Abstract
Objective
To report a Chinese family with combined m.14459G>A mutation and m.6064A>T mutation of which the female proband presenting unique Leber hereditary optic neuropathy and dystonia (LDYT) overlapping mitochondrial encephalomyopathy with lactic acidosis and stroke-like episodes (MELAS) phenotype.
Methods
Clinical information of the pedigree was collected. We performed muscle biopsy and whole-length mitochondrial DNA (mtDNA) sequencing on the proband. The activity of respiratory chain complexes in immortalized lymphoblasts was determined.
Results
The current 23-year-old proband suffered from vision decline at age 15 and developed seizures and dystonia with bilateral lesions in precentral gyri at age 18. When she was 21, the lesions in bilateral putamen were found with elevated cerebrospinal fluid lactate. Her mother had optic atrophy; one of her brother died at age 4 with respiratory distress; and the other 8-year-old brother was asymptomatic. Muscle biopsy of the proband was unremarkable. The mtDNA sequencing revealed a heteroplasmic m.14459G>A mutation and a previously unreported m.6064A>T mutation. The respiratory chain complex I activity in the proband’s immortalized lymphoblasts was 50% less than the normal control; while there was no statistical difference between the proband and the normal control in the activity of complex IV.
Conclusions
We presented the first case exhibiting LDYT and MELAS phenotype with m.14459G>A mutation, and the decreased complex I activity contributed to the pathogenicity. Our study expanded the clinical spectrum of m.14459G>A mutation.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Mitochondrial DNA (mtDNA) mutations are associated with a broad spectrum of clinical disorders. The G to A transition at nucleotide position 14459 in mtDNA leads to substitution of alanine to valine at amino acid residue 72 within evolutionarily conserved region of NADH dehydrogenase subunit 6 (ND6) in mitochondrial respiratory chain (MRC) complex I, which plays important roles in electron transfer, electrochemical gradient maintenance, and reactive oxygen species (ROS) generation [1]. The clinical phenotypes of complex I deficiency are heterogeneous.
In 1994, m.14459G>A mutation was first reported in a Hispanic family of which the affected individuals expressed Leber hereditary optic neuropathy (LHON), early-onset dystonia, or LHON and dystonia (LDYT), and others were asymptomatic [2]. LHON is characterized by bilateral painless visual loss, acute or subacute, occurring in the young adult life, and males are predominantly affected [3,4,5]. To date, the most prevalent variations for LHON are m.11778G>A, m.3460G>A, and m.14484T>C mutations, located in MT-ND4, MT-ND1, and MT-ND6 genes, respectively, accounted for approximately 90–95% of all the reported cases (http://www.mitomap.org/). The m.14459G>A mutation is rare for LHON. A study of 1218 Chinese Han LHON patients revealed that the m.14459G>A mutation was present in only one patient (0.08%) [6]. Dystonia is also a phenotype of m.14459G>A mutation. The patients with m.14459G>A mutation usually have focal dystonia younger than 5 years of age, which is gradually progressed to generalized dystonia [7]. In addition, the carriers with m.14459G>A mutation could have the phenotype of Leigh syndrome (LS) with a poor prognosis [8, 9].
Here we describe a Chinese family with combined m.14459G>A mutation and m.6064A>T mutation, and the proband developed a LDYT overlapping mitochondrial encephalomyopathy with lactic acidosis and stroke-like episodes (MELAS) phenotype that has not been reported to our knowledge.
Methods
Subjects
The proband and her family members gave informed consent, and our study was approved by the Ethic Committees of Qilu Hospital of Shandong University. A comprehensive medical history, physical examination, ophthalmic examination, and neuroimaging data of the proband were collected.
Muscle biopsy
A muscle biopsy from the left biceps brachii was performed on the proband. Muscle serial frozen sections, 6 μm in thickness, were stained with hematoxylin and eosin (H&E), nicotinamide adenine dinucleotide hydrogen (NADH)-tetrazolium reductase, modified Gomori trichrome (MGT), cytochrome c oxidase (COX), succinate dehydrogenase (SDH), SDH/COX.
Mitochondrial DNA sequencing
The total DNA was extracted from peripheral blood, urinary sediment, buccal smears, and/or biopsied muscle samples of the proband and her family members by TIANamp Genomic DNA Kit (TIANGEN, China) according to the manufacturer’s protocol. The whole mitochondrial genome sequencing from the proband’s blood sample was performed using the next generation sequencing. The Sanger screening was used to identify m.14459G>A and m.6064A>T mutations as previously described [10].
Respiratory chain enzyme activity assays of immortalized lymphoblastic cell lines
Leukocytes from the proband and healthy normal control were transformed with the Epstein-Barr virus as previously detailed [11]. The generated lymphoblasts were immortalized. The cell lines were grown in RPMI 1640 media (Gibco) with 10% fetal bovine serum (FBS).
The enzymatic activities determination including MRC complex I (NADH-ubiquinone oxidoreductase), II (succinate dehydrogenase), IV (cytochrome c oxidase), and citrate synthase of immortalized lymphoblasts between the proband and the normal control were completed by spectrophotometric method as described before [12].
Statistical analysis
The statistical analysis was performed using SPSS 22.0 software (IBM, USA). Numerical variables were presented with mean ± standard deviation. The unpaired t test was used to compare the values between the proband and the normal control. A p value < 0.05 was considered statistically significant.
Results
Clinical features
The current 23-year-old female proband (III1, Fig. 1a) had rough development milestones compared with the peers. She originally complained of painless vision decline in both eyes at age 15. In the local hospital, she was diagnosed with optic neuritis and optic atrophy and received prednisone therapy. The visual acuity was only slightly promoted. At the age of 18, she suffered from a tonic-clonic seizure on the bus, and then, she was admitted to our hospital. The electroencephalogram showed short bursts of theta on vertex and bilateral frontal regions. No clear epileptiform activity was found. The lactic acid level of cerebrospinal fluid was elevated to 2.7 mmol/L (normal value 1.2–2.1 mmol/L). The levels of urine organic acid, blood lactate, blood amino acid, and acylcarnitines were normal. Since then, she showed an onset of dystonia mainly manifested in the right upper limb and left lower limb. The brain MRI demonstrated symmetric abnormal high signals in the bilateral precentral gyri on diffusion-weighted images (DWI) and T2-weighted images (T2WI) without post-contrast enhancement, which were roughly unchanged on follow-up MRI performed 3 months later (Fig. 2a–d). Her parents were not consanguineous. Her mother (II5) had visual acuity of 7/10 and 8/10 in the left and right eye, respectively, with pale optic disks. One of her brother (III2) died at age 4 with respiratory distress, and the other 8-year-old brother (III3) was asymptomatic up to now.
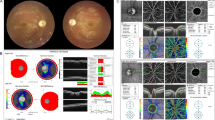
The pedigree (a) and optical coherence tomography (OCT) examination (b) of the proband. III1 was the proband. The proband’s mother (II5) had optic atrophy. The proband’s brother (III2) died at age 4 with respiratory distress. The OCT showed the retinal nerve fiber layer (RNFL) thickness of the proband at diameter: 3.45 mm from the center of optic discs, which was diffusely thinner than the normal except the superior nasal (SN) quadrant
Brain MRI findings of the proband. There were hyperintense lesions in the precentral gyri on DWI (a, b) and T2-FLAIR(c, d), without basal ganglia involvement at age 18. The bilateral precentral gyrus lesions turned to be isointense on DWI (e); meanwhile, the hyperintense lesions appeared in putamen on DWI (f), T2WI (g), and T2-FLAIR (h) at age 22. Arrows indicated the lesions
The proband had a height of 160 cm and a weight of 60 kg at age 22. Neurological examinations revealed dystonia and mildly reduced muscle strength in the right upper limb and left lower limb, especially in the former. There was also intention tremor in the right upper limb. The Babinski sign and meningeal irritation signs were absent. Her score of mini-mental state examination was 28 with the left hand writing. On ophthalmic examination, the visual acuity was 1/10 in both eyes. Fundus photography revealed temporal pallor in the optic disks. The thickness of retinal nerve fiber layer (RNFL) is diffusely reduced except the superior nasal section on optical coherence tomography (OCT) examination (Fig. 1b). The visual field tests showed central scotoma. The brain MRI demonstrated hyperintense lesions in the bilateral basal ganglia and precentral gyri on T2WI and T2-fluid-attenuated inversion recovery imaging (T2-FLAIR); in addition, the DWI signal abnormality was resolved in the precentral gyri (Fig. 2e–h). It was roughly the same as the manifestation of the brain MRI performed 5 months ago when she was 21.
Over the past 4 years, she received treatment with coenzyme Q10, vitamin B1, vitamin B2, clonazepam, and levetiracetam with the diagnosis of LDYT and MELAS. She had tonic-clonic seizures, unstable walking, and involuntary movement in the right upper limb and left lower limb. The basic activities of daily living were maintained almost independently.
Histopathological study
A biopsy of left biceps brachii from the proband showed no necrosis, regenerating or inflammatory features on H&E staining. – There were no convincing ragged red fibers on MGT staining, or ragged blue fibers on SDH/COX staining; COX staining revealed no COX-deficient fibers. Slight mitochondrial accumulations and mildly intensive SDH and COX activity were observed in subsarcolemmal regions of muscle fibers (Fig. 3). This muscle sample exhibited no muscle denervation atrophy or fiber type grouping.
Histopathological study in frozen sections of the biopsied muscle of the proband. H&E stain showed a mild variation in fiber size (a). Slightly red-stained mitochondrial accumulations in subsarcolemmal regions of few muscle fibers were observed on MGT stain (b). Mildly intensive activity was observed in subsarcolemmal regions on SDH (c) and COX stain (d)
Genetic analysis
The whole-length mtDNA sequencing of the proband identified a m.14459G>A mutation and a previously unreported m.6064A>T mutation. The heteroplasmy of m.14459G>A mutation was at the levels of 39.1% in blood, 88.1% in urine, 80.8% in buccal mucosa, and 94% in the biopsied muscle. The proportions of m.6064A>T mutation determined in blood, urine, buccal mucosa, and muscle were 97.7 %, 96.6%, 100%, and 95.7%, respectively. The mother (II5) had m.14459G>A and m.6064A>T mutant load at 13.5% and 93%, respectively, in blood. The m.14459G>A and m.6064A>T mutation rates were 15.5% and 93% in blood from the younger brother (III3).
Decreased activity of complex I
The activity of MRC complex I from the proband’s immortalized lymphoblastic cells with m.14459G>A and m.6064A>T mutations is reduced to 50% of the normal control (p < 0.01, Fig. 4). There is no statistical difference between the proband and the normal control in the activities of complex II and IV (p > 0.05, Fig. 4).
Discussion
In this study, we present the first case of a Chinese female exhibiting previously unreported LDYT and MELAS phenotype with m.14459G>A mutation. This mutation has been so far reported in patients with LHON, LDYT, dystonia, or LS, and asymptomatic individuals. A literature review about the clinical and genetic features of m.14459G>A mutation is summarized in Table 1.
LHON is characterized by midlife onset, acute painless central vision loss in one eye, and then the contralateral eye within weeks or months [26]. Some patients also experience vision loss in both eyes simultaneously. At the acute stage of LHON, fundus examination could reveal peripapillary telangiectasia and swelling of RNFL near optic discs [5]. The optic atrophy and thinning of RNFL were observed during chronic stage [5, 26]. The central visual field and color vision could have a certain recovery even many years later in some patients. The m.14459G>A mutation was considered rare for LHON. It has been more than 6 years since the painless vision declined until the proband received detailed ophthalmologic examination in our hospital. The presentation of low visual acuity, thinning RNFL, and central scotoma of the proband was compatible with the diagnosis of LHON at the chronic stage.
Our proband suffered from dystonia at age 18, whereas the dystonia associated with m.14459G>A mutation typically developed before 5 years of age and progressed gradually from focal to generalized [5, 7, 13, 14, 16, 17]. Brain MRI of the patients with m.14459G>A related dystonia may show symmetrical lesions in the putamen, caudate nucleus, or globus pallidum [2, 5, 7, 13,14,15,16,17,18].
LDYT is an association of LHON with progressive dystonia. The most frequent genetic defect in LDYT was m.14459G>A mutation. As mentioned above, in LDYT, the involvement of visual pathway was generally later in contrast to that occurred in the early-onset childhood dystonia [19, 20]. LDYT patients harboring m.14459G>A mutation usually exhibited the characteristic neuroradiological findings of abnormal signal intensity in the bilateral striatum [19,20,21]. Unlike the typical cases in literature, our present proband developed vision decline at age 15 and dystonia at 18. The dystonia didn’t significantly affect her daily life currently at age 23. Apart from juvenile-onset LHON and late-onset dystonia, she presented with seizures in adulthood without cognitive dysfunction. The lactate level of cerebrospinal fluid was elevated. Additionally, the brain MRI showed only abnormal signals in the bilateral precentral gyri/cortex without basal ganglia involvement at the early stage and the hyperintense signals on DWI that lasted for more than 3 months. The symmetrical lesions in bilateral putamen appeared later; meanwhile, the previous lesions in precentral gyri turned to be isointense on DWI. Therefore, this patient was diagnosed with LDYT overlapping MELAS.
In our present study, the genetic sequencing confirmed the heteroplasmic m.14459G>A mutation in MT-ND6 gene, with a mutant load of 39.1% in the proband’s blood. This mutation alters the structure of ND6 polypeptide and leads to the incorrect assembly of MRC complex I subunits, affecting the electron transfer function of complex I in oxidative phosphorylation. By fusing the cytoplasts from Epstein-Barr virus-transformed lymphoblast cell lines to mtDNA-less ρ0 cell lines, Jun et al. found a reduction in complex I activity of cybrids harboring the m.14459G>A mutation and speculated that the mutation might alter the coenzyme Q-binding site of complex I through polarographic and kinetic analysis [27]. As shown in Fig. 4, we found decreased complex I activity in the proband’s immortalized lymphoblastic cells, in accord with the result of the previous study [27].
Our present study found that the proband’s mother (II5) manifested a mild visual disturbance with optic atrophy, and the little brother (III3) was asymptomatic. Gene analysis identified the heteroplasmy of m.14459G>A mutations at levels of 13.5% and 15.5% in their blood, respectively. The low mutant load might contribute to the phenotypic heterogeneity. However, this threshold effect of mutation rate cannot completely explain their phonotypic manifestations, since some of the other carriers with homoplasmic m.14459G>A mutation reported in literature were asymptomatic. The heteroplasmy level of m.14459G>A mutation in some other affected tissues such as optic nerve pathway and basal ganglia would be informative but was unknown in our present study yet. In literature, the reported carriers with m.14459G>A mutation from different races had various mtDNA haplotypes, nuclear genetic background, and environment factors, which may modify the clinical presentations as well [9, 22].
Also in our present study, a novel m.6064A>T mutation in MT-CO1 gene was found in samples extracted from the proband, her mother and little brother. The m.6064A>T mutation can lead to the substitution of tyrosine to phenylalanine at the 54 amino acid in COI subunit of MRC complex IV. This mutation was relatively conserved in species, but the activity of complex IV in immortalized lymphoblast was not decreased. And actually, the unaffected brother harbored almost homoplasmic m.6064A>T mutation. Therefore, the m.6064A>T mutation in itself may be non-pathogenic. In addition, this mutation is not a haplogroup-defining variant which appears to have an effect on the penetrance of LHON. However, the potential pathogenic role of the secondary mutation cannot be completely ruled out. It is reported that some secondary mutations may have additive and synergetic effects on the phenotype of the primary pathogenic mutations [28, 29]. Hence, the potential pathogenic effect of m.6064A>T mutation still needs to be explored.
Conclusion
In conclusion, we reported a unique overlapping phenotype of LDYT and MELAS with m.14459G>A mutation in a Chinese family. The decreased activity of MRC complex I was involved in the mechanism of this particular phenotype. In addition, the co-existing m.6064A>T mutation might influence the clinical phenotype with m.14459G>A mutation, which needs to be elucidated in future studies.
References
Fassone E, Rahman S (2012) Complex I deficiency: clinical features, biochemistry and molecular genetics. J Med Genet 49(9):578–590
Jun AS, Brown MD, Wallace DC (1994) A mitochondrial DNA mutation at nucleotide pair 14459 of the NADH dehydrogenase subunit 6 gene associated with maternally inherited Leber hereditary optic neuropathy and dystonia. Proc Natl Acad Sci U S A 91(13):6206–6210
Wallace DC, Lott MT (2017) Leber hereditary optic neuropathy: exemplar of an mtDNA disease. Handb Exp Pharmacol 240:339–376
Wallace DC, Singh G, Lott MT, Hodge J, Schurr T, Lezza A, Elsas L, Nikoskelainen E (1988) Mitochondrial DNA mutation associated with Leber’s hereditary optic neuropathy. Science 242(4884):1427–1430
Shoffner JM, Brown MD, Stugard C, June AS, Pollock S, Haas RH, Kaufman A, Koontz D, Kim Y, Graham JR, Smith E, Dixon J, Wallace DC (1995) Leber’s hereditary optic neuropathy plus dystonia is caused by a mitochondrial DNA point mutation. Ann Neurol 38(2):163–169
Liang M, Jiang P, Li F, Zhang J, Ji Y, He Y, Xu M, Zhu J, Meng X, Zhao F, Tong Y, Liu X, Sun Y, Zhou X, Mo JQ, Qu J, Guan MX (2014) Frequency and spectrum of mitochondrial ND6 mutations in 1218 Han Chinese subjects with Leber’s hereditary optic neuropathy. Invest Ophthalmol Vis Sci 55(3):1321–1331
Kim I-S, Ki C-S, Park K-J (2010) Pediatric-onset dystonia associated with bilateral striatal necrosis and G14459A mutation in a Korean family: a case report. J Korean Med Sci 25(1):180–184
Kirby DM, Kahler SG, Freckmann ML, Reddihough D, Thorburn DR (2000) Leigh disease caused by the mitochondrial DNA G14459A mutation in unrelated families. Ann Neurol 48(1):102–104
Ronchi D, Cosi A, Tonduti D et al (2011) Clinical and molecular features of an infant patient affected by Leigh disease associated to m.14459G > A mitochondrial DNA mutation: a case report. BMC Neurol 11(1):85
Zhang M, Zhou X, Li C, Zhao F, Zhang J, Yuan M, Sun YH, Wang J, Tong Y, Liang M, Yang L, Cai W, Wang L, Qu J, Guan MX (2010) Mitochondrial haplogroup M9a specific variant ND1 T3394C may have a modifying role in the phenotypic expression of the LHON-associated ND4 G11778A mutation. Mol Genet Metab 101(2-3):192–199
Miller G, Lipman M (1973) Release of infectious Epstein-Barr virus by transformed marmoset leukocytes. Proc Natl Acad Sci U S A 70(1):190–194
Birch-Machin MA, Turnbull DM (2001) Assaying mitochondrial respiratory complex activity in mitochondria isolated from human cells and tissues. Methods Cell Biol 65:97–117
Koide A, Ozawa H, Kubota M, Goto Y (2014) Childhood-onset progressive dystonia with mitochondrial DNA G14459A mutation. Child Neurol Open 1(1):2329048X1455067
Hirayanagi K, Okamoto Y, Takai E, Ishizawa K, Makioka K, Fujita Y, Kaneko Y, Tanaka M, Takashima H, Ikeda Y (2017) Bilateral striatal necrosis caused by a founder mitochondrial 14459G > A mutation in two independent Japanese families. J Neurol Sci 378:177–181
Brady L, Sadikovic B, Rupar CA, Tarnopolsky MA (2019) Complete elimination of a pathogenic homoplasmic mtDNA mutation in one generation. Mitochondrion 45:18–21
Gropman A, Chen TJ, Perng CL, Krasnewich D, Chernoff E, Tifft C, Wong LJC (2004) Variable clinical manifestation of homoplasmic G14459A mitochondrial DNA mutation. Am J Med Genet A 124A(4):377–382
Kurt YG, Çoku J, Akman HO et al (2016) A de novo mutation in MTND6 causes generalized dystonia in 2 unrelated children. Child Neurol Open 3:2329048X15627937
Tarnopolsky MA, Baker SK, Myint T, Maxner CE, Robitaille J, Robinson BH (2004) Clinical variability in maternally inherited leber hereditary optic neuropathy with the G14459A mutation. Am J Med Genet A 124A(4):372–376
Watanabe M, Mita S, Takita T, Goto YI, Uchino M, Imamura S (2006) Leber’s hereditary optic neuropathy with dystonia in a Japanese family. J Neurol Sci 243(1-2):31–34
Saracchi E, Difrancesco JC, Brighina L et al (2013) A case of Leber hereditary optic neuropathy plus dystonia caused by G14459A mitochondrial mutation. Neurol Sci 34(3):407–408
Cui S, Yang L, Jiang H, Peng J, Shang J, Wang J, Zhang X (2020) Clinical features of chinese sporadic leber hereditary optic neuropathy caused by rare primary mtDNA mutations. J Neuroophthalmol 40(1):30–36
Funalot B, Reynier P, Vighetto A, Ranoux D, Bonnefont JP, Godinot C, Malthièry Y, Mas JL (2002) Leigh-like encephalopathy complicating Leber’s hereditary optic neuropathy. Ann Neurol 52(3):374–377
Lee JS, Kim H, Lim BC, Hwang H, Choi J, Kim KJ, Hwang YS, Chae JH (2016) Leigh syndrome in childhood: neurologic progression and functional outcome. J Clin Neurol 12(2):181–187
Wei Y, Cui L, Peng B (2018) Mitochondrial DNA mutations in late-onset Leigh syndrome. J Neurol 265(10):2388–2395
Yu XL, Yan CZ, Ji KQ, Lin PF, Xu XB, Dai TJ, Li W, Zhao YY (2018) Clinical, neuroimaging, and pathological analyses of 13 Chinese Leigh syndrome patients with mitochondrial DNA mutations. Chin Med J 131(22):2705–2712
Ueda K, Morizane Y, Shiraga F, Shikishima K, Ishikawa H, Wakakura M, Nakamura M (2017) Nationwide epidemiological survey of Leber hereditary optic neuropathy in Japan. J Epidemiol 27(9):447–450
Jun AS, Trounce IA, Brown MD, Shoffner JM, Wallace DC (1996) Use of transmitochondrial cybrids to assign a complex I defect to the mitochondrial DNA-encoded NADH dehydrogenase subunit 6 gene mutation at nucleotide pair 14459 that causes Leber hereditary optic neuropathy and dystonia. Mol Cell Biol 16(3):771–777
Johns DR, Smith KH, Savino PJ, Miller NR (1993) Leber’s hereditary optic neuropathy. Clinical manifestations of the 15257 mutation. Ophthalmology 100(7):981–986
Bi R, Logan I, Yao Y-G (2017) Leber hereditary optic neuropathy: a mitochondrial disease unique in many ways. Handb Exp Pharmacol 240:309–336
Acknowledgments
The authors thank the proband and her family for giving consent, samples, and additional information for this study.
Funding
This work was supported by the National Natural Science Foundation of China (No. 81671235 and No. 81701237), People's benefit project of science and technology in Qingdao (16-6-2-1-nsh), Qingdao Key Health Discipline Development Fund and the Taishan Scholars Program of Shandong Province.
Author information
Authors and Affiliations
Corresponding authors
Ethics declarations
Conflict of interest
The authors declare no competing interests
Ethical approval
None
Additional information
Publisher’s note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary Information
ESM 1
(PDF 113 kb)
Rights and permissions
About this article
Cite this article
Yu, X., Ji, K., Lin, Y. et al. Leber hereditary optic neuropathy and dystonia overlapping mitochondrial encephalomyopathy with lactic acidosis and stroke-like episodes due to m.14459G>A mutation. Neurol Sci 42, 5123–5130 (2021). https://doi.org/10.1007/s10072-021-05155-9
Received:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10072-021-05155-9