Abstract
This overview of reviews aimed to synthesize the effectiveness of non-pharmacological approaches to enhance self-efficacy in people with osteoarthritis. The CINAHL, Embase, PsycINFO, PubMed, SPORTDiscus, and the Cochrane Library databases were searched from inception to December 2023. We considered systematic reviews with meta-analysis of randomized clinical trials evaluating any non-pharmacological intervention. We used AMSTAR 2 to assess the methodological quality of reviews. The overlap between reviews was calculated. We included eight systematic reviews with meta-analysis evaluating 30 different clinical trials. Overall, mind–body exercises, psychological interventions, and self-management strategies may improve arthritis self-efficacy. Specifically, the meta-analyses showed tai chi exercises, coping skills training, and the arthritis self-management program are more effective than controls to enhance arthritis self-efficacy in people with hip and/or knee osteoarthritis. In addition, inconsistent results were detected across meta-analyses regarding the effectiveness of multidisciplinary interventions. Finally, the degree of overlap between all reviews was moderate (CCA = 6%) and many included reviews reported most of the items of AMSTAR 2. Tai chi exercises, coping skills training, and the arthritis self-management program may be beneficial for enhancing arthritis self-efficacy. Open Science Framework Registration: https://doi.org/10.17605/OSF.IO/VX2T6.
Similar content being viewed by others
Avoid common mistakes on your manuscript.
Introduction
Osteoarthritis is a chronic disease that mainly causes cartilage degradation, acute and chronic synovial inflammation, subchondral bone alteration, and osteophytes [1]. Osteoarthritis is probably the most common type of arthritis along with rheumatoid arthritis. In 2020, 595 million people reported this condition, entailing an increase of 132% in comparison to 1990. The prevalence of osteoarthritis is higher in women and in those individuals over 70 years. [2] In addition, osteoarthritis is an important cause of general practitioner consultations, admissions to hospitals, suicide ideation, and all-cause mortality [3, 4].
A large number of pharmacological and non-pharmacological interventions have been proposed in osteoarthritis [5,6,7]. The European League Against Rheumatism (EULAR) recommends that non-pharmacological approaches should be focused on improving lifestyle habits in people with hip and knee osteoarthritis, using strategies such as education, tailored exercise, and behavior change techniques [8]. EULAR has also recommended that self-management approaches may be useful in hand osteoarthritis [9], and self-efficacy beliefs have emerged as a core part in the design of self-management strategies [10] as well as rehabilitation adherence [11].
Self-efficacy is a cognitive construct proposed by Albert Bandura within his social cognitive theory as part of the process of self-regulation of behavior [12]. Self-efficacy fosters proactive behaviors and is followed by a personal estimate that certain behaviors will lead to specific results [12]. Bandura proposed four modulating sources of self-efficacy: performance accomplishments, vicarious experience, verbal persuasion, and emotional arousal [12, 13] and a recent meta-analysis seems to confirm this, especially in the first three factors [14].
In osteoarthritis, different forms of self-efficacy have been studies such as pain self-efficacy and arthritis self-efficacy [15,16,17]. In observational studies, pain self-efficacy has been associated with less physical disability [18]. Furthermore, arthritis self-efficacy has been related to fewer depression symptoms, neuroticism, negative affect, better vitality, extraversion, positive affect, problem-solving, and positive thinking [15, 16]. Arthritis self-efficacy may also mediate the association between resilience and pain in osteoarthritis [15] and mediate the effects of telehealth-delivered exercises on pain and disability [19].
In the last decade, different clinical trials [20, 21] and systematic reviews with meta-analysis have evaluated the effectiveness of non-pharmacological approaches to modulate self-efficacy in osteoarthritis [22,23,24,25]. Therefore, it is timely to conduct an overview of reviews that synthetizes these meta-analyses and detect potential gaps in knowledge that allow us to propose future recommendations on this topic. The objective of this overview was to summarize the effectiveness of non-pharmacological interventions to enhance self-efficacy in people with any type of osteoarthritis using systematic reviews with meta-analysis.
Methods
We used the Preferred Reporting Items for Overviews of Reviews (PRIOR) [26] and the Preferred Reporting Items for Systematic Reviews and Meta-Analyses (PRISMA) 2020 for abstracts [27]. The review protocol was prospectively registered at Open Science Framework: https://doi.org/https://doi.org/10.17605/OSF.IO/VX2T6.
Deviations from the review protocol
Several deviations from the review protocol were made. Most of these decisions allowed us to reach more direct conclusions. The overview was only focused on non-pharmacological interventions aiming to modulate self-efficacy. Manual searches including expert opinion and reviews related to our scope were developed. Manual searches in the list of references of the included studies were not conducted. Study selection was eventually developed by one reviewer. Only non-pharmacological interventions were included. Only systematic reviews with meta-analysis were selected. Upset plots were changed to a bar plot.
Search strategies and data sources
One reviewer (JMC) searched the CINAHL (via EBSCOhost), Embase, PsycINFO, PubMed, SPORTDiscus (via EBSCOhost), and the Cochrane Library databases from inception to December 10, 2023. No search filters were applied. The most important search terms were osteoarthritis, arthrosis, self-efficacy, systematic-review, meta-analysis, meta-review, and meta-analytic-review. Supplementary File 1 shows the full search strategy for each electronic database. In addition, the systematic search was checked for completeness with manual search searching for expert opinions, and studies (e.g., systematic reviews or overviews) related to our scope.
Eligibility criteria
One reviewer (JMC) used the Patient, Intervention, Comparison, Outcome, Study Design (PICOS) framework to select studies [28]. We only considered systematic reviews with meta-analyses published in peer-reviewed journals and written in English or Spanish language. The following inclusion criteria were applied: (1) people with any type of osteoarthritis without sociodemographic (e.g., age) and clinical (e.g., duration of symptoms) restrictions, (2) any type of non-pharmacological (e.g., exercise) intervention, (3) any type of control group, (4) any form of self-efficacy assessed as a primary or secondary outcome (e.g., pain self-efficacy or arthritis self-efficacy), and (5) systematic reviews with meta-analysis included non-randomized and randomized clinical trials. Pilot and feasibility trials were also considered.
The exclusion criteria were as follows: (1) conference abstracts or proceedings, (2) thesis dissertations, (3) impossibility of accessing full text, (4) meta-analysis combined studies evaluating osteoarthritis with studies evaluating other populations, (5) meta-analysis combined studies evaluating self-efficacy with studies assessing other factors, (6) preprint, and (7) review protocols.
Study selection
One reviewer (JMC) used Zotero 6.0.9 Citation Management Software to include all references retrieved from the electronic databases. Afterward, this reviewer manually removed duplicates [29] and read titles and abstracts. Then, full texts were evaluated when abstracts seemed eligible or when abstracts were unavailable. No consensus was required.
Methodological quality assessment
Two reviewers (JMS and MIC) used AMSTAR 2 to independently analyze the methodological quality of reviews [30]. This tool is composed of 16 items that can be rated as yes, partial yes, or no. An overall score is not recommended, but seven items are considered critical domains: items 2, 4, 7, 9, 11, 13, and 15 [30]. Disagreements among reviewers were solved by consensus. The two reviewers met by video call and discussed the items where they agreed or disagreed. In those items where they disagreed, they debated them until to reach a consensus. Afterward, the percentage of agreement between these reviewers was calculated. This percentage was calculated considering the number of items JMS and MIC rated with the same score before pooling the results of their independent assessments.
Data extraction
Two reviewers (JMS and MIC) developed data extraction. The reviewers met by video call and discussed the items where they agreed or disagreed. In those items where they disagreed, they debated them until to reach a consensus. The following information was extracted when possible: first author, year of publication, if the authors developed: meta-regressions, subgroup meta-analysis, and sensitivity analysis, if the authors evaluated the certainty of evidence using the GRADE system [31], the replication of the reviewed interventions using the TIDieR checklist [32], and the methodological quality/risk of bias assessment of primary studies. In addition, details regarding interventions, controls, and outcomes of interest were extracted. Finally, the main findings were collected. Disagreements among reviewers were solved by consensus.
Data analysis
Furthermore, we aimed to report in the main text the effects of non-pharmacological interventions reported by type of intervention and type of self-efficacy in the main text. These results were reported narratively and quantitively using the meta-analyses reported by the included reviews. We included as multidisciplinary interventions those reviews that meta-analyzed primary studies that included more than one type of intervention in their experimental groups (e.g., exercise plus diet or exercise plus manual therapy). We made this decision in four reviews, although these reviews focused mainly their objectives on exercise [22, 33], family-based interventions [25], or self-management approaches [34].
We developed citation matrices to calculate the corrected covered area (CCA), which is needed to evaluate the degree of overlap between reviews [35]. The CCA refers to the area that is covered after removing studies the first time they are counted. The degree of overlap between reviews can be classified as slight (CCA 0–5%), moderate (CCA 6–10%), high (CCA 11–15%), or very high (CCA > 15%) [35]. Finally, one reviewer (CGM) built a bar plot to depict the degree of overlap between reviews. We only calculated the CCA when at least two reviews meta-analyzed the same type of intervention.
Results
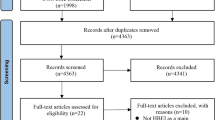
A total of 542 references were retrieved from the electronic databases. Of them, 427 titles and abstracts were read, and the rest (k = 115) were directly removed (duplicates). Then, 189 full texts were analyzed. In addition, seven references were manually found and analyzed in full text. Finally, eight systematic reviews with meta-analysis were included (Fig. 1) [22,23,24,25, 33, 34, 36, 37]. Supplementary File 2 shows the list of excluded studies with reasons. Supplementary File 3 shows the list of studies manually found. Table 1 shows the characteristics of the included reviews.
The degree of overlap between reviews
The degree of overlap between reviews considering all reviews (k = 8) was moderate (CCA = 6%). In addition, the degree of overlap between reviews regarding multidisciplinary or psychological reviews was slight (CCA = 5%) and very high (CCA = 25%), respectively (Fig. 2 and Supplementary Files 4, 5, 6, 7).
Methodological quality assessment
The methodological quality of the included reviews was evaluated with AMSTAR 2 (Table 2, the inter-rater agreement was 86.72%). Overall, the included reviews did not show important methodological flaws. However, some methodological aspects were not completely managed. For example, many reviews did not specify the reasons for selecting a specific research design in their eligibility criteria. The sources of funding for primary studies were not reported by most of the included reviews. In addition, no reviews assessed the impact of the risk of bias of primary studies on the results of the meta-analysis.
Mind–body exercises
Hu et al. 2021 meta-analyzed the effectiveness of tai chi exercises in people with knee osteoarthritis [37]. One meta-analysis of interest was included and showed that this intervention was more effective than education or physical therapy in improving arthritis self-efficacy (SMD = 0.27 [95% CI 0.06 to 0.48], p = 0.01; I2 = 44%). The certainty of evidence using the GRADE system was low.
Multidisciplinary and multimodal interventions
Ariie et al. meta-analyzed the effectiveness of multidisciplinary (e.g., exercise plus psychological intervention) and multimodal (e.g., different exercise modalities) programs in people with knee osteoarthritis [22]. One meta-analysis of interest was included in this overview, which evaluated different forms of self-efficacy: arthritis self-efficacy-pain, pain self-efficacy, and general self-efficacy. Multidisciplinary and multimodal programs with or without usual care were not more effective than usual care alone at 3–10.5 months after the end of the intervention (SMD = 0.04 [95% CI − 0.39 to 0.47], p = 0.85; I2 = 72%, k = 5, N = 329). The certainty of evidence using the GRADE system was very low.
Fritsch et al. 2021 meta-analyzed the effectiveness of family-based interventions (patients plus spouses) based mainly on multidisciplinary interventions (e.g., education plus psychological intervention) in people with osteoarthritis in different body locations (back, hip, and/or knee) [25]. Two meta-analyses of interest were selected and showed that this intervention was not more effective than similar interventions without the involvement of spouses to improve arthritis self-efficacy at ≤ 10 weeks after intervention (SMD = − 8.35 [95% CI − 19.42, 2.71], p = 0.14; I2 = 89%) and > 10 weeks up to 6 months (SMD = − 4.83 [95% CI − 12.24, 2.58], p = 0.20; I2 = 76%). The GRADE system was not applied in these subgroup meta-analyses.
Hurley et al. 2018 meta-analyzed the effectiveness of multidisciplinary interventions including exercise or mind–body exercises (e.g., tai chi) in people with hip or knee osteoarthritis [33]. The global meta-analysis showed that multidisciplinary interventions were more effective than multiple controls (e.g., education, sham intervention, usual care, or waitlist) in enhancing different forms of self-efficacy (e.g., arthritis self-efficacy) from 12 weeks up to 18 months (SMD = 0.46 [95% CI 0.34 to 0.58], p < 0.00001; I2 = 47%, k = 11, N = 1138). The certainty of evidence using the GRADE system was low. In addition, two subgroup meta-analyses were selected and showed that multidisciplinary interventions were more effective than different types of controls (e.g., sham intervention or usual care) in improving arthritis self-efficacy pain (SMD = 0.37 [95% CI 0.11 to 0.63], p = 0.0059; I2 = 77%, k = 2, N = 230) from 12 weeks up to 52 weeks and global arthritis self-efficacy (pain, function, and other symptoms) (SMD = 0.95 [95% CI 0.63 to 1.27], p < 0.00001; I2 = 0%, k = 2, N = 168) at 12 weeks. The GRADE system was not applied in these subgroup meta-analyses.
Kroon et al. 2014 included one meta-analysis of interest evaluating the effectiveness of multidisciplinary interventions in people with hip and/or knee osteoarthritis [34]. This meta-analysis showed that multidisciplinary interventions including education, spoused assisted coping skills training, or exercise were not more effective than different types of control such as education, exercise, or spousal support to improve arthritis self-efficacy immediately after the intervention (SMD = 0.42 [95% CI − 0.05 to 0.89], p = 0.08; I2 = 55.88%, k = 3, N = 186). The GRADE system was not applied in these subgroup meta-analyses.
Psychological interventions
Wang et al. included one meta-analysis of interest analyzing the effectiveness of pain coping skills training in people with hip and/or knee osteoarthritis [24]. This meta-analysis showed that this intervention was more effective than controls (unspecified) in improving arthritis self-efficacy (SMD = 0.27 [95% CI 0.07 to 0.46], p = 0.007; I2 = 55%, k = 8, N = 1114). The follow-up was not specified. The GRADE system was not applied.
Zhang et al. included three meta-analyses of interest also analyzing the effectiveness of coping skills training in people with hip and/or knee osteoarthritis [36]. Mainly, coping skills training strategies included pain coping, spouse coping, and internet-based coping training. The meta-analyses showed that coping skills training is more effective than different controls (e.g., spousal support or usual care) in improving arthritis self-efficacy after intervention (SMD = 0.58 [95% CI 0.40 to 0.75], p < 0.00001; I2 = 4%, k = 5, N = 575), 6 months (SMD (CI 95%) = 0.35 [95% CI 0.10 to 0.60], p = 0.006, I2 = 76%, k = 2, N = 315), and 12 months follow-up (SMD = 0.36 [95% CI 0.10 to 0.63], p = 0.007, I2 = 60%, k = 2, N = 315). The GRADE system was not applied.
Self-management approaches
Wu et al. 2022 included two meta-analyses of interest evaluating the effectiveness of the arthritis self-management program plus usual care in people with knee osteoarthritis [23]. The meta-analyses showed that this intervention was more effective than usual care alone in enhancing arthritis self-efficacy pain (MD = 2.82 [95% CI 0.35 to 5.29], p = 0.03; I2 = 0%, k = 2, N = 197) and arthritis self-efficacy other symptoms (MD = 3.99 [95% CI 1.55 to 6.43], p = 0.001; I2 = 25%, k = 2, N = 197) from 1 to 48 weeks. The GRADE system was not applied in these subgroup meta-analyses.
Discussion
This overview of reviews aimed to summarize the effectiveness of non-pharmacological interventions to enhance different forms of self-efficacy in people with osteoarthritis. Eighth systematic reviews with meta-analysis evaluating 30 different randomized controlled trials were selected. These meta-analyses analyzed the effectiveness of mind–body exercises, multidisciplinary interventions, psychological interventions, and self-management strategies.
Tai chi exercises were the only type of mind–body exercise included in the meta-analyses of interest. This intervention seems to be effective in improving arthritis self-efficacy in people with knee osteoarthritis. Positive effects in favor of tai chi exercises have been found in other types of arthritis. For example, tai chi exercises may enhance psychological factors in people with rheumatoid arthritis such as motivation, self-esteem, and self-efficacy [38]. In addition, tai chi exercises combined with auricular acupressure may enhance pain self-efficacy in this population [39].
Although multidisciplinary interventions mainly including exercise may improve arthritis self-efficacy (e.g., arthritis self-efficacy pain) in people with hip and/or knee osteoarthritis, the effectiveness of these interventions was inconsistent across the meta-analyses [22, 25, 33, 34]. It was not unexpected since important disparities in the type of intervention were observed if we compared the included meta-analyses. For example, Ariie et al. included multidisciplinary (e.g., exercise plus psychological intervention) and multimodal exercise (e.g., aerobic and strengthening) with or without usual care [22], whereas Hurley et al. 2018 included a large number of interventions such as exercise + advice, breathing techniques, counseling, diet, education, family (spouses) coping interventions, manual therapy, mind–body exercises, relaxation techniques, and self-management strategies [33]. In this sense, we encourage readers to be cautious with the conclusions regarding multidisciplinary interventions.
On the other hand, coping skills training based on pain coping skills, spouses coping skills, and internet-based coping skills have shown positive effects in enhancing arthritis self-efficacy in people with hip and/or knee osteoarthritis. These results are also in line with individual studies that have evaluated the importance of coping skills training in other types of arthritis. For example, the combination of pain coping skills training and a lifestyle weight loss intervention has been found to improve self-efficacy for weight control in people with rheumatoid arthritis [40]. In addition, the inclusion of coping skills training in an online program with other psychological interventions such as psychoeducation and stress management may enhance arthritis self-efficacy in adolescents with juvenile idiopathic arthritis [41].
The arthritis self-management program is probably one of the most known interventions to foster self-management strategies in individuals with arthritis. Two meta-analyses found this intervention may produce benefits in improving arthritis self-efficacy for pain and arthritis self-efficacy for other symptoms in people with knee osteoarthritis [23]. Previous results also support these findings in other types of arthritis. For example, a community-based lay-led Arthritis Self-Management Program showed positive results in improving arthritis self-efficacy in people with chronic inflammatory arthritis [42]. This program has also found positive effects on arthritis self-efficacy among individuals with arthritis or fibromyalgia [43].
Altogether, the results of this overview may have important public health and clinical implications. Although recent advances and recommendations have been proposed in the pharmacological management of osteoarthritis [5], evidence also underlines effective disease-modifying drugs are lacking [44]. In this context, EULAR has recently developed eight recommendations to integrate non-pharmacological interventions into current osteoarthritis management protocols [8]. Some of them are in line with the results of this overview. EULAR has proposed that individuals with hip or knee osteoarthritis should be offered strategies for self-management (e.g., information and education) that should be reinforced in booster sessions. Additionally, exercise and mind–body exercises modalities using adequate dosage and mode of delivery, as well as the use of tailoring approaches should be applied according to the preferences of patients and available facilities. We also recommended clinicians to use coping skills training in individuals with osteoarthritis and adapt this intervention factors should be specifically increased. For example, some patients may need to improve their skills to manage pain, whereas other patients may require their spouse help them better handle the course of symptoms.
Limitations
We acknowledge as a limitation of this overview that we only included systematic reviews with meta-analyses published in peer-reviewed journals and written in English or Spanish language. This could cause that important information had been missed. This information may appear in systematic reviews without meta-analysis and other types of research (e.g., thesis dissertation). We also encourage readers to be caution with our findings due to the overlap found between some reviews. Specifically, we observed a very high overlap between reviews exploring psychological interventions. Although some differences were found between the objectives of the included reviews evaluating psychological interventions, these reviews shared clinical trials in their meta-analyses. We encourage authors of systematic reviews to check those databases that register reviews such as PROSPERO, Open Science Framework, or INPLASY before registering their protocols. This may help decrease the degree of overlap on this topic.
Conclusions
Overall, this overview of systematic reviews with meta-analysis can be helpful for clinicians who aim to enhance arthritis self-efficacy in people with hip and/or knee osteoarthritis. Mainly, the results show that tai chi exercises, coping skills training, and the arthritis self-management program may be beneficial for these patients. We encourage the research community in this field to increase the body of knowledge on this topic as well as the use of the GRADE system to reach more robust and direct conclusions.
Clinical messages
-
Tai chi exercises may improve arthritis self-efficacy in people with knee osteoarthritis.
-
Coping skills training may enhance arthritis self-efficacy among individuals with hip and/or knee osteoarthritis.
-
The arthritis self-management program may improve arthritis self-efficacy in people with knee osteoarthritis.
Data availability
All data relevant to the study are included in the article or are available as supplementary files.
References
Arden N, Nevitt MC (2006) Osteoarthritis: epidemiology. Best Pract Res Clin Rheumatol 20:3–25
GBD 2021 Osteoarthritis collaborators (2023) Global, regional and national burden of osteoarthritis 1990–2020 and projections to 2050: a systematic analysis for the Global Burden of Disease Study 2021. Lancet Rheumatol 5(9):e508–22. https://doi.org/10.1016/S2665-9913(23)00163-7
Swain S, Coupland C, Sarmanova A, Kuo CF, Mallen C, Doherty M et al (2023) Healthcare utilisation and mortality in people with osteoarthritis in the UK: findings from a national primary care database. Br J Gen Pract J R Coll Gen Pract 73:e615–e622
Jung JH, Seok H, Kim J-H, Song GG, Choi SJ (2018) Association between osteoarthritis and mental health in a Korean population: a nationwide study. Int J Rheum Dis 21:611–619
Alexander LAM, Ln D, Eg Z, Is D, Ay K, Ss R et al (2021) Pharmacological Management of osteoarthritis with a focus on symptomatic slow-acting drugs: recommendations from leading Russian experts. J Clin Rheumatol Pract Rep Rheum Musculoskelet Dis 27:e533–e539
Patel S, Gahlaut S, Thami T, Chouhan DK, Jain A, Dhillon MS (2024) Comparison of conventional dose versus superdose platelet-rich plasma for knee osteoarthritis: a prospective, triple-blind, randomized clinical trial. Orthop J Sports Med 12:23259671241227864
Bierma-Zeinstra S, van Middelkoop M, Runhaar J, Schiphof D (2020) Nonpharmacological and nonsurgical approaches in OA. Best Pract Res Clin Rheumatol 34:101564
Moseng T, Vliet Vlieland TPM, Battista S, Beckwée D, Boyadzhieva V, Conaghan PG, Costa D, Doherty M, Finney AG, Georgiev T, Gobbo M, Kennedy N, Kjeken I, Kroon FPB, Lohmander LS, Lund H, Mallen CD, Pavelka K, Pitsillidou IA, Rayman MP, Tveter AT, Vriezekolk JE, Wiek D, Zanoli G, Østerås N (2024) EULAR recommendations for the non-pharmacological core management of hip and knee osteoarthritis: 2023 update. Ann Rheum Dis ard-2023–225041. https://doi.org/10.1136/ard-2023-225041
Kloppenburg M, Kroon FP, Blanco FJ, Doherty M, Dziedzic KS, Greibrokk E et al (2019) 2018 update of the EULAR recommendations for the management of hand osteoarthritis. Ann Rheum Dis 78:16–24
Lorig KR, Holman H (2003) Self-management education: history, definition, outcomes, and mechanisms. Ann Behav Med Publ Soc Behav Med 26:1–7
Picha KJ, Howell DM (2018) A model to increase rehabilitation adherence to home exercise programmes in patients with varying levels of self-efficacy. Musculoskeletal Care 16:233–237
Bandura A (1977) Self-efficacy: toward a unifying theory of behavioral change. Psychol Rev 84:191–215
Bandura A (1982) Self-efficacy mechanism in human agency. Am Psychol 37:122–147
Byars-Winston A, Diestelmann J, Savoy JN, Hoyt WT (2017) Unique effects and moderators of effects of sources on self-efficacy: a model-based meta-analysis. J Couns Psychol 64:645–658
Wright LJ, Zautra AJ, Going S (2008) Adaptation to early knee osteoarthritis: the role of risk, resilience, and disease severity on pain and physical functioning. Ann Behav Med Publ Soc Behav Med 36:70–80
Uritani D, Kubo T, Yasuura Y, Fujii T (2023) Reliability and validity of the Japanese short-form arthritis self-efficacy scale in patients with knee osteoarthritis: a cross-sectional study. PLoS ONE 18:e0292426
Jayakumar P, Crijns TJ, Misciagna W, Manickas-Hill O, Malay M, Jiranek W, Mather RC 3rd, Lentz TA (2024) What are the underlying mental health constructs associated with level of capability in people with knee and hip osteoarthritis? Clin Orthop Relat Res 482(4):633–44. https://doi.org/10.1097/CORR.0000000000003003
Nanjo K, Ikeda T, Nagashio N, Sakai T, Jinno T (2023) Psychological factors associated with instrumental activities of daily living disability in older adults with moderate to severe knee osteoarthritis. J Back Musculoskelet Rehabil 36:911–920
Lawford BJ, Hinman RS, McManus F, Lamb KE, Egerton T, Keating C et al (2023) How does exercise, with and without diet, improve pain and function in knee osteoarthritis? A secondary analysis of a randomized controlled trial exploring potential mediators of effects. Arthritis Care Res 75:2316–2327
Kania-Richmond A, Beaupre LA, Jessiman-Perreault G, Tribo D, Martyn J, Hart DA et al (2024) “I do hope more people can benefit from it.”: the qualitative experience of individuals living with osteoarthritis who participated in the GLA:DTM program in Alberta. Canada. PloS One 19:e0298618
Davis AM, Kennedy D, Wong R, Robarts S, Skou ST, McGlasson R et al (2018) Cross-cultural adaptation and implementation of Good Life with osteoarthritis in Denmark (GLA:D™): group education and exercise for hip and knee osteoarthritis is feasible in Canada. Osteoarthritis Cartilage 26:211–219
Ariie T, Takasaki H, Okoba R, Chiba H, Handa Y, Miki T et al (2023) The effectiveness of exercise with behavior change techniques in people with knee osteoarthritis: a systematic review with meta-analysis. PM R 15:1012–1025
Wu Z, Zhou R, Zhu Y, Zeng Z, Ye Z, Wang Z, Liu W, Xu X (2022) Self-management for knee osteoarthritis: a systematic review and meta-analysis of randomized controlled trials. Pain Res Manag 2022:2681240. https://doi.org/10.1155/2022/2681240
Wang L, Zhang L, Yang L, Cheng-qi H (2021) Effectiveness of pain coping skills training on pain, physical function, and psychological outcomes in patients with osteoarthritis: a systemic review and meta-analysis. Clin Rehabil 35:342–355
Fritsch CG, Ferreira ML, Da Silva AKF, Simic M, Dunn KM, Campbell P et al (2021) Family-based interventions benefit individuals with musculoskeletal pain in the short-term but not in the long-term: a systematic review and meta-analysis. Clin J Pain 37:140–157
Gates M, Gates A, Pieper D, Fernandes RM, Tricco AC, Moher D et al (2022) Reporting guideline for overviews of reviews of healthcare interventions: development of the PRIOR statement. BMJ 378:e070849
Beller EM, Glasziou PP, Altman DG, Hopewell S, Bastian H, Chalmers I et al (2013) PRISMA for abstracts: reporting systematic reviews in journal and conference abstracts. PLoS Med 10:e1001419
Richardson WS, Wilson MC, Nishikawa J, Hayward RS (1995) The well-built clinical question: a key to evidence-based decisions. ACP J Club 123:A12–A13
Kwon Y, Lemieux M, McTavish JWN (2015) Identifying and removing duplicate records from systematic review searches. J Med Libr Assoc 103:184–188
Shea BJ, Reeves BC, Wells G, Thuku M, Hamel C, Moran J et al (2017) AMSTAR 2: a critical appraisal tool for systematic reviews that include randomised or non-randomised studies of healthcare interventions, or both. BMJ Online 358:1–9
Schünemann H, Brożek J, Guyatt G, Oxman A (eds) (2013) GRADE handbook for grading quality of evidence and strength of recommendations. Updated October 2013. The GRADE Working Group. Available from https://guidelinedevelopment.org/handbook.
Hoffmann TC, Glasziou PP, Boutron I, Milne R, Perera R, Moher D et al (2014) Better reporting of interventions: template for intervention description and replication (TIDieR) checklist and guide. BMJ 348:g1687
Hurley M, Dickson K, Hallett R, Grant R, Hauari H, Walsh N et al (2018) Exercise interventions and patient beliefs for people with hip, knee or hip and knee osteoarthritis: a mixed methods review. Cochrane Database Syst Rev 4:CD010842
Kroon FPB, van der Burg LRA, Buchbinder R, Osborne RH, Johnston RV, Pitt V (2014) Self-management education programmes for osteoarthritis. Cochrane Database Syst Rev (1):CD008963. https://doi.org/10.1002/14651858.CD008963.pub2
Pieper D, Antoine SL, Mathes T, Neugebauer EAM, Eikermann M (2014) Systematic review finds overlapping reviews were not mentioned in every other overview. J Clin Epidemiol 67:368–375
Zhang L, Fu T, Zhang Q, Yin R, Zhu L, He Y et al (2018) Effects of psychological interventions for patients with osteoarthritis: a systematic review and meta-analysis. Psychol Health Med 23:1–17
Hu L, Wang Y, Liu X, Ji X, Ma Y, Man S et al (2021) Tai Chi exercise can ameliorate physical and mental health of patients with knee osteoarthritis: systematic review and meta-analysis. Clin Rehabil 35:64–79
Waite-Jones JM, Hale CA, Lee H-Y (2013) Psychosocial effects of Tai Chi exercise on people with rheumatoid arthritis. J Clin Nurs 22:3053–3061
Lee H-Y, Hale CA, Hemingway B, Woolridge MW (2012) Tai Chi exercise and auricular acupressure for people with rheumatoid arthritis: an evaluation study. J Clin Nurs 21:2812–2822
Somers TJ, Blumenthal JA, Dorfman CS, Huffman KM, Edmond SN, Miller SN et al (2022) Effects of a weight and pain management program in patients with rheumatoid arthritis with obesity: a randomized controlled pilot investigation. J Clin Rheumatol Pract Rep Rheum Musculoskelet Dis 28:7–13
Connelly M, Schanberg LE, Ardoin S, Blakley M, Carrasco R, Chira P et al (2019) Multisite randomized clinical trial evaluating an online self-management program for adolescents with juvenile idiopathic arthritis. J Pediatr Psychol 44:363–374
Leung Y-Y, Kwan J, Chan P, Poon PKK, Leung C, Tam L-S et al (2016) A pilot evaluation of arthritis self-management program by lay leaders in patients with chronic inflammatory arthritis in Hong Kong. Clin Rheumatol 35:935–941
Lorig KR, Ritter PL, Laurent DD, Plant K (2008) The internet-based arthritis self-management program: a one-year randomized trial for patients with arthritis or fibromyalgia. Arthritis Rheum 59:1009–1017
Hunter DJ, Bierma-Zeinstra S (2019) Osteoarthritis. Lancet Lond Engl 393:1745–1759
Author information
Authors and Affiliations
Contributions
Conceptualization: JMC; data curation: JMC, JMS, and MIC; formal analysis: JMC, JMS, CGM, and MIC; funding acquisition: not applicable; investigation: not applicable; methodology: JMC, JMS, CGM, and MIC; project administration: JMC; resources: not applicable; software: CGM; supervision: JMC; validation: not applicable; visualization: not applicable; writing—original draft: FJCG, CRB, and JMC; writing—review and editing: all authors.
Corresponding author
Ethics declarations
Consent to participate
Not applicable.
Disclosures
None.
Additional information
Publisher's Note
Springer Nature remains neutral with regard to jurisdictional claims in published maps and institutional affiliations.
Supplementary information
Below is the link to the electronic supplementary material.
Rights and permissions
Springer Nature or its licensor (e.g. a society or other partner) holds exclusive rights to this article under a publishing agreement with the author(s) or other rightsholder(s); author self-archiving of the accepted manuscript version of this article is solely governed by the terms of such publishing agreement and applicable law.
About this article
Cite this article
Martinez-Calderon, J., Cano-García, F.J., García-Muñoz, C. et al. How can clinicians enhance self-efficacy beliefs in osteoarthritis? An overview of systematic reviews with meta-analysis. Clin Rheumatol 43, 1435–1446 (2024). https://doi.org/10.1007/s10067-024-06943-2
Received:
Revised:
Accepted:
Published:
Issue Date:
DOI: https://doi.org/10.1007/s10067-024-06943-2