1, a novel hypha-specific G1 cyclin-related protein regulates Candida albicans hyphal morphogenesis. EMBO J 23(8):1845–1856
Trynka G, Hunt KA, Bockett NA et al (2011) Dense genotyping identifies and localizes multiple common and rare variant association signals in celiac disease. Nat Genet 43(12):1193–1201
Oosting M, Ter Hofstede H, Sturm P et al (2011) TLR1/TLR2 heterodimers play an important role in the recognition of Borrelia spirochetes. PLoS One 6(10):e25998
Lehrer RI, Cline MJ (1969) Interaction of Candida albicans with human leukocytes and serum. J Bacteriol 98(3):996–1004
Kanehisa M, Goto S (2000) KEGG: Kyoto Encyclopedia of Genes and Genomes. Nucleic Acids Res 28(1):27–30
da Huang W, Sherman BT, Lempicki RA (2009) Systematic and integrative analysis of large gene lists using DAVID bioinformatics resources. Nat Protoc 4(1):44–57
Takeuchi O, Akira S (2010) Pattern recognition receptors and inflammation. Cell 140(6):805–820
International HapMap Consortium, Frazer KA, Ballinger DG et al (2007) A second generation human haplotype map of over 3.1 million SNPs. Nature 449(7164):851–861
Gabriel SB, Schaffner SF, Nguyen H et al (2002) The structure of haplotype blocks in the human genome. Science 296(5576):2225–2229
Qu HQ, Marchand L, Grabs R, Polychronakos C (2008) The association between the IFIH1 locus and type 1 diabetes. Diabetologia 51(3):473–475
Liu S, Wang H, Jin Y et al (2009) IFIH1 polymorphisms are significantly associated with type 1 diabetes and IFIH1 gene expression in peripheral blood mononuclear cells. Hum Mol Genet 18(2):358–365
Smyth DJ, Cooper JD, Bailey R et al (2006) A genome-wide association study of nonsynonymous SNPs identifies a type 1 diabetes locus in the interferon-induced helicase (IFIH1) region. Nat Genet 38(6):617–619
Downes K, Pekalski M, Angus KL et al (2010) Reduced expression of IFIH1 is protective for type 1 diabetes. PLoS One 5(9)e12646
van der Lee R, Buljan M, Lang B et al (2014) Classification of intrinsically disordered regions and proteins. Chem Rev 114(13):6589–6631
Wu B, Peisley A, Richards C et al (2013) Structural basis for dsRNA recognition, filament formation, and antiviral signal activation by MDA5. Cell 152(1–2):276–289
Hou F, Sun L, Zheng H, Skaug B, Jiang QX, Chen ZJ (2011) MAVS forms functional prion-like aggregates to activate and propagate antiviral innate immune response. Cell 146(3):448–461
Chen G, Zhou D, Zhang Z et al (2012) Genetic variants in IFIH1 play opposite roles in the pathogenesis of psoriasis and chronic periodontitis. Int J Immunogenet 39(2):137–143
Yang H, Wang Z, Xu K et al (2012) IFIH1 gene polymorphisms in type 1 diabetes: genetic association analysis and genotype–phenotype correlation in Chinese Han population. Autoimmunity 45(3):226–232
Sutherland A, Davies J, Owen CJ et al (2007) Genomic polymorphism at the interferon-induced helicase (IFIH1) locus contributes to Graves’ disease susceptibility. J Clin Endocrinol Metab 92(8):3338–3341
Cen H, Wang W, Leng RX et al (2013) Association of IFIH1 rs1990760 polymorphism with susceptibility to autoimmune diseases: a meta-analysis. Autoimmunity 46(7):455–462
Martínez A, Santiago JL, Cénit MC et al (2008) IFIH1-GCA-KCNH7 locus: influence on multiple sclerosis risk. Eur J Hum Genet 16(7):861–864
Nejentsev S, Walker N, Riches D, Egholm M, Todd JA (2009) Rare variants of IFIH1, a gene implicated in antiviral responses, protect against type 1 diabetes. Science 324(5925):387–389
van der Graaf C, Kullberg BJ, Joosten L et al (2005) Functional consequences of the Asp299Gly Toll-like receptor-4 polymorphism. Cytokine 30(5):264–268
van der Graaf CA, Netea MG, Drenth IP, te Morsche RH, van der Meer JW, Kullberg BJ (2003) Candida-specific interferon-gamma deficiency and toll-like receptor polymorphisms in patients with chronic mucocutaneous candidiasis. Neth J Med 61(11):365–369
Van der Graaf CA, Netea MG, Morré SA et al (2006) Toll-like receptor 4 Asp299Gly/Thr399Ile polymorphisms are a risk factor for Candida bloodstream infection. Eur Cytokine Netw 17(1):29–34
Liu F, Shinomiya H, Kirikae T, Hirata H, Asano Y (2004) Characterization of murine grancalcin specifically expressed in leukocytes and its possible role in host defense against bacterial infection. Biosci Biotechnol Biochem 68(4):894–902
Lollike K, Johnsen AH, Durussel I, Borregaard N, Cox JA (2001) Biochemical characterization of the penta-EF-hand protein grancalcin and identification of L-plastin as a binding partner. J Biol Chem 276(21):17762–17769
Trinklein ND, Aldred SF, Hartman SJ, Schroeder DI, Otillar RP, Myers RM (2004) An abundance of bidirectional promoters in the human genome. Genome Res 14(1):62–66
Michalak P (2008) Coexpression, coregulation, and cofunctionality of neighboring genes in eukaryotic genomes. Genomics 91(3):243–248
Roes J, Choi BK, Power D, Xu P, Segal AW (2003) Granulocyte function in grancalcin-deficient mice. Mol Cell Biol 23(3):826–830
Kato H, Takeuchi O, Sato S et al (2006) Differential roles of MDA5 and RIG-I helicases in the recognition of RNA viruses. Nature 441(7089):101–105
Rice GI, del Toro Duany Y, Jenkinson EM et al (2014) Gain-of-function mutations in IFIH1 cause a spectrum of human disease phenotypes associated with upregulated type I interferon signaling. Nat Genet 46(5):503–509
Majer O, Bourgeois C, Zwolanek F et al (2012) Type I interferons promote fatal immunopathology by regulating inflammatory monocytes and neutrophils during Candida infections. PLoS Pathog 8(7):e1002811
Netea MG, Gow NA, Munro CA et al (2006) Immune sensing of Candida albicans requires cooperative recognition of mannans and glucans by lectin and Toll-like receptors. J Clin Invest 116(6):1642–1650
Djeu JY (1990) Role of tumor necrosis factor and colony-stimulating factors in phagocyte function against Candida albicans. Diagn Microbiol Infect Dis 13(5):383–386
Ferwerda G, Girardin SE, Kullberg BJ et al (2005) NOD2 and toll-like receptors are nonredundant recognition systems of Mycobacterium tuberculosis. PLoS Pathog 1(3):279–285
Rahman A, Sobia P, Gupta N, Kaer LV, Das G (2014) Mycobacterium tuberculosis subverts the TLR-2-MyD88 pathway to facilitate its translocation into the cytosol. PLoS One 9(1):e86886
Stamm LM, Morisaki JH, Gao LY et al (2003) Mycobacterium marinum escapes from phagosomes and is propelled by actin-based motility. J Exp Med 198(9):1361–1368
Wagener J, Malireddi RK, Lenardon MD et al (2014) Fungal chitin dampens inflammation through IL-10 induction mediated by NOD2 and TLR9 activation. PLoS Pathog 10(4):e1004050
Acknowledgments
We thank Martin Oti for the helpful discussions. MJ and MGN were supported by an ERC Consolidator Grant (nr. 310372 to MGN). RvdL and MAH were supported by the Virgo Consortium, funded by the Dutch government (FES0908), and by the Netherlands Genomics Initiative (050-060-452). CW was supported by the ERC Advanced Grant, ERC-671274. XW was supported by NSFC 11101321 and NSFC 61263039 grants.
Conflict of interest
The authors declare that they have no conflict of interest.
Author information
Authors and Affiliations
Corresponding author
Additional information
M. Jaeger, R. van der Lee, and S.-C. Cheng contributed equally to this work.
Electronic supplementary material
Below is the link to the electronic supplementary material.
ESM 1
(DOCX 7.91 mb)
Rights and permissions
About this article
Cite this article
Jaeger, M., van der Lee, R., Cheng, SC. et al. The RIG-I-like helicase receptor MDA5 (IFIH1) is involved in the host defense against Candida infections. Eur J Clin Microbiol Infect Dis 34, 963–974 (2015). https://doi.org/10.1007/s10096-014-2309-2
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10096-014-2309-2